Abstract
Background
Acotiamide is widely used to improve symptoms in patients with functional dyspepsia (FD) in multiple large-scale clinical studies, but there are few reports about the drug’s mechanism of action. The aim of this study was to assess the effects of acotiamide on gastric accommodation and gastric emptying, gastrointestinal symptoms, and health-related quality of life (HR-QOL) in a placebo-controlled study.
Methods
We conducted a randomized, double-blind placebo-controlled study. Fifty Japanese FD patients were randomly assigned to either placebo (n = 25) or acotiamide 100 mg × 3/day for 2 weeks (n = 25). At baseline and at 2 weeks of treatment, we evaluated the patients’ gastric motility using scintigraphy to determine the accommodation and emptying values, gastrointestinal symptom rating scale (GSRS), HR-QOL (SF-8), and anxiety and depression scale (HADS).
Results
Four patients failed to complete the medication regimen and were omitted from analysis; data from 24 placebo patients and 22 acotiamide patients were analyzed. Acotiamide significantly increased gastric accommodation compared to the placebo (p = 0.04 vs. p = 0.08; respectively). Acotiamide significantly accelerated gastric emptying (50 % half-emptying time) (p = 0.02 vs. p = 0.59). Acotiamide significantly improved the total GSRS scores compared to placebo (p = 0.0007 vs. p = 0.14). HR-QOL did not differ significantly between the two groups, but acotiamide significantly improved the HADS anxiety score compared to placebo (p = 0.04 vs. p = 0.20).
Conclusions
Our placebo-controlled study demonstrated that acotiamide significantly increased both gastric accommodation and gastric emptying in Japanese FD patients. Acotiamide also improved the patients’ dyspeptic symptoms and anxiety score.
Clinical Trials Registry no: UMIN000013544.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Functional dyspepsia (FD) involves chronical epigastric symptoms that persist in the absence of organic disease [1]. The primary pathologic factors of FD include gastric motility dysfunction, hypersensitivity, and psychosocial factors, and effective treatment requires a thorough understanding of each individual patient’s condition [1–6]. Many large-scale clinical studies have shown that acotiamide hydrochloride trihydrate (acotiamide) provides greater improvement than placebo in FD epigastric symptoms such as postprandial fullness, early satiation, and upper abdominal bloating, and acotiamide has been approved for the treatment of FD in Japan [7–17].
To date, acotiamide-induced improvements in gastric motility have been reported primarily from animal experiments, with little information available regarding the drug’s effects on human gastric motility. In hopes of partially remedying this information deficit, we conducted a placebo-controlled study to assess the effects of acotiamide on gastric accommodation and gastric emptying in Japanese patients with FD as defined by the Rome III classification [1].
Methods
Study design
This randomized, double-blind, placebo-controlled, parallel group study enrolled 50 patients with FD at a single site in Japan. We recruited outpatients with FD-postprandial distress syndrome (PDS) as defined by the Rome III classification who visited our department from April 2014 to June 2015. After written informed consent was obtained from every patient, patients were randomly assigned to receive either 100 mg of acotiamide (25 patients) or placebo (25 patients) three times daily before meals for 2 weeks by drawing lots from a sealed envelope that contained a preassigned random group. The randomization code was concealed until the end of the trial. The placebo consisted of lactose, indistinguishable in appearance from the acotiamide. We performed all experiments in accordance with human ethics regulations (Hyogo College of Medicine: no 1626). This clinical study is registered with the University Hospital Medical Information Network Clinical Trials Registry (Number UMIN000013544). The trial was conducted according to the principles governing human research in the Declaration of Helsinki. All authors had access to the study data, and reviewed and approved the final manuscript.
Patients
The study enrolled 50 patients (13 men and 37 women). Average patient age was 56.3 ± 16.9 years at the start of the study. All patients met the following criteria: outpatients, at least 20 years of age, upper abdominal endoscopy performed within 1 year from consultation to exclude organic disease as a cause of epigastric symptoms, not using prokinetics, antacids drugs, gastric mucosa-protective agents, antidepressants, anti-anxiety drugs, sleep-inducing agents, or antipsychotics. Patients were also excluded, if they had undergone Helicobacter pylori eradication within the last 6 months or were currently under eradication treatment, or if they had a past history of hypersensitivity to acotiamide.
Outcome measures
The primary end point was to compare the effects of acotiamide with those of placebo by evaluating each patient’s gastric motility (gastric accommodation and emptying) based on scintigraphy findings before and after study drug administration in each group. Secondary end points were to evaluate each patient’s dyspeptic symptoms, health related quality of life (HR-QOL) and anxiety, and depression based on the results from questionnaires.
Gastric motility (Scintigraphic procedure)
The subjects fasted for at least 6 h before undergoing gastric scintigraphy. In the sitting position, the subjects consumed a test meal containing 99mTc-labeled tin colloid (37 MBq) within 5 min. The composition of the test meal (retort curry, rice, and processed pork loin; total caloric content, 270.9 kcal; carbohydrate, 45.4 g; protein, 8.8 g; fat, 6.0 g), was almost the same as that of the standard meal recommended by the American Neurogastroenterology and Motility Society and the Society of Nuclear Medicine in 2008 [18]. During scintigraphy, the subjects remained in the sitting position. Using a gamma camera (RC2600i; HITACHI, Tokyo, Japan), we obtained scintigraphic images of the entire stomach in the anteroposterior and posteroanterior positions for 3 min each immediately after consumption of the meal and at 15, 30, 45, 60, 90, and 120 min after the meal. We simultaneously measured gastric accommodation and gastric emptying. In order to evaluate gastric accommodation, we measured the radioactivities of upper part of the stomach just after meal intake, and regarded it as a marker of gastric accommodation. Gastric emptying time was determined as the time required for radioactivity in the entire stomach to reach one half of the initial level, which is called half-emptying time (T1/2).
Questionnaires (Symptoms, QOL, Anxiety and depression)
We evaluated digestive symptoms on the gastrointestinal symptom rating scale (GSRS) in the Japanese edition [19]. The GSRS consists of 15 question items, with each item belonging to one of five lower domains (reflux, abdominal pain, dyspepsia, diarrhea, constipation). Each question is rated on a seven-point Likert scale: 1 means that a digestive symptom does not affect the everyday life of the patient at all, and 7 means that it adversely affects the everyday life of the patient to an extent completely unacceptable to the patient. The mean value for each item was considered to be the lower domain score, and the mean value for all lower domain scores was considered to be the overall score. Regarding the HR-QOL, we used the SF-8 questionnaire [20]. The SF-8 measures eight parameters of health status: physical functioning (PF), role physical (RP), bodily pain (BP), general health (GH), vitality (VT), social functioning (SF), role emotional (RE), and mental health (MH). Physical component summary (PCS) and mental component summary (MCS) were also assessed. We used the HADS (hospital anxiety and depression scale) as our anxiety and depression scale [21]. The HADS consists of seven anxiety questions and seven depression questions, which we used to evaluate the anxiety score, the depression score, and the total score. A high score is considered to indicate a high level of psychological suffering. In this study, we evaluated both items before and after taking the study drug, and compared the effects of acotiamide with those of placebo.
Sample size determination
Sample size was determined by two reports on the effects of acotiamide on gastric motility in humans [7, 8]. Since the proportions of placebo and acotiamide responders for overall treatment effect were expected to be 10 and 45 %, respectively, and the additive effect was expected to be 35 %, a sample size of 50 (25 patients in each arm) was calculated to provide a one-sided level of significance of 5 % and a detection power of 80 %.
Statistical analysis
All results were expressed as mean ± standard deviation (SD). Characteristics of enrolled patients were analyzed by Fisher’s exact test, and only sex was analyzed by Chi-square test. Gastric accommodation and emptying, gastrointestinal symptoms (GSRS), HR-QOL (SF-8) and psychological score (HADS) before and after study drug administration were analyzed by paired t test in the placebo or acotiamide group, respectively. Regarding the data between placebo-pre and acotiamide-pre, statistical differences in both gastric accommodation and emptying were determined using unpaired t test. Statistical significance was defined as a value of p < 0.05.
Results
Enrollment and baseline characteristics of patients
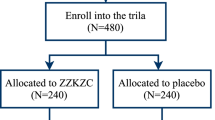
Fifty registered patients were randomized to the acotiamide group (n = 25) or the placebo group (n = 25). In regard to the subtype of FD subjects, we recruited outpatients with PDS subtype. In addition, there was no overlap between EPS subjects and PDS subjects. Four patients that failed to complete the medication regimen were excluded from the full analysis set, leaving 46 patients for consideration; data from 24 placebo patients and 22 acotiamide patients were analyzed. Characteristics of enrolled patients are shown in Table 1. The patient’s flowchart is summarized in Fig. 1.
Effect of acotiamide on gastric accommodation and emptying
There was no significance difference of data between placebo and acotiamide both gastric accommodation and emptying. Acotiamide significantly increased gastric accommodation compared to the placebo (pre 29.6 ± 14.8 %, post 35.1 ± 13.4 %, p = 0.04 vs. pre 38.5 ± 15.1 %, post 35.6 ± 15.0 %, p = 0.08) (Fig. 2). Acotiamide significantly accelerated the gastric emptying (T1/2) (pre 52.3 ± 15.3 min, post 46.9 ± 14.2 min, p = 0.02 vs. pre 52.2 ± 16.3 min, post 51.1 ± 16.8 min, p = 0.6) (Figs. 3, 4).
Change in gastric accommodation pre- and post-dosing in Japanese FD patients. Acotiamide significantly increased gastric accommodation (the radioactivities of upper part of the stomach just after meal intake / the radioactivities of the whole stomach just after meal intake x 100, %) compared to the placebo (pre: 29.6 ± 14.8 %, post: 35.1 ± 13.4 %, p = 0.04 vs. pre: 38.5 ± 15.1 %, post: 35.6 ± 15.0 %, p = 0.08). Box plot represents gastric accommodation before and after study drug administration in the placebo or acotiamide group (placebo group: n = 24, acotiamide group: n = 22), respectively. ‘Boxes’ show 25–75th centiles, with the horizontal line representing the median. ‘Whiskers’ represent the minimum and maximum
Change in gastric emptying pre- and post-dosing in Japanese FD patients. Acotiamide significantly accelerated the gastric emptying (T1/2) (pre: 52.3 ± 15.3 min, post: 46.9 ± 14.2 min, p=0.02 vs. pre: 52.2 ± 16.3 min, post: 51.1 ± 16.8 min, p = 0.59). Box plot represents gastric accommodation before and after study drug administration in the placebo or acotiamide group (placebo group: n = 24, acotiamide group: n = 22), respectively. ‘Boxes’ show 25–75th centiles, with the horizontal line representing the median. ‘Whiskers’ represent the minimum and maximum
Representative picture of gastric scintigraphy of the patient in acotiamide dosing. Radioactivities of the upper part of the stomach were apparently increased after 2 weeks dosing of acotiamide, suggesting that gastric accommodation was clearly improved. Regarding the gastric emptying, the radioactivity of these patients disappeared faster at post-dosing of acotiamide than before medication
Improvement in both gastric accommodation and emptying was noted in 40.9 % (9/22) of the acotiamide group, and improvement in either gastric accommodation or emptying was noted in 86.4 % (19/22) of that group.
Effects of acotiamide on gastrointestinal symptoms
The reflux score on the GSRS questionnaire showed no significant difference before and after study drug administration in the placebo group (pre 2.5 ± 1.3, post 2.1 ± 0.8, p = 0.20). A trend toward improvement in the reflux score was noted in the acotiamide group, with no statistically significant difference before and after study drug administration (pre 2.1 ± 1.0, post 1.8 ± 1.0, p = 0.06).
The abdominal pain score was significantly improved after study drug administration both in the placebo group and the acotiamide group (placebo group: pre 2.4 ± 0.9, post 2.0 ± 0.9, p = 0.04, acotiamide group: pre 2.4 ± 1.3, post 1.8 ± 0.6, p = 0.04).
The GSRS dyspepsia score showed no statistically significant difference before and after study drug administration in the placebo group (pre 2.8 ± 1.1, post 2.5 ± 0.7, p = 0.09), but was significantly improved in the acotiamide group (pre 2.8 ± 0.8, post 2.3 ± 0.8, p = 0.0003).
The total GSRS score showed no statistically significant difference before and after study drug administration in the placebo group (pre: 2.6 ± 0.8, post: 2.3 ± 0.7, p = 0.14), but was significantly improved in the acotiamide group (pre 2.5 ± 0.6, post 2.1 ± 0.6, p = 0.0007) (Table 2).
HR-QOL (SF-8) score
Within the SF-8 score outcomes, PF, RP, BP, VT, SF, RE, MH, PCS, and MCS did not differ significantly between the two groups.
GH showed no statistically significant difference before and after study drug administration in the placebo group (pre 40.6 ± 7.4, post 43.4 ± 7.8, p = 0.07), but was significantly improved in the acotiamide group (pre 42.6 ± 8.6, post 45.3 ± 8.0, p = 0.007).
Psychological score (HADS)
Acotiamide significantly improved the HADS anxiety score compared to placebo (pre 5.4 ± 3.5, post 4.3 ± 2.7, p = 0.04 vs. pre 4.9 ± 3.0, post 4.3 ± 2.8, p = 0.20).
The HADS depression score showed no statistically significant difference before and after study drug administration in either group (placebo group: pre 7.2 ± 4.2, post 7.3 ± 4.2, p = 0.90, acotiamide group: pre 5.3 ± 3.2, post 6.0 ± 2.6, p = 0.05).
No significant difference in the total HADS score before and after study drug administration was noted in either group (placebo group: pre 12.1 ± 5.3, post 11.6 ± 5.3, p = 0.60, acotiamide group: pre 10.7 ± 6.0, post 10.3 ± 4.7, p = 0.50) (Table 3).
Discussion
Acotiamide has been confirmed to improve symptoms of FD patients in multiple large-scaled clinical studies, but there are few reports about the drug’s mechanism of action [7–17]. Therefore, we conducted a randomized, double-blind, placebo-controlled study at a single site to assess the effects of acotiamide on gastric accommodation, gastric emptying, digestive symptoms, HR-QOL, and anxiety. Gastric accommodation and emptying were improved by receiving acotiamide for 2 weeks. Digestive symptoms, especially abdominal pain and dyspepsia, also improved significantly, as did scores on the anxiety scale.
The pathophysiology of FD is still insufficiently characterized, but gastric motility and hypersensitivity have been reported as causes of the primary symptoms [1–4, 22–26]. Previous studies have focused on areas of disturbed gastric motor function such as delayed gastric emptying, impaired gastric accommodation, abnormal intragastric meal distribution, degradation of interdigestive migrating motor complex, and unsuppressed postprandial phasic contractility in the proximal stomach [27–34]. Especially, delayed gastric emptying and impaired gastric accommodation are associated with epigastric symptoms in FD patients.
Acotiamide is classified as prokinetic drug and is known to inhibit acetylcholinesterase (AchE) activity, and, thus, to inhibit the degradation of acetylcholine (Ach) released from the parasympathetic nerve endings and to increase the quantity of Ach in the synaptic cleft [35]. To date, placebo-controlled studies both within and outside Japan have shown beneficial effects of acotiamide for the FD symptoms of upper abdominal bloating and postprandial fullness [7–9]. Several animal studies have shown that acotiamide improves gastric motility, but few human studies have been performed [36–39].
Kusunoki et al. used ultrasonography (US) in humans to investigate the superiority of acotiamide over placebo [7]. Forty-two FD patients who had symptoms of postprandial fullness, upper abdominal bloating, or early satiation were examined by US before and after treatment with acotiamide or placebo. The investigators also used US to assess gastric accommodation reflex and gastroduodenal motility. They reported that the gastric expansion rate increased with greater food intake in the acotiamide group, and that acotiamide expanded the stomachs of the FD patients. There was no significant difference in gastric emptying rate between the two groups. However, when examining the amount of change before and after administration, they reported that the gastric emptying rate increased significantly in the acotiamide group (15.4 vs. 5.3 %). There was no significant change in the placebo group, suggesting that the effects of acotiamide on improving symptoms of FD may result from improving gastric expansion and emptying.
Tack et al. investigated the effect of different doses of acotiamide for gastric emptying by using the 13C octanoic acid breath test in FD patients and comparing with placebo [8]. They reported no difference in gastric emptying time between placebo and acotiamide. These findings differ from the results of our study. This may be due in part to differences in laboratory procedures and test meals, since such factors can greatly affect study results. For example, in their study using US, Kusunoki et al. evaluated gastric motility with a liquid meal and with patients in a face-up position. In the Tack et al. study using a 13C urea breath test, the authors evaluated gastric emptying with a solid meal and with patients in a seated position.
We have focused our attention on gastric scintigraphy, which is considered the gold standard for examination of gastric emptying, and have previously reported that gastric scintigraphy is a useful technique for assessing gastric accommodation and emptying [40]. We used a solid meal and performed our examination with patients in a seated position. This is the first clinical report to describe the effects of acotiamide after eating a solid meal, assessed by gastric scintigraphy, in a double-blind, placebo-controlled, parallel-group study. We evaluated digestive symptoms and gastric motility at the same time. Our results confirmed that acotiamide improved both gastric accommodation and gastric emptying and also improved the GI symptom of dyspepsia. No such improvement was seen in the placebo arm.
In the present evaluation, acotiamide improved two functions of gastric motility in 41 % (9/22) of the patients. Of the nine patients with improved gastric motility, seven patients (77.8 %) showed improvement in the total GSRS score and in dyspeptic symptoms. The mechanism of acotiamide in improving FD symptoms has not yet been clearly characterized. It is impossible to explain the mechanism of the effect of acotiamide from the results of this study alone; however, the data suggests that improvement in gastric motility induced by acotiamide led to improvement in digestive symptoms.
Animal experiments have also reported that acotiamide exhibits a gastrokinetic effect in dogs and rats through its AchE inhibitory action and that acotiamide significantly improves hypomotility of the gastric antrum induced by clonidine, which is an adrenergic α 2 receptor agonist [36, 37]. Interestingly, it has been shown that acotiamide does not accelerate gastric emptying in rats under stress-free conditions but does improve delayed gastric emptying that is induced by restraint stress [39]. This indicates that acotiamide acts on gastric motility as a stress modulator in the medulla oblongata or hypothalamus [41]. Thus, the following two mechanisms may be involved in the mechanism of action of acotiamide: acceleration of Ach release from cholinergic nerve endings and inhibition of Ach hydrolysis, and modulation of the stress response. In this study, depression and anxiety scores were assessed on the HADS. The anxiety score was significantly improved after study drug administration in the acotiamide group; findings did not differ before and after study drug administration in the placebo group. This finding indicates that the direct action of acotiamide may have improved the score, serving as a stress modulator in the medulla oblongata or hypothalamus.
We also evaluated HR-QOL in this study. Decreased QOL has been widely reported in FD patients, and has often been rated with the SF-8, a standard HR-QOL scale that is used worldwide [42]. A score of less than 50 on each item means that the patient has relatively low health perception. In the 46 patients who were included in analysis in this study, the mean score was less than 50 for all of the eight domains and two summary scores, with particularly low scores for GH. Although digestive symptoms were significantly improved in the acotiamide group, the SF-8 subscales showed improvement in HR-QOL only in the GH category. However, PCS was improved in nine (60 %) of the 15 patients who had improved gastric emptying and 11 (84.6 %) of the 13 patients who had improved gastric accommodation in the acotiamide group. Among the nine patients whose gastric accommodation and emptying were both improved, eight patients (88.9 %) showed improvement in PCS.
This study was designed to administer acotiamide for 2 weeks, which was shorter than the duration of administration in previous studies that have reported QOL improvement. Generally, improvement in QOL is delayed compared to improvement in symptoms. The short observation period may have been the reason for no difference in improvement in QOL between the groups.
This study was limited by the fact that it was conducted at a single site. The patients in this study were selected from only those who visited our university hospital, which may have affected the study results.
In conclusion, this was a randomized, double-blind, placebo-controlled, parallel-group comparative study where gastric motility was first evaluated in Japanese FD patients using gastric scintigraphy. Acotiamide significantly increased gastric accommodation and emptying, and improved dyspeptic symptoms and anxiety score. Further investigation with a larger sample size is needed to provide more in-depth analysis.
Change history
25 January 2021
A Correction to this paper has been published: https://doi.org/10.1007/s00535-020-01758-9
Abbreviations
- FD:
-
Functional dyspepsia
- HR-QOL:
-
Health-related quality of life
- GSRS:
-
Gastrointestinal symptom rating scale
- HADS:
-
Anxiety and depression scale
- PDS:
-
Postprandial distress syndrome
- PF:
-
Physical functioning
- RP:
-
Role physical
- BP:
-
Bodily pain
- GH:
-
General health
- VT:
-
Vitality
- SF:
-
Social functioning
- RE:
-
Role emotional
- MH:
-
Mental health
- PCS:
-
Physical component summary
- MCS:
-
Mental component summary
- AchE:
-
Acetylcholinesterase
- Ach:
-
Acethlcholine
- US:
-
Ultrasonography
References
Tack J, Talley NJ, Camilleri M, et al. Functional gastroduodenal disorders. Gastroenterology. 2006;130:1466–79.
Mimidis K, Tack J. Pathogenesis of dyspepsia. Dig Dis. 2008;26:194–202.
Talley NJ, Vakil NB, Moayyedi P. American gastroenterological association technical review on the evaluation of dyspepsia. Gastroenterology. 2005;129:1756–80.
Hammer J, Führer M, Pipal L, et al. Hypersensitivity for capsaicin in patients with functional dyspepsia. Neurogastroenterol Motil. 2008;20:125–33.
Henningsen P, Zimmermann T, Sattel H. Medically unexplained physical symptoms, anxiety, and depression: a meta-analytic review. Psychosom Med. 2003;65:528–33.
Aro P, Talley NJ, Ronkainen J, et al. Anxiety is associated with uninvestigated and functional dyspepsia (Rome III criteria) in a Swedish population-based study. Gastroenterology. 2009;137:94–100.
Kusunoki H, Haruma K, Manabe N, et al. Therapeutic efficacy of acotiamide in patients with functional dyspepsia based on enhanced postprandial gastric accommodation and emptying: randomized controlled study evaluation by real-time ultrasonography. Neurogastroenterol Motil. 2012;24:540–e251.
Tack J, Masclee A, Heading R, et al. A dose-ranging, placebo-controlled, pilot trial of Acotiamide in patients with functional dyspepsia. Neurogastroenterol Motil. 2009;21:272–80.
Matsueda K, Hongo M, Tack J, et al. A placebo-controlled trial of acotiamide for meal-related symptoms of functional dyspepsia. Gut. 2012;61:821–8.
Ueda M, Iwasaki E, Suzuki H. Profile of acotiamide in the treatment of functional dyspepsia. Clin Exp Gastroenterol. 2016;9:83–8.
Matsushita M, Masaoka T, Suzuki H. Emerging treatments in neurogastroenterology: acotiamade, a novel treatment option for functional dyspepsia. Neurogastroenterol Motil. 2016;28:631–8.
Matsueda K, Hongo M, Ushijima S, et al. A long-term study of acotiamide in patients with functional dyspepsia: results from an open-label phase III trial in Japan on efficacy, safety and pattern of administration. Digestion. 2011;84:261–8.
Xiao G, Xie X, Fan J, et al. Efficacy and safety of acotiamide for the treatment of functional dyspepsia: systematic review and meta-analysis. Sci World J. 2014;2014:541950.
Altan E, Masaoka T, Farré R, et al. Acotiamide, a novel gastroprokinetic for the treatment of patients with functional dyspepsia: postprandial distress syndrome. Expert Rev Gastroenterol Hepatol. 2012;6:533–44.
Matsueda K, Hongo M, Tack J, et al. Clinical trial: dose-dependent therapeutic efficacy of acotiamide hydrochloride (Z-338) in patients with functional dyspepsia—100 mg t.i.d. is an optimal dosage. Neurogastroenterol Motil. 2010;22:618–e173.
Tack J, Janssen P. Acotiamide (Z-338, YM443), a new drug for the treatment of functional dyspepsia. Expert Opin Investig Drugs. 2011;20:701–12.
Suzuki H, Hibi T. Acotiamide (Z-338) as a possible candidate for the treatment of functional dyspepsia. Neurogastroenterol Motil. 2010;22:595–9.
Abell TL, Camilleri M, Donohoe K, et al. American Neurogastroenterology and Motility Society and the Society of Nuclear Medicine. Consensus recommendations for gastric emptying scintigraphy: a joint report of the American Neurogastroenterology and Motility Society and the Society of Nuclear Medicine. Am J Gastroenterol. 2008;103:753–63.
Dimenäs E, Glise H, Hallerbäck B, et al. Quality of life in patients with upper gastrointestinal symptoms. An improved evaluation of treatment regimens? Scand J Gastroenterol. 1993;28:681–7.
Turner-Bowker DM, Bayliss MS, Ware JE Jr, et al. Usefulness of the SF-8 health survey for comparing the impact of migraine and other conditions. Qual Life Res. 2003;12:1003–12.
Zigmond AS, Snaith RP. The hospital anxiety and depression scale. Acta Psychiatr Scand. 1983;67:361–70.
Zai H, Kusano M. Investigation of gastric emptying disorders in patients with functional dyspepsia reveals impaired inhibitory gastric emptying regulation in the early postcibal period. Digestion. 2009;79(Suppl 1):13–8.
Azpiroz F, Feinle-Bisset C, Grundy D, et al. Gastric sensitivity and reflexes: basic mechanisms underlying clinical problems. J Gastroenterol. 2014;49:206–18.
Farré R, Vanheel H, Vanuytsel T, et al. In functional dyspepsia, hypersensitivity to postprandial distention correlates with meal-related symptom severity. Gastroenterology. 2013;145:566–73.
Vanheel H, Farré R. Changes in gastrointestinal tract function and structure in functional dyspepsia. Nat Rev Gastroenterol Hepatol. 2013;10:142–9.
Kindt S, Tack J. Impaired gastric accommodation and its role in dyspepsia. Gut. 2006;55:1685–91.
Lee KJ, Kindt S, Tack J. Pathophysiology of functional dyspepsia. Best Pract Res Clin Gastroenterol. 2004;18:707–16.
Tominaga K, Higuchi K, Ochi M, et al. Concurrent assessment of reservoir and emptying of the stomach for dyspepsia patients. Hepatogastroenterology. 2008;55:744–9.
Tack J, Bisschops R. Mechanisms underlying meal-induced symptoms in functional dyspepsia. Gastroenterology. 2004;127:1844–7.
Quartero AO, de Wit NJ, Lodder AC, et al. Disturbed solid-phase gastric emptying in functional dyspepsia: a meta-analysis. Dig Dis Sci. 1998;43:2028–33.
Ahluwalia NK, Thompson DG, Mamtora H, et al. Evaluation of gastric antral motor performance in patients with dysmotility-like dyspepsia using real-time high-resolution ultrasound. Neurogastroenterol Motil. 1996;8:333–8.
Gilja OH, Hausken T, Wilhelmsen I, Berstad A. Impaired accommodation of proximal stomach to a meal in functional dyspepsia. Dig Dis Sci. 1996;41:689–96.
Guo WJ, Yao SK, Zhang YL, Yan J, Yin LJ, Li HL. Relationship between symptoms and gastric emptying of solids in functional dyspepsia. J Int Med Res. 2012;40:1725–34.
Tack J, Talley NJ. Functional dyspepsia–symptoms, definitions and validity of the Rome III criteria. Nat Rev Gastroenterol Hepatol. 2013;10:134–41.
Matsunaga Y, Tanaka T, Saito Y. et al [Pharmacological and clinical profile of acotiamide hydrochloride hydrate (Acofide(®) Tablets 100 mg), a novel therapeutic agent for functional dyspepsia (FD)]. Nihon Yakurigaku Zasshi. 2014;143:84–94.
Kawachi M, Matsunaga Y, Tanaka T, et al. Acotiamide hydrochloride (Z-338) enhances gastric motility and emptying by inhibiting acetylcholinesterase activity in rats. Eur J Pharmacol. 2011;666:218–25.
Nagahama K, Matsunaga Y, Kawachi M, et al. Acotiamide, a new orally active acetylcholinesterase inhibitor, stimulates gastrointestinal motor activity in conscious dogs. Neurogastroenterol Motil. 2012;24:566–74.
Matsunaga Y, Tanaka T, Yoshinaga K, et al. Acotiamide hydrochloride (Z-338), a new selective acetylcholinesterase inhibitor, enhances gastric motility without prolonging QT interval in dogs: comparison with cisapride, itopride, and mosapride. J Pharmacol Exp Ther. 2011;336:791–800.
Seto K, Sasaki T, Katsunuma K, et al. Acotiamide hydrochloride (Z-338), a novel prokinetic agent, restores delayed gastric emptying and feeding inhibition induced by restraint stress in rats. Neurogastroenterol Motil. 2008;20:1051–9.
Tomita T, Okugawa T, Yamasaki T, et al. Use of scintigraphy to evaluate gastric accommodation and emptying: comparison with barostat. J Gastroenterol Hepatol. 2013;28:106–11.
Akaike H, Jang II, Hori N, et al. Effects of Z-338, a novel gastroprokinetic agent, on the actions of excitatory and inhibitory neurotransmitters on neurons in area postrema. J Smooth Muscle Res. 2010;46:31–47.
Kaji M, Fujiwara Y, Shiba M, et al. Prevalence of overlaps between GERD, FD and IBS and impact on health-related quality of life. J Gastroenterol Hepatol. 2010;25:1151–6.
Acknowledgments
Toshihiko Tomita and Hiroto Miwa contributed to the concept and design of the study. Kumiko Nakamura and Toshihiko Tomita were involved in data acquisition and analysis. All authors contributed to data interpretation and critically reviewed the manuscript for important intellectual contents. All authors approved the final version of the manuscript. Tadayuki Oshima provided statistical design. Jiro Watari and Hiroto Miwa coordinated acquisition of data and trial supervision. This study was funded by Astellas Pharma Inc. and Zeria Pharmaceutical Co., Ltd. Tokyo, Japan.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Nakamura, K., Tomita, T., Oshima, T. et al. A double-blind placebo controlled study of acotiamide hydrochloride for efficacy on gastrointestinal motility of patients with functional dyspepsia. J Gastroenterol 52, 602–610 (2017). https://doi.org/10.1007/s00535-016-1260-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-016-1260-7