Abstract
Objectives
Perioperative oral care was reported to decrease postoperative pneumonia after cancer resections. However, the effect remains controversial because previous studies were limited due to their small sample sizes and lack of strict control for patient backgrounds. The present study evaluated the association between perioperative oral care and postoperative pneumonia using high-dimensional propensity score (hd-PS) matching to adjust for confounding factors.
Materials and methods
Using a Japanese health insurance claims database, we identified patients who underwent surgical treatment of cancer from April 2014 to March 2015. To compare outcomes (postoperative pneumonia and procedure-related complications) between patients with and without perioperative oral care, we performed hd-PS matching and conventional PS matching and chi-square test.
Results
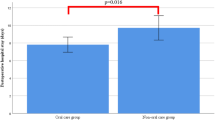
We identified 621 patients with oral care and 4374 patients without oral care. The occurrences of postoperative pneumonia were not significantly different between patients with and without oral care in the unmatched (2.9% vs. 3.2%), conventional PS-matched (2.9% vs. 2.9%), or hd-PS-matched (2.9% vs. 3.3%) groups. The occurrences of procedure-related complication were not significantly different between patients with and without oral care in the unmatched (23.8% vs. 24.5%), conventional PS-matched (23.8% vs. 26.4%), or hd-PS-matched (24.4% vs. 27.7%) groups.
Conclusions
There was no significant difference in postoperative pneumonia or procedure-related complications between patients with and without perioperative oral care.
Clinical relevance
While maintaining optimal oral care in cancer patients is an important goal, the present study revealed no significant difference in postoperative outcomes. Further investigations would be needed to determine the effect of perioperative oral care.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Oral care has been reported to be an effective approach to decrease pneumonia. Several systematic reviews and meta-analyses showed oral care including chlorhexidine use significantly decreased mechanically ventilator-associated pneumonia [1,2,3,4]. Furthermore, routine oral care for elderly residents in nursing home was reported to prevent nursing home-acquired pneumonia [5,6,7]. Oral care can improve poor oral condition, severe periodontal disease, and dental plaque, which is associated with increase in pathogens colonizing in oral cavity [8, 9]. For intubated patients and elderly residents in nursing home, pathogens in saliva can easily leak into trachea and may cause lung infection [10, 11].
Perioperative oral care was also likely to decrease postoperative pneumonia after head and neck cancer resection, esophageal cancer resection, and lung cancer resection [12,13,14,15,16,17]. Postoperative pneumonia is one of the most common fatal complications after cancer resections. The incidence rates of postoperative pneumonia were reported to 7.3–38% of patients after esophagectomy [18, 19], and 3.5% of patients after several major cancer surgeries [20]. Postoperative pneumonia significantly increased morbidity, mortality, length of hospital stay, and treatment costs [1]. Several studies have investigated the association between perioperative oral care and postoperative pneumonia; however, these studies were limited due to their small sample sizes and lack of strict control for patient backgrounds [13,14,15,16,17,18,19,20,21,22].
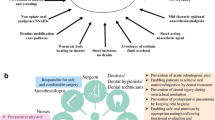
In the present study, we evaluated the effect of perioperative oral care by dental providers to prevent postoperative pneumonia in several types of cancer patients, using a Japanese administrative claims database. We performed high-dimensional propensity score (hd-PS) matching and conventional PS matching analyses for balancing patient backgrounds and adjusting confounding factors.
Methods
Data source
This study was performed using a health insurance claims database developed by the Japan Medical Data Centre Co. Ltd. (Tokyo, Japan). The details of the database have been described elsewhere [23, 24]. As of 2015, the database included outpatient and inpatient health insurance claims of approximately 1.6 million patients, which accounted for about 1.3% of the entire Japanese population. The data consisted of encrypted unique identifiers, age, and sex, diagnoses coded according to the International Classification of Diseases, 10th Revision (ICD-10) codes; and medications and procedures coded according to Japanese original codes. The database also included data on body mass index, smoking status, and alcohol consumption. The Institutional Review Board at The University of Tokyo approved the study protocol. Informed consent was waived because of the anonymous nature of the data.
Patients
We identified patients who underwent resection of the following types of cancer from April 2014 to March 2015: head and neck, lung, gastric, colorectal, breast, and esophageal cancer. We excluded patients who were first enrolled in the database within 365 days before the day of admission. When patients underwent two or more cancer resections, the first surgery was included in our analysis. Patients who had undergone perioperative oral care by dentists were identified using Japanese original procedure codes. Perioperative oral care was defined as a reimbursement when surgeons for each cancer treatment requested dentists to provide oral care before cancer resections.
Outcomes
The primary outcomes of the present study were postoperative pneumonia (ICD-10 codes J12-J18, J69, and J84) and procedure-related complications (T81).
Hd-PS estimation
Hd-PS analysis has been proposed as an approach to improve the ability to control for confounding factors in comparative effectiveness studies using administrative claims databases [25,26,27,28]. We performed hd-PS matching between patients with and without perioperative oral care. The detailed methods for hd-PS estimation were reported in a previous study [26]. Briefly, the following five steps were implemented: (1) identification of different data dimensions, (2) identification of hundreds of the most prevalent codes in each data dimension as candidate covariates during the preoperative period, (3) assessment of candidate covariates with their frequencies, (4) ranking of candidate covariates across all dimensions by their potential of confounding factors based on Bross’s formula [29], and (5) selection of the top of n highest potential covariates for PS modeling.
In the present study, the preoperative period was defined as the period within 365 days before the day of admission. We structured the following five dimensions: outpatient diagnoses, inpatient diagnoses, outpatient procedures, inpatient procedures, and outpatient and inpatient drug use. We included the top of 500 highest potential covariates in the logistic regression model for receiving perioperative oral care to estimate the hd-PS. We also included the following covariates in the model: age (≤ 50, 51–60, and > 60 years), sex, cancer site, type of hospital (academic or nonacademic), and annual hospital volume (average number of patients in each hospital who underwent perioperative oral care per year). The annual hospital volume was categorized into low-volume (< 12 cases per year) and high-volume (≥ 12 cases per year) groups to ensure almost equal numbers of patients in the two categories.
Conventional PS estimation
We included demographic factors and hospital factors in a logistic regression model for receiving oral care to estimate conventional PS. Demographic factors included age, sex, type of cancer resection, and disease history during the preoperative period. Disease history included hypertension (ICD 10 codes I10 or I15), diabetes mellitus (E10–E14), ischemic heart disease (I20–I25), heart failure (I50), renal failure (N17–N19), chronic obstructive pulmonary disease (J44), asthma (J45), pneumonia (J12–J18, J69, J84, and J95.8), and cerebrovascular disease (I60–I69). Hospital factors included the type of hospital and annual hospital volume.
PS matching and absolute standardized differences
We performed one-to-one and nearest-neighbor matching with 0.20 times the standard deviations of the logit of the PS as a caliper value without replacement.
To test the ability to balance the distribution of covariates between patients with and without oral care, we calculated the absolute standardized differences for 21 categories of 6 covariates included in the PS estimation: 3 categories of age (≤ 50, 51–60, and > 60 years), 1 category of sex (female), 6 categories of cancer site (head and neck, esophagus, lung, stomach, colon and rectum, and breast), 1 category of hospital type (academic hospital), 1 category of annual hospital volume (≥ 12 cases per year), and 9 categories of disease history (hypertension, diabetes mellitus, ischemic heart disease, heart failure, renal failure, chronic obstructive pulmonary disease, asthma, pneumonia, and cerebrovascular diseases).
We also calculated the absolute standardized differences for 10 categories of 3 variables that were not included in the PS estimation: 4 categories of body mass index (< 18.5, 18.5–24.9, and ≥ 25.0 kg/m2 and missing data), 3 categories of smoking status (ex- or current smoker, nonsmoker, and missing data), and three categories of alcohol consumption (drinker, nondrinker, and missing data). These variables may be confounding factors, but we could not include them in the PS estimation models because there were too many missing values.
An absolute standardized difference of > 0.1 was defined as out of balance. The proportions of the outcomes were compared using the chi-square test between patients with and without perioperative oral care. The threshold for significance was a p value of ≤ 0.05. All analyses were performed using R version 3.1.2. (R Foundation for Statistical Computing, Vienna, Austria).
Statistical power analysis
We conducted a priori sample size estimation. Following a previous study [30], we set the prevalence proportions of postoperative pneumonia after cancer resection in the control group and the perioperative oral care group at 25% and 15%, respectively. Alpha and beta errors were set 0.05 and 0.80, respectively.
Results
We determined the optimal sample size to detect the effect difference was 250 cases per group. We identified 4995 eligible patients. These patients were categorized into those with oral care (n = 621) and without oral care (n = 4374). We generated 618 pairs by conventional PS matching. We also generated 581 pairs for postoperative pneumonia and 574 pairs for procedure-related complications by hd-PS matching (Fig. 1).
Table 1 shows the patients’ baseline characteristics that were included in the PS estimation model for the unmatched group, conventional PS-matched group, hd-PS-matched group for postoperative pneumonia, and hd-PS-matched group for procedure-related complications. Patients were more likely to receive perioperative oral care if they had the following characteristics: older age, non-academic hospital, larger hospital volume, head and neck cancer, esophageal cancer, gastric cancer, non-lung cancer, non-breast cancer, hypertension, diabetes mellitus, and cerebrovascular disease. The number of categories with an absolute standardized difference of > 0.1 was 12 in the unmatched group, 1 in the conventional PS-matched group, and 0 in the hd-PS-matched group.
Table 2 shows the distribution of the variables that were not included in the PS estimation model. The number of categories with an absolute standardized difference of > 0.1 was 7 in the unmatched group, 1 in the conventional PS-matched group, and 0 in the hd-PS-matched group. In the conventional PS matched groups, the absolute values of the standardized difference were < 10% for all baseline characteristics.
Table 3 presents the proportions of postoperative pneumonia and procedure-related complications. The proportions of postoperative pneumonia did not differ significantly between patients with and without oral care in the unmatched (2.9% vs. 3.2%), conventional PS-matched (2.9% vs. 2.9%), or hd-PS-matched (2.9% vs. 3.3%) groups. The proportions of procedure-related complication did not differ significantly between patients with and without oral care in the unmatched (23.8% vs. 24.5%), conventional PS-matched (23.8%% vs. 26.4%), or hd-PS-matched (24.4% vs. 27.7%) groups.
Discussion
The present study showed that there was no significant difference in postoperative pneumonia or procedure-related complications between patients with and without perioperative oral care using hd-PS matched analysis and conventional PS matched analysis.
The proportion of postoperative pneumonia in our study was lower than those in previous studies. There are two considerable reasons. First, our database did not include patients older than 75 years, but a previous study showed significant association between age and postoperative pneumonia [20]. Second, our study included relatively high numbers of patients with gastric, breast, and colorectal cancer resections, whereas the numbers of patients with esophagectomy and head and neck cancer resections were small. Reportedly, these two surgeries were associated with higher frequency of postoperative pneumonia [31,32,33].
The proportions of procedure-related complication were reported to 21–63.6% in head and neck cancer resection [21, 22]. Previous studies reported that perioperative oral care reduced the risk of postoperative surgical site infection [21]. However, data were lacking on the relationship between perioperative oral care and procedure-related complication. In the present study, procedure-related complications were likely to be lower in the perioperative oral care group than the control group, although not statistically significant.
Unmeasured confounders generally exist in observational studies, particularly in administrative claim data studies. Several methods for controlling unmeasured confounders have been developed to date. Hd-PS-matched analysis was reported to have several advanced points compared with conventional PS-matched analysis. First, hd-PS matching has been shown to balance patient backgrounds better than did conventional PS in empirical settings [28, 34,35,36,37,38,39,40]. Performance of PS matching should be assessed with respect to its ability to balance the backgrounds of the patient groups being compared [36]. Second, an hd-PS algorithm has the potential to control unmeasured confounders with adjustment for thousands of covariates [36], whereas conventional PS-matched analysis only adjusts for factors included in the PS estimation model. We used hd-PS-matched analysis and conventional PS-matched analysis to adjust for confounding factors. The results in the hd-PS-matched analysis showed a similar trend to those in the conventional analysis.
To the best of our knowledge, this paper was the first study that evaluated the association between perioperative oral care and postoperative pneumonia with control of biases using hd-PS-matched method. Furthermore, our study has the largest sample size of any to have examined the association between perioperative oral care and postoperative pneumonia [12,13,14,15,16,17].
The present study had several limitations. First, recorded diagnoses are generally less well validated in administrative data. Regarding Japanese claims databases, a previous validation study showed that recorded diagnoses had high specificity but lower sensitivity, while recorded medications and procedures had high sensitivity and specificity [41]. Second, we had no data on several potential confounders, including each patient’s dental services and dental conditions. Third, the small sample size precluded us from performing subset analyses for different types of cancer. However, for example, patients with head and neck cancer may have different responses to perioperative oral care, compared with patients with colorectal cancer. Fourth, the sample size in the present study may have been underpowered to judge the effect. Contrary to prior expectation, we obtained a relatively small difference in postoperative pneumonia—only 0.4%—in the hd-PS-matched groups.
Conclusion
While maintaining optimal oral care in cancer patients is an important goal, the present study showed no significant difference in postoperative pneumonia or procedure-related complications between patients with and without perioperative oral care.
References
Spreadborough P, Lort S, Pasquali S et al (2016) A systematic review and meta-analysis of perioperative oral decontamination in patients undergoing major elective surgery. Perioper Med 5:6–12
Zuckerman LM (2016) Oral chlorhexidine use to prevent ventilator-associated pneumonia in adult. Dimens Crit Care Nurs 35(1):25–36
Silvestri L, Weir I, Gregori D et al (2014) Effectiveness of oral chlorhexidine on nosocomial pneumonia, causative micro-organisms and mortality in critically ill patients: a systematic review and meta-analysis. Minerva Anestesiol 80(7):805–820
Vilela MC, Ferreira GZ, Santos PS, Rezende NP (2015) Oral care and nosocomial pneumonia: a systematic review. Einstein 13(2):290–296
Ono S, Ishimaru M, Yamana H et al (2017) Enhanced oral care and health outcomes among nursing facility residents: analysis using the national long-term care database in Japan. J Am Med Dir Assoc 18(3):e1–e5
Sjögren P, Wårdh I, Zimmerman M, Almståhl A, Wikström M (2016) Oral care and mortality in older adults with pneumonia in hospitals or nursing homes: systematic review and meta-analysis. J Am Geriatr Soc 64(10):2109–2115
Kaneoka A, Pisegna JM, Miloro KV, Lo M, Saito H, Riquelme LF, LaValley MP, Langmore SE (2015) Prevention of healthcare-associated pneumonia with oral care in individuals without mechanical ventilation: a systematic review and meta-analysis of randomized controlled trials. Infect Control Hosp Epidemiol 36(8):899–906
Tohara T, Kikutani T, Tamura F, Yoshida M, Kuboki T (2017) Multicentered epidemiological study of factors associated with total bacterial count in the saliva of older people requiring nursing home. Geriatr Gerontol Int 17(2):219–225
Ishikawa A, Yoneyama T, Hirota K, Miyake Y, Miyatake K (2008) Professional oral health care reduces the number of oropharyngeal bacteria. J Dent Res 87:594–598
El-Solh AA, Pietrantoni C, Bhat A et al (2004) Colonization of dental plaques: a reservoir of respiratory pathogens for hospital acquired pneumonia in institutionalized elders. Chest 126:1575–1582
Bágyi K, Haczku A, Márton I, Szabó J, Gáspár A, Andrási M, Varga I, Tóth J, Klekner A (2009) Role of pathogenic oral flora in postoperative pneumonia following brain surgery. BMC Infect Dis 9:104–113
Wren SM, Martin M, Yoon JK, Bech F (2010) Postoperative pneumonia-prevention program for the inpatient surgical ward. J Am Coll Surg 210:491–495
Akutu Y, Matsubara H, Okazumi S et al (2008) Impact of preoperative dental plaque culture for predicting postoperative pneumonia in esophageal cancer patients. Dig Surg 25:93–97
Akutsu Y, Matsubara H, Shuto K, Shiratori T, Uesato M, Miyazawa Y, Hoshino I, Murakami K, Usui A, Kano M, Miyauchi H (2010) Pre-operative dental brushing can reduce the risk of postoperative pneumonia in esophageal cancer patients. Surgery 147:497–502
Yamazaki M, Matsuura K, Kato K et al (2009) Perioperative oral care reduced postoperative complications after head and neck reconstruction surgery. Tokeibu Geka 19:105–110 (Japanese)
Hoshikawa Y, Tanda N, Matsuda Y et al (2016) Current status of preoperative professional oral care by dentists for elderly patients undergoing lung resection and occurrence of postoperative pneumonia. Kyobu Geka 69(1):25–29 (Japanese)
Soutome S, Yanamoto S, Funahara M, Hasegawa T, Komori T, Oho T, Umeda M (2016) Preventive effect on post-operative pneumonia of oral health care among patients who undergo esophageal resection: a multi-center retrospective study. Surg Infect 17(4):479–484 (Japanese)
Atkinsm BZ, Shah AS, Hutcheson KA et al (2004) Reducing hospital morbidity and mortality following esophagectomy. Ann Thorac Surg 78:1170–1176
Fang W, Kato H, Tachimori Y, Igaki H, Sato H, Daiko H (2003) Analysis of pulmonary complications after three-field lymph node dissection for esophageal cancer. Ann Thorac Surg 76:903–908
Trinh VQ, Ravi P, Abd-El-Barr AM et al (2016) Pneumonia after major cancer surgery: temporal trends and patterns of care. Can Respir J 2016:1–7
Sato J, Goto J, Harahashi A, Murata T, Hata H, Yamazaki Y, Satoh A, Notani KI, Kitagawa Y (2011) Oral health care reduced the risk of postoperative surgical site infection in inpatients with oral squamous cell carcinoma. Support Care Cancer 19:409–416
Ueno T, Ota Y (2012) The importance of perioperative oral care. Jpn J Anesthesiol (Masui) 61(3):276–281 (Japanese)
Kimura S, Sato T, Ikeda S, Noda M, Nakayama T (2010) Development of a database of health insurance claims: standardization of disease classifications and anonymous record linkage. J Epidemiol 20:413–419
Ono S, Ono Y, Matsui H, Yasunaga H (2016) Factors associated with hospitalization for seasonal influenza in a Japanese nonelderly cohort. BMC Public Health 16:922–929
Garbe E, Kloss S, Suling M, Pigeot I, Schneeweiss S (2013) High-dimensional versus conventional propensity scores in a comparative effectiveness study of coxibs and reduced upper gastrointestinal complications. Eur J Clin Pharmacol 69:549–557
Schneeweiss S, Rassem JA, Glynn RJ et al (2009) High-dimensional propensity score adjustment in studies of treatment effects using health care claims data. Epidemiology 20:512–522
Toh S, Rodríguez LAG, Hernán MA (2011) Confounding adjustment via a semi-automated high-dimensional propensity score algorithm: an application to electronic medical records. Pharmacoepidemiol Drug Saf 20:849–857
Franklin JM, Eddings W, Glynn RJ, Schneeweiss S (2015) Regularized regression versus the high-dimensional propensity score for confounding adjustment in secondary database analyses. Am J Epidemiol 182:651–659
Bross ID (1966) Spurious effects from an extraneous variable. J Chronic Dis 19:637–647
Soutome S, Yanamoto S, Funahara M, Hasegawa T, Komori T, Yamada SI, Kurita H, Yamauchi C, Shibuya Y, Kojima Y, Nakahara H, Oho T, Umeda M (2017) Effect of perioperative oral care on prevention of postoperative pneumonia associated with esophageal cancer surgery: a multicenter case-control study with propensity score matching analysis. Medicine (Baltimore) 96(33):e7436–e7440
Yang CK, Teng A, Lee DY, Rose K (2015) Pulmonary complications after major abdominal surgery: National Surgical Quality Improvement Program analysis. J Surg Res 198(2):441–449
Kiuchi J, Komatsu S, Ichikawa D, Kosuga T, Okamoto K, Konishi H, Shiozaki A, Fujiwara H, Yasuda T, Otsuji E (2016) Putative risk factors for postoperative pneumonia which affects poor prognosis in patients with gastric cancer. Int J Clin Oncol 21:920–926
Pettke E, Ilonzo N, Ayewah M, Tsantes S, Estabrook A, Ma AM (2016) Short-term, postoperative breast cancer outcomes in patients with advanced age. Am J Surg 212(4):677–681
Hall MK, Taylor RA, Luty S, Allen IE, Moore CL (2016) Impact of point-of-care ultrasonography on ED time to disposition for patients with nontraumatic shock. Am J Emerg Med 34:1022–1030
Rassen JA, Schneeweiss S (2012) Using high-dimensional propensity scores to automate confounding control in a distributed medical product safety surveillance system. Pharmacoepidemiol Drug Saf 21:41–49
Guertin JR, Rahme E, LeLorier J (2016) Performance of the high-dimensional propensity score in adjusting for unmeasured confounders. Eur J Clin Pharmacol 72(12):1497–1505
Guertin JR, Rahme E, Dormuth CR, LeLorier J (2016) Head to head comparison of the propensity score and the high-dimensional propensity score matching methods. BMC Med Res Methodol 16:22–31
Chien SC, Ou SM, Shih CJ et al (2015) Comparative effectiveness of angiotensin-converting enzyme inhibitor and angiotensin II receptor blockers in terms of major cardiovascular disease outcomes in elderly patients. Medicine 94:1–10
Le HV, Poole C, Brookhart MA et al (2013) Effects of aggregation of drug and diagnostic codes on the performance of the high-dimensional propensity score algorithm: an empirical example. BMC Med Res Methodol 13:142–152
Hernandez I, Zhang Y (2015) Comparing clinical and economic outcomes of biologic and conventional medications in postmenopausal women with osteoporosis. J Eval Clin Pract 21:840–847
Yamana H, Moriwaki M, Horiguchi H et al (2017) Validity of diagnoses, procedures, and laboratory data in Japanese administrative data. J Epidemiol 1–7
Funding
This work was supported by grants from the Ministry of Health, Labour and Welfare, Japan (H29-Policy-Designated-009 and H29-ICT-General-004); Ministry of Education, Culture, Sports, Science, and Technology, Japan (17H04141); and the Japan Agency for Medical Research and Development (AMED).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The Institutional Review Board at The University of Tokyo approved the study protocol.
Informed consent
Informed consent was waived because of the anonymous nature of the data.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ishimaru, M., Ono, S., Matsui, H. et al. Association between perioperative oral care and postoperative pneumonia after cancer resection: conventional versus high-dimensional propensity score matching analysis. Clin Oral Invest 23, 3581–3588 (2019). https://doi.org/10.1007/s00784-018-2783-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-018-2783-5