Abstract
The aim of this study was to investigate the effects of low-level laser (LLL) irradiation on the turnover of fibronectin and collagen type I in periodontal tissue during tooth movement in rats by immunohistochemistry. Thirty male Sprague–Dawley rats aged 15 weeks were assigned to either an experimental group (n = 15) that underwent LLL irradiation during tooth movement, or a control group (n = 15). In the experimental group, the gallium–aluminum–arsenide (Ga-Al-As) diode LLL (wavelength 808 nm; output 96 mW) was used to irradiate three areas on both the palatal side and the labial side of the maxillary incisor. The radiation was administered by the contact method for 10 s at 0.83 J/cm2 energy dose, once a day for 7 days. Total energy dose over the complete schedule was 34.86 J/cm2. The animals were killed on days 1, 3, 7, 14 and 21. There was no difference between the two groups in the amount of tooth movement. The immunohistochemistry results showed that the expression of fibronectin and collagen type I in the experimental group had significantly increased from day 1, with a more even distribution than in the control group, and that this difference was maintained until the end of the experiment. These results suggest that LLL irradiation facilitates the reorganization of the connective tissues during tooth movement in rats.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Orthodontic treatment is a process of achieving appropriate bite functions and esthetics by the movement of a tooth through the application of an external physical force. In order to obtain physiological tissue reactions around a tooth, while avoiding the side effects of an external force, however, long-term therapy of as long as 2 to 3 years is required. Accordingly, faster tooth movement without harmful effect on periodontal tissue has been an issue of significant interest to patients as well as orthodontists.
In an effort to achieve efficient tooth movement, many scientists have employed biochemical methods involving medicines such as prostaglandin E2 (PGE2) [1], 1,25-dihydroxyvitamin D3 (1,25-(OH)2D3) [2] and parathyroid hormone [3]. However, they had an influence on body metabolism, and, for that reason, their application to orthodontics is difficult [4].
Recently, many researchers have shown that low-level laser (LLL) affects the proliferation of fibroblasts and collagen synthesis [5–7]. Therapeutic methods using the under 500 mW range are called low-level laser therapies (LLLTs), and they have a bio-stimulatory effect on the tissue [8]. LLL therapy was defined as being performed with a low-energy output that does not increase the tissue temperature of the treated region above the normal body temperature.
In the dental area, there have been reports on effects such as pain reduction after dental treatment, [9] mucositis, [10] nerve damage following extraction of the third molar, [11] paralysis after jaw surgery, [12] and implant stability [13–15]. In orthodontics as well, various studies have been performed to enhance the treatment’s effects, such as rapid palatal expansion [16], pain reduction after orthodontic force application, [17] and rapid tooth movement [18]. However, they have seldom focused on the changes in the connective tissue surrounding the moving tooth.
Maintenance of the periodontium during tooth movement requires the balance of proliferation and differentiation of extracellular matrix [19]. With regard to the matrix molecules, collagen type I is abundant at the periodontal ligament space, and fibronectin is apparent throughout the mesenchyme [20]. Fibronectins are located above collagen fibers and support the proliferation and chemotaxis of periodontal ligament fibroblasts [21]. In addition, cultures of periodontal ligament fibroblasts in vitro have revealed increasing production of collagen type I and fibronectin in response to mechanical stress [22]. Therefore, changes in collagen type I and fibronectin expression demonstrate the effect of LLL irradiation on tooth movement. The aim of this study was to determine the effects of LLL irradiation on the periodontal tissue surrounding the tooth during tooth movement in rats.
Materials and methods
Experimental tooth movement and low-level laser irradiation
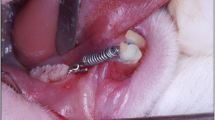
The experiment was performed on 30 male Sprague–Dawley rats of body weights ranging from 300 g to 350 g. The rats were randomly assigned to an LLL-irradiated group (n = 15) or a control group (n = 15). They were cared for in accordance with national guidelines for laboratory animals. Elastic rubber ligatures (Unistick colored ligatures, American Orthodontics, Sheboygan, WI, USA) were inserted into the maxillary inter-incisal area and kept there during the experiments. The magnitude of the force was approximately 19.6 ± 3.2 g in both groups. A gallium–aluminum–arsenide (Ga-Al-As) diode LLL (500DPSS®, LVI Technology, Seoul, Korea) of 808 nm wavelength, 0.384 cm diameter, 96 mW output, and 0.83 J/cm2 dose irradiation was used. The three gingival regions of the labial and palatal sides of the maxillary incisors of the rats in the experimental group were irradiated for 10 s by the contact method. Such laser irradiation was applied to the above regions once a day for 7 days, according to the following outputs: energy dose per point, 0.83 J/cm2; total energy dose per session at six points, 4.98 J/cm2; total energy dose over the complete schedule, 34.86 J/cm2. All animals in the experimental and control groups were killed on days 1, 2, 7, 14, and 21 following tooth movement. The study was approved by the Committee of Ethics in Research at the Pusan National University Hospital, Pusan, Korea, under protocol number 01/2006.
Immunohistochemistry of fibronectin and collagen type I
The animals were anesthetized with a mixture of 10 mg/kg of xylazine hydrochloride (Rompun®, Bayer, Korea) and 100 mg/kg of ketamine chloride (Ketalar®, Yuhan Corporation, Korea), administered by intramuscular injection. To fix tissues by cardiac perfusion, we washed the blood in the body for 20 min with phosphate-buffered saline (PBS) solution. Then, a 4% paraformaldehyde fixing agent of pH 7.2 was injected for 30 min with a perfusion pump. Immediately after perfusion fixing, the maxillary bone, including the incisors, was sectioned to a 1 cm2 thickness. The sections were decalcified for 7 weeks with a decalcification agent formulated by the dissolution of 250 g of ethylenediamine tetra-acetic acid (EDTA) and 25 g of sodium hydroxide (NaOH) in 1,750 ml of distilled water. Subsequently, the tissue was put into a tissue capsule and washed for 12 h in running water. Then, it was dehydrated and made transparent with alcohol and xylene, in the normal way, and afterwards was embedded in paraffin to make sagittal serial sections of 6 μm thickness. The paraffin was removed from the tissue sections with xylene. The sections were passed through graded alcohol and washed in running water. To eliminate the endogenous peroxidase, we treated the sections for 20 min in absolute methyl alcohol added to 0.3% hydrogen peroxide and then washed them in PBS solution three times for 10 min. We applied normal goat serum (5%) for 30 minutes, to determine the fibronectin distribution, and normal horse serum (5%) for 30 min, to identify the distribution of collagen type I. Then, the tissue sections were softly blotted without being washed, and rabbit anti-human fibronectin (the first antibody) (DAKO, Denmark) diluted with mouse anti-human collagen type I (Serotec, USA) at a ratio of 1:400 was applied for 16 h at 4°C. After that, the sections were washed in PBS solution three times for 10 min, and biotinylated goat anti-rabbit immunoglobulin G (IgG) (the second antibody) (Verotor Lab., USA) diluted with biotinylated horse anti-mouse IgG (Verotor Lab) at a ratio of 1:200 was applied for 1 h at room temperature. Thereafter, the tissue sections were washed in PBS solution three times for 10 min each, and a solution of avidin–biotin horseradish peroxidase complex (ABC) (A 10 μl, B 10 μl in 1 ml PBS solution, Verotor Lab.), formulated and left at room temperature for 30 min before, was applied to the tissue sections for 1 h at room temperature. Thereafter, the tissue sections were washed in PBS solution three times for 10 min and was colored for 3 min in a solution mixed with 0.05 M Tris-HCl buffer of pH 7.6, 0.05% diaminobenzidine (DAB) and 0.01% hydrogen peroxidase. Then, the sections were washed in Tris buffer, PBS solution and distilled water for 10 min each. After that, they were counterstained with Harris hematoxylin and sealed with Pemount (Polysciences, USA). All the sections of each specimen were viewed with a light microscope (Axioskope, Carl Zeiss, Germany) and photographically recorded with graphics software (Axiovision rel. 4.5, Carl Zeiss, German).
The distribution and localization of the antibody staining pattern were assessed. The intensity of the staining for each antibody was determined by a semi-qualitative assessment. Immunoreactivity for each of the antibodies in the tissue sections was given a score (0.+,++,+++). The scores ranged from negative stain (0) to very strong positive stain (+++). A score of + represented tissues that had positive weak staining, and a score of ++ represented tissues that had positive strong staining.
Results
Histologically, there was revealed a dense connective tissue, with a variable number of fibroblasts, osteoblasts, and undifferentiated mesenchymal cells all arranged among collagen fibers and blood vessels. The immunohistochemistry showed positive staining for fibronectin on the tension side in both groups from the first day, but the degree of expression in the experimental group was high and the distribution was also even (Fig. 1, Table 1). This state was maintained until day 3. From day 7, a decrease in the degree of expression was found on the pressure side in the control group (Fig. 2). By contrast, high expression was maintained in the experimental group, and the distribution was even on both the pressure and tension sides. Overall, the degree of fibronectin expression was stronger and more even in the experimental group than in the control group throughout the observation period.
Photomicrographs of fibronectin expression. a One day after experimental tooth movement in the experimental group (EX); b 1 day after experimental tooth movement in the control group (CO); c 3 days after (EX); d 3 days after (CO); e 21 days after (EX); f 21 days after (CO). Comparing a and b, c and d, e and f, we found that the expression of fibronectin in rats in the experimental group was significantly greater than that in rats in the control group. Black arrows strong expression area; white arrows weak expression area. Sagittal section, 6 μm thick, tension side, ×100. DR dental root, PDL periodontal ligament, ALB alveolar bone
Photomicrographs of fibronectin expression in rats in the control group. a Seven days, pressure side; b 7 days, tension side; c 14 days, pressure side; d 14 days, tension side. Black arrows strong expression area; white arrows weak expression area. Sagittal section, 6 μm thick, ×400. DR dental root, PDL periodontal ligament, ALB alveolar bone
An immunohistochemical expression of collagen type I in the experimental group was higher than in the control group during all experimental periods (Fig. 3, Table 2). Reorganization of collagen fibrils in the experimental group was high from 1 day, but that in the control group increased from day 7.
Photomicrographs of collagen type I expression. a 1 day after experimental tooth movement in the experimental group (EX); b 1 day after experimental tooth movement in the control group (CO); c 3 days after (EX); d 3 days after (CO); e 21 days after (EX); f 21 days after (CO). Comparing a and b, c and d, e and f, we found that the expression of collagen type I in the rats in the experimental group was significantly greater than that in the rats in the control group. Arrows strong expression area. Sagittal section, 6 μm thick, tension side, ×100. R dental root, P periodontal ligament, AB alveolar bone
Discussion
For LLL irradiation, many researchers have described the anabolic effects, such as acceleration of bone formation [16], attachment of bone contact to implant surface [14, 15], and tooth movement by bone resorption and formation [23]. However, its effect on tissue reorganization by tooth movement has not been shown. We performed our study to investigate the effect of LLL irradiation on periodontal tissue reorganization during tooth movement in rats.
We initiated tooth movement in this study by inserting an elastic rubber ligature between the maxillary incisors. A force (19.6 ± 3.2 g) of this magnitude does not to cause blood vessel breakdown [24, 25]. Tooth movement took place through direct bone resorption, and the blood vessels contacting the bone surface of the periodontal ligament space were extended but retained their integrity (Fig. 1b,e). In experimental tooth movement in rats, Kawasaki and Shimizu [26] showed that the amount of tooth movement in an LLL irradiation group was significantly greater than that of a group that was not irradiated. As there were no data on the mechanical properties of the elastic rubber ligatures, such as force decay, we did not investigate the differences in the amounts of tooth movement affected by LLL irradiation, but we investigated the histological changes brought about by LLL irradiation in the surrounding tissues.
With respect to the output amount and capacity of LLL, Cruz et al. [27] conducted an experiment on 11 young patients who required tooth movement for extraction space closure. They were irradiated with LLL of 780 nm wavelength (for 10 s at 20 mW; 5 J/cm2) on one side of the maxilla for 4 days in a month and were not irradiated on the opposite side, which acted as the control. The results showed that the experimental side demonstrated significantly more rapid progression of space closure than the control side. Following tooth movement experiments on 12 young adults, however, Limpanichkul et al. [18] reported that no difference was found in tooth movement rate after application of LLL for 3 days in a month. They concluded that the energy capacity of LLL (25 J/cm2) in their study was probably too low to produce stimulatory effects on orthodontic tooth movement. However, their LLL application method for orthodontic tooth movement was different from ours. They used a 0.09 cm2 spectral area to irradiate the alveolar mucosa at some point. This restricted application might be a lack for the whole periodontium surrounding the tooth.
Recently, Seifi et al. [28] reported the effects of two types of LLL wavelengths (850 nm and 630 nm) on orthodontic tooth movements in rabbits. The total amount of energy in 850 nm and 630 nm laser groups was 8.1 J/cm2 and 27 J/cm2, respectively. The authors showed that the amount of orthodontic tooth movement, after LLL application, was diminished, and there was no significant difference between the laser groups. This seems to have been the result of varying laser power density. Breugel and Bär [29] showed that the power density of helium–neon (He-Ne) laser irradiation was more important than the total energy dose in the bio-modulation of human fibroblasts in vitro. Their application power density of 5 mW might be low to cause the bio-stimulation.
As to the difference in effects due to capacity application methods, Saito and Shimizu, [30] and Ozawa et al. [31] reported that repetitive irradiation for more than 3 days more than doubled the bio-stimulatory effects of LLL irradiation. Additionally, they reported that the energy capacity suitable for bio-stimulation was 0.5–10 J/cm2. Accordingly, in our study as well, LLL irradiation was employed at a wavelength of 808 nm (power density of 96 mW; 4.98 J/cm2 once a day) and this seems to have been enough to cause bio-stimulation.
A mechanical load incurring orthodontic tooth movement transforms extracellular substrates in the periodontal ligament, which are, in turn, transmitted to cell skeletons through cell surface proteins [32]. Fibronectin, which is synthesized in osteoblasts and fibroblasts, is a high-molecular-weight glycoprotein that is distributed in all extracellular substrates [33]. It is attached to collagen and plays an important role in cell movement and differentiation during periodontal ligament reorganization. Howard et al. [34] reported that when a tensile force was applied to a fibroblast cultured from an extracted molar, fibronection synthesis increased conspicuously. Immunohistochemical expression of fibronectin, in our study, was also observed in the periodontal ligament from day 1 of tooth movement in both groups (Fig. 1, Table 1). However, the degree of expression was much higher in the experimental group, and the distribution was even. The findings on day 7 following tooth movement showed a sharp drop in the degree of expression on the pressure side of the control group (Fig. 2).
Collagen represents a major element of an extracellular substrate, and it is known that collagen type I is most frequently found in connective tissues (Fig. 3, Table 2). Especially, periodontal ligament shows a high collagen replacement rate, whether it is a physiologic or a pathologic change. Yamamoto et al. [35] and Skinner et al. [36] found that LLL irradiation affected collagen metabolism in cultured cells. However, Marques et al. [5] showed that LLL (904 nm, 3 J/cm2) irradiation causes ultrastructural changes in cultured fibroblasts and decreases the amount of protein synthesis. In our study, immunohistochemical localization of collagen type I in the alveolar bone and the periodontal ligament was observed from day 1 in both groups. As time passed, an increase in the expression of collagen type I was clearly observed in the experimental group in comparison with the control group. Also, the distribution of collagen type I was more even in the experimental group. This result differed from that of Marques et al. [5]. This seems to be the experimental state of cultured cells resulting from the external orthodontic force in this study. In the normal state of cultured cells, protein synthesis showed no differences between LLL irradiation and non-irradiation. Under an inflammation state of tissue, however, LLL irradiation might stimulate protein synthesis. Further studies will be required to investigate different effects between normal and inflamed tissues. As with the expression of fibronectin, this seems to indicate that LLL irradiation facilitates the reorganization of the connective tissues of the periodontal ligament and the alveolar bone in orthodontic treatment.
Many researchers have reported the effect of LLL irradiation on cellular responses [17, 31]. Conlan et al. [37] showed that the stimulation of photoreceptors in the mitochondrial respiratory chain changed the cellular adenosine triphosphate (ATP) levels and cell membrane stabilization through bioelectric effects. Like these, it is generally accepted that the LLL irradiation effects on cells are wavelength and dose dependent, and molecular absorption of laser light is a prerequisite for any cellular effect. Our study also found that the reorganization of the periodontal tissues could be further facilitated with the addition of LLL irradiation by immunohistochemistry. Because of the difference in changes between animal and human periodontal tissue, however, we were not able to characterize the exact mechanism of the bio-stimulatory effect of LLL irradiation on the human physiologic state. Further investigations, using LLL, for a suitable application method for humans would be required.
Conclusions
The Ga-Al-As diode LLL (wavelength 808 nm; output 96 mW; energy dose per point 0.83 J/cm2; 10 s each time in a contact method with a 4.98 J/cm2 dose once a day for 7 days) increased the expression of fibronectin and collagen type I in the experimental group from the first day of the experiment, with an even distribution, and this difference was maintained until the end of the experiment. This result suggests that LLL irradiation facilitates the turnover of connective tissues during tooth movement in rats.
References
Yamasaki K, Shibata Y, Fukuhara T (1982) The effect of prostaglandins on experimental tooth movement in monkeys (Macaca fuscata). J Dent Res 61:1444–1446
Yamamoto T, Kawakami M, Kobayasi Y (1992) The effect of local application of 1,25-dihydroxycholecalciferol on osteoclast numbers in orthodontically treated rats. J Dent Res 71:53–59
Soma S, Iwamoto M, Higuchi Y, Kurisu K (1999) Effect of continuous infusion of PTH on experimental tooth movement. J Bone Miner Res 14:546–554 doi:10.1359/jbmr.1999.14.4.546
Pongsri B, Per R (1991) Root resorption after local injection of prostaglandin E2 during experimental tooth movement. Eur J Orthod 13:255–263
Marques MM, Pereira AN, Fujihara NA, Nogueira FN, Eduardo CP (2004) Effect of low-power laser irradiation on protein synthesis and ultrastructure of human gingival fibroblasts. Lasers Surg Med 34:260–265 doi:10.1002/lsm.20008
Pourzarandian A, Watanabe H, Ruwanpura SMPM, Aoki A, Ishikawa I (2005) Effect of low-level Er:Yag laser irradiation on cultured human gingival fibroblasts. J Periodontol 76:187–193 doi:10.1902/jop.2005.76.2.187
Kreisler M, Christoffers AB, Willerstausen B, d’Hoedt B (2003) Effect of low-level GaAlAs laser irradiation on the proliferation rate of human periodontal ligament fibroblasts: an in vitro study. J Clin Periodontol 30:353–358 doi:10.1034/j.1600-051X.2003.00001.x
Mester E, Mester AF, Mester A (1985) The biomedical effects of laser application. Lasers Surg Med 5:31–39 doi:10.1002/lsm.1900050105
Gerschman JA, Ruben J, Gebart-Eaglemont J (1994) Low level laser therapy for dentinal tooth hypersensitivity. Aust Dent J 39:353–357
Bensadoun RJ, Franqiun JC, Ciasis G, Darcourt V, Schubert MM, Viot M et al (1999) Low-energy He/Ne laser in the prevention of radiation-induced mucositis. A multicenter phase III randomized study in patients with head and neck cancer. Support Care Cancer 7:244–252 doi:10.1007/s005200050256
Khullar SM, Brodin P, Barkvoll P, Haanaes HR (1996) Preliminary study of low-level laser for treatment of long-standing sensory aberrations in the inferior alveolar nerve. J Oral Maxillofac Surg 54:2–7 doi:10.1016/S0278-2391(96)90290-6
Khullar SM, Emami B, Westermark A, Haanaes HR (1996) Effect of low-level laser treatment on neurosensory deficits subsequent to sagittal split ramus osteotomy. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 82:132–138 doi:10.1016/S1079-2104(96)80215-0
Khadra M, Lyngstadaas SP, Haanaes HR, Mustafa K (2005) Effect of laser therapy on attachment, proliferation and differentiation of human osteoblast-like cells cultured on titanium implant material. Biomaterials 26:3503–3509 doi:10.1016/j.biomaterials.2004.09.033
Kim YD, Kim SS, Hwang DS et al (2007) Effect of low-level laser treatment after installation of dental titanium implant—immunohistochemical study of RANKL, RANK, OPG: an experimental study in rats. Lasers Surg Med 39:441–450 doi:10.1002/lsm.20508
Kim YD, Kim SS, Hwang DS et al (2007) Effect of low-level laser treatment after installation of dental titanium implant—immunohistochemical study of vascular endothelial growth factor: an experimental study in rats. Laser Phys Lett 4:681–685 doi:10.1002/lapl.200710036
Saito S, Shimizu N (1997) Stimulatory effects of low-power laser irradiation on bone regeneration in mid-palatal suture during expansion in rat. Am J Orthod Dent Orthop 111:525–532 doi:10.1016/S0889-5406(97)70152-5
Lim HM, Lew KK, Tay DK (1995) A clinical investigation of the efficacy of low level laser therapy in reducing orthodontic postadjustment pain. Am J Orthod Dentofacial Orthop 108:614–622 doi:10.1016/S0889-5406(95)70007-2
Limpanichkul W, Godfrey K, Srisuk N, Rattanayatikul C (2006) Effects of low-level laser therapy on the rate of orthodontic tooth movement. Orthod Craniofac Res 9:38–43 doi:10.1111/j.1601-6343.2006.00338.x
Mussig E, Tomakidi P, Steinberg T (2005) Molecules contributing to the maintenance of periodontal tissues. J Orofac Orthop 66:422–433 doi:10.1007/s00056-005-0520-6
Pitaru S, Aubin JE, Bhargava U, Melcher AH (1987) Immunoelectron microscopic studies on the distributions of fibronectin and actin in a cellular dense connective tissue: the periodontal ligament of the rat. J Periodontal Res 22:64–74 doi:10.1111/j.1600-0765.1987.tb01541.x
Kapila YL, Lancero H, Johnson PW (1998) The response of periodontal ligament cells to fibronectin. J Periodontol 69:1008–1019
Howard PS, Kucich U, Taliwal R, Korostoff JM (1998) Mechanical forces alter extracellular matrix synthesis by human periodontal ligament fibroblasts. J Periodontal Res 33:500–508
Kim YD, Kim SS, Kim TG, Kim GC, Park SB, Son WS (2007) Effect of low-level laser treatment during tooth movement—immunohistochemical study of RANKL, RANK, OPG: an experimental study in rats. Laser Phys Lett 4:616–623 doi:10.1002/lapl.200710032
Ren Y, Mantha JC, Juijpers-Jagtman A (2003) Optimum force magnitude for orthodontic tooth movement: a systematic literature review. Angle Orthod 73:86–92
Ren Y, Maltha JC, Kuijpers-Jagtman A (2004) The rat as model for orthodontic tooth movement—a critical review and a proposed solution. Eur J Orthod 26:483–490 doi:10.1093/ejo/26.5.483
Kawasaki K, Shimizu N (2000) Effects of low-energy laser irradiation on bone remodeling during experimental tooth movement in rats. Lasers Surg Med 26:282–291 doi:10.1002/(SICI)1096–9101(2000)26:3<282::AID–LSM6>3.0.CO;2–X
Cruz DR, Kohara EK, Ribeiro MS, Wetter NU (2004) Effects of low-intensity laser therapy on the orthodontic movement velocity of human teeth: a preliminary study. Lasers Surg Med 35:117–120 doi:10.1002/lsm.20076
Seifi M, Shafeei HL, Daneshdoost S, Mir M (2007) Effects of two types of low-level laser wave lengths (850 and 630 nm) on the orthodontic tooth movements in rabbits. Lasers Med Sci 22:261–264 doi:10.1007/s10103-007-0447-9
von Breugel HHFI, Bär D (1992) Power density and exposure time of He-Ne laser irradiation are more important than total energy dose in photo-biomodulation of human fibroblasts in vitro. Lasers Surg Med 12:528–537 doi:10.1002/lsm.1900120512
Saito S, Shimizu N (1997) Stimulatory effects of low-power laser irradiation on bone regeneration in mid-palatal suture during expansion in the rat. Am J Orthod Dent Orthop 111:525–532 doi:10.1016/S0889-5406(97)70152-5
Ozawa Y, Shimizu N, Kariya G, Abiko Y (1998) Low-energy laser irradiation stimulates bone nodule formation at early stages of cell culture in rat calvarial cells. Bone 22:347–354 doi:10.1016/S8756-3282(97)00294-9
Krishnan V, Davidovitch Z (2006) Cellular, molecular, and tissue-level reactions to orthodontic force. Am J Orthod Dentofacial Orthop 129:469, e1–32
Hynes RO (1992) Integrins: versatility, modulation, and signal in cell adhesion. Cell 69:11–25 doi:10.1016/0092-8674(92)90115-S
Howard PS, Kucich U, Taliwal R, Korostoff JM (1998) Mechanical forces alter extracellular matrix synthesis by human periodontal ligament fibroblast. J Periodont Res 33:500–508
Yamamoto Y, Kono T, Kotani H, Kasai S, Mito M (1996) Effect of low-power laser irradiation on procollagen synthesis in human fibroblasts. J Clin Laser Med Surg 14:129–132
Skinner SM, Gage JP, Wilce PA, Shaw RM (1996) A preliminary study of the effects of laser radiation on collagen metabolism in cell culture. Aust Dent J 41:188–192
Conlan MJ, Rapley JW, Cob CM (1996) Biostimulation of wound healing by low-energy laser irradiation. A review. J Clin Periodontol 23:492–496 doi:10.1111/j.1600-051X.1996.tb00580.x
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kim, YD., Kim, SS., Kim, SJ. et al. Low-level laser irradiation facilitates fibronectin and collagen type I turnover during tooth movement in rats. Lasers Med Sci 25, 25–31 (2010). https://doi.org/10.1007/s10103-008-0585-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-008-0585-8