Abstract
This paper describes a rare right paraduodenal hernia discovered during an elective laparoscopic colon resection. Our patient was a 60-year-old Asian man with a history of multiple bouts of diverticulitis and a lifelong history of mild constipation and postprandial abdominal pain. Prior CT scans and preoperative barium enema confirmed the diagnosis of diverticular disease, and no other abnormalities were appreciated. At laparoscopic exploration, a right paraduodenal hernia was found with complete herniation of the small intestine under the ascending colon and hepatic flexure. The unclear anatomy prompted conversion to an open laparotomy. This allowed safe reduction of the hernia and sac excision. Adhesions were lysed to relieve a partial duodenal obstruction, and a Ladd’s procedure was performed to correct the incomplete rotation. Additionally, a sigmoid colectomy was performed. After prolonged ileus, the patient was discharged on postoperative day 14. At 6-month follow-up, the patient was asymptomatic and doing well.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Case report
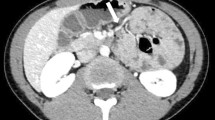
Our patient was a 60-year-old Asian male, referred for surgical evaluation at the time of his fourth episode of diverticulitis. He had been successfully managed by his internist as an outpatient with antibiotic therapy during three prior episodes. Colonoscopy 6 months earlier had shown diverticulosis. Review of systems revealed a history of occasional constipation, managed with a high-fiber diet and psyllium. Physical exam showed a nondistended abdomen without scars or palpable masses. On admission, computed tomography showed a thickened left colon without evidence of abscess, and no rotational abnormalities were identified. He required hospitalization with IV antibiotic therapy, and his symptoms resolved. At follow-up, a barium enema was obtained that showed descending and sigmoid colon diverticulosis with resolution of inflammation. The patient was counseled and agreed to proceed with an elective laparoscopic sigmoid colectomy.
At laparoscopic exploration, nearly all of the small intestine was contained in a retroperitoneal sac (Fig. 1). A free margin was noted in the right lower quadrant and allowed visualization of normal-appearing small intestine. Cautious blunt and sharp dissection was attempted laparoscopically (Fig. 2). Due to unclear anatomy, a midline laparotomy was performed. The entire small bowel was contained within a sac in the central abdomen (Fig. 3). The right colon had only lateral attachments and completely lacked retroperitoneal fixation. The small bowel was herniated posterior to the right colonic mesentery. The diagnosis of a right paraduodenal hernia was established. After division of the lateral attachments of the ascending colon, a tortuous duodenum was identified. Due to additional fixation abnormalities, the duodenum and pancreatic head were easily lifted from the retroperitoneum without requiring any dissection (Fig. 4). Adhesions were lysed to relieve the partial duodenal obstruction, and a Ladd’s procedure was done to alleviate the rotational abnormalities. Additionally, a sigmoid colectomy was performed as planned. At the completion of the procedure, the colon was positioned on the left of the abdomen and the small bowel on the right (Fig. 5).
A postoperative ileus prompted parenteral nutritional support. The patient was discharged tolerating a regular diet on postoperative day 14. At 6-month follow-up, he remains asymptomatic and is doing well. On further questioning, the patient admitted to a lifelong history of postprandial discomfort. He reported minimizing his symptoms by slowly eating small amounts of food.
Discussion
Paraduodenal or mesocolic hernias are rare congenital errors of midgut fixation and are considered part of the spectrum of malrotational anomalies [1, 2]. Fewer than 500 cases have been reported in the world’s literature. Some patients have vague abdominal complaints and subclinical symptoms related to long-term intermittent or partial obstruction, while others present with acute closed-loop obstruction or intestinal ischemia [3]. Autopsy series estimate the incidence of paraduodenal hernia at approximately 0.2% [4]. While the overall incidence is low, paraduodenal hernias account for 53% of congenital internal hernias [5, 6]. They are three times more common in males [7].
Paraduodenal hernias are classified as left- or right-based on the relationship of the small bowel to the superior mesenteric vessels, with a 3:1 left-to-right predominance [8]. In right paraduodenal hernias, the superior mesenteric and ileocolic arteries course along the left margin of the hernia sac [9]. In left paraduodenal hernias, the inferior mesenteric artery and vein are closely associated with the right sac margin [10]. During sac excision, care must be exercised to prevent injury to the intestinal vasculature [11].
Surgical management requires opening of the sac and reduction of the herniated small bowel, with resection as needed of nonviable segments [12]. A Ladd’s procedure is performed to eliminate colonic fixation abnormalities and includes division of the lateral colonic attachments, medial rotation of the ascending colon to the left of the midline, appendectomy, broadening of the small bowel mesentery, and alleviation of duodenal obstruction.
Laparoscopic management of paraduodenal hernias has been described [13]. For patients diagnosed with a paraduodenal hernia preoperatively by computed tomography or barium upper gastrointestinal imaging, a minimally invasive approach may be feasible. However, an open laparotomy may be required, and we recommend that sound surgical judgment be used to guide the operative approach.
Conclusion
A clear understanding of colonic fixation and midgut embryology is important for surgeons who may encounter paraduodenal hernias. With appropriate surgical management, paraduodenal hernias may be safely reduced with relief of often long-standing symptoms.
References
Scott DJ, Jones DB (2000) Hernias and abdominal wall defects. In: Norton JA, Bolinger RR, Chang AE, Lowry SF, Mulvihill SJ, Pass HI, Thompson RW (eds) Surgery: Scientific Basis and Current Practice. Springer Berlin Heidelberg New York, pp 787–823
Scott DJ, Jones DB (1999) Hernia. In: McClelland RN (ed) Selected Readings In General Surgery. Volume 26, No. 4, Issues 1–2
Groff D III (1993) Malrotation. In: Ashcraft KW, Holder TM (eds) Pediatric Surgery, 2nd Edition. W.B. Saunders Company, Philadelphia, pp 320–330
Armstrong O, Letessier E, Genier F, Lasserre P, Le Néel JC (1997) Internal hernia. Report of nine cases. Hernia 1:271–273
Berardi RS (1981) Paraduodenal Hernias. Surg Gynecol Obstet 152:99–110
Yoo HY, Mergela J, Seibert DG (2000) Paraduodenal Hernia: A Treatable Cause of Upper Gastrointestinal Tract Symptoms. J Clin Gastroenterol 31:226–229
Khan MA, Lo AY, Vande Maele DM (1998) Paraduodenal Hernia. Am Surg 64:1218–1222
Brigham RA, Fallon WF, Saunders JR, Harmon JW, d’Avis JC (1984) Paraduodenal Hernia: Diagnosis and surgical management. Surgery 96:498–502
Ghahremani GG (1984) Internal Abdominal Hernias. Surg Clin North Am 64:393–406
Sato TT, Oldham KT (2001) Pediatric Abdomen. In: Greenfield LJ, Mulholland MW, Oldham KT, Zelenock GB, Lillemoe KD (eds) Surgery: Scientific Principles and Practice, Lippincott, Williams & Wilkins, Philadelphia, pp 1968–2042
Brigham RA (1995) Paraduodenal Hernia. In: Nyhus LM, Condon RE (eds) Hernia, 4th Edition, JB Lippincott Company, Philadelphia, pp 485–490
Bartlett MK, Wang C, Williams WH (1968) The Surgical Management of Paraduodenal Hernia. Ann Surg 168:249–254
Uematsu T, Kitamura H, Iwase M, Yamashita K, Ogura H, Nakamuka T, Oguri H (1998) Laparoscopic repair of a paraduodenal hernia. Surg Endosc 12:50–52
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Brunner, W.C., Sierra, R., Dunne, J.B. et al. Incidental paraduodenal hernia found during laparoscopic colectomy. Hernia 8, 268–270 (2004). https://doi.org/10.1007/s10029-004-0207-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-004-0207-8