Abstract
Background
Choledochal cysts (CC) are a cystic dilation of the intra- or extrahepatic biliary tree. They are rare, and are associated with a risk of malignant transformation. Due to the close proximity to the pancreas, Type II CC, in which a diverticular outpouching is connected to the extrahepatic bile duct via a narrow stalk, can be difficult to differentiate from pancreatic cysts. The aim of this study was to determine the role of endoscopic ultrasound (EUS) in the diagnosis of Type II CC.
Methods
A retrospective review of all patients seen in the Multidisciplinary Pancreatic Cyst Clinic at Johns Hopkins Hospital from November 2010 to March 2014 was performed to identify patients classified as having Type II CC on computed tomography (CT) or magnetic resonance imaging (MRI) who also underwent EUS. Patient demographics, clinical presentation, imaging, and follow-up were recorded.
Results
Four female patients with median age of 52 years, three of whom were identified as having Type II CC and one as equivocal for CC on MRI, and two as having Type II CC, one equivocal for CC and one as branch-duct intraductal papillary mucinous neoplasm on CT. On EUS, no communication was seen in any cases between the CC and common bile duct. EUS-guided fluid aspiration from each cyst demonstrated clear fluid with undetectable bilirubin and either elevated CEA or amylase confirming the diagnosis of pancreatic cyst.
Conclusions
EUS is a useful tool for the differentiation of equivocal cases of CC. It can show a very small separation as little as 1 mm between two structures, and cyst fluid analysis can be performed and used to further differentiate between biliary cysts and other cystic structures.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
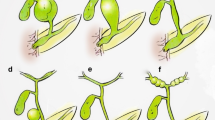
Choledochal cysts (CC) are cystic dilation of the intrahepatic or extrahepatic biliary tree. They are classified into five different subtypes based on their location and distribution within the biliary tree [1]. Type I is a dilation of the common bile duct (CBD); Type II, is a diverticular outpouching from the CBD; Type III is a cystic dilation of the distal CBD within the ampulla of Vater; Type IV consists of multiple dilations involving the intrahepatic and/or extrahepatic biliary tree; and Type V (Caroli’s disease) is cystic dilation confined to the intrahepatic biliary tree (Fig. 1).
CC are rare, with a worldwide incidence of 1 in 100,000 to 1 in 150,000 [1]. Historically, they frequently presented in children with jaundice, right upper quadrant pain and an abdominal mass. However, recent studies have shown a higher prevalence among adults whose only presenting symptom is abdominal pain [2]. One of the most feared complications of CC is cholangiocarcinoma, with an incidence of 6–11 % [2–4]. Given the risk of malignant transformation, surgical resection is recommended for patients with Type I, II, and IV CC [5].
Computed tomography (CT)/computed tomography cholangiography (CTC) and magnetic resonance imaging (MRI)/magnetic resonance cholangiopancreatography (MRCP) are most frequently used to identify CC, with very high sensitivities of 90–100 % reported [6, 7]. However, Type II CC, where a diverticular outpouching is connected to the extrahepatic bile duct via a narrow stalk, can be difficult to differentiate from pancreatic cysts within the head of the pancreas which lie close to the intrapancreatic portion of the bile duct. The aim of this study was to determine the role of endoscopic ultrasound (EUS) in the diagnosis of Type II CC.
Materials and methods
Clinical and radiological data were prospectively collected on patients who attend the Multidisciplinary Pancreatic Cyst Clinic and entered into a database [8]. A retrospective review of data collected from November 2010 to March 2014 was performed to identify patients classified as having Type II CC on either CT or MRI/MRCP, who also underwent EUS. Patient demographics, clinical presentation, imaging, and follow-up were recorded. Ethical approval for this study was obtained from the Institutional Review Board for Human Research and the study complied with Health Insurance Portability and Accountability Act (HIPAA) regulations.
Results
There were 822 patients seen in the Multidisciplinary Pancreatic Cyst Clinic from November 2010 to March 2014; 564 patients underwent EUS and CT or MRI. We identified four patients in whom the initial diagnosis of Type II CC was made on either CT or MRI/MRCP and an alternate diagnosis was made based on EUS. All four patients were female with a median age of 52 (range 31–65) years. Two presented with right upper quadrant pain and the other two were asymptomatic (Table 1); all four patients underwent CT, MRI/MRCP, and EUS. MRI/MRCP classified three cysts as Type II CC, and as equivocal in one case, while CT identified two cysts as a Type II CC, one as equivocal for Type II CC and one as a branch-duct intraductal papillary mucinous neoplasm (BD-IPMN) (Video 1). On EUS there was no communication identified between the cysts and the extrahepatic bile duct (Video 2), suggesting that these cysts were pancreatic, rather than biliary in origin in all four patients. EUS-guided fine needle aspiration (EUS-FNA) was performed in all cases, and revealed clear fluid with no evidence of bile staining consistent with a non-biliary origin. In addition, in one case bilirubin level was tested and was undetectable. Cyst fluid analysis (Table 1) showed a CEA <0.5 ng/mL, consistent with a serous cystadenoma in two cases [9]. The two other cases were diagnosed as BD-IPMN based on either a cyst fluid CEA >192 ng/mL or the presence of mucin on cytology [10]. One patient underwent surveillance with no change in the cyst size or features over a 3 year period and another had an increase in cyst size over a year period but no evidence of malignancy on repeat EUS-FNA. The other two patients were followed locally.
Discussion
EUS can help confirm the presence of a choledochal cyst by identifying a long common pancreaticobiliary channel [11, 12]. However, to our knowledge, this is the first study to highlight the role of EUS in discriminating Type II CC from pancreatic cysts. This differentiation is critical, as the management of pancreatic cysts is often entirely different to CC. Two of the cysts in this series were serous cystadenomas, which have a very low risk of malignant transformation of less than 1.5 %, with surgery only performed in symptomatic patients, or when differentiation from a mucinous cyst with concerning features is not possible [13, 14]. The other two cysts were BD-IPMNs which have the potential to progress to high-grade dysplasia or invasive adenocarcinoma; however that risk is small, and in the absence of any worrisome or suspicious features, international consensus guidelines recommend surveillance of the cysts [15]. In contrast, surgery is recommended for all patients with Type II CC due to the risk of cholangiocarcinoma, which occurs in 6–11 % of patients [2–4]. Thus, differentiating CC from pancreatic cysts is critical to identify those patients with CC in whom surgical resection is recommended, from patients with pancreatic cysts in whom surveillance is appropriate.
Studies have shown MRI/MRCP as the best test to identify CC with sensitivities of 96–100 % [6, 7, 16]; however, it is less accurate at detecting an aberrant pancreaticobiliary junction, one of the hallmarks of CC, with sensitivities as low as 53 % reported [7]. This may be because despite its high resolution, the images are static. In addition, image quality can be impaired if patients are unable to perform breath holding. EUS has been shown to be superior to MRI and CT for the identification of small pancreaticobiliary lesions [17]. It is particularly good at visualizing the distal bile duct, and is superior to MRI for the identification of small (<5 mm) CBD stones [18]. This may be due to visualization of lesions as small as 2 mm. In addition, EUS images are dynamic and allow better visualization of the presence or absence of a small communication between the cyst and CBD (Video 2). Furthermore, EUS-FNA can be performed which allows assessment of cyst fluid. Bile duct fluid can easily be differentiated from pancreatic juice based on its color (Video 2), with the absence of bilirubin providing further evidence of a non-biliary origin for the cyst. Based upon our experience, we propose an algorithm (Fig. 2) in which patients with an equivocal diagnosis of CC on transabdominal imaging studies can be considered for assessment with EUS and EUS-FNA.
This study has limitations that should be considered when interpreting the results. It is a single center, retrospective study. Although this is the largest number of patients in whom the role of EUS in CC has been reported, the numbers are still small. There may be a bias in the patient selection, as only cases in which the diagnosis was unclear may have been referred for EUS.
In conclusion, this study highlights the role of EUS as an adjunct to CT or MRI/MRCP in cases of presumed Type II CC where the diagnosis may be equivocal.
References
Todani T, Watanabe Y, Narusue M, Tabuchi K, Okajima K (1977) Congenital bile duct cysts: Classification, operative procedures, and review of thirty-seven cases including cancer arising from choledochal cyst. Am J Surg 134:263–269
Edil BH, Cameron JL, Reddy S, Lum Y, Lipsett PA, Nathan H, Pawlik TM, Choti MA, Wolfgang CL, Schulick RD (2008) Choledochal cyst disease in children and adults: a 30-year single-institution experience. J Am Coll Surg 206:1000–1005 discussion 1005-1008
Gong L, Qu Q, Xiang X, Wang J (2012) Clinical analysis of 221 cases of adult choledochal cysts. Am Surg 78:414–418
Cho MJ, Hwang S, Lee YJ, Kim KH, Ahn CS, Moon DB, Lee SK, Kim MH, Lee SS, Park DH, Lee SG (2011) Surgical experience of 204 cases of adult choledochal cyst disease over 14 years. World J Surg 35:1094–1102
Edil BH, Olino K, Cameron JL (2009) The current management of choledochal cysts. Adv Surg 43:221–232
Sacher VY, Davis JS, Sleeman D, Casillas J (2013) Role of magnetic resonance cholangiopancreatography in diagnosing choledochal cysts: case series and review. World J Radiol 5:304–312
Singham J, Yoshida EM, Scudamore CH (2009) Choledochal cysts: part 2 of 3: diagnosis. Can J Surg 52:506–511
Lennon AM, Manos LL, Hruban RH, Ali SZ, Fishman EK, Kamel IR, Raman SP, Zaheer A, Hutfless S, Salamone A, Kiswani V, Ahuja N, Makary MA, Weiss MJ, Hirose K, Goggins M, Wolfgang CL (2014) Role of a multidisciplinary clinic in the management of patients with pancreatic cysts: A Single-Center Cohort Study. Ann Surg Oncol (in press)
van der Waaij LA, van Dullemen HM, Porte RJ (2005) Cyst fluid analysis in the differential diagnosis of pancreatic cystic lesions: a pooled analysis. Gastrointest Endosc 62:383–389
Brugge WR, Lewandrowski K, Lee-Lewandrowski E, Centeno BA, Szydlo T, Regan S, del Castillo CF, Warshaw AL (2004) Diagnosis of pancreatic cystic neoplasms: a report of the cooperative pancreatic cyst study. Gastroenterology 126:1330–1336
Huang SP, Wang HP, Chen JH, Wu MS, Shun CT, Lin JT (1999) Clinical application of EUS and peroral cholangioscopy in a choledochocele with choledocholithiasis. Gastrointest Endosc 50:568–571
Sugiyama M, Atomi Y (1997) Endoscopic ultrasonography for diagnosing anomalous pancreaticobiliary junction. Gastrointest Endosc 45:261–267
Lennon AM, Wolfgang C (2013) Cystic neoplasms of the pancreas. J Gastrointest Surg 17:645–653
Tanaka M, Fernandez-Del Castillo C, Adsay V, Chari S, Falconi M, Jang JY, Kimura W, Levy P, Pitman MB, Schmidt CM, Shimizu M, Wolfgang CL, Yamaguchi K, Yamao K (2012) International consensus guidelines 2012 for the management of IPMN and MCN of the pancreas. Pancreatology 12:183–197
Sahora K, Mino-Kenudson M, Brugge W, Thayer SP, Ferrone CR, Sahani D, Pitman MB, Warshaw AL, Lillemoe KD, Fernandez-del Castillo CF (2013) Branch duct intraductal papillary mucinous neoplasms: does cyst size change the tip of the scale? A critical analysis of the revised international consensus guidelines in a large single-institutional series. Ann Surg 258:466–475
Park DH, Kim MH, Lee SK, Lee SS, Choi JS, Lee YS, Seo DW, Won HJ, Kim MY (2005) Can MRCP replace the diagnostic role of ERCP for patients with choledochal cysts? Gastrointest Endosc 62:360–366
Khashab MA, Yong E, Lennon AM, Shin EJ, Amateau S, Hruban RH, Olino K, Giday S, Fishman EK, Wolfgang CL, Edil BH, Makary M, Canto MI (2011) EUS is still superior to multidetector computerized tomography for detection of pancreatic neuroendocrine tumors. Gastrointest Endosc 2011:691–696
Scheiman JM, Carlos RC, Barnett JL, Elta GH, Nostrant TT, Chey WD, Francis IR, Nandi PS (2001) Can endoscopic ultrasound or magnetic resonance cholangiopancreatography replace ERCP in patients with suspected biliary disease? A prospective trial and cost analysis. Am J Gastroenterol 96:2900–2904
Acknowledgments
Supported by Full Moon Full Circle; Dr Law is the Volker Dolch Fellow in Gastroenterology at Johns Hopkins Hospital.
Disclosures
Drs. Oduyebo, Law, Zaheer, Weiss, and Wolfgang have no conflicts of interests or financial ties to disclose. Dr. Lennon is a consultant for Boston Scientific.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary material 1 (MP4 20152 kb)
Supplementary material 2 (MP4 62602 kb)
Rights and permissions
About this article
Cite this article
Oduyebo, I., Law, J.K., Zaheer, A. et al. Choledochal or pancreatic cyst? Role of endoscopic ultrasound as an adjunct for diagnosis: a case series. Surg Endosc 29, 2832–2836 (2015). https://doi.org/10.1007/s00464-014-3998-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-014-3998-4