Abstract
Purpose
Various external fixation systems for lower extremity long bone deformities have been used to various degrees of success, while newer mechanical lengthening nail (MLN) systems offer the potential for improved patient outcomes. Proponents of MLNs argue that they reduce the number of operations, infectious complications, and improve quality of life; however, the evidence to support these claims is scant. This systematic review aims to evaluate the optimal lengthening system for treating post-traumatic long bone deformity.
Methods
The systematic review was conducted in accordance with PRISMA guidelines. PUBMED, EMBASE, CINAHL, and the Cochrane Library were searched for comparative studies of lengthening techniques among adult patients with axial deformities. Studies were screened and data extracted in duplicate. Treatment groups were pooled into external fixation (EF) alone, combined internal and external fixation (CIF), and mechanical lengthening nail (MLN). Outcomes were mean lengthening achieved, lengthening index, and reported complications.
Results
Thirteen studies with 725 patients (mean age: 29.6 years, 74% male) were included. Nearly all of the studies were either prospective or retrospective cohort studies (n = 12), with one randomized controlled trial of moderate study quality. The mean limb lengthening achieved, lengthening index, and rate of reoperation were similar among the MLN, EF, and CIF groups.
Conclusion
The purported decreased the duration of lengthening and the risk of reoperation associated with MLNs was not demonstrated in this review. Patients with post-traumatic leg length deformities remain a challenging patient population to treat, with intervention being associated with high rates of infectious complications and need for revision operations.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Longitudinal bone deformities secondary to traumatic injury, infection, or defects of other etiologies severely impact a patient’s quality of life [1]. Further, the health utility for a patient suffering from a post-traumatic lower extremity limb defect may be lower than that of a patient suffering from a myocardial infarction or respiratory exacerbation[2, 3]. Over time orthopedic surgeons have developed various invasive techniques to address long bone deformities or defects. In the last 40 years, surgeons attempted lengthening or bone transport with the Ilizarov ring external fixator (IRF) to utilize distraction osteogenesis[4, 5]. The IRF offered the ability to accurately control transport through small adjustments to the rings, bars, and hinges of the fixator, typically distracting by about one millimeter per day. Although the IRF is accurate, it is relatively cumbersome and comes with multiple drawbacks, including pin site infections, soft tissue pain from pin site cutting through soft tissues, and skin muscle contractures and docking site nonunion[6].Patients treated with an IRF have a nearly 100% rate of pin tract infection and need to maintain diligent pin site care to reduce more serious complications and are at risk for muscle contractures and docking site non-unions[7, 8].
Variations in external fixator designs include uniplanar articulating or spanning external fixators, which offer some unique advantages but expose patients to complications associated with utilizing an external device. These fixators utilize fewer but larger pins and offer a lower rate of pin tract infection, however only have the ability to address single plane deformities in comparison with the multiplanar IRFs [9, 10]. Additional advantages may be yielded when used in combination with an intramedullary nail (IMN), which has been shown shorten the duration of external fixation placement, and decrease the amount of time required to achieve lengthening or transport [11]. An IMN is placed within the intramedullary canal and positioned without locking at one end of the nail to allow for lengthening or transport of the bone segment along the implant with the uniplanar EF, which is placed around the nail, fixed in each segment and distracted. Although combined internal/external lengthening approaches have improved the treatment course for patients with these complex post-traumatic deformities, they still often have to undergo multiple operations to achieve the desired correction. Namely, patients are burdened with the need for multiple unplanned adjustments, irrigation and debridement surgeries, and external fixator revisions to mitigating the common complications of lengthening, in addition to the standard procedures required for the initial implantation and final removal of the implants once lengthening is achieved. Additionally, the risk of local and systemic infections in these combined internal external fixation (CIF) systems remains high[12].
In an effort to reduce the number of operations while also reducing the risk of infections, all internal lengthening systems have been proposed. These systems consist of intramedullary nails or rods that have the capacity to elongate over time[13,14,15]. An internal mechanism allows the portions of the nail (which is locked at both ends) to mechanically separate over time and lengthen the bone. These all internal mechanical nail systems can be either controlled through a magnetic stimulus or through a movement-based (kinetic) activation system such as rotating the limb back and forth. The kinetic lengthening nails (KN), such as the intramedullary skeletal kinetic distractor (ISKD), are at risk of severe complications such as runaway nails where the kinetic lengthening mechanism does not stop when desired, or iatrogenic fractures that may also occur with uncontrolled distraction [16].
In contrast to KN’s, a variety of mechanical nails utilize magnetic lengthening mechanisms (e.g., Precice nail [NuVasive, San Diego, CA]), which are collectively be referred to as mechanical lengthening nails (MLNs). Internal distraction in MLNs is controlled through an external device, which triggers nail lengthening through non-kinetic means. For these nails lengthening is programmed to occur through external stimulation, such as an electromagnetic or ultrasound probe being placed over the implanted device, which in-turn triggers the MLN to lengthen by a set amount. While MLNs have the potential to decrease costs due to multiple procedures and cutaneous infections associated with EF and CIF techniques, high upfront implant costs in combination with reports of complications in early clinical series have limited wider implementation[17, 18].
Multiple lengthening options exist, including IRF or other EF systems, CIF techniques where an EF lengthens over an IMN, or all internal mechanical lengthening nail systems using either KNs or MLNs; however, there is little available evidence to favor one strategy over the other based on clinical outcomes or cost. This systematic review aims to evaluate the highest quality of evidence surrounding lengthening systems for long bones in the context of traumatic or acquired long bone defects or deformities in the adult population. The primary outcomes evaluated will be time to lengthening, rate of unplanned operations, and reported costs for each technique.
Methods
Search strategy
The authors systematically searched MEDLINE, OVID, CINAHL, and the cochrane central register of controlled trials (CENTRAL) databases from inception to March 30th, 2020. A search strategy was developed using controlled vocabulary such as medical subject headings (MeSH) terms and keywords. The main search concentrated on bone lengthening using external fixation (alone or over a nail, EF or CIF, respectively) ormechanical nail (MN). Conference abstracts, protocols or reviews were excluded from the search results. Regular alerts were established to regularly update the search until final manuscript submission (last updated-June 15 2020).
Study screening
This review was conducted according to the preferred reporting items for systematic review and meta-analysis (PRISMA) guidelines[19]. Systematic article screening was performed in duplicate with 3 reviewers (DA, LR, AS) through an independent screening and extraction process, from titles to full text review. Throughout the title and abstract screening stages, any article with discordance between reviewers was included to ensure that no relevant articles were prematurely excluded. The reviewers discussed any disagreements at the full text stage and study eligibility was resolved through review by the senior author (HJ). The reference lists of all included studies were additionally screened for relevant articles.
Assessment of study eligibility
The search included all comparative studies in any language investigating the treatment of longitudinal bone defects/deformity through bone lengthening in adults (age > 18). Studies primarily assessing congenital defects, or exclusively pediatric populations were excluded. Studies addressing only non-axial (i.e., rotational or angular) deformities or corrections were excluded. Additionally, studies that evaluated multiplanar correction alone were excluded. Case series, case reports, conference abstracts, and previous reviews were also excluded.
Relevant outcomes included the amount of lengthening in centimeters (cm), time spent lengthening, standardized lengthening score, paley complication scores, all cause reoperation, length of stay and infection.
Data extraction
Data extraction occurred in duplicate. The year of publication, author, location of study, and study design were recorded. Lengthening protocols were described and reported including type of external fixation (if used), length of immobilization, time spent lengthening, and all serious complications.
Outcome data were analyzed quantitatively when possible, and outcomes reported across multiple studies were pooled and reported as a frequency-weighted mean. Outcomes to be considered for meta-analysis were decided a priori if study heterogeneity was low (I2 < 60%). A methodological quality assessment was reported using the risk of bias tool in non-randomized studies (ROBINS-I)[20]. It was determined a priori that a meta-analysis would not be performed if the studies were of low quality (I2 > 60).
Assessment of agreement
Unweighted kappa (κ) and 95% confidence intervals (CI) were calculated for the title, abstract, and full text screening stages. The interpretation of kappa values was decided a priori where a κ > 0.60 indicated substantial agreement; 0.20 ≤ κ ≤ 0.60 indicated moderate agreement; and κ < 0.20 indicated slight agreement(21). Statistical analyses were calculated in R (Version 3.1, open access online). The alpha level was set to 0.05.
Results
Characteristics of included studies
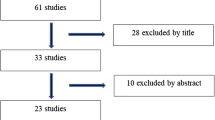
The search strategy yielded a total of 2572 articles after removal of duplicates, with 257 articles remaining after title and abstract screening, of which 13 articles were included for final analysis (one randomized controlled trial, 2 prospective cohort studies, and 10 retrospective cohort studies met the inclusion criteria) (Fig. 1)[10, 22, 23,24,25,26,27,28,29,30, 31,32,33, ]. Authors were in moderate agreement through title and abstract screening, with an unweighted kappa of 0.75. Agreement improved in full text screening, with kappa statistic of 0.9
The most common technique studied was use of EF alone (utilized in 14 groups), then CIF [6], followed by all internal MN’s [5] (Table 1). The most common implant utilized was the Ilizarov ring fixator, utilized in 6 groups. In the majority of remaining studies, a “monorail” technique (lengthening over a nail or CIF) was utilized, without further specification of implants.
Seventy-four percent of patients were male and an average age of 29.6 years at time of initial operation (range: 16–70). Treatment arms were an average size of 24 patients (range:11–46), and the median length of follow up was 33.2 months. A total of 746 limbs were included in the review among 725 individual patients.
The participating study treatment groups were subdivided into 3 categories determined a priori (external fixation (EF) alone, combined internal and external fixation (CIF), and all internal mechanical nails (MNs)). However, a formal meta-analysis comparing subgroups was not performed due to low-moderate quality of evidence, with substantial study heterogeneity (I2 > 60%). Thus, reported outcomes could not be combined across studies. Instead, descriptive statistics are reported below.
Quality assessment
The overall quality of studies was moderate, utilizing the ROBINS-I tool (Table 2). The majority (9/13) of studies was downgraded due to confounding as they represented either non-randomized studies that did not perform adequate statistical analysis (multivariate regression or propensity matching) to reduce risk of bias. However, the majority of studies had little concern for bias in treatment selection, intervention classification or missing data.
Lengthening and healing outcomes
Across all treatments, mean lengthening achieved per limb averaged 4.17 cm (SD: 1.02 cm), averaged across all 13 included studies. An external healing index (cm/month) was reported in 11 studies, with a mean score of 1.51 (0.7). Time to union was reported in 7 studies, with mean time to union of 5.24 months (1.8). Duration of EF placement was similar to reported time to union, with mean duration of fixation of 5.58 months (3.6). Lastly, distraction consolidation index (days/cm) was reported for half of potential studies (4 of 8 studies), with mean score of 188.7 (35.3).
Unplanned revision operations and complications
Unplanned revision operations were reported in 9 studies, with an average of 6.2 unplanned operations per treatment group. Pin tract infection rates were reported in all studies utilizing EFs and ranged from 0% of patients (in 2 studies assessing the CIF technique, n = 45) to near 100% infection rate in those undergoing Ilizarov fixation (44 infections reported for 48 patients).
The Paley reporting method for problems, obstacles, and complications (for IRF) was utilized in 4 studies with 1.3 total complications per limb on average. Otherwise, complications were inconsistently reported. Common complications reported included: limb length discrepancy greater than 2 cm (17/373, 4.5%.), aseptic loosening of implant (4 patients, 1%), magnetic nail malfunction (2 patients, 2.3%), and delayed union (2 patients, 0.5%).
Outcome scores
The association for the study and application of methods of Ilizarov score (ASAMI) was the only score reported in more than one study (four out of thirteen studies). A higher proportion of patients reported excellent scores (0.55), than either good (0.26) or fair scores (0.188). Hip or knee function scores were reported in only 3 studies. Given that each study utilized non-validated scores, results are not reported here.
Lengthening outcome
The mean limb lengthening achieved appeared similar across all 3 groups achieved (EF: 4.9 cm, CIF: 4.4, MN: 4.4) Similarly, the external fixation index was not meaningfully different among the groups (EF: 1.35, CIF: 1.78, MN: 1.32).
Complications
As mentioned above, complications were either reported using either the Paley complication scoring system or simply through listing all complications deemed relevant by the author. The only complication routinely reported was number of revision operations (9/14 studies). The number of revision operations per limb was similar in patients treated with MN (5.25) when compared to either EF alone (7.2) or CIF [5].
Discussion
This study represents the first systematic review to focus on longitudinal deformity correction in the lower extremity for traumatic or infectious defects. The main findings of this systematic review were that mean limb lengthening, external fixation index and number of revision operation did not appear to be different among groups. A formal meta-analysis could be undertaken due to the wide variation in reporting of outcomes and heterogeneity of study data, highlighting the fragility of primary research studies investigating this topic.
Our study demonstrated that patients with lower limb deformities can expect to have between 5 and 8 revision operations over the course of their treatment. Although MN’s are endorsed as a technique to reduce total number of operations, the pooled data do not convincingly support this claim [15, 34, 35]. In examining the safety of each technique, it was found that among all patients treated with MNs (109patients), only two (2%) had instances of mechanical failure, a dreaded complication in this cohort. Though serious complications and revision operations appear to occur at a similar rate to other techniques used in this patient population, MNs have substantially increased upfront implant costs. In particular, MLN systems can range from $20,000 to 50,000 USD [31, 36]. Given the scarcity of evidence, judicious use of all internal MNs needs to be exercised, until further evidence of improved outcomes and decreased complication relative to EF or CIF is demonstrated.
Our review shows that studies on the subject continue to report mainly on mean limb lengthening and external fixation index and not routinely on functional outcome scores or duration of fixation that may be more clinically relevant to the patient. The most common outcome score utilized was the ASAMI score in 4 studies. The ASAMI score is explained in more detail in Table 2. The ASAMI score has been widely utilized in previous studies[32, 37] and have been deemed consistent across different patient population receiving Ilizarov ring fixation[38]. It is recommended that future studies comparing these techniques continue to use the ASAMI score to allow the possibility of future meta-analysis.
With this said, it would be prudent for future studies in this domain to include a detailed cost analysis of the different techniques, including both direct and indirect costs. While there may be potential benefits of MN treatment as outlined above, these benefits must be put in the context of elevated upfront implant costs, along with other resource utilization (e.g., hospitalizations (reoperations), home visits (pin site care, out-patient visits) before widespread adoption of this surgical treatment. This comparison of health utilities and cost data would determine the cost per added quality-adjusted life year of limbl engthening treatment, with complications factored in. A cost effectiveness analysis, has been performed for many other orthopedic implants, would be essential before widespread adoption [39,40,41].
There are limitations in this review. This systematic review represents pooling of non-randomized comparative studies of level II or III evidence, with few studies sufficiently accounting for confounding and other sources of bias (Table 3). We chose to eliminate comparative studies focused only on cosmetic or stature-based limb lengthening to strengthen validity. Despite focusing solely on the traumatic limb population, studies utilized no classification systems used making pooling of results non-generalizable. Furthermore, reporting of outcomes for lengthening procedures are non-standardized, making it challenging to compare the relative efficacy of different techniques. Specifically, revisions operations reported often were unrelated to the index procedure or included planned reoperations (such as hardware removal). Accordingly, we can only report findings with a low-moderate level of confidence. Moreover, MLNs were only included as a treatment group in 5 studies, and revision operations were only reported in 9 studies total. Lastly, both kinetic (KN) and mechanical lengthening (MLN) systems were pooled together as all internal techniques, which may have diluted the effect of either group.
This is a timely review topic with the utilization rate of all internal lengthening MN systems on the rise. Our review sheds light on the challenge of navigating the multifactorial decision making process of treating complex longitudinal bone deformities using either EF, CIF or MN techniques and the absence of high-quality evidence to support one approach over another. It will be important for future research at the primary level to include ASAMI scores and cost-utility data, in the hopes of sufficient homogeneity for eventual pooled analysis.
In conclusion, this review demonstrated the paucity of high-quality literature comparing lower extremity lengthening with EF, CIF, and MN. A comparison of outcomes between the treatments highlighted that MN yielded a similar rate of revision operations and duration of fixation to EF and CIF. These results are a compilation of mainly retrospective cohort studies without adjustment for bias, representing low quality evidence. These results support the need for a high-quality randomized comparison of CIF and MN for the treatment of post-traumatic longitudinal limb deformities, utilizing the ASAMI outcome and collecting cost-utility data. This would provide valuable information to guide the management of patients who present with these challenging conditions.
References
Saddawi-Konefka D, Kim HM, Chung KC (2008) A systematic review of outcomes and complications of reconstruction and amputation for type IIIB and IIIC fractures of the tibia. Plast Reconstr Surg 122(6):1796–1805
Giannoudis PV, Harwood PJ, Kontakis G, Allami M, Macdonald D, Kay SP et al (2009) Long-term quality of life in trauma patients following the full spectrum of tibial injury (fasciotomy, closed fracture, grade IIIB/IIIC open fracture and amputation). Inj 40(2):213–219
Mollon L, Bhattacharjee S (2017) Health related quality of life among myocardial infarction survivors in the United States: a propensity score matched analysis. Health Qual Life Outcomes 15(1):235
Paley D (1990) Problems, obstacles, and complications of limb lengthening by the Ilizarov technique. Clin Orthop Relat Res NA(250):81–104
Paley D, Maar DC (2000) Ilizarov bone transport treatment for tibial defects. J Orthop Trauma 14(2):76–85
Dias RS, Harshavardhan JKG (2018) Tibial deformity correction by Ilizarov method. Int J Res Orthop 4(2):321
Parameswaran AD, Roberts CS, Seligson D, Voor M (2003) Pin tract infection with contemporary external fixation: how much of a problem? J Orthop Trauma 17(7):503–507
Antoci V, Ono CM, Antoci VJ, Raney EM (2008) Pin tract infection during limb lengthening using external fixation. Am J Orthop (Belle Mead NJ) 37(9):E150–E154
Kamegaya M, Shinohara Y, Shinada Y (1996) Limb lengthening and correction of angulation deformity: immediate correction by using a unilateral fixator. J Pediatr Orthop 16(4):477–479
Rozbruch SR, Kleinman D, Fragomen AT, Ilizarov S (2008) Limb lengthening and then insertion of an intramedullary nail: a case-matched comparison. Clin Orthop Relat Res 466(12):2923–2932
Paley D, Herzenberg JE, Paremain G, Bhave A (1997) Femoral lengthening over an intramedullary nail a matched-case comparison with Ilizarov femoral lengthening. J Bone Joint Surg Am 79(10):1464–1480
Kim S-J, Mandar A, Song S-H, Song H-R (2012) Pitfalls of lengthening over an intramedullary nail in tibia: a consecutive case series. Arch Orthop Trauma Surg 132(2):185–191
Hwang N, Grimer RJ, Carter SR, Tillman RM, Abudu A, Jeys LM (2012) Early results of a non-invasive extendible prosthesis for limb-salvage surgery in children with bone tumours. J Bone Joint Surg Br 94(2):265–269
Paley D (2015) PRECICE intramedullary limb lengthening system. Expert Rev Med Devices 12(3):231–249
Thaller PH, Furmetz J, Wolf F, Eilers T, Mutschler W (2014) Limb lengthening with fully implantable magnetically actuated mechanical nails (PHENIX((R)))-preliminary results. Inj 45(Suppl 1):S60–S65
Tiefenboeck TM, Zak L, Bukaty A, Wozasek GE (2016) Pitfalls in automatic limb lengthening-first results with an intramedullary lengthening device. Orthop Traumatol Surg Res 102(7):851–855
Schiedel FM, Vogt B, Tretow HL, Schuhknecht B, Gosheger G, Horter MJ et al (2014) How precise is the PRECICE compared to the ISKD in intramedullary limb lengthening? Reliability and safety in 26 procedures. Acta Orthop 85(3):293–298
Fragomen AT, Rozbruch SR (2017) Retrograde magnetic internal lengthening nail for acute femoral deformity correction and limb lengthening. Expert Rev Med Devices 14(10):811–820
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med 151(4):264–269
Sterne JAC, Hernán MA, Reeves BC, Savović J, Berkman ND, Viswanathan M et al (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919
Viera AJ, Garrett JM (2005) Understanding interobserver agreement: the kappa statistic. Fam med 37(5):360–363
Bhardwaj R, Singh J, Kapila R, Boparai RS (2019) Comparision of Ilizarov ring fixator and rail fixator in infected nonunion of long bones: a retrospective followup study. Indian J Orthop 53(1):82–88
Burghardt RD, Manzotti A, Bhave A, Paley D, Herzenberg JE (2016) Tibial lengthening over intramedullary nails: a matched case comparison with Ilizarov tibial lengthening. Bone Joint Res 5(1):1–10
Dammerer D, Kirschbichler K, Donnan L, Kaufmann G, Krismer M, Biedermann R (2011) Clinical value of the Taylor spatial frame: a comparison with the Ilizarov and orthofix fixators. J Child Orthop 5(5):343–349
El-Husseini TF, Ghaly NAM, Mahran MA, Al Kersh MA, Emara KM (2013) Comparison between lengthening over nail and conventional Ilizarov lengthening: a prospective randomized clinical study. Strateg Trauma Limb Reconstr 8(2):97–101
Emara KM, Allam MF (2008) Ilizarov external fixation and then nailing in management of infected nonunions of the tibial shaft. J Trauma 65(3):685–691
Fragomen AT, Kurtz AM, Barclay JR, Nguyen J, Rozbruch SR (2018) A comparison of femoral lengthening methods favors the magnetic internal lengthening nail when compared with lengthening over a nail. HSS J 14(2):166–176
Horn J, Grimsrud O, Dagsgard AH, Huhnstock S, Steen H (2015) Femoral lengthening with a motorized intramedullary nail. Acta Orthop 86(2):248–256
Laubscher M, Mitchell C, Timms A, Goodier D, Calder P (2016) Outcomes following femoral lengthening: an initial comparison of the precice intramedullary lengthening nail and the LRS external fixator monorail system. Bone Joint J 98B(10):1382–1388
Mahboubian S, Seah M, Fragomen AT, Rozbruch SR, Seah M et al (2012) Femoral lengthening with lengthening over a nail has fewer complications than intramedullary skeletal kinetic distraction. Clin Orthop Relat Res 470(4):1221–1231
Richardson SS, Schairer WW, Fragomen AT, Rozbruch SR (2019) Cost comparison of femoral distraction osteogenesis with external lengthening over a nail versus internal magnetic lengthening nail. JAAOS-J Am Acad Orthop Surg 27(9):e430–e436
Rohilla R, Wadhwani J, Devgan A, Singh R, Khanna M (2016) Prospective randomised comparison of ring versus rail fixator in infected gap nonunion of tibia treated with distraction osteogenesis. Bone Joint J 98-B(10):1399–1405
Sun X-T, Easwar TR, Stephen M, Song S-H, Kim S-J, Song H-R (2011) Comparative study of callus progression in limb lengthening with or without intramedullary nail with reference to the pixel value ratio and the Ru Li’s classification. Arch Orthop Trauma Surg 131(10):1333–1340
Hammouda AI, Jauregui JJ, Gesheff MG, Standard SC, Conway JD, Herzenberg JE (2017) Treatment of post-traumatic femoral discrepancy with PRECICE magnetic-powered intramedullary lengthening nailsm. J Orthop Trauma 31(7):369–374
Nasto LA, Coppa V, Riganti S, Ruzzini L, Manfrini M, Campanacci L et al (2020) Clinical results and complication rates of lower limb lengthening in paediatric patients using the PRECICE 2 intramedullary magnetic nail: a multicentre study. J Pediatr Orthop B 29(6):611–617
Eltorai AEM, Fuentes C (2018) Magnetic growth modulation in orthopaedic and spine surgery. J Orthop 15(1):59–66
Brinker MR, O’Connor DP (2007) Outcomes of tibial nonunion in older adults following treatment using the Ilizarov method. J Orthop Trauma 21(9):634–642
Chaudhary MM, Malhotra M, Neeli U, Vaishnani K, Banik S, Jagani N (2019) Ilizarov techniques for upper tibial nonunions: How difficult is it to achieve excellent results? J Limb Lengthening Reconstr 5(2):71
Paxton EW, Kiley M-L, Love R, Barber TC, Funahashi TT, Inacio MCS (2013) Kaiser permanente implant registries benefit patient safety, quality improvement, cost effectiveness. Jt Comm J Qual Patient Saf 39(6):246-AP4
Barlow BT, McLawhorn AS, Westrich GH (2017) The cost-effectiveness of dual mobility implants for primary total hip arthroplasty: a computer-based cost-utility model. J Bone Jt Surg 99(9):768–777
Fisman DN, Reilly DT, Karchmer AW, Goldie SJ (2001) Clinical effectiveness and cost-effectiveness of 2 management strategies for infected total hip arthroplasty in the elderly. Clin Infect Dis 32(3):419–430
Funding
The research did not receive any funding and none of the participating authors report and conflicts of interests or competing interest.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
No ethics approval was required for this research.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Axelrod, D., Rubinger, L., Shah, A. et al. How should we lengthen post-traumatic limb defects? a systematic review and comparison of motorized lengthening systems, combined internal and external fixation and external fixation alone. Eur J Orthop Surg Traumatol 31, 1015–1022 (2021). https://doi.org/10.1007/s00590-020-02831-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-020-02831-y