Summary
Objective
The purpose of this study is to determine the effectiveness of the diffusion-weighted magnetic resonance imaging (DWI) of the differentiation of benign and malignant testicular masses.
Methods
Fifteen male patients who admitted to our clinic with the diagnosis of testicular mass detected by ultrasound were enrolled to this study. The patients were between 20 and 61 years old (mean 25.7). Apparent diffusion coefficient (ADC) values were measured from ADC maps of lesion and normal testicular tissue. In addition, mean signal intensity (SI) measurements were obtained by using b: 1,000 of normal testicular tissue and lesion with three regions of interest (ROI). SI ratio values are obtained by dividing the value lesion SI to the normal testicular parenchyma SI. Histopathology of orchiectomy materials and ADC values and lesion SI rates were compared statistically.
Results
There were no significant correlation (p = 0.97) between ADC values of benign and malign lesions and histopathological diagnosis in Student’s t test. There were statistically significant relationship with the histopathology of the lesion and the SI ratio in Student’s t test (p = 0.027).
Conclusions
DWI is an effective method in differentiation of benign and malignant testicular masses. Important information can be obtained about nature of testis masses with quantitative measurements of the ADC and ratio of SI.
Zusammenfassung
Ziel
Der Zweck dieser Studie ist es, die Wertigkeit der Diffusions-gewichteten Magnetresonanz Bildgebung (DMB) in der Differenzierung von benignen und malignen Hodentumoren zu erfassen.
Methodik
Fünfzehn Männer, die an unsere Klinik mit im Ultraschall festgestellten Hodentumoren zugewiesen worden waren, wurden in die Studie aufgenommen. Das Alter der Patienten lag zwischen 20 und 61 Jahren (im Mittel 25,7). Apparente Diffusionskoeffizienten (ADK) wurden von Gebieten der Läsion und vom normalen Hodengewebe gemessen. Zusätzlich wurde Messungen der mittleren Signalintensität (SI) von Gebieten der Tumoren mit drei regions of interest (ROI) und vom normalen Hodengewebe durchgeführt. Die SI Quotienten wurden durch Division des SI Werte, die über der Läsion erhoben wurden, durch die im normalen Hodenparenchym gemessenen errechnet. Die Pathohistologie des Orchiektomie Materials wurden mit den ADK sowie mit den Tumor SI Quotienten statistisch verglichen.
Ergebnisse
Im Student’s t-Test bestand keine signifikante Beziehung (p = 0,97) zwischen den ADK Werten und den benignen, beziehungsweise den malignen Tumoren. Die Beziehung zwischen dem pathohistologischem Ergebnis und den SI Quotienten war im Student t-Test signifikant (p = 0,027).
Schlussfolgerungen
Die DMB ist eine Methode, die zur Differenzierung von malignen und benignen Hodentumoren gut geeignet ist. Wichtige Informationen über die Art des Hodentumors können mit quantitativen Messungen der ADK und den SI Quotienten gewonnen worden.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Imaging plays an important role in the differential diagnosis of testicular masses. Ultrasonography (US) is the primary imaging method of choice for the evaluation of testicular pathology, but it remains insufficient in characterizing the tissue [1]. Magnetic resonance imaging (MRI) displays high soft-tissue contrast, is capable of multiplanar cross-sectional imaging, and does not include ionizing radiation. Thus, it is used in differentiating testicular and extratesticular masses, tissue characterization, and screening for metastasis [1].
Diffusion-weighted imaging (DWI) attempts to define tissue characteristics by measuring the microscopic diffusion of water molecule protons. This method was initially used in the diagnosis of central nervous system ischemia, but when it was found that it could help differentiate benign from malignant tissues, it began to be used extensively [2–5]. In this article, we aimed to investigate the value of DWI in the differential diagnosis of testicular neoplasms.
Material and methods
Patients
Between January 2009 and November 2011, 15 male patients who had presented to our clinic with the diagnosis of testicular mass detected by ultrasound were enrolled in this study. The patients were between 20 and 61 years of age (mean 25.7). US examinations were performed with 10–13 MHz linear-array transducers (Logiq 9, GE Healthcare, Milwaukee, WI). The opposite healthy testicular parenchyme or ipsilateral normally appearing testicular tissue was used as the control group.
MRI
Abdominal contrast-enhanced MRI was performed for the investigation of intraabdominal lymph node metastasis with phase-array body coil and surface coils in 1.5 Tesla scanner (Siemens Avanto, Erlangen, Germany). Conventional T1-weighted FS (TR/TE, 363/9.2 ms) and T2-weighted FS (TR/TE, 6,180/64 ms) axial view images were acquired with 5 mm slice thickness, 1 mm intersectional gap, 20–25 cm FOV and matrix of 512 × 512. Contrast-enhanced images were acquired with fat-saturated axial T1-weighted sequences after IV administration of 0.2 mmol/kg gadodiamide (Omniscan, GE, Healthcare). DWI was performed separately for the upper and lower abdomen with 3-directional axial single-shot spin-echo echo planar (4,000/81; echo-planar imaging factor, 77; sensitizing gradients in x, y, and z directions) imagings. The images were acquired with 0, 500, and 1000 mm2/s b values. Apparent diffusion coefficient (ADC) maps were calculated afterwards. Lesion localization was determined using images with low b values at DWI and conventional sequences.
Image analysis
ADC values were measured from the ADC maps with the average of three ROIs (region of interest) with constant area (0.32 cm2) from the lesion and normal testicular tissue. Measurement of the cystic areas, border zones, and areas of calcification were avoided, and solid areas were measured. Furthermore, the mean signal intensity (SI) measurements were obtained by using b: 1,000 mm2/s of normal testicular tissue and lesion with three ROIs. The SI ratio values were obtained by dividing the value lesion SI by the normal testicular parenchyma SI. Measurements were obtained by the codecision of two experienced radiologists from the work station (Leonardo Workstation, Siemens).
Statistical analysis
The histopathology of orchiectomy materials and ADC values and the lesion SI rates were compared statistically. The one-sample Kolmogorov–Smirnov and the Student’s t tests were used for the statistical analysis. A p level of < 0.05 was accepted as statistically significant. The optimal cut-off value was calculated with the receiver operating characteristic (ROC) analysis, and accordingly the sensitivity, specificity, positive predictive value (PPV), negative predictive value (NPV) analyses were performed. The SPSS software was used for the statistical analysis.
Results
Eight (53.3 %) of the masses were on the right side and seven (46.7 %) were on the left. The lesion size varied from 15 to 43 mm with an average of 27.9 mm. The ADC value of normal testicular tissue varied from 0.95 to 1.41 with an average of 1.08 ± 0.06.
In one patient, there were bilateral testicular masses and adrenal hyperplasia. In that particular patient, we diagnosed congenital adrenal hyperplasia and bilateral adrenal rest in the testis with supportive hormone profile, and that patient received medical treatment. The remaining 14 patients underwent orchiectomy. After the histopathological examinations, there were a total of five benign and ten malignant lesions. There were three epidermoid cysts, five seminomas, one leydig cell tumor, four malignant mixed germ cell tumor, one congenital adrenal rest, and one postinfectious granuloma (see Figs. 1, 2, and 3). The ADC value of all lesions varied from 0.56 to 2.48 with an average of 0.93 ± 0.2. The ADC value of benign lesions varied from 0.63 to 1.38 with an average of 0.93. In the malignant lesions, the ADC value varied from 0.56 to 2.48, with an average of 0.94 (Table 1). There was no significant correlation (p = 0.97) between the ADC values of benign and malignant lesions and the histopathological diagnosis in the Student’s t test.
In the case diagnosed with epidermoid cyst histopathologically. a In the T1-weighted MR image, a mass lesion localized at the right testis which demonstrates iso-hypointensity to normal testicular parenchyma. b In the T2-weighted MR image, a smooth-margined hyperintense mass with a hypointense rim is observed. c In the “b: 1,000” DWI, the lesion is observed to be significantly hyperintense. d In the ADC map, when the mass lesion is compared with the left testis, it is hypointense and it demonstrates a diffusion restriction (the average ADC of the lesion is 0.81 × 10-3 mm2/s)
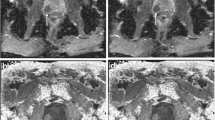
In the case diagnosed with mixed mesenchymal tumor histopathologically. a In the “b: 1,000” DWI, both hypointense and hyperintense focuses are observed. b In the ADC map, the significant differences in the ADC values between the lower and upper parts of the lesion demonstrate that the lesion has a mixed histological structure (the average ADC at the upper part of the lesion is 1.27 × 10-3 mm2/s, and the average ADC at the lower part of the lesion is 2.72 × 10-3 mm2/s)
In the case diagnosed with seminoma histopathologically. a In the T1-weighted MR image, due to the localized mass, an increase in the volume of the right testis is observed. b In the T2-weighted MR image, the lesion is observed to be hypointense in comparison with the normal testicular structure. c In the “b: 1,000” DWI, the inner structure of the lesion has a similar intensity with the normal parenchyma and the hypointensity of its borders can be monitored. d In the ADC map, when the lesion is compared with the normal testicular parenchyma, it is hypointense and it demonstrates a diffusion restriction (the average ADC of the lesion is 0.66 × 10-3 mm2/s)
In b: 1,000 DWI images, the SI value of the lesions was indexed to the normal testicular tissue SI values and compared with the histopathology. The average SI value was 0.65 in the malignant lesions and 1.4 in the benign lesions (Table 2). There was a statistically significant relationship between the histopathology of the lesion and the SI ratio in the Student’s t test (p = 0,027). When we considered the threshold value as 1 for the differentiation of benign and malignanttesticular masses with the SI rate, the sensitivity, specificity, PPV, NPV, and accuracy were 90, 60, 81, 75, and 73 %, respectively in the ROC analysis. The average SI ratio values of the three epidermoid cysts was 1.96 and this was above the threshold values.
Discussion
Radical orchiectomy is the preferred method of treatment for malignant testicular masses. Therefore, in order to prevent unnecessary radical surgery, it is very important to make a distinction between benign and malignant masses. MRI is superior to US, which is the most commonly used imaging modality for evaluation of the scrotum, in differentiating testicular and extratesticular pathologies, multiplanar imaging with high soft-tissue contrast and for demonstrating anatomical details [6–8].
Unlike conventional MRI sequences, DWI provides information about the function of the tissue. This sequence does not require contrast media or expensive and complex hardware. It is not invasive and the scanning time is not prolonged. Therefore, it has begun to be widely used in abdominal diseases [9]. With the help of the new ultrafast sequences in abdominal MRI, movement artifacts have been largely eliminated, and the quality of the images has increased; hence, it has become a commonly used method [10]. DWI has become an oncological imaging modality with short imaging duration, no radiation risk, and a physiological imaging method such as PET/CT [11]. Many specific organ studies such as that on the liver, kidney, and the bladder have been conducted for the effectiveness of DWI in abdominal imaging [3, 9–13]. However, to the best of our knowledge, there is no DWI study in the literature on the differential diagnosis of testicular masses.
In previous studies, the effectiveness of MRI was investigated for the differential diagnosis in testicular neoplasms [1, 8, 14, 15]. In these studies, the signal characteristics, morphology, and enhancement of the mass were evaluated using conventional sequences for the differential diagnosis. Cramer et al. [8] interpreted 54 of 200 cases as malignant in their study according to MRI, which were all confirmed histopathologically [8]. In this study, there were no false-negative or false-positive results. Johnson et al. [16] reported that they accurately differentiated between seminoma and nonseminoma with MRI in 13 of 15 patients (87 %) [16]. Schultz-Lampel et al. [17] were able to separate seminomatous from nonseminomatous in 42 of 67 patients (62 %) [17]. Serra et al. [18] reported that they managed to differentiate malignant lesions from benign masses with 91 % accuracy [18]. Tsili et al. [15] reported that they were able to make the distinction between seminoma and nonseminoma in 19 of 21 (91 %) patients using MRI-enhancement of the features of tumor tissue and the content of fibrovascular septa [15]. They also tried to characterize testicular masses and local spreads preoperatively with MRI and obtained similar results to previous studies [1]. In this study, they evaluated 33 patients with 36 testis masses with a lesion characterization accuracy of 96.4 %.
In our study, we could not make a distinction between benign and malignant lesions according to the ADC values. However, there were epidermoid cysts in the benign lesion group, which were reported to have low ADC values due to restricted diffusion [19]. Therefore, the ADC values of malignant neoplasms and epidermoid cysts may overlap. In our study, the mean ADC value of the epidermoid cysts was 0.75 and the mean ADC value of malignant testicular neoplasms was 0.94. Malignant germ cell tumors were also included in the malignant neoplasms group. In that tumors of two cases, the ADC values were 2.48 and 1.5, respectively. The histopathology of these cases were: 80 % teratoma and 20 % seminoma in the first one and 1 % teratoma , 4 % seminoma, and 95 % yolksac carcinoma in the second one. If we exclude these two tumors from the malignant group, the average ADC value of the malignant tumors was 0.67, which is lower than the ADC value of epidermoid cysts (The mean ADC value is 0.61 in pure seminomas in five patients).
The accuracy of our study was 73 % according to the SI rate. The mean SI value of malignant neoplasms is 0.65, which is significantly lower than benign lesions including all epidermoid cysts. It was possible to distinguish between malignant and benign lesions using the SI rates. The mean SI rates (0.44) were also lower than the cut-off value in malignant mixed germ cell tumor cases which had higher ADC values. The mean SI value in pure seminoma cases was 0.79.
Our study had some limitations. One of them was the number of benign lesions and their diversity. The other was the epidermoid cyst in the benign group which displayed diffusion restriction and had overlapping ADC values with malignant lesions. However, we think that epidermoid cysts can be distinguished from other benign testicular masses with the help of conventional MRI sequences. Therefore, except for the epidermoid cyst, it will not be difficult to differentiate benign lesions from malignant lesions using DWI.
On conclusion, DWI is an effective method in the differentiation of benign and malignant testicular masses with a short examination duration.
References
Tsili AC, Argyropoulou MI, Giannakis D, Sofikitis N, Tsampoulas K. MRI in the characterization and local staging of testicular neoplasms. Am J Roentgenol. 2010;194(3):682–9.
Sonmez G, Cuce F, Mutlu H, et al. Value of diffusion-weighted MRI in the differentiation of benign and malign breast lesions. Wien Klin Wochenschr. 2011;123(21–22):655–61.
Sonmez G, Sivrioglu AK, Mutlu H, et al. Is it possible to differentiate between hydatid and simple cysts in the liver by means of diffusion-weighted magnetic resonance imaging? Clin Imaging. 2012;36(1):41–5.
Mutlu H, Sivrioglu AK, Sonmez G, et al. Role of apparent diffusion coefficient values and diffusion-weighted magnetic resonance imaging in differentiation between benign and malignant thyroid nodules. Clin Imaging. 2012;36(1):1–7.
Satoh S, Kitazume Y, Ohdama S, Kimula Y, Taura S, Endo Y. Can malignant and benign pulmonary nodules be differentiated with diffusion-weighted MRI? Am J Roentgenol. 2008;191(2):464–70.
Thurnher S, Hricak H, Carroll PR, Pobiel RS, Filly RA. Imaging the testis: comparison between MR imaging and US. Radiology. 1988;167(3):631–6.
Akbar SA, Sayyed TA, Jafri SZ, Hasteh F, Neill JS. Multimodality imaging of paratesticular neoplasms and their rare mimics. Radiographics. 2003;23(6):1461–76.
Cramer BM, Schlegel EA, Thueroff JW. MR imaging in the differential diagnosis of scrotal and testicular disease. Radiographics. 1991;11(1):9–21.
Sugita R, Ito K, Fujita N, Takahashi S. Diffusion-weighted MRI in abdominal oncology: clinical applications. World J Gastroenterol. 2010;16(7):832–6.
Avcu S, Koseoglu MN, Ceylan K, Bulut MD, Unal O. The value of diffusion-weighted MRI in the diagnosis of malignant and benign urinary bladder lesions. Br J Radiol. 2011;84(1006):875–82.
Kwee TC, Takahara T, Ochiai R, et al. Complementary roles of whole-body diffusion-weighted MRI and 18F-FDG PET: the state of the art and potential applications. J Nucl Med. 2010;51:1549–58.
Kim T, Murakami T, Takahashi S, Hori M, Tsuda K, Nakamura H. Diffusion-weighted single-shot echoplanar MR imaging for liver disease. Am J Roentgenol. 1999;173(2):393–8.
Yamada I, Aung W, Himeno Y, Nakagawa T, Shibuya H. Diffusion coefficients in abdominal organs and hepatic lesions: evaluation with intravoxel incoherent motion echo-planar MR imaging. Radiology. 1999;210(3):617–23.
Sohaib SA, Koh DM, Husband JE. The role of imaging in the diagnosis, staging, and management of testicular cancer. Am J Roentgenol. 2008;191(2):387–95.
Tsili AC, Tsampoulas C, Giannakopoulos X, et al. MRI in the histologic characterization of testicular neoplasms. Am J Roentgenol. 2007;189(6):331–7.
Johnson JO, Mattrey RF, Phillipson J. Differentiation of seminomatous from nonseminomatous testicular tumors with MR imaging. Am J Roentgenol. 1990;154(3):539–43.
Schultz-Lampel D, Bogaert G, Thüroff JW, Schlegel E, Cramer B. MRI for evaluation of scrotal pathology. Urol Res. 1991;19(5):289–92.
Serra AD, Hricak H, Coakley FV, et al. Inconclusive clinical and ultrasound evaluation of the scrotum: impact of magnetic resonance imaging on patient management and cost. Urology. 1998;51(6):1018–21.
Langer JE, Ramchandani P, Siegelman ES, Banner MP. Epidermoid cysts of the testicle: sonographic and MR imaging features. Am J Roentgenol. 1999;173(5):1295–9.
Conflict of interest
The authors declare that there is no conflict of interest in relation to this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sonmez, G., Sivrioglu, A., Velioglu, M. et al. Optimized imaging techniques for testicular masses: fast and with high accuracy. Wien Klin Wochenschr 124, 704–708 (2012). https://doi.org/10.1007/s00508-012-0233-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00508-012-0233-y
Schlüsselwörter
- Apparente Diffusionskoeffizienten
- Diffusionsgewichtete Magnetresonanz
- Signalintensität
- Hoden
- Hodentumore