Abstract
Purpose
To address the gap highlighted in the literature on the effect of professional interventions to facilitate continued employment, this study aims to evaluate the effect of workplace accommodations on the continued employment 5 years after a cancer diagnosis.
Methods
This study is based on VICAN5, a French survey conducted in 2015–2016 to examine the living conditions of cancer survivors 5 years after diagnosis. Two subsamples, one with and one without workplace accommodations, were matched using a propensity score to control for the individual, professional, and medical characteristics potentially associated with receipt of workplace accommodations.
Results
The study sample was composed of 1514 cancer survivors aged 18–54 and employed as salaried at diagnosis. Among them, 61.2% received workplace accommodations within 5 years after diagnosis: 35.5% received a modified workstation, 41.5% received a modified schedule, and 49.2% received reduced hours. After matching, receipt of workplace accommodations appeared to improve the continued employment rate 5 years after cancer diagnosis from 77.8% to 95.0%.
Conclusions
Receipt of workplace accommodations strongly increases the continued employment of cancer survivors 5 years after diagnosis. More research is needed to better understand the differences in receipt of workplace accommodations along with the related selection effect.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
In developed countries, increased early screening and improved treatments have led to a more frequent diagnosis of cancer and to a rise in the number of cancer survivors in working age [1]. Studies have shown that the main indicators of professional life deterioration after cancer diagnosis are lower employment rate, decrease in the likelihood of being employed, and working time reduction [2,3,4,5,6]. In these studies, this effect was found to be socially differentiated: the most vulnerable individuals on the labour market are also the most likely to experience a deterioration of their professional life (especially task performers, temporary contract workers, and the oldest workers). This negative effect stems mostly from damage to physical and psychological health which can have chronic or permanent effects on survivors [5, 7,8,9].
In view of the above, French law encourages employers to effectively redeploy employees diagnosed with cancer and to adjust their workload [10]. However, the implementation of workplace accommodations is not mandatory, and there are no guidelines on how they should be put in place. In the international literature, some studies have identified a positive association between receipt of workplace accommodations after cancer diagnosis and return to work [2, 4, 11,12,13]. However, two systematic reviews analysed studies about interventions made to enhance return-to-work for cancer patients and highlighted the lack of study about the evaluation of professional intervention as workplace accommodation for cancer survivors [14, 15]. The authors conclude on the need to investigate the effect of accommodations made on the professional environment on return to work and continued employment, which has been shown to be positive in the context of other diseases [16, 17]. However, to our knowledge, no international English-written study have investigated the effect of simple accommodation such as reduced hours or working change on return to work of cancer survivors. Yet, while between a quarter and a half of cancer survivors receive workplace accommodations upon returning to work in the French context [11], very few studies have analysed the effect of these accommodations on return to work after cancer diagnosis. To our knowledge, the study by Duguet et al. is the only one that examined this effect in the context of France: It found that men and women who receive workplace accommodations return to work more quickly after sick leave than those who do not [11]. In this study, we aim principally to investigate the effect of workplace accommodations on the continued employment of cancer survivors, 5 years after diagnosis. Then, this study aims secondarily to investigate the effect of workplace accommodations on continued employment of cancer survivors according to their gender on the one hand and their time spent on sick leave on the other hand.
Materials and methods
VICAN5 survey
The VICAN5 national survey was conducted in France to explore the life conditions of individuals aged 18–82, living in metropolitan France, and diagnosed 5 years earlier with a first malignant cancer located in one of 12 common tumour sites, which together account for 88% of global cancer incidence in France [18]. The data collected for VICAN5 came from three sources: (1) a patient questionnaire administered mostly by phone; (2) a medical questionnaire administered to the physician who initiated the cancer treatment; and (3) the medico-administrative databases of the French National Health Insurance Fund known as Système National d’Information Interrégimes de l’Assurance Maladie (SNIIRAM). The patient and medical questionnaires were administered between 2015 and 2016, namely, 5 years after the cancer diagnosis. Finally, the medico-administrative data have been available for the 5 years following diagnosis.
Study population
Only individuals employed at diagnosis (n = 1921) were included in the analysis. Moreover, our study population was restricted to individuals aged under 55 at diagnosis (n = 1690) to ensure that sample participants would be under statutory retirement age (i.e. 60 years in France). Lastly, individuals who did not provide their employment status and those who did not answer the questions about workplace accommodations were excluded from the analysis. Thus, of the 4174 individuals who participated in the VICAN5 survey, 1514 were included in this study.
Main indicators
Occupational status at the survey (yes/no)
This variable indicates if individuals are employed at the time of the survey or not.
Workplace accommodations (yes/no)
In the patient questionnaire, people were asked about if, since the cancer diagnosis, they had a modified work station (yes/no) (e.g. having switched from construction to warehouse work), a modified schedule (yes/no) (e.g. having switched from night to day schedule), or reduced hours (yes/no) (e.g. therapeutic part-time work). Each of these three workplace accommodations was used as one variable. In addition, having received at least one of the workplace accommodations above (yes/no) was also used as a main indicator.
Secondary indicators
Aggregated socio-professional category (task performer/manager)
It provided information on the socio-professional category of the job held at diagnosis. Managers, company directors, and some intermediate professions were grouped together in the “manager” category, while blue collar workers, employees, shopkeepers, craftsmen, and farmers were all classified as “task performers”.
Adverse cancer event (yes/no)
Created from the SNIIRAM databases, it provided information on the evolution of the disease in the 5 years after diagnosis. Individuals presenting metastases or diagnosed with recurrence or a second cancer were considered as having had an adverse cancer event. Individuals treated with chemotherapy, radiotherapy, and/or targeted therapy and those who received palliative care in the 3 years before survey were also considered as having had an adverse cancer event.
Comorbidity score at diagnosis
Continuous variable measured using a score of individual chronic conditions (excluding cancer) based on the SNIIRAM databases [19].
Statistical analyses
Student’s t-tests and Chi-square tests were performed to compare receipt of workplace accommodations according to different individual, professional, and medical characteristics.
Using propensity score matching, two groups of comparable cancer survivors were constituted to measure the effect of workplace accommodations on continued employment: the first group received workplace accommodations (treatment group) and the second did not (control group). The propensity score was estimated from a probit model performed on the probability to receive workplace accommodations after cancer diagnosis according to different explanatory variables (matching variables) [20,21,22]. These explicative variables were defined based on the assumption that they simultaneously affected both the treatment variables and the performance variable. Since we measured the effect of four treatment variables cited below, we performed four different matching.
The performance variable was being employed at the time of the survey (yes/no). Its effect was separately estimated for each following treatment variables: (1) having received a modified work station (yes/no) (e.g. having switched from construction to warehouse work); (2) having received a modified schedule (yes/no) (e.g. having switched from night to day schedule); (3) having received reduced hours (yes/no) (e.g. therapeutic part-time work); and (4) having received at least one of the workplace accommodations above (yes/no). The matching variables were sex (male/female), age at diagnosis (continuous variable ranging from 18 to 54), education level (less than high school/high school degree or more), type of employment contract at diagnosis (permanent/temporary), sector of employment (public/private), company size (microenterprise/other), socio-professional category (task performer/manager), receipt of chemotherapy (yes/no), and comorbidity score at diagnosis (continuous variable).
Based on these variables, individuals in the treatment group were matched with their nearest neighbours in the control group, according to the Caliper method (with a 0.005 threshold) [23]. To obtain a more accurate estimation of the effect of the treatment variables on the performance variable, we used a 95% confidence interval calculated with the bootstrap method. This effect, presented in the Results section, corresponds to the mean of the treatment effects calculated for each 1000 sample replicates [22].
Finally, we performed sensitivity analyses to test the robustness of our results. We began by stratifying samples by sex and by sick leave duration. We then tested the only type of workplace accommodation for which detailed data was available: therapeutic part-time work. Specifically, we sought to determine whether the timing and duration of this specific type of accommodation contributed to continued employment among cancer survivors.
Results
Sample description
The study population was mostly female, as only 19.4% of participants aged 18–54 and employed at diagnosis were men. Mean age was around 44 years old; it was slightly (but significantly) higher for men (45 years old) than for women (44 years old). Half of the sample (55.2%) had a breast cancer, and each other type of cancer represented from 3.2% (lung cancer) to 10.2% (thyroid cancer) of the sample. Furthermore, the majority of survivors employed at diagnosis had a permanent contract (62.4%), held a full-time job (76.3%), and worked in the private sector (74.1%). Half of the study population received chemotherapy (50.9%), and less than one in five (18.4%) had an adverse cancer event within 5 years after diagnosis.
Receipt of workplace accommodations
In our study, three in five (61.2%) cancer survivors received workplace accommodations (modified work station, modified schedule, and/or reduced hours) within 5 years after diagnosis.
Receipt of workplace accommodations was strongly associated with the individual, professional, and medical characteristics listed in Table 1. First, receipt of workplace accommodations varied by sex in favour of female survivors. Second, receipt of workplace accommodations was positively associated with two professional characteristics, namely, company size larger than a microenterprise and permanent contract at diagnosis. Lastly, receipt of workplace accommodations was strongly associated with tumour site and with receipt of chemotherapy, except in the case of modified work stations.
More specifically, 35.5%, 41.5%, and 49.2% of the study population received a modified work station, a modified schedule, and/or reduced hours, respectively. These different types of workplace accommodation were not exclusive: some survivors received two or three types of accommodation, whether simultaneously or not. Among individuals who received at least one type of workplace accommodation, seven in ten (70.3%) received several types of accommodation within 5 years after cancer diagnosis. Half of these (50.8%) received all three types of accommodation and the other half received two out of three. The most common pair was reduced hours and modified schedule. Furthermore, of the three in ten survivors (29.7%) who received only one type of accommodation, 51.1% received reduced hours, 36.1% received a modified work station, and only 12.8% received a modified schedule.
Lastly, the association between receipt of workplace accommodations and individual, professional, and medical characteristics varied by type of workplace accommodation (Table 1).
Continued employment among cancer survivors 5 years after diagnosis and positive effect of workplace accommodations
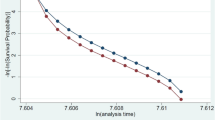
Among the study population, 85.1% was still employed 5 years after cancer diagnosis. Receipt of workplace accommodations was strongly associated with continued employment, as 89.7% of individuals who received workplace accommodations were employed at the time of the survey against 77.8% who were not (odds ratio was estimated at 2.48 with a 95% confidence interval [1.860; 3.305]). This association was observed for each type of workplace accommodation studied (Fig. 1).
As shown in Table 3 presented in supplementary files, the balancing property was satisfied, and data were properly matched. Among comparable cancer survivors, receipt of workplace accommodations significantly increased the continued employment rate 5 years after diagnosis irrespective of the type of accommodation received (Table 2). Receipt of at least one type of workplace accommodation increased the continued employment rate from 77.8% to 95.0%Footnote 1.
The case of therapeutic part-time work
In our study, 27.8% of cancer survivors had their hours temporarily reduced for therapeutic reasons. On average, this hour reduction was granted 17.5 months after diagnosis and lasted 3.9 months. Therapeutic part-time work increases by 9.5 percentage points (SD = 2.8%, p value < 0.001) the probability to be still employed 5 years after cancer diagnosis. Specifically, this type of accommodation increased the continued employment rate from 82.3% to 91.8%.
A positive effect higher for men than for women
Given the high proportion of women in our study population, sensitivity analyses were conducted by stratifying on sex: the effect of receiving at least one type of workplace accommodation on continued employment 5 years after cancer diagnosis was estimated separately for women and for men. It remained unchanged for women: receipt of workplace accommodations increased the continued employment rate from 73.0% to 86.6% (p value < 0.001). The effect was stronger for men: the continued employment rate increased from 64.6% to 80.9% (p value < 0.001). However, given the small number of men in the sample, no clear conclusions could be drawn from the differences observed between men and women.
Receipt of workplace accommodations had a positive effect on cancer survivors who took a short sick leave
We stratified also the sample according to time spent in sick leave within the 5 years following diagnosis: the first subsample was made of individuals who took a long sick leave (1 month or moreFootnote 2) (n = 1263Footnote 3), and the second subsample included individuals who took a short sick leave (less than 1 month) (n = 235). After matching, the effect of workplace accommodations on the continued employment of cancer survivors 5 years after diagnosis was slightly higher in the second subsample (difference of 17.5 points compared to an increase of 9.3 points for the first subsample). This difference was not significant.
Discussion
Our study shows that receipt of workplace accommodations (modified work station, modified schedule, and/or reduced hours) among individuals diagnosed with cancer is far from systematic. Indeed, we found that only six cancer survivors out of ten (61.2%) aged 18–54 and employed at diagnosis received workplace accommodations within 5 years after diagnosis. As receipt of workplace accommodations varied by individual, professional, and medical characteristics, two subsamples (one with and one without workplace accommodations) were matched using a propensity score to estimate the effect of workplace accommodations on the continued employment of cancer survivors 5 years after diagnosis. Among comparable cancer survivors, this effect was positive and estimated at 17.2 percentage points.
Strengths and limitations of the study
This is the first study to explore the effect of workplace accommodations on continued employment in a representative sample of cancer survivors in France. Moreover, VICAN5 is the first survey to provide such a wide range of individual, professional, and medical data on cancer survivors. Our study, however, has some limitations. The first limitation is due to the cross-sectional nature of the data involving that the estimations are all conditional to cancer survival. In the survey, we know nothing about the occupational status and potential arrangements of workstation of people diagnosed with a cancer 5 years before and who died before the survey or were out of sight. In addition, the strong prevalence of breast cancer survivors in our sample (55.2%) could be considered as a limit. This distribution may nevertheless be explained by the epidemiological characteristics of the studied diseases, namely, the high frequency and high survival rate of breast cancer, the low survival rate of lung cancer, and the low frequency of bladder cancer, kidney cancer, and prostate cancer in the age group selected for the study [24]. Furthermore, some individuals may have forgotten that they received workplace accommodations or may have failed to perceive them as such. However, this possibility is unlikely considering the high prevalence of receipt of workplace accommodations in our sample. Finally, although matching by propensity score helped us to control some important confounders to estimate the effect of receiving a workplace accommodation on the continued employment, our findings should be interpreted with caution since the selection effect cannot be completely and perfectly controlled. This would require far more detailed information about occupational and personal conditions that could influence the decision to request or to accept a workplace accommodation (such as the prospects of professional development, both at the individual level and at the company level).
Prevalence of receipt of workplace accommodations
In our study, more than six in ten cancer survivors (61.2%) received at least one of type of workplace accommodation within 5 years after cancer diagnosis: 49.2% received reduced hours, 41.5% received a modified schedule, and 35.5% received a modified work station. These percentages are higher than those reported in similar studies conducted 2 years after diagnosis [25]. By extending the period of observation to 5 years, we were able to study the provision of workplace accommodations to individuals who returned to work after at least 2 years of sick leave [26]. However, we had no information on the timing and duration of workplace accommodations, which means that these could have been implemented any time between diagnosis and survey. We can nevertheless assume that their implementation occurred within 3 years after diagnosis (3 years being the maximum duration of paid sick leave in France). This assumption is supported by the first findings of the VICAN5 survey published by the French National Institute of Cancer: therapeutic part-time work was implemented on average one and a half years after cancer diagnosis (16.8 months, standard deviation: 9 months), which corresponds to the end of the first sick leave [26].
Differences in receipt of workplace accommodations according to medical, individual, and professional characteristics
First, as expected, receipt of workplace accommodations varied by medical characteristics: individuals who were diagnosed with breast cancer, lung cancer, or lymphoma, those who received chemotherapy, those who had an adverse cancer event, and those who had comorbidities before diagnosis were more likely to receive workplace accommodations. This finding supports the hypothesis that workplace accommodations are implemented in order to ensure the continued employment of cancer survivors [13].
Second, receipt of workplace accommodations varied by individual characteristics, as it was systematically more frequent in women than in men. This finding is consistent with the literature [11, 26] and raises questions regarding the pervasiveness of gender representations in the labour market. For instance, is working time reduction more acceptable for female workers than for male workers due to the already high prevalence of part-time work among women? Conversely, are men less likely to reduce their working hours because they are still viewed as the main breadwinner in the household [27]? Or is it due to the intrinsic characteristics of the male occupations that may be less suitable for accommodations? In order to answer these questions, a specific survey including a larger sample of workers is needed. This would allow us to control more precisely the characteristics of the jobs held by men and women.
Third, receipt of workplace accommodations varied by professional characteristics. Cancer survivors who were more likely to receive workplace accommodations had the most favourable professional characteristics. This selection effect may be due to employees who are more likely to remain in the company after cancer diagnosis request workplace accommodations with greater frequency, and, conversely, such employees are more often offered workplace accommodations by their employers. Furthermore, given that workplace accommodations are usually recommended by occupational physicians in France, we can assume that companies that have an occupational health department are more likely to provide workplace accommodations to their employees than those who have not such department. Finally, company policy may have an effect on the continued employment of employee after cancer diagnosis: companies with a high turnover rate may be less likely to provide workplace accommodations to their employees than companies that favour staff stability.
Effect of workplace accommodations on the continued employment of cancer survivors five years after diagnosis
In our study, 85.1% of cancer survivors were still employed 5 years after diagnosis, a rate that is fairly higher than that reported in the first published findings of the VICAN5 survey [26]. This difference can be explained by the fact that 115 individuals who did not answer the questions about workplace accommodations were excluded from our study sample.
After adjusting for medical characteristics (receipt of chemotherapy and comorbidity score at diagnosis), individual characteristics (sex, age at diagnosis, and education level), professional characteristics (type of employment contract at diagnosis, sector of employment, company size and socio-professional category), and receipt of workplace accommodations significantly favoured the continued employment of cancer survivors 5 years after diagnosis. Moreover, additional analyses have shown that the estimated effect increased with the number of accommodations received, but this increase was no significant. The threshold effect was found from receiving at least one accommodation. There are several possible explanations for this positive effect. First, it may be that adapting working conditions to the new physical and psychological capacities of employees helps them cope with the sequelae of cancer in the short term, and thereby reduces both the termination rate and the rate of dismissal due to medical inability. Indeed, survivors who receive workplace accommodations enjoy better working conditions, which in turn encourage them to remain at work. Second, it may be that receipt of workplace accommodations allows for a progressive return to work that is beneficial to long-term health. In fact, even temporary workplace accommodations (such as therapeutic part-time work, which lasts 4 months on average [26]) can be kept in place when they meet the expectations of both employee and employer and can thereby preserve the long-term health of cancer survivors. Conversely, it may be that cancer survivors who do not receive workplace accommodations must work harder to maintain the expected productivity level, which in turn contributes to the deterioration of their physical and psychological health and may drive them to exit the labour market.
Lastly, the effect measured was especially strong in survivors who took a short sick leave or no sick leave at all. In addition to a progressive return to work, they have emerged as a tool to remain at work, combining occupational and medical schedules.
In conclusion, our study suggests that workplace accommodations are an important tool for ensuring the continued employment of cancer survivors, and not just their return to work. The provision of workplace accommodations entails a change in perspective: it is no longer employees who must adapt to the workplace but the workplace that must be adapted to meet the employee needs. In view of these findings, we recommend the systematic provision of workplace accommodations to all workers concerned. Further studies are needed to describe in greater detail the mode of implementation of workplace accommodations as well as the most favourable conditions for this implementation.
Notes
Constructed for each individual from the number of successive days of paid sick leave, as recorded in the SNIIRAM databases. The one-month threshold was selected because employees in France are required to undergo a medical examination with an occupational physician 1 month after the start of sick leave
Individuals for whom this information was not available were excluded from our analyses (n = 16)
References
Colonna M, Mitton N, Bossard N, Belot A, Grosclaude P, The French Network of Cancer Registries (FRANCIM) (2015) Total and partial cancer prevalence in the adult French population in 2008. BMC Cancer ;15. doi:https://doi.org/10.1186/s12885-015-1168-2
Spelten ER, Sprangers MAG, Verbeek JHAM (2002) Factors reported to influence the return to work of cancer survivors: a literature review. Psychooncology 11:124–131
de Boer AGEM, Taskila T, Ojajärvi A, van Dijk FJH, Verbeek JHAM (2009) Cancer survivors and unemployment: a meta-analysis and meta-regression. JAMA 301:753–762. https://doi.org/10.1001/jama.2009.187
Mehnert A (2011) Employment and work-related issues in cancer survivors. Crit Rev Oncol Hematol 77:109–130. https://doi.org/10.1016/j.critrevonc.2010.01.004
Alleaume C, Bendiane M-K, Bouhnik A-D, Rey D, Cortaredona S, Seror V et al (2018) Chronic neuropathic pain negatively associated with employment retention of cancer survivors: evidence from a national French survey. J Cancer Surviv 12:115–126. https://doi.org/10.1007/s11764-017-0650-z
Torp S, Paraponaris A, Van Hoof E, Lindbohm M-L, Tamminga SJ, Alleaume C, et al. (2018) Work-Related Outcomes in Self-Employed Cancer Survivors: A European Multi-country Study. J Occup Rehabil. doi:https://doi.org/10.1007/s10926-018-9792-8
Duijts SFA, van Egmond MP, Spelten E, van Muijen P, Anema JR, van der Beek AJ (2014) Physical and psychosocial problems in Cancer survivors beyond return to work: a systematic review. Psycho-Oncology 23(5):481–492. https://doi.org/10.1002/pon.3467
Green CR, Hart-Johnson T, Loeffler DR (2011) Cancer-related chronic pain. Cancer 117(9):1994–2003. https://doi.org/10.1002/cncr.25761
Wolvers MDJ, Leensen MCJ, Groeneveld IF, Frings-Dresen MHW, De Boer AGEM (2019) Longitudinal associations between fatigue and perceived work ability in Cancer survivors. J Occup Rehabil 29(3):540–549. https://doi.org/10.1007/s10926-018-9814-6
French Law L (2017) 1226–2. Incapacity resulting from a non-occupational illness or accident. Inaptitude consécutive à une maladie ou un accident non professionnel
Duguet E, Clainche CL (2016) Une évaluation de l’impact de l’aménagement des conditions de travail sur la reprise du travail après un cancer. Revue économique 67:49–80. https://doi.org/10.3917/reco.pr2.0053
Tamminga SJ, Boer AGEM (2010) de, Verbeek JH a. M, Frings-Dresen MHW. Return-to-work interventions integrated into cancer care: a systematic review. Occup Environ Med 67:639–648. https://doi.org/10.1136/oem.2009.050070
Lindbohm M-L, Viikari-Juntura E (2010) Cancer survivors’ return to work: importance of work accommodations and collaboration between stakeholders. Occup Environ Med 67:578–579. https://doi.org/10.1136/oem.2009.051847
de Boer AGEM, Taskila TK, Tamminga SJ, Feuerstein M, Frings-Dresen MHW, Verbeek JH (2015) Interventions to enhance return-to-work for cancer patients. Cochrane Database Syst Rev:CD007569. https://doi.org/10.1002/14651858.CD007569.pub3
Caron M, Durand M-J, Tremblay D (2017) Interventions to support the return-to-work process after cancer: a literature review. Sante Publique 29:655–664. https://doi.org/10.3917/spub.175.0655
Franche R-L, Cullen K, Clarke J, Irvin E, Sinclair S, Frank J, The Institute for Work & Health (IWH) Workplace-Based RTW Intervention Literature Review Research Team (2005) Workplace-based return-to-work interventions: a systematic review of the quantitative literature. J Occup Rehabil 15(4):607–631. https://doi.org/10.1007/s10926-005-8038-8
Varekamp I, Verbeek JHAM, van Dijk FJH (2006) How can we help employees with chronic diseases to stay at work? A review of interventions aimed at job retention and based on an empowerment perspective. Int Arch Occup Environ Health 80(2):87–97. https://doi.org/10.1007/s00420-006-0112-9
Bouhnik A-D, Bendiane M-K, Cortaredona S, Sagaon Teyssier L, Rey D, Berenger C et al (2015) The labour market, psychosocial outcomes and health conditions in cancer survivors: protocol for a nationwide longitudinal survey 2 and 5 years after cancer diagnosis (the VICAN survey). BMJ Open 5:e005971–e005971. https://doi.org/10.1136/bmjopen-2014-005971
Cortaredona S, Pambrun E, Verdoux H, Verger P (2017) Comparison of pharmacy-based and diagnosis-based comorbidity measures from medical administrative data: comorbidity measures. Pharmacoepidemiol Drug Saf 26:402–411. https://doi.org/10.1002/pds.4146
Rubin DB (1973) Matching to remove Bias in observational studies. Biometrics 29:159–183. https://doi.org/10.2307/2529684
Rosenbaum PR, Rubin DB (1983) The central role of the propensity score in observational studies for causal effects. Biometrika 70:41–55. https://doi.org/10.1093/biomet/70.1.41
Becker SO, Ichino A (n.d.) Estimation of average treatment effects based on propensity scores. Stata J 2:358–377
Austin PC (2011) Optimal caliper widths for propensity-score matching when estimating differences in means and differences in proportions in observational studies. Pharm Stat 10:150–161. https://doi.org/10.1002/pst.433
INCa (2010) Survie attendue des patients atteints de cancer: état des lieux 2010
INCa (2014) La vie deux ans après un diagnostic de cancer - De l’annonce à l’après-cancer
INCa (2018) La vie cinq ans après un diagnostic de cancer :364
Bodier M, Buisson G, Lapinte A, Robert-Bobée I (2015) Couples et familles - Edition 2015
Acknowledgements
The VICAN5 survey was funded by the National Institute of Cancer (INCa), « Contrat de recherche et développement no. 05-2011 ». The authors would like to thank the French league against cancer (La Ligue contre le cancer) for the doctoral fellowship. Many thanks also go to Asmaa Janah and Sebastien Cortaredona for their precious advice. Thanks also to all the members of the VICAN team. Lastly, the authors thank Arianne Dorval for revising the English manuscript.
Funding
The VICAN survey was funded by the National Institute of Cancer (INCa), « Contrat de recherche et développement No. 05-2011 ». However, this institute did not fund this study. This work was supported by French National Research Agency grant ANR-17-EURE-0020.
Author information
Authors and Affiliations
Contributions
CA and AP designed the study. ADB and MKBD collected the data. CA, AP, and PPW interpreted the data. CA performed data analysis and drafted the manuscript. All authors discussed, revised, and finally approved the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The survey methodology was approved by three national ethics commissions: the CCTIRS (Comité Consultatif sur le Traitement de l’Information en Matière de Recherche dans le Domaine de la Santé, study registered under no 11-143), the ISP (Institute of Public Health, study registered under no C11-63), and the CNIL (French Commission on Individual Data Protection and Public Liberties, study registered under no 911290). Confidentiality is assured for all participants with regard to any personal responses and information provided, as all data collected are anonymized. Results of the study will be disseminated through national and international research conferences and in articles published in international peer-reviewed journals.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 15 kb)
Rights and permissions
About this article
Cite this article
Alleaume, C., Paraponaris, A., Bendiane, MK. et al. The positive effect of workplace accommodations on the continued employment of cancer survivors five years after diagnosis. Support Care Cancer 28, 4435–4443 (2020). https://doi.org/10.1007/s00520-019-05189-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-019-05189-y