Abstract
TFF3 is a member of the trefoil factor family (TFF) predominantly secreted by mucous epithelia. Minute amounts are also expressed in the immune system and the brain. In the latter, particularly the hypothalamo-pituitary axis has been investigated in detail in the past. Functionally, cerebral TFF3 has been reported to be involved in several processes such as fear, depression, learning and object recognition, and opiate addiction. Furthermore, TFF3 has been linked with neurodegenerative and neuropsychiatric disorders (e.g., Alzheimer’s disease, schizophrenia, and alcoholism). Here, using immunohistochemistry, a systematic survey of the TFF3 localization in the adult human brain is presented focusing on extrahypothalamic brain areas. In addition, the distribution of TFF3 in the developing human brain is described. Taken together, neurons were identified as the predominant cell type to express TFF3, but to different extent; TFF3 was particularly enriched in various midbrain and brain stem nuclei. Besides, TFF3 immunostaining staining was observed in oligodendroglia and the choroid plexus epithelium. The wide cerebral distribution should help to explain its multiple effects in the CNS.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
TFF3 (formerly intestinal trefoil factor, hP1.B) belongs to the trefoil factor family (TFF) of secretory peptides (for review, see Hoffmann 2013). The mature peptide consists of 59 amino acid residues including seven cysteine residues (Hauser et al. 1993). At least in the intestine it forms disulfide-linked heteromers with the mucus-associated IgG Fc binding protein (FCGBP, Albert et al. 2010). TFF3 is widely expressed in mucous epithelia and their glands and it enhances mucosal restitution and modulates apoptosis and angiogenesis (for reviews, see May and Westley 1997; Hoffmann and Jagla 2002; Kjellev 2009; Hoffmann 2013). TFF3 is also detectable in body fluids, such as circulating blood (Gardiner et al. 2013), sputum (Jagla et al. 1999; Wiede et al. 1999; Samson et al. 2011), cerebrospinal fluid (Jagla et al. 2000; Paterson et al. 2014); urine (Rinnert et al. 2010), gastric juice (Kouznetsova et al. 2004), tears (Paulsen et al. 2002), and breast milk (Vestergaard et al. 2008). Interestingly, during pregnancy blood serum concentrations of TFF3 show a more than 47-fold increase (Samson 2013). Pathologically, TFF3 expression is dysregulated in inflammatory diseases and many neoplastic conditions (for reviews, see Kjellev 2009; Hoffmann 2013). Interestingly, lectin activity has been reported for TFF3 (Reeves et al. 2008).
Of special note, TFF3 expression has also been detected in the brain (Probst et al. 1995; reviews: Hoffmann et al. 2001; Hoffmann and Jagla 2002), where the peptide is capable of modulating various cell physiological (Probst et al. 1996; Jagla et al. 2000; Derbyshire and Ludwig 2004; Shi et al. 2012a; Liu et al. 2013; Wu et al. 2014) and behavioral processes such as fear (Schwarzberg et al. 1999), depression (Shi et al. 2012a), learning and object recognition (Shi et al. 2012b), and opiate addiction (Wu et al. 2014) processes. Moreover, molecular variants of the TFF3 gene and/or its altered expression in peripheral tissues have been linked with neurodegenerative and neuropsychiatric disorders (Alzheimer disease, Paterson et al. 2014; Parkinson’s disease: Kriks et al. 2011; schizophrenia, Chissoe St et al. 2008; Gardiner et al. 2013; alcoholism, Hashimoto et al. 2011). While local synthesis of TFF3 has unambiguously been demonstrated in oxytocin-producing neurons situated in the paraventricular and supraoptic hypothalamic nuclei (Probst et al. 1995, 1996; Griepentrog et al. 2000; Jagla et al. 2000; Schwarz et al. 2001) as well as in neurons of the rodent cerebellar internal granular layer (Fu et al. 2014), there is yet no consensus regarding the possible occurrence of TFF3 peptide in other brain regions. Remarkably, there are numerous reports on the presence of low to moderate TFF3 mRNA concentrations in most (if not all) brain areas of developing and adult murine and human brain and spinal cord (Probst et al. 1995, 1996; Reymond et al. 2002; Hinz et al. 2004; Cui et al. 2006; Pereira et al. 2009; Cadet et al. 2010; Kriks et al. 2011; Hashimoto et al. 2011; Fu et al. 2014; Allen Brain Atlas, http://human.brain-map.org/microarray/gene/show/6991?rw=t; GeneNetwork, http://www.genenetwork.org/webqtl/WebQTL.py?cmd=search&gene=Tff3; GeneCards, http://www.genecards.org/cgi-bin/carddisp.pl?gene=TFF3). Furthermore, TFF3 protein expression was detected in MAP2-expressing neurons in primary cell cultures prepared from rat cortex and hippocampus and in activated microglial cells in vitro, indicating a function for TFF3 in immunomodulatory processes of the CNS (Fu et al. 2014). However, for the human brain nearly no information is yet available on the cellular localization of TFF3 peptide in extrahypothalamic areas, although detailed knowledge of its precise distribution patterns is an indispensible prerequisite for a better understanding of the impact of TFF3 for the normal brain function as well as to rate possible disease-related changes. To fill this knowledge gap, we decided to systematically map adult and developing human brains for their regional distribution and cellular localization of TFF3 immunoreactivity.
Materials and methods
Subjects
Human postmortem brains were obtained from the New Magdeburg brain collection. The case recruitment, acquisition of personal data, performance of autopsy, and handling of autoptic material were conducted in accordance with the Declaration of Helsinki and was approved by the Ethical Committee of Magdeburg. In addition, written consent was obtained from the next-of-kin. The brains of four human subjects (three males, one female; mean age 53.4 ± 3.1 years) without a history of neuropsychiatric disorder were investigated. None of the subjects had a history of substance abuse or alcoholism. An experienced neuropathologist ruled out changes due to neurodegenerative or traumatic processes.
Prenatal brains
Human prenatal brains were obtained from three spontaneously aborted fetuses (17th gestational week, abortion; N = 1; 19th gestational week, abortions; N = 2). Brains were removed as quickly as possible (post-mortem delay between 2 and 7 h after death) and dissected into tissue blocks of about 1 cm3 or smaller volumes as previously described (Bernstein et al. 1987). Further tissue processing procedures were carried out as for adult brains. The comprehensive “the embryonic human brain: an atlas of developmental stages” (O’Rahilly and Müller 2005) was used for morphological orientation and help with the identification of developmental stages.
Human pituitary glands
Three pituitaries were obtained at autopsy (Department of Forensic Medicine, University of Essen, Germany). The donors were two female subjects (aged 55 and 59 years, who died from generalized sepsis and suicide by hanging; post-mortem intervals 24 and 14 h, respectively) and one male (aged 33 years, who was killed in a car accident; post-mortem interval 31 h). Pituitary glands were removed from the cranium, fixed in toto in 8 % formalin, embedded in paraffin, and cut at 20 μm using a sliding microtome. For morphological orientation every eighth section was stained with Azan as described earlier.
As a positive reference tissue (i.e., tissue with a known TFF3 immunostaining pattern) human colon was used.
Tissue processing
The adult subjects’ brains were removed within 9–22 h after death and fixed in toto in 8 % phosphate-buffered formaldehyde for at least 2 months (pH 7.0; T = 15–20 °C). The frontal and occipital poles were separated by coronal sectioning anterior to the genu and posterior to the splenium of the corpus callosum. After embedding in paraffin, serial coronal sections of the middle block were cut (20 μm) and mounted. The distance between the sections was 1 mm. Every 50th section was Nissl and myelin stained (Heidenhain/Woelke).
Immunohistochemistry
To immunolocalize TFF3 we used monospecific polyclonal anti-TFF3 antisera generated in rabbits. In pilot studies, the three different antisera anti-rTFF3-1 (Probst et al. 1995), anti-hTFF3-2 (Wiede et al. 1999), and anti-hTFF3-8 (same epitope as anti-hTFF3-2) were tested. All three antibodies yielded comparable and specific staining results (i.e., immunolabeling of identical cell populations) in the colon, the human hypothalamus, and the human hippocampus. Because of the somewhat lower background we performed this study with the polyclonal antiserum anti-hTFF3-2 against the C-terminal of human TFF3 (Wiede et al. 1999).
Whole brain frontal sections were collected at intervals of about 1.8 cm from the level 2 cm rostral to the splenium to the posterior splenium and from the central portion of the Raphe nuclei to the caudal portion of the olivary nuclei. After dewaxing, the sections were boiled in 10 mM citrate buffer (pH 6.0) and then pre-incubated with methanol/H2O2 to suppress endogenous peroxidases. After repeated washing with phosphate-buffered saline (PBS), the respective antibodies (anti-hCAT 1-3) were applied at dilutions of 1:200 in PBS. For visualization, the avidin–biotin method (Vectastain-peroxidase kit) with 3,3′-diaminobenzidine as chromogen was used. The color reaction was enhanced by adding 2 ml of a 0.5 % nickel ammonium sulfate solution to the diaminobenzidine as described previously (Bernstein et al. 1999). The procedure yielded a dark purplish-blue to dark-blue color reaction product. The specificity of the anti-hTFF3-2 antiserum was demonstrated by competition with the corresponding synthetic peptide, i.e., 200 μl anti-hTFF3-2 (1:200 dilution) was pre-adsorbed with 4 μg synthetic peptide overnight at 4 °C. Further specificity controls involved the replacement of the primary antibody with buffer or normal serum. No specific immunostaining was found in control sections.
Results
Frontal whole brain sections were used allowing to localize a given antigen in several brain regions at one section. TFF3 immunoreactive material was predominantly expressed in multiple neurons. However, a population of white matter (but not gray) oligodendroglial cells and choroid plexus epithelial cells were also immunopositive for TFF3. No obvious gender differences with regard to brain regional expression patterns of TFF3 were noticed.
Adult human brain
Cerebral cortex
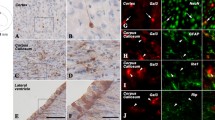
The following cortical gyri were studied: anterior and posterior cingulate, orbitofrontal, dorsolateral prefrontal, parahippocampal, entorhinal, inferior temporal, medial temporal, insular, medial frontal, and superior frontal cortex. TFF3 immunopositive neurons were found in all cortical areas under investigation. However, the number of TFF3 expressing nerve cells was rather low in most cortical areas, with the immunostaining being mostly restricted to some large layer III and V pyramidal cells and a subset of interneurons. In the entorhinal cortex, TFF3 was only found in neurons forming the pre-alpha clusters. Intracellularly, the immunoreaction was located in the perikarya and the dendrites of the nerve cells. Typically, cell nuclei were free of reaction product (Fig. 1a–e). In all regions of the forebrain, TFF3 neuronal immunostaining completely disappeared after competitive inhibition with the corresponding synthetic peptide (Fig. 1f).
TFF3 immunopositive neurons in human neocortical areas. a Layer III pyramidal neurons and some interneurons express TFF3 in the anterior cingulate cortex. b TFF3 immunoreactive neurons in the orbitofrontal cortex. c TFF3 immunoreactive neurons forming a pre-alpha cluster in the entorhinal cortex. d Moderately immunostained neurons in the temporal cortex. e A strongly TFF3 immunoreactive pyramidal cell in layer V of the posterior cingulate cortex, alongside with moderately immunostained interneurons. f Specificity control: no TFF3 immunostaining is detectable after competition with the corresponding synthetic peptide (posterior cingulate cortex, section adjacent to the section shown in d), scale bars 30 µm
Hippocampus and amygdala
In the amygdala, TFF3 was weakly expressed in a subpopulation of neurons. A considerable portion of hippocampal CA1, CA2, CA3, polymorphic and subicular pyramidal neurons showed moderate TFF3 immunostaining (Fig. 2a, b). Dentate gyrus neurons were only faintly immunostained for TFF3.
TFF3 expression in the hippocampus, basal ganglia, thalamus, and the hypothalamo-neurohypophysial system. a Moderate TFF3 expression in numerous neurons of the hippocampal polymorphic layer, bar = 30 µm. b Some intensely immunostained neurons located in the subiculum bar = 30 µm. c TFF3 expressing neurons located in the Nuc. basalis of Meynert, bar = 30 µm. d Moderate immunlabeling of small neurons situated in the medial habenula, bar = 30 µm. e Intense TFF3 immunostaining appears in many SON neurons, bar = 40 µm. f A subpopulation of PVN neurons stands out by strong immunostaining for TFF3, bar = 40 µm. g Very strong immunolabeling of multiple nerve fibers in the hypophysial stalk, bar = 30 µm. h TFF3 is highly expressed in the neurohypophysis, while the intermediate lobe is (nearly) free of immunoreaction, bar = 75 µm
Basal ganglia and thalamus
Moderately immunostained neurons were found to be scattered throughout the entire thalamus. The majority of Nucleus basalis of Meynert and medial habenular neurons were revealed to express TFF3 (Fig. 2a, d). Most neurons belonging to the lateral geniculate nucleus were also immunostained for TFF3. Multiple TFF3 expressing cells were observed in the subventricular zone.
Hypothalamus, neurohypophysis
The hypothalamus was among the brain regions with the most prominent immunolocalization of TFF3. The most pronounced immunostaining appeared in numerous supraoptic neurons and a subpopulation of neurons located in the paraventricular nucleus (Fig. 2e, f). In addition, TFF3 immunoreactive neurons were also observed in the lateral and the arcuate nuclei. A very strong immunoreactivity was present in the nerve fibers of the median eminence, the hypophysial stalk (Fig. 2g), and the neurohypophysis (Fig. 2h).
Cerebellum
Somata of a majority of Purkinje neurons were strongly immunostained for TFF3. Besides, many granule cells and a few Golgi cells stood out by intense immunostaining (Fig. 3a). However, this immunostaining was strongly but only incompletely inhibited after competition with the corresponding synthetic peptide (Fig. 3b). A moderate immunolabeling for TFF3 was also detected in neurons of deep cerebellar nuclei (i.e., dentate, emboliform and fastigial nuclei; Fig. 3c).
TFF3 expression in the cerebellum, the midbrain, and the brain stem. a Intense immunolabeling of cerebellar Purkinje cells and granular cells, bar = 30 µm. b Specificity control. A very weak immunostaining is still visible after the employment of TFF3 antiserum preadsorbed with TFF3 peptide before use, bar = 30 µm. c TFF3 immunoreactive neurons in a deep cerebellar nucleus (Nuc. dentatus), bar = 50 µm. d Neurons situated in the Nuc. ruber appear to be heavily laden with immunoreaction product. Please note that besides the purplish immunoreaction product a red–brown color appears in some neurons due to the accumulation of iron, bar = 50 µm. e Very strong immunostaining in neurons of the oculomotoric nucleus, bar = 40 µm. f Numerous trigeminal neurons appeared prominently stained for TFF3 immunoreactivity, bar = 40 µm. g Pontine nuclei neurons highly express TFF3, bar = 30 µm. h TFF3 immunoreactivity in neurons of the Raphe nuclei, bar = 30 µm (color figure online)
Midbrain
Some moderately immunopositive neurons were seen in the substantia nigra and the ventral tegmentum. Neurons belonging to of the nucleus ruber (magnocellular part) and the oculomotoric nucleus showed strong TFF3 immunoreactivity (Fig. 3d, e), while nerve cells of the Edinger-Westphal nucleus were only moderately immunolabeled.
Brain stem
Intense TFF3 immunostaining was observed in some brain stem nuclei (especially in neurons belonging to the pontine, trigeminal and abducens nuclei; Fig. 3e–g). Raphe nucleus neurons stood out by strong immunostaining (Fig. 3h), whereas the inferior olivar nucleus showed only a faint TFF3 immunoreaction.
White matter
A considerable portion of white matter oligodendrocytes was revealed to express TFF3 immunoreactive material. In addition, a few interstitial white matter neurons were found to be immunopositive for TFF3 (Fig. 4a). This immunoreaction disappeared after preabsortion of the antiserum with TFF3 peptide (Fig. 4b).
TFF3 in adult brain white matter, choroid plexus, developing human brain, and colon. a TFF3 expression in white matter cells. A portion of oligodendrocytes and some small interstitial white matter neurons (asterisk) moderately express the peptide, bar = 40 µm. b No specific immunostaining is visible after preabsorption of the antiserum with TFF3 peptide before use, bar = 40 µm. c Strong TFF3 expression in choroid plexus epithelial cells, bar = 50 µm. d Lack of specific immunostaining in choroid plexus epithelia cells after preabsorption, bar = 40 µm. e Developing human brain. Multiple TFF3 immunopositive neuroblasts in the cortex anlage. 17th gestational week, bar = 30 µm. f Developing human brain. Multiple TFF3 immunopositive neuroblasts in the cortex anlage. 19th gestational week, bar = 30 µm. g Developing human brain. Strongly immunoreactive striatal neuroblasts, bar = 30 µm. h Positive reaction control. Intensely immunostained goblet cells in the colon, bar = 75 µm
Choroid plexus
TFF3 was highly expressed in the cuboidal epithelial cells (Fig. 4c). This immunostaining was not seen after preabsorption (Fig. 4d). Faint staining was found in endothelial cells of a few capillaries. In larger blood vessels some TFF3 immunoreactive leukocytes could be observed.
The results of TFF3 immunostaining and corresponding specificity controls are summarized in Table 1.
Prenatal brains
Immunohistochemical evidence for the presence of TFF3 was noticed at the 17th gestational week, when multiple immunoreactive cells appeared in the cortex anlage (Fig. 4e). At the 19th gestational week, TFF3 is expressed in some radial glial cells and is also visible in numerous cortical and thalamic neurons (Fig. 4f, g). Intense intracellular immunostaining was localized in the cytoplasm. A small portion of neuroblast cell nuclei, however, did also show a faint staining.
Colon
As a positive control for the antiserum anti-hTFF3-2, human colon was stained. As expected, very intense immunostaining of goblet cells was observed (Fig. 4h).
Discussion
Although a wide distribution of TFF3 transcripts has been reported for the human brain, there is only limited evidence on protein level for the presence of TFF3 in brain regions outside the hypothalamus. Our immunohistochemical survey shows here for the first time that TFF3 immunoreactivity can be found in many regions of the adult and developing human brain. However, it is not known by now if TFF3 is secreted as a monomer, modified monomer, homodimer, or heterodimer (e.g., together with FCGBP).
A crucial point was the specificity of the anti-TFF3 antisera used because conflicting results may arise from using different commercial TFF3 antibodies. For example, some suppliers emphasize that their TFF3 antibodies do not stain nervous tissue at all (e.g., monoclonal ab 108599 from Abcam), whereas others recommend even human brain tissue as a good example for positive cellular TFF3 staining (e.g., polyclonal antiserum PAB 19439 from Abnova). To avoid such problems, we used three well-characterized specific TFF3 antisera (Probst et al. 1995; Wiede et al. 1999). Their specificity has been tested carefully including competitive inhibition with the corresponding synthetic peptides (e.g., Fig. 1f) and staining of colon sections as a positive control (Fig. 4h). Carrying out such immunoabsorption controls, we were able to completely depress specific immunostaining in neurons of almost all brain regions as well as in white matter oligodendrocytes and chororid plexus epithelial cells. In the cerebellum, however, a faint staining remained in Purkinje cells. Of note, a similar result was obtained in the rat indicating probably non-specific TFF3 staining of these cerebellar cells (Fu et al. 2014). Furthermore, notwithstanding the obtained depletion of specific immunostaining after preabsorption in certain non-neural cells (i.e., oligodendroglia and choroid plexus epithelia) we are skeptic with regard to a local synthesis of TFF3 in these cells, since there is yet no evidence for the presence of TFF3 mRNA. For example, the human choroid plexus has been previously reported to lack TFF3 transcripts (Probst et al. 1996). Thus, immunostaining might appear because of an uptake and/or binding of TFF3 by choroid plexus epithelial cells. Of note, TFF3 expression has been reported to occur also in aldynoglial cells of the rat olfactory bulb, i.e., CNS macroglia which seem to be related to Schwann cells (Rojas-Mayorquín et al. 2008). In addition, TFF3 immunoreactive material was detected in human median eminence tanycytes by others (Griepentrog et al. 1999). Thus, further studies are needed to learn more about TFF3 in non-neuronal cells of the brain.
No immunoreactivity was associated with astrocytes and microglia. The latter is in agreement with a recent report where TFF3 peptide was not detectable by the means of double immunohistochemistry in rat brain astrocytes both in vitro and in vivo (Fu et al. 2014). The lack of TFF3 in resting microglial cells observed here is also interesting with respect to a recent report that TFF3 is expressed in rat microglial cells in vitro (primary cultures), where these cells enter an activated state (Fu et al. 2014). Thus, TFF3 expression is expected to be induced only after activation of microglial cells, e.g., during inflammatory conditions such as stroke, multiple sclerosis, neurodegenerative diseases, and after cerebral infection.
Clearly, neurons were identified as the predominant (and perhaps only) cell type to contain TFF3 peptide in normal conditions. Predominant staining of neuronal cells is in line with the situation described in the human and porcine hypothalamo-pituitary axis (Probst et al. 1995, 1996; Jagla et al. 2000; Schwarz et al. 2001), the adult rodent cerebellum (Fu et al. 2014), as well as primary cultures of the rat hippocampus and cortex (Fu et al. 2014). Of note, the strongest intracellular immunostaining appeared in neurons belonging to various midbrain and brain stem nuclei, followed by a subset of hypothalamic neurons. This is in accordance with previous data on the local distribution of TFF3 transcripts in adult human brain (Allen Brain Atlas; http://human.brainmap.org/microarray/gene/show/6991?rw=t). Interestingly, the cerebellum, which stood out by intense immunostaining in our hands (Fig. 3a), and which is known to abundantly express TFF3 in rodents (Hinz et al. 2004; Fu et al. 2014), does only contain medium concentrations of TFF3 mRNA (according to Allen Brain Atlas data).
Based on the wide-spread expression of TFF3 in neurons of human brain, the question on possible consequences for our understanding of its function(s) in the brain is intriguing. Generally, there is accumulating evidence that TFF3 plays important roles in the development of the CNS, in its normal function in the adulthood, as well as during brain diseases. In particular, TFF3 expression in the cortex anlage at the 17th gestational week is interesting with respect to results from the mouse where TFF3 expression was drastically reduced in the cortex at about P2 (Hinz et al. 2004). Functionally, in rodents the administration of TFF3 has been reported to induce c-Fos expression in neurons of the hypothalamus, the basolateral amygdala, and the medial prefrontal cortex (Derbyshire and Ludwig 2004; Shi et al. 2012a, b), to modulate PI3 K/Akt signaling in the amygdala (Shi et al. 2012a), to exert neuroprotective effects in experimental cerebral ischemia/reperfusion injury (Liu et al. 2013), to facilitate learning, object recognition and retention of memory (Schwarzberg et al. 1999; Shi et al. 2012a, b), to evoke anti-depressant-like activities (Shi et al. 2012a), to have pronounced anxiolytic effects at low doses but anxiogenic effects at a high doses (Schwarzberg et al. 1999), and to attenuate naloxone-precipitated withdrawal in morphine-dependent mice (Wu et al. 2014). However, all these activities have to be considered as merely pharmacologic effects of TFF3 as long as there is no evidence for the natural occurrence of the peptide in these brain regions. A local TFF3 peptide synthesis (as shown here) would thus increase the chance to interpret these effects as physiologically meaningful. Furthermore, there are indications for an involvement of TFF3 in various brain diseases ranging from alcohol dependence to Alzheimer disease. While a putative role of TFF3 in some of these disorders was proposed because of the presence of disease-related TFF3 gene polymorphisms or altered TFF3 expression in peripheral tissues (i.e., schizophrenia; Chissoe St et al. 2008; Gardiner et al. 2013), other disorders have been studied with regard to TFF3 expression changes in the brain. For example, altered TFF3 expression has been reported for the rat neocortex during abstinence following alcohol intoxication (Hashimoto et al. 2011). Recently, TFF3 was identified as a reliable cerebrospinal fluid biomarker associated with neurodegeneration in amyloid-positive individuals with Alzheimer pathology (Paterson et al. 2014), although TFF3 mRNA levels do not significantly differ between Alzheimer disease patients and control cases (according to two independent data sets published by GeneNetwork,http://www.genenetwork.org/webqtl/WebQTL.py?cmd=search&gene=Tff3).
Taken together, neurons (and probably also activated microglial cells; Fu et al. 2014) should be regarded as the major cellular sources for local TFF3 synthesis in the brain. Thus, the detection of a wide cerebral distribution not only of TFF3 transcripts, but also of TFF3 peptide, should help explain its multiple effects on the CNS.
References
Albert TK, Laubinger W, Müller S, Hanisch FG, Kalinski T, Meyer F, Hoffmann W (2010) Human intestinal TFF3 forms disulfide-linked heteromers with the mucus-associated FCGBP protein and is released by hydrogen sulfide. J Proteome Res 9:3108–3117
Bernstein HG, Schön E, Ansorge S, Röse I, Dorn A (1987) Immunolocalization of dipeptidyl aminopeptidase (DAP IV) in the developing human brain. Int J Dev Neurosci 5:237–242
Bernstein HG, Baumann B, Danos P, Diekmann S, Bogerts B, Gundelfinger ED, Braunewell KH (1999) Regional and cellular distribution of neural visinin-like protein immunoreactivities (VILIP-1 and VILIP-3) in human brain. J Neurocytol 28:655–662
Cadet JL, Jayanthi S, McCoy MT, Beauvais G, Cai NS (2010) Dopamine D1 receptors, regulation of gene expression in the brain, and neurodegeneration. CNS Neurol Disord Drug Targ 9:526–528
Chissoe St, Ehm MG, Jean P St (2008) Genes associated with schizophrenia, US Patent Application Publication US 2008/0176239 A1, pp 1–49
Cui D, Dougherty KJ, Machacek DW, Sawchuk M, Hochman S, Baro DJ (2006) Divergence between motoneurons: gene expression profiling provides a molecular characterization of functionally discrete somatic and autonomic motoneurons. Physiol Genomics 24:276–289
Derbyshire A, Ludwig M (2004) TFF3 induced Fos protein expression in the magnocellular oxytocin neurons of the hypothalamus. Peptides 25:833–838
Fu T, Stellmacher A, Znalesniak EB, Dieterich DC, Kalbacher H, Hoffmann W (2014) Tff3 is expressed in neurons and microglial cells. Cell Physiol Biochem 34:1912–1919
Gardiner EJ, Cairns MJ, Liu B, Beveridge NJ, Carr V, Kelly B, Scott RJ, Tooney PA (2013) Gene expression analysis reveals schizophrenia-associated dysregulation of immune pathways in peripheral blood mononuclear cells. J Psychiatr Res 47:425–437
Griepentrog T, Bauer M, Hornstein C, Sauer H, Jirikowski GF (1999) Tanycytes in the human median eminence contain intestinal trefoil factor (hITF). Eur J Anat 3:111–114
Griepentrog T, Bauer M, Hornstein C, Sauer H, Jirikowski GF (2000) Coexistence of intestinal trefoil factor (hITF) and oxytocin in magnocellular neurons in the human hypothalamus. Horm Metab Res 32:121–124
Hashimoto JG, Forquer MR, Tanchuck MA, Finn DA, Wiren KM (2011) Importance of genetic background for risk of relapse shown in altered prefrontal cortex gene expression during abstinence following chronic alcohol intoxication. Neuroscience 173:57–75
Hauser F, Poulsom R, Chinery R, Rogers LA, Hanby AW, Wright NA, Hoffmann W (1993) hP1.B, a human P-domain peptide homologous with rat intestinal trefoil factor, is expressed also in the ulcer-associated cell lineage and the uterus. Proc Natl Acad Sci USA 90:6961–6965
Hinz M, Schwegler H, Chwieralski CE, Laube G, Linke R, Pohle W, Hoffmann W (2004) Trefoil factor family (TFF) expression in the mouse brain and pituitary: changes in the developing cerebellum. Peptides 25:827–832
Hoffmann W (2013) TFF peptides. In: Kastin AJ (ed) Handbook of biologically active peptides, 2nd edn. Elsevier, San Diego, pp 1338–1345
Hoffmann W, Jagla W (2002) Cell type specific expression of secretory TFF peptides: colocalization with mucins and synthesis in the brain. Int Rev Cytol 213:147–181
Hoffmann W, Jagla W, Wiede A (2001) Molecular medicine of TFF-peptides: from gut to brain. Histol Histopathol 16:319–334
Jagla W, Wiede A, Hinz M, Dietzmann K, Gülicher D, Gerlach KL, Hoffmann W (1999) Secretion of TFF-peptides by human salivary glands. Cell Tissue Res 298:161–166
Jagla W, Wiede A, Dietzmann K, Rutkowski K, Hoffmann W (2000) Co-localization of TFF3 peptide and oxytocin in the human hypothalamus. FASEB J 14:1126–1131
Kjellev S (2009) The trefoil factor family—small peptides with multiple functionalities. Cell Mol Life Sci 66:1350–1369
Kouznetsova I, Peitz U, Vieth M, Meyer F, Vestergaard EM, Malfertheiner P, Roessner A, Lippert H, Hoffmann W (2004) A gradient of TFF3 (trefoil factor family 3) peptide synthesis within the normal human gastric mucosa. Cell Tissue Res 316:155–165
Kriks S, Shim JW, Piao J, Ganat YM, Wakeman DR, Xie Z, Carrillo-Reid L, Auyeung G, Antonacci C, Buch A, Yang L, Beal MF, Surmeier DJ, Kordower JH, Tabar V, Studer L (2011) Dopamine neurons derived from human ES cells efficiently engraft in animal models of Parkinson’s disease. Nature 480:547–551
Liu SQ, Roberts D, Zhang B, Ren Y, Zhang LQ, Wu YH (2013) Trefoil factor 3 as an endocrine neuroprotective factor from the liver in experimental cerebral ischemia/reperfusion injury. PLoS One 8:e77732
May FE, Westley BR (1997) Trefoil proteins: their role in normal and malignant cells. J Pathol 183:4–7
O´Rahilly R, Müller F (2005) The embryonic human brain: an atlas of developmental stages, 3rd edn. Wiley, New York
Paterson RW, Bartlett JW, Blennow K, Fox NC, Shaw LM, Trojanowski JQ, Zetterberg H, Schott JM (2014) Cerebrospinal fluid markers including trefoil factor 3 are associated with neurodegeneration in amyloid-positive individuals. Transl Psychiatry 4:e419
Paulsen FP, Hinz M, Schaudig U, Thale AB, Hoffmann W (2002) TFF peptides in the human efferent tear ducts. Invest Ophthalmol Vis Sci 43:3359–3364
Pereira PL, Magnol L, Sahún I, Brault V, Duchon A, Prandini P, Gruart A, Bizot JC, Chadefaux-Vekemans B, Deutsch S, Trovero F, Delgado-García JM, Antonarakis SE, Dierssen M, Herault Y (2009) A new mouse model for the trisomy of the Abcg1-U2af1 region reveals the complexity of the combinatorial genetic code of Down syndrome. Hum Mol Genet 18:4756–4769
Probst JC, Skutella T, Müller-Schmid A, Jirikowski GF, Hoffmann W (1995) Molecular and cellular analysis of rP1.B in the rat hypothalamus: in situ hybridization and immunohistochemistry of a new P-domain neuropeptide. Brain Res Mol Brain Res 33:269–276
Probst JC, Zetzsche T, Weber M, Theilemann P, Skutella T, Landgraf R, Jirikowski GF (1996) Human intestinal trefoil factor is expressed in human hypothalamus and pituitary: evidence for a novel neuropeptide. FASEB J 10:1518–1523
Reeves EP, Ali T, Leonard P, Hearty S, O’Kennedy R, May FE, Westley BR, Josenhans C, Rust M, Suerbaum S, Smith A, Drumm B, Clyne M (2008) Helicibacter pylori lipopolysaccharide interacts with TFF1 in a pH-dependent manner. Gastroenterology 135:2043–2054
Reymond A, Marigo V, Yaylaoglu MB, Leoni A, Ucla C, Scamuffa N, Caccioppoli C, Dermitzakis ET, Lyle R, Banfi S, Eichele G, Antonarakis SE, Ballabio A (2002) Human chromosome 21 gene expression atlas in the mouse. Nature 420:582–586
Rinnert M, Hinz M, Buhtz P, Reiher F, Lessel W, Hoffmann W (2010) Synthesis and localization of trefoil factor family (TFF) peptides in the human urinary tract and TFF2 excretion into the urine. Cell Tissue Res 339:639–647
Rojas-Mayorquín AE, Torres-Ruíz NM, Ortuño-Sahagún D, Gudiño-Cabrera G (2008) Microarray analysis of striatal embryonic stem cells induced to differentiate by ensheathing cell conditioned media. Dev Dyn 237:979–994
Samson MH (2013) Quantitative measurements of trefoil factor family peptides: possibilities and pitfalls. Scand J Clin Lab Invest 73:193–202
Samson MH, Chaiyarit P, Nortvig H, Vestergaard EM, Ernst E, Nexo E (2011) Trefoil factor family peptides in human saliva and cyclical cervical mucus. Method evaluation and results on healthy individuals. Clin Chem Lab Med 49:861–868
Schwarz H, Jagla W, Wiede A, Hoffmann W (2001) Ultrastructural co-localization of TFF3-peptide and oxytocin in the neural lobe of the porcine pituitary. Cell Tissue Res 305:411–416
Schwarzberg H, Kalbacher H, Hoffmann W (1999) Differential behavioral effects of TFF peptides: injections of synthetic TFF3 into the rat amygdala. Pharmacol Biochem Behav 62:173–178
Shi HS, Zhu WL, Liu JF, Luo YX, Si JJ, Wang SJ, Xue YX, Ding ZB, Shi J, Lu L (2012a) PI3 K/Akt signaling pathway in the basolateral amygdala mediates the rapid antidepressant-like effects of trefoil factor 3. Neuropsychopharmacology 37:2671–2683
Shi HS, Yin X, Song L, Guo QJ, Luo XH (2012b) Neuropeptide Trefoil factor 3 improves learning and retention of novel object recognition memory in mice. Behav Brain Res 227:265–269
Vestergaard EM, Nexo E, Wendt A, Guthmann F (2008) Trefoil factors in human milk. Early Hum Dev 84:631–635
Wiede A, Jagla W, Welte T, Köhnlein T, Busk H, Hoffmann W (1999) Localization of TFF3, a new mucus-associated peptide of the human respiratory tract. Am J Respir Crit Care Med 159:1330–1335
Wu P, Shi HS, Luo YX, Zhang RX, Li JL, Shi J, Lu L, Zhu WL (2014) Neuropeptide trefoil factor 3 attenuates naloxone-precipitated withdrawal in morphine-dependent mice. Psychopharmacol 2014. (Epub ahead of print)
Acknowledgments
The authors wish to thank B. Jerzykiewicz for skilled technical assistance.
Conflict of interest
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Handling Editor: M. S. Palma.
Rights and permissions
About this article
Cite this article
Bernstein, HG., Dobrowolny, H., Trübner, K. et al. Differential regional and cellular distribution of TFF3 peptide in the human brain. Amino Acids 47, 1053–1063 (2015). https://doi.org/10.1007/s00726-015-1938-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00726-015-1938-9