Abstract
It is still unclear whether the gender difference in the rate of depression cuts across cultures or is specific to some depressive symptoms. This study evaluated the gender difference in current prevalence, symptoms, comorbidity, and correlates of depression in Lagos, Nigeria. A total of 11,246 adult participants (6525 females and 4712 males) in a face-to-face household survey were assessed for symptoms of depression. They were also assessed for symptoms of anxiety, somatic symptoms, alcohol and substance use disorders, and disability. The difference between the point prevalence for symptoms of depression in females (6.3%, s.e 0.3) and males (4.4%, s.e 0.3) was significant (OR 1.28, 95% CI 1.14–1.59). Compared to males, females had significantly higher rates for anhedonia (OR 1.20), hypersomnia (OR 2.15), fatigue (OR 1.49), guilt/worthless feeling (OR 1.41), poor concentration (OR 1.32), psychomotor retardation (OR 1.51), and suicidal ideation (OR 1.32). However, poor appetite (OR 0.69) and comorbidity with alcohol use (OR 0.25) was significantly lower in females compared to males. The significantly higher rates for depression in females were only restricted to below 45 years and higher socioeconomic status. Our study further contributed to the growing literature suggesting that the gender differences in rates of depression not only cut across many cultures, but most pronounced with atypical symptoms, not affected by recall bias and seems to disappear with increasing age. These need to be considered when formulating mental health policies for equitable and acceptable health services.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Depression is the most common psychological disorder with a 12-month prevalence of between 5.5 and 5.9% and affecting about 350 million people worldwide (World Health Organization 2001). It is the leading neuropsychiatric cause of burden of diseases globally and is projected to be overall, the second leading cause of burden of diseases by 2020 (Ustun et al. 2004; WHO 2008). Cross culture epidemiologic studies have reported that women are 1.3–2 times more likely than men to meet the criteria for depression (Ustün 2000; Angst et al. 2002; Marcus et al. 2005; Schuch et al. 2014; Kim et al. 2015). While many explanations have been offered for this, if, truly the symptoms of depression differ according to gender, depression rates can then be influenced by including gender-dimorphic items in rating scales and diagnostic algorithms.
While we concentrate on the gender difference in the rates of depression, very little attention has been paid to gender differences in either the individual symptoms of depression, comorbidity with other disorders and in associated factors. Some studies have reported that atypical and somatic symptoms of depression like fatigue, hypersomnia, weight gain, and psychomotor retardation are more prevalent in women (Romans et al. 2007; Moskvina et al. 2008; Smith et al. 2008; Alexandrino-Silva et al. 2013; Parker et al. 2014; Silverstein et al. 2013), while other studies have found no difference (Bogner and Gallo 2004; Delisle et al. 2012). While studies had frequently reported comorbid alcohol use disorders in depressed men, depression in women had been frequently associated with comorbid anxiety and somatization disorders (Schuch et al. 2014).
There had been several cross-national surveys, with the most recent being the World Mental Health Survey (WMHS) (Kessler et al. 2009). However, reservations have been expressed regarding adopting the WMHS data for planning intervention in some low and middle income countries like Nigeria. Experts have suggested that the extremely low rates of disorders reported from Nigeria in the WMHS may be due to problems with cultural applicability/validity of the diagnostic instrument (Composite International Diagnostic Interview-CIDI) (Gureje et al. 2006; Kessler and Bromet 2013; Patel et al. 2013). Studies have shown that the CIDI had fair specificity and low sensitivity in detecting depression in Africa (Gelaye et al. 2013). Another issue is the possibility of recall bias in the African culture that tends to “somatize” emotional symptoms (probably leading to difficulty remembering lifetime or 12-month details of non-current emotional problems). Recently, there have been arguments (even from the WMHS team) in favor of evaluating for current prevalence of mental disorders rather than the lifetime/12-month rates (Bromet et al. 2011). Lastly, of concern was the moderate sample size of the Nigerian survey as only 4984 and 1682 participants were interviewed for the first and second stages of the survey respectively.
Lagos, with about 16 million people (National Bureau of Statistics 2014) accounts for about 10% of Nigeria’s population and is reputed to be among the top five most densely populated and stressful cities in the world. Lagos State has a very diverse population because of heavy migration from other parts of Nigeria and surrounding countries. All the Nigerian ethnic groups are well represented in Lagos. To generate data for planning mental health services, the Lagos State Mental Health Survey (LSMHS) was initiated to assess the types, patterns, and severity of common mental health problems among citizens of Lagos State, Nigeria. The overall aim of this study was to evaluate the gender difference in the “current” (point) prevalence, symptoms, comorbidity, and correlates of depression using the data from the LSMHS. We hypothesized that there will be significant gender difference not only in the prevalence of depression but in the individual symptoms, comorbid conditions, and the associated sociodemographic factors. We aim to use a gendered approach to improve our understanding of depression epidemiology and treatment and help expand the frontiers of gender equality to health outcomes.
Method
Sampling strategies and subject recruitment
Lagos state is divided into five administrative divisions with a total of 57 Local Council Development Authorities (LCDA). A mixed method of both cluster and systematic random sampling were used to determine the areas included in the project. This was to minimize potential bias, increase the power to examine the social contexts of mental health problems, and make it possible to compare individuals recruited in different geographical areas of the state. From each of the five administrative divisions, 2 LCDAs were randomly selected. From each of the 10 selected LCDA, enumeration areas (EAs) were determined according to the National Population Commission (NPC) demarcation. All selected EAs were visited by research interviewers prior to the interview phase of the survey and an enumeration and listing of all the housing units and households contained therein were done. On the average, there were about three to five households per housing unit. These lists were entered into a centralized computer data file thus creating a sample in which the probability of any individual household being selected to participate in the survey was equal for every household within an EA. A systematic random sampling was used to select 5720 housing units. In the final stage of the selection, two households were randomly selected from a housing unit (making 11,440 households in all) and the interviewers obtained a full listing of all residents in each household above 18 years. The Kish table selection method (Kish 1985) was used to select one eligible person as the respondent from each household. The Kish method is essentially designed to ensure that the person most likely to answer a question is not different in a specific way from the rest of the population. When the primary respondent was either unavailable following repeated calls or refused participation, no replacement was made within the household.
Ethical considerations
The International Guidelines for Ethical Review of Epidemiological Studies was followed throughout the project. The Ethics and Research Committee of the Lagos State University Teaching Hospital (LASUTH) gave the ethical approval for the project. Written informed consent was obtained from the participants before the questionnaire was administered.
Instruments
The LSMHS instruments were included in a booklet used for each participant. The household questionnaire included the following:
-
1.
Sociodemographic details: This included age, gender, occupation, working status, marital status, ethnicity, highest education, and religion
-
2.
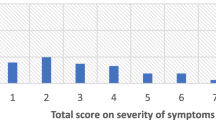
Depression: Symptoms of depression were assessed using the 9-item Depression module of Patient Health Questionnaire (PHQ-9) (Kroenke et al. 2001). The PHQ-9 is based on the DSM-IV criteria for depression with each item ranked from “not at all” (0) to “nearly every day” (3) giving PHQ-9 score range of 0–27. The authors of the scale recommended interpreting the scores as mild depression (score 5–9), moderate depression (score 10–14), moderately severe depression (score 15–19), and severe depression (score 20–27). It had been validated in Nigeria with good psychometric properties with a cutoff score of 10 and above signifying clinically significant depressive symptoms (Adewuya et al. 2006; Amoran et al. 2012; Ogunsemi et al. 2010). For all but one of the items, endorsement of either “more than half of the days” (score = 2) or “nearly every day” (score = 3) indicates presence of the symptom, apart from the suicidal ideation item which had “several days” (score = 1) also rated as endorsement as advised by the developers of the scale (Kroenke et al. 2001).
-
3.
Assessment of other conditions
-
a.
Anxiety and Somatic symptoms—These were assessed by the anxiety and the somatic modules of the Patient Health Question. Both the anxiety module (GAD-7) (Spitzer et al. 2006) and the somatic module (PHQ-15) (Kroenke et al. 2002) had been well validated in Nigeria (Amoran et al. 2012; Ogunsemi et al. 2010) and both have the score of 10 and above considered as clinically significant symptoms
-
b.
Alcohol Use Disorders (AUDs) was assessed using the short form of the Alcohol Use Disorders Identification Test (AUDIT-C) (Bush et al. 1998) which had been validated in Nigeria with good psychometric properties (Adewuya 2005). This 3-item scale has a cutoff score of 4 and above for men and 3 and above for women considered as diagnostic of AUDs
-
c.
Psychoactive Substance Use Disorders (SUDs) was assessed using the modified SUD module of the 5th version of the Mini International Neuropsychiatric Interview (M.I.N.I) (Sheehan et al. 1998). The M.I.N.I is a short structured clinical interview which enables researchers to make diagnoses of psychiatric disorders according to DSM-IV or ICD-10. It was designed for epidemiological studies and multi-center clinical trials. It was modified to include common locally used psychoactive substances.
-
d.
Disability was assessed using the 12-item version of the WHO Disability Assessment Schedule (WHODAS 2.0) (Üstün et al. 2010). The WHODAS is generic assessment instrument for health and disability applicable in both clinical and general population settings. It produces standardized disability levels and profiles and is applicable across cultures. A score of 13 and more on WHODAS is considered as moderate to severe disability.
-
a.
All the instruments were translated into the three major languages and Pidgin English (spoken by nearly 80% of Lagos population) using the WHO translation protocols. The translated versions were pilot tested on 100 participants before data collection.
Pre-field work training and pilot study
Research assistants (n = 50), supervisors (n = 5), monitors (n = 3), and the overall coordinator (n = 1) who were experienced field workers of the National Population Commission (NPC) with at least a university degree underwent a 1-week standardized training in interviewing skills and in administration of the questionnaire. Training includes field practical and dummy exercises.
Procedure and quality control
Survey data collection exercise was done over a period of 4 weeks of August to September 2015. Data collection was via face-to-face interviews via the paper and pencil method. In order to increase self-disclosure, self-completion of the questionnaire booklet was encouraged for literate participants and were given the self-administered booklets (of any language of their choice). For the non-literate participants, the questionnaires were read to them in private and their responses ticked.
Data analysis
Data was centrally analyzed using the IBM SPSS Statistics for Windows, Version 22.0 (IBM Corp 2013) by independent statisticians. The sample was weighted to account for the stratified, multistage sampling procedure, the household clustering, and to also adjust for the differences between the sample and the total Nigerian population. Results were calculated as frequencies (%), means, and standard deviations. Cross tabulations were used to estimate and compare females and males for point prevalence of depression, the depression symptoms, comorbidity with other disorders, and associated sociodemographic factors. Chi square analysis was performed with p values recorded. For ease of interpretation, best subset model logistic regression analysis was done with adjustment made for age, education level, and working status. The coefficients of multiple determination were used to determine the amount of predictability of the criterion variable based upon the set of predictor variables. Odds ratio (and 95% confidence interval) was reported for female using males as reference. Statistical significance was set at 0.05.
Results
Sociodemographic profiles
A total of 168 (1.5%) of the 11,414 participants listed for interview could not be reached despite repeated home visits, so 11,246 were interviewed giving a response rate of 98.5%. The mean age was 36.75 (SD = 12.3) years with a range of 18–74 years. Most (40.5%) of the participants were of age group 31–45 years while there were 611 (5.4%) aged above 60 years. There were 6525 (58.0%) females, 7797 (69.3%) were married, 5958 (53.0%) had secondary school education, 7526 (66.9%) were petty traders or artisans, 2867 (25.5%) were not presently working, 5503 (48.9%) were from Yoruba ethic group, and 6276 (55.8%) were Christians.
As shown in Table 1, there were significantly higher proportion of females compared to males in the lower (18–30 years) age group and this is reversed in older age groups. Also, females have significantly higher rates of being divorced, widowed, or separated while males are significantly more likely to be single. A significantly larger proportion of the females are in the lower educational and occupational groups while the males are significantly more likely to have tertiary education or be at a higher occupational status.
Internal consistency of instruments
The internal consistency of the instruments used measured by Cronbach alpha is 0.85 for PHQ-9, 0.76 for GAD-7, 0.77 for AUDIT-C, and 0.82 for WHODAS-2.0.
Gender difference in rates of depression and its symptoms
The current (point) prevalence of clinically significant depressive symptoms (PHQ-9 score 10 and above) for the population was 5.5% (s.e 0.2, 95% CI 5.1–5.9). The rate for female was 6.3% (s.e 0.3, 95% CI 5.6–6.8) and for male was 4.4% (s.e 0.3, 95% CI 3.8–5.0) and the difference was statistically significant with OR 1.28. Table 2 showed that females showed significantly higher rates than males in mild depression (OR 1.31) and all depressive symptoms (OR 1.33). With regard to the 12 symptoms of depression outlined, Table 2 showed there are significant female preponderance in the areas of anhedonia (OR 1.20, 95% CI 1.04–1.33), hypersomnia (OR 2.15, 95% CI 1.70–3.10), fatigue (OR 1.49, 95% CI 1.21–1.81), bad/guilt feelings (OR 1.41, 95% CI 1.19–1.67), poor concentration (OR 1.32, 95% CI 1.13–1.53), psychomotor retardation (OR 1.51, 95% CI 1.09–2.11), and suicidal ideation (OR 1.32, 95% CI 1.18–1.68). The only symptoms with significantly lower proportion in females compared to male was poor appetite (OR 0.69, 95% CI 0.51–0.97). There was no statistically significant gender difference in the rates for depressed mood, insomnia, overeating, and psychomotor agitation.
Gender difference in comorbidity with other disorders
Table 3 revealed that of all the comorbid disorders tested, only alcohol use disorders showed a significant gender where females have significantly lower comorbidity rates (6.6%) compared with males (22.8%) with OR 0.25 (95% CI 0.17–0.45).
Gender difference in sociodemographic correlates
Gender difference in rates of depression was tested across the sociodemographic variables of age, marital status, educational status, occupational status, and present working condition. As outlined in Table 4, after adjusting for possible cofounders, while females have significantly higher rates of depression across ages 18–30 years (OR 1.63, 95% CI 1.21–2.52) and 31–45 years (OR 1.48, 95% CI 1.15–2.19), this is not sustained at higher age groups 46–60 years (OR 1.01, 95% CI 0.58–1.42) and 61–75 years (OR 0.85, 95% CI 0.42–1.77). The opposite trend could be found with occupational status as the significantly higher rates of depression in females than males at higher level occupation like professional/business (OR 3.14, 95% CI 1.32–7.29) and civil service (OR 3.00, 95% CI 1.38–6.71) disappeared with lower occupation status groups like petty trading (OR 1.12, 95% CI 0.91–1.73) and housewife/student (OR 1.22, 95% CI 0.74–1.98).
Discussion
We set out to evaluate any possible gender difference in the prevalence, symptoms, comorbidity, and correlates of depression in Nigeria. We had conducted a face-to-face interview with a large ethnically diverse community population; we had estimated for point prevalence which is relatively free from recall bias. Moreover, to capture the true essence of depression, we had used self-rating scales that had been well validated locally and we had made comparison between females and males not only on the prevalence of depression but on the individual depression symptoms, the commonly comorbid mental disorders, disability, and associated sociodemographic factors. Our main findings had been the female preponderance in rates of both the categories of depression and in some individual symptoms of depression and the specificity of the gender difference to younger age group and higher socioeconomic status.
Although the female to male ratio found in our study (1.4:1) is a bit lower than the figures reported in earlier large cross-national surveys (Ustün 2000; Angst et al. 2002; Schuch et al. 2014; Kim et al. 2015), our study still support the notion of a true gender difference in depression rates across cultures. Many explanations have been proffered for this gender difference, including possibility of artefactual determinants such as differences in threshold for caseness, measurement procedures, effect of recall bias, course of illness, help seeking and illness behavior, and depression spectrum. Also, other explanations proffered were differences in social roles and cultural norms, adverse life events to different exposure to gonadal hormones, dysregulation of the adrenal axis, and genetic factors (Piccinelli and Wilkinson 2000). In view of these, we had used a well-validated scale, we had made efforts to eliminate recall bias by assessing the point prevalence, and we had assessed for the individual cognitive, atypical, and somatic symptoms of depression.
The highest female preponderance in our study was in the symptoms of hypersomnia, easy fatigability, and psychomotor retardation. This specificity of gender difference to some atypical features of depression had been reported across cultures (Romans et al. 2007; Moskvina et al. 2008; Smith et al. 2008; Alexandrino-Silva et al. 2013; Parker et al. 2014; Schuch et al. 2014; Kim et al. 2015; 14). It has been shown that atypical symptoms, apart from being more prevalent in females, are associated with earlier age of onset, more depressive symptoms, chronicity, increased comorbidity rate of other mental disorders, higher suicidal risk, increased disability, and greater functional impairment (Angst et al. 2006). It is worth-noting that, in agreement with some studies, we found higher female preponderance in suicidal ideation (Romans et al. 2007; Kim et al. 2015).
However, while we found statistically significant male preponderance of poor appetite, no gender difference was found in symptoms of overeating. In explaining this, it is important to remember that there is wide difference between cultures in the perception of the ideal female weight and body built with Africans favoring a bigger and more rounded built (Oloruntoba-Oju 2007; Townsend et al. 2014). How this may have affected the females eating habit during healthy and depressed periods will require further exploration. We can also view this from the male angle as there is a possibility of an association between lack of appetite and increased consumption of alcoholic beverages, and this could reflect a possible cultural way of male response at situation of stress (Kelly et al. 2008).
The only significant gender difference in comorbid disorders found in our study was preponderance of alcohol use disorders in men (22.8 vs 6.6%). This is expected and in agreement with earlier studies (Schuch et al. 2014). There has been a long standing reported association between depression and alcohol use disorders. Men have been reported to drink more than women particularly in the low and middle income countries, and while excessive alcohol use could precipitate depression, depressed men also tend to use alcohol more than non-depressed men (Davidson and Ritson 1993; Grant and Harford 1995). Despite significant female preponderance of atypical (somatic) depression symptoms, we could not find a significant gender difference in comorbid somatization disorder. Issues regarding importance and contribution of somatic symptoms to the gender difference in depression are still controversial (Delisle et al. 2012; Silverstein et al. 2013).
We found that while there was significant female preponderance in rate of depression below the age of 45 years, this difference could not be sustained with increasing age. While some earlier studies have suggested an inverted U-shaped female/male ratio for depression rates over the life cycle (Eaton et al. 1989; Bebbington et al. 1998; Gutiérrez-Lobos et al. 2002), others have found a weaker association between depression and gender with increasing age (Patten et al. 2016), both of these probably due to depression in women becoming less frequent after the menopause.
A similar trend is seen with occupational status in our study. While we found significant female/male ratio in depression with the higher occupational status, this gender difference disappears with lower occupational groups. This contrasts with the overall effect of occupational and educational status on depression with higher rates among the lower occupational and educational groups. Further studies are needed to confirm our findings and explore why highly educated female professionals are likely to suffer from depression more than their male counterparts while there is no difference between the gender at the lower occupational and educational levels.
Our study has some limitations. First, we had used rating scales (instead of diagnostic instruments) to assess for depression and other comorbid disorders, but these were well validated scales in our environment with good psychometric properties. Secondly our study was limited to only Lagos in southwestern Nigeria which is one of the 36 states in Nigeria which made our sample biased towards the predominant tribe (Yoruba) and religion (Christianity) of the region. But Lagos is cosmopolitan in nature encompassing all tribes and religious groups in the country and is about 10% of the country’s population. The strength of our study lies in its assessing for the point prevalence of depression, our large sample size, and exploring both the symptom frequencies and comorbidity of depression.
Conclusion
In conclusion, our study has further contributed to the growing literature that the gender differences in rates of depression cut across many cultures including those in sub-Sahara Africa. It also further supports the argument that the difference is most pronounced with atypical symptoms of depression. Moreover, our assessment of current symptoms suggests that the gender difference is real and not due to differences in symptoms recall bias and we have further shown that the gender difference seems to disappear with increasing age. It is therefore imperative that in formulating mental health policies, careful attention must be paid to the gender differences in depression and possibly other disorders for equitable and acceptable health services.
References
Adewuya AO (2005) Validation of the alcohol use disorders identification test (audit) as a screening tool for alcohol-related problems among Nigerian university students. Alcohol Alcohol 40:575–577
Adewuya AO, Ola BA, Afolabi OO (2006) Validity of the patient health questionnaire (PHQ-9) as a screening tool for depression amongst Nigerian university students. J Affect Disord 96:89–93
Alexandrino-Silva C, Wang YP, Carmen Viana M, Bulhões RS, Martins SS, Andrade LH (2013) Gender differences in symptomatic profiles of depression: results from the São Paulo Megacity Mental Health Survey. J Affect Disord 147:355–364
Amoran OE, Ogunsemi OO, Lasebikan VO (2012) Assessment of mental disorders using the patient health questionnaire as a general screening tool in western Nigeria: a community-based study. J Neurosci Rural Pract 3:6–11
Angst J, Gamma A, Gastpar M, Lépine JP, Mendlewicz J, Tylee A (2002) Depression Research in European Society Study. Gender differences in depression. Epidemiological findings from the European DEPRES I and II studies. Eur Arch Psychiatry Clin Neurosci 252:201–209
Angst J, Gamma A, Benazzi F, Silverstein B, Ajdacic-Gross V, Eich D, Rössler W (2006) Atypical depressive syndromes in varying definitions. Eur Arch Psychiatry Clin Neurosci 256:44–54
Bebbington PE, Dunn G, Jenkins R, Lewis G, Brugha T, Farrell M, Meltzer H (1998) The influence of age and sex on the prevalence of depressive conditions: report from the National Survey of Psychiatry Morbidity. Psychol Med 28:9–19
Bogner HR, Gallo JJ (2004) Are higher rates of depression in women accounted for by differential symptom reporting? Soc Psychiatry Psychiatr Epidemiol 39:126–132
Bromet E, Andrade LH, Hwang I, Sampson NA, Alonso J, de Girolamo G, de Graaf R, Demyttenaere K, Hu C, Iwata N, Karam AN, Kaur J, Kostyuchenko S, Lépine JP, Levinson D, Matschinger H, Mora ME, Browne MO, Posada-Villa J, Viana MC, Williams DR, Kessler RC (2011) Cross-national epidemiology of DSM-IV major depressive episode. BMC Med 9:90
Bush K, Kivlahan DR, McDonell MB, Fihn SD, Bradley KA (1998) The AUDIT alcohol consumption questions (AUDIT-C): an effective brief screening test for problem drinking. Ambulatory Care Quality Improvement Project (ACQUIP). Alcohol Use Disorders Identification Test. Arch Intern Med 158:1789–1795
Davidson KM, Ritson EB (1993) The relationship between alcohol dependence and depression. Alcohol Alcohol 28:147–155
Delisle VC, Beck AT, Dobson KS, Dozois DJ, Thombs BD (2012) Revisiting gender differences in somatic symptoms of depression: much ado about nothing? PLoS One 7:e32490
Eaton WW, Kramer M, Anthony JC, Dryman A, Shapiro S, Locke BZ (1989) The incidence of specific DIS/DSM-III mental disorders: data from the NIMH Epidemiologic Catchment Area Program. Acta Psychiatr Scand 79:163–178
Gelaye B, Williams MA, Lemma S, Deyessa N, Bahretibeb Y, Shibre T, Wondimagegn D, Lemenih A, Fann JR, Stoep AV, Zhou XH (2013) Diagnostic validity of the composite international diagnostic interview (CIDI) depression module in an East African population. Int J Psychiatry Med 46:387–405
Grant BF, Harford TC (1995) Comorbidity between DSM-IV alcohol use disorders and major depression: results of a national survey. Drug Alcohol Depend 39:197–206
Gureje O, Lasebikan VO, Kola L, Makanjuola VA (2006) Lifetime and 12-month prevalence of mental disorders in the Nigerian Survey of Mental Health and Well-Being. Br J Psychiatry 188:465–471
Gutiérrez-Lobos K, Scherer M, Anderer P, Katschnig H (2002) The influence of age on the female/male ratio of treated incidence rates in depression. BMC Psychiatry 2:3
IBM Corp (2013) IBM SPSS Statistics for Windows, Version 22.0. Armonk: IBM Corp
Kelly MM, Tyrka AR, Price LH, Carpenter LL (2008) Sex differences in the use of coping strategies: predictors of anxiety and depressive symptoms. Depress Anxiety 25:839–846
Kessler RC, Bromet EJ (2013) The epidemiology of depression across cultures. Annu Rev Public Health 34:119–138
Kessler RC, Aguilar-Gaxiola S, Alonso J, Chatterji S, Lee S, Ormel J, Ustün TB, Wang PS (2009) The global burden of mental disorders: an update from the WHO World Mental Health (WMH) surveys. Epidemiol Psychiatr Soc 18:23–33
Kim JH, Cho MJ, Hong JP, Bae JN, Cho SJ, Hahm BJ, Lee DW, Park JI, Lee JY, Jeon HJ, Chang SM (2015) Gender differences in depressive symptom profile: results from nationwide general population surveys in Korea. J Korean Med Sci 30:1659–1666
Kish L (1985) Survey sampling. Wiley, New York
Kroenke K, Spitzer RL, Williams JB (2001) The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med 16:606–613
Kroenke K, Spitzer RL, Williams JBW (2002) The PHQ-15: validity of a new measure for evaluating somatic symptom severity. Psychosom Med 64:258–266
Marcus SM, Young EA, Kerber KB, Kornstein S, Farabaugh AH, Mitchell J, Wisniewski SR, Balasubramani GK, Trivedi MH, Rush AJ (2005) Gender differences in depression: findings from the STAR*D study. J Affect Disord 87:141–150
Moskvina V, Farmer A, Jones IR, Brewster S, Ferrero F, Gill M, Jones LA, Maier W, Mors O, Owen MJ, Perry J, Preisig M, Rietschel M, McGuffin P, Craddock N, Korszun A (2008) Sex differences in symptom patterns of recurrent major depression in siblings. Depress Anxiety 25:527–534
National Bureau of Statistics (2014) Lagos Household Survey. Central Office of Statistics (COS) - Lagos State Government
Ogunsemi OO, Oluwole FA, Abasiubong F, Erinfolami AR, Amoran OE, Ariba AJ (2010) Detection of mental disorders with the Patient Health Questionnaire in primary care settings in Nigeria. Ment Illn 2:e10
Oloruntoba-Oju T (2007) Body images, beauty culture and language in the Nigeria, African context. Understanding Human Sexuality, 2007 Series
Parker G, Fletcher K, Paterson A, Anderson J, Hong M (2014) Gender differences in depression severity and symptoms across depressive subtypes. J Affect Disord 167:351–357
Patel V, Minas H, Cohen A, Prince MJ (Eds) (2013) Global mental health: principles and practice. Oxford University Press
Patten SB, Williams JV, Lavorato DH, Wang JL, Bulloch AG, Sajobi T (2016) The association between major depression prevalence and sex becomes weaker with age. Soc Psychiatry Psychiatr Epidemiol 51:203–210
Piccinelli M, Wilkinson G (2000) Gender differences in depression. Critical review. Br J Psychiatry 177:486–492
Romans SE, Tyas J, Cohen MM, Silverstone T (2007) Gender differences in the symptoms of major depressive disorder. J Nerv Ment Dis 195:905–911
Schuch JJ, Roest AM, Nolen WA, Penninx BW, de Jonge P (2014) Gender differences in major depressive disorder: results from the Netherlands study of depression and anxiety. J Affect Disord 156:156–163
Sheehan D, Lecruiber Y, Sheehan KH, Amorim P, Janavs J, Weiller E, Hergueta T, Baker R, Dunbar GC (1998) The Mini International Neuropsychiatric Interview (MINI): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry 59:22–33
Silverstein B, Edwards T, Gamma A, Ajdacic-Gross V, Rossler W, Angst J (2013) The role played by depression associated with somatic symptomatology in accounting for the gender difference in the prevalence of depression. Soc Psychiatry Psychiatr Epidemiol 48:257–263
Smith DJ, Kyle S, Forty L, Cooper C, Walters J, Russell E, Caesar S, Farmer A, McGuffin P, Jones I, Jones L, Craddock N (2008) Differences in depressive symptom profile between males and females. J Affect Disord 108:279–284
Spitzer RL, Kroenke K, Williams JBW, Löwe B (2006) A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med 166:1092–1097
Townsend C, Takishima-Lacasa JY, Latner JD, Grandinetti A, Keawe'aimoku Kaholokula J (2014) Ethnic and gender differences in ideal body size and related attitudes among Asians, Native Hawaiians, and Whites. Hawaii J Med Public Health 73:236–243
Ustün TB (2000) Cross national epidemiology of depression and gender. J Gend Specif Med 3:54–58
Ustun TB, Ayuso-Mateos J, Chatterji S, Mathers C, Murray C (2004) Global burden of depressive disorders in the year 2000. Br J Psychiatry 184:386–392
Üstün TB, Kostanjsek N, Chatterji S, Rehm J (2010) Measuring health and disability: manual for WHO disability assessment schedule (WHODAS 2.0). WHO; Geneva
World Health Organization (2001) The World Health Report 2001. Mental health: new understanding, new hope
World Health Organization (2008) The global burden of disease 2004. Switzerland, Geneva
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The International Guidelines for Ethical Review of Epidemiological Studies was followed throughout the project. The Ethics and Research Committee of the Lagos State University Teaching Hospital (LASUTH) gave the ethical approval for the project. Written informed consent was obtained from the participants before the questionnaire was administered.
Conflict of interest
Author 1 (Adewuya) received funding for the LSMHS from the Lagos State Ministry of Health. Authors 8 and 9 (Fasawe and Idris) work for the Lagos State Ministry of Health. Authors 2–7 (Coker, Atilola, Ola, Zachariah, Adewumi, and Olugbile) declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Adewuya, A.O., Coker, O.A., Atilola, O. et al. Gender difference in the point prevalence, symptoms, comorbidity, and correlates of depression: findings from the Lagos State Mental Health Survey (LSMHS), Nigeria. Arch Womens Ment Health 21, 591–599 (2018). https://doi.org/10.1007/s00737-018-0839-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00737-018-0839-9