Abstract
Purpose
Oswestry Disability Index (ODI) was established by Fairbank in 1989 to assess functional disabilities in low back pain (LBP). It was last updated in 2019 as ODI version 2.1b (ODI AU_2.1b). ODI was first translated into Simplified Chinese Oswestry Disability Index (CODI) in 2008 by Lue. The construct validity, internal consistency, level of agreement and the floor and ceiling effects of CODI were found unclear by Yao in 2016. This study will verify how well the adapted Cantonese–Hong Kong Oswestry Disability Index version 2.1b (HKCODI) aligns with ODI AU_2.1b in the Southern Chinese population.
Methods
The translation of ODI AU_2.1b was performed according to guidelines from MAPI Research Trust and American Association of Orthopaedic Surgeons. Psychometric properties of HKCODI were tested statistically by Pearson’s correlation, Cronbach’s Alpha and Intraclass Correlation Coefficient (ICC).
Results
A total of 200 subjects (109 males, 91 females) aged from 15 to 85 (mean age = 58.91) with LBP scored from 3/10 to 10/10 in the Visual Analogue Scale (VAS) were recruited in the Occupational Therapy Department of a tertiary referral center. HKCODI demonstrated strong construct validity in comparing with Hong Kong Roland–Morris Disability Questionnaire (HKRMDQ) (r = 0.666, p = 0.000), Short Form Health Survey (SF-36) Physical Composite Summary (− 0.700, p = 0.000) and VAS (0.487, p = 0.000). Excellent internal consistency and test–retest reliability were confirmed with Cronbach’s Alpha of 0.997 and ICC of 0.993 at 95% confidence level.
Conclusion
Cross-cultural adaptation of ODI AU_2.1b has been translated and validated as HKCODI and Item-8 (Sex Life) was suggested to skip for patient older than 60. HKCODI is a fully self-administered and highly reliable tool in assessing the functional disability of patients with LBP in the Southern Chinese population.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Low back pain (LBP) is a common cause of functional disability in affecting an individual’s daily life, work and quality of life (QOL) [1]. Occupational therapists and clinicians work hard in establishing a simple and culturally relevant outcome measurement for quantifying the therapeutic effectiveness in the activity of daily living (ADL) function in the rehabilitation of LBP. The Oswestry Disability Index (ODI) is the most commonly used outcome measures with good psychometric properties for both acute and chronic LBP in the past 30 years. The ODI was developed and published by Fairbank et al. in 1980 [2]. ODI measures the impact on patient’s functional disability on 10 ADL-related items, including “Pain Intensity,” “Self Care,” “Lifting Ability,” “Walking,” “Sitting,” “Standing,” “Sleeping Quality,” “Sex Life,” “Social Life” and “Traveling” [3]. Each of the 10 items was given a score of 0 to 5 depending on the severity of the disability and that was reflected in six corresponding description statements. The percentage of the total possible score obtained from the completed items was named as the ODI score, with a range from 0 to 100. The greater the ODI score, the more functional disabilities in ADL.
In 1985, a group of Medical Research Council investigators removed the reference to analgesic intake in item-1 “Pain Intensity” and supplemented an option of “no pain” in the ODI version 2.0 [4]. In the same year, Fairbank changed few words in the last description statement in the “Traveling” section. He changed the phrase “to the doctor or hospital” into “to receive treatment” and set up the ODI version 2.1. The phrase “is affected” in the opening sentence of ODI version 2.1 was changed to “effects” in the advanced version named ODI version 2.1a (ODI AU_2.1a) and was published in 2000 after validation [3]. The latest version, ODI AU_2.1b, is now used and distributed by the copyright holder, the MAPI Research Trust website (https://eprovide.mapi-trust.org/instruments/oswestry-disability-index#member_access_content) without amending any single word but only a minor change in the physical layout of the questionnaire.
ODI AU_2.1b is a self-reported questionnaire assessing how LBP affects one’s functional disability in ADL. According to the MAPI Research Trust, 68 translated versions in different languages and cultures have been distributing in 2021. Among the official translations listed in the ODI website (https://mapi-trust.org/questionnaires/odi/), Lue et al. had translated ODI version 2.0 in 2008 as the Traditional Chinese ODI (TCODI) [5] for Mandarin-speaking Taiwanese, and the Simplified Chinese ODI AU_2.1a (SCODI) was translated by Liu et al. for Mandarin-speaking Chinese population in 2009 [6]. TCODI is the only Chinese version distributed officially by the MAPI Research Trust. Mandarin is the national dialect, whereas Cantonese is the Southern Chinese dialect spoken in Hong Kong and they could not be fully understood by each other.
In 2005, Chow & Chan [7] had translated and validated the ODI version 2.0 into the Chinese Oswestry Disability Index (CODI) for chronic LBP patients in Hong Kong. However, the construct validity, internal consistency, level of agreement and the floor and ceiling effects of CODI were still unclear. They had adapted and changed the description of walking distance in “miles” into walking duration in “ hours and minutes,” which was a totally different dimension in specifying the walking capability. The tolerable duration could not provide the same perception as the walking distance since it varied with the adopted speed, pace and intermittent resting during the walk. These variations were common in patients with active LBP whose movement would be restricted by pain. This ambiguity in the description statement confused the patients and they always requested additional explanation from therapists in the process, which made the CODI not fully “self-administered” and the resulting scores could be biased.
Materials and methods
This study aimed to verify the adapted Cantonese (Hong Kong) Oswestry Disability Index (HKCODI) in alignment with the ODI AU_2.1b for the Southern Chinese population. The English version of ODI AU_2.1b for the UK was adopted with permission from MAPI Research Trust, Lyon, France.
Cross-cultural adaptation of HKCODI
The cross-cultural adaptation to Cantonese for the Southern Chinese population had been confirmed and approved by the MAPI Research Trust, while prior approval for the study was obtained from the Institutional Review Board (IRB) (UW 12–369).
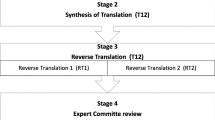
The cross-cultural adaption process of the ODI AU_2.1b was performed based on the MAPI guidelines, “American Association of Orthopaedic Surgeons (AAOS) Guidelines for the Process of Cross-Cultural Adaption of Self-Report Measures” and comments in the “Systematic Review of Cross-cultural Adaption of the Oswestry Disability Index” by Yao in 2016 [8, 9].
The synthesized Cantonese questionnaire was initially translated by an experienced English teacher and an occupational therapist with Chinese-Cantonese as their first language. It was then translated back to English by another two professional English–Chinese translators who had no medical background and knowledge of ODI AU_2.1b.
All translations were discussed among the Expert Committee of another two professional translators, a doctor and two occupational therapists; the pre-final questionnaire was created upon mutual agreement. In the pilot study, 31 patients aged 25 to 60 (18 male and 13 female) with symptomatic Prolapsed Intervertebral Disk (PID) were recruited in a single center, the Occupational Therapy Department (OCC) of the principal author. All subjects with active psychiatric issue or work-related injury with unsettled worker’s compensation were excluded from the pilot study. Comments from subjects on fluency, ease of understanding and meaning of the statements were discussed in the debriefing session, especially the adapted item “Walking.” The expert committee and the principal investigator would confirm the final version of HKCODI if no problem arose.
Sample recruitment
Sample size calculation by the G-Power 3.1.9.4 indicated that a total of 144 subjects were required for an alpha of 0.05, the statistical power of 0.80, a lower limit of the estimated value of rho (ρ0) 0.7 and upper limit of the estimated value of rho (ρ1) 0.9. To ensure an effective sample size, 200 individuals, i.e., around 38% reserve, were recruited, to prevent undesirable withdrawal and missing data. They were all recruited from OCC by convenience sampling between 2014 and 2018.
Inclusion criteria
Acute or chronic LBP patients with functional disability in ADL resulted from PID, spinal fracture, spondylolisthesis, lumbar stenosis or chronic non-specific back pain. They were all Hong Kong Chinese aged above 15 who could understand written Chinese and no history of spinal surgery or systemic diseases, such as ankylosing spondylitis or diseases that would possibly lead to joint deformities and contractures. All active or chronic psychiatric patients with cognitive deficit were excluded. Subjects should free from worker’s compensation or legal procedures related to their current back injury. Written informed consent was obtained from each participant prior to the study.
Procedure of evaluation
Two hundred subjects aged from 15 to 85 had completed HKCODI, Visual Analogue Scale (VAS), Hong Kong version of Roland–Morris Disability Questionnaire (HKRMDQ) [9] and Hong Kong Short Form Health Survey (SF-36) [10] at first seen. All measurements were self-administered; interpretation from the investigators was prohibited. All participants were asked to repeat the HKCODI after 24 h, any significant fluctuation of symptoms should be avoided. All participants completed the questionnaires in OCC and the attending therapist had checked the completeness of all replied questionnaires before dismissing in both the first and second administrations to avoid any missing data.
Statistical analysis
The normal distribution of the HKCODI score was confirmed by the Kolmogorov–Smirnov test to ensure the appropriateness for further parametric statistical analysis. The Bland–Altman plot of differences in HKCODI scores of each subject should be less than 15% to eliminate the floor and ceiling effect [11]. A negligible floor and ceiling effect was a prerequisite for an effective and reliable validation process for a self-reported questionnaire [11]. In alignment with the findings from the validation studies of other countries, HKCODI was expected to have a strong construct validity; the Pearson’s correlation coefficient (r) with VAS, HKRMDQ and SF-36 should be above ± 0.4 [12]. All analysis was performed at a 95% confidence level to ensure a valid calculation with the IBM SPSS Statistics version 25 software.
An excellence internal consistency and agreement among the tested items were anticipated with Cronbach’s Alpha above 0.80 [12]. “Cronbach’s Alpha if the item was deleted” adopted should be less than Cronbach’s Alpha if a high relevance and importance of that particular item subsist within the questionnaire [5].
The test–retest reliability of HKCODI was confirmed with an insignificant difference in the Paired-samples t test in different administrations and the intraclass correlation coefficient (ICC) should stay above 0.60 to demonstrate good test–retest reliability [13]. Standard Error of Measurement (SEM) at 95% confidence level could quantify possible errors in the measurement, which was acceptable within 10% of full marks in HKCODI with the cutoff values in individual items at 0.5 and HKCODI score at 10 [11]. The Minimum Detectable Change (MDC) was calculated as the product of SEM times 1.96 and square root of 2 (\({\text{MDC}} = {\text{SEM}} \times 1.96 \times \surd 2\)); the cutoff value of the acceptable MDC should be less than 1.386 for individual items and 27.72 for the overall HKCODI score [5].
Results
There were 109 males and 91 females with mean age of 58.91 had completed the questionnaires (Fig. 1). Nearly half of the population had secondary education or higher (45%) and most of them were retiree (47.5%); 21% was professionals and only 6.5% was heavy manual workers (Table 1).
Translation and cross-cultural adaptation of ODI AU_2.1b
In the forward translation, both translators mentioned the description of item 4 “Walking” which was difficult for local patients to understand the distance in imperial unit “mile”; as Hong Kong uses the metric system. No matter which system was adopted, it was quite abstract for a laity to comprehend in the self-estimation of performance. To obtain a more accurate judgment without changing the original construct and meaning of the questionnaire, a translator suggested adding a note to elucidate the description. He proposed using the perception of the running track in a standard sports ground in Hong Kong, which is 400 m long (equivalent to ¼ mile). Such sports grounds were available in every district in Hong Kong; and easily accessible by all social classes as a convenient venue for daily exercise and family activities. A mutual consensus had attained among the translators, expert committee and the chief investigator; the final version of HKCODI was formed. The finalized version of HKCODI has registered in the MAPI Research Trust for official distribution under copyright permission of access and application.
HKCODI had good interpretability in the translated questions and adapted descriptions to facilitate a completely self-administration without additional assistance.
The most common diagnosis in the population was chronic non-specific LBP (56%), followed by lumbar stenosis (32.5%), PID (20.5%), spondylolisthesis (9.5%), spinal fractures (5.5%) and other spinal pathologies causing LBP (4%) (Table 1). The severity of pain ranged from VAS 0.3/10 to 10/10 (mean = 6.61/10) (Table 2).
The score achieved in HKCODI ranged from 2 to 92% with a mean score of 50.92% (SD = 19.28). The mean HKRMDQ score was 9.65 (SD = 4.13) with a total score of 24. The SF-36 subscales mean score in “Physical Functioning” (PF) was 60.95 (SD = 20.23), “Role-Physical” (RP) was 24.75 (SD = 32.48), “Bodily Pain” (BP) was 36.14 (SD = 19.21), “General Health” (GH) was 46.28 (SD = 14.28), “Vitality” (VT) was 70.00 (SD = 23.05), “Social Functioning” (SF) was 56.16 (SD = 21.17), “Role-Emotional” (RE) was 53.20 (SD = 38.03), and “Mental Health” (MH) was 77.98 (SD = 17.28) (Table 2). The overall performance was summarized as mean “Physical Composite Summary” (PCS) at 32.26 and mean “Mental Composite Summary” (MCS) at 54.46 out of the total score of 100 in each summary.
Validation of HKCODI
The distribution of HKCODI scores proved to be normal in the Kolmogorov–Smirnov tests (Fig. 2) and the Bland–Altman plot (Fig. 3) with a mean difference of − 0.2685 (SD = 2.2764) had demonstrated an insignificant floor and ceiling effect at a 95% limit of agreement with a negligible percentage of flooring and ceiling at 3% and 5%, respectively [11, 14].
HKCODI had an excellent construct validity with Pearson’s correlation coefficients (r) 0.666 (p = 0.000) with HKRMDQ, − 0.700 (p = 0.000) with SF-36 PCS and 0.487 (p = 0.000) with VAS. HKCODI was proven to be valid in assessing the functional disability in LBP incomparable to other well-recognized assessment tools.
The Cronbach’s Alpha 0.997 indicated a strong internal consistency and a smaller “Cronbach’s Alpha if item deleted” of an individual item (Table 3) ranged from 0.875 to 0.893, suggested good reliability with excellent relevance and agreement of included items in HKCODI; all items in the questionnaire should be preserved.
No significant difference was found in HKCODI scores between the first and second administrations; it showed a strong test–retest reliability with ICC at 0.993 (p = 0.000). The SEM (0.161) shown in Table 4 was less than 10% of the total range of score (100) and MDC (0.446) was less than the cutoff values at 1.386 for individual items and 27.72 for the overall HKCODI score at 95% confidence level. Negligible possible errors [12] had further verified the excellent test–retest reliability of the adapted HKCODI.
Discussion
Only HKCODI and TCODI had strong correlations with the golden standard, HKRMDQ [5], but the concurrent validity of SCODI and CODI was not mentioned in the publications (Table 5) [6, 7]. In this study, the comparison with SF-36 was perfectly in line with all Chinese versions, except CODI. Subscales BP, SF, RP and PF in SF-36 showed relatively strong relationships, which was parallel to the cross-cultural adaptation and validation studies in Japan [15], South Korea [16], China [6], Taiwan [5], India [17], the Republic of Croatia [18], Italy [19], Brazil [20] and Norway [21].
One hundred and twenty-eight subjects including 71 females (78%) and 57 males (52%) had skipped the item 8 “Sex Life” in HKCODI with a response rate of 36%. Similar phenomenon was mentioned in the validation studies in Finland (14.8%) [22], Polish (22%) [23], Taiwan (29.4%) [5], India (31.5%) [24], China (69.27%) [6] and the Republic of Croatia (71.1%) [18].
The low response rate in “Sex life “was explicated by lacking opportunity and a conservative mindset, especially in the Chinese population [5, 6]. The “Sex Motive” was suggested by Costa in 2015 to be a key issue leading to the low response rate in item 8 [25]. Theoretically, young adults were more active in sex life than old adults, who may not be able to answer without recent sexual experiences. To testify the effect of sex motives on the response rate and value in item 8, the subjects were divided into the “Sexually Active” group (SA) aged 15 to 60 and the “Sexually Inactive” group (SI) aged above 60 for further analysis.
There were 87 Sexually Active and 113 Sexually Inactive subjects. 90.8% of SA was workers and the majority was working as professionals, while 77.0% of SI was retirees. SA had a response rate of 62.1% to HKCODI item 8 and SI only got 15.9%. The mean VAS in SI was slightly higher (6.95) than SA (6.14). SI (53.72) showed a more severe functional disability than that of SA (47.29). Correlations with HKRMDQ, VAS and SF-36 pertained with SA, which was stronger than the SI (Table 6).
All HKCODI items in SA showed high relevance with Cronbach’s Alpha (0.879) greater than “Cronbach’s Alpha if item deleted” (0.871) (Table 7), and no item was indicated for deletion. On the contrary, the Cronbach’s Alpha in SI (0.929) was greater than 0.9, which suggested that some items were redundant. Moreover, item 8 in SI (0.931) was the only one that exceeded Cronbach’s Alpha (Table 7), which indicated its redundancy and was recommended to delete from the questionnaire. It sounds reasonable to eliminate item 8, “Sex Life,” for those who had no sex life and motives at all.
Quality of life (QOL) showed to be more dependent on physical performance than mental acceptance and adaptations in all ages (Table 6) had a stronger correlation to physical satisfaction than mental satisfaction in SF-36. (Table 5) As expected, SA had a stronger correlation with PF, RP, BP and SF that aligned with the findings in the cultural adaptation studies in China [6], Taiwan [5], Japan [15], Italy [19], Norway [21] and Poland [23]. In contrast, only BP was strongly correlated with HKCODI in SI indicated that pain had a potent influence on functional disabilities in older LBP patients than the youngsters (Table 5).
Conclusion
The ODI AU_2.1b has successfully translated into Cantonese and culturally adapted for the Southern Chinese population as HKCODI. The good psychometric properties had been confirmed with high comparability and validity to the well-recognized assessment tools for LBP, including HKRMDQ and SF-36. Excellent test–retest reliability had been testified by ICC at 0.993 having an insignificant floor and ceiling effect.
Excellent internal consistency of HKCODI was proven with Cronbach’s Alpha at 0.879. The redundancy of items 8 “Sex Life” was confirmed and suggested to be deleted for those Sexually Inactive. This result suggested using all items for younger patients aged below 60 and skipped item 8 “Sex Life” for those aged above 60.
This fully self-administered HKCODI was a valid and reliable tool in assessing the functional status of the Southern Chinese population with LBP.
References
Ma C, Wu S, Xiao L et al (2011) Responsiveness of the Chinese version of the Oswestry disability index in patients with chronic low back pain. Eur Spine J 20:475–481. https://doi.org/10.1007/s00586-010-1624-2
Fairbank JC, Couper J, Davies JB et al (1980) Convergent correlations. Physiotherapy 66:271–273
Fairbank JCT, Pynsent PB (2000) The oswestry disability index. Spine (Phila Pa 1976) 25:2940–2953. https://doi.org/10.1097/00007632-200011150-00017
Fairbank JCT (2007) Use and abuse of oswestry disability index. Spine (Phila Pa 1976) 32:2787–2789. https://doi.org/10.1097/BRS.0b013e31815b9e9d
Lue YJ, Hsieh CL, Huang MH et al (2008) Development of a Chinese version of the Oswestry disability index version 2.1. Spine (Phila Pa 1976) 33:2354–2360. https://doi.org/10.1097/BRS.0b013e31818018d8
Liu H, Tao H, Luo Z (2009) Validation of the simplified Chinese version of the Oswestry disability index. Spine (Phila Pa 1976) 34:1211–1216. https://doi.org/10.1097/BRS.0b013e31819e2b34
Chow JHW, Chan CCH. (2005) Validation of the Chinese version of Oswestry Disability Index. Work. 25:307–14. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L43949841
Yao M, Wang Q, Li Z et al (2016) A systematic review of cross-cultural adaptation of the Oswestry Disability Index. Spine (Phila Pa 1976) 41:E1470–E1478. https://doi.org/10.1097/BRS.0000000000001891
Beaton DE, Bombardier C, Guillemin F et al (2000) Guidelines for the process of cross-cultural adaptation of self-report measures. Spine (Phila Pa 1976) 25(24):3186–3191. https://doi.org/10.1097/00007632-200012150-00014
Lam CLK, Lam DTP, Gandek B (2000) Hong Kong SF-36 Validation and Norming Validation and norming of the MOS 36-item Short Form Health Survey in Hong Kong Chinese adults. Health Serv Res Comm (Hong Kong) Rep. 1–6.
Dean K, Walker Z, Jenkinson C (2018) Data quality, floor and ceiling effects, and test–retest reliability of the mild cognitive impairment questionnaire. Patient Relat Outcome Meas 9:43–47. https://doi.org/10.2147/prom.s145676
Crocker L, Algina J (1986) What is test theory ? In: Introduction to modern and classical test theory.
Sheahan PJ, Nelson-Wong EJ, Fischer SL (2015) A review of culturally adapted versions of the Oswestry Disability Index: the adaptation process, construct validity, test-retest reliability and internal consistency. Disabil Rehabil 37:2367–2374. https://doi.org/10.3109/09638288.2015.1019647
Lim CR, Harris K, Dawson J et al (2015) Floor and ceiling effects in the OHS: an analysis of the NHS PROMs data set. BMJ Open 5:e007765. https://doi.org/10.1136/bmjopen-2015-007765
Fujiwara A (2009) Japanese version of the Oswestry disability index. J Japanese Soc Lumbar Spine Disord 15:11–16. https://doi.org/10.3753/yotsu.15.11
Kim DY, Lee SH, Lee HY et al (2005) Validation of the Korean version of the Oswestry disability index. Spine (Phila Pa 1976) 30:123–127. https://doi.org/10.1097/01.brs.0000157172.00635.3a
Nishant CHS, Kapoor KS (2014) New modified english and hindi oswestry disability index in low back pain patients treated conservatively in Indian population. Asian Spine J 8:632–638. https://doi.org/10.4184/asj.2014.8.5.632
Domazet I, Nemir J, Barl P et al (2018) Validation of the Croatian version of the Oswestry disability index. Eur Spine J 27:2814–2822. https://doi.org/10.1007/s00586-018-5757-z
Monticone M, Baiardi P, Ferrari S et al (2009) Development of the Italian version of the Oswestry disability index (ODI-I): a cross-cultural adaptation, reliability, and validity study. Spine (Phila Pa 1976) 34:2090–2095. https://doi.org/10.1097/BRS.0b013e3181aa1e6b
Coelho RA, Siqueira FB, Ferreira PH et al (2008) Responsiveness of the Brazilian-Portuguese version of the Oswestry disability index in subjects with low back pain. Eur Spine J 17:1101–1106. https://doi.org/10.1007/s00586-008-0690-1
Grotle M, Brox JI, Vøllestad NK (2003) Cross-cultural adaptation of the Norwegian versions of the Roland-Morris disability questionnaire and the Oswestry disability index. J Rehabil Med 35:241–247. https://doi.org/10.1080/16501970306094
Pekkanen L, Kautiainen H, Ylinen J et al (2011) Reliability and validity study of the finnish version 2.0 of the oswestry disability index. Spine (Phila Pa 1976) 36:332–338. https://doi.org/10.1097/BRS.0b013e3181cdd702
Miekisiak G, Kollataj M, Dobrogowski J et al (2013) Validation and cross-cultural adaptation of the polish version of the oswestry disability index. Spine (Phila Pa 1976) 38:237–243. https://doi.org/10.1097/BRS.0b013e31827e948b
Mohan V, Prashanth GS, Meravanigi G et al (2016) Adaptation of the Oswestry disability index to Kannada language and evaluation of its validity and reliability. Spine (Phila Pa 1976) 41(11):E674–E680. https://doi.org/10.1097/BRS.0000000000001368
Costa M, Marshman LAG (2015) Sex life and the Oswestry disability index. Spine J 15:1225–1232. https://doi.org/10.1016/j.spinee.2015.02.022
Acknowledgements
No funding has been applied for this study. The study has been approved by the Institutional Review Board of the University of Hong Kong/ Hospital Authority Hong Kong West Cluster (HKU/HA HKW IRB). We would like to present our gratitude to all translators who have participated in the cultural adaptation of the Cantonese (Hong Kong) Oswestry Disability Index version 2.1b (HKCODI). Special thanks to staff of the Occupational Therapy Department, the Duchess of Kent Children’s Hospital at Sandy Bay, for the subject recruitment administration in this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare that are relevant to the content of this article. All authors had no financial or proprietary interests in any material discussed in this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Law, K.K.P., Lee, P.L., Kwan, W.W. et al. Cross-cultural adaptation of Cantonese (Hong Kong) Oswestry Disability Index version 2.1b. Eur Spine J 30, 2670–2679 (2021). https://doi.org/10.1007/s00586-021-06922-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-021-06922-0