Abstract
Previous studies have identified numerous risk factors associated with necrotizing enterocolitis (NEC) in very low birth weight (VLBW; birth weight less than 1500 g) infants. One of the potential pathophysiological contributors could be antibiotic therapy. Our aim was to explore the association between antibiotic exposure and NEC in VLBW infants. We designed a retrospective 1:2 case-control cohort study in a level III neonatal intensive care unit. Our study group composed of VLBW infants born between January 2012 and December 2014 with a diagnosis of NEC stage IIA or greater (Bell’s modified criteria). Our intent was to match every case in the study group to two controls. Our primary outcome was an association between antibiotic exposure and NEC. Twenty-two cases of NEC were matched to 32 controls. The infants who developed NEC were exposed to a statistically significantly more frequent number of antibiotic courses and to more days on any antibiotic prior to the development of NEC. There were significant differences between cases and controls with respect to the duration of exposure to gentamicin and meropenem specifically.
Conclusion: The data from our study demonstrate that prolonged exposure to antibiotic therapy is associated with an increased risk of NEC among VLBW infants. Furthermore, gentamicin and meropenem, but not other antibiotics, had a significant association with the incidence of NEC.
What is known: • Early antibiotic exposure is a risk factor for the development of necrotising enterocolitis (NEC) in very low birth weight infants • Prolonged initial empirical antibiotic course for ≥ 5 days, despite sterile blood culture, is associated with an increased risk of developing NEC | |
What is new: • The cumulative total number of days of antibiotic exposure is associated with an increased risk of developing NEC • Gentamicin and meropenem, but not other antibiotics, had a significant association with the incidence of NEC in our study |
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Necrotizing enterocolitis (NEC) is a gastrointestinal emergency which mainly affects preterm infants. The incidence of NEC varies highly, not only from country to country, but also among different hospitals in the same country [3, 4, 11]. Despite the progress in overall neonatal care, NEC is still a leading cause of mortality and morbidity in preterm infants, especially those with very low birth weight (< 1500 g, VLBW) [14]. NEC is associated with serious complications, including short- and long-term gastrointestinal (GI) morbidities and neurodevelopmental problems [11, 19].
The pathogenesis of NEC is multifactorial, and it has frequently been associated with intestinal microbiota, prematurity and enteral feeding [20]. In clinical neonatology, antibiotic regimens (including indications for treatment, duration of the antibiotic therapy, type of antibiotics for late onset sepsis) are highly variable and are usually initiated empirically in infants where there is a clinical suspicion of sepsis or in the presence of risk factors [17]. The widespread use of broad-spectrum antimicrobial agents in the neonatal intensive care unit (NICU) has many obvious drawbacks. The initiation of antibiotic therapy leads to a perturbation of the neonatal gut microbiome, which may then predispose a preterm infant to NEC [10, 15].
Although numerous studies have been conducted to explore the pathogenesis, prophylaxis and treatment of NEC, only minor reductions in the incidence of NEC have been achieved [2, 9, 13, 18]. The aim of our study was to investigate whether the widespread use of broad-spectrum antibiotics in VLBW infants is an associated risk factor for the development of NEC.
Material and methods
We designed a single-centre, retrospective, 1:2 case-control study of VLBW infants admitted to the NICU of the Coombe Women and Infants University Hospital (Dublin, Ireland) between January 1st, 2012 and December 31st, 2014. The cases were VLBW infants with a confirmed NEC stage ≥ IIA according to modified Bell’s criteria [5]. We intended to match each case for gender, gestational age (± 1 week), birth weight (± 150 g), small for gestational age (SGA) status, mode of delivery and maternal chorioamnionitis to two controls. Infants with clinical or radiological evidence of major congenital anomalies and congenital heart diseases apart from patent ductus arteriosus (PDA) were excluded from the study. For the control group, we excluded infants who died before the postnatal age of onset of NEC in the corresponding case. Data were collected for each case and the controls from birth up to the day before documented onset of NEC in the case and corresponding controls. For example, if the case developed NEC on day of life 10, data for the case and its assigned controls were collected from birth up to day of life 9.
We defined early-onset sepsis (EOS) and late-onset sepsis (LOS) according to National Institute for Health and Care Excellence (NICE) guidelines [6]. Confirmed EOS was defined as a blood culture-positive bacterial infection within the first 3 days of life. LOS was defined as sepsis presenting after 72 h of life. Cumulative days of antibiotic exposure were defined as the total number of days an infant was on any antibiotic prior to diagnosis of NEC.
SGA was defined as weight less than the 10th percentile for a baby’s gestational age, and the growth charts that were used in the study have been adopted as policy by the Department of Health and have been adapted for Ireland from materials originally developed by the WHO and Royal College of Paediatrics and Child Health in the UK. [21]
Mechanical ventilation days were defined as cumulative number of days an infant was intubated and needed mechanical ventilation prior to diagnosis of NEC. Non-invasive oxygen treatment days were defined as the total number of days an infant was on oxygen therapy without using an invasive artificial airway (endotracheal tube).
PDA was diagnosed on the basis of echocardiographic findings and was considered hemodynamically significant in our study if the measured diameter was greater than 2 mm and diagnosed prior to the onset of NEC.
Full feeds were defined as a successful enteral intake of at least 130 mls/kg/day.
The primary outcome of the study was the difference between cases and controls in relation to antibiotic usage prior to NEC diagnosis in the study group (data were collected for each case and the controls from the birth up to the day before documented onset of NEC in each case and corresponding controls). Our secondary aim was to explore possible association between potential risk factors and development of NEC (incidence of proven EOS/LOS, duration of mechanical ventilation, surfactant therapy, oxygen treatment/exposure, significant PDA, use of umbilical catheters, requirement of red cell transfusion and feeding history).
The software used for analysis was SPSS version 22.0 and StatsDirect v.3.1.12 (StatsDirect Ltd., Cheshire, UK). Descriptive statistics were used for all demographic variables of interest, and comparisons between case group and control group were made using frequency distribution and percentage for categorical variables. Mean and standard deviation (SD) were used for parametric numeric data, while non-parametric numeric data were summarised using median and interquartile range (IQR). Univariate analysis was conducted using Pearson’s chi-square test or Fisher exact test for categorical data. Parametric numeric data were evaluated using independent sample t test. When the numeric data were non-parametric, the Mann–Whitney test was used for two-sample comparisons. Our results were summarised using p value and 95% confidence intervals. P values < 0.05 were considered statistically significant.
The research ethics committee of the Coombe Women and Infants University Hospital approved the study (Study No. 2-2015).
Results
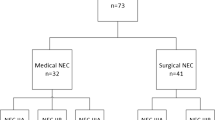
A total of 371 VLBW infants were admitted to the NICU of the Coombe Women and Infants University Hospital during the study period. Of these, 33 infants (8%) were diagnosed with NEC, and 22 infants (6%) met the criteria for NEC stage ≥ IIA according to the modified Bell’s criteria. We identified 32 controls who met the criteria for matching. We sought to match each case with two controls according to several variables, including the gender, gestational age, sex, maternal chorioamnionitis, growth parameters and mode of delivery. However, because of strict guidelines which were used in choosing the two controls for each case, a number of cases either could not be matched to any control or could be matched only to one control. Four cases could not be matched to any control and another four cases were matched to only one control. The mean birth weight (±SD) of the NEC cohort was 728 g (± 162) vs. 778 g (± 163) for the control group and mean gestational age at birth (±SD) was 25.3 weeks (± 1.9) of postmenstrual age vs. 25.9 weeks (± 1.7) respectively. Demographic characteristics of both groups are presented in Table 1.
Of the 22 cases, 14 received the standard feeding regimen (starting at 20–30 mls/kg/day and increased after 24 h by 20–30 mls/kg/day) and four received trophic feeds (up to 20 mls/kg/day started on day 1 and continued at 20 ml/kg/day for 3 days, indicated in the presence of antenatal risk factors). In two infants, enteral feeding was advanced quicker than per the hospital protocol and in two infants, enteral feeding was not started and full TPN was provided. Full enteral feeding was achieved at a median age of 9 days [IQR 7–13]. NEC was diagnosed at a median postnatal age of 16 days [IQR 9–26] (median postconceptional age of 28.2 weeks [IQR 25.3–30.7]). Although the median age at the diagnosis of NEC was lower in the medical cases (13 days) compared to the surgical cases (22 days), there was no statistically significant association between the age of NEC diagnosis and management of NEC (p = 0.6).
The total number of days an infant was on any antibiotic (prior to diagnosis of NEC) was higher in the NEC group with a median of 5 days [IQR 3–10] in comparison to controls which were 3 days [IQR 2–6] (Table 2). Prolonged duration of initial empirical antibiotic exposure was significantly associated with an increased risk of NEC (cases 5 [IQR 3–6] days vs. controls 3 [IQR 0–5] days, p = 0.05) (Table 2). The infants who developed NEC were exposed to a more frequent number of antibiotic courses than those who did not develop NEC (cases 1 [IQR 1–2] course of ATB vs. controls 1 [IQR 0.3–1] course of ATB, p = 0.03) (Table 2).
There were significant differences between cases and controls with respect to the duration of exposure to gentamicin (cases 6 [IQR 0–6] days vs. controls 3 [IQR 3–8] days, p = 0.03) and meropenem (cases 0 [IQR 0–4] days vs. controls 0 [IQR 0–0] days, p = 0.03). However, no significant differences were noticed between the two groups regarding the duration of exposure to other antibiotics.
Although there was no significant association between sepsis and NEC, the infants who had proven early-onset sepsis with a positive culture were removed from the analysis to eliminate the confounding potential effects. Antibiotic exposure was still significantly associated with NEC after removal of these cases (Table 3).
There were no statistical differences in our secondary outcomes except for red cell transfusion and mortality (Table 4).
Discussion
The main findings of our study support the hypothesis that antibiotic exposure is a risk factor for the development of NEC in VLBW infants. Various studies have investigated the relationship between antibiotic exposure and NEC. Cotten et al. (2009) examined initial empirical antibiotic practices for 4039 extremely-low-birth-weight (< 1000 g, ELBW) infants between 1998 and 2001. They reported that exposure to prolonged initial empirical antibiotic for ≥ 5 days, despite sterile blood cultures, was associated with an increased risk of developing NEC (OR 1.34, 95% CI 1.04–1.73) [7]. Our results are in agreement with this finding, as in our study, prolonged exposure to initial antibiotics for more than 5 days was associated with a 3.6-fold increase in the risk of a baby developing NEC (OR 3.6; 95%CI 1.13–11.47). Unlike the previous study, we have included in our case-control study the cumulative total number of days of antibiotic exposure prior to the diagnosis of NEC, and this was also significantly associated with an increased probability of developing NEC. The association between the prolonged initial empirical antibiotic treatment (≥ 5 days) and composite outcome of death, LOS, and NEC after day 7 of life was observed by Kuppala et al. [16]. The association between the prolonged initial empirical antibiotic treatment and NEC alone was not significant in their study. Alexander et al. (2011) performed a 1:2 case-control study to examine whether the antibiotic use is a risk factor for NEC [1]. Unlike our result, they reported that the cumulative days on antibiotics was a non-significant risk factor for NEC (OR 1.02; 95% CI 0.98–1.07).
Another notable finding in our study was that gentamicin and meropenem had a significant association with the incidence of NEC. Infants exposed to gentamicin or meropenem for a prolonged duration of time were at higher risk of having NEC compared to other antibiotics. We speculate that the broad spectrum antibacterial effect of gentamicin and meropenem on the intestinal flora leads to a reduction in bacteria from beneficial genera such as Bifidobacterium and the Lactobacilli which may have a key role in prevention of NEC development [8, 12].
There are several limitations in this study that should be taken into consideration when seeking to generalise the results. Firstly, our study is a retrospective analysis of many clinical associations, which can be considered to be limited by incomplete data in some charts, in addition to being influenced by confounding related variables. In addition, we sought to match each case with two controls according to several variables, including the gender, gestational age, maternal chorioamnionitis, growth parameters and mode of delivery. However, because of strict guidelines which were used in choosing the two controls for each case, a number of cases either could not be matched to any control or could only be matched to one control. Lastly, the sample size of our study was relatively small and this might lead to unidentified important differences in the measures between the two groups.
The strength of our study relates to the fact that it utilised a recent dataset obtained from a neonatal intensive care unit with strict guidelines for the management of VLBW infants, in particular for the administration of antibiotics and nutritional management.
The data from our study demonstrates that prolonged exposure to antibiotic therapy is associated with an increased risk of NEC among VLBW infants. Therefore, to prevent the potential serious side effects of antibiotics, such as NEC, clinicians should prescribe antibiotic agents that have optimal effects, and for the shortest possible duration of time in infants with suspected or proven sepsis. We believe that further prospective trials are required in this area to examine whether judicious limitation of empirical antibiotics might decrease the risk of NEC in VLBW infants.
Abbreviations
- BW:
-
Birth weight
- C/S:
-
Caesarean section
- CI:
-
Confidence interval
- EOS:
-
Early onset sepsis
- IUGR:
-
Intrauterine growth restriction
- IQR:
-
Interquartile range
- OR:
-
Odds ratio
- LOS:
-
Late onset sepsis
- NEC:
-
Necrotizing enterocolitis
- NICU:
-
Neonatal intensive care unit
- PDA:
-
Patent ductus arteriosus
- SD:
-
Standard deviation
- SVD:
-
Spontaneous vaginal delivery
- VLBW:
-
Very low birth weight
References
Alexander VN, Northrup V, Bizzarro MJ (2011) Antibiotic exposure in the newborn intensive care unit and the risk of necrotizing enterocolitis. J Pediatr 159:392–397
AlFaleh K, Anabrees J (2014) Probiotics for prevention of necrotizing enterocolitis in preterm infants. Cochrane Database Syst Rev (Online):CD005496
Battersby C, Longford N, Mandalia S, Costeloe K, Modi N, group UKNCNEs (2017) Incidence and enteral feed antecedents of severe neonatal necrotising enterocolitis across neonatal networks in England, 2012-13: a whole-population surveillance study. Lancet Gastroenterol Hepatol 2:43–51
Battersby C, Santhalingam T, Costeloe K, Modi N (2018) Incidence of neonatal necrotising enterocolitis in high-income countries: a systematic review. Arch Dis Child Fetal Neonatal Ed 103:F182–F189
Bell MJ, Ternberg JL, Feigin RD, Keating JP, Marshall R, Barton L, Brotherton T (1978) Neonatal necrotizing enterocolitis. Therapeutic decisions based upon clinical staging. Ann Surg 187:1–7
Caffrey Osvald E, Prentice P (2014) NICE clinical guideline: antibiotics for the prevention and treatment of early-onset neonatal infection. Arch Dis Child Educ Pract Ed 99:98–100
Cotten CM, Taylor S, Stoll B, Goldberg RN, Hansen NI, Sánchez PJ, Ambalavanan N, Benjamin DK, Jr. (2009) Prolonged duration of initial empirical antibiotic treatment is associated with increased rates of necrotizing enterocolitis and death for extremely low birth weight infants. Pediatrics 123:58–66
Cotter PD, Stanton C, Ross RP, Hill C (2012) The impact of antibiotics on the gut microbiota as revealed by high throughput DNA sequencing. Discov Med 13:193–199
Downard CD, Renaud E, St Peter SD, Abdullah F, Islam S, Saito JM, Blakely ML, Huang EY, Arca MJ, Cassidy L, Aspelund G, American Pediatric Surgical Association Outcomes Clinical Trials C (2012) Treatment of necrotizing enterocolitis: an American Pediatric Surgical Association Outcomes and Clinical Trials Committee systematic review. J Pediatr Surg 47:2111–2122
Gasparrini AJ, Crofts TS, Gibson MK, Tarr PI, Warner BB, Dantas G (2016) Antibiotic perturbation of the preterm infant gut microbiome and resistome. Gut Microbes 7:443–449
Gephart SM, McGrath JM, Effken JA, Halpern MD (2012) Necrotizing enterocolitis risk: state of the science. Advances in neonatal care : official journal of the National Association of Neonatal Nurses 12:77–87 quiz 88-79
Giuliano M, Barza M, Jacobus NV, Gorbach SL (1987) Effect of broad-spectrum parenteral antibiotics on composition of intestinal microflora of humans. Antimicrob Agents Chemother 31:202–206
Horbar JD, Edwards EM, Greenberg LT, Morrow KA, Soll RF, Buus-Frank ME, Buzas JS (2017) Variation in performance of neonatal intensive care units in the United States. JAMA Pediatr 171:e164396
Hull MA, Fisher JG, Gutierrez IM, Jones BA, Kang KH, Kenny M, Zurakowski D, Modi BP, Horbar JD, Jaksic T (2014) Mortality and management of surgical necrotizing enterocolitis in very low birth weight neonates: a prospective cohort study. J Am Coll Surg 218:1148–1155
Jiang P, Jensen ML, Cilieborg MS, Thymann T, Wan JM, Sit WH, Tipoe GL, Sangild PT (2012) Antibiotics increase gut metabolism and antioxidant proteins and decrease acute phase response and necrotizing enterocolitis in preterm neonates. PLoS One 7:e44929
Kuppala VS, Meinzen-Derr J, Morrow AL, Schibler KR (2011) Prolonged initial empirical antibiotic treatment is associated with adverse outcomes in premature infants. J Pediatr 159:720–725
Metsvaht T, Nellis G, Varendi H, Nunn AJ, Graham S, Rieutord A, Storme T, McElnay J, Mulla H, Turner MA, Lutsar I (2015) High variability in the dosing of commonly used antibiotics revealed by a Europe-wide point prevalence study: implications for research and dissemination. BMC Pediatr 15:41
Pammi M, Suresh G (2017) Enteral lactoferrin supplementation for prevention of sepsis and necrotizing enterocolitis in preterm infants. Cochrane Database Syst Rev 6:CD007137
Rees CM, Pierro A, Eaton S (2007) Neurodevelopmental outcomes of neonates with medically and surgically treated necrotizing enterocolitis. Arch Dis Child Fetal Neonatal Ed 92:F193–F198
Siggers RH, Siggers J, Thymann T, Boye M, Sangild PT (2011) Nutritional modulation of the gut microbiota and immune system in preterm neonates susceptible to necrotizing enterocolitis. J Nutr Biochem 22:511–521
Wollmann HA (1998) Intrauterine growth restriction: definition and etiology. Horm Res 49(Suppl 2):1–6
Funding
Jana Semberova’s work was supported by the HIP Trial funding (the European Union Seventh Framework Programme (FP7/2007–2013) under grant agreement no. 260777).
Author information
Authors and Affiliations
Contributions
Dr. Ali Raba designed the study, contributed substantially to the data collection and analysis and drafted the initial manuscript.
Ms. O’Sullivan contributed substantially to the data collection and analysis and reviewed and revised the manuscript.
Dr. Semberova contributed substantially to the study concept and design and reviewed and revised the manuscript.
Prof Martin contributed substantially to the study concept and design and reviewed and revised the manuscript critically for important intellectual content.
Prof Miletin conceptualised and designed the study, supervised the conduct of the study and coordinated the data analysis. He reviewed and revised the manuscript critically for important intellectual content.
All the authors approved the final manuscript as submitted. They agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The research ethics committee of the Coombe Women and Infants University Hospital approved the study.
Informed consent
Informed consent was not required because of the retrospective nature of the study.
Additional information
Communicated by Patrick Van Reempts
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Raba, A.A., O’Sullivan, A., Semberova, J. et al. Are antibiotics a risk factor for the development of necrotizing enterocolitis—case-control retrospective study. Eur J Pediatr 178, 923–928 (2019). https://doi.org/10.1007/s00431-019-03373-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-019-03373-0