Abstract
The objectives of this study are to analyze the association between anti-nuclear matrix protein 2 (NXP2) autoantibody and idiopathic inflammatory myopathies (IIMs) and to assess the diagnostic and prognostic relevance of anti-NXP2 autoantibody in patients with IIMs. A systematic search was performed in PubMed, Web of Science, EMBASE, the Cochrane Library, and Scopus to identify studies published as of February 29, 2020. Data was analyzed using Stata 12.0 and Meta-DiSc 1.4. Twenty-eight studies (4764 patients with IIMs and 1981 controls) were included in the meta-analysis. Anti-NXP2 autoantibody showed a significant association with IIMs (odds ratio (OR) = 26.36, 95% confidence interval (CI): 12.05–57.67, P < 0.001), especially juvenile IIMs (OR = 62.48, 95% CI: 16.97–229.98, P < 0.001). The pooled sensitivity, specificity, and area under the curve were 0.19 (95% CI = 0.16–0.21), 1.00 (95% CI = 1.00–1.00), and 0.95 for patients with juvenile IIMs versus controls. Anti-NXP2 autoantibody was associated with an increased risk of developing five characteristics (edema, muscle weakness, myalgia/myodynia, dysphagia, and calcinosis) and reduced risk of interstitial lung disease (ILD) (P < 0.001). Anti-NXP2 autoantibody showed no association with increased risk of death in IIMs (P = 0.463). These findings suggest that anti-NXP2 autoantibody is specially related to IIMs and is related to edema, muscle weakness, myalgia/myodynia, dysphagia, calcinosis, and ILD in patients with IIMs. However, there is no evidence to suggest that the presence of anti-NXP2 autoantibody confers a poor prognosis with respect to overall survival.
Key Points • This study summarized the diagnostic and prognostic accuracies of anti-NXP2 autoantibody for patients with IIMs. Anti-NXP2 autoantibody is related to edema, muscle weakness, myalgia/myodynia, dysphagia, calcinosis, and ILD in patients with IIMs. |
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Idiopathic inflammatory myopathies (IIMs) refer to a rare group of heterogeneous autoimmune disorders, including polymyositis, immune-mediated necrotizing myopathy, dermatomyositis, and inclusion body myositis (IBM) [1]. Autoimmunity is known to play a key role in the pathogenesis of IIMs and autoantibodies have been found in over 50% of patients [2]. Conventionally, autoantibodies found in patients with IIMs are classified into myositis-specific autoantibodies (MSAs) and myositis-associated autoantibodies. MSAs are clinically useful biomarkers with diagnostic and prognostic relevance [3].
Anti-nuclear matrix protein 2 (NXP2) autoantibody, originally termed as anti-MJ autoantibody, is one of the MSAs. The reported frequency of anti-NXP2 autoantibody in juvenile and adult IIMs ranges from 2 to 20% [3]. To date, results pertaining to the diagnostic accuracy of anti-NXP2 autoantibody for IIMs have been largely inconsistent. In addition, there is no clear consensus on the association between anti-NXP2 autoantibody and the clinical signs of IIMs. For example, Bodoki et al. found an association between anti-NXP2 autoantibody and malignancy [4]; however, some studies have found no significant difference in the prevalence of malignancy between patients with and without anti-NXP2 autoantibody [5, 6].
There is no consensus on the diagnostic and prognostic relevance of anti-NXP2 autoantibody for IIMs, as well as on the association between anti-NXP2 autoantibody and the clinical manifestations of patients with IIMs. Therefore, we performed a meta-analysis of studies to assess the correlation of anti-NXP2 autoantibody with IIMs and to assess the diagnostic and prognostic relevance of this autoantibody in the context of IIMs. Moreover, we also investigated the relationship of anti-NXP2 autoantibody with the demographic, clinical, and laboratory characteristics of patients with IIMs.
Methods
Search strategy
The PICO strategy was used to develop the search strategy. A systematic search was performed independently on PubMed, Web of Science, EMBASE, the Cochrane Library, and Scopus databases to identify English-language studies published as of February 29, 2020, by L Li and C Liu. A combination of the following keywords was used to retrieve studies: “myositis,” “myopathy,” “polymyositis,” “immune-mediated necrotizing myopathy,” “inclusion body myositis,” “dermatomyositis,” “nuclear matrix protein 2,” “NXP2,” “MJ,” and “p140.” The reference lists of the retrieved articles were also manually screened independently to identify additional relevant studies (L Li and C Liu). Any discrepancies in selecting articles will be resolved by a third author (L Cheng).
Inclusion and exclusion criteria
Original research articles that qualified the following eligibility criteria were included: (1) patients with IIMs fulfilled the Bohan and Peter criteria [7, 8], Sontheimer criteria [9], the criteria of the European Neuromuscular Centre (ENMC) workshop [10], the 2017 European League Against Rheumatism/American College of Rheumatology classification criteria [11], Griggs diagnostic criteria [12] for inclusion body myositis (IBM), or Connors diagnostic criteria [13] for antisynthetase syndrome; (2) availability of data pertaining to the anti-NXP2 autoantibody status of patients with IIMs; (3) availability of adequate data to calculate the odds ratios (OR) or weighted mean differences and the corresponding 95% confidence intervals (CI); (4) adequate data to evaluate the utility of anti-NXP2 autoantibody in the diagnosis of IIMs. Literature reviews, case reports, commentaries, letters, and meeting abstracts were excluded.
Data extraction
The full texts of potentially eligible articles were reviewed and data from the selected studies were extracted independently using a standardized form by two reviewers (L Li and C Liu). The form included the following information: first author, publication year, diagnosis, age at disease onset, age at disease diagnosis, follow-up period, country or region, ethnicity, detection method, total number of cases and controls, frequency of anti-NXP2 autoantibody in cases and controls, demographics, clinical characteristics, laboratory results, and prognostic information of patients with IIMs. Discrepancies, if any, were resolved through discussion and consensus.
Quality assessment
The Newcastle-Ottawa Scale with a star rating system (http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp) was used to evaluate the quality of the included studies. A study is judged based on three criteria: selection of the study groups; comparability of the groups; and ascertainment of either the exposure or outcome of interest for studies. Studies awarded 7–9 stars, 4–6 stars, and < 3 stars were regarded as high-quality, moderate-quality, and low-quality studies, respectively.
Data analysis
This meta-analysis was performed using Stata 12.0 software (Stata Corporation, College Station, TX, USA). The overall odds ratios (ORs) with 95% confidence intervals (CIs) were calculated to evaluate the association between anti-NXP2 autoantibody and IIMs, as well as characteristics. The overall relative risk (RR) with 95% CIs was calculated to evaluate the prognostic value. Heterogeneity among the included studies was evaluated using the Cochrane Q test and I2 statistics. In the event of significant heterogeneity (P ≤ 0.1 for the Cochrane Q test or I2 ≥ 50%), a sensitivity analysis was conducted to assess the stability of the combined results by sequential omission of individual studies, and the random-effects model was used to calculate the summary ORs and corresponding 95% CIs; otherwise, a fixed-effects model was used. The pooled sensitivity, specificity, and area under the curve (AUC) of anti-NXP2 autoantibody for IIMs were assessed using the Meta-DiSc statistical software (version 1.4, Unit of Clinical Biostatistics, Ramon y Cajal Hospital, Madrid, Spain).
Results
Characteristics and quality of the included studies
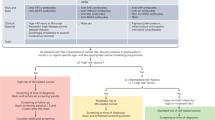
As shown in Fig. 1, a total of 2143 studies were retrieved on search of the databases. Twenty-eight studies [4,5,6, 14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38] with a combined study population of 4764 patients with IIMs and 1981 controls (including 369 healthy controls, 183 systemic lupus erythematosus, 577 systemic sclerosis, 414 juvenile idiopathic arthritis, 27 muscular dystrophies, 25 rheumatoid arthritis, 25 Sjögren syndrome, 124 idiopathic pulmonary fibrosis, 47 genetic muscle disease, 45 Behcet’s disease, 145 psoriatic arthritis) qualified the inclusion criteria and were included in the meta-analysis. Fourteen studies [16,17,18, 22, 23, 26, 27, 29,30,31, 34, 36,37,38] with a combined study population of 2877 patients with IIMs and 1981 controls were assessed for the association between anti-NXP2 autoantibody and IIMs, as well as the diagnostic accuracy of anti-NXP2 autoantibody for IIMs. Twenty-three studies [4,5,6, 14,15,16,17,18,19,20,21,22, 24,25,26, 28, 30,31,32,33,34,35,36] (3538 patients with IIMs) were evaluated for the correlation of anti-NXP2 autoantibody with two demographic (male and female), 18 clinical (edema, muscle weakness, myalgia/myodynia, arthritis/arthralgia, interstitial lung disease, dysphagia, malignancy, heliotrope rash, Gottron’s sign or papules, mechanics hand, skin ulcers, calcinosis, alopecia, Raynaud’s phenomenon, lateral hip rash, facial erythema, palmar papules, and heart involvement), and one laboratory (elevation of creatine kinase (CK)) characteristics. Two studies [19, 33] enrolling 74 patients with IIMs were used to assess the prognostic value of anti-NXP2 autoantibody for IIMs. The characteristics of the 28 eligible studies are presented in Table 1. All the included studies showed moderate-quality or high-quality scores.
Heterogeneity test
The results of the heterogeneity tests are summarized in Table 2. No significant heterogeneity (I2 < 50% and P > 0.1) was observed during the assessment of the association between anti-NXP2 autoantibody and IIMs (including subgroup analysis according to control group, age, and region); the relationship between anti-NXP2 autoantibody and two demographic features, 15 clinical manifestations, and one laboratory result; and the correlation between anti-NXP2 autoantibody and mortality. Significant heterogeneity (I2 ≥ 50% and P ≤ 0.1) was observed for three clinical manifestations (arthritis/arthralgia, malignancy, and calcinosis). Owing to no significant heterogeneity, a fixed-effects model was used to calculate the overall ORs or the overall RR. A random-effects model was used to calculate the overall ORs between anti-NXP2 autoantibody and arthritis/arthralgia, malignancy, and calcinosis, respectively (Table 2). Sensitivity analyses showed that the combined results of association between anti-NXP2 autoantibody and arthritis/arthralgia, malignancy, and calcinosis were stable (data not shown).
Association between anti-NXP2 autoantibody and IIMs
On comparing 2877 patients with IIMs and 1981 controls from 13 studies, the frequency of anti-NXP2 autoantibody in patients with IIMs was significantly greater than that in controls (OR = 26.36, 95% CI: 12.05–57.67, P < 0.001) (Table 3).
Subgroup analyses were performed disaggregated by the type of control group (healthy control and disease control), age (adult and juvenile), and region (Asia, Europe, and North America) (Table 3). In the subgroup analysis disaggregated by the type of control group, 11 studies (2268 IIMs versus 369 healthy controls) as well as 7 studies (1449 IIMs versus 1612 disease controls) were assessed. The overall OR was 10.72 (95% CI: 4.55–25.22, P < 0.001) for the healthy control subgroup and 40.39 (95% CI: 13.62–119.80, P < 0.001) for the disease control subgroup. On subgroup analysis disaggregated by age, the overall OR from eight studies of 1251 adult IIMs versus 1284 controls was 11.81 (95% CI: 4.01–34.78, P < 0.001), and the overall OR from six studies of 874 juvenile IIMs versus 1373 controls was 62.48 (95% CI: 16.97–229.98, P < 0.001). Subgroup analysis disaggregated by region involved six studies of 1631 IIMs versus 963 controls in Asia, five studies of 942 IIMs versus 951 controls in Europe, and two studies of 304 IIMs versus 67 controls in North America. The frequency of anti-NXP2 autoantibody in IIMs was significantly greater than that in controls in Asia (OR = 11.03, 95% CI: 3.40–35.76, P < 0.001), in Europe (OR = 58.70, 95% CI: 15.85–217.33, P < 0.001), and in North America (OR = 14.35, 95% CI: 1.96–105.28, P = 0.009).
Diagnostic ability of anti-NXP2 autoantibody for IIMs
The pooled sensitivity, specificity, and AUC of the summary receiver operating characteristic curve of anti-NXP2 autoantibody for IIMs versus controls were 0.11 (95% CI = 0.10–0.12), 1.00 (95% CI = 1.00–1.00), and 0.91, respectively (Table 3).
The diagnostic accuracy of anti-NXP2 autoantibody for IIMs versus controls was calculated in the subgroup analysis disaggregated by the type of control group (healthy control and disease control), age (adult and juvenile), and region (Asia, Europe, and North America) (Table 3). In the subgroup analysis by control group, the pooled sensitivity, specificity, and AUC values of anti-NXP2 autoantibody were 0.13 (95% CI = 0.11–0.14), 1.00 (95% CI = 0.99–1.00), and 0.83 in IIMs versus healthy controls, and 0.10 (95% CI = 0.08–0.11), 1.00 (95% CI = 1.00–1.00), and 0.93 in IIMs versus disease controls, respectively. On subgroup analysis disaggregated by age, the pooled sensitivity, specificity, and AUC values of anti-NXP2 autoantibody, respectively, were 0.07 (95% CI = 0.06–0.09), 1.00 (95% CI = 1.00–1.00), and 0.84 in adult IIMs versus controls, and 0.19 (95% CI = 0.16–0.21), 1.00 (95% CI = 1.00–1.00), and 0.95 in juvenile IIMs versus controls. On subgroup analysis disaggregated by region, the pooled sensitivity for diagnosing IIMs was 0.06 (95% CI = 0.05–0.07) in Asia, 0.17 (95% CI = 0.15–0.20) in Europe, and 0.18 (95% CI = 0.14–0.23) in North America. The pooled specificity for diagnosis of IIMs was 1.00 (95% CI = 1.00–1.00) both in Asia and Europe, and 1.00 (95% CI = 0.95–1.00) in North America. The AUC values were 0.83 and 0.95 for IIM diagnosis in Asia and Europe, respectively. The AUC value for diagnosis of IIMs in North America was not evaluated due to the small sample size of participants examined.
Association of anti-NXP2 autoantibody with demographic, clinical, and laboratory characteristics
The association of anti-NXP2 autoantibody with demographic, clinical, and laboratory characteristics is shown in Table 4. Five clinical features showed a positive association with anti-NXP2 autoantibody. The overall ORs, 95% CIs, and the associated P values were as follows: edema (four studies with 1147 IIMs patients) (OR = 3.94, 95% CI = 2.63–5.91, P < 0.001); muscle weakness (three studies with 1211 IIMs patients) (OR = 9.89, 95% CI = 4.55–21.50, P < 0.001); myalgia/myodynia (three studies with 1122 IIMs patients) (OR = 2.97, 95% CI = 1.97–4.46, P < 0.001); dysphagia (five studies with 1719 IIMs patients) (OR = 3.81, 95% CI = 2.71–5.36, P < 0.001); calcinosis (15 studies with 2633 IIMs patients) (OR = 4.19, 95% CI = 2.44–7.18, P < 0.001). Based on the analysis of 14 studies (2371 IIMs patients), anti-NXP2 autoantibody was negatively associated with interstitial lung disease (ILD) (OR = 0.26, 95% CI = 0.18–0.38, P < 0.001).
Anti-NXP2 autoantibody showed no correlation with sex, 12 clinical manifestations (arthritis/arthralgia, malignancy, heliotrope rash, Gottron’s sign or papules, mechanics hand, skin ulcers, alopecia, Raynaud’s phenomenon, lateral hip rash, facial erythema, palmar papules and heart involvement), and one laboratory characteristic (elevated CK level) (all P > 0.05).
Prognostic relevance of anti-NXP2 autoantibody for IIMs
The overall RR determined from two studies (74 patients with IIMs) was 1.83 (95% CI = 0.36–9.21, P = 0.463).
Discussion
Nuclear matrix protein 2 (NXP2) is a protein involved in the regulation of transcriptional and RNA metabolism [39]. Anti-NXP2 autoantibody was first identified in 1997 in childhood myositis [40] and was regarded as a key biomarker for diagnosis of IIMs. A previous meta-analysis evaluated the association of anti-NXP2 autoantibody with calcinosis, ILD, and malignancy in IIM patients [41]. However, the association of anti-NXP2 autoantibody with other demographic, clinical, and laboratory characteristics as well as the diagnostic and prognostic relevance of anti-NXP2 autoantibodies for IIMs is worth studying. Thus, we included a greater number of studies and performed a meta-analysis to analyze the diagnostic accuracy, clinical phenotypic association, and prognostic significance of anti-NXP2 autoantibody for IIMs.
This meta-analysis showed that the frequency of anti-NXP2 autoantibody was specific to IIMs. Based on the overall ORs, the anti-NXP2 autoantibody showed a stronger association with juvenile IIMs than adults IIMs (62.48 vs. 11.81). Anti-NXP2 autoantibody showed the strongest association with IIMs among European patients as compared with that in Asian and North American patients (overall ORs: 58.70 vs. 11.03 vs. 14.35). However, further studies are required to confirm the correlation between anti-NXP2 autoantibody and patients with IIMs in North America due to the small sample size. Additionally, related studies conducted in other regions are few or absent; therefore, we could not evaluate the association between anti-NXP2 autoantibody and IIMs in other geographical regions. Analysis of the diagnostic indices demonstrated that anti-NXP2 autoantibody had good specificity but low sensitivity for diagnosis of IIMs. The frequency of anti-NXP2 autoantibody ranged from 1.2 to 64.3% [4,5,6, 14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38], but was absent in the sera of healthy controls and disease controls.
The association of anti-NXP2 autoantibodies with demographic, clinical, and laboratory features is conflicting. In particular, contradictory results have been reported with respect to the relationship of anti-NXP2 autoantibody with malignancy and calcinosis [3]. Our meta-analysis showed that anti-NXP2 autoantibody increased the risk of calcinosis. However, there was no association between anti-NXP2 autoantibody and malignancy. These results are consistent with those of a previous study [41]. In addition, we also found a relation of anti-NXP2 autoantibody with edema, muscle weakness, myalgia/myodynia, dysphagia, and ILD.
The prognostic relevance of anti-NXP2 autoantibodies was also analyzed in the current meta-analysis. We found no connection between the presence of anti-NXP2 autoantibody and poor prognosis of patients with IIMs. However, due to the small number of patients examined, the result should be interpreted with caution and additional studies are required to confirm this outcome.
Some limitations of this meta-analysis should be acknowledged. Due to the small sample size of studies conducted in North America, further studies are required to obtain more definitive evidence. In addition, the relationship of anti-NXP2 autoantibody with other demographic, clinical, and laboratory characteristics was not investigated because of the limited number of studies available.
In conclusion, our findings indicate that anti-NXP2 autoantibody has a high specificity and low sensitivity for diagnosis of IIMs. Anti-NXP2 autoantibody is related to edema, muscle weakness, myalgia/myodynia, dysphagia, calcinosis, and ILD in patients with IIMs, but is not associated with overall survival of these patients.
References
Lundberg IE, Tjarnlund A, Bottai M, Werth VP, Pilkington C, de Visser M, Alfredsson L, Amato AA, Barohn RJ, Liang MH, Singh JA, Aggarwal R, Arnardottir S, Chinoy H, Cooper RG, Danko K, Dimachkie MM, Feldman BM, Garcia-De La Torre I, Gordon P, Hayashi T, Katz JD, Kohsaka H, Lachenbruch PA, Lang BA, Li Y, Oddis CV, Olesinska M, Reed AM, Rutkowska-Sak L, Sanner H, Selva-O’Callaghan A, Song YW, Vencovsky J, Ytterberg SR, Miller FW, Rider LG, International Myositis Classification Criteria Project Consortium tER, the Juvenile Dermatomyositis Cohort Biomarker S, Repository (2017) 2017 European League Against Rheumatism/American College of Rheumatology Classification Criteria for adult and juvenile idiopathic inflammatory myopathies and their major subgroups. Arthritis Rheum 69:2271–2282. https://doi.org/10.1002/art.40320
Betteridge Z, McHugh N (2016) Myositis-specific autoantibodies: an important tool to support diagnosis of myositis. J Intern Med 280:8–23. https://doi.org/10.1111/joim.12451
McHugh NJ, Tansley SL (2018) Autoantibodies in myositis. Nat Rev Rheumatol 14:290–302. https://doi.org/10.1038/nrrheum.2018.56
Bodoki L, Nagy-Vincze M, Griger Z, Betteridge Z, Szollosi L, Danko K (2014) Four dermatomyositis-specific autoantibodies-anti-TIF1gamma, anti-NXP2, anti-SAE and anti-MDA5-in adult and juvenile patients with idiopathic inflammatory myopathies in a Hungarian cohort. Autoimmun Rev 13:1211–1219. https://doi.org/10.1016/j.autrev.2014.08.011
Rogers A, Chung L, Li S, Casciola-Rosen L, Fiorentino DF (2017) Cutaneous and systemic findings associated with nuclear matrix protein 2 antibodies in adult dermatomyositis patients. Arthritis Care Res 69:1909–1914. https://doi.org/10.1002/acr.23210
Albayda J, Pinal-Fernandez I, Huang W, Parks C, Paik J, Casciola-Rosen L, Danoff SK, Johnson C, Christopher-Stine L, Mammen AL (2017) Antinuclear matrix protein 2 autoantibodies and edema, muscle disease, and malignancy risk in dermatomyositis patients. Arthritis Care Res 69:1771–1776. https://doi.org/10.1002/acr.23188
Bohan A, Peter JB (1975) Polymyositis and dermatomyositis (second of two parts). N Engl J Med 292:403–407. https://doi.org/10.1056/NEJM197502202920807
Bohan A, Peter JB (1975) Polymyositis and dermatomyositis (first of two parts). N Engl J Med 292:344–347. https://doi.org/10.1056/NEJM197502132920706
Sontheimer RD (2002) Would a new name hasten the acceptance of amyopathic dermatomyositis (dermatomyositis sine myositis) as a distinctive subset within the idiopathic inflammatory dermatomyopathies spectrum of clinical illness? J Am Acad Dermatol 46:626–636. https://doi.org/10.1067/mjd.2002.120621
Hoogendijk JE, Amato AA, Lecky BR, Choy EH, Lundberg IE, Rose MR, Vencovsky J, de Visser M, Hughes RA (2004) 119th ENMC international workshop: trial design in adult idiopathic inflammatory myopathies, with the exception of inclusion body myositis, 10-12 October 2003, Naarden, The Netherlands. Neuromuscul Disord 14:337–345. https://doi.org/10.1016/j.nmd.2004.02.006
Lundberg IE, Tjarnlund A, Bottai M, Werth VP, Pilkington C, Visser M, Alfredsson L, Amato AA, Barohn RJ, Liang MH, Singh JA, Aggarwal R, Arnardottir S, Chinoy H, Cooper RG, Danko K, Dimachkie MM, Feldman BM, Torre IG, Gordon P, Hayashi T, Katz JD, Kohsaka H, Lachenbruch PA, Lang BA, Li Y, Oddis CV, Olesinska M, Reed AM, Rutkowska-Sak L, Sanner H, Selva-O’Callaghan A, Song YW, Vencovsky J, Ytterberg SR, Miller FW, Rider LG, International Myositis Classification Criteria Project consortium TEr, The Juvenile Dermatomyositis Cohort Biomarker S, Repository (2017) 2017 European League Against Rheumatism/American College of Rheumatology Classification Criteria for adult and juvenile idiopathic inflammatory myopathies and their major subgroups. Ann Rheum Dis 76:1955–1964. https://doi.org/10.1136/annrheumdis-2017-211468
Griggs RC, Askanas V, DiMauro S, Engel A, Karpati G, Mendell JR, Rowland LP (1995) Inclusion body myositis and myopathies. Ann Neurol 38:705–713. https://doi.org/10.1002/ana.410380504
Connors GR, Christopher-Stine L, Oddis CV, Danoff SK (2010) Interstitial lung disease associated with the idiopathic inflammatory myopathies: what progress has been made in the past 35 years? Chest 138:1464–1474. https://doi.org/10.1378/chest.10-0180
Ye L, Zuo Y, Yang H, Li W, Peng Q, Lu X, Wang G, Shu X (2019) Specific autoantibodies and clinical phenotypes correlate with the aberrant expression of immune-related microRNAs in dermatomyositis. J Immunol Res 2019:2927061–2927012. https://doi.org/10.1155/2019/2927061
Li S, Ge Y, Yang H, Wang T, Zheng X, Peng Q, Lu X, Wang G (2019) The spectrum and clinical significance of myositis-specific autoantibodies in Chinese patients with idiopathic inflammatory myopathies. Clin Rheumatol 38:2171–2179. https://doi.org/10.1007/s10067-019-04503-7
Li L, Wang H, Wang Q, Wu C, Liu C, Zhang Y, Cheng L, Zeng X, Zhang F, Li Y (2019) Myositis-specific autoantibodies in dermatomyositis/polymyositis with interstitial lung disease. J Neurol Sci 397:123–128. https://doi.org/10.1016/j.jns.2018.12.040
Wang L, Huang L, Yang Y, Chen H, Liu Y, Liu K, Liu M, Xiao Y, Luo H, Zuo X, Li Y, Xiao X, Zhang H (2018) Calcinosis and malignancy are rare in Chinese adult patients with myositis and nuclear matrix protein 2 antibodies identified by an unlabeled immunoprecipitation assay. Clin Rheumatol 37:2731–2739. https://doi.org/10.1007/s10067-018-4216-x
Yang H, Lu X, Peng Q, Jiang W, Shi J, Zhang Y, Chen H, Wang G (2018) Differential clinical associations of anti-nuclear matrix protein 2 autoantibodies in patients with idiopathic inflammatory myopathies. Arthritis Rheum 70:1288–1297. https://doi.org/10.1002/art.40491
Ueki M, Kobayashi I, Takezaki S, Tozawa Y, Okura Y, Yamada M, Kuwana M, Ariga T (2019) Myositis-specific autoantibodies in Japanese patients with juvenile idiopathic inflammatory myopathies. Mod Rheumatol 29:351–356. https://doi.org/10.1080/14397595.2018.1452353
Aouizerate J, De Antonio M, Bader-Meunier B, Barnerias C, Bodemer C, Isapof A, Quartier P, Melki I, Charuel JL, Bassez G, Desguerre I, Gherardi RK, Authier FJ, Gitiaux C (2018) Muscle ischaemia associated with NXP2 autoantibodies: a severe subtype of juvenile dermatomyositis. Rheumatology (Oxford) 57:873–879. https://doi.org/10.1093/rheumatology/kex516
Best M, Jachiet M, Molinari N, Manna F, Girard C, Pallure V, Cosnes A, Lipsker D, Hubiche T, Schmutz JL, Le Corre Y, Cordel N, Dandurand M, Dereure O, Guillot B, Du-Thanh A, Bulai Livideanu C, Chasset F, Bouaziz JD, Frances C, Bengoufa D, Vincent T, Bessis D, Study Group of Systemic Diseases in D (2018) Distinctive cutaneous and systemic features associated with specific antimyositis antibodies in adults with dermatomyositis: a prospective multicentric study of 117 patients. J Eur Acad Dermatol Venereol 32:1164–1172. https://doi.org/10.1111/jdv.14759
Yang H, Peng Q, Yin L, Li S, Shi J, Zhang Y, Lu X, Shu X, Zhang S, Wang G (2017) Identification of multiple cancer-associated myositis-specific autoantibodies in idiopathic inflammatory myopathies: a large longitudinal cohort study. Arthritis Res Ther 19:259. https://doi.org/10.1186/s13075-017-1469-8
Tansley SL, Simou S, Shaddick G, Betteridge ZE, Almeida B, Gunawardena H, Thomson W, Beresford MW, Midgley A, Muntoni F, Wedderburn LR, McHugh NJ (2017) Autoantibodies in juvenile-onset myositis: their diagnostic value and associated clinical phenotype in a large UK cohort. J Autoimmun 84:55–64. https://doi.org/10.1016/j.jaut.2017.06.007
Merlo G, Clapasson A, Cozzani E, Sanna L, Pesce G, Bagnasco M, Burlando M, Parodi A (2017) Specific autoantibodies in dermatomyositis: a helpful tool to classify different clinical subsets. Arch Dermatol Res 309:87–95. https://doi.org/10.1007/s00403-016-1704-1
Fredi M, Bartoli F, Cavazzana I, Ceribelli A, Carabellese N, Tincani A, Satoh M, Franceschini F (2017) Calcinosis in poly-dermatomyositis: clinical and laboratory predictors and treatment options. Clin Exp Rheumatol 35:303–308
Ceribelli A, Isailovic N, De Santis M, Generali E, Fredi M, Cavazzana I, Franceschini F, Cantarini L, Satoh M, Selmi C (2017) Myositis-specific autoantibodies and their association with malignancy in Italian patients with polymyositis and dermatomyositis. Clin Rheumatol 36:469–475. https://doi.org/10.1007/s10067-016-3453-0
Mammen AL, Casciola-Rosen L, Christopher-Stine L, Lloyd TE, Wagner KR (2015) Myositis-specific autoantibodies are specific for myositis compared to genetic muscle disease. Neurol Neuroimmunol Neuroinflamm 2:e172. https://doi.org/10.1212/NXI.0000000000000172
Troyanov Y, Targoff IN, Payette MP, Raynauld JP, Chartier S, Goulet JR, Bourre-Tessier J, Rich E, Grodzicky T, Fritzler MJ, Joyal F, Koenig M, Senecal JL (2014) Redefining dermatomyositis: a description of new diagnostic criteria that differentiate pure dermatomyositis from overlap myositis with dermatomyositis features. Medicine (Baltimore) 93:318–332. https://doi.org/10.1097/md.0000000000000222
Ceribelli A, Fredi M, Taraborelli M, Cavazzana I, Tincani A, Selmi C, Chan JY, Chan EK, Satoh M, Franceschini F (2014) Prevalence and clinical significance of anti-MDA5 antibodies in European patients with polymyositis/dermatomyositis. Clin Exp Rheumatol 32:891–897
Yu HH, Chang HM, Chiu CJ, Yang YH, Lee JH, Wang LC, Lin YT, Chiang BL (2016) Detection of anti-p155/140, anti-p140, and antiendothelial cells autoantibodies in patients with juvenile dermatomyositis. J Microbiol Immunol Infect 49:264–270. https://doi.org/10.1016/j.jmii.2014.05.012
Tansley SL, Betteridge ZE, Shaddick G, Gunawardena H, Arnold K, Wedderburn LR, McHugh NJ, Juvenile Dermatomyositis Research G (2014) Calcinosis in juvenile dermatomyositis is influenced by both anti-NXP2 autoantibody status and age at disease onset. Rheumatology (Oxford) 53:2204–2208. https://doi.org/10.1093/rheumatology/keu259
Valenzuela A, Chung L, Casciola-Rosen L, Fiorentino D (2014) Identification of clinical features and autoantibodies associated with calcinosis in dermatomyositis. JAMA Dermatol 150:724–729. https://doi.org/10.1001/jamadermatol.2013.10416
Kang EH, Kuwana M, Okazaki Y, Lee EY, Lee YJ, Lee EB, Song YW (2014) Comparison of radioimmunoprecipitation versus antigen-specific assays for identification of myositis-specific autoantibodies in dermatomyositis patients. Mod Rheumatol 24:945–948. https://doi.org/10.3109/14397595.2014.896494
Fiorentino DF, Chung LS, Christopher-Stine L, Zaba L, Li S, Mammen AL, Rosen A, Casciola-Rosen L (2013) Most patients with cancer-associated dermatomyositis have antibodies to nuclear matrix protein NXP-2 or transcription intermediary factor 1gamma. Arthritis Rheum 65:2954–2962. https://doi.org/10.1002/art.38093
Ceribelli A, Fredi M, Taraborelli M, Cavazzana I, Franceschini F, Quinzanini M, Tincani A, Ross SJ, Chan JY, Pauley BA, Chan EK, Satoh M (2012) Anti-MJ/NXP-2 autoantibody specificity in a cohort of adult Italian patients with polymyositis/dermatomyositis. Arthritis Res Ther 14:R97. https://doi.org/10.1186/ar3822
Ishikawa A, Muro Y, Sugiura K, Akiyama M (2012) Development of an ELISA for detection of autoantibodies to nuclear matrix protein 2. Rheumatology (Oxford) 51:1181–1187. https://doi.org/10.1093/rheumatology/kes033
Ichimura Y, Matsushita T, Hamaguchi Y, Kaji K, Hasegawa M, Tanino Y, Inokoshi Y, Kawai K, Kanekura T, Habuchi M, Igarashi A, Sogame R, Hashimoto T, Koga T, Nishino A, Ishiguro N, Sugimoto N, Aoki R, Ando N, Abe T, Kanda T, Kuwana M, Takehara K, Fujimoto M (2012) Anti-NXP2 autoantibodies in adult patients with idiopathic inflammatory myopathies: possible association with malignancy. Ann Rheum Dis 71:710–713. https://doi.org/10.1136/annrheumdis-2011-200697
Gunawardena H, Wedderburn LR, Chinoy H, Betteridge ZE, North J, Ollier WE, Cooper RG, Oddis CV, Ramanan AV, Davidson JE, McHugh NJ, Juvenile Dermatomyositis Research Group UK, Ireland (2009) Autoantibodies to a 140-kd protein in juvenile dermatomyositis are associated with calcinosis. Arthritis Rheum 60:1807–1814. https://doi.org/10.1002/art.24547
Suzuki S, Uruha A, Suzuki N, Nishino I (2017) Integrated diagnosis project for inflammatory myopathies: an association between autoantibodies and muscle pathology. Autoimmun Rev 16:693–700. https://doi.org/10.1016/j.autrev.2017.05.003
Oddis CV, Fertig N, Goel A, Espada G, Gregorian MC, Cocco JAM, Londino AV (1997) Clinical and serological characterization of the anti-MJ antibody in childhood myositis. Arthritis Rheum 40:652–652
Zhong L, Yu Z, Song H (2019) Association of anti-nuclear matrix protein 2 antibody with complications in patients with idiopathic inflammatory myopathies: a meta-analysis of 20 cohorts. Clin Immunol 198:11–18. https://doi.org/10.1016/j.clim.2018.11.008
Funding
This study was supported by grants from the National Natural Science Foundation of China Grants (81671618, 81871302), and the CAMS Initiative for Innovative Medicine (2017-I2M-3-001, 2017-I2M-B&R-01).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOC 66 kb)
Rights and permissions
About this article
Cite this article
Li, L., Liu, C., Cheng, L. et al. Assessment of diagnostic utility, clinical phenotypic associations, and prognostic significance of anti-NXP2 autoantibody in patients with idiopathic inflammatory myopathies: a systematic review and meta-analysis. Clin Rheumatol 40, 819–832 (2021). https://doi.org/10.1007/s10067-020-05291-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-020-05291-1