Abstract
Previous work has shown that dietary l-arginine (Arg) supplementation reduced white fat mass in obese rats. The present study was conducted with cell models to define direct effects of Arg on energy-substrate oxidation in hepatocytes, skeletal muscle cells, and adipocytes. BNL CL.2 mouse hepatocytes, C2C12 mouse myotubes, and 3T3-L1 mouse adipocytes were treated with different extracellular concentrations of Arg (0, 15, 50, 100 and 400 µM) or 400 µM Arg + 0.5 mM NG-nitro-l-arginine methyl ester (L-NAME; an NOS inhibitor) for 48 h. Increasing Arg concentrations in culture medium dose-dependently enhanced (P < 0.05) the oxidation of glucose and oleic acid to CO2 in all three cell types, lactate release from C2C12 cells, and the incorporation of oleic acid into esterified lipids in BNL CL.2 and 3T3-L1 cells. Arg at 400 µM also stimulated (P < 0.05) the phosphorylation of AMP-activated protein kinase (AMPK) in all three cell types and increased (P < 0.05) NO production in C2C12 and BNL CL.2 cells. The inhibition of NOS by L-NAME moderately reduced (P < 0.05) glucose and oleic acid oxidation, lactate release, and the phosphorylation of AMPK and acetyl-CoA carboxylase (ACC) in BNL CL.2 cells, but had no effect (P > 0.05) on these variables in C2C12 or 3T3-L1 cells. Collectively, these results indicate that Arg increased AMPK activity and energy-substrate oxidation in BNL CL.2, C2C12, and 3T3-L1 cells through both NO-dependent and NO-independent mechanisms.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Nitric oxide (NO) is a free radical produced from l-arginine (Arg) by NO synthases (NOS) (Förstermann and Sessa 2012). Three isoforms of the NOS are expressed in various tissues, including insulin-sensitive tissues (liver, muscle and adipose tissue) that play an important role in whole-body homeostasis of energy substrates (Alderton et al. 2001; Förstermann et al. 1994; Jobgen et al. 2006). Besides endothelial cells (Raman et al. 1998), macrophages (Kröncke et al. 1991), and neurons (Schuman and Madison 1991), NO production has been detected for many other cell types, including hepatocytes (Nicholls-Grzemski et al. 1999), skeletal muscle cells (Williams et al. 1994), and white adipocytes (Yan et al. 2002) under both basal and stimulated conditions. The actions of NO are mediated primarily by the activation of guanylyl cyclase and the resultant production of guanosine 3´,5´-cyclic monophosphate (cGMP) (Denninger and Marletta 1999).
Our previous studies using Zucker diabetic fatty rats (Fu et al. 2005) and diet-induced obese rats (Jobgen 2007; Jobgen et al. 2009) demonstrated that dietary supplementation with Arg increased glucose and fatty acid oxidation in skeletal muscle and white adipose tissue, therefore reducing body white-fat mass. Beneficial effects of Arg supplementation on reducing white fat, increasing lean tissue mass, and improving metabolic profiles have also been reported by many research groups for rodents and other members of the animal kingdom, including diet-induced obese rats (Alam et al. 2013; Miczke et al. 2015), mice (Sellmann et al. 2017), and sheep (Satterfield et al. 2012); growing-finishing pigs (Tan et al. 2011), poultry (Fouad et al. 2013), and fish (Li et al. 2020); individuals with diabetes mellitus (Mariotti 2020; Szlas et al. 2022); and obese persons (Boon et al. 2019; Khosroshahi et al. 2020; McNeal et al. 2018). Further, we found that the beneficial effect of Arg on metabolic health was mediated partially through the activation of hepatic AMP-activated protein kinase (AMPK) (Jobgen 2007; Jobgen and Wu 2022). However, the underlying biochemical mechanisms remain largely unknown (McKnight et al. 2010; Mariotti 2020; Szlas et al. 2022).
There is growing evidence that NO regulates energy metabolism in cells and animals (Dai et al. 2013; Durante 2020; Jobgen et al. 2006; Sansbury and Hill 2014; San Martín et al. 2017). Therefore, we hypothesized that Arg increased energy metabolism through enhancing NO production and activating AMPK. This hypothesis was tested using established cell models for hepatocytes, skeletal muscle cells and adipocytes (Chen et al. 2018; Lee et al. 1997; Wang and Watford 2007).
Materials and methods
Materials
BNL CL.2 mouse hepatocytes, C2C12 mouse skeletal muscle cells and 3T3-L1 mouse preadipocytes were obtained from ATCC (Manassa, VA). Arg-free customized Dulbecco’s modified Eagle medium (DMEM) with 5 mM glucose and concentrations of other amino acids found in the plasma of adult rats (Jobgen et al. 2009), nutrient-rich DMEM, horse serum, trypsin–EDTA solution, penicillin (10,000 U/mL), streptomycin (10,000 µg/mL), and 4–12% NuPAGE Bis–Tris gels were purchased from Invitrogen (Grand Island, NY). Fetal bovine serum (FBS), NCS-II, and the bicinchoninic acid kit were procured from Hyclone (Logan, UT), Amersham (Piscataway, NJ), and Pierce (Rockford, IL), respectively. HPLC-grade methanol and water were purchased from Fisher Scientific (Houston, TX). d-[U-14C]glucose and [1-14C]oleic acid were products of American Radiolabeled Chemicals (St Louis, MO). Protease inhibitor and phosphatase inhibitor cocktails were obtained from Calbiochem (La Jolla, CA). Unless indicated, all other chemicals were procured from Sigma-Aldrich (St Louis, MO).
Cell culture
BNL CL.2 cells, C2C12 cells, and 3T3-L1 cells were cultured in 100-mm dishes with 20 ml of nutrient-rich DMEM containing 10% FBS and 100 U/mL penicillin plus 100 µg/mL streptomycin until 75–80% confluent. Cells were trypsinized and split into 25-cm2 Falcon flasks with approximately 2 × 105 cells per flask (10 ml medium) and maintained at 37 °C in a 5% CO2 incubator. The basal nutrient-rich DMEM for cell culture contained 25 mM glucose, 4 mM glutamine, and 0.4 mM Arg. For our experiments, BNL CL.2 cells at confluence were used directly, whereas differentiated C2C12 and 3T3-L1 cells were employed. After C2C12 cells reached confluence, differentiation was initiated by substituting 10% FBS with 2% horse serum in the culture medium. The medium was changed every 2 days. Four days after the initiation of differentiation, myotubes were formed and then used for the experiment.
For differentiating 3T3-L1 cells, they were cultured in 20 ml of nutrient-rich DMEM with 10% FBS until confluence. Two days post-confluence, differentiation was initiated by switching the cells to nutrient-rich DMEM containing 10% FBS, 10 µg/mL insulin, 0.5 mM 3-isobutyl-1-methylxanthine, and 10 µM dexamethasone. Two days later, the medium was changed to nutrient-rich DMEM containing 10% FBS and 10 µg/mL insulin. After an additional 2 days, cells were switched to nutrient-rich DMEM containing 10% FBS. The medium was then changed every other day. Eight days after the initiation of cell differentiation, mature white adipocytes were obtained and then used for the experiment.
The day before performing an experiment, 3T3-L1 adipocytes and BNL CL.2 hepatocytes in 25-cm2 Falcon flasks were switched to 10 ml of nutrient-rich DMEM containing 0.5% FBS for overnight, whereas C2C12 cells in 25-cm2 Falcon flasks were maintained in 10 ml of nutrient-rich DMEM containing 2% horse serum. The concentrations of serum were chosen on the basis of the consideration that a high level might mask the effect of Arg, while cell viability might be compromised in serum-free medium. On the day of the experiment, all the three types of cells were switched to 10 ml of Arg-free customized DMEM containing 5 mM D-glucose, 0.5 mM l-glutamine, and 0.5% FBS; and this basal culture medium contained 0.7 µM Arg. Arg was then added to the medium, providing concentrations of 0, 15, 50, 100, or 400 µM. In some experiments, culture medium contained 400 µM Arg plus 500 µM NG-nitro-l-arginine methyl ester (L-NAME, an NOS inhibitor). To ensure optimal inhibition of NO production in cells, L-NAME was added to the medium 1 h earlier than Arg. All the cells were cultured at 37 °C for 48 h, with the medium being changed every 24 h. At the end of the 48-h culture period, cells were used for biochemical studies and the media were analyzed for nitrite (an indicator of NO synthesis) and amino acids (Jobgen et al. 2009). We determined that at the end of the last 24-h culture in the 10 ml fresh medium with initial concentrations of 0, 15, 50, 100, and 400 µM Arg, the concentrations of Arg in the conditioned medium (means ± SEM, n = 4) for C2C12 cells were 0.53 ± 0.05, 8.5 ± 0.8, 39 ± 2.5, 83 ± 4.0, and 356 ± 9.7 µM, respectively; the concentrations of Arg in the conditioned medium for BNL CL.2 cells were 0.51 ± 0.04, 7.9 ± 0.6, 35 ± 3.1, 78 ± 4.6, and 334 ± 9.2 µM, respectively; the concentrations of Arg in the conditioned medium for 3T3-L1 mouse adipocytes were 0.54 ± 0.04, 8.2 ± 0.9, 37 ± 3.6, 80 ± 3.7, and 342 ± 10 µM, respectively.
Glucose and oleic acid oxidation
Cells obtained through the above culture were rinsed with phosphate-buffered saline (PBS) three times, and were then incubated in the same 25-cm2 Falcon flasks (placed within an unshaken cell culture incubator) at 37 °C in 2 mL of oxygenated (95%O2/5%CO2) Krebs–Henseleit bicarbonate buffer (KHB, pH 7.4) containing 5 mM d-glucose and either 0.5 μCi d-[U-14C]glucose or 0.2 mM oleic acid plus 0.5 μCi [1-14C]oleic acid. Arg or L-NAME was added to incubation medium to obtain the same respective concentrations as in the previous 48-h culture medium. The flasks were sealed tightly with rubber stoppers fitted with hanging center-wells, as we did in our previous studies of substrate oxidation by mammalian cells incubated in 25-ml polypropylene conical flasks (Wu et al. 1995). At the end of a 2-h incubation period, flasks were placed in the straight-up position, and 0.2 mL NCS-II (an alkaline solution to trap 14CO2) was added through the stopper into a 500-μl microcentrifuge tube placed in the center-well, followed by the addition of 0.2 mL of 1.5 M HClO4 to the incubation medium. Such a position of the flasks was adopted to prevent the drop of NCS-II to the incubation medium. After an additional 1-h incubation, the microcentrifuge tubes with NCS-II were carefully transferred to scintillation vials. Fifteen milliliters of counting cocktail (He and Wu 2022) were added to the vials and 14C radioactivity was determined by a Packard liquid scintillation counter (Wu et al. 1995). The specific activities of d-[U-14C]glucose and [1-14C]oleic acid in the incubation media were used to calculate the rate of CO2 production from glucose and oleic acid, respectively. The acid-lysed cell solution was centrifuged at 600 g for 10 min. The supernatant fluid was analyzed for lactate using an enzymatic method (Wu et al. 1995). The pellet fraction (protein) was washed three times with 5 ml of 2% trichloroacetic acid through centrifugation (600 g, 10 min), and then solubilized in 0.5 ml of 1 M NaOH (Wu and Thompson 1990) before the determination of protein concentration using the bicinchoninic acid kit.
Incorporation of glucose into lipids and of oleic acid into esterified lipids
The determination of d-[U-14C]glucose incorporated into lipids was performed as described by Ceddia et al. (2000). Briefly, the acidified incubation medium from the glucose oxidation experiment above was collected and mixed with 5 mL of Doles’s reagent (isopropanol/n-heptane/H2SO4; 4:1:0.25, v/v/v; Dole and Meinertz 1960). The heptane layer, which contained lipids, was carefully transferred to scintillation counting vials and dried under a fumehood. Then, 15 mL of counting cocktail (Hionic Fluor, Packard, Meriden, CT) was added to the vials for the measurement of 14C radioactivity.
The incorporation of [1-14C]oleic acid into esterified lipids was determined as described by Oliveira and Vaughan (1964) with modifications. Briefly, the acidified incubation medium from the oleic acid oxidation experiment above was mixed with 15 mL of a chloroform–methanol solution (2:1, v/v). After shaking for 20 min, 9 mL of 4% Na2CO3 (w/v in water) was added, followed by 20 min of mixing. The tubes were then centrifuged to allow the separation of aqueous and chloroform layers. The chloroform layer was transferred into clean tubes and subjected to two more washes with 4% Na2CO3. After the chloroform layer [containing esterified lipids (triglycerides and other glycerol-based esters) but no oleic acid] was transferred to a scintillation vial and dried under a fumehood, 15 mL of counting cocktail (Hionic Fluor) was added to the vials for the measurement of 14C radioactivity.
Nitrite analysis
Nitrite in cell culture medium was analyzed using an HPLC method as described by Li et al. (2000). This technique offers the advantages of high sensitivity and specificity for the determination of nitrite as an oxidation product of nitric oxide (Jobgen et al. 2007). The medium without cells was included as blanks.
Western blot analysis
BNL CL.2 cells, C2C12 cells, and 3T3-L1 cells were cultured for 48 h in the presence of 0, 50, 400 µM Arg, or 400 µM Arg plus 500 µM L-NAME, as described above. After the 48-h culture period, cells were washed with PBS three times, followed by lysis in a buffer containing 20 mM Tris–HCl (pH 7.4), 50 mM NaCl, 50 mM NaF, 50 mM EDTA, 1% Triton X-100, 1 × protease inhibitor cocktail, and 1 × phosphatase inhibitor cocktail. Cells were then scraped off into tubes and centrifuged for 10 min at 10,000g. Protein content in the supernatant fraction was analyzed using the bicinchoninic acid kit. For western blot analysis, 30 µg of protein in a sample was separated on 4–12% polyacrylamide gradient gels, transferred to nitrocellulose membranes, blocked with 5% fat-free dry milk in TTBS, and incubated with the following primary antibodies overnight at 4 °C with gentle rocking: AMPKα (Cat. #2532, Cell Signaling, 1:1000); phosphorylated AMPKα (Thr172) (Cat. #2531, Cell Signaling, 1:1000); ACC (Cat. #3662, Cell Signaling, 1:1000, detecting all isoforms of ACC protein); and phosphorylated ACC (Ser79) (Cat. #3661, Cell Signaling, 1:1000, recognizing both ACC1 and ACC2 proteins). After being washing three times with TTBS, the membranes were incubated at 25 °C for 3 h with secondary antibodies at 1:50,000 (peroxidase-labeled donkey anti-goat or anti-rabbit IgG, Jackson Immuno Research). Finally, the membranes were washed with TTBS, followed by development using Supersignal West Dura Extended Duration Substrate according to the manufacturer’s instructions (Pierce, Rockford, IL). The signals were detected on Fujifilm LAS-3000 (Tokyo, Japan).
After the last immunodetection, membrane-bound proteins were stained with Coomassie Blue R250 (Imperial™ Protein Stain; Pierce, Rockford, IL, USA) according to the manufacturer’s instructions to verify the equal loading/transfer of tissue proteins. Briefly, the blotting membrane was washed for 2 min twice with deionized water and then stained with 0.1% Coomassie R-250 (Pierce) for 5 min. The stained membrane was washed 3 times with a solution of 50% methanol/10% acetic acid and then rinsed with 10% methanol. The dry membrane was scanned using Typhoon (Amersham Bioscience, Piscataway NJ, USA) and the staining density for all proteins in each complete lane was analyzed in the DeCyder software 6.5 (Amersham Bioscience), with the area outside the protein lanes being the background, as we described previously (Wang et al. 2008).
Data expression and statistical analysis
In the western blotting, 4 samples (cell lysates) from each of the three treatment groups in Figs. 1, 2, 3, 4, 5 and 6 and from each of the two treatment groups in Figs. 7, 8 and 9 were loaded onto the same gel and the proteins were transferred to the same blotting membrane. Thus, the mean value in the bar graph represents the 4 samples per treatment group. Data, expressed as means ± SEM, were analyzed using one-way ANOVA (Assaad et al. 2014). The Tukey multiple comparison method was used to determine differences among the means of the treatment groups for 0–400 µM Arg. The paired t test was employed to analyze the data for cells treated with either 400 µM Arg or 400 µM Arg plus 0.5 mM L-NAME. Probability values ≤ 0.05 were taken to indicate statistical significance.
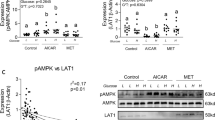
Relative protein levels for total AMPKα, phosphorylated AMPKα (P-AMPKα) and the ratio of P-AMPKα to total AMPKα in BNL CL.2 hepatocytes. Cells were cultured for 48 h in customized DMEM containing 0, 50 or 400 µM L-arginine. The same amount of cell proteins (30 µg) from different treatment groups was loaded into 4–12% SDS–polyacrylamide gels for the separation of AMPKα and phosphorylated AMPKα proteins. The protein images were developed with the use of the Supersignal West Dura Extended Duration Substrate, and two representative blots from each treatment group are shown. Data, expressed as relative values to the cells cultured without added l-arginine, are means ± SEM, n = 4. Means with different letters are different (P < 0.05)
Relative protein levels for total ACC, phosphorylated ACC (P-ACC) and the ratio of P-ACC to total ACC in BNL CL.2 hepatocytes. Cells were cultured for 48 h in customized DMEM containing 0, 50 or 400 µM l-arginine. The same amount of cell proteins (30 µg) from different treatment groups was loaded into 4–12% SDS–polyacrylamide gels for the separation of ACC and phosphorylated ACC proteins. The protein images were developed with the use of the Supersignal West Dura Extended Duration Substrate, and two representative blots from each treatment group are shown. Data, expressed as relative values to the cells cultured without added l-arginine, are means ± SEM, n = 4
Relative protein levels for total AMPKα, phosphorylated AMPKα (P-AMPKα) and the ratio of P-AMPKα to total AMPKα in C2C12 myotubes. Cells were cultured for 48 h in customized DMEM containing 0, 50 or 400 µM l-arginine. The same amount of cell proteins (30 µg) from different treatment groups was loaded into 4–12% SDS–polyacrylamide gels for the separation of AMPKα and phosphorylated AMPKα proteins. The protein images were developed with the use of the Supersignal West Dura Extended Duration Substrate, and two representative blots from each treatment group are shown. Data, expressed as relative values to the cells cultured without added L-arginine, are means ± SEM, n = 4. Means with different letters are different (P < 0.05)
Relative protein levels for total ACC, phosphorylated ACC (P-ACC) and the ratio of P-ACC to total ACC in C2C12 myotubes. Cells were cultured for 48 h in customized DMEM containing 0, 50 or 400 µM l-arginine. The same amount of cell proteins (30 µg) from different treatment groups was loaded into 4–12% SDS–polyacrylamide gels for the separation of ACC and phosphorylated ACC proteins. The protein images were developed with the use of the Supersignal West Dura Extended Duration Substrate, and two representative blots from each treatment group are shown. Data, expressed as relative values to the cells cultured without added L-arginine, are means ± SEM, n = 4. Means with different letters are different (P < 0.05)
Relative protein levels for total AMPKα, phosphorylated AMPKα (P-AMPKα) and the ratio of P-AMPKα to total AMPKα in 3T3-L1 adipocytes. Cells were cultured for 48 h in customized DMEM containing 0, 50 or 400 µM l-arginine. The same amount of cell proteins (30 µg) from different treatment groups was loaded into 4–12% SDS–polyacrylamide gels for the separation of AMPKα and phosphorylated AMPKα proteins. The protein images were developed with the use of the Supersignal West Dura Extended Duration Substrate, and two representative blots from each treatment group are shown. Data, expressed as relative values to the cells cultured without added L-arginine, are means ± SEM, n = 4. Means with different letters are different (P < 0.05)
Relative protein levels for total ACC, phosphorylated ACC (P-ACC) and the ratio of P-ACC to total ACC in 3T3-L1 adipocytes. Cells were cultured for 48 h in customized DMEM containing 0, 50 or 400 µM L-arginine. The same amount of cell proteins (30 µg) from different treatment groups was loaded into 4–12% SDS–polyacrylamide gels for the separation of ACC and phosphorylated ACC proteins. The protein images were developed with the use of the Supersignal West Dura Extended Duration Substrate, and two representative blots from each treatment group are shown. Data, expressed as relative values to the cells cultured without added L-arginine, are means ± SEM, n = 4. Means for each measured variable are not different (P > 0.05) among the three concentrations of Arg
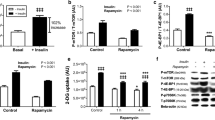
The effect of L-NAME on glucose and oleic acid oxidation, lactate release, the incorporations of glucose into lipids, and the incorporation of oleic acid into esterified lipids (A), as well as total and phosphorylated levels of AMPKα and ACC (B) in BNL CL.2 hepatocytes. Cells were cultured for 48 h in customized DMEM containing either 400 µM l-arginine (open bars) or 400 µM l-arginine plus 0.5 mM L-NAME (black bars). The same amount of cell proteins (30 µg) from different treatment groups was loaded into 4–12% SDS–polyacrylamide gels for the separation of AMPKα and phosphorylated AMPKα proteins, as well as ACC and phosphorylated ACC proteins. The protein images were developed with the use of the Supersignal West Dura Extended Duration Substrate, and two representative blots from each treatment group are shown. Data, expressed as relative values to the cells cultured without added L-arginine, are means ± SEM, n = 5 for biochemical assays and n = 4 for western blots. *P < 0.05: Different from the group without L-NAME
The effect of L-NAME on glucose and oleic acid oxidation, lactate release, the incorporations of glucose into lipids, and the incorporation of oleic acid into esterified lipids (A), as well as total and phosphorylated levels of AMPKα and ACC (B) in C2C12 myotubes. Cells were cultured for 48 h in customized DMEM containing either 400 µM l-arginine (open bars) or 400 µM L-arginine plus 0.5 mM L-NAME (black bars). The same amount of cell proteins (30 µg) from different treatment groups was loaded into 4–12% SDS–polyacrylamide gels for the separation of AMPKα and phosphorylated AMPKα proteins, as well as ACC and phosphorylated ACC proteins. The protein images were developed with the use of the Supersignal West Dura Extended Duration Substrate, and two representative blots from each treatment group are shown. Data, expressed as relative values to the cells cultured without added L-arginine, are means ± SEM, n = 6 for biochemical assays and n = 4 for western blots. Inhibition of NO synthesis by L-NAME did not affect (P > 0.05) the measured variables in C2C12 cells
The effect of L-NAME on glucose and oleic acid oxidation, lactate release, the incorporations of glucose into lipids, and the incorporation of oleic acid into esterified lipids (A), as well as total and phosphorylated levels of AMPKα and ACC (B) in 3T3-L1 adipocytes. Cells were cultured for 48 h in customized DMEM containing either 400 µM l-arginine (open bars) or 400 µM l-arginine plus 0.5 mM L-NAME (black bars). The same amount of cell proteins (30 µg) from different treatment groups was loaded into 4–12% SDS-polyacrylamide gels for the separation of AMPKα and phosphorylated AMPKα proteins, as well as ACC and phosphorylated ACC proteins. The protein images were developed with the use of the Supersignal West Dura Extended Duration Substrate, and two representative blots from each treatment group are shown. Data, expressed as relative values to the cells cultured without added l-arginine, are means ± SEM, n = 5 for biochemical assays and n = 4 for western blots. Inhibition of NO synthesis by L-NAME did not affect (P > 0.05) the measured variables in 3T3-L1 adipocytes
Results
BNL CL.2 hepatocytes
Table 1 summarizes data on glucose and oleic acid oxidation, lactate production, and the incorporation of glucose into lipids and of oleic acid into esterified lipids in BNL CL.2 cells. There were no differences in glucose oxidation, oleic acid oxidation, or the incorporation of oleic acid into esterified lipids between 0 and 50 µM Arg. However, increasing medium concentrations of Arg from 50 to 400 µM increased (P < 0.05) glucose and oleic acid oxidation, as well as the incorporation of oleic acid into esterified lipids. Exposure of the cells up to 400 µM Arg had no effect on lactate production or the incorporation of glucose into lipids. In the presence of various concentrations of Arg, a large amount of lactate was produced from glucose relative to the oxidation of glucose to CO2, whereas 85–90% of metabolized oleic acid was incorporated into esterified lipids in BNL CL.2 cells.
Staining intensities of total proteins bound to the blotting membrane for BNL CL.2 cells cultured with 0, 50, and 400 µM Arg were 1.000 ± 0.026, 1.030 ± 0.038, and 1.018 ± 0.025 AU, respectively (P > 0.05). Total and phosphorylated levels of AMPK and ACC in BNL CL.2 cells are presented in Figs. 1 and 2, respectively. There were no differences in total or phosphorylated AMPK or ACC between 0 and 50 µM Arg. Increasing Arg concentrations from 50 to 400 µM had no effect on total AMPK levels but increased (P < 0.05) phosphorylated AMPK levels by approximately 110%, and therefore, the ratio of phosphorylated AMPK to total AMPK by 80%. Compared with 0 or 50 µM Arg, exposure of the cells to 400 µM Arg did not affect (P > 0.05) total or phosphorylated levels of ACC, or the ratio of phosphorylated ACC to total ACC.
C2C12 skeletal muscle cells
In C2C12 myotubes, increasing extracellular concentrations of Arg from 0 to 50 µM increased (P < 0.05) oleic acid oxidation but had no effect (P > 0.05) on glucose oxidation or lactate production (Table 2). Increasing Arg concentration from 50 to 400 µM increased (P < 0.05) glucose oxidation and lactate production, but had no effect (P > 0.05) on oleic acid oxidation. The rate of oleic acid oxidation was 23% greater (P < 0.05) in the presence of 400 µM Arg than in the absence of its addition. In C2C12 cells cultured in the presence or absence of Arg, the rate of lactate production from glucose was much greater than the rate of glucose oxidation to CO2.
Staining intensities of total proteins bound to the blotting membrane for C2C12 cells cultured with 0, 50, and 400 µM Arg were 1.000 ± 0.033, 0.983 ± 0.036, and 1.025 ± 0.041 AU, respectively (P > 0.05). Increasing extracellular concentrations of Arg from 0 to 50 and 400 µM had no effect (P > 0.05) on total AMPK levels in C2C12 myotubes but progressively increased (P < 0.05) phosphorylated AMPK levels by 117% and 256%, respectively, and thus the ratio of phosphorylated AMPK to total AMPK by 92% and 231%, respectively (Fig. 3). Arg at 50 µM increased (P < 0.05) both total ACC and phosphorylated ACC levels approximately by 100%, as compared with 0 µM Arg. Arg at 400 µM further increased (P < 0.05) total ACC and phosphorylated ACC levels by 174% and 236%, respectively, in comparison with the values obtained at 0 µM Arg. As a result, the ratio of phosphorylated ACC to ACC was not changed (P > 0.05) by 50 µM Arg, but was increased (P < 0.05) by 400 µM Arg in C2C12 cells (Fig. 4).
3T3-L1 adipocytes
Table 3 summarizes the effect of Arg on glucose and oleic acid metabolism in 3T3-L1 cells. Lactate was the major product of glucose metabolism in adipocytes. Increasing extracellular concentrations of Arg from 0 up to 400 µM did not affect (P > 0.05) lactate production or the incorporation of glucose into lipids in these cells. The rates of glucose oxidation in 3T3-L1 cells did not differ (P > 0.05) between 0 and 100 µM Arg, but were 45% greater (P < 0.05) in the presence of 400 µM Arg than in the absence of its addition. Incorporation into esterified lipids was the major fate (80–90%) of oleic acid utilization by 3T3-L1 cells. Increasing extracellular concentrations of Arg from 0 to 50 µM had no effect (P > 0.05) on the oxidation of oleic acid or its incorporation into esterified lipids in these cells. However, the rates of oleic acid oxidation in 3T3-L1 cells were approximately 40% greater (P < 0.05) in the presence of 100–400 µM Arg than in its absence. Also, increasing Arg concentration from 50 to 100 and 400 µM increased (P < 0.05) the incorporation of oleic acid into esterified lipids in these cells by 136% and 190%, respectively.
Staining intensities of total proteins bound to the blotting membrane for 3T3-L1 cells cultured with 0, 50, and 400 µM Arg were 1.000 ± 0.037, 1.045 ± 0.049, and 1.040 ± 0.053 AU, respectively (P > 0.05). Increasing extracellular concentrations of Arg from 0 to 400 µM did not affect (P > 0.05) total AMPK but increased (P < 0.05) phosphorylated AMPK levels. Arg at 400 µM increased (P < 0.05) the ratio of phosphorylated AMPK to total AMPK by approximately 90% compared to 0 µM Arg (Fig. 5). In contrast, increasing Arg concentrations from 0 to 400 µM had no effect (P > 0.05) on total or phosphorylated ACC levels, or the ratio of phosphorylated ACC to total ACC in 3T3-L1 adipocytes (Fig. 6).
NO synthesis by BNL CL.2, C2C12, and 3T3-L1 cells
Increasing extracellular concentrations of Arg from 0 to 400 µM did not affect (P > 0.05) nitrite production in 3T3-L1 cells (Table 4). In both BNL CL.2 and C2C12 cells, nitrite production did not differ (P > 0.05) between 0 and 100 µM Arg (Table 4). However, rates of NO synthesis were 42% and 47% greater (P < 0.05) in the presence of 400 µM Arg than in its absence in BNL CL.2 and C2C12 cells, respectively. The addition of 0.5 mM L-NAME to culture medium inhibited the production of NO in the three cell lines by approximately 80% (Table 4).
Effect of L-NAME on BNL CL.2, C2C12 and 3T3-L1 cells
Addition of 0.5 mM L-NAME to culture media reduced (P < 0.05) glucose oxidation, oleic acid oxidation and lactate production by approximately 20% in BNL CL.2 cells but had no effect (P > 0.05) on the incorporation of glucose into lipids and of oleic acid into esterified lipids, compared with the absence of the NOS inhibitor (Fig. 7A). Staining intensities of total proteins bound to the blotting membrane for BNL CL.2 cells cultured with 400 µM Arg and 400 µM Arg + 0.5 mM L-NAME were 1.000 ± 0.047 and 1.028 ± 0.042 AU, respectively; those for C2C12 cells were 1.000 ± 0.042 and 1.035 ± 0.051 AU, respectively (P > 0.05); and those for 3T3-L1 cells were 1.000 ± 0.044 and 0.993 ± 0.037 AU, respectively (P > 0.05). L-NAME treatment did not affect (P > 0.05) total or phosphorylated AMPK levels, but reduced (P < 0.05) the ratio of phosphorylated AMPK to total AMPK. Total ACC levels were not altered (P > 0.05) by 0.5 mM L-NAME, but both phosphorylated ACC levels and the ratio of phosphorylated ACC to total ACC in hepatocytes were reduced (P < 0.05) by L-NAME treatment (Fig. 7B). In C2C12 myotubes (Fig. 8) or 3T3-L1 adipocytes (Fig. 9), 500 μM L-NAME did not affect (P > 0.05) glucose oxidation, oleic acid oxidation, lactate release, or protein levels for AMPK and ACC.
Discussion
Plasma concentrations of Arg in healthy overnight-fasted and fed adults are approximately 100 and 200 μM, respectively (Wu and Morris 1998; Wu et al. 2004a). Dietary supplementation with 1% Arg to animals can increase plasma Arg concentrations to about 500 μM (Wu et al. 2007, 1999). Interestingly, as low as 15 and 30 μM Arg are present in the plasma of liver-transplant recipients (Reid et al. 2007) and preterm infants (Wu et al. 2004b), due to the release of arginase from the liver and the underdevelopment of endogenous Arg synthesis pathways, respectively. In contrast, porcine allantoic fluid contains 4–6 mM Arg during early gestation (Wu et al. 1996, 1998). Thus, the concentrations of Arg used in the present study (15–400 μM) are within the physiological and pathological ranges found in mammals, and the findings are of nutritional and clinical relevance.
Arg enters mammalian cells via cationic amino acid transporters (Closs et al. 2006). Much evidence shows that increasing extracellular concentrations of Arg augments its intracellular concentrations (Wu and Meininger 2002). In BNL CL.2 hepatocytes, C2C12 myotubes and 3T3-L1 adipocytes, glucose and oleic acid oxidation increased in response to elevated extracellular concentrations of Arg from 0 to 400 µM (Tables 1, 2 and 3), indicating a role for Arg in stimulating energy substrate oxidation in these cells. In addition, the Arg treatment enhanced glycolysis in skeletal muscle cells, as indicated by the increased production of lactate (Table 2). These results were consistent with the findings of the previous in vivo studies that dietary Arg supplementation increased the metabolism of energy substrates in the skeletal muscle and adipose tissue of obese rats (Fu et al. 2005; Jobgen 2007), as well whole-body glucose oxidation and insulin sensitivity in obese men (Boon et al. 2019). Because the BNL CL.2, C2C12, and 3T3-L1 cells were derived from the fetal mouse liver, the dystrophic adult mouse skeletal muscle, and the mouse embryonic fibroblast (Kuppusamy et al. 2021; Muller and Danner 2004), these cell lines may differ from the hepatocytes, skeletal muscle, and white adipocytes of rats in both metabolism and cells signaling.
We found that phosphorylated AMPK levels in all the three cell types used in the present study were increased in response to an increase in extracellular concentrations of Arg from 0 to 400 μM (Figs. 1, 3 and 5), as reported for AMPK activation in the liver of diet-induced obese rats receiving dietary supplementation with Arg (Jobgen and Wu 2022). This result may provide a mechanism for explaining the increased oxidation of glucose and fatty acids in Arg -treated hepatocytes, skeletal muscle cells and adipocytes, on the basis of the previous reports that AMPK phosphorylation promotes substrate oxidation in insulin-sensitive cells (Kahn et al. 2005a, b). Also, in C2C12 cells, elevated levels of phosphorylated ACC, a downstream target of AMPK, increased in response to Arg supplementation, leading to reductions in ACC enzymatic activity and, therefore, the generation of malonyl-CoA [a potent inhibitor of carnitine palmitoyltransferase I (CPT-I)] from acetyl-CoA. In addition, phosphorylated AMPK stimulates malonyl-CoA decarboxylase, resulting in the increased conversion of malonyl-CoA into CO2 and acetyl-CoA (Ruderman and Prentki 2004). Thus, the inactivation of ACC and the activation of malonyl-CoA decarboxylase via their phosphorylation will lead to a decrease in intracellular concentrations of malonyl-CoA and, consequently, an increase in the activity of CPT-I (Viollet et al. 2006), thereby facilitating the transport of long-chain fatty acids from the cytosol to mitochondria for oxidation into CO2 in Arg-treated C2C12 cells.
Arg is catabolized by multiple pathways to form NO, ornithine, and proline in cultured cells (Wu and Morris 1998). The addition of 0.1 mM ornithine plus proline (the major products of Arg catabolism via the arginase pathway) to culture medium had no effect on glucose or oleic acid oxidation in endothelial cells or enterocytes (our unpublished data). These results suggest that ornithine or proline do not mediate the effect of Arg on metabolism in these cell types. Whether ornithine and proline affect substrate metabolism in BNL CL.2 hepatocytes, C2C12 myotubes and 3T3-L1 adipocytes remains to be determined.
As a stimulator of mitochondrial biogenesis, a vasodilator, and cell signaling molecule, NO has been suggested to modulate energy metabolism, fat deposition in white adipocytes, and insulin resistance in mammals including humans (Sansbury and Hill 2014) and rats (McKnight et al. 2010; Peyton et al. 2018; Wu 2022). Interestingly, increasing extracellular concentrations of Arg from 0 to 400 μM increased NO synthesis in BNL CL.2 cells, as reported for Arg-treated rat hepatocytes (Morita et al. 1996). However, an inhibition of NO synthesis by ~ 80% (Table 4) only moderately attenuated the effect of Arg on the phosphorylation of AMPK and ACC as well as glucose oxidation, glycolysis, and oleic acid oxidation in BNL CL.2 cells (Fig. 4). This result is consistent with the report that NO or cGMP can stimulate fatty acid oxidation through reducing ACC activity and enhancing CPT-I activity in rat hepatocytes (Garcia-Villafranca et al. 2003). However, an inhibition of NO synthesis had no effect on AMPK and ACC phosphorylation or glucose and oleic acid metabolism in C2C12 skeletal muscle cells and 3T3-L1 adipocytes (Figs. 5 and 6). These findings suggest that, under the experimental conditions used in the present study where culture medium contained 500 μM l-glutamine to reduce NO synthesis (Meininger and Wu 1997; Houdijk et al. 1998; Wu et al. 2001), NO was not a major regulator of AMPK and ACC activity or the oxidation of energy substrates in the three cell lines used in the present study. Consistent with this view are the following observations. First, NO synthesis in 3T3-L1 cells did not differ between 0 and 400 μM Arg (Table 4). Second, increasing extracellular concentrations of Arg from 0 to 100 μM increased glucose and oleic acid oxidation in BNL CL.2 cells (Table 1) and C2C12 cells (Table 2) but did not affect NO production in these two cell types (Table 4). It is possible that Arg catabolism is not necessary for exerting its stimulatory effect on substrate oxidation in hepatocytes, adipocytes and muscle cells and that Arg may directly activate AMPK in a cell-specific manner. In support of this notion, previous studies have shown that Arg can directly increase the expression of GTP cyclohydrolase-I in endothelial cells (Shi et al. 2004) and stimulate mTOR phosphorylation in intestinal cells (Rhoads et al. 2007).
In both BNL CL.2 hepatocytes and 3T3-L1 adipocytes, Arg increased the incorporation of oleic acid into esterified lipids. Liver and white adipose tissue are the two major sites for de novo fatty acid synthesis in rodents (Bergen and Mersmann 2005; Kalupahana et al. 2010). Because high concentrations of free long-chain fatty acids are toxic to cells (Jobgen et al. 2006), an increase in their packaging into esterified lipids may have important implications for cell integrity and the regulation of plasma concentrations of free fatty acids. This may help explain the finding that dietary Arg supplementation reduced the circulating levels of free fatty acids in ZDF rats (Fu et al. 2005) and serum concentrations of triglycerides in diet-induced obese rats (Jobgen et al. 2009). The proposed mechanisms for the beneficial effects of Arg on reducing white adipose tissue are summarized in Fig. 10. Because the liver is the principal organ for both de novo fatty acid synthesis and fatty acid oxidation in rats and humans (Bergen and Mersmann 2005), augmentation in the esterification of long-chain fatty acids into triacylglycerols, an inhibition of fatty acid synthesis, and an increase in fatty acid oxidation in hepatocytes provide a key molecular basis for the anti-obesity effect of Arg. These findings indicate that dietary supplementation with Arg coordinately regulates the expression of key genes and activity of proteins that are involved in the metabolism of energy substrates, thereby reducing excessive fat and improving insulin sensitivity in diet-induced obese rats.
The proposed mechanisms responsible for the beneficial effect of l-arginine on the oxidation of energy substrates and the synthesis of triacylglycerol in animals. Physiological concentrations of l-arginine stimulate the phosphorylation of AMPK, which then phosphorylates ACC and malonyl-CoA decarboxylase. This results in the inactivation of ACC [and thus a reduction in the generation of malonyl-CoA (an inhibitor of CPT-I) from acetyl-CoA], as well as the activation of malonyl-CoA decarboxylase [and thus an increase in the conversion of malonyl-CoA into CO2 and acetyl-CoA], leading to a decrease in intracellular concentrations of malonyl-CoA. In addition, activated AMPK stimulates the transport of glucose primarily by skeletal muscle, hepatocytes, and white adipocytes. Consequently, l-arginine enhances the activity of CPT-I and the oxidation of long-chain fatty acids to CO2, as well as the oxidation of glucose to CO2, in insulin-sensitive tissues. The symbol ( +) denotes an increase in gene expression and/or enzyme activation. The symbol (−) denotes an inhibition of gene expression and/or enzyme activity. ACC acetyl-CoA carboxylase, AMPK AMP-activated protein kinase, CPT-I carnitine palmitoyltransferase I, LCFA long-chain fatty acids, MCD malonyl-CoA decarboxylase, SCD-1 stearoyl-CoA desaturase 1, TCA tricarboxylic acid
In summary, results of the present study demonstrate that Arg enhances glucose and oleic acid oxidation in BNL CL2 hepatocytes, C2C12 myotubes, and 3T3-L1 adipocytes in association with increased AMPK phosphorylation. These effects of Arg were mediated only to a small extent by an NO-dependent mechanism in BNL CL2 cells and was independent of NO production in C2C12 and 3T3-L1 cells. We suggest that Arg itself may directly activate AMPK, thereby stimulating the oxidation of energy substrates in insulin-sensitive cells. Future experiments with AMPK inhibitors are warranted to test this hypothesis.
Abbreviations
- ACC:
-
Acetyl-CoA carboxylase
- AMPK:
-
AMP-activated protein kinase
- AU:
-
Arbitrary unit
- CPT-I:
-
Carnitine palmitoyltransferase I
- GAPDH:
-
Glyceraldehyde-3-phosphate dehydrogenase
- KHB:
-
Krebs–Henseleit bicarbonate
- MCD:
-
Malonyl-CoA decarboxylase
- L-NAME:
-
NG-Nitro-l-arginine methyl ester
- NO:
-
Nitric oxide
- NOS:
-
Nitric oxide synthase
- SCD-1:
-
Stearoyl-CoA desaturase 1
- SDS:
-
Sodium dodecyl sulfate
- S6K1:
-
Ribosomal protein S6 kinase beta-1
- TTBS:
-
Tris–Tween-buffered saline
References
Alam MA, Kauter K, Withers K, Sernia C, Brown L (2013) Chronic l-arginine treatment improves metabolic, cardiovascular and liver complications in diet-induced obesity in rats. Food Funct 4:83–91
Alderton WK, Cooper CE, Knowles RG (2001) Nitric oxide synthases: structure, function and inhibition. Biochem J 357:593–615
Assaad H, Zhou L, Carroll RJ, Wu G (2014) Rapid publication-ready MS word tables for one-way ANOVA. Springer plus 3:474
Bergen W, Mersmann HJ (2005) Comparative aspects of lipid metabolism: impact on contemporary research and use of animal models. J Nutr 135:2499–2502
Boon MR, Hanssen MJW, Brans B, Hülsman CJM, Hoeks J, Nahon KJ, Bakker C, van Klinken JB, Havekes B, Schaart G, Jazet IM, Rensen PCN, van Marken Lichtenbelt WD (2019) Effect of l-arginine on energy metabolism, skeletal muscle and brown adipose tissue in South Asian and Europid prediabetic men: a randomised double-blinded crossover study. Diabetologia 62:112–122
Ceddia RB, William WN Jr, Lima FB, Flandin P, Curi R, Giacobino JP (2000) Leptin stimulates uncoupling protein-2 mRNA expression and Krebs cycle activity and inhibits lipid synthesis in isolated rat white adipocytes. Eur J Biochem 267:5952–5958
Wu G, Jaeger LA, Bazer FW, Rhoads JM (2004b) Arginine deficiency in preterm infants: biochemical mechanisms and nutritional implications. J Nutr Biochem 15:442–451
Chen JQ, Ma XS, Yang Y, Dai ZL, Wu ZL, Wu G (2018) Glycine enhances expression of adiponectin and IL-10 in 3T3-L1 adipocytes without affecting adipogenesis and lipolysis. Amino Acids 50(5):629–640. https://doi.org/10.1007/s00726-018-2537-3
Closs EI, Boissel JP, Habermeier A, Rotmann A (2006) Structure and function of cationic amino acid transporters (CATs). J Membr Biol 213:67–77
Dai ZL, Wu ZL, Yang Y, Wang JJ, Satterfield MC, Meininger CJ, Bazer FW, Wu G (2013) Nitric oxide and energy metabolism in mammals. BioFactors 39:383–391
Denninger JW, Marletta MA (1999) Guanylate cyclase and the NO/cGMP signaling pathway. Biochim Biophys Acta 1411:334–350
Dole VP, Meinertz H (1960) Microdetermination of long-chain fatty acids in plasma and tissues. J Biol Chem 235:2595–2599
Durante W (2020) Amino acids in circulatory function and health. Adv Exp Med Biol 1265:39–56
Förstermann U, Sessa WC (2012) Nitric oxide synthases: regulation and function. Eur Heart J 33:829–837
Förstermann U, Closs EI, Pollock JS, Nakane M, Schwarz P, Gath I, Kleinert H (1994) Nitric oxide synthase isozymes. Characterization, purification, molecular cloning, and functions. Hypertension 23:1121–1131
Fouad AM, El-Senousey HK, Yang XJ, Yao JH (2013) Dietary L-arginine supplementation reduces abdominal fat content by modulating lipid metabolism in broiler chickens. Animal 7:1239–1245
Fu WJ, Haynes TE, Kohli R, Hu J, Shi W, Spencer TE, Carroll RJ, Meininger CJ, Wu G (2005) Dietary L-arginine supplementation reduces fat mass in Zucker diabetic fatty rats. J Nutr 135:714–721
Wu G, Bazer FW, Cudd TA, Jobgen WS, Kim SW, Lassala A, Li P, Matis JH, Meininger CJ, Spencer TE (2007) Pharmacokinetics and safety of arginine supplementation in animals. J Nutr 137:1673S-1680S
Garcia-Villafranca J, Guillen A, Castro J (2003) Involvement of nitric oxide/cyclic GMP signaling pathway in the regulation of fatty acid metabolism in rat hepatocytes. Biochem Pharmacol 65:807–812
He WL, Wu G (2022) Oxidation of amino acids, glucose, and fatty acids as metabolic fuels in enterocytes of developing pigs. Amino Acids 54(7):1025–1039. https://doi.org/10.1007/s00726-022-03151-7
Houdijk APJ, Visser JJ, Rijinsburger ER, Teerlink T, van Leeuwen PAM (1998) Dietary glutamine supplementation reduces plasma nitrate levels in rats. Clin Nutr 17:11–14
Jobgen WS (2007) Dietary L-arginine supplementation reduces fat mass in diet-induced obese rats. PhD Dissertation. Texas A&M University, College Station, TX, USA
Jobgen WS, Wu G (2022) Dietary L-arginine supplementation increases the hepatic expression of AMP-activated protein kinase in rats. Amino Acids. https://doi.org/10.1007/s00726-022-03194-w
Jobgen WS, Fried SK, Fu WJ, Meininger CJ, Wu G (2006) Regulatory role for the arginine-nitric oxide pathway in metabolism of energy substrates. J Nutr Biochem 17:571–588
Jobgen WS, Jobgen SC, Li H, Meininger CJ, Wu G (2007) Analysis of nitrite and nitrate in biological samples using high-performance liquid chromatography. J Chromatogr B 851:71–82
Jobgen WJ, Meininger CJ, Jobgen SC, Li P, Lee M-J, Smith SB, Spencer TE, Fried SK, Wu G (2009) Dietary L-arginine supplementation reduces white-fat gain and enhances skeletal muscle and brown fat masses in diet-induced obese rats. J Nutr 139:230–237
Kahn BB, Alquier T, Carling D, Hardie DG (2005a) AMP-activated protein kinase: ancient energy gauge provides clues to modern understanding of metabolism. Cell Metab 1:15–25
Kahn R, Buse J, Ferranini E, Stern M (2005b) The metabolic syndrome: time for a critical appraisal. Joint statement from the American Diabetes Association and the European Association for the Study of Diabetes. Diabetologia 48:1684–1699
Kalupahana NS, Claycombe KJ, Newman SJ, Stewart T, Siriwardhana N, Matthan N, Lichtenstein AH, Moustaid-Moussa N (2010) Eicosapentaenoic acid prevents and reverses insulin resistance in high-fat diet-induced obese mice via modulation of adipose tissue inflammation. J Nutr 140:1915–1922
Khosroshahi MZ, Asbaghi O, Moradi S, Kelishadi MR, Kaviani M, Mardani M, Jalili C (2020) The effects of supplementation with L-arginine on anthropometric indices and body composition in overweight or obese subjects: a systematic review and meta-analysis. J Funct Foods 71:104022
Yan H, Aziz E, Shillabeer G, Wong A, Shanghavi D, Kermouni A, Abdel-Hafez M, Lau DC (2002) Nitric oxide promotes differentiation of rat white preadipocytes in culture. J Lipid Res 43:2123–2129
Kröncke KD, Kolb-Bachofen V, Berschick B, Burkart V, Kolb H (1991) Activated macrophages kill pancreatic syngeneic islet cells via arginine-dependent nitric oxide generation. Biochem Biophys Res Commun 175:752–758
Kuppusamy P, Kim D, Soundharrajan I, Hwang I, Choi KC (2021) Adipose and muscle cell co-culture system: A novel in vitro tool to mimic the in vivo cellular environment. Biology 10:6
Lee BS, Kang HS, Pyun KH, Choi IP (1997) Roles of tyrosine kinases in the regulation of nitric oxide synthesis in murine liver cells: Modulation of NF-kappa B activity by tyrosine kinases. Hepatology 25(4):913–919. https://doi.org/10.1002/hep.510250421
Li H, Meininger CJ, Wu G (2000) Rapid determination of nitrite by reversed-phase high-performance liquid chromatography with fluorescence detection. J Chromatogr B 746:199–207
Li SL, Zhang YC, Liu N, Chen JQ, Guo LN, Dai ZL, Wang C, Wu ZL, Wu G (2020) Dietary L-arginine supplementation reduces lipid accretion by regulating fatty acid metabolism in Nile tilapia (Oreochromis niloticus). J Anim Sci Biotechnol 11:82
Mariotti F (2020) Arginine supplementation and cardiometabolic risk. Curr Opin Clin Metab Care 23:29–34
McKnight JR, Satterfield MC, Jobgen WS, Smith SB, Spencer TE, Meininger CJ, McNeal CJ, Wu G (2010) Beneficial effects of L-arginine on reducing obesity: potential mechanisms and important implications for human health. Amino Acids 39:349–357
McNeal CJ, Meininger CJ, Wilborn CD, Tekwe CD, Wu G (2018) Safety of dietary supplementation with arginine in adult humans. Amino Acids 50:1215–1229
Meininger CJ, Wu G (1997) l-Glutamine inhibits nitric oxide synthesis in bovine venular endothelial cells. J Pharmacol Exp Ther 281:448–453
Miczke A, Suliburska J, Pupek-Musialik D, Ostrowska L, Jabłecka A, Krejpcio Z, Skrypnik D, Bogdański P (2015) Original Article Effect of L-arginine supplementation on insulin resistance and serum adiponectin concentration in rats with fat diet. Int J Clin Exp Med 8:10358–10366
Morita T, Shimada Y, Ueki H, Kanagawa A (1996) Stimulation of nitric oxide-cyclic GMP pathway by L-arginine increases the release of hepatic lipase from cultured rat hepatocytes. Biol Pharm Bull 19:1371–1373
Muller EA, Danner DJ (2004) Tissue-specific translation of murine branched-chain α-ketoacid dehydrogenase kinase mRNA is dependent upon an upstream open reading frame in the 5’-untranslated region. J Biol Chem 279:44645–44655
Nicholls-Grzemski FA, Tirmenstein MA, Fariss MW (1999) Time-dependent production of nitric oxide by rat hepatocyte suspensions. Biochem Pharmacol 57:1223–1226
Oliveira MM, Vaughan M (1964) Incorporation of fatty acids into phospholipids of erythrocyte membranes. J Lipid Res 5:156–162
Peyton KJ, Liu XM, Shebib AR, Johnson FK, Johnson RA, Durante W (2018) Arginase inhibition prevents the development of hypertension and improves insulin resistance in obese rats. Amino Acids 50:747–754
Raman CS, Li H, Martasek P, Kral V, Masters BS, Poulos TL (1998) Crystal structure of constitutive endothelial nitric oxide synthase: a paradigm for pterin function involving a novel metal center. Cell 95:939–950
Reid KM, Tsung A, Kaizu T, Jeyabalan G, Ikeda A, Shao L, Wu G, Murase N, Geller DA (2007) Liver I/R Injury is improved by the arginase inhibitor, N-ω-Hydroxy-Nor-L-arginine (Nor-NOHA). Am J Physiol 292:G512-517
Rhoads JM, Corl BA, Harrell R, Niu X, Gatlin L, Phillips O, Blikslager A, Moeser A, Wu G, Odle J (2007) Intestinal ribosomal p70s6k signaling is increased in piglet rotavirus enteritis. Am J Physiol 292:G913-922
Ruderman N, Prentki M (2004) AMP kinase and malonyl-CoA targets for therapy of the metabolic syndrome. Nat Rev Drug Discov 3:340–351
San Martín A, Arce-Molina R, Galaz A, Pérez-Guerra G, Felipe Barros L (2017) Nanomolar nitric oxide concentrations quickly and reversibly modulate astrocytic energy metabolism. J Biol Chem 292:9432–9438
Sansbury BE, Hill BG (2014) Regulation of obesity and insulin resistance by nitric oxide. Free Radic Biol Med 73:383–399
Satterfield MC, Dunlap KA, Keisler DH, Bazer FW, Wu G (2012) Arginine nutrition and fetal brown adipose tissue development in diet-induced obese sheep. Amino Acids 43:1593–1603
Schuman EM, Madison DV (1991) A requirement for the intercellular messenger nitric oxide in long-term potentiation. Science 254:1503–1506
Sellmann C, Degen C, Jin CJ, Nier A, Engstler AJ, Alkhatib DH, De Bandt J-P, Bergheim I (2017) Oral arginine supplementation protects female mice from the onset of non-alcoholic steatohepatitis. Amino Acids 49:1215–1225
Shi W, Meininger CJ, Haynes TE, Hatakeyama K, Wu G (2004) Regulation of tetrahydrobiopterin synthesis and bioavailability in endothelial cells. Cell Biochem Biophys 41:415–433
Szlas A, Kurek JM, Krejpco Z (2022) The potential of L-arginine in prevention and treatment of disturbed carbohydrate and lipid metabolism—a review. Nutrients 14:961
Tan B, Yin Y, Liu Z, Tang W, Xu H, Kong X, Xi L, Yao K, Gu W, Smith SB, Wu G (2011) Dietary L-arginine supplementation differentially regulates expression of lipid-metabolic genes in porcine adipose tissue and skeletal muscle. J Nutr Biochem 22:441–445
Viollet B, Foretz M, Guigas B, Horman S, Dentin R, Bertrand L, Hue L, Andreelli F (2006) Activation of AMP-activated protein kinase in the liver: a new strategy for the management of metabolic hepatic disorders. J Physiol 574:41–53
Wang YX, Watford M (2007) Glutamine, insulin and glucocorticoids regulate glutamine synthetase expression in C2C12 myotubes, Hep G2 hepatoma cells and 3T3 L1 adipocytes. Biochim Biophys Acta 1770:594–600
Wang JJ, Chen LX, Li DF, Yin YL, Wang XQ, Li P, Dangott LJ, Hu WX, Wu G (2008) Intrauterine growth restriction affects the proteomes of the small intestine, liver and skeletal muscle in newborn pigs. J Nutr 138:60–66
Williams G, Brown T, Becker L, Prager M, Giroir BP (1994) Cytokine-induced expression of nitric oxide synthase in C2C12 skeletal muscle myocytes. Am J Physiol 267:R1020-1025
Wu G (2022) Amino acids: biochemistry and nutrition, 2nd edn. CRC Press, Boca Raton
Wu G, Meininger CJ (2002) Regulation of nitric oxide synthesis by dietary factors. Annu Rev Nutr 22:61–86
Wu G, Morris SM Jr (1998) Arginine metabolism: nitric oxide and beyond. Biochem J 336:1–17
Wu G, Thompson JR (1990) The effect of glutamine on protein turnover in chick skeletal muscle in vitro. Biochem J 265:593–598
Wu G, Knabe DA, Yan W, Flynn NE (1995) Glutamine and glucose metabolism in enterocytes of the neonatal pig. Am J Physiol 268:R334-342
Wu G, Bazer FW, Tuo W, Flynn SP (1996) Unusual abundance of arginine and ornithine in porcine allantoic fluid. Biol Reprod 54:1261–1265
Wu G, Pond WG, Ott T, Bazer FW (1998) Maternal dietary protein deficiency decreases amino acid concentrations in fetal plasma and allantoic fluid of pigs. J Nutr 128:894–902
Wu G, Flynn NE, Flynn SP, Jolly CA, Davis PK (1999) Dietary protein or arginine deficiency impairs constitutive and inducible nitric oxide synthesis by young rats. J Nutr 129:1347–1354
Wu G, Haynes TE, Li H, Yan W, Meininger CJ (2001) Glutamine metabolism to glucosamine is necessary for glutamine inhibition of endothelial nitric oxide synthesis. Biochem J 353:245–252
Wu G, Knabe DA, Kim SW (2004a) Arginine nutrition in neonatal pigs. J Nutr 134:2783S-2790S
Acknowledgements
We thank Dr. Stephen B. Smith and Dr. Cynthia J. Meininger for helpful discussions, as well as Mr. Scott Jobgen for assistance in laboratory analyses of metabolites. This research was supported by grants from American Heart Association–Texas (#0755024Y and 10GRNT4480020).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics statement
Established cell lines available from commercial companies were used for this study. Thus, the present work did not require the approval for the use of animals by Institutional Animal Care and Use Committee of Texas A&M University.
Informed consent
No informed consent is required for this study.
Additional information
Handling editor: E. Ildicho Closs.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Jobgen, W.S., Wu, G. l-Arginine increases AMPK phosphorylation and the oxidation of energy substrates in hepatocytes, skeletal muscle cells, and adipocytes. Amino Acids 54, 1553–1568 (2022). https://doi.org/10.1007/s00726-022-03195-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00726-022-03195-9