Abstract
Aims
Prognostic significance of apolipoproteins in diabetic retinopathy risk has not been well investigated. The aim of this study was to reveal the relationship between the risk of diabetic retinopathy and the levels of several apolipoproteins and their ratios in a 10-year prospective cohort.
Methods
A total of 1023 diabetic patients without retinopathy were selected from a 10-year hospital-based diabetic cohort. In this cohort, all subjects had type 2 diabetes. Blood samples were obtained, and serum levels of several apolipoproteins were measured. In the follow-up period, diabetic retinopathy was diagnosed by two ophthalmologists through a series of ophthalmologic examinations. A Cox proportional hazard analysis was adopted to determine the relationship between the risk of diabetic retinopathy and the levels of several apolipoproteins and their ratios.
Results
In the follow-up period, 315 diabetic patients were suffered from diabetic retinopathy, and the remaining 708 patients did not. Baseline serum level of apoAI ≥ 7.4 μmol/L was related to the decreased risk of diabetic retinopathy (HR 0.86, 95% CI 0.70–0.99). Baseline levels of apoCIII ≥ 6.3 μmol/L, apoE ≥ 1.1 μmol/L, apoCIII-to-apoAI ratio ≥ 0.9 and apoE-to-apoAI ratio ≥ 0.2 were associated with the increased risk of this complication (HR 1.25, 95% CI 1.04–1.49; HR 1.23, 95% CI 1.03–1.47; HR 1.34, 95% CI 1.11–1.60; HR 1.21, 95% CI 1.01–1.46).
Conclusion
Elevated level of apoAI might be a protective factor for diabetic retinopathy. Increased levels of apoCIII, apoE, apoCIII-to-apoAI and apoE-to-apoAI ratios might be risk factors for this complication.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Diabetes mellitus (DM) is a common chronic disease with several metabolic disorders. In 2013, among adults in China, the estimated overall prevalence of DM is 10.9% and that for prediabetes is 35.7% [1]. In 2016, about 422 million people have DM globally, and more than 90% of them are type 2 DM patients [2]. Diabetic retinopathy (DR) is one of the major chronic microvascular complications. It affects more than 80% of patients with a diabetic duration of more than 20 years, and eventually leads to irreversible blindness [3]. In the USA, DR accounts for about 12% of new blind cases annually [4]. In China, the prevalence of DR in DM is more than 27.0% in a multi-hospital-based population [5]. Hyperglycemia, hypertension, disease duration and body mass index (BMI) are risk factors for DR, but other risk factors are still not clear [5,6,7].
Traditional lipids such as high density lipoprotein cholesterol (HDL-C) are useful prognostic indicators for type 2 DM [8]. But, the potential role of these traditional lipids in the development and progression of DR remains controversial. To date, some studies had confirmed the relationship between the traditional lipids and DR risk [9, 10], and others had failed to do so [11, 12].
Apolipoproteins are one kind of protein which combine with lipids to form lipoproteins. These combinations have good solubility in water and facilitate the transport of lipids in peripheral circulation. Furthermore, serum levels of many apolipoproteins are not disturbed by dietary status [13].
Recently, some studies focused on the prognostic role of apolipoproteins in DM risk and reported that some apolipoproteins (i.e., apoA1 and apoB) were good or even better prognostic indicators compared with the traditional lipids [14, 15]. An increasing number of studies also focused on the relationship between the serum levels of apolipoproteins and the risk of DR in DM patients, and provided some interesting results [16,17,18]. But, there were obvious limitations in these studies. First, most of the studies had a cross-sectional design and included a few subjects. Second, nearly all these studies focused on the apoA1 and apoB and did not explore other apolipoproteins. So, the prognostic significance of the apolipoproteins in the risk of DR remains to be fully elucidated.
Therefore, we conducted a 10-year prospective cohort study, included more than 1000 subjects, focused on several apolipoproteins (i.e., apoA1, apoCIII, apoD and apoE) and their ratios to apoA1 and tried to reveal the relationship between the serum level of apolipoproteins and the risk of DR in type 2 DM patients.
Materials and methods
Diabetic cohort
The study was approved by the ethics committee of Shuyang People’s Hospital.
There was a hospital-based prospective diabetic cohort in Shuyang People’s Hospital. All type 2 diabetic patients in Department of Endocrinology, Shuyang People’s Hospital between January 2004 and December 2006 were invited to join this cohort. A total of 2654 patients agreed with the request and signed the written informed consents. The rest of 175 patients or their family rejected to participate this cohort, and rejection rate was 6.2% (175/2829). In the follow-up period, 211 patients were lost, and loss rate was 8.0% (211/2654). All patients in the cohort were confirmed type 2 diabetic patients, and their diabetic durations at baseline were more than 1 year. Demographic information, eating habit, personal history, medical history and other medical information were recorded. Physical, serological, imaging, ophthalmic and other examinations were also performed.
The first follow-up for each patient was conducted between January 2009 and December 2011, and the second follow-up was conducted between January 2014 and December 2016. The examination items of the first and second follow-ups were the same as that at baseline.
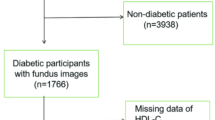
In this study, we only selected the patients without baseline retinopathy from this cohort. Finally, 1023 diabetic patients without retinopathy between January 2004 and December 2006 were included in our study (Fig. 1).
Serological examination
Three blood samples of each patient were collected during the whole study period (separately at baseline, the first and second follow-ups). The samples were sent to our biochemical laboratory in Shuyang People’s Hospital immediately and were centrifugated, extracted and stored at − 70 °C. All these samples were determined in this laboratory.
Serum levels of total cholesterol (TC), triglycerides (TG), HDL-C were measured by a Bayer ADVIA-1650 Chemistry System (Bayer Co., Tarrytown, NY, USA). Serum levels of apoA1, apoCIII, apoD, and apoE were detected using latex-particle-enhanced immunonephelometric assays on a BN ProSpec nephelometer (Dade Behring Co., Liederbach, Germany). Serum level of non-HDL-C was calculated using a formula: non-HDL-C (mmol/L) = TC (mmol/L) − HDL-C (mmol/L).
Each serological marker (i.e., glycosylated hemoglobin and traditional lipids) was measured three times using three serum samples separately collecting at baseline, the first and second follow-ups. Average value of each marker was calculated. Both baseline and average values of these serological markers were included in the study.
Diagnosis of diabetes mellitus and its ophthalmic complication
All patients in our study were diagnosed with DM according to the World Health Organisation standard [19]. The diagnostic criteria was listed as follows: (1) fasting blood glucose level ≥ 7.0 mmol/L, (2) 2-h postprandial blood glucose level ≥ 11.1 mmol/L; (3) blood glucose level 2 h after a 75 g oral glucose load in a glucose tolerance test ≥ 11.1 mmol/L.
A preliminary diagnosis of DR was made by a professional ophthalmologist and was rechecked by another professional ophthalmologist. The final diagnosis was made by them both. In this process, each patient received a visual acuity test and an ophthalmoscopy (after pupil dilation). If some signs of DR (such as leaking blood vessels and macular edema) were found, fundus fluorescein angiography was performed.
The severity of DR was determined according to a modified airlie house classification system [20]. Severe non-proliferative DR, proliferative DR and macular edema were regarded as vision threatening DR (VTDR).
Definition
Smoking was defined as having at least one cigarette per week for 1 year or more after the diagnosis of DM. Alcohol drinking was defined as drinking alcohol at least one time per week for 1 year or more after the diagnosis of DM. Tea drinking was defined as having at least a cup of tea per day for 1 year or more after the diagnosis of DM.
History of chronic diseases was defined as having one kind of chronic disease for 1 year or more after the diagnosis of DM. History of cardiovascular disease was defined as a history of angina pectoris, myocardial infarction, percutaneous coronary intervention or coronary artery bypass graft surgery and was verified by an electrocardiographic examination. History of cerebrovascular disease was defined as a history of cerebral infarction or cerebral hemorrhage and was verified by a cranial CT examination (if necessary). History of hypertension was defined as a history of taking antihypertensive drugs and was verified by a blood pressure examination. A physical examination was conducted, and BMI was calculated according to a formula: BMI (kg/m2) = weight (kg)/height2 (m2). Underweight, overweight and obesity were separately defined as BMI < 18.5 kg/m2, 23.0–24.9 kg/m2 and ≥ 25 kg/m2. History of hepatic dysfunction was defined as a history of virus hepatitis, hepatic adipose infiltration or other type of chronic liver disease and was verified by a liver function examination (total bilirubin > 34.2 μmol/L, glutamic pyruvic transaminase > 80 U/L or glutamic oxaloacetic transaminase > 80 U/L). History of renal dysfunction was defined as a history of diabetic nephropathy, glomerular nephritis or other type of chronic kidney disease and was verified by a renal function examination and an urinary albumin examination (serum creatinine > 133 μmol/L, urinary albumin > 30 mg/24 h). Diabetic nephropathy was defined as urinary albumin excretion > 30 mg/24 h coupled with exclusion of other causes of albuminuria in our diabetic patients.
Drug history relating to the following drug classes: statins, fibrates, calcium channel blockers, emictories, β-receptor blockers, antiepileptic drugs, and antipsychotic drugs, was documented based on taking any of these medications regularly for at least 1 year after the diagnosis of DM.
Active physical activity was defined as carrying out some kinds of physical activities (such as running) 1 h per day for 1 year or more after the diagnosis of DM. Negative physical activity was defined as never carrying out any kind of physical activity after the diagnosis of DM.
History of taking edible oils was defined as having edible oils ≥ 30 g/days for 1 year or more after the diagnosis of DM. History of taking beans and nuts was defined as having beans and nuts ≥ 50 g/days for 1 year or more after the diagnosis of DM. History of taking animal proteins was defined as having animal proteins ≥ 100 g/days for 1 year or more after the diagnosis of DM. History of taking vegetables was defined as having vegetables ≥ 400 g/days for 1 year or more after the diagnosis of DM.
This information was mainly collected from their medical records and follow-up records. If these records were unavailable, an interview would be performed. All these confirmations were completed by two physicians.
Statistical analysis
Continuous variables (such as age) were showed as arithmetical mean and standard deviation. Categorical variables (such as gender) were expressed as frequency and constituent ratio. Difference of two continuous variables was measured using independent sample t test. Difference of three continuous variables was measured using one-way variance analysis. Difference of those categorical variables was determined by Chi-square test. If a P value was less than 0.05, the difference was statistically significant. Relationships between the levels of apolipoproteins and the risk of retinopathy were measured using a Cox proportional hazard analysis. Because many variables could affect the serum levels of apolipoproteins or the risk of DM, two multifactorial models were performed. In model 1, it was adjusted by age and gender. In model 2, it was adjusted by age, gender, smoking, alcohol drinking, tea drinking, cardiovascular disease, cerebrovascular disease, hypertension, obesity, overweight, underweight, hepatic dysfunction, diabetic nephropathy, other type of renal dysfunction, oral agents, physical activity, diet, hypoglycemic therapy, glycosylated hemoglobin, duration of diabetes, serum levels of lipids and apolipoproteins. Hazard ratios (HRs) and 95% confidence intervals (CIs) were obtained. If a 95% CI included value one, the relationship was statistically significant. All analyses were performed using SPSS 19.0 (SPSS Inc, Chicago, IL, USA).
Results
In the follow-up period, a total of 315 diabetic patients were suffered from DR, and the remaining 708 patients did not. Table 1 shows the characteristics of the diabetic patients with retinopathy and the patients without retinopathy. Age, duration of DM, baseline and average serum level of glycosylated hemoglobin were higher in the patients with DR than in the patients without DR (P = 0.005, P < 0.001, P < 0.001, P < 0.001). Compared with the patients without DR, hypertension, total renal dysfunction, diabetic nephropathy and obesity/overweight were more common in the patients with DR (P = 0.007, P = 0.002, P = 0.001, P = 0.003). The patients without DR tended to carry out some more physical activities than the patients with DR did (P = 0.001, P = 0.016).
One-way variance analysis revealed that there was a significant difference among three measured values of TC, TG or non-HDL-C (P = 0.031, P = 0.020, P = 0.045), and there was no difference among three measured values of HDL-C, apoAI, apoCIII, apoD, apoE, apoCIII-to-apoAI ratio, apoD-to-apoAI ratio or apoE-to-apoAI ratio (P = 0.088, P = 0.165, P = 0.658, P = 0.712, P = 0.134, P = 0.453, P = 0.147, P = 0.361). So, both baseline and average values of the traditional lipids were included in the study, and only baseline values of the apolipoproteins were included in the study. This arrangement reduced the bias and enhanced the practical importance of the conclusion.
Table 2 shows the serum levels of the lipids and apolipoproteins in the diabetic patients with retinopathy and the patients without retinopathy. The baseline serum level of apoAI was lower in the patients with DR than in the patients without DR (P = 0.032). On the contrary, the baseline serum levels of apoCIII and apoE were higher in the patients with DR than in the patients without DR (P = 0.005, P = 0.043). The baseline apoCIII-to-apoAI and apoE-to-apoAI ratios were also higher in the patients with DR than in the patients without DR (P = 0.001, P = 0.005). There was no significant difference in the baseline levels as well as the average levels of these traditional lipids between the patients with DR and the patients without DR (P > 0.05).
Table 3 shows the associations of serum lipids and apolipoproteins levels with DR risk. The baseline serum level of apoAI ≥ 7.4 μmol/L was related to the decreased risk of DR in the diabetic patients (HR 0.86, 95% CI 0.70–0.99). The baseline levels of apoCIII ≥ 6.3 μmol/L, apoE ≥ 1.1 μmol/L, apoCIII-to-apoAI ratio ≥ 0.9 and apoE-to-apoAI ratio ≥ 0.2 were associated with the increased risk of DR (HR 1.25, 95% CI 1.04–1.49; HR 1.23, 95% CI 1.03–1.47; HR 1.34, 95% CI 1.11–1.60; HR 1.21, 95% CI 1.01–1.46).
Because apoAI, apoCIII, apoE, apoCIII-to-apoAI and apoE-to-apoAI ratios provided some statistically significant results, these apolipoproteins and their ratios were included in the following analysis. Table 4 shows the relationship between the DR risk and serum apolipoproteins levels in the different level groups. With the increase in levels in these markers, the associations of the DR risk with these apolipoproteins and their ratios were even stronger. Serum apoAI ≥ 8.47 μmol/L showed a stronger protective effect (HR 0.76, 95% CI 0.61–0.98). And, apoCIII ≥ 7.18 μmol/L, apoE ≥ 1.34 μmol/L, apoCIII-to-apoAI ratio ≥ 1.01 or apoE-to-apoAI ratio ≥ 0.22 showed a stronger pathogenic effect (HR 1.49, 95% CI 1.12–1.93; HR 1.36, 95% CI 1.05–1.76; HR 1.72, 95% CI 1.30–2.25; HR 1.89, 95% CI 1.42–2.47).
Of the 315 patients with DR, 110 patients had VTDR in the study. Table 5 shows the associations of serum apolipoproteins levels with the risk of VTDR. The associations of the complication risk with apoAI ≥ 7.4 μmol/L, apoCIII ≥ 6.3 μmol/L, apoE ≥ 1.1 μmol/L, apoCIII-to-apoAI ratio ≥ 0.9 and apoE-to-apoAI ratio ≥ 0.2 were possibly strengthened in the patients with VTDR compared with the patients with common DR. The detailed results are listed in Table 5.
Discussion
In this study, we revealed that several apolipoproteins (i.e., apoAI, apoCIII, apoE) and their ratios (i.e., ApoCIII-to-apoAI, ApoE-to-apoAI ratio) were significantly associated with the risk of DR in DM patients. Among them, apoAI seemed to be a protective factor against DR. If serum apoAI level ≥ 7.4 μmol/L at baseline, the risk of DR in the follow-up period might be reduced by approximately 15%. ApoCIII, apoE and their ratios to apoAI should be pathogenic factors for DR. If one of these indicators had a relatively high serum level (apoCIII ≥ 6.3 μmol/L, apoE ≥ 1.1 μmol/L, apoCIII-to-apoAI ratio ≥ 0.9 or apoE-to-apoAI ratio ≥ 0.2), the risk of DR might has an increase in 20–30% in the next 10 years. Furthermore, if the levels of these indicators further increased, their prognostic significance became even stronger (Table 4). These results were partly consistent with a previous study focusing on the relationship between serum apolipoproteins levels and incident type 2 DM [14].
However, we failed to confirm any prognostic significance of several traditional lipids in DR. In this study, there was no difference in the baseline or average levels of TC, TG, HDL-C and non-HDL-C between the DM patients with DR and the patients without DR. Subsequent multifactorial Cox proportional hazard analyses reported no statistically significant HRs and 95% CIs. So, serum apolipoproteins might be stronger prognostic indicators of DR than traditional lipids, which was consistent with a cross-sectional study including 224 diabetic patients [21]. A possible explanation for this result was that traditional blood lipids were unstable markers, and their serum levels were greatly influenced by diets and other factors.
In addition, these apolipoproteins showed more prognostic significance in VTDR than in common DR. Elevated level of apoAI (≥ 7.4 μmol/L) at baseline contributed to a 35% decrease in VTDR risk in the follow-up period. Increased levels of apoCIII (≥ 6.3 μmol/L), apoE (≥ 1.1 μmol/L), apoCIII-to-apoAI ratio (≥ 0.9) and apoE-to-apoAI ratio (≥ 0.2) indicated a 50–90% increase in VTDR risk. So, serum apolipoproteins levels might be better prognostic indicators for VTDR.
At present, there were few studies focusing on the potential mechanisms by which these apolipoproteins were protective or facilitate the development of DR. Previous studies suggested that apoAI and apoCIII could be involved in the physiopathology of DR [22, 23]. Vitreous fluid level of apoAI was elevated in the diabetic patients with PDR [22], and apoAI overexpression is an early event in the retina of diabetic patients [22, 23]. Serum apoAI was associated with increased vasomotor responsiveness to acetylcholine and flickering light and inversely related to retinal vessel tortuosity, indicating that higher serum apoAI was associated with better microvascular function in DM patients [24]. On the contrary, elevated serum apoCIII level was related to greater risk of subclinical atherosclerosis in DM patients [25]. In the DCCT/EDIC cohort, there was an independent positive association of serum apoCIII level with microvascular complications of type 1 DM [26].
Prognostic effect of apolipoproteins on microvascular complication DR might be explained by their mechanisms on large vessel disease. ApoAI was the major protein component in serum HDL particles, and reflected lipid accumulation in vessel tissues. It was involved in retrograde transport of fat molecules, formation of serum cholesteryl esters and anti-clotting process and had significant antioxidant, anti-inflammatory and atheroprotective effects [27]. ApoAI was regarded as a protective factor for coronary heart disease [28]. ApoCIII was a component of very low density lipoprotein (VLDL). It decreased the clearance of VLDL, stimulated the secretion of VLDL, inhibited the activities of several fat metabolism enzymes (such as hepatic lipase) and reduced the hepatic uptake of TC particles [29]. It was a predictor of coronary heart disease risk and a pro-inflammatory mediator [30]. These biological functions and characteristics of apoAI and apoCIII might partly explain their prognostic effect on DR.
ApoE was part of the chylomicron (CM) and intermediate density lipoprotein (IDL). It was a gene polymorphic protein with three alleles: ApoE-ε2, ApoE-ε3 and ApoE-ε4 [31]. ApoE-ε2 and apoE-ε4 were implicated in the development of atherosclerosis, but apoE-ε3 was considered to be a “neutral” genotype [32, 33]. However, another study suggested that apoE-ε2 and apoE-ε3, but not apoE-ε4, promoted retinal pathologic neovascularization in the patients with PDR [34]. In our study, apoE and apoE-to-apoAI ratio were pathogenic factors for DR. This result was likely to be affected by genetic polymorphisms of apoE. So, further studies should be carried out to explore the relationship between the genetic polymorphisms of apoE and the pathogenic effect of apoE on DR.
As mentioned above, these apolipoproteins were parts of HDL, IDL, VLDL or CM. Changes in serum apolipoprotein levels inevitably affected the serum lipids levels. So, these lipids became very important confounding factors in this study. In order to avoid these bias, we adopted the molar ratios of serum apolipoproteins levels to apoA1 and offset the interference effects from the lipids. Then, apoCIII-to-apoAI ratio and apoE-to-apoAI ratio still showed great prognostic significance in DR risk.
Compared with some previous studies, there were several characteristics in this study. First, this was a prospective cohort study, which might avoid the potential causality confusion. Second, considering that DR was a chronic complication in DM, the follow-up period of this study was 10 years. Third, the study enrolled more than 1000 subjects and had a relatively large sample size. Fourth, almost all the subjects who met the inclusion criteria were included in the study, and the rejection rate was 6.2% and the loss rate was 8.0%. Fifth, this was a comprehensive study, which focused on the association of DR risk with several traditional lipids, apolipoproteins and their ratios.
The findings in this study had several clinical implications. First, the significant variability of serum traditional lipids concentrations limited the clinical application in prediction of long-term prognosis in DM patients. Second, due to the stability of serum apolipoproteins, their concentrations at baseline provided some useful predictive information about the risk of DR in the 10-year follow-up. Apolipoproteins might be a much better predictor for DR risk in DM patients. Third, elucidating the prognostic role of the apolipoproteins in DR was helpful to explore the pathogenesis of this complication.
In conclusion, elevated level of apoAI might be a protective factor for DR. On the contrary, increased levels of apoCIII, apoE, apoCIII-to-apoAI and apoE-to-apoAI ratios might be risk factors for this complication in DM. The prognostic significance of these apolipoproteins and ratios might be strengthened in VTDR compared with common DR.
References
Wang L, Gao P, Zhang M, Huang Z, Zhang D, Deng Q, Li Y, Zhao Z, Qin X, Jin D, Zhou M, Tang X, Hu Y, Wang L (2017) Prevalence and ethnic pattern of diabetes and prediabetes in China in 2013. JAMA 317(24):2515–2523
World Health Organization (2016) Global Report on Diabetes, Geneva
Keel S, Xie J, Foreman J, van Wijngaarden P, Taylor HR, Dirani M (2017) The prevalence of diabetic retinopathy in Australian adults with self-reported diabetes: The National Eye Health Survey. Ophthalmology 124:977–984
Engelgau MM, Geiss LS, Saaddine JB, Boyle JP, Benjamin SM, Gregg EW, Tierney EF, Rios-Burrows N, Mokdad AH, Ford ES, Imperatore G, Narayan KM (2004) The evolving diabetes burden in the United States. Ann Intern Med 140:945–950
Pan CW, Wang S, Qian DJ, Xu C, Song E (2017) Prevalence, awareness, and risk factors of diabetic retinopathy among adults with known type 2 diabetes mellitus in an urban community in China. Ophthalmic Epidemiol 24(3):188–194
Cheung N, Mitchell P, Wong TY (2010) Diabetic retinopathy. Lancet 376:124–136
Hirsch IB, Brownlee M (2010) Beyond hemoglobin A1c-need for additional markers of risk for diabetic microvascular complications. JAMA 303:2291–2292
Haffner SM, Stern MP, Hazuda HP, Mitchell BD, Patterson JK (1990) Cardiovascular risk factors in confirmed prediabetic individuals. Does the clock for coronary heart disease start ticking before the onset of clinical diabetes? JAMA 263:2893–2898
Miljanovic B, Glynn RJ, Nathan DM, Manson JE, Schaumberg DA (2004) A prospective study of serum lipids and risk of diabetic macular edema in type 1 diabetes. Diabetes 53:2883–2892
Dornan TL, Carter RD, Bron AJ, Turner RC, Mann JI (1982) Low density lipoprotein cholesterol: an association with the severity of diabetic retinopathy. Diabetologia 22:167–170
Klein BE, Moss SE, Klein R, Surawicz TS (1991) The Wisconsin Epidemiologic Study of Diabetic Retinopathy. XIII. Relationship of serum cholesterol to retinopathy and hard exudate. Ophthalmology 98:1261–1265
Keech AC, Mitchell P, Summanen PA, O’Day J, Davis TM, Moffitt MS, Taskinen MR, Simes RJ, Tse D, Williamson E, Merrifield A, Laatikainen LT, d’Emden MC, Crimet DC, O’Connell RL, Colman PG, FIELD Study Investigators (2007) Effect of fenofibrate on the need for laser treatment for diabetic retinopathy (FIELD study): a randomised controlled trial. Lancet 370:1687–1697
Davidson MH (2009) Apolipoprotein measurements: Is more widespread use clinically indicated? Clin Cardiol 32:482–486
Brahimaj A, Ligthart S, Ikram MA, Hofman A, Franco OH, Sijbrands EJ, Kavousi M, Dehghan A (2017) Serum levels of apolipoproteins and incident type 2 diabetes: a prospective cohort study. Diabetes Care 40:346–351
Onat A, Hergenç G, Bulur S, Uğur M, Küçükdurmaz Z, Can G (2010) The paradox of high apolipoprotein A-I levels independently predicting incident type-2 diabetes among Turks. Int J Cardiol 142:72–79
Prakash G, Agrawal R, Satsangi SK, Prakash S (2016) Comparison of serum apolipoproteins and traditional lipids in eyes with diabetic retinopathy in Indian population: a case series. Middle East Afr J Ophthalmol 23:212–214
Crosby-Nwaobi R, Chatziralli I, Sergentanis T, Dew T, Forbes A, Sivaprasad S (2015) Cross talk between lipid metabolism and inflammatory markers in patients with diabetic retinopathy. J Diabetes Res 2015:191382
Sasongko MB, Wong TY, Nguyen TT, Kawasaki R, Jenkins AJ, Shaw J, Robinson C, Wang JJ (2012) Serum apolipoproteins are associated with systemic and retinal microvascular function in people with diabetes. Diabetes 61:1785–1792
Botas P, Delgado E, Castaño G, Díaz de Greñu C, Prieto J, Díaz-Cadórniga FJ (2003) Comparison of the diagnostic criteria for diabetes mellitus, WHO-1985, ADA-1997 and WHO-1999 in the adult population of Asturias (Spain). Diabet Med 20:904–908
Wong TY, Klein R, Islam FM, Cotch MF, Folsom AR, Klein BE, Sharrett AR, Shea S (2006) Diabetic retinopathy in a multi-ethnic cohort in the United States. Am J Ophthalmol 141:446–455
Sasongko MB, Wong TY, Nguyen TT, Kawasaki R, Jenkins A, Shaw J, Wang JJ (2011) Serum apolipoprotein AI and B are stronger biomarkers of diabetic retinopathy than traditional lipids. Diabetes Care 34:474–479
Simó R, Higuera M, García-Ramírez M, Canals F, García-Arumí J, Hernández C (2008) Elevation of apolipoprotein A-I and apolipoprotein H levels in the vitreous fluid and overexpression in the retina of diabetic patients. Arch Ophthalmol 126(8):1076–1081
Simó R, García-Ramírez M, Higuera M, Hernández C (2009) Apolipoprotein A1 is overexpressed in the retina of diabetic patients. Am J Ophthalmol 147(2):319–325
Sasongko MB, Wong TY, Nguyen TT, Kawasaki R, Jenkins AJ, Shaw J, Robinson C, Wang JJ (2012) Serum apolipoproteins are associated with systemic and retinal microvascular function in people with diabetes. Diabetes 61(7):1785–1792
Qamar A, Khetarpal SA, Khera AV, Qasim A, Rader DJ, Reilly MP (2015) Plasma apolipoprotein C-III levels, triglycerides, and coronary artery calcification in type 2 diabetics. Arterioscler Thromb Vasc Biol 35:1880–1888
Klein RL, McHenry MB, Lok KH, Hunter SJ, Le NA, Jenkins AJ, Zheng D, Semler A, Page G, Brown WV, Lyons TJ, Garvey WT, DCCT/EDIC Research Group (2005) Apolipoprotein C-III protein concentrations and gene polymorphisms in type 1 diabetes: associations with microvascular disease complications in the DCCT/EDIC cohort. J Diabetes Complicat 19(1):18–25
Yui Y, Aoyama T, Morishita H, Takahashi M, Takatsu Y, Kawai C (1988) Serum prostacyclin stabilizing factor is identical to apolipoprotein A-I (Apo A-I). A novel function of Apo A-I. J Clin Invest 82:803–807
McQueen MJ, Hawken S, Wang X, Ounpuu S, Sniderman A, Probstfield J, Steyn K, Sanderson JE, Hasani M, Volkova E, Kazmi K, Yusuf S, INTERHEART Study Investigators (2008) Lipids, lipoproteins, and apolipoproteins as risk markers of myocardial infarction in 52 countries (the INTERHEART study): a case-control study. Lancet 372:224–233
Mendivil CO, Zheng C, Furtado J, Lel J, Sacks FM (2010) Metabolism of very-low-density lipoprotein and low-density lipoprotein containing apolipoprotein C-III and not other small apolipoproteins. Arterioscler Thromb Vasc Biol 30:239–245
Xiong X, Liu H, Hua L, Zhao H, Wang D, Li Y (2015) The association of HDL-apoCIII with coronary heart disease and the effect of statin treatment on it. Lipids Health Dis 9(14):127
Singh PP, Singh M, Mastana SS (2006) APOE distribution in world populations with new data from India and the UK. Ann Hum Biol 33:279–308
Mahley RW (1988) Apolipoprotein E: cholesterol transport protein with expanding role in cell biology. Science 240:622–630
Civeira F, Pocoví M, Cenarro A, Casao E, Vilella E, Joven J, González J, Garcia-Otín AL, Ordovás JM (1996) Apo E variants in patients with type III hyperlipoproteinemia. Atherosclerosis 127:273–282
Masuda T, Shimazawa M, Hashimoto Y, Kojima A, Nakamura S, Suemori S, Mochizuki K, Kawakami H, Kawase K, Hara H (2017) Apolipoprotein E2 and E3, but Not E4, promote retinal pathologic neovascularization. Invest Ophthalmol Vis Sci 58(2):1208–1217
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Statement of human and animal rights
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Declaration of Helsinki of 1975, as revised in 2008.
Statement of informed consent
Informed consent was obtained from all patients for being included in the study.
Additional information
Managed by Massimo Porta.
Rights and permissions
About this article
Cite this article
Zhang, Q., Hu, J., Hu, Y. et al. Relationship between serum apolipoproteins levels and retinopathy risk in subjects with type 2 diabetes mellitus. Acta Diabetol 55, 681–689 (2018). https://doi.org/10.1007/s00592-018-1136-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-018-1136-9