Abstract
The International Reflux Study in Children was set up to compare prospectively the outcome of medical or surgical management of children with grade III or IV vesicoureteral reflux and a history of symptomatic urinary tract infection. Development of new radiological scars was the main end point. Of the 306 children randomized, 302 (153 medical, 149 surgical) were available for radiological follow-up at 5 years. New scars had developed in 19 medically and 21 surgically treated children. Among 223 patients (113 medical, 110 surgical) who continued follow-up with urography at 10 years, only 2 further new scars developed. Overall, 47 new scars were acquired in 42 patients (20 medical, 22 surgical), 25 of them in children with unscarred kidneys at entry (13 medical, 12 surgical). New scars occurred mostly in children under 5 years of age and were observed more frequently in children with grade IV than grade III reflux. We conclude that with careful management, only a small proportion of children with severe reflux developed new scars and rarely after the first 5-year follow up period, and that there was no difference between children treated medically or surgically.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The International Reflux Study in Children (IRSC) was designed to determine whether medical or surgical treatment is more effective in protecting children with grade III or IV vesicoureteral reflux (VUR) from renal damage. The development of new renal scars was defined as a main end point. At 5 years, a similar number of patients developed new radiological scars on serial intravenous urography (IVU) in the two treatment groups of both the United States branch (132 children) [1] and the European branch (306 children) [2, 3] of the study.
After completing the 5-year study, five of the eight original European participating centers agreed to extend the follow-up with clinical observation and an additional IVU at 10 years. The radiological results are reported in the 302 children who entered the study and were followed for more than 6 months, and in 223 children (113 medical, 110 surgical) who were followed radiologically for 10 years.
Patients and methods
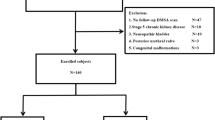
The entry characteristics, exclusion factors, and management of children who entered the European limb of the IRSC have been reported [2, 3]. The children were under 11 years of age with grade III or IV VUR [4], without outflow obstruction, with a history of symptomatic urinary tract infection (UTI), and with a glomerular filtration rate ≥70 ml/min per 1.73 m2.
The methods have been fully described previously [2, 3, 5]. Serial IVU was performed using a standardized technique [5]. All IVU was evaluated by at least three experts blinded as to treatment; serial IVU was examined in each child without the corresponding cystograms. The renal parenchymal thickness was measured in the upper and lower poles and lateral zone, and the parenchymal area by planimetry. The results were expressed as the standard deviation score derived from a nomogram relating the measurements to the height of L1-L3 [6].
A radiological renal scar was defined as a calyceal deformity together with thinning of the overlying parenchyma [7]. Renal scars were typed according to Smellie et al. [8]: A with one or two scars, B affecting more than two areas but with some normal parenchyma remaining, C generalized irregular parenchymal reduction and calyceal deformity, and D small end-stage kidney.
In 4 (2 medical, 2 surgical) of the 306 patients reported previously [2, 3], IVU was not performed after 6 months from entry. They are omitted from this report.
Parallel 99mTc-dimercaptosuccinic acid (DMSA) imaging studies were also carried out [9] and will be reported separately. This paper reports the radiological findings.
Clinical follow-up was continued up to 10 years in 252 children. The final outcome will be published separately. There was no difference in entry characteristics between the treatment groups among the 302 children who completed 5 years and the 223 who had an IVU at 10 years (Table 1) or the 29 patients with only a 10-year clinical follow-up (12 medical, 17 surgical). Among the 302 children, 155 (51%) had unscarred kidneys at entry and 147 had established scars, 102 (34%) unilateral and 45 (15%) bilateral, with similar proportions among the 223 followed for 10 years. The proportions of children with different severity of scarring were similar in those managed medically and surgically (Table 1).
Cohen and Politano-Leadbetter were the main surgical techniques used [10]. Low-dose antibacterial prophylaxis with nitrofurantoin or trimethoprim (alone or in combination with sulfonamide) was continued for 6 months after successful surgery, or in the medical group until VUR had resolved or improved to grade I. If kidneys were unscarred, prophylaxis was usually discontinued at the age of 8 years. Regular complete voiding, double micturition at bedtime, and regular bowel action were also recommended. At 5 years, VUR with dilatation was seen in 57 (56%) of 102 children managed on a medical regimen, but at 10 years this was reduced to 27 (26%) [11].
Statistical methods
The computer software used for analysis was SAS for PC, version 8 (SAS Institute, Cary, N.C., USA). Statistical methods have been described previously [5, 10]. The outcome was analyzed according to ‘intention to treat’. A life-table analysis and generalized rank test of Gehan-Wilcoxon was performed to compare both groups in the primary outcome of exponential distributed events of renal scars. Because of successfully completed stratified randomization, it was not necessary to take any co-variable into account.
The study protocol was approved in accordance with the standards in the declaration of Helsinki by the local ethics committee of each participating hospital and by the External Monitoring Committee of the Study.
Results
During the first 5-year period, 40 children developed new radiological scars, 19 medical (23 kidneys) and 21 surgical (22 kidneys) (1 patient was reported late) [2, 3]. Of these children, 28 were among the 223 followed radiologically for 10 years (14 medical, 14 surgical).
Between 5 and 10 years’ follow-up, only 2 new scars developed among 223 patients, both in girls (1 medical, 1 surgical):
- (a):
-
A girl entered aged 3.8 years with left grade IV VUR and unscarred kidneys, managed medically. At 5 years, her IVU remained normal, VUR had improved, and was absent at 10 years. No further UTI was recorded during follow-up, but her 10-year IVU at 14 years of age showed a type A scar in the left upper pole. The DMSA study showed a new image defect.
- (b):
-
A girl entered aged 4.3 years with a history of recurrent UTI, bilateral VUR, right grade II, left grade IV, and bilateral renal scarring types A and B. Left ureteral reimplantation was successful. A febrile UTI occurred 18 months later, but thereafter no further UTI was reported. IVU was unchanged at 5 years, there was no VUR at 10 years, but the final IVU (aged 17 years) showed a further single left renal scar developing in a normal area of the scarred kidney. No new image defect was seen on the DMSA scintigraphy, but there was a reduction in the proportionate function from 33% to 28%.
Of 155 children who had unscarred kidneys at entry, 25 (16%) (12 medical, 13 surgical) developed new scars. In 17 children (8 medical, 9 surgical), scars developed in new areas of previously scarred kidneys (12% of 147). The type of the new scars is shown in Table 2. Of the 47 new scars, 25 (53%) were of type A. The type C scars in the surgical group were all left-sided and related to postoperative obstruction in 5 of the 7 children. One medically treated boy developed bilateral type C scars. In 8 of the 25 children who developed new radiological scars in kidneys that were normal on IVU at entry, the DMSA image at entry was already abnormal. New scars were observed more frequently in children with grade IV reflux, 38 of 248 (15%), compared with grade III reflux, 4 of 54 (7%, P<0.05).
Table 3 indicates the age at entry of children developing new scars in each treatment group, and the age at which the new scars were detected. More new scars developed among children under 5 years of age (in 31 of 42 children), with similar numbers in each treatment group. New scars were observed in 14 boys, 12 of them <2 years of age at entry, and in 28 girls, 11 of them <2 years of age at entry.
The timing of the observation of new scars is demonstrated on the Kaplan-Meier curves (Fig. 1). New scars were detected sooner after entry among surgically than medically treated patients, but this difference was not significant (P=0.57, log-rank test).
Discussion
In this multicenter study comparing medical and surgical management of a large number of children with grade III or IV VUR and a history of symptomatic UTI, there was no difference after 5 years in the numbers of patients acquiring new radiological scars between the two treatment groups among 306 patients randomized [2, 3]. This has been the experience of others conducting similar studies over 5 years [1, 12, 13]. However, in few other studies has careful observation continued for 10 years [14]. In the large international trial reported here, only 2 further patients acquired new scars between 5 and 10 years of follow-up, 1 in each treatment group, 1 in a previously normal kidney and 1 in a kidney with already established scarring.
Although not statistically significant, new scars tended to be observed earlier in the surgical than in the medical group. Seven surgical patients, including 3 boys under 2 years of age, developed type C scars compared with 1 medically treated child. However, in both treatment groups most new scars developed under the age of 5 years.
Recent studies on familial reflux have indicated the genetic factors that may predispose to VUR [15]. Permanent renal damage may be present at birth, particularly in infant boys, and is usually associated with severe VUR [16]. This needs to be differentiated from acquired damage that is seen more often in girls who are more prone to recurrent UTI [17, 18, 19]. However, it has not usually been possible on DMSA studies to differentiate between congenital and acquired damage without serial investigations, since it is difficult to distinguish between acute uptake defects caused by inflammation and established permanent damage. In the study reported here, based on good-quality serial IVU, it has been possible to identify change from structurally normal unscarred kidneys to scarred kidneys. These changes have been seen in similar proportions in the two treatment groups over a period of 10 years. New scars were observed especially in the younger children, and it should be noted that such scars were also found in 14 boys, 12 of whom were <2 years of age at entry. It is of interest that 8 patients who entered the study with unscarred kidneys on IVU but abnormal DMSA images subsequently showed a new radiological scar at the corresponding site.
Some variations in renal morphology and areas of thinned parenchyma were observed during serial prospective radiological follow up. These have been documented and discussed [2]. However, the IRSC study was carried out according to a protocol aimed at determining the outcome of two methods of treatment based on the development of well-defined new scars, but was not designed to examine the pathogenesis of such scarring. At the end of 10 years there was no difference between the treatment groups in the acquisition of new scars.
References
Weiss R, Duckett J, Spitzer A (1992) Results of a randomised clinical trial of medical versus surgical management of infants and children with grades III and IV primary vesicoureteral reflux (United States). J Urol 148:1667–1673
Olbing H, Claesson I, Ebel KD, Seppänen U, Smellie JM, Tamminen-Möbius T, Wikstad I (1992) Renal scars and parenchymal thinning in children with vesicoureteral reflux: a 5-year report of the International Reflux Study in Children (European branch). J Urol 148:1653–1656
Smellie JM, Tamminen-Möbius T, Olbing H, Claesson I, Wikstad I, Jodal U, Seppänen U (1992) Five-year study of medical and surgical treatment in children with severe reflux: radiological renal findings. Pediatr Nephrol 6:223–230
Lebowitz RL, Olbing H, Parkkulainen KV, Smellie JM, Tamminen-Möbius T (1985) International system of radiographic grading of vesico-ureteric reflux. Pediatr Radiol 15:154–162
Olbing H, Hirche H, Koskimies O, Lax-Gross H, Seppänen U, Smellie JM, Tamminen-Möbius T, Wikstad I (2000) Renal growth in children with severe vesicoureteral reflux: 10-year prospective study of medical and surgical treatment. Radiology 216:731–737
Claesson I, Jacobsson B, Olsson T, Ringertz H (1981) Assessment of renal parenchymal thickness in normal children. Acta Radiol Diagn (Stockh) 22:305–314
Hodson CJ (1959) The radiological diagnosis of pyelonephritis. Proc R Soc Med 52:669–672
Smellie JM, Edwards D, Hunter N, Normand ICS, Prescod N (1975) Vesicoureteric reflux and renal scarring. Kidney Int 8:S65–S72
Piepsz A, Tamminen-Möbius T, Reiners C, Heikkilä J, Kivisaari A, Nilsson NJ, Risdon RA, Smellie JM, Söderborg B (1998) Five-year study of medical and surgical treatment in children with severe vesico-ureteral reflux—dimercaptosuccinic acid findings. Eur J Pediatr 157:753–758
Hjälmås K, Löhr G, Tamminen-Möbius T, Seppänen J, Olbing H, Wikström S (1992) Surgical results in the international reflux study in children (Europe). J Urol 148:1657–1661
Smellie JM, Jodal U, Lax H, Tamminen-Möbius T, Hirche H, Olbing H (2001) Outcome at 10 years of severe vesicoureteric reflux managed medically: report of the international reflux study in children. J Pediatr 139:656–663
Birmingham Reflux Study Group (1983) Prospective trial of operative versus non-operative treatment of severe vesicoureteral reflux—2-years’ observation in 96 children. BMJ 287:171–174
Birmingham Reflux Study Group (1987) Prospective trial of operative versus non-operative treatment of severe vesicoureteral reflux—5-years’ observation. BMJ 295:237–241
Smellie JM, Barratt TM, Chantler C, Gordon I, Prescod N, Ransley PG, Woolf AS (2001) Medical versus surgical treatment in children with severe bilateral vesicoureteric reflux and bilateral nephropathy: a randomised trial. Lancet 357:1329–1333
Feather SA, Malcolm S, Woolf AS, Wright V, Blaydon D, Reid CJ, Flinter FA, Proesmans W, Devriendt K, Carter J, Warwicker P, Goodship TH, Goodship JA (2000) Primary, nonsyndromic vesicoureteric reflux and its nephropathy is genetically heterogeneous, with a locus on chromosome 1. Am J Hum Genet 66:1420–1425
Risdon RA, Yeung CK, Ransley PG (1993) Reflux nephropathy in children submitted to unilateral nephrectomy: a clinico-pathological study. Clin Nephrol 40:308–314
Clarke SE, Smellie JM, Prescod N, Gurney S, West DJ (1996) Technetium-99m-DMSA studies in pediatric urinary infection. J Nucl Med 37:823–828
Wennerström M, Hansson S, Jodal U, Stokland E (2000) Primary and acquired scarring in boys and girls with urinary tract infection. J Pediatr 136:30–34
Smellie JM, Ransley PG, Normand ICS, Prescod N, Edwards D (1985) Development of new renal scars: a collaborative study. BMJ 290:1957–1960
Acknowledgements
This study was supported by the VW Foundation (grants AZ 35 807 and AZ I/37 504) and by the Government of the Federal Republic of Germany (Bundesministerium für Forschung und Technologie, grant 07068343; Bundesministerium für Wissenschaft und Forschung, grants 07 06570/0 GFF and 01 EP 95084/4 DLR). We are grateful to Frau Monica Höhnke and Mrs. Jan Port for secretarial help.
Author information
Authors and Affiliations
Corresponding author
Additional information
The authors are the writing committee of the European arm of the International Reflux Study in Children. H. Olbing is deceased. Co-ordinating center, Essen, Germany: chairman H. Olbing, scientific co-ordinator T. Tamminen-Möbius, statistics H. Hirche, documentation H. Lax. Participating university hospitals and investigators: Bonn, Germany: R. Mallmann, D. Emons; Brussels, Belgium: M. Hall, A. Piepsz, C. Schulmann; Essen, Germany: H.J. Bachmann, W. Rascher, E. Brunier, C. Reiners, J. Behrendt, P. Mellin (deceased); Gothenburg, Sweden: U. Jodal, K. Hjälmås, E. Hanson, N. Nilsson, J. Bjure (deceased), R. Sixt; Hamburg, Germany: R. Busch, C. Montz; Helsinki, Finland: O. Koskimies, S. Wikström, E. Marttinen, A. Kivisaari, T. Korppi-Tommola; Oulu, Finland: J. Seppänen (deceased), N.P. Huttunen, U. Seppänen, J. Heikkilä; Stockholm, Sweden: A. Aperia, G. Löhr, P. Herin, U. Freyschuss, L. Blom, U. Erasmi, B. Söderborg. Consultants: I. Claesson, K.-D. Ebel, R.A. Lebowitz, K. Parkkulainen, J.M. Smellie, I. Wikstad, and J. Winberg (deceased)
Rights and permissions
About this article
Cite this article
Olbing, H., Smellie, J.M., Jodal, U. et al. New renal scars in children with severe VUR: a 10-year study of randomized treatment. Pediatr Nephrol 18, 1128–1131 (2003). https://doi.org/10.1007/s00467-003-1256-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-003-1256-4