Abstract
Introduction
High-turnover bone disease is a major consequence of SHPT and may explain the high risk for fracture in patients with advanced chronic kidney disease (CKD). Bisphosphonates suppress bone turnover and improve bone strength, but their effects have not been fully characterized in advanced CKD with severe SHPT. Bisphosphonates also increase 1,25-dihydroxyvitamin D levels in normal and uremic rats, but the underlying mechanism remains to be determined.
Materials and methods
We investigated the skeletal and mineral metabolic effects of RIS, a pyridinyl bisphosphonate, in rats with severe SHPT induced by 5/6 nephrectomy plus a high phosphate diet.
Results
Nephrectomized rats developed severe SHPT, along with hyperphosphatemia, low 1,25-dihydroxyvitamin D, and markedly increased FGF23. Moreover, these rats exhibited characteristic features of high-turnover renal osteodystrophy, including increased indices of trabecular bone turnover, decreased cortical bone thickness, inferior cortical biomechanical properties, and a prominent increase in peritrabecular fibrosis. RIS treatment increased bone volume and partially attenuated trabecular bone remodeling, cortical bone loss, and mechanical properties, whereas it produced a marked improvement in peritrabecular fibrosis along with a corresponding decrease in osteogenic gene markers. RIS treatment also suppressed the elevation of FGF23, which was associated with increased 1,25-dihydroxyvitamin D.
Conclusions
In a rat model of severe SHPT, treatment with RIS partially attenuated histological manifestations of high-turnover bone disease. RIS treatment also suppressed the elevation of FGF23, which may explain the increased 1,25-dihydroxyvitamin D production during the treatment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Patients with chronic kidney disease (CKD) have an increased risk of fracture. The risk of fracture increases as kidney function declines, with end-stage renal disease (ESRD) patients at particularly high risk for fracture [1,2,3]. Disturbances in mineral metabolism are common in CKD patients and result in a systemic disorder termed CKD-mineral and bone disorder (CKD-MBD) [4]. Renal osteodystrophy (ROD) is one component of CKD-MBD and may explain the high risk of fracture in this population. High-turnover bone disease caused by secondary hyperparathyroidism (SHPT) is the predominant form of ROD and likely contributes to bone fragility, as several, but not all, observational studies have shown significant associations of higher parathyroid hormone (PTH) levels with an elevated risk for fracture [5,6,7]. Notably, recent clinical studies suggested that treatment of SHPT with either calcimimetics or parathyroidectomy could improve high-turnover ROD and reduce the risk of fracture [8,9,10,11]. However, the fracture incidence in ESRD patients remains unacceptably high [12, 13], underscoring the need for additional therapeutic options.
Risedronate (RIS) is a potent pyridinyl bisphosphonate that reduced the risk of fracture in women with postmenopausal osteoporosis in randomized, controlled clinical trials [14, 15]. In a secondary analysis of these trials, RIS effectively preserved bone mineral density and reduced the incidence of vertebral fractures in osteoporotic women with mild CKD [16]. However, these trials excluded patients with elevated creatinine or PTH levels; hence, the efficacy and safety of RIS in patients with more advanced CKD and high-turnover ROD remain unknown. According to experimental studies, several types of bisphosphonates improve high-turnover ROD in animal models of CKD [17,18,19,20,21,22,23]. However, most of these studies used rats with less severe renal failure and relatively mild SHPT. Thus, the skeletal effect of bisphosphonate in more severe renal impairment and SHPT remains to be determined.
One of the key features of CKD-MBD is a progressive decline in 1,25-dihydroxyvitamin D (1,25(OH)2D) levels, which contributes to the development and progression of SHPT. The etiology of the progressive reduction in 1,25(OH)2D levels in CKD is multifactorial, but recent evidence indicates that fibroblast growth factor 23 (FGF23), a bone-derived hormone, plays a central role [24,25,26]. Interestingly, previous experiments have shown that bisphosphate treatment increased 1,25(OH)2D production in normal rats [27] and nephrectomized rats [19]. This effect was also observed in parathyroidectomized rats [28, 29], suggesting that an additional mechanism independent of PTH likely contributes.
Therefore, the purpose of this study was twofold: [1] to determine the effects of RIS on bone metabolism in rats with severe SHPT induced by 5/6 nephrectomy plus a high phosphate diet and [2] to investigate the underlying mechanism of the increased 1,25(OH)2D production during bisphosphonate treatment.
Materials and methods
Animals and experimental design
Five-week-old male Sprague–Dawley rats were purchased from CLEA Japan (Tokyo, Japan). The rats were housed under standard environmental conditions (23 ± 2 °C, 55 ± 10% humidity, 12:12 h light–dark cycle) and had free access to water and standard rodent chow that contained 0.9% calcium and 0.8% phosphate (CLEA Japan), except when otherwise specified. All experiments were approved by the Institutional Review Board of Tokai University School of Medicine.
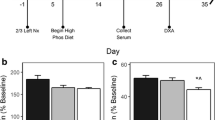
The experimental design is summarized in Fig. 1. At 6 weeks of age, rats were subjected to 5/6 nephrectomy or sham surgery. In the 5/6 nephrectomy, rats were anesthetized, and two-thirds of the right kidney (upper and lower poles) was resected and returned to the renal fossa. After 1 week of recovery, total nephrectomy of the left kidney was performed. To promote the severity of ROD, we switched nephrectomized rats to a high phosphate diet, which contained 0.9% calcium and 1.2% phosphate (CLEA Japan), 1 week after the second surgery. Sham-operated rats were kept on the standard diet.
After 6 weeks of disease progression, nephrectomized rats were randomly assigned to vehicle (0.9% saline) or 5 μg/kg body weight RIS (a gift from EA Pharma Co., Ltd., Tokyo, Japan) administered subcutaneously twice weekly for 8 weeks. The drug dose was chosen on the basis of previous publications on RIS treatment in rats [30]. All sham-operated rats received twice-weekly injections of vehicle. After 8 weeks of treatment with RIS or vehicle, rats were placed in metabolic cages for 24-h urine collection and were killed for analyses.
Serum and urine biochemistries
Serum and urine calcium, phosphorus, creatinine, and blood urea nitrogen (BUN) levels were measured using standard methods. Serum PTH levels were measured using a rat intact PTH ELISA (Immutopics, San Clemente, CA). Serum FGF23 levels were measured using both an intact FGF23 ELISA, which exclusively measures the full-length protein (Kainos Laboratories, Tokyo, Japan), and a murine C-terminal FGF23 ELISA, which recognizes the intact protein and its C-terminal cleavage fragments (Immutopics, San Clemente, CA). Serum 1,25(OH)2D levels were measured using a radioimmunoassay (Immunodiagnostics Systems, Fountain Hills, AZ). Serum levels of the N-terminal propeptide of type I procollagen (PINP) and C-terminal telopeptide fragments of type I collagen (CTX) were measured using enzyme immunoassays (Immunodiagnostic Systems).
Bone histology and histomorphometry
For dynamic histomorphometry, rats were injected intraperitoneally with fluorochromes tetracycline hydrochloride (25 mg/kg body weight; Nacalai Tesque, Kyoto, Japan) and calcein (8 mg/kg body weight; Nacalai Tesque) 9 and 2 days prior to sacrifice, respectively. At the time of sacrifice, the right tibia was harvested and fixed in 70% ethanol. The fixed bones were dehydrated in acetone and embedded in methyl methacrylate. Undecalcified bones were cut into 6-μm-thick sections by a motorized microtome (RM2255; Leica, Nussloch, Germany). The first consecutive section was left unstained to analyze fluorescent labeling for dynamic parameters. The second section was stained with Villanueva-Goldner for analysis of osteoclasts, osteoblasts, and osteoids. The bone sections were viewed using an Olympus BX51 microscope equipped with a Penguin 150CL digital camera (Pixera, Los Gatos, CA). Bone histomorphometric analysis was performed within the secondary spongiosa (0.8–1.2 mm away from the growth plate) under 20 × magnification using a semiautomatic image analysis system (Histometry RT Camera; System Supply, Nagano, Japan). Structural, dynamic, and cellular parameters are presented according to the standardized nomenclature [31].
Biomechanical testing
The mechanical strength of the left femur was determined with a three-point bending test using MZ-500D (Maruto, Tokyo, Japan). Bones were thawed, hydrated in saline, and then placed posterior side down on the bottom support (span = 13 mm). Load was applied vertically downwards to the midshaft with a constant rate of displacement of 2 mm/min until fracture. Based on the load-deformation curve, the maximum load (N), displacement (mm), stiffness (N/mm), and energy to failure (N mm) were determined.
Gene expression
Total RNA was isolated from the right femur and kidney using TRIzol reagent (Thermo Fisher Scientific, Waltham, MA) and an RNAqueous-4PCR kit (Thermo Fisher Scientific), respectively. For isolation from femurs, epiphyses were cut off, bone marrow was removed by centrifugation, and bone tissue was homogenized using a Shake Master NEO (Bio Medical Sciences, Tokyo, Japan) together with TRIzol reagent and 5-mm stainless beads. cDNA synthesis was performed using 0.5 μg total RNA and SuperScript IV VILO Master Mix with ezDNase Enzyme (Thermo Fisher Scientific). Quantitative real-time PCR was performed on the StepOnePlus System using the TaqMan One-Step RT-PCR Master Mix Reagents kit (Thermo Fisher Scientific). Glyceraldehyde-3-phosphate dehydrogenase (GAPDH) served as the reference gene to normalize expression.
Statistical analysis
Data are represented as mean ± SD. Differences were evaluated using one-way analysis of variance (ANOVA) followed by Tukey’s post hoc test. Correlations were examined by Spearman's rank test. P < 0.05 was considered statistically significant. All analyses were performed using IBM SPSS Statistics 24 (IBM, Tokyo, Japan).
Results
Biochemistry of 5/6 nephrectomized rats treated with RIS and vehicle
Compared to sham-operated control rats, nephrectomized rats developed progressive uremia (Fig. 2a–c) and displayed reduced body weight (Fig. 2d) regardless of the treatment received. The kidney function of nephrectomized rats was approximately 15–20% of that of sham-operated rats as assessed by creatinine clearance, which corresponds to late stage 4 and early stage 5 CKD. These uremic rats showed low serum calcium (Fig. 2e), elevated serum phosphorus (Fig. 2f), and severe SHPT, but there was a nonsignificant trend towards lower PTH levels in those receiving RIS (Fig. 3a). Interestingly, nephrectomized rats receiving vehicle showed low serum 1,25(OH)2D levels, but this decrease in serum 1,25(OH)2D was not observed in RIS-treated uremic rats (Fig. 3b), despite the similar degree of uremia and SHPT. These results were consistent with those of a previous work [19] and led us to investigate whether FGF23 could be involved in the increased 1,25(OH)2D levels. Compared to the sham-operated control rats, nephrectomized rats receiving vehicle showed markedly elevated intact FGF23 levels. However, these changes were attenuated and not significant in uremic rats treated with RIS (Fig. 3c, d). Similar findings were observed for C-terminal FGF23 (Fig. 3d). Furthermore, there was a modest correlation between 1,25(OH)2D and FGF23 levels (r = − 0.545, P = 0.01; Fig. 3e) after 8 weeks of treatment with RIS or vehicle (at 22 weeks of age). Quantitative real-time PCR analysis demonstrated a large but nonsignificant increase in Cyp27b1 expression and a trend towards lower Cyp24a1 expression in the kidney of RIS-treated uremic rats compared to those in rats receiving vehicle (Figs. 3f). These results suggest that RIS treatment for ROD led to decreased FGF23 production, which in turn resulted in stimulation of renal 1,25(OH)2D synthesis. Consistent with the relatively low FGF23 in the RIS-treated uremic rats, there was a trend towards lower urinary phosphorus excretion (Fig. 3g) and higher renal expression of Napi2a (Fig. 3f) compared to those in uremic rats receiving vehicle, although the differences were nonsignificant.
a Blood urea nitrogen (BUN), b serum creatinine, c creatinine clearance, d body weight, e serum calcium, and f serum phosphorus in sham-operated rats receiving vehicle (sham), 5/6 nephrectomized rats receiving vehicle (5/6 Nx), and 5/6 nephrectomized rats receiving RIS (5/6 Nx + RIS). Data are shown as mean ± SD. *P < 0.05 versus sham (one-way ANOVA followed by Tukey’s post hoc test). n = 6–7 in each group
a PTH, b 1,25(OH)2D, c intact FGF23, and d C-terminal FGF23 in sham-operated rats receiving vehicle (sham), 5/6 nephrectomized rats receiving vehicle (5/6 Nx), and 5/6 nephrectomized rats receiving RIS (5/6 Nx + RIS) at 18 and 22 weeks of age. e Relationship between the 1,25(OH)2D and intact FGF23 levels at 22 weeks of age (r = − 0.545, P = 0.01 by Spearman's rank test). f Quantitative real-time PCR in the kidney at 22 weeks of age. g Fractional excretion of phosphate (FEP) at 18 and 22 weeks of age. Data are shown as mean ± SD. *P < 0.05 versus sham; #P < 0.05 versus 5/6 Nx (one-way ANOVA followed by Tukey’s post hoc test). n = 6–7 in each group
Bone histomorphometry and biomechanics in uremic rats treated with RIS and vehicle
Next, we performed histomorphometric analysis of the tibia to evaluate the impact of RIS on ROD. Nephrectomy resulted in an increase in bone volume fraction and trabecular number and a decrease in trabecular separation (Table 1), but this finding is consistent with previous observations in uremic animals [20, 32,33,34,35]. Nephrectomized rats exhibited a significant increase in osteoblast surface and mineral apposition rate along with a trend towards increased mineralizing surface, bone formation rate, activation frequency (Table 1), and bone formation marker PINP (Fig. 4a). These rats also showed a trend towards an increase in osteoclasts (Table 1) and significantly elevated levels of bone resorption marker CTX (Fig. 4b). Moreover, we found a prominent increase in peritrabecular fibrosis, which was not detected in the sham-operated controls (Table 1 and Fig. 4c). We also found that the nephrectomized rats showed unequivocal loss of cortical bone (Fig. 4c). These histological changes were associated with marked deterioration of the biomechanical properties of the femur (Table 2). Collectively, these findings indicate that our uremic rats fed for 14 weeks on a high phosphate diet demonstrated characteristic features of osteitis fibrosa, a high-turnover state driven by SHPT.
a Serum N-terminal propeptide of type I procollagen (PINP) and b C-terminal telopeptide fragments of type I collagen (CTX) in sham-operated rats receiving vehicle (sham), 5/6 nephrectomized rats receiving vehicle (5/6 Nx), and 5/6 nephrectomized rats receiving RIS (5/6 Nx + RIS) at 18 and 22 weeks of age. c Villanueva-Goldner staining of trabecular and cortical bone in the proximal tibia at 22 weeks of age. d Quantitative real-time PCR in the femur at 22 weeks of age. Data are shown as mean ± SD. *P < 0.05 versus sham; #P < 0.05 versus 5/6 Nx (one-way ANOVA followed by Tukey’s post hoc test). n = 6–7 in each group
The RIS treatment of the uremic rats resulted in a further increase in the already elevated bone volume fraction and trabecular number (Table 1). There was no significant difference in the osteoblast surface, mineral apposition rate, mineralizing surface, bone formation rate, or activation frequency between nephrectomized rats receiving vehicle and RIS (Table 1), but bone formation marker PINP tended to decrease in uremic rats treated with RIS (Fig. 4a). The eroded surface did not change, but uremic rats treated with RIS showed a trend towards decreases in osteoclasts (Table 1) and bone resorption marker CTX (Fig. 4b). Moreover, RIS treatment led to a striking reduction in peritrabecular fibrosis (Table 1 and Fig. 4c). Furthermore, RIS treatment attenuated cortical bone loss in nephrectomized rats (Fig. 4c). These results indicate that the histological features of high-turnover bone disease could be ameliorated by RIS treatment. We also found a significant increase in the stiffness of femurs in uremic rats that received RIS, although the improvement in other biomechanical properties was small and nonsignificant (Table 2).
Skeletal gene expression in nephrectomized rats treated with RIS and vehicle
Finally, we investigated the underlying mechanism by comparing gene expression profiles in femurs from these rats (Figs. 4D). Nephrectomy resulted in a significant upregulation of osteogenic gene markers, including runt-domain transcription factor 2 (Runx2), alkaline phosphatase (ALP), osteopontin (OPN), and osterix, along with a trend towards increased collagen type 1 (Col1a1) and osteocalcin (OCN), indicating increased osteoblastic activity. These changes were partially attenuated by RIS treatment. Nephrectomy also resulted in a trend towards a higher ratio of receptor activator of NF-κB ligand (RANKL) to osteoprotegerin (OPG), which is a marker of osteoblast- and osteocyte-mediated osteoclastogenesis. In contrast to the inhibited bone resorption in the uremic rats administered RIS, these rats revealed a further increase in the RANKL/OPG ratio. These findings are in agreement with recent in vitro studies [36] and suggest that RIS treatment activated the osteoclastogenic action of osteoblast lineage cells. However, the direct pharmacological effect on osteoclasts was even more potent and resulted in inhibition of bone resorption.
In accordance with the results of serum FGF23 levels, compared to sham-operated control rats, nephrectomized rats receiving vehicle showed a large increase in FGF23 expression of borderline significance (P = 0.07), but this increase in FGF23 expression was partially attenuated in uremic rats treated with RIS.
Discussion
High-turnover ROD is a major consequence of SHPT and could lead to increased bone fragility in CKD patients. In this study, we successfully established a rat model of hyperparathyroid bone disease induced by 5/6 nephrectomy and a high phosphate diet. These rats developed severe SHPT and demonstrated characteristic features of high-turnover ROD, including increased trabecular bone turnover, decreased cortical bone thickness, and inferior cortical biomechanical properties. Notably, these skeletal alterations were accompanied by a prominent increase in peritrabecular fibrosis, which was remarkably enhanced compared to that in previous studies [17,18,19,20,21,22,23]. These rats also showed an increase in trabecular bone volume, but this finding is consistent with previous rodent studies [20, 32,33,34,35] as well as the clinical observation that ESRD patients with high PTH levels have increased cancellous volume but decreased cortical thickness [37, 38].
Several previous studies have evaluated the skeletal effects of bisphosphonates, such as ibandronate, pamidronate, and zoledronate, in rats with CKD and relatively mild SHPT [17,18,19,20,21,22,23]. In this study, we examined the effects of RIS on bone metabolism in rats with more severe SHPT driven by 5/6 nephrectomy and a high phosphate diet. In accordance with previous animal studies [17,18,19,20,21,22,23], RIS treatment resulted in increased bone volume along with suppression of bone formation and resorption markers, supporting the improvement in high-turnover ROD. However, there was no significant improvement in the bone formation rate or eroded surface and only a partial recovery of mechanical properties. These results indicate a limited skeletal effect of RIS in the context of severe SHPT and may indicate the relative importance of lowering PTH levels over using bisphosphonate.
Interestingly, however, we found striking improvement in peritrabecular fibrosis in uremic rats treated with RIS. Peritrabecular fibrosis is a hallmark of osteitis fibrosa where fibroblast-like preosteoblasts produce a copious amount of poorly organized extracellular matrix in response to persistently elevated PTH [39, 40]. Because uremic rats treated with RIS showed elevated 1,25(OH)2D levels, as discussed below, along with a trend towards lower PTH compared to those receiving vehicle, these metabolic changes might explain the improvement in peritrabecular fibrosis by RIS treatment. Another more likely mechanism for the improvement in peritrabecular fibrosis is the direct effect of RIS on bone-resident cells. We observed a consistent decrease in the expression of osteogenic gene markers in uremic rats treated with RIS, suggesting that RIS treatment suppressed the activity of preosteoblasts and thereby the synthesis of fibrotic extracellular matrix. In agreement with our findings, several animal studies have shown that bisphosphonate inhibits osteoblastic differentiation and activity [41,42,43]. Our in vivo findings are not consistent with prior in vitro studies [44, 45] but could be explained by assuming that in vivo bisphosphonate can inhibit osteoclast activity, which in turn leads to disruption of osteoclast-osteoblast coupling and subsequent depression of osteoblastic activity. However, we should note that in a previous study, pamidronate, another bisphosphonate, did not improve osteitis fibrosa in uremic rats with SHPT [19]. These different results may be explained by differences in the types of bisphosphonates; treatment duration; and the severity of uremia, SHPT, and high-turnover bone disease. Thus, further research is clearly needed to confirm the effect of bisphosphonate on osteitis fibrosa and identify factors that may modify the effect.
Peritrabecular fibrosis is a cause of renal anemia. Thus, the marked reduction in peritrabecular fibrosis by RIS treatment raise the hypothesis of improved anemia. Unfortunately, as we did not measure red blood cell counts or hemoglobin levels in the current study, this possibility remains to be confirmed in future experiments.
Another interesting finding of this study is that RIS treatment attenuated the decrease in 1,25(OH)2D levels in uremic rats with SHPT. According to several previous studies, bisphosphonate administration increases 1,25(OH)2D levels [19, 27], but the underlying mechanisms have not been identified. Bisphosphonate stimulates renal 1-hydroxylase activity in vivo but not in vitro [29], suggesting an indirect mechanism. Early studies suggested that bisphosphonate-induced inhibition of bone resorption causes increased systemic demand for calcium, which stimulates PTH secretion and thereby enhances renal 1,25(OH)2D production [46, 47]. However, bisphosphonates also increase 1,25(OH)2D levels even in parathyroidectomized rats [28, 29], suggesting a PTH-independent action. In this study, RIS treatment in uremic rats led to decreased FGF23 levels, which were associated with increased 1,25(OH)2D levels. Although this finding does not establish a direct causal relationship, we suggest that the reduction in FGF23 by RIS treatment contributed to increased 1,25(OH)2D.
The molecular mechanism for decreased FGF23 upon RIS treatment is unknown but is consistent with the decrease in other osteogenic genes. Furthermore, a recent study demonstrated sustained suppression of osteoblast and osteocyte activity after alendronate treatment [43]. Although we could not find clear evidence of increased apoptotic osteocytes or empty lacunae, it could be inferred that RIS-induced inhibition of the biological activity of osteoblast lineage cells underlies the decreased FGF23 synthesis. Importantly, recent experimental and epidemiological studies suggest but do not prove that FGF23 has a causal role in left ventricular hypertrophy, inflammation, and immunosuppression [48,49,50]. Whether bisphosphonates such as RIS can decrease FGF23 levels in CKD patients and if so, whether the reduction in FGF23 translates into improved clinical outcomes are intriguing questions and should be explored further.
Both PTH and FGF23 increase urinary phosphate excretion by inhibiting the renal sodium-phosphate co-transporters. However, there was no difference in FEP between RIS- and vehicle-treated uremic rats, despite the trend toward lower levels of PTH and FGF23 in those receiving RIS. We have no clear explanation for this observation, but it could be assumed that the PTH and FGF23 levels in RIS-treated uremic rats were still sufficient to maximize the tubular phosphate reabsorption. It is also noteworthy that in uremic rats treated with RIS, serum calcium levels did not increase despite increased 1,25(OH)2D levels. Again, the underlying mechanism is unclear, but these findings might be explained by the increased influx of calcium into bone. Regulation of mineral metabolism is a complex process, and additional studies are required to confirm these possibilities.
In this study, we observed that nephrectomized rats exhibited increased trabecular bone volume despite severe high-turnover bone disease. This finding was unexpected but have been observed by other investigators [20, 32,33,34,35]. The exact mechanism for the increased bone volume in uremic animals has not been determined, but it is possible that the bone anabolic action of PTH overrode the activation of osteoclasts in response to elevated PTH. In this regard, it should be noted that rats have continuous longitudinal bone growth unlike humans, which might have favored the anabolic action of PTH and contributed to the increased bone volume after nephrectomy. Thus, our results should be interpreted with caution, and additional studies are required to determine whether the results of this animal study could be extrapolated to patients with advanced CKD.
Bisphosphonates are excreted primarily by the kidney. Thus, renal impairment leads to decreased clearance of bisphosphonates [51], but there is no evidence showing whether this issue actually leads to increased skeletal accumulation [52]. In this study, the dose of RIS was based on previous studies of rats with normal renal function [30]; hence, one may argue that the dose we used might be relatively high for uremic rats. However, the skeletal effect of RIS in our uremic rats was rather modest, and there were no signs of adynamic bone disease, suggesting that an even higher dose might be required in the setting of high-turnover bone disease associated with severe SHPT. Nonetheless, it should be noted that high concentrations of bisphosphonates are toxic to kidney cells. Furthermore, if oversuppression of bone formation occurs following bisphosphonate use, it might lead to serious adverse effects such as osteonecrosis of the jaw and atypical femoral fractures. Although not yet proven, this risk might be increased in ESRD given the decreased renal clearance. Thus, the pharmacokinetics of bisphosphonates in ESRD should be better defined, and further studies should determine if the optimal dose of bisphosphonates varies with the severity of SHPT or the degree of bone turnover.
There are several limitations to the present study. First, we did not confirm our histomorphometric findings on bone volume with other imaging methods such as dual-energy X-ray bone densitometry. Second, the sample size was small, which limited statistical power to detect relevant differences in some analyses. Third, the experimental design featured nephrectomy prior to achievement of adult size, which could have confounded the interpretation of the biomechanics.
In conclusion, in a rat model of severe SHPT and high-turnover ROD, treatment with RIS partially attenuated trabecular bone remodeling, cortical bone loss, and mechanical properties, whereas it produced a marked improvement in peritrabecular fibrosis along with a corresponding decrease in osteogenic gene markers. Additionally, RIS treatment suppressed the elevation of FGF23, which may explain the increased 1,25(OH)2D production during the treatment. Although PTH-lowering treatment should be offered as the first-line therapy and use of bisphosphonates should be considered with caution in patients with advanced CKD, our data support the need for clinical trials to test the efficacy and safety of RIS or other bisphosphonates in this population with increased bone fragility and increased risk of clinical events and mortality associated with high FGF23.
References
Nickolas TL, McMahon DJ, Shane E (2006) Relationship between moderate to severe kidney disease and hip fracture in the United States. J Am Soc Nephrol 17:3223–3232
Ensrud KE, Lui LY, Taylor BC, Ishani A, Shlipak MG, Stone KL, Cauley JA, Jamal SA, Antoniucci DM, Cummings SR (2007) Renal function and risk of hip and vertebral fractures in older women. Arch Intern Med 167:133–139
Tentori F, McCullough K, Kilpatrick RD, Bradbury BD, Robinson BM, Kerr PG, Pisoni RL (2014) High rates of death and hospitalization follow bone fracture among hemodialysis patients. Kidney Int 85:166–173
Moe S, Drueke T, Cunningham J, Goodman W, Martin K, Olgaard K, Ott S, Sprague S, Lameire N, Eknoyan G (2006) Definition, evaluation, and classification of renal osteodystrophy: a position statement from kidney disease: improving global outcomes (KDIGO). Kidney Int 69:1945–1953
Block GA, Klassen PS, Lazarus JM, Ofsthun N, Lowrie EG, Chertow GM (2004) Mineral metabolism, mortality, and morbidity in maintenance hemodialysis. J Am Soc Nephrol 15:2208–2218
Danese MD, Kim J, Doan QV, Dylan M, Griffiths R, Chertow GM (2006) PTH and the risks for hip, vertebral, and pelvic fractures among patients on dialysis. Am J Kidney Dis 47:149–156
Jadoul M, Albert JM, Akiba T, Akizawa T, Arab L, Bragg-Gresham JL, Mason N, Prutz KG, Young EW, Pisoni RL (2006) Incidence and risk factors for hip or other bone fractures among hemodialysis patients in the dialysis outcomes and practice patterns study. Kidney Int 70:1358–1366
Behets G, Spasovski G, Sterling L, Goodman WG, Spiegel DM, De Broe ME, D'Haese PC (2015) Bone histomorphometry before and after long-term treatment with cinacalcet in dialysis patients with secondary hyperparathyroidism. Kidney Int 87:846–856
Moe S, Abdalla S, Chertow G, Parfrey P, Block GA, Correa-Rotter R, Floege J, Herzog CA, London GM, Mahaffey KW, Wheeler DC, Dehmel B, Goodman WG, Drüeke TB (2015) Effects of cinacalcet on fracture events in patients receiving hemodialysis: the EVOLVE trial. J Am Soc Nephrol 26:1466–1475
Yajima A, Ogawa Y, Takahashi H, Tominaga Y, Inou T, Otsubo O (2003) Changes of bone remodeling immediately after parathyroidectomy for secondary hyperparathyroidism. Am J Kidney Dis 42:729–738
Rudser K, de Boer I, Dooley A, Young B, Kestenbaum B (2007) Fracture risk after parathyroidectomy among chronic hemodialysis patients. J Am Soc Nephrol 18:2401–2407
Arneson T, Li S, Liu J, Kilpatrick R, Newsome B, Peter W (2013) Trends in hip fracture rates in US hemodialysis patients, 1993–2010. Am J Kidney Dis 62:747–754
Wakasugi M, Kazama J, Wada A, Hamano T, Masakane I, Narita I (2018) Hip fracture trends in Japanese dialysis patients, 2008–2013. Am J Kidney Dis 71:173–181
Harris ST, Watts NB, Genant HK, McKeever CD, Hangartner T, Keller M, Chesnut CH 3rd, Brown J, Eriksen EF, Hoseyni MS, Axelrod DW, Miller PD (1999) Effects of risedronate treatment on vertebral and nonvertebral fractures in women with postmenopausal osteoporosis: a randomized controlled trial. JAMA 282:1344–1352
McClung MR, Geusens P, Miller PD, Zippel H, Bensen WG, Roux C, Adami S, Fogelman I, Diamond T, Eastell R, Meunier PJ, Reginster JY (2001) Effect of risedronate on the risk of hip fracture in elderly women. N Engl J Med 344:333–340
Miller PD, Roux C, Boonen S, Barton IP, Dunlap LE, Burgio DE (2005) Safety and efficacy of risedronate in patients with age-related reduced renal function as estimated by the Cockcroft and Gault method: a pooled analysis of nine clinical trials. J Bone Miner Res 20:2105–2115
Geng Z, Monier-Faugere MC, Bauss F, Malluche HH (2000) Short-term administration of the bisphosphonate ibandronate increases bone volume and prevents hyperparathyroid bone changes in mild experimental renal failure. Clin Nephrol 54:45–53
Tomat A, Gamba CA, Mandalunis P, De Grandi MC, Somoza J, Friedman S, Zeni S (2005) Changes in bone volume and bone resorption by olpadronate treatment in an experimental model of uremic bone disease. J Musculoskelet Nueronal Interact 5:174–181
Jokihaara J, Pörsti IH, Kööbi P, Jolma PM, Mustonen JT, Saha HH, Sievänen H, Kannus P, Iwaniec UT, Turner RT, Järvinen TL (2008) Treatment of experimental renal osteodystrophy with pamidronate. Kidney Int 74:319–327
Lomashvili KA, Monier-Faugere M-C, Wang X, Malluche HH, O'Neill WC (2009) Effect of bisphosphonates on vascular calcification and bone metabolism in experimental renal failure. Kidney Int 75:617–625
Fischer D-C, Jensen C, Rahn A, Salewski B, Kundt G, Behets GJ, D'Haese P, Haffner D (2010) Ibandronate affects bone growth and mineralization in rats with normal and reduced renal function. Pediatr Nephrol 26:111–117
Allen MR, Chen NX, Gattone VH II, Chen X, Carr AJ, LeBlanc P, Brown D, Moe SM (2012) Skeletal effects of zoledronic acid in an animal model of chronic kidney disease. Osteoporos Int 24:1471–1481
Moe SM, Chen NX, Newman CL, Gattone VH II, Organ JM, Chen X, Allen MR (2014) A comparison of calcium to zoledronic acid for improvement of cortical bone in an animal model of CKD. J Bone Miner Res 29:902–910
Gutierrez O, Isakova T, Rhee E, Shah A, Holmes J, Collerone G, Jüppner H, Wolf M (2005) Fibroblast growth factor-23 mitigates hyperphosphatemia but accentuates calcitriol deficiency in chronic kidney disease. J Am Soc Nephrol 16:2205–2215
Hasegawa H, Nagano N, Urakawa I, Yamazaki Y, Iijima K, Fujita T, Yamashita T, Fukumoto S, Shimada T (2010) Direct evidence for a causative role of FGF23 in the abnormal renal phosphate handling and vitamin D metabolism in rats with early-stage chronic kidney disease. Kidney Int 78:975–980
Komaba H, Fukagawa M (2010) FGF23—parathyroid interaction: implications in chronic kidney disease. Kidney Int 77:292–298
Felsenfeld A, Jara A, Avedian G, Kleeman C (2000) Effects of fasting, feeding, and bisphosphonate administration on serum calcitriol levels in phosphate-deprived rats. Kidney Int 58:1016–1022
Bonjour J-P, Treschel U, Taylor CM, Fleisch H (1988) Parathyroid hormone-independent regulation of 1,25(OH)2D in response to inhibition of bone resorption. Am J Physiol 254:E260–E264
Nagao Y, Ishitobi Y, Kinoshita H, Fukushima S, Kawashima H (1991) YM175, a new bisphosphonate, increases serum 1,25-dihydroxyvitamin D in rats via stimulating renal 1-hydroxylase activity. Biochem Biophys Res Commun 180:1172–1178
Ito M, Nakayama K, Konaka A, Sakata K, Ikeda K, Maruyama T (2006) Effects of a prostaglandin EP4 agonist, ONO-4819, and risedronate on trabecular microstructure and bone strength in mature ovariectomized rats. Bone 39:453–459
Dempster DW, Compston JE, Drezner MK, Glorieux FH, Kanis JA, Malluche H, Meunier PJ, Ott SM, Recker RR, Parfitt AM (2013) Standardized nomenclature, symbols, and units for bone histomorphometry: a 2012 update of the report of the ASBMR Histomorphometry Nomenclature Committee. J Bone Miner Res 28:2–17
Tamagaki K, Yuan Q, Ohkawa H, Imazeki I, Moriguchi Y, Imai N, Sasaki S, Takeda K, Fukagawa M (2006) Severe hyperparathyroidism with bone abnormalities and metastatic calcification in rats with adenine-induced uraemia. Nephrol Dial Transplant 21:651–659
Finch JL, Tokumoto M, Nakamura H, Yao W, Shahnazari M, Lane N, Slatopolsky E (2010) Effect of paricalcitol and cinacalcet on serum phosphate, FGF-23, and bone in rats with chronic kidney disease. Am J Physiol Renal Physiol 298:F1315–F1322
Nikolov I, Joki N, Nguyen-Khoa T, Ivanovski O, Phan O, Lacour B, Drüeke TB, Massy ZA, Dos Reis LM, Jorgetti V, Lafage-Proust MH (2010) Chronic kidney disease bone and mineral disorder (CKD–MBD) in apolipoprotein E-deficient mice with chronic renal failure. Bone 47:156–163
Komaba H, Kaludjerovic J, Hu D, Nagano K, Amano K, Ide N, Sato T, Densmore MJ, Hanai JI, Olauson H, Bellido T, Larsson TE, Baron R, Lanske B (2017) Klotho expression in osteocytes regulates bone metabolism and controls bone formation. Kidney Int 92:599–611
Koch F, Merkel C, Ziebart T, Smeets R, Walter C, Al-Nawas B (2012) Influence of bisphosphonates on the osteoblast RANKL and OPG gene expression in vitro. Clin Oral Invest 16:79–86
Lindergard B, Johnell O, Nilsson BE, Wiklund PE (1985) Studies of bone morphology, bone densitometry and laboratory data in patients on maintenance hemodialysis treatment. Nephron 39:122–129
Nickolas T, Stein E, Dworakowski E, Nishiyama KK, Komandah-Kosseh M, Zhang CA, McMahon DJ, Liu XS, Boutroy S, Cremers S, Shane E (2013) Rapid cortical bone loss in patients with chronic kidney disease. J Bone Miner Res 28:1811–1820
Lotinun S, Sibonga JD, Turner RT (2005) Evidence that the cells responsible for marrow fibrosis in a rat model for hyperparathyroidism are preosteoblasts. Endocrinology 146:4074–4081
Hruska KA, Saab G, Mathew S, Lund R (2007) Renal osteodystrophy, phosphate homeostasis, and vascular calcification. Semin Dial 20:309–315
Bikle DD, Morey-Holton ER, Doty SB, Currier PA, Tanner SJ, Halloran BP (1994) Alendronate increases skeletal mass of growing rats during unloading by inhibiting resorption of calcified cartilage. J Bone Miner Res 9:1777–1787
Iwata K, Li J, Follet H, Phipps RJ, Burr DB (2006) Bisphosphonates suppress periosteal osteoblast activity independently of resorption in rat femur and tibia. Bone 39:1053–1058
Tsuboi K, Hasegawa T, Yamamoto T, Sasaki M, Hongo H, de Freitas PH, Shimizu T, Takahata M, Oda K, Michigami T, Li M, Kitagawa Y, Amizuka N (2016) Effects of drug discontinuation after short-term daily alendronate administration on osteoblasts and osteocytes in mice. Histochem Cell Biol 146:337–350
Reinholz GG, Getz B, Pederson L, Sanders ES, Subramaniam M, Ingle JN, Spelsberg TC (2000) Bisphosphonates directly regulate cell proliferation, differentiation, and gene expression in human osteoblasts. Cancer Res 60:6001–6007
Im GI, Qureshi SA, Kenney J, Rubash HE, Shanbhag AS (2004) Osteoblast proliferation and maturation by bisphosphonates. Biomaterials 25:4105–4115
Papapoulos SE, Harinck HI, Bijvoet OL, Gleed JH, Fraher LJ, O'Riordan JL (1986) Effects of decreasing serum calcium on circulating parathyroid hormone and vitamin D metabolites in normocalcaemic and hypercalcaemic patients treated with APD. Bone Miner 1:69–78
Adami S, Frijlink WB, Bijvoet OL, O'Riordan JL, Clemens TL, Papapoulos SE (1982) Regulation of calcium absorption by 1,25-dihydroxy-vitamin D: studies of the effects of a bisphosphonate treatment. Calcif Tissue Int 34:317–320
Faul C, Amaral A, Oskouei B, Hu MC, Sloan A et al (2011) FGF23 induces left ventricular hypertrophy. J Clin Invest 121:4393–4408
Singh S, Grabner A, Yanucil C, Schramm K, Czaya B, Krick S, Czaja MJ, Bartz R, Abraham R, Di Marco GS, Brand M, Wolf M, Faul C (2016) Fibroblast growth factor 23 directly targets hepatocytes to promote inflammation in chronic kidney disease. Kidney Int 90:985–996
Rossaint J, Oehmichen J, Van Aken H, Reuter S, Pavenstädt HJ, Meersch M, Unruh M, Zarbock A (2016) FGF23 signaling impairs neutrophil recruitment and host defense during CKD. J Clin Invest 126:962–974
Mitchell DY, St Peter JV, Eusebio RA, Pallone KA, Kelly SC, Russell DA, Nesbitt JD, Thompson GA, Powell JH (2000) Effect of renal function on risedronate pharmacokinetics after a single oral dose. Br J Clin Pharmacol 49:215–222
Allen M, Aref M (2017) What animal models have taught us about the safety and efficacy of bisphosphonates in chronic kidney disease. Curr Osteoporos Rep 15:171–177
Acknowledgements
This work was supported in part by a Grant from EA Pharma Co., Ltd. We thank Ms. Chigusa Ishioka for her excellent technical assistance. We are also grateful to Ms. Sachie Tanaka and Mr. Shuho Hori, the Support Center for Medical Research and Education, Tokai University.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Komaba has received honoraria, consulting fees, and/or grant support from Bayer Yakuhin, Chugai Pharmaceutical, Japan Tobacco, Kyowa Kirin, Novartis, and Ono Pharmaceutical. Dr. Wada has received honoraria, consulting fees, and/or grant support from Chugai Pharmaceutical, Daiichi Sankyo, Kyowa Kirin, and Otsuka Pharmaceutical. Dr. Nakamura received grant support from Astellas Pharma and Novartis. Dr. Fukagawa has received honoraria, consulting fees, and/or grant support from Astellas Pharma, Bayer Yakuhin, EA Pharma Co., Ltd., Kissei Pharmaceutical, Kyowa Kirin, Ono Pharmaceutical, and Torii Pharmaceutical. The remaining authors declare no competing interests.
Ethical approval
All experiments were approved by the Institutional Review Board of Tokai University School of Medicine.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Ishida, H., Komaba, H., Hamano, N. et al. Skeletal and mineral metabolic effects of risedronate in a rat model of high-turnover renal osteodystrophy. J Bone Miner Metab 38, 501–510 (2020). https://doi.org/10.1007/s00774-020-01095-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00774-020-01095-0