Abstract
The antiviral effect of nitric oxide (NO)-releasing compounds was investigated. Using bacterially expressed and purified proteinases 2A and 3C of coxsackievirus B3, in vitro assays demonstrated the inhibition of the 2A proteinase activity in the presence of S-nitroso-N-acetyl-penicillamine (SNAP), 3-morpholinosydnonimine (SIN-1), 4-phenyl-3-furoxancarbonitrile (PFC), glyceryl trinitrate (GTN), and isosorbide dinitrate (ISDN). Sodium nitroprusside (SNP), which releases NO after metabolization, had no effect. The 3C proteinase was inactivated by SNAP, GTN, and ISDN. The vasodilators GTN and ISDN, widely used in the treatment of angina pectoris, exhibited antiviral activity in CVB3-infected GMK cells. CVB3-infected NMRI outbred mice showed significantly reduced signs of myocarditis after treatment with GTN or ISDN. Inhibitors of the cellular inducible NO synthase (iNOS) such as N G-nitro-l-arginine methyl ester (L-NAME), N G-nitro-l-arginine (L-NNA), and S-methyl-isothiourea (SMT), had no deleterious effect on CVB3-infected NMRI mice, indicating that endogenous NO synthesis is unlikely to be a major defense mechanism after enterovirus infection of outbred mice.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Enteroviruses of the picornavirus family are positive-strand RNA viruses. A single open reading frame encodes a polyprotein of approximately 2,200 amino acids in length. During the enteroviral life cycle, the proteinases 2A (2Apro) and 3C (3Cpro) cleave the viral polyprotein in order to release capsid proteins and functional non-structural proteins [26]. Beside the polyprotein proteolysis, both proteinase activities lead to the processing of a number of cellular proteins [4, 11, 13, 14, 32]. This contributes to the host cell shut-off of RNA and protein synthesis and leads to the development of the cytopathic effect of virus-infected cells. Depending on differences in the tissue tropism of the respective serotypes, enteroviruses are the etiological agents of several diseases, e.g. neuronal diseases, acute hemorrhagic conjunctivitis, hand-foot-mouth disease and heart diseases (acute myocarditis, dilated inflammatory cardiomyopathy) [21]. Since acute myocarditis and dilated inflammatory cardiomyopathy are the major causes of human heart failure, great efforts have been made to elucidate the pathogenesis of enterovirus-induced heart disease. In order to study the course of experimental coxsackievirus infection, several mouse models have been established. Depending on the host genetic background and the virus strain used for experimental infection, coxsackievirus B3 (CVB3) induces acute or chronic myocarditis, which may either heal or lead to death. As the animal models differ considerably in the outcome of the artificial infection, controversy has arisen over the explanation of the pathogenesis of the enterovirus-induced heart failure. Two pathogenic mechanisms have been described: (1) virus-induced dysfunction and cytolysis of infected myocytes and (2) destruction of myocytes by a virus-stimulated immune process [12, 20].
A very attractive pathogenic mechanism of the cardiac damage observed in human and experimental animals was recently suggested by Badorff and colleagues who described dystrophin proteolysis by the enteroviral 2Apro [2]. Activity of this proteinase is thought to lead to the disruption of the cytoskeleton network connecting the actin filaments with the sarcolemma. Other non-viral substrate proteins of this proteinase are cytokeratin-8 [29], the poly(A)-binding protein (PABP) [13, 14] and the eucaryotic initiation factor eIF 4G [11]. The other enteroviral proteinase, 3Cpro, also cleaves the PABP [13] and was shown to process several cellular transcription factors [4, 5, 32, 33].
The inhibition of viral replication and the protection of the host from the deleterious effect of viral factors are the major aims of antiviral chemotherapy. Recently, the HIV polymerase and the HIV proteinase were shown to be targets of inhibitory compounds (for reviews, see [6, 7]). For the cardiotropic coxsackie B viruses, another approach could be the selective chemical modification of the viral proteinases by nitric oxide (NO), as previously shown [1, 27, 36]. NO plays a role in a number of physiological and pathophysiological functions in humans. Among these, the cGMP-mediated relaxation of blood vessels is best understood [8]. An alternative cGMP-independent pathway was proposed for blood pressure regulation, host defense and neurotransmission [23]. In vivo, NO is synthesized from l-arginine by calcium-dependent and calcium-independent NO synthases (endothelial, neuronal and inducible isoforms). Since NO is a diatomic free radical, it is unstable and readily undergoes chemical reactions with a variety of atoms and radicals. This yields NO+ equivalents and ONOO- (peroxynitrite). The transfer of a NO+ equivalent to a free thiol group of a cysteine residue yields the formation of nitrosothiol. Such S-nitrosylation of proteins is considered to be a post-translational modification which may influence enzyme activity [3]. A number of compounds capable of generating NO in situ (i.e., NO donors) have been identified and studied with regard to their chemical activities and possible pharmacological applications (for a review, see [31]). Due to the diversity of NO donor structures, NO-generating pathways and biochemical properties of these compounds may differ significantly. In this study, we demonstrate the inhibition of purified enterovirus proteinases by several NO donors in vitro. We also show the protective effect of GTN and ISDN, two organic nitrates widely used as vasodilators, in HeLa cells and in coxsackievirus B3-infected NMRI mice while inhibitors of the inducible NO synthase (iNOS) have no deleterious effect.
Materials and methods
Plasmid construction, expression, and purification of recombinant coxsackievirus B3 proteinases 2A and 3C
For the construction of the expression plasmids, cDNAs of the genomic regions encoding the 2Apro and the 3Cpro of CVB3 were amplified using the oligonucleotides 2A-Nde (5′-GATCCATATGCAACAATCAGGGGCAGTGTATGTG-3′, NdeI site underlined), 2A-Xho (5′-GATCCTCGAGCTGTTCCATTGCATCATCTTCCAG-3′, XhoI site underlined), 3C-F (5′-GGAGATATACATATGGGCCCTGCCTTTGAGTTCGCCGTC-3′, NdeI site underlined) and 3C-B-his (5′-CATCGGCTCGAGTTGCTCATCATTGAAGTAGTGTTTGAGGAG-3′, XhoI site underlined) and plasmid pCVB3-M2 as template DNA [16]. The PCR fragments corresponding to the reading frames of CVB3 2Apro and 3Cpro were digested with NdeI-XhoI and ligated to the NdeI-XhoI fragment of the expression vector pET23a(+) (Novagen, Madison, Wis.) to yield plasmids pET23a-2A-his and pET23a-3C-his. The DNA sequence of these plasmids was verified. For expression, the E. coli strains BL21 (DE3) transformed with pET23a-3C-his and BL21 (DE3) lysS transformed with pET23a-2A-his were grown at 37°C. When the cultures reached an OD595 of 0.5, expression of the fusion proteins was induced by adding 0.5 mM IPTG (isopropyl-β-d-thiogalactopyranoside). After incubation for 3 h at 37°C, the cells were harvested, resuspended in buffer A (40 mM Tris-HCl pH 7.9, 100 mM NaCl, 15 mM mercaptoethanol) and lysed with a French press (3 cycles at 1,000 psi). The lysate was clarified by centrifugation at 17,500 rpm (4°C) for 20 min. The soluble his-tagged recombinant proteins were purified using Ni-NTA agarose according to the manufacturer's description (Qiagen, Hilden, Germany).
NO donors and iNOS inhibitors
NO donors were dissolved as follows: Organic nitrates: glyceryl trinitrate (GTN, Nitrolingual) was obtained from Pohl-Boskamp GmbH (Hohenlockstedt, Germany); stock solution: 1 mg/ml in water (4.4 mM). Isosorbide dinitrate (ISDN, Nitrosorbon) was obtained from ICN Biomedicals GmbH (Eschwege, Germany); stock solution: 1.09 mg/ml in water (4.6 mM). Nitrosamine: S-nitroso-N-acetyl-penicillamine (SNAP) was obtained from Calbiochem (Bad Soden, Germany); stock solution: 25 mg/ml in DMSO (113.5 mM). Furoxan: 4-phenyl-3-furoxancarbonitrile (PFC) was obtained from Calbiochem; stock solution: 1.87 mg/ml (10 mM) in DMSO. Sydnonimine: 3-morpholinosydnonimine (SIN-1) was obtained from Calbiochem; stock solution: 25 mg/ml (48 mM) in DMSO. Metal-NO complex: sodium nitroprusside (SNP) was obtained from Calbiochem; stock solution: 1.5 mg/ml (5 mM) in phosphate-buffered saline. All NO donors were stored at −20°C and handled in the dark.
iNOS inhibitors were dissolved as follows: N G-nitro-l-arginine methyl ester (L-NAME), N G-nitro-l-arginine (L-NNA), and S-methyl-isothiourea (SMT) were obtained from Calbiochem and Novabiochem, respectively; stock solutions: 1 mg/ml.
Proteinase activity and inhibition assays
Proteolytic activity was assayed using poly(A)-binding protein (PABP) as a substrate [13]. Bacterial expression of this protein was previously described [10]. Crude extracts of PABP-overexpressing bacteria were incubated in the presence or absence of 5 μM purified 2Apro and 3Cpro respectively for 8 h at ambient temperature and analyzed by SDS polyacrylamide gel electrophoresis (PAGE). For the inhibition assays, proteinases were pre-incubated for 8 h with SNAP, SIN-1, PFC, GTN, ISDN, and SNP, respectively. After pre-incubation, proteinase activity was assayed by addition of substrate protein as described.
Cells and viruses
Virus propagation was performed in HeLa Ohio (human cervix carcinoma; ATCC No. CCL-136) and GMK (green monkey kidney, Schaper & Brümmer, Salzgitter) cells. HeLa cells were grown in Eagle's minimum essential medium (EMEM) supplemented with 10% newborn calf serum, 100 U/ml penicillin and 100 μg/ml streptomycin. GMK cells were grown in Dulbecco's modified EMEM supplemented with 10% fetal bovine serum, 100 U/ml penicillin and 100 μg/ml streptomycin. CVB3 Nancy (gift of the Institute of Poliomyelitis and Virus Encephalitides, Moscow) was grown in HeLa Ohio cells. Virus yields were determined by endpoint titrations using four replicates of serial tenfold dilutions in 96-well plates containing GMK or HeLa cell monolayers. The 50% tissue culture infective dose (TCID50) was calculated according to Reed and Muench [24].
Cytotoxicity
The cytotoxicity of the test compounds was determined on confluent HeLa Ohio and GMK cell monolayers grown in flat-bottomed microtiter plates as described previously [28]. After removing the growth medium, nine twofold dilutions of the compounds in 100 μl of test medium were added. Following a 72 h incubation (37°C, 5% CO2), the supernatant was aspirated. The cell monolayers were washed, fixed, and stained with a crystal violet/methanol solution. After extraction of the dye, the optical density of individual wells was quantified spectrophotometrically at 550/630 nm with a microplate reader (Dynatech, Guernsey, UK). Cell viability was evaluated as the percentage of the mean value of optical density resulting from six mock-treated cell controls, set as 100%. The 50% cytotoxic concentration (CC50) was defined as the compound concentration reducing the viability of untreated cell cultures by 50%.
Cytopathic effect inhibitory assay
The cytopathic effect (CPE) inhibitory assay used in the primary antiviral screening was designed to detect agents acting at any stage of the virus reproductive cycle [28]. Assays were carried out in confluent GMK cell monolayers grown in 96-well flat-bottomed microtiter plates. 50 μl of drug solution and a constant amount of virus (1 multiplicity of infection of CVB3) in a volume of 50 μl were distributed into 96-well plates. Three wells on each plate served as cell controls (no test compound added) and three wells served as virus controls. In addition, the 50% and 100% plaque inhibitory concentrations of guanidine hydrochloride (3 wells each) were included as positive controls in each microtiter plate. Using the crystal violet uptake assay described for cytotoxic investigations, the inhibition of the virus-induced CPE was scored 24 h post infection when untreated infected control cells showed maximum CPE. The IC50 values of active compounds were determined from the mean dose-response curves (two parallels per concentration) of three separate experiments.
Determination of nitrate/nitrite release by the NO donor compounds (Griess assay)
HeLa and GMK cells were seeded in 24-well plates and grown to confluency (48h, 37°C, 5% CO2). The growth medium was removed and replaced by 500 μl medium supplemented with 2% NCS or FCS, respectively, containing various amounts of SNAP, GTN or ISDN. At various timepoints (15 min, 30 min, 1, 2, 4, 8, 24, and 48 h), 220 μl of culture supernatant were removed from each well and frozen at –20°C until NO determination. The amount of nitrite released into the medium was quantified with a colorimetric assay kit from Alexis Deutschland GmbH (Grünberg, Germany) according to the instructions of the manufacturer.
Plaque reduction assay
Confluent GMK cells grown in 24-well plates were infected with approximately 40 plaque forming units CVB3. After 1 h of virus adsorption (37°C), the infecting media was removed and the cell monolayer was overlayed with agar containing different dilutions of NO donors. After 30 h of incubation at 37°C, the plates were fixed and stained with a crystal violet/formalin solution.
Design of mouse experiments
All animal procedures were officially approved in accordance with the German Animal Protection Law. To evaluate the influence of NO donors (GTN, ISDN) and iNOS inhibitors (L-NAME, L-NNA, and SMT) on lethality and severity of myocarditis, groups of 5–10 male 7- to 9-week-old NMRI mice were inoculated with 5,000 TCID50 of CVB3 Nancy and treated with the respective drug (Table 1). The following compounds were diluted with water daily: GTN (10 μg/ml), L-NAME (500 μg/ml), L-NNA (100 μg/ml), SMT (10 μg/ml). Treatment by feeding of GTN and iNOS inhibitors respectively, was started 1 h before virus inoculation and continued until day 14. ISDN was dissolved in 5 mg/ml water and 0.3 ml of this solution (corresponding to 1.5 mg) was applied orally each day until day 28. The following controls were included: one group of non-infected, non-treated animals and two groups of male, 7- to 9-week old NMRI mice which were infected with 5,000 TCID50 CVB3 but not treated. The body weights of the mice were determined daily. The mice were exsanguinated under ether anaesthesia at either day 14 or day 28 post-infection (p.i.) and specimens of heart and blood were collected. The organ weights of the specimens were determined and the hearts were used for histologic evaluation. The sera were checked for CVB3-specific antibodies by enzyme-linked immunosorbent assays (ELISA) on the day of exsanguination as described previously [22], and for NO release (at days 4, 7, 14, and 28 p.i.) with the Cayman chemical nitrate/nitrite assay kit (Alexis Deutschland GmbH).
Histology
Heart tissue was fixed in 6% formalin solution for at least 24 h and mounted in paraffin. For histologic examination, 5 μm sections were stained with hematoxylin and eosin. At least three adjacent sections were examined microscopically for the presence of lesions. Histologic evidence of myocarditis and inflammation was classified in terms of the degree of cellular infiltration, myocardial cell necrosis, extent of calcification and fibrosis, and scored on a scale of 0 to 4. Score 0 described no lesions. Score 1 (slight) describes rare groups of two or three mononuclear cells displacing myocytes, the presence of one or two small lesions (focal myocytic degeneration and/or necrosis, calcification of necrotic myocytes), and insignificant reaction of interstitial connective tissue. Score 2 (mild) describes larger and more frequent mononuclear cell aggregates without confluence between adjacent foci, the presence of several small lesions scattered throughout the myocardium, and an increase in interstitial connective tissue with the foci. Score 3 (medium) describes larger and more frequent mononuclear cell infiltrates with confluent foci present, multiple small lesions or several large lesions, and areas of myocyte drop-out replaced by dense stellate scars with tendril-like extension into the surrounding myocardium. Score 4 (severe) describes many large foci of inflammatory cells, multiple large lesions, focal scars accentuated and heavily collagenized, and thickening of unscarred reticulum fibers. The myocarditis index included the histopathological parameters as a ratio of infiltration, necrosis, and fibrosis of each animal. The statistical comparisons were carried out using Student's t test.
Results
Proteolytic activity of recombinant enteroviral proteinases 2A and 3C
In order to study the inhibition of the viral proteinases 2Apro and 3Cpro by NO-releasing compounds, the reading frames of both proteinases were cloned into the NdeI-XhoI sites of the expression vector pET23a(+). The recombinant proteinases were overexpressed in BL21 (DE3) bacteria transformed with pET23a-2Ahis and pET23a-3Chis, respectively, and purified by affinity chromatography using Ni-NTA agarose. The proteinase-containing elution fractions contained virtually pure protein as judged from the Coomassie brilliant blue-stained gels (data not shown). The proteolytic activity of the purified proteinases were studied with human poly(A)-binding protein (PABP) as a substrate. This host cell protein (70.7 kDa, 636 amino acids) was recently shown to be a natural substrate of both proteinases [13, 14]. For a typical proteinase assay reaction, crude extracts of bacteria overexpressing human PABP were incubated with 5 μM purified 2Apro or 3Cpro at 37°C for 2–12 h. Subsequent SDS-PAGE of the mixtures revealed characteristic cleavage products, i.e., a 54.7 kDa N-terminal fragment (corresponding to processing at amino acids S486-T487 by 2Apro) and a 60.4 kDa N-terminal fragment (corresponding to processing at amino acids Q540-G541 by 3Cpro), respectively (Fig. 1). Additional cleavage products which appear in some gels are bands of 33.3 and 37.4 kDa, corresponding to processing at Q292-G293 by 3Cpro, and a band of approximately 31 kDa, corresponding to 2Apro cleavage either near amino acid 275 or near amino acid 360 (compare Fig. 1 and Fig. 2). Low proteolytic activity as indicated by long incubation time and high amounts of proteinase appears not to be due to denatured proteinase, because CD spectroscopy indicated that at least the purified 3Cpro was folded [37].
Proteolytic activity of purified recombinant proteinases 2A and 3C of coxsackievirus B3. Bacterial extracts containing approximately 180 pmol of poly(A)-binding protein (PABP) were incubated for 8 h in absence or presence of the respective proteinase (5 μM), subjected to 12.5% SDS-PAGE and stained with Coomassie brilliant blue
Inhibition of proteolytic activity in vitro. A Inhibition of 2Apro and 3Cpro activity by SNAP. B Inhibition of 2Apro activity by 2 mM PFC, 9.6 mM SIN-1, 22.8 μM SNAP, and 1 mM SNP. C Inhibition of 2Apro and 3Cpro activity by 880 μM GTN and 92 μM ISDN. As a control, inhibition reactions with 22.8 μM SNAP are also shown
Inhibition of 2Apro and 3Cpro mediated proteolysis by NO-releasing compounds
It was previously shown that SNAP, spermine-NONOate, and PAPA-NONOate inhibit both coxsackievirus replication and substrate processing by 3Cpro [27] and 2Apro [1]. As an explanation, it was suggested that S-nitrosylation of both proteinases should lead to inactivation. In order to extend these investigations to other NO-releasing compounds, we assayed the inhibitory effect of SIN-1, PFC, GTN, and ISDN. A positive control (SNAP) and a negative control (SNP, which releases NO after metabolization) were also included. For in vitro assays, the respective inhibitor and the proteinase were pre-incubated for 8 h. Proteinase inhibition assay reactions contained NO donors at concentrations as indicated in Fig. 2. After pre-incubation, the PABP-containing E. coli extract was added and the mixture was incubated again at ambient temperature for 4–12 h then separated by SDS PAGE. Figure 2A shows that pre-incubation of 2Apro and 3Cpro with SNAP at concentrations as low as 22.8 μM is sufficient to completely inhibit proteinase activity. Figure 2B shows the result with other NO donors. While SNAP, PFC and SIN-1 inhibit 2Apro activity, SNP does not. The inhibition of 2Apro and 3Cpro by organic nitrates was also tested. GTN inhibited the activity of 3Cpro and 2Apro, respectively, while ISDN inhibited 3Cpro but not 2Apro (Fig. 2C).
Cytotoxicity, NO release and anti-CVB3 activity
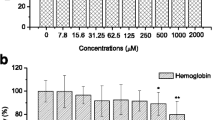
In order to assess the antiviral effect of organic nitrates in cell cultures, the cytotoxicity, the NO release into culture supernatants, and the inhibition of the cytopathic effect (CPE) of GTN and ISDN were investigated (Table 2, Fig. 3A, B).
NO release and antiviral activity of SNAP, GTN, and ISDN. A Time-dependent NO release into cell culture supernatant by the test compounds. GMK cell monolayers were exposed to 250 μM SNAP, 250 μM GTN, and 5 mM ISDN respectively for the indicated time periods. B Inhibition of the CVB3-induced cytopathic effect in GMK cells by NO releasing compounds, as reflected in their dose-response curves to SNAP, GTN, and ISDN treatment. Values shown are the mean±standard deviation of three separate experiments. C Inhibition of CVB3 replication in GMK cells by the NO releasing compounds SNAP, GTN, and ISDN as reflected by the plaque reduction assay. Values shown are the mean±standard deviation of three independent experiments
Cytotoxicity on confluent monolayers of HeLa Ohio and GMK cells was tested to exclude non-specific antiviral activities of SNAP, GTN and ISDN. The 50% cytotoxic concentrations (CC50) were calculated from the single or the mean dose-response curve of three separate assays, respectively. Table 2 summarizes the CC50 values of the test compounds in both cell lines [SNAP (HeLa: >200 μg/ml = >907.8 μM, GMK: 110.7 μg/ml = 502 μM), GTN (HeLa: 86.2 μg/ml = 397 μM, GMK: >200 μg/ml = >921 μM), ISDN (HeLa: >1,000 μg/ml = >4,235 μM, GMK: >1,000 μg/ml = >4,235 μM)]; even 5 mM ISDN concentration was not cytotxic.
Based on these results, 250 μM SNAP, 250 μM GTN, and 5,000 μM ISDN were used to investigate the time course of NO release in HeLa and GMK cell cultures. The results show that 4–8 h after SNAP administration, nearly all NO was released into the media (Fig. 3A). In contrast, GTN and ISDN led to a continuous rise of NO concentrations in the culture supernatant. Using non-cytotoxic concentrations of the individual compounds, different maximum NO values were determined: 29 μM for SNAP, 28 μM for GTN and 13 μM for ISDN. NO was not detected in mock-treated cell controls under identical experimental conditions.
The antiviral activity of GTN and ISDN was demonstrated with the CPE inhibition assay (Fig. 3B) and the plaque reduction assay (Fig. 3C). In both assays, GTN showed the strongest antiviral effect: (1) the CVB3-induced CPE was reduced by 60% compared to a 20–30% reduction by SNAP and ISDN; (2) the plaque reduction was greater than 90% compared to 65% by ISDN. SNAP administration did not lead to a significant plaque reduction at any concentration assayed.
GTN and ISDN have a protective effect in CVB3 infected NMRI mice
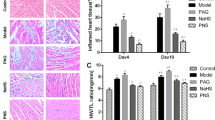
Since GTN and, to a lesser extent, ISDN have the ability to inhibit enteroviral proteinases and have a significant antiviral effect in cell culture, we assayed whether these NO donors could play a protective role in experimental CVB3 infection. Groups of male 7–9 weeks old NMRI outbred mice were intraperitoneally infected with CVB3 Nancy and treated either with GTN (by feeding it with the drinking water) or ISDN (daily oral application). As a control, one group of litter mates was not infected, and a second group was infected with CVB3 but not treated with a NO donor. At day 14 p.i., GTN-treated mice were exsanguinated and examined. Since initial experiments had indicated that ISDN-treated mice showed no significant differences in comparison with untreated mice at day 14 (Fig. 4A), treatment with ISDN was extended until day 28 p.i. At the end of the experiments, the heart weights of treated and untreated animals did not differ, and similar virus titers were observed at days 7, 14, and 28 p.i. (data not shown). The survival rate of ISDN-treated mice (100% vs 76.7% at 28 days) but not of GTN-treated mice (84.6% vs 82.4% at 14 days) was elevated. The levels of iNOS mRNA was increased and raised levels of NO were detectable in heart tissue at days 7, 14, and 28, respectively [9]. The hearts of the mice were histologically examined and the myocarditis index was determined. Figure 4 summarizes the results of these experiments. GTN significantly reduces signs of myocarditis, while ISDN has a less pronounced effect: treatment for 14 days does not lead to a significant reduction in all investigated parameters, but prolongation of oral ISDN administration up to day 28 p.i. significantly reduces signs of myocarditis (Fig. 4A). Figure 4B and C show typical examples of heart sections of treated and non-treated animals. At day 14, CVB3-infected mice have large areas of infiltrates. At this early stage, fibrosis is already increased. GTN-treated mice have significantly reduced infiltrates and fibrosis. At day 28, untreated mice have only a small number of infiltrating cells but large areas of fibrosis. In contrast, ISDN-treated mice have only few infiltrates and a slight fibrosis.
Histologic examination of murine hearts. Hearts of treated and untreated CVB3-infected mice were removed at days 14 and 28 p.i., respectively, and histologically examined for cellular infiltration, myocardial cell necrosis, calcification, and fibrosis. A Myocarditis index of each mouse group (mean values±SD). B Representative example of a heart section of a virus-infected mouse treated with GTN for 14 days p.i. (left panel) compared to heart sections of an untreated CVB3-infected mouse (middle panel) and a non-infected mouse (right panel). Note the significantly reduced infiltrations and the lack of fibrosis in the GTN-treated mouse. C Representative example of a heart section of a virus-infected mouse treated with ISDN for 28 days p.i. (left panel) compared to a heart section of an untreated CVB3-infected mouse (right panel). At this stage of infection, the number of areas showing infiltrations is decreased in the untreated animal (compare to panel B), and large areas of fibrosis are observed in this mouse
The effect of iNOS inhibitors
In order to study the effect of iNOS inhibitors, four groups of male 7- to 9-week-old NMRI mice were infected with CVB3. Three groups of these infected mice were treated for 14 days with the iNOS inhibitors L-NAME (500 μg/ml), L-NNA (100 μg/ml), and SMT (10 μg/ml) by feeding these compounds with drinking water. Comparison of treated and untreated mouse hearts revealed no significant differences in the heart weight (data not shown), virus titers in the heart and pancreas at day 14 p.i. (data not shown), and the myocarditis index (Fig. 4A). However, at day 4 p.i. L-NNA-treated mice had a significantly increased virus titer in the heart (6.26±1.07 vs 4.91±0.58 log TCID50) and in the spleen (7.3±0.69 vs 5.9±0.08 log TCID50), and the survival rate was reduced for mice treated with L-NNA (40% vs 66%) and L-NAME (50% vs 82.4%). Mice which were treated with SMT showed no significant difference in the survival rate. (93.3% vs 86.2%).
Discussion
NO is a biologic messenger which acts as a neurotransmitter, a vasodilator, and as a cytotoxic immune effector. Beside these pleiotropic effects, direct S-nitrosylation of viral proteins has been discussed [3]. NO is produced by NO synthases of which an inducible isoform (iNOS, NOS2) is expressed in activated, but not in resting macrophages [18]. Since iNOS is induced after viral infections by interferon-gamma and tumor necrosis factor-alpha, NO is part of the host nonspecific immune response.
Due to the antiviral potential of NO, several NO-releasing substances were tested and shown to be effective inhibitors of several viruses (for a compilation, see [25]) including coxsackievirus B3 and poliovirus [17, 19]). Saura and colleagues [27] and Badorff and colleagues [1] have provided experimental evidence that NO donors like SNAP, PAPA-NONOate and spermine-NONOate directly inactivate the enteroviral proteinases 2Apro and 3Cpro by S-nitrosylation of the active site cysteine residue. We have extended these works and assessed the feasibility of using other NO donors as inhibitors of enteroviral proteinases by pre-incubation of recombinant 2Apro and 3Cpro with SNAP (a nitrosamine), GTN and ISDN (organic nitrates), PFC (a furoxan), SIN-1 (a sydnonimine), and SNP (a metal-NO complex) followed by addition of the substrate protein to this mixture (Fig. 2). With the exception of SNP and ISDN, all assayed NO donors were found to inhibit the 2Apro. Failure of SNP to inhibit proteinase activity was expected since this compound does not spontaneously release NO but requires metabolism by an unknown enzymatic activity derived from the microsomal membrane fraction [15]. Failure of ISDN to inhibit 2Apro but not 3Cpro in vitro may be the result of its insufficient spontaneous NO release. As shown in Fig. 3A, only 2.5 μM nitrite released by 5,000 μM ISDN (corresponding to 0.05%) was detectable in the Griess assay after an 8 h incubation. On the other hand, 2Apro has seven cysteine residues. Three of these cysteines (C50, C110, C116) are in a sequence context which partially match the 'S-nitrosylation motif' [30]. As the S-nitrosylation reaction is dose-dependent, complete modification of 2Apro cysteines within the pre-incubation time would require ISDN concentrations exceeding the solubility in aqueous solutions. Moreover, the significance of the S-nitrosylation motif seems to be questionable, as the sequence context of the single cysteine residue of 3Cpro does not match the S-nitrosylation motif but seems to be readily S-nitrosylated by SNAP and GTN (Fig. 2B) as well as NOR-3 and SIN-1 (data not shown). Therefore, we cannot exclude that most of the seven cysteines are susceptible to S-nitrosylation.
Inhibition of virus replication by SNAP, GTN, and ISDN was investigated by the CPE inhibition assay and the plaque reduction assay (Fig. 3). The results confirm that all NO donors inhibit CVB3 replication in a dose-dependent manner. However, clear differences were observed between the compounds with regard to the pattern of NO release and their antiviral efficacy. Whereas the well-characterized NO donor SNAP releases nearly all the NO into the culture media within 2–4 h, continuously increasing levels of NO were detected in the culture supernatant after incubation with of GTN and ISDN. Both the time course of NO release and the amounts of NO in the cell culture supernatant seem to play an important role for antiviral efficacy. The most effective inhibitor of the CVB3-induced cytopathic effect was GTN (up to 65%), which continuously releases high amounts of NO (Fig. 2). In the plaque reduction assay, GTN again showed the best results: a dose-dependent plaque reduction of up to 95% and a significantly reduced plaque size was observed. ISDN was less efficient (up to 25% CPE inhibition and up to 65% plaque reduction). The control compound SNAP exhibited a moderate CPE inhibition (up to 30%) but no plaque reduction (Fig. 2).
CVB3-infected NMRI outbred mice treated with GTN (14 days) and ISDN (28 days), respectively, have decreased values of the myocarditis index (1.37±1.06 for GTN, 1.75±0.89 for ISDN) in comparison to untreated CVB3-infected mice (3.15±0.13 at day 14 p.i., 2.64±0.19 at day 28 p.i.). This result provides evidence that NO plays a role in the host defense against viral infections. NO-mediated reduction of viral myocarditis in CVB3-infected mice could depend on two mechanisms: (1) in a nonspecific response, the vasodilating action of NO might increase vascular perfusion thereby permitting lymphocyte infiltration, and (2) NO might transiently or permanently inhibit the activity of the enteroviral proteinases by S-nitrosylation. Increased lymphocyte infiltration due to enhanced blood circulation would increase the signs of inflammation. However, less infiltrates and less necrosis was observed in our mice (Fig. 4B, C). This observation favors the alternative explanation, namely a direct inactivation of proteinases. S-nitrosylation of 2Apro and 3Cpro was previously described by Saura and colleagues [27] and Badorff and colleagues [1] and is supported by our in vitro experiments (Fig. 2). Antiviral activity of both compounds, GTN and ISDN, was also observed in cultured HeLa and GMK cells (Fig. 3), indicating that vasodilation may play only a minor role in the experimental infection of mice.
Although the number of reports demonstrating antiviral activity of NO is increasing, the role of endogenous NO production is still unclear. Previous results indicated that iNOS mRNA is induced after CVB3 infection of mice [9]. Other reports demonstrate that NO deficiency in NOS null mutants exacerbates murine CVB3 infection [34, 35]). Virus titers in all organs were increased and mortality of the NOS2 null mice was 100%. CVB3-infected NMRI mice treated with iNOS inhibitors (L-NNA, L-NAME, SMT) did not respond as strongly; their virus titers and histologic myocarditis scores were not elevated and only mice treated with L-NNA and L-NAME showed a moderate increase in mortality. Our results lead to the conclusion that endogenous NO production is not sufficient to significantly contribute to the host response to viral infection. This view is supported by another line of evidence. In poliovirus-infected HeLa and U937 cells, an endogenous virus-stimulated NO synthesis was observed which did not prevent virus replication and cell lysis [17]. However, administration of 4 μg/ml GTN lead to a prolonged replication cycle and strongly reduced poliovirus titers.
Future experiments should elucidate whether treatment with various NO-releasing drugs may ameliorate the symptoms and the outcome of acute and chronic enteroviral diseases.
References
Badorff C, Fichtlscherer B, Rhoads RE, Zeihe AM, Muelsch A, Dimmeler S, Knowlton KU (2000) Nitric oxide inhibits dystrophin proteolysis by coxsackieviral protease 2A through S-nitrosylation. A protective mechanism against enteroviral cardiomyopathy. Circulation 102:2276–2281
Badorff C, Lee GH, Lamphear BJ, Martone ME, Campbell KP, Rhoads RE, Knowlton KU (1999) Enteroviral protease 2A cleaves dystrophin: evidence of cytoskeletal disruption in an acquired cardiomyopathy. Nat Med 5:320–326
Broillet MC (1999) S-Nitrosylation of proteins. Cell Mol Life Sci 55:1036–1042
Clark ME, Lieberman PM, Berk AJ, Dasgupta A (1993) Direct cleavage of human TATA-binding protein by poliovirus protease 3C in vivo and in vitro. Mol Cell Biol 13:1232–1237
Clark ME, Hämmerle T, Wimmer E, Dasgupta A (1991) Poliovirus proteinase 3C converts an active form of transcription factor IIIC to an inactive form: a mechanism for inhibition of host cell polymerase III transcription by poliovirus. EMBO J 10:2941–2947
De Clercq E (2002a) Strategies in the design of antiviral drugs. Nat Rev Drug Discov 1:13–25
De Clercq E (2002b). New developments in anti-HIV chemotherapy. Biochim Biophys Acta 1587:258–275
Fleming I, Busse R (1999) NO: the primary EDRF. J Mol Cell Cardiol 31:5–14
Glück B, Merkle I, Dornberger G, Stelzner A (2000) Expression of inducible nitric oxide synthase in experimenatal viral myocarditis. Herz 25:255–260
Görlach M, Burd CG, Dreyfuss G (1994) The mRNA poly(A)-binding protein: localization, abundance and RNA-binding specificity. Exp Cell Res 211:400–407
Gradi A, Svitkin YV, Imataka H, Sonenberg N (1998) Proteolysis of human eukaryotic translation initiation factor eIF4GII, but not eIF4GI, coincides with the shutoff of host protein synthesis after poliovirus infection. Proc Natl Acad Sci USA 95:11089–11094
Huber SA (1992) Viral myocarditis - a tale of two diseases. Lab Invest 66:1–3
Joachims M, Van Breugel PC, Lloyd RE (1999) Cleavage of poly(A)-binding protein by enterovirus proteases concurrent with inhibition of translation in vitro. J Virol 73:718–727
Kerekatte V, Keiper BD, Badorff C, Cai A, Knowlton KU, Rhoads RE (1999) Cleavage of poly(A)-binding protein by coxsackievirus 2A protease in vitro and in vivo: another mechanism for host protein synthesis shutoff? J Virol 73:709–717
Kowaluk EA, Seth P, Fung HL. (1992) Metabolic activation of sodium nitroprusside to nitric oxide in vascular smooth muscle. J Pharmacol Exp Ther 262:916–22
Lindberg AM, Crowell RL, Zell R, Kandolf R, Pettersson U (1992) Mutations in capsid polypeptide VP2 alter the tropism of the Nancy strain of Coxsackievirus B3. Virus Res 24:187–196
Lopez-Guerrero JA, Carrasco L (1998) Effect of nitric oxide on poliovirus infection of two human cell lines. J Virol 72:2538–2540
Lowenstein CJ, Glatt CS, Bredt DS, Snyder SH (1992) Cloned and expressed macrophage nitric oxide synthase contrasts with the brain enzyme. Proc Natl Acad Sci USA 89:6711–6715
Lowenstein CJ, Hill SL, Lafond-Walker A, Wu J, Allen G, Landavere M, Rose NR (1996) Nitric oxide inhibits viral replication in murine myocarditis. J Clin Invest 97:1837–1843
McManus BM, Chow LH, Wilson JE, Anderson DR, Gulizia JM, Gauntt CJ, Klingel K, Beisel BW, Kandolf R (1993) Direct myocardial injury by enterovirus: a central role in the evolution of murine myocarditis. Clin Immunol Immunopathol 68:159–169
Melnick JL (1996) Enteroviruses: polioviruses, coxsackieviruses, echoviruses, and newer enteroviruses. In: Fields BN, Knipe DM, Howley PM (eds) Virology, 3rd edn. Lippincott-Raven, Philadelphia, pp 655–712
Merkle I, Tonew M, Glück B, Schmidtke M, Egerer R, Stelzner A (1999) Coxsackievirus B3-induced chronic myocarditis in outbred NMRI mice. J Hum Virol 2:369–379
Moncada S, Higgs A (1993) The L-arginine-nitric oxide pathway. N Engl J Med 329:2002–12
Reed LJ, Muench HA (1938) A simple method of estimating fifty per cent endpoints. Am J Hyg 27:493
Reiss CS, Komatsu T (1998) Does nitric oxide play a critical role in viral infections? J Virol 72:4547–4551
Ryan MD, Flint M (1997) Virus-encoded proteinases of the picornavirus super-group. J Gen Virol 78:699–723
Saura M, Zaragoza C, McMillan A, Quick RA, Hohenadl C, Lowenstein JM, Lowenstein CJ (1999) An antiviral mechanism of nitric oxide: inhibition of a viral protease. Immunity 10:21–28
Schmidtke M, Schnittler U, Jahn B, Dahse HM, Stelzner A (2001) A rapid assay for evaluation of antiviral activity against coxsackie virus B3, influenza virus A, and herpes simplex virus type 1. J Virol Methods 95:133–143
Seipelt J, Liebig HD, Sommergruber W, Gerner C, Kuechler E (2000) 2A proteinase of human rhinovirus cleaves cytokeratin 8 in infected HeLa cells. J Biol Chem 275:20084–20089
Stammler JS, Toone EJ, Lipton SA, Sucher NS (1997) (S)NO signals: Translocation, regulation, and a consensus motif. Neuron 18:691–696
Wang PG, Xian M, Tang X, Wu X, Wen Z, Cai T, Janczuk AL (2002) Nitric oxide donors: Chemical activities and biological applications. Chem Rev 102:1091–1134
Yalamanchili P, Datta U, Dasgupta A (1997a) Inhibition of host cell transcription by poliovirus: cleavage of transcription factor CREB by poliovirus-encoded protease 3Cpro. J Virol 71:1220–1226
Yalamanchili P, Weidman K, Dasgupta A (1997b) Cleavage of transcriptional activator Oct-1 by poliovirus encoded protease 3Cpro. Virology 239:176–185
Zaragoza C, Ocampo CJ, Saura M, Bao C, Leppo M, Lafond-Walker A, Thiemann DR, Hruban R, Lowenstein CJ (1999) Inducible nitric oxide synthase protection against coxsackievirus pancreatitis. J Immunol 163:5497–5504
Zaragoza C, Ocampo CJ, Saura M, Leppo M, Wei XQ, Quick R, Moncada S, Liew FY, Lowenstein CJ (1998) The role of inducible nitric oxide synthase in the host response to coxsackievirus myocarditis. Proc Natl Acad Sci USA 95:2469–2474
Zaragoza C, Ocampo CJ, Saura M, McMillan A, Lowenstein CJ (1997) Nitric oxide inhibition of coxsackievirus replication in vitro. J Clin Invest 100:1760–1767
Zell R, Sidigi K, Bucci E, Stelzner A, Görlach M (2002) Determinants of the recognition of enteroviral cloverleaf RNA by coxsackievirus B3 proteinase 3C. RNA 8:188–201
Acknowledgements
The excellent technical assistance of Gesche Dornberger, Veronika Güntzschel, Birgit Jahn, Birgit Meissner, Birgit Schikowski, and Sabine Wachsmuth is acknowledged.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zell, R., Markgraf, R., Schmidtke, M. et al. Nitric oxide donors inhibit the coxsackievirus B3 proteinases 2A and 3C in vitro, virus production in cells, and signs of myocarditis in virus-infected mice. Med Microbiol Immunol 193, 91–100 (2004). https://doi.org/10.1007/s00430-003-0198-6
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00430-003-0198-6