Abstract
The aim of our study is to examine the plasma levels of the four kinds of neurodegenerative proteins in plasma: α-syn, T-tau, P-tau181, and Aβ-42 in Parkinson’s disease (PD) and to evaluate the relationship between their plasma levels and PD motor subtypes. 84 patients with PD were enrolled in our study, and finally, 73 of them were classified into the tremor-dominant subtype (TD) and the postural instability gait difficulty subtype (PIGD). Their motor performance was evaluated by a series of clinical assessments: Freezing of Gait Questionnaire (FOGQ), Timed Up and Go (TUGs), Tinetti balance, and Tinetti gait. Plasma levels of these proteins were measured by enzyme-linked immunosorbent assay (ELISA). The plasma level of α-syn was significantly higher in PD patients when compared to controls (p = 0.004), and significantly higher in the PIGD group when compared to the TD group (p = 0.03). While the plasma level of Aβ-42 was significantly lower in PD patients than in controls (p = 0.002), and significantly lower in the PIGD group than in the TD group (p = 0.05). In PD patients, the plasma level of α-syn (r = −0.355, p < 0.001) was significantly related to the severity of Tenitti Gait score, even after performing multiple linear regression (p = 0.002). While the plasma level of Aβ-42 (r = −0.261, p < 0.05) was significantly associated with the severity of PIGD score and remained correlate when performed multiple linear regression (p = 0.005). The patients with PIGD subtype are characterized with a lower level of plasma Aβ-42 and a higher plasma level of α-syn, which may be used as biomarkers for diagnosis and progression of the subtypes of PD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
It is well known that Parkinson’s disease (PD) should be considered as a neurological movement disorder with variable clinical phenotypes. According to the clinical symptoms, patients with PD can be classified into three subtypes: the tremor-dominant (TD) subtype, the postural instability gait difficulty (PIGD) subtype, and the mixed subtype (Jankovic et al. 1990). Compared to the TD subtype, patients with PIGD have more severe motor disorders, such as freezing of gait (FOG), falling, and postural instability, as well as a higher risk of cognitive dysfunction. Moreover, the PIGD subtype patients have less response to dopamine replacement therapy (Auyeung et al. 2012; Bohnen and Cham 2006).
The diagnosis of PD subtype is critically dependent on clinical examination. However, a readily accessible biomarker for diagnosis of the motor subtypes of PD remains to be discovered. Previous studies have made preliminary attempts. For example, Iacono et al. reported that the cerebrospinal fluid (CSF) level of 5-HT in the PIGD group was lower than in the TD group (Iacono et al. 1997). Yu et al. found that the glutamic acid (GLU) and γ-aminobutyric acid (GABA) were associated with the clinical heterogeneity (Yu et al. 2012). Among all these biomarker candidates, the neurodegenerative proteins, such as α-syn, T-tau, P-tau181, and Aβ-42, were sought to be accessible biomarkers for the diagnosis of PD subtypes (Ohrfelt et al. 2009; Jellinger 2012). In a clinical study, increased plasma level was found in PD patients with FOG as compared to controls (Wang et al. 2014). The levels of T-tau and the ratio of levels of T-tau and Aβ-42 in CSF were lower significantly in the TD group (Kang et al. 2013).
However, only a few of studies have shown that neurodegenerative proteins may related to the TD subtype, and whether there is a relationship between the plasma levels of neurodegenerative proteins and PIGD subtype is still unclear. Hence, in our study, we measured the plasma levels of four kinds of neurodegenerative proteins (α-syn, T-tau, P-tau181, and Aβ-42) in PD patients with different motor subtypes and tried to find the potential biomarkers for diagnosis of the motor subtypes of PD.
Methods
Patients
A total of 84 patients who met the diagnosis of idiopathic PD according to the UK Parkinson’s disease Brain Bank criteria were involved in our study consecutively (Hughes et al. 1992). Patients with other movement disorders, such as Parkinsonian plus syndromes, neurological disease, a history of family PD, and other signs of blood disease, were excluded from our study. Our patients were in “off” state, and the clinical assessments and blood samples were carried out after more than 12 h withdrawal of anti-parkinsonian medications. The Unified Parkinson’s disease Rating Scale (UPDRS) scores were used to evaluate the severity of patients and help us define the clinical subtype of PD (Fahn et al. 1987). Meanwhile, 26 age-matched volunteers took participate in our study. The exclusion criteria were neurological disease, dementia, history of family PD, and other sign of blood disease. All participants were included only if their scores of Mini-Mental State Examination (MMSE) ≥24 (Folstein et al. 1975). This study was approved by the ethics committee of the First Affiliated Hospital of Nanjing Medical University. Informed written consent was obtained from all volunteers.
Classification into PIGD and TD subtypes
The all 84 patients were divided into the postural instability gait difficulty dominant (PIGD) group or the tremor-dominant (TD) group according to the ratio of mean tremor score/mean PIGD score. The mean tremor score was the sum of UPDRS item 16, 20, 21 divided by 9, whereas the mean PIGD score was the sum of UPDRS item 13, 14, 15, 29, 30 divided by 5. Accurately, 37 patients with the ratio ≤1 were placed in PIGD group, whereas 36 patients with the ratio ≥1.5 were placed in the TD group (Jankovic et al. 1990). Finally, there were 73 patients included in our study, and another 11 patients were excluded for their scores in-between.
Clinical assessments
The severity of disease was evaluated using the Hoehn and Yahr staging scale (H&Y) and UPDRS (Hoehn and Yahr 1967). The motor performances of balance and gait were evaluated with Freezing of Gait Questionnaire (FOGQ) (Hanakawa et al. 1999), Tinetti balance and Tinetti Gait (Kegelmeyer et al. 2007), as well as Timed Up and Go (TUGs) (Shumway-Cook et al. 2000). The levodopa equivalent daily dose (LEDD) was calculated based on established methods (Tomlinson et al. 2010).
Plasma sample collection and biological assays
5 ml of blood was obtained from all our volunteers in the morning after an overnight fast and then collected into these tubes containing EDTA, which was recommended by manufacturer. The plasma was separated immediately within 2 h by a designated person. We centrifuged the plasma at 3000 rpm for 15 min at 4 °C according to the recommendation by manufacturer and previous reports. Plasma was then stored at −80 °C until analysis. Plasma α-syn, T-tau, P-tau181, and Aβ-42 concentrations were detected using commercially available enzyme-linked immunosorbent assay (ELISA) according to the manufacturer’s protocol (SBJ-H1552, SBJ-H2051, SBJ-H2050, and SBJ-H0250; Senbeijia, Nanjing, China).
Statistical analysis
Shapiro–Wilk test was used to exam the normality of distribution of our data (p > 0.05). Comparisons between patients and controls were made using T test, Manu–Whitney U test, or Kruskal–Wallis H test for continuous variables, and Chi-squared test for categorical data. Least significant difference (LSD) method or Nemenyi test was adopted for post hoc multiple comparisons. The correlation between plasma levels of neurodegenerative proteins and clinical variables was examined with Spearman’s rank-correlation analysis. Multiple linear regression analysis was also performed to further examine the impact of neurodegenetative proteins on the motor symptoms. A p value less than 0.05 was statistically significant. All analyses were performed using the SPSS software (19.0, SPSS InC., Chicago, IL, USA).
Results
Demographic and clinical characteristics of PD patients and controls
Demographic and clinical characteristics of PD patients and controls are summarized in Table 1. A total of 73 PD patients and 26 age-matched healthy controls were recruited in our study. There were no significant differences between PD patients and controls in age (67.60 ± 8.70 vs. 64.77 ± 4.16, p = 0.085) and MMSE score (28.15 ± 4.38 vs. 27.95 ± 2.24, p = 0.101). No significant differences were found in gender, disease duration, MMSE score, UPDRS I score, and UPDRS III score between two motor subtype groups. However, those items of age (71.58 ± 7.02 vs. 63.73 ± 8.49, p < 0.001), LEDD (473.43 ± 297.58 vs. 279.39 ± 227.66, p = 0.008), and H–Y stage (2.18 ± 0.43 vs. 1.76 ± 0.65, p = 0.002) were significantly higher in the PIGD group when compared to the TD group. As expected, gait and balance impairments were more severe in the PIGD group compared with the TD group, as assessed by the Tinetti Gait (p < 0.001), the TUG test (p < 0.001), the FOGQ test (p < 0.001), and the Tinetti Balance (p < 0.001).
Plasma levels of neurodegenerative proteins in PD patients and controls
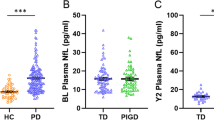
As shown in Table 2, PD patients had a lower plasma level of Aβ-42 (266.73 ± 78.50 vs. 320.39 ± 62.72, p = 0.002) and a higher plasma level of α-syn (319.56 ± 64.22 vs. 274.31 ± 70.71, p = 0.004) than controls. However, there were no significant differences in the plasma levels of T-tau and P-tau181 between PD patients and controls. In the different motor subgroups, as summarized in Table 3, the PIGD group had a significantly higher level of α-syn than the TD group (340.60 ± 56.00 vs. 299.09 ± 65.79, p < 0.05). Moreover, the PIGD group also showed a slightly lower plasma level of Aβ-42 when compared to the TD group at a marginal significance (242.81 ± 73.45 vs. 290.02 ± 77.14, p = 0.05).
Correlations between plasma levels of neurodegenerative proteins and clinical manifestations of PD patients
As summarized in Table 4, the plasma level of α-syn was negatively correlated with the Tinetti Gait score (r = −0.355, p = 0.002, Fig. 1), a scale with less score meaning more severe symptoms and positively correlated with the FOGQ test score (r = 0.234, p = 0.046), a scale with more score meaning more severe symptoms. The plasma level of Aβ-42 was negatively correlated with the PIGD score (r = −0.261, p = 0.026, Fig. 2), and the FOGQ test score (r = −0.256, p = 0.029) and positively associated with the tremor score (r = 0.239, p = 0.042).
Multiple linear regression analysis
Multiple linear regressions were carried out with PIGD score (Table 5) and Tinetti Gait score (Table 6) as dependent variables in each respective model. Factors of age, disease duration, LEDD, UPDRS I score, UPDRS II score, UPDRS III score, and H–Y stage, as well as plasma levels of α-syn, T-tau, P-tau181, and Aβ-42, were included. The regression model of PIGD score was significant (p < 0.001) and accounted for 68.1% of variance. The plasma level of Aβ-42 (β = −0.202, p = 0.005), UPDRS II score (β = 0.801, p = 0.000), UPDRS I score (β = −0.253, p = 0.004), as well as age (β = −0.223, p = 0.003) was found to be significantly related to PIGD score. Moreover, the regression model of Tinetti Gait score was also significant (p < 0.001) and accounted for 46.3% of variance. The plasma level of α-syn (β = −0.284, p = 0.002), UPDRS II score (β = −0.259, p = 0.045), UPDRS III score (β = −0.268, p = 0.032), as well as age (β = −0.244, p = 0.011) was found to be significantly related to Tinetti Gait score.
Although the plasma levels of α-syn and Aβ-42 were related to the FOGQ score, as previously noted, the multiple regression analysis with the FOGQ score as the dependent variable was failed to perform for its non-normality even after data transformation.
Discussion
In the past few decades, great progress has been made in the pathophysiology and clinical features of PD. Emerging evidence from biochemical and postmortem studies shows that neurodegenerative proteins, such as α-syn, T-tau, P-tau181, and Aβ-42, may contribute to the pathogenesis of PD. Previous studies have found that α-syn, T-tau, and Aβ-42 in the CSF, as biomarkers, were involved in motor symptoms of PD (Kang et al. 2013). However, few systematic works have been made to reveal the relationship between all these neurodegenerative proteins and motor subtype properties of PD, especially in their plasma levels. Accumulating evidence has shown that the plasma levels of neurodegenerative proteins might partially reflect their activity in the brain (Lee et al. 2006; Molina et al. 1997; Lehallier et al. 2015). Based on these data, we sought to measure the plasma levels of α-syn, T-tau, P-tau181, and Aβ-42 in PD patients and investigate their association with clinical features.
Our findings indicated that, first, the plasma levels of α-syn and Aβ-42 in the PD patients were significantly different from those in HCs. Second, the plasma levels of α-syn and Aβ-42 in the PIGD group were significantly different from those in the TD group. Third, the plasma level of α-syn was significantly related to the score of Tinetti gait. Forth, the plasma level of Aβ-42 was significantly associated with the score of PIGD.
Lewy bodies (LBs) and Lewy neurites (LNs)—major composed of α-syn—were sought to be the defining feature of idiopathic PD (Spillantini 1997). The studies contain conflicting results as to whether the plasma levels of α-syn differ between PD patients and controls. We observed that the plasma level of α-syn in PD patients was significantly higher than controls with the method of ELISA. In agreement with us, Duran et al. and Lee et al. also reported increased plasma level of α-syn in PD patients with the method of ELISA (Duran et al. 2010; Lee et al. 2006). While Park et al. suggested that there was no difference between PD patients and controls in the plasma level of α-syn (Park et al. 2011). The inconsistency may result from the different in sample size. The sample size of Park et al. was 52 (PD 23, control 29). However, in Duran’s, Lee’s, and our studies, the size was 155 (PD 95, controls 60), 194 (PD 105, controls 51, MAS 38), and 99 (PD 73, controls 26). There was a larger sample size in the latter studies as compared to Park’s, and perhaps a larger sample size may lead to a stronger statistical power. Difference in measurement may also result in inconsistency. For example, Li et al. found decreased level of α-syn in PD patients with the method of western blot (Li et al. 2007). Compared to western blot, ELISA was easier to operate and quantify. Another important factor of the inconsistency is residual red blood cells (RBC) or hemolysis during collecting samples, as RBC is thought to be a major source of α-syn. In our study, we arranged a designated person to collect plasma samples. The plasma was separated within 2 h to avoid hemolysis. Appropriate care was also taken to avoid the contamination from pellet during centrifugation. Some studies tried to detect specific structure or antibody of α-syn to avoid this problem. For example, Foulds et al. suggested that the plasma level of phosphorylated α-syn was higher in PD patients than controls (Foulds et al. 2011). Besong-Agbo and his colleague demonstrated that naturally occurring auto-antibody levels were lower in PD patients (Besong-Agbo et al. 2013). The literature in this field is limited, and further validation is critically needed.
Importantly, our study found that the plasma level of α-syn was much higher in the PIGD group than in the TD group, implying that α-syn might be even more associated with the PIGD group in PD patients. Kang et al. reported that the CSF level of α-syn was lower in the PIGD group than in the TD group when the hemoglobin (HGB) in CSF < 200 ng/ml, in line with us (Kang et al. 2013). Although the pathophysiological mechanisms of PIGD are complex and remained to be further explored, accumulating evidence supports the idea that aggregation of α-syn might be involved in the progression of PIGD much more. It is well known that the PIGD group has more severe motor disorders and a faster disease progression. One hypothesis is that α-syn is a possible biomarker for progression, particularly in the motor symptoms. Majbour and his colleague noted a correlation between the oligomeric α-syn/total α-syn ratio in the CSF level and a worsening of motor signs, especially in the PIGD group (Majbour et al. 2016). A functional MRI study also reported that CSF level of α-syn was related to sensorimotor functional connectivity in PD (Campbell et al. 2015). When it came to genetic research, Ritz et al. demonstrated that the variants of SNCA were powerful predictors of faster motor decline in idiopathic PD (Ritz et al. 2012). Taken together, all these data suggest that α-syn contributes to a faster progression of motor disorders in PD. Further studies are needed to investigate the clear mechanism.
It is noteworthy that our study observed the relationship between the plasma level of α-syn and the score of Tenitti Gait, a scale which evaluates the severity of gait in PD patients. However, previous studies have shown that other clinical characteristics, such as age, disease duration, etc., may be related to the plasma level of α-syn in PD (Parkkinen et al. 2001). To exclude the influence of these factors, multiple linear regression was used to examine the association between the plasma level of α-syn and symptoms of PIGD and the result showed that a increased level of α-syn might still contribute to the severity of PIGD. An animal study from Gruden showed that rigidity and locomotor activity resulted from the accumulating of α-syn plus fibrils in the mice brain (Gruden et al. 2013). A clinical study demonstrated that plasma α-syn could discriminate freezing of gait (FOG) from controls, although no significant difference between the PD with FOG group and PD without FOG group (Wang et al. 2014). Hence, we can postulate that the accumulating of α-syn may contribute to the occurrence of gait disturbance in PD patients.
It is also worth noting that the plasma level of Aβ-42 in patients with PD was significantly lower than in HCs. It is strongly supposed that decreased Aβ-42 concentration in the brain of PD patients could be reflected by its Aβ-42 level in plasma. Although Aβ-42 is a biomarker of Alzheimer’s disease, it is also closely related to PD. Previous studies have suggested decreased concentration of Aβ-42 in CSF of PD patients (Kang et al. 2013). Leverence et al. demonstrated the strong role of Aβ-42 in cognitive processing in PD (Lehallier et al. 2015). In agreement with our findings, a study from Kang et al. has shown that the Aβ-42 level in CSF was associated with PIGD group in his multivariate logistic regression (MLGR) model (Kang et al. 2013). A clinical study also reported that lower CSF level of Aβ-42 was found in the PIGD phenotype even in the newly diagnosed and untreated PD patients when compared to the TD phenotype (Alves et al. 2013).
We also measured the two other neurodegenerative proteins—including T-tau and P-tau181—in the level of plasma. We observed that the plasma level of T-tau and P-tau181 was lower in PD patients than in controls, although the difference was not statistically significant. When compared between the two patient groups, there was also a decreased tend of the plasma level of T-tau and P-tau181 in the PIGD group. Tau was thought to play an important role in the pathology of PD through a lot of mechanisms, including mitochondrial dysfunction, unbalanced basal ganglia circuit and excitotoxicity (Menzie et al. 2014). We field to find the plasma level of tau and p-tau in PD patients. The literature contains conflicting reports about whether T-tau in CSF level differs between controls and PD patients. A study from Karin reported unchanged T-tau and p-tau levels in CSF in PD patients and controls, which was in line with our result (Karin et al. 2013). While Kang et al. found that the CSF levels of T-tau and p-tau were significantly lower in PD patients than in controls (Kang et al. 2013). The inconsistency may result from the difference in sample size and measurement.
Some limitations should be noted in our study. First, we only performed a peripheral association of α-syn by measuring them in plasma level. It was discovered that plasma exosomal α-syn, which was transported from CSF α-syn readily, might be the most promising candidate for the diagnosed of PD (Atik et al. 2016). Second, the size of samples in our study was relatively small for correlation analysis. Third, the focus of our study was only restricted to two subtypes of PD, and the other subtypes were not brought into. Forth, other forms of α-syn, such as oligomeric and phosphoryed forms, were not measured in our study. Fifth, we did not measure the plasma level of hemoglobin in our study. It is more rigorous to evaluate the situation of hemolysis in the study. Therefore, a large sample study for all subtypes of PD and more kinds of measurements should be taken for further investigation.
In conclusion, the results from our study showed that a lower level of Aβ-42 and a higher level of α-syn were found in plasma in PD patients when compared to controls. Moreover, compared to the TD group, a lower level of Aβ-42 and a higher level of α-syn were found in the PIGD group. The plasma level of α-syn was related to the severity of gait, while the plasma level of Aβ-42 was associated with the score of PIGD. A lower level of plasma Aβ-42 and a higher level of plasma α-syn may be as biomarkers indicating the severity of posture and gait disorders of PD, although further study is needed to validate our results.
References
Alves G, Pedersen KF, Bloem BR et al (2013) Cerebrospinal fluid amyloid-beta and phenotypic heterogeneity in de novo Parkinson’s disease. J Neurol Neurosurg Psychiatry 84(5):537–543
Atik A, Stewart T, Zhang J (2016) Alpha-Synuclein as a Biomarker for Parkinson’s Disease. Brain Pathol 26(3):410–418
Auyeung M, Tsoi TH, Mok V et al (2012) Ten year survival and outcomes in a prospective cohort of new onset Chinese Parkinson’s disease patients. J Neurol Neurosurg Psychiatry 83(6):607–611
Besong-Agbo D, Elias W, Frank J et al (2013) Naturally occurring a-synuclein autoantibody levels are lower in patients with Parkinson disease. Neurology 80:169–175
Bohnen NI, Cham R (2006) Postural control, gait, and dopamine functions in parkinsonian movement disorders. Clin Geriatr Med 22(4):797–812 (vi)
Campbell MC, Koller JM, Snyder AZ et al (2015) CSF proteins and resting-state functional connectivity in Parkinson disease. Neurology 84:2413–2421
Duran R, Francisco JB, Blas M et al (2010) Plasma a-synuclein in patients with Parkinson’s disease with and without treatment. Mov Disord 25:489–493
Fahn S, Elton RL, Committee UD (1987) Unified Parkinson’s disease rating scale. Recent Dev Parkinson's Dis 2:153–163
Folstein MF, Folstein SE, McHugh PR (1975) “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12(3):189–198
Foulds PG, Mitchell D, Parker A et al (2011) Phosphorylated -synuclein can be detected in blood plasma and is potentially a useful biomarker for Parkinson’s disease. FASEB J 25:4127–4137
Gruden MA, Davidova TV, Yanamandra K et al (2013) Nasal inoculation with alpha-synuclein aggregates evokes rigidity, locomotor deficits and immunity to such misfolded species as well as dopamine. Behav Brain Res 243:205–212
Hanakawa T, Katsumi Y, Fukuyama H et al (1999) Mechanisms underlying gait disturbance in Parkinson’s disease: a single photon emission computed tomography study. Brain 122(Pt 7):1271–1282
Hoehn MM, Yahr MD (1967) Parkinsonism: onset, progression and mortality. Neurology 17(5):427–442
Hughes AJ, Daniel SE, Kilford L, Lees AJ (1992) Accuracy of clinical diagnosis of idiopathic Parkinson’s disease: a clinico-pathological study of 100 cases. J Neurol Neurosurg Psychiatry 55(3):181–184
Iacono RP, Kuniyoshi SM, Ahlman JR, Zimmerman GJ, Maeda G, Pearlstein RD et al (1997) Concentrations of indoleamine metabolic intermediates in the ventricular cerebrospinal fluid of advanced Parkinson’s patients with severe postural instability and gait disorders. J Neural Transm (Vienna) 104(4–5):451–459
Jankovic J, McDermott M, Carter J et al (1990) Variable expression of Parkinson’s disease: a base-line analysis of the DATATOP cohort. The Parkinson Study Group. Neurology 40(10):1529–1534
Jellinger KA (2012) CSF biomarkers in different phenotypes of Parkinson disease. J Neural Transm (Vienna) 119(4):455–456
Kang JH, Irwin DJ, Chen-Plotkin AS et al (2013) Association of cerebrospinal fluid beta-amyloid 1–42, T-tau, P-tau181, and alpha-synuclein levels with clinical features of drug-naive patients with early Parkinson disease. JAMA Neurol 70(10):1277–1287
Karin DD, Wesley J, Johennes AH et al (2013) Cerebrospinal fliud and plasma clusterin levels in Parkinson’s disease. Parkinsonism Relat Disord 19(12):1079–1083
Kegelmeyer DA, Kloos AD, Thomas KM et al (2007) Reliability and validity of the Tinetti Mobility Test for individuals with Parkinson disease. Phys Ther 87(10):1369–1378
Lee PH, Lee G, Park HJ et al (2006) The plasma alpha-synuclein levels in patients with Parkinson’s disease and multiple system atrophy. J Neural Transm (Vienna) 113(10):1435–1439
Lehallier B, Essioux L, Gayan J et al (2015) Combined plasma and cerebrospinal fluid signature for the prediction of midterm progression from mild cognitive impairment to Alzheimer disease. JAMA Neurol 2015:1–10
Li QX, Mok SS, Laughton KM et al (2007) Plasma α-synuclein is decreased in subjects with Parkinson’s disease. Exp Neurol 204:583–588
Majbour NK, Vaikath NN, Eusebi P et al (2016) Longitudinal changes in CSF alpha-synuclein species reflect Parkinson’s disease progression. Mov Disord 31(10):1535–1542
Menzie J, Pan C, Prentice H et al (2014) Taurine and central nervous system disorders. Amino Acids 46(1):31–46
Molina JA, Jiménez-Jiménez FJ, Gomez P et al (1997) Decreased cerebrospinal fluid levels of neutral and basic amino acids in patients with Parkinson's disease. J Neurol Sci 150(2):123–127
Ohrfelt A, Grognet P, Andreasen N et al (2009) Cerebrospinal fluid alpha-synuclein in neurodegenerative disorders-a marker of synapse loss? Neurosci Lett 450(3):332–335
Park MJ, Cheon SM, Bae HR et al (2011) Elevated levels of α-synuclein oligomer in the cerebrospinal fluid of drug-naïve patients with Parkinson’s disease. J Clin Neurol 7:215–222
Parkkinen L, Soininen H, Laakso M et al (2001) Alpha-synuclein pathology is highly dependent on the case selection. Neuropathol Appl Neurobiol 27(4):314–325
Ritz B, Rhodes SL, Bordelon Y et al (2012) a-synuclein genetic variants predict faster motor. Symptom progression in idiopathic Parkinson disease. PLoS One 7:e36199
Shumway-Cook A, Brauer S, Woollacott M (2000) Predicting the probability for falls in community-dwelling older adults using the Timed Up & Go Test. Phys Ther 80(9):896–903
Spillantini MG (1997) a-Synuclein in Lewy bodies. Nature 399:839–840
Tomlinson CL, Stowe R, Patel S et al (2010) Systematic review of levodopa dose equivalency reporting in Parkinson’s disease. Mov Disord 25(15):2649–2653
Wang XY, Kang WY, Yang Q et al (2014) Using gastrocnemius sEMG and plasma alpha-synuclein for the prediction of freezing of gait in Parkinson’s disease patients. PLoS One 9(2):e89353
Yu X, He GR, Sun L et al (2012) Assessment of the treatment effect of baicalein on a model of Parkinsonian tremor and elucidation of the mechanism. Life Sci 91(1–2):5–13
Acknowledgements
This work was supported by the Natural science foundation of Jiangsu Province (No. BK20141494), the Jiangsu Provincial Personnel Department “the Great of Six Talented Man Peak” Project (No. 2014-WSN-013), the University Natural Science Research Project in Jiangsu Province (No. 13KJB32009), the Opening Project of Jiangsu Key Laboratory of Neurodegeneration (No. SJ11KF01),and Project Funded by the Priority Academic Program Development of Jiangsu Higher Education Institutions (PAPD) and Science and Technology Project of Jiangsu Bureau of Traditional Chinese Medicine (No. YB2015163).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
J. Ding, J. Zhang, and X. Wang contributed equally to this work.
Rights and permissions
About this article
Cite this article
Ding, J., Zhang, J., Wang, X. et al. Relationship between the plasma levels of neurodegenerative proteins and motor subtypes of Parkinson’s disease. J Neural Transm 124, 353–360 (2017). https://doi.org/10.1007/s00702-016-1650-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00702-016-1650-2