Abstract
Background
Diabetic retinopathy is associated with osmotic stress resulting from hyperglycemia and intracellular sorbitol accumulation. Systemic hypertension is a risk factor of diabetic retinopathy. High intake of dietary salt increases extracellular osmolarity resulting in systemic hypertension. We determined the effects of extracellular hyperosmolarity, chemical hypoxia, and oxidative stress on the gene expression of enzymes involved in sorbitol production and conversion in cultured human retinal pigment epithelial (RPE) cells.
Methods
Alterations in the expression of aldose reductase (AR) and sorbitol dehydrogenase (SDH) genes were examined with real-time RT-PCR. Protein levels were determined with Western blot analysis. Nuclear factor of activated T cell 5 (NFAT5) was knocked down with siRNA.
Results
AR gene expression in RPE cells was increased by high (25 mM) extracellular glucose, CoCl2 (150 μM)-induced chemical hypoxia, H2O2 (20 μM)-induced oxidative stress, and extracellular hyperosmolarity induced by addition of NaCl or sucrose. Extracellular hyperosmolarity (but not hypoxia) also increased AR protein level. SDH gene expression was increased by hypoxia and oxidative stress, but not extracellular hyperosmolarity. Hyperosmolarity and hypoxia did not alter the SDH protein level. The hyperosmotic AR gene expression was dependent on activation of metalloproteinases, autocrine/paracrine TGF-β signaling, activation of p38 MAPK, ERK1/2, and PI3K signal transduction pathways, and the transcriptional activity of NFAT5. Knockdown of NAFT5 or inhibition of AR decreased the cell viability under hyperosmotic (but not hypoxic) conditions and aggravated the hyperosmotic inhibition of cell proliferation.
Conclusions
The data suggest that sorbitol accumulation in RPE cells occurs under hyperosmotic, but not hypoxic and oxidative stress conditions. NFAT5- and AR-mediated sorbitol accumulation may protect RPE cells under conditions of osmotic stress.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Diabetic retinopathy is the leading cause of vision loss in working age adults [1]. Arterial vasoregression and capillary closure result in retinal ischemia-hypoxia and oxidative stress [2, 3], which initiate the development of retinal neovascularization and macular edema, the most relevant vision-threatening complications of diabetic retinopathy [1]. In addition to pathological alterations of the inner retina, diabetic retinopathy is characterized by early functional and degenerative alterations in the outer retina including the retinal pigment epithelium (RPE) resulting in, for example, a breakdown of the outer blood-retinal barrier [4–8]. Hyperglycemia is the primary and systemic hypertension is the main secondary risk factor of diabetic retinopathy [9, 10]. Control of blood pressure, even in the normotensive range, reduces the risk of diabetic retinopathy and prevents microvascular complications and vision loss from diabetic retinopathy independently of glycemia [11, 12].
Diabetes is associated with systemic and local osmotic stresses. Hyperglycemia entails systemic extracellular hyperosmolarity [13], and the increased glucose flux through the polyol pathway leads to intracellular sorbitol accumulation and increased intracellular osmotic pressure [14]. Activation of the polyol (sorbitol) pathway of glucose metabolism is suggested to be the main cause of diabetic retinal degeneration [15, 16]. In animal models, inhibition of sorbitol production prevents the apoptotic death of retinal neurons and other signs of diabetic retinopathy such as oxidative stress, pericyte loss, glial activation, edema, and neovascularization [17, 18].
The main condition that causes acute rises of the blood pressure is the increase of the extracellular osmolarity following intake of dietary salt (NaCl) [19]. Hypernatremia causes systemic hyperosmolarity [13, 20], which results in blood volume expansion and thus hypertension [19]. The plasma osmolarity and the blood pressure-raising effect of dietary salt increase with age [21, 22]. In experimental diabetic retinopathy, high salt intake aggravates diabetes-induced retinal alterations independently from changes in blood pressure [23]. Extracellular hyperosmolarity or increased extracellular NaCl also induce production of angiogenic cytokines in RPE cells [24, 25].
Cells possess a number of adaptive mechanisms that allow them to survive under osmotic stress conditions by the restoration of the osmotic balance. Cell survival under hyperosmotic conditions is initially maintained by the activation of ion transport systems and thereafter by intracellular accumulation of small organic osmolytes, in particular, sorbitol [26, 27]. Intracellular sorbitol accumulation upon hyperosmotic stress is mediated by increased production from glucose by aldose reductase (AR), the first enzyme of the polyol pathway [28]. Accumulation of sorbitol also requires attenuation of its conversion to fructose by sorbitol dehydrogenase (SDH), the second enzyme of the polyol pathway. In renal cells, hyperosmotic stress induces upregulation of AR and downregulation of SDH [26, 28]. The hyperosmotic transcriptional activation of the AR gene in renal cells is induced by nuclear factor of activated T cell 5 (NFAT5), also known as tonicity-responsive enhancer binding protein (TonEBP/OREBP) [29]. The RPE of the human eye contains large amounts of AR that are increased in diabetic retinopathy [4]. It was shown recently in mice that the retinal expression of NFAT5 is increased in diabetic retinopathy, and that knockdown of NFAT5 reduces the expression of AR and proapoptotic proteins and increases the expression of antiapoptotic proteins in the retina and RPE cells under hyperglycemic conditions [30]. Thus, NFAT5-induced AR expression may be crucially involved in mediating retinal degeneration under hyperglycemic conditions.
It was shown that high extracellular NaCl induces expression of AR in RPE cells [31, 32]. However, it is not known whether high NaCl also regulates the expression of the sorbitol-converting enzyme SDH, and whether further pathogenic factors of diabetic retinopathy, e.g., hypoxia and oxidative stress [1–3], regulate the expression of AR and SDH in RPE cells. Therefore, we compared the effects of high extracellular NaCl and further pathogenic conditions on the expression of enzymes involved in sorbitol production and conversion, i.e., AR and SDH, in cultured human RPE cells, and examined which intracellular signal transduction pathways and transcription factors mediate the effects of high extracellular NaCl and hypoxia on the expression of the AR gene. In addition, we determined the impact of NFAT5-mediated AR expression for the viability and proliferation of RPE cells under hyperosmotic and hypoxic conditions.
Material and methods
Materials
Tissue culture components and solutions were purchased from Gibco BRL (Paisley, UK). Fetal bovine serum was from Invitrogen (Paisley, UK). AG490, the inhibitor of hypoxia-inducible transcription factor 1 (HIF-1) 3-[2-(4-adamantan-1-yl-phenoxy)-acetylamino]-4-hydroxybenzoic acid methyl ester, LY294002, PD98059, SP600125, and SU1498 were obtained from Calbiochem (Bad Soden, Germany). AG1478 was from Alexis (Grünberg, Germany), and Stattic was from Enzo Life Science (Lörrach, Germany). A-438079, caffeic acid phenethyl ester, MRS2179, and SB203580 were obtained from Tocris (Ellisville, MO, USA). The recombinant human IL-1 receptor antagonist was from R&D Systems (Abingdon, UK). Ac-YVAD-CHO and human-specific small interfering RNA (siRNA) against NFAT5 (sc-43968) were purchased from Santa Cruz Biotechnology (Heidelberg, Germany). Nontargeted control siRNA was obtained from Qiagen (Hilden, Germany). Ethyl 1-benzyl-3-hydroxy-2(5H)-oxopyrrole-4-carboxylate (EBPC) and all other agents used were from Sigma-Aldrich (Taufkirchen, Germany), unless stated otherwise. The following antibodies were used: a rabbit anti-AR (1:1500; Thermo Scientific, Dreieich, Germany), a mouse anti-SDH (1:1000; Abcam, Cambridge, UK), a rabbit anti-β-actin (1:2000; Cell Signaling, Frankfurt/M., Germany), a goat anti-mouse IgG (1:2000; Cell Signaling), and a goat anti-rabbit IgG (1:2000; Cell Signaling).
Ethical approval
All procedures performed were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The use of human material was approved by the ethics committee of the University of Leipzig (approval #745, 07/25/2011). Informed consent was obtained from the relatives of all donors of eyes included in the study.
Cell culture
Post-mortem eyes from human cornea donors without reported eye disease were obtained within 48 h of death with the written informed consent from the relatives for the use of retinal tissue in basic science. RPE cells were prepared and cultured as described [33]. Cell lines derived from different donors were used in passage numbers 3 to 5. Certain experiments were also carried out using the human retinal glial (Müller) cell line MIO-M1 [34]. Near-confluent cultures were growth arrested in medium without serum for 16 h, and subsequently, serum-free media with and without test substances were added. The cells were preincubated with the pharmacological inhibitors for 30–60 min. Hyperglycemia was induced by addition of 25 mM glucose. Hyperosmotic media were made up by adding 100 mM NaCl or sucrose. Chemical hypoxia was induced by addition of CoCl2 (150 μM), and oxidative stress was induced by addition of H2O2 (20 μM).
Preparation of total RNA
Total RNA was extracted with the RNeasy Mini Kit (Qiagen, Hilden, Germany). The quality of the RNA was analyzed by agarose gel electrophoresis. The A260/A280 ratio of the optical density was measured using the NanoDrop 1000 device (Peqlab, Erlangen, Germany), and was between 1.8 and 2.1 for all RNA samples, indicating sufficient quality. After treatment with DNase I (Roche, Mannheim, Germany), cDNA was synthesized from 1 μg of total RNA using the RevertAid H Minus First Strand cDNA Synthesis kit (Fermentas, St. Leon-Roth, Germany).
Real-Time RT-PCR
Real-time RT-PCR was performed with the Single-Color Real-Time PCR Detection System (BioRad, Munich, Germany) using the primer pairs described in Table 1. The PCR solution contained 1 μL of cDNA, specific primer set (0.2 μM each) and 10 μL of a 2x mastermix (iQ SYBR Green Supermix, BioRad) in a final volume of 20 μL. The following conditions were used: initial denaturation and enzyme activation (one cycle at 95 °C for 3 min); denaturation, amplification and quantification, 45 cycles at 95 °C for 30 s, 58 °C for 20 s, and 72 °C for 45 s; melting curve, 55 °C with the temperature gradually increased (0.5 °C) up to 95 °C. The amplified samples were analyzed by standard agarose gel electrophoresis. The mRNA expression was normalized to the level of ß-actin mRNA. The changes in mRNA expression were calculated according to the 2-ΔΔCT method (CT, cycle threshold), with ΔCT = CTtarget gene - CTACTB and ΔΔCT = ΔCTtreatment - ΔCTcontrol.
Cell viability
Cell viability was determined by trypan blue exclusion. Cells were seeded at 5 × 104 cells per well in 6-well plates. After reaching a confluency of ∼90 %, the cells were cultured in serum-free medium for 5 h and then in fetal calf serum (0.5 %)-containing iso- or hyperosmotic medium (+100 mM NaCl), and in the presence of CoCl2 (150 μM), respectively, for 24 h. After trypsinization, the cells were stained with trypan blue (0.4 %), and the number of viable (non-stained) and dead (stained) cells were determined using a hemocytometer.
Cell proliferation
The proliferation rate of RPE cells was determined by measuring the incorporation of bromodeoxyuridine (BrdU) into the genomic DNA. Cells were seeded at 3 × 103 cells per well in 96-well microtiter plates (Greiner), and were allowed to attach for 48 h. Thereafter, the cells were growth arrested in medium without serum for 5 h and, subsequently, medium containing 0.5 % serum with and without test substances was added for another 24 h. BrdU incorporation was determined by using the Cell Proliferation ELISA BrdU Kit (Roche, Mannheim, Germany). BrdU (10 μM) was added to the culture medium 5 h before fixation.
Western blot analysis
Cells were seeded at 5 × 105 cells per well in 6-well plates in 1.5 mL of complete medium, and were allowed to growth up to a confluency of ∼80 %. After growth arrest for 16 h, the cells were treated with hyperosmotic medium (+100 mM NaCl) or CoCl2 (150 μM) for 6, 24, or 48 h. Then, the medium was removed, the cells were washed twice with prechilled phosphate-buffered saline (pH 7.4; Invitrogen), and the monolayer was scraped into 150 μL of lysis buffer (Mammalian Cell Lysis-1 Kit; Sigma). Total cell lysates were centrifuged at 10,000×g for 10 min, and the supernatants were analyzed by immunoblots. Equal amounts of proteins were separated by 10 % SDS-polyacrylamide gel electrophoresis. Immunoblots were probed with primary and secondary antibodies, and immunoreactive bands were visualized using 5-bromo-4-chloro-3-indolyl phosphate/nitro blue tetrazolium.
siRNA transfection
Cells were seeded at 7 × 104 cells per well in 12-well culture plates and were allowed to growth up to confluency of 60–80 %. Thereafter, the cells were transfected with NFAT5 siRNA (5 nM) and nontargeted siRNA (5 nM), respectively, using HiPerfect reagent (Qiagen) in F-10 medium containing 10 % fetal bovine serum according to the manufacturer’s instructions. After 48 h, the medium was removed and fresh medium without serum was added for 5 h. Thereafter, serum-free medium containing high (+100 mM) NaCl and CoCl2 (150 μM), respectively, was added for 24 h.
Statistics
For each test, at least three independent experiments using cells from different donors were carried out. Data are expressed as means ± SEM. Statistical analysis was made with Prism (Graphpad Software, San Diego, CA, USA). Significance was determined by one-way ANOVA followed by Bonferroni’s multiple comparison test and Mann–Whitney U test, respectively, and was accepted at P < 0.05.
Results
Regulation of AR and SDH gene expression
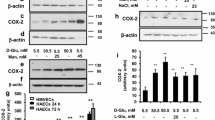
Hyperglycemia results in increased polyol pathway flux of glucose which leads to sorbitol accumulation in retinal cells [14, 17]. In order to determine whether hyperglycemia alters the gene expression of proteins involved in sorbitol synthesis and conversion in RPE cells in vitro (Fig. 1a), we stimulated cultured cells with high (25 mM) glucose. As shown in Fig. 1b, high glucose induced an increase in the expression of the AR gene while the expression of the SDH gene was initially decreased and then increased compared to the control level. In addition to hyperglycemia, hypoxia, and oxidative stress are known pathogenic factors of diabetic retinopathy [1–3]. In the presence of the hypoxia mimetic CoCl2 [35], the expression of AR and SDH genes was increased (Fig. 1c). Oxidative stress induced by addition of H2O2 to the culture medium induced significant increases (P < 0.05) in the expression of AR and SDH genes (Fig. 1d). In order to determine whether extracellular hyperosmolarity induces alterations in the expression of AR and SDH, we added NaCl (100 mM) to the culture medium. As shown in Fig. 1e, high NaCl induced a marked expression of the AR gene and did not significantly alter (P > 0.05) the expression of the SDH gene. The high NaCl-induced upregulation of the AR gene expression was dose-dependent (Fig. 1f). The expression of the AR gene was also increased by addition of sucrose (100 mM) to the culture medium (Fig. 1g). The expression of the AR gene induced by chemical hypoxia and high (+100 mM) NaCl was additive (Fig. 1h). This suggests that different intracellular signal transduction pathways mediate the induction of AR gene expression under both conditions.
Regulation of the expression of AR and SDH genes in RPE cells. mRNA levels were determined with real-time RT-PCR analysis after stimulation of the cells for 2, 6, and 24 h (as indicated by the panels of the bars) and are expressed as fold change relative to the unstimulated control (1). a mRNA expression in RPE cells from different donors (1, 2) determined by RT-PCR analysis. Negative controls (0) were done by adding double-distilled water instead of cDNA as template. b-e The cells were stimulated with high (25 mM) glucose (b), CoCl2 (150 μM; c), H2O2 (20 μM; d), and high (+100 mM) NaCl (e). f Dose-dependent effect of high extracellular NaCl on the cellular level of AR mRNA. The cells were cultured in media which were made up hyperosmotic by addition of 10 to 100 mM NaCl. g Effect of extracellular hyperosmolarity induced by addition of sucrose (100 mM) to the culture medium. h High (+100 mM) NaCl and CoCl2 (150 μM) stimulated additively the expression of AR and SDH genes. The data were obtained after 24 h of stimulation. Each bar represents data obtained in 4–10 independent experiments using cell lines from different donors. Significant difference vs. unstimulated control: *P < 0.05
A similar upregulation of the AR gene expression and no alteration in the SDH gene expression in the presence of high extracellular NaCl were observed in cells of a human retinal glial (Müller) cell line, MIO-M1 (Fig. 2a). High glucose induced a moderate increase in the AR mRNA level and no alteration of the SDH mRNA level in MIO-M1 cells (Fig. 2b). In contrast to the effect of chemical hypoxia in RPE cells (Fig. 1c), CoCl2 induced only moderate increases in the AR and SDH gene expression in MIO-M1 cells (Fig. 2c).
Regulation of the expression of AR and SDH genes in human retinal glial (MIO-M1) cells. mRNA levels were determined with real-time RT-PCR analysis after stimulation of the cells for 2, 6, and 24 h and are expressed as fold change relative to the unstimulated control (1). The cells were stimulated with high (+100 mM) NaCl (a), high (25 mM) glucose (b), and CoCl2 (150 μM; c), respectively. Each bar represents data obtained in 5–6 independent experiments. Significant difference vs. unstimulated control: *P < 0.05
In RPE cells, high (+100 mM) extracellular NaCl also induced an increase in the cellular AR protein level (Fig. 3a,c) while the SDH protein level remained unchanged (Fig. 3a,d). The increase in the cellular AR protein level was observed after 24 and 48 h, but not after 6 h, of stimulation (Fig. 3a). CoCl2 (150 μM)-induced chemical hypoxia did not alter the cellular levels of AR (Fig. 3a,c) and SDH proteins (Fig. 3a,d) in RPE cells.
Hyperosmotic stress induces time-dependent increase in AR protein content of RPE cells. a AR and SDH protein levels in lysates of cells that were cultured 6, 24, and 48 h in isoosmotic (control) and hyperosmotic (+100 mM NaCl) media and in isoosmotic medium containing CoCl2 (150 μM), respectively. β-Actin was used as a control for equal protein loading. b Negative controls obtained by omission of the first antibodies. c,d Mean ± SEM cellular levels of AR (c) and SDH (d) proteins, as determined by densitometric analysis. The data were normalized to the level of β-actin protein, and are expressed as percent of unstimulated control (100 %). Data were obtained with Western blot analysis in 3–4 independent experiments using cells from different donors. Equal amounts of protein (10 μg for AR and β-actin analysis, 20 μg for SDH analysis) were separated. Significant difference vs. unstimulated control (100 %): *P < 0.05. ●P < 0.05
Intracellular signaling involved in hyperosmotic and hypoxic AR gene expression
It was shown that high extracellular NaCl induces activation of various intracellular signal transduction pathways including p38 mitogen-activated protein kinase (p38 MAPK) and extracellular signal-regulated kinases 1 and 2 (ERK1/2) pathways in RPE cells [24, 36]. In order to determine the intracellular signaling that regulates the hyperosmotic expression of the AR gene in RPE cells, we tested pharmacological blockers of key intracellular signal transduction pathways. Under unstimulated control conditions, the cellular level of AR gene transcripts was moderately increased in the presence of the c-Jun NH2-terminal kinase (JNK) inhibitor SP600125 (Fig. 4a), suggesting that JNK activity inhibits the expression of the AR gene. The expression of the AR gene induced by high extracellular NaCl was significantly reduced (P < 0.05) by inhibitors of p38 MAPK, ERK1/2, and phosphatidylinositol-3 kinase (PI3K)-Akt signal transduction pathways (Fig. 4b). On the other hand, the JNK inhibitor SP600125 significantly increased (P < 0.05) the cellular level of AR gene transcripts in the presence of high extracellular NaCl (Fig. 4b), suggesting that JNK activity also inhibits the expression of the AR gene under hyperosmotic conditions. The increase in the cellular level of AR gene transcripts induced by the hypoxia mimetic CoCl2 was reduced by inhibitors of p38 MAPK, ERK1/2, JNK, and PI3K signal transduction pathways (Fig. 4c). The data suggest that both high extracellular NaCl and hypoxia induce expression of the AR gene by activation of various intracellular signal transduction pathways. JNK activity results in inhibition of AR gene expression under control and hyperosmotic conditions, but is involved in mediating AR gene expression under hypoxic conditions.
Cellular signaling involved in osmotic (b) and hypoxic (c) induction of AR gene expression in RPE cells. The AR mRNA level was determined with real-time RT-PCR analysis in cells cultured 24 h in isoosmotic control medium (a), hyperosmotic medium (+100 mM NaCl; b), and in the presence of CoCl2 (150 μM; c), respectively, and is expressed as fold change relative to the unstimulated control (1). The following inhibitors of intracellular signal transduction molecules were tested: the inhibitor of p38 MAPK activation, SB203580 (10 μM), the inhibitor of ERK1/2 activation, PD98059 (20 μM), the JNK inhibitor SP600125 (10 μM), and the inhibitor of PI3K-related kinases, LY294002 (5 μM). The following receptor and metalloproteinase inhibitors were tested: the inhibitor of VEGF receptor-2, SU1498 (10 μM), the inhibitor of the PDGF receptor tyrosine kinase, AG1296 (10 μM), the inhibitor of the EGF receptor tyrosine kinase, AG1478 (600 nM), the inhibitor of TGF-β1 superfamily activin receptor-like kinase receptors, SB431542 (10 μM), the FGF receptor kinase inhibitor, PD173074 (500 nM), and the broad-spectrum metalloproteinase inhibitor 1,10-phenanthroline (1,10-Phen; 10 μM), the P2Y1 receptor antagonist MRS2179 (30 μM), and the P2X7 receptor antagonist A-438079 (50 nM). The following inhibitors of transcription factors were tested: a HIF inhibitor (HIF Inh; 5 μM), the STAT3 inhibitor Stattic (1 μM), and the NF-kB inhibitor caffeic acid phenethyl ester (CAPE; 1 μg/mL). In addition, triamcinolone acetonide (Triam; 150 μM), the caspase-1 inhibitor Ac-YVAD-CHO (Ac-Y; 500 nM), and a recombinant human IL-1 receptor antagonist (IL1RA; 1 μg/mL) were tested. Vehicle controls were made with dimethylsulfoxide (DMSO; 1:1000), phosphate-buffered saline (PBS; 1:2000), and ethanol (1:1000). Each bar represents data obtained in 3–22 independent experiments using cell lines from different donors. Significant difference vs. unstimulated control: *P < 0.05. Significant difference vs. NaCl control: ●P < 0.05. Significant difference vs. CoCl2 control: ○P < 0.05
Anti-inflammatory steroids such as triamcinolone acetonide are clinically used for the rapid resolution of diabetic retinal edema [37]. Triamcinolone acetonide did not alter the cellular level of AR gene transcripts under control, hyperosmotic, and hypoxic conditions (Fig. 4a–c). In addition, a caspase-1 inhibitor (Ac-YVAD-CHO) and a recombinant human IL-1 receptor antagonist had no effects (Fig. 4b), suggesting that activation of inflammasomes (i.e., cytosolic protein-signaling complexes which drive the activation of caspase-1 and maturation of the inflammatory cytokine IL-1β [38]) is not involved in mediating the hyperosmotic expression of the AR gene.
Intracellular signaling involved in hypoxic SDH gene expression
Under unstimulated control conditions, the cellular level of SDH gene transcripts was increased in the presence of the JNK inhibitor SP600125 (Fig. 5a). This suggests that, under control conditions, JNK activity inhibits the expression of both AR and SDH genes. The hypoxic SDH gene expression was significantly reduced (P < 0.05) in the presence of an inhibitor of the PI3K-Akt signal transduction pathway and of triamcinolone acetonide (Fig. 5b).
Cellular signaling involved in hypoxic induction of SDH gene expression in RPE cells. The SDH mRNA level was determined with real-time RT-PCR analysis in cells cultured 24 h in isoosmotic control medium (a) and in the presence of CoCl2 (150 μM; b), respectively, and is expressed as fold change relative to the unstimulated control (1). The following inhibitors of intracellular signal transduction molecules were tested: the inhibitor of p38 MAPK activation, SB203580 (10 μM), the inhibitor of ERK1/2 activation, PD98059 (20 μM), the JNK inhibitor SP600125 (10 μM), and the inhibitor of PI3K-related kinases, LY294002 (5 μM). The following inhibitors of receptor kinases and metalloproteinases were tested: the inhibitor of VEGF receptor-2, SU1498 (10 μM), the inhibitor of the PDGF receptor tyrosine kinase, AG1296 (10 μM), the inhibitor of the EGF receptor tyrosine kinase, AG1478 (600 nM), the inhibitor of TGF-β1 superfamily activin receptor-like kinase receptors, SB431542 (10 μM), the FGF receptor kinase inhibitor, PD173074 (500 nM), and the broad-spectrum metalloproteinase inhibitor 1,10-phenanthroline (1,10-Phen; 10 μM). The following inhibitors of transcription factors were tested: a HIF inhibitor (HIF Inh; 5 μM), the STAT3 inhibitor Stattic (1 μM), and the NF-kB inhibitor caffeic acid phenethyl ester (CAPE; 1 μg/mL). In addition, triamcinolone acetonide (Triam; 150 μM) was tested. Vehicle control was made with dimethylsulfoxide (DMSO; 1:1000). Each bar represents data obtained in 3–15 independent experiments using cell lines from different donors. Significant difference vs. unstimulated control: *P < 0.05. Significant difference vs. CoCl2 control: ○P < 0.05
Extracellular signaling involved in hyperosmotic and hypoxic AR gene expression
We described recently that extracellular hyperosmolarity induces secretion of vascular endothelial growth factor (VEGF), basic fibroblast growth factor (bFGF), and transforming growth factor (TGF)-β from RPE cells [24, 25]. In order to determine whether autocrine/paracrine growth factor receptor signaling is required for the hyperosmotic expression of the AR gene in RPE cells, we tested inhibitors of receptor kinases. Under unstimulated control conditions, the cellular level of AR gene transcripts was moderately increased in the presence of the inhibitor of VEGF receptor-2, SU1498 (Fig. 4a). This suggests that RPE cells constitutively secrete VEGF which activates VEGF receptors in an autocrine/paracrine manner; autocrine activation of VEGF receptors results in suppression of AR gene expression. The expression of the AR gene induced by high extracellular NaCl was significantly reduced (P < 0.05) by the inhibitor of TGF-β1 superfamily activin receptor-like kinase receptors, SB431542, and the metalloproteinase inhibitor 1,10-phenanthroline (Fig. 4b). This suggests that the hyperosmotic expression of the AR gene is, at least in part, mediated by a release of TGF-β and subsequent autocrine/paracrine activation of the respective receptors. Activation of matrix metalloproteinases (MMPs) may be involved in shedding growth factors, e.g., TGF-β [39], from the extracellular matrix. Inhibitors of PDGF and EGF receptor tyrosine kinases (AG1296 and AG1478, respectively), and of purinergic P2Y1 (MRS2179) and P2X7 receptors (A-438079) had no effect on the hyperosmotic expression of the AR gene (Fig. 4b). We found that inhibitors of the VEGF receptor-2 and the FGF receptor tyrosine kinase significantly increased (P < 0.05) the cellular level of AR gene transcripts in the presence of high extracellular NaCl (Fig. 4b). The data suggest that autocrine/paracrine VEGF and bFGF signaling inhibits the expression of the AR gene under hyperosmotic conditions. The hypoxic expression of the AR gene was reduced in the presence of inhibitors of platelet-derived growth factor (PDGF) and epidermal growth factor (EGF) receptor tyrosine kinases, and of TGF-β1 superfamily activin receptor-like kinase receptors (Fig. 4c). The data may suggest that hypoxic induction of the AR gene expression is, at least in part, mediated by autocrine/paracrine PDGF, EGF, and TGF-β signaling.
Extracellular signaling involved in hypoxic SDH gene expression
Under unstimulated control conditions, the cellular level of SDH gene transcripts was increased in the presence of the inhibitor of VEGF receptor-2, SU1498 (Fig. 5a). The data suggest that autocrine/paracrine VEGF signaling inhibits the expression of both AR and SDH genes under control conditions. The CoCl2-induced expression of the SDH gene (Fig. 1c) is reduced in the presence of inhibitors of PDGF and EGF receptor tyrosine kinases (Fig. 5b). The data may suggest that autocrine/paracrine PDGF and EGF signaling is involved in mediating the expression of the SDH gene under hypoxic conditions.
Role of transcription factor activities in hyperosmotic and hypoxic AR gene expression
In order to determine which transcription factors mediate the hyperosmotic and hypoxic induction of AR gene expression, we tested pharmacological inhibitors. Under unstimulated control conditions, the cellular level of AR gene transcripts was increased in the presence of the nuclear factor (NF)-kB inhibitor caffeic acid phenethyl ester [40] (Fig. 4a), suggesting that NF-kB activity normally inhibits the expression of the AR gene. The high NaCl-induced expression of the AR gene remained unaltered in the presence of inhibitors of HIF-1 [41], signal transducer and activator of transcription 3 (STAT3) [42], and NF-kB (Fig. 4b). The CoCl2-induced expression of the AR gene was significantly (P < 0.05) reduced by HIF and STAT3 inhibitors, and remained unaltered in the presence of the NF-kB inhibitor (Fig. 4c).
The activity of NFAT5 is critically involved in the cellular adaptation to hyperosmotic stress [27]. We described recently that high extracellular NaCl induces increased NFAT5 gene and protein expression, and DNA binding of NFAT5, in RPE cells [24]. AR is a prototypical NFAT5 target gene [43]. It is known that the expression of the AR gene in RPE cells in response to hyperglycemia is dependent on NFAT5 activity [30]. However, it is not known whether the expression of the AR gene in response to high NaCl (Fig. 1e) and CoCl2-induced chemical hypoxia (Fig. 1c) also depends on NFAT5 activity. In order to prove the role of NFAT5 activity in the expression of the AR gene, we knocked down NFAT5 with siRNA. Transfection with NFAT5 siRNA reduced significantly (P < 0.05) the level of NFAT5 gene transcripts by approximatly 60 % in RPE cells cultured for 24 h in hyperosmotic medium (Fig. 6a) and in isoosmotic medium containing CoCl2 (Fig. 6b), respectively, when compared to cells transfected with nontargeted siRNA. Transfection with a nontargeted siRNA did not alter the cellular level of NFAT5 gene transcripts under both conditions (Fig. 6a,b). Cells transfected with NFAT5 siRNA displayed also a reduced expression level of the AR gene (Fig. 6a) under hyperosmotic, but not under hypoxic conditions (Fig. 6b) when compared to cells transfected with nontargeted siRNA. The data suggest that the hyperosmotic induction of AR gene expression is, at least in part, mediated by NFAT5 activity, but not by the activities of HIF-1, STAT3, and NF-kB. On the other hand, the hypoxic AR gene expression is mediated by HIF-1 and STAT3 activities, but not by the activities of NF-kB and NFAT5.
The hyperosmotic, but not the hypoxic expression of the AR gene depends on the activity of NFAT5. mRNA levels were determined by real-time RT-PCR analysis after stimulation of the cells for 24 h with a hyperosmotic (+100 mM NaCl) medium and an isoosmotic medium containing CoCl2 (150 μM), respectively. mRNA data were normalized to control values (1) obtained in nontransfected cells. a Knocking down the gene expression of NFAT5 with siRNA (siNFAT5; 5 nM) reduced the levels of NFAT5 and AR mRNAs in cells cultured in hyperosmotic medium when compared to cells transfected with nontargeted siRNA (siNon; 5 nM). b In cells cultured in the presence of CoCl2, NFAT5 siRNA (siNFAT5; 5 nM) reduced the level of NFAT5 mRNA, but not the level of AR mRNA, when compared to cells transfected with nontargeted siRNA (siNon; 5 nM). Each bar represents data obtained in 3–5 independent experiments using cell lines from different donors. Significant difference vs. nontargeted siRNA: *P < 0.05
Role of transcription factor activities in hypoxic SDH gene expression
Under unstimulated control conditions, the cellular level of SDH gene transcripts was increased in the presence of a NF-kB (Fig. 5a). This suggests that NF-kB activity normally inhibits the expression of both AR (Fig. 4a) and SDH genes. The SDH gene expression induced by chemical hypoxia (Fig. 1c) was significantly reduced (P < 0.05) by HIF and STAT3 inhibitors (Fig. 5b), suggesting that the hypoxic expression of the SDH gene is mediated by the activities of HIF-1 and STAT3.
Roles of AR and NFAT5 activities in cell viability and proliferation
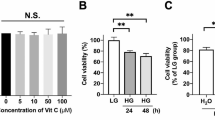
In various cell systems, the transcriptional activity of NFAT5 is critical for the cell survival under hyperosmotic conditions [44, 45]. However, knockdown of retinal NFAT5 was recently shown to have antiapoptotic effects in experimental diabetic retinopathy, suggesting that NFAT5 activity may contribute to retinal degeneration [30]. In order to prove whether NFAT5 activity has pro- or antisurvival effects in RPE cells under hyperosmotic and hypoxic conditions, we knocked down NFAT5 with siRNA. To determine the role of AR activity, we used the selective AR inhibitor EBPC [46]. As shown in Fig. 7a, an increase of the extracellular NaCl level induced a moderate, dose-dependent decrease in the viability of RPE cells. CoCl2-induced chemical hypoxia did not significantly decrease (P > 0.05) the cell viability (Fig. 7a). The AR inhibitor EBPC decreased significantly (P < 0.05) the viability of RPE cells under hyperosmotic, but not under control and hypoxic conditions (Fig. 7b), suggesting that aldose reductase activity plays a protective role in RPE cells in osmotic stress. Transfection of the cells with NFAT5 siRNA or nontargeted siRNA did not alter the cell viability under unstimulated control conditions (Fig. 7c). RPE cells transfected with NFAT5 siRNA displayed a significantly reduced (P < 0.05) viability under hyperosmotic (+100 mM NaCl) conditions compared to nontransfected cells and to cells transfected with nontargeted negative control siRNA (Fig. 7c). In contrast, transfection with NFAT5 siRNA did not alter the viability of RPE cells in chemical hypoxia (Fig. 7c).
Involvement of AR and NFAT5 activities in the maintenance of RPE cell viability and proliferation under hyperosmotic and hypoxic conditions. Extracellular hyperosmolarity was induced by addition of NaCl to the culture medium; chemical hypoxia was induced by addition of CoCl2. Data were obtained after 24 h of stimulation and are expressed as percent of unstimulated control (100 %). a Dose-dependent alteration of the cell viability induced by high extracellular NaCl. The doses of NaCl (in mM) added to the culture media are given in the bars. CoCl2 (150 μM) had no effect on the cell viability. b Effect of the AR inhibitor EBPC (1 μM) on the cell viability. EBPC was tested in the absence and presence of high (+100 mM) extracellular NaCl and CoCl2 (150 μM), respectively. c Effect of NFAT5 gene expression depletion with siRNA (siNFAT5; 5 nM) on the cell viability under unstimulated control conditions and in the presence of high (+100 mM) extracellular NaCl and CoCl2 (150 μM), respectively. As control, nontargeted negative control siRNA (siNon; 5 nM) was used. d Dose-dependent decreases of the proliferation rate induced by high extracellular NaCl and CoCl2, respectively. The doses of NaCl (mM) and CoCl2 (μM) added to the culture media are given in the bars. e Effect of the AR inhibitor EBPC (1 μM) on the proliferation rate. EBPC was tested in the absence and presence of high (100 mM) extracellular NaCl and CoCl2 (150 μM), respectively. f Effect of NFAT5 gene expression depletion with siRNA (siNFAT5; 5 nM) on the proliferation rate of cells cultured in isoosmotic control medium, and in the presence of high NaCl (+100 mM) and CoCl2 (150 μM), respectively. As controls, transfection reagent (TR) and nontargeted negative control siRNA (siNon; 5 nM) were used. Each bar represents data obtained in 3–11 independent experiments using cell lines from different donors. Significant difference vs. unstimulated control: *P < 0.05. Significant difference vs. NaCl control: ●P < 0.05. ○P < 0.05. n.s., not significant
High extracellular NaCl and CoCl2-induced chemical hypoxia induced strong dose-dependent decreases in the proliferation of RPE cells (Fig. 7d). The AR inhibitor EBPC decreased significantly (P < 0.05) the proliferation rate of RPE cells under hyperosmotic, but not under control and hypoxic conditions (Fig. 7e). Transfection of the cells with NFAT5 siRNA or nontargeted siRNA did not alter the proliferation rate under unstimulated control conditions (Fig. 7f). RPE cells transfected with NFAT5 siRNA displayed a significantly reduced (P < 0.05) proliferation rate under hyperosmotic (+100 mM NaCl) conditions compared to cells transfected with nontargeted siRNA and to non-transfected cells in the absence and presence of transfection reagent, respectively (Fig. 7e). In contrast, transfection with NFAT5 siRNA did not alter the proliferation rate of RPE cells in chemical hypoxia (Fig. 7e). The data indicate that knockdown of NFAT5 increases the cell cycle arrest in RPE cells under hyperosmotic, but not hypoxic, conditions.
Discussion
Activation of the polyol pathway under hyperglycemic conditions is suggested to be a main cause of diabetes-induced tissue damage [15, 16]. The cellular sorbitol level depends on the balance between sorbitol production from glucose and conversion to fructose. Here, we show that the gene expression of the sorbitol-producing enzyme AR in RPE cells is stimulated by various pathological conditions including high extracellular glucose (Fig. 1b), chemical hypoxia (Fig. 1c), oxidative stress (Fig. 1d), and NaCl- (Fig. 1e,f) or sucrose-induced extracellular hyperosmolarity (Fig. 1g). NaCl-induced extracellular hyperosmolarity, but not CoCl2-induced hypoxia, also induced increased AR protein content of RPE cells (Fig. 3a, c). A similar effect of high extracellular NaCl on the AR gene expression was found in cells of a human retinal glial cell line (Fig. 2a). The present results are in agreement with previous studies which showed that high extracellular NaCl induces AR gene expression in RPE cells [31, 32] and that AR gene transcription in various cell systems including RPE cells is also nonosmotically regulated, e.g., by oxidative stress [47, 48].
The gene expression of the sorbitol-converting enzyme SDH in RPE cells is differentially regulated under various conditions. High extracellular glucose induced initial downregulation followed by upregulation of SDH gene expression (Fig. 1b). The expression of the SDH gene was also increased by chemical hypoxia and oxidative stress (Fig. 1c,d), but not by NaCl- or sucrose-induced hyperosmolarity (Fig. 1e, g). NaCl-induced extracellular hyperosmolarity did also not induce increased SDH protein content of RPE cells (Fig. 3a, d). Although chemical hypoxia induced increased expression of the SDH gene (Fig. 1c), it did not induce increased SDH protein content of the cells (Fig. 3a, d). The data suggest that extracellular hyperosmolarity, but not hypoxia, results in sorbitol accumulation in RPE cells.
The expression of the AR gene induced by chemical hypoxia and high NaCl was additive (Fig. 1h). This suggests that the induction of AR gene expression under both conditions is mediated by different mechanisms. Indeed, we found that different cellular signal transduction pathways and transcription factors mediate the effects of chemical hypoxia and high extracellular NaCl on the expression of the AR gene. The hyperosmotic stimulation of the AR gene expression is mediated by autocrine/paracrine TGF-β signaling and the activity of NFAT5, and is counterbalanced by autocrine/paracrine VEGF and FGF signaling (Fig. 8b). A suppression of AR gene expression by autocrine VEGF signaling was also found under isoosmotic control conditions (Fig. 8a). The hypoxic stimulation of AR gene expression is mediated by autocrine/paracrine PDGF, EGF, and TGF-β signaling, and the activities of HIF-1 and STAT3 (Fig. 5b). We found a slow time dependency of the hyperosmotic expression of the AR gene, with maximal increase after 24 h of stimulation (Fig. 1e, g), which can be explained by the fact that human RPE cells normally contains large amounts of AR [4]. In renal cells, the hyperosmotic activation of NFAT5, resulting in an increased amount of NFAT5 and translocation to the nucleus, is slow and usually requires 24–48 h for full activation [29]. In RPE cells, upregulation of NFAT5 gene and protein expression was observed after 6 h of stimulation with high NaCl [24]. We found that inhibition of VEGF receptor-2 increases AR gene expression under iso- and hyperosmotic conditions (Fig. 4a, b), suggesting that autocrine/paracrine VEGF signaling suppresses AR gene expression. Agents that inhibit VEGF activity are clinically used in the treatment of diabetic macular edema [49], suggesting that anti-VEGF therapies may also modulate the AR level in RPE cells.
Schematic summary of the signal transduction pathways involved in hyperosmotic expression of AR in RPE cells. a Under unstimulated control conditions, autocrine/paracrine VEGF signaling and the activities of JNK and NF-kB inhibit the expression of AR and SDH genes. b High extracellular NaCl induces expression of the AR gene which is mediated by autocrine/paracrine TGF-β signaling and the activities of matrix metalloproteinases, p38 MAPK, ERK1/2, PI3K, and NFAT5. Autocrine/paracrine VEGF and FGF signaling, and JNK activity, reduce the AR gene expression induced by high NaCl. High extracellular NaCl also induces increased level of AR protein. AR catalyzes the production of sorbitol from glucose while the conversion of sorbitol to fructose is limited because the level of SDH protein is not increased. This results in intracellular accumulation of sorbitol and increased intracellular osmolarity, which compensates the osmotic gradient across the plasma membrane under high NaCl conditions
NFAT5-mediated transcription of osmoprotective genes is critical for cellular survival under hyperosmotic stress [27, 44, 45]. However, it was shown that NFAT5-induced AR expression is also involved in mediating retinal degeneration under hyperglycemic conditions [30]. Here, we show that high extracellular osmolarity results in a moderate decrease of the RPE cell viability (Fig. 7a) and a strong decrease in the proliferation rate (Fig. 7d). The data are in agreement with previous studies which showed that high extracellular osmolarity induces cell cycle arrest in various cell systems including RPE cells [36, 47]. We also found that chemical hypoxia does not alter the viability of RPE cells (Fig. 7a), but strongly decreases cellular proliferation (Fig. 7d). Inhibition of AR activity or knocking down NFAT5 decreased the cell viability (Fig. 7b, c) and reduced cellular proliferation (Fig. 7e, f) under hyperosmotic conditions. These effects were not observed under hypoxic conditions. The data suggest that NFAT5 and AR activities are required to maintain RPE cell viability and a distinct level of RPE cell proliferation under osmotic stress conditions. It can be concluded that inhibition of NFAT5 may aggravate osmotic injury of RPE cells. The present data which show a protective role of NFAT5 activity in osmotic stress are in contradiction to a recent study which showed that knockdown of NFAT5 has protective effects in RPE cells under high-glucose conditions [30]. The reasons for the different findings are unclear and may be related to different stimulation conditions.
The high glucose-induced regulation of SDH gene expression found in the present study (Fig. 1b) suggests a biphasic regulation of sorbitol production in RPE cells under hyperglycemic conditions; the initial downregulation of the SDH gene expression may support intracellular accumulation of sorbitol, while the long-lasting upregulation of the SDH gene expression may support the conversion of sorbitol to fructose. Apparently, the cells switch from accumulation to conversion of sorbitol when sufficient sorbitol is produced to compensate the osmotic gradient caused by the hyperglycemic conditions used in the present study. The data support the assumption that sorbitol accumulation in RPE cells occurs under osmotic stress conditions induced by elevated extracellular glucose or NaCl, or by addition of sucrose to the culture medium. Under conditions which are not associated with osmotic stress, e.g., long-lasting exposure of high glucose, hypoxia, and oxidative stress, sorbitol is converted to fructose. This assumption is in agreement with a previous study, which showed increased levels of both sorbitol and fructose in the retina of diabetic rats [17]. It is conceivable, but remains to be proven, that in diabetic retinopathy, NFAT5-induced upregulation of AR is protective to compensate osmotic gradients; however, increased glucose flux through the polyol pathway caused by upregulation of both AR and SDH may have deleterious effects on retinal cell survival, possibly via the induction of oxidative/nitrosative stress and production of inflammatory mediators [50–52], which are also causative factors of osmotic retinal cell swelling [53]. The role of the polyol pathway activation in inducing retinal cell death under hyperglycemic conditions remains to be further determined.
Systemic hypertension is the most important secondary risk factor of diabetic retinopathy [9, 10]. Because acute hypertension mainly results from high extracellular osmolarity following intake of dietary salt [19], we investigated whether extracellular hyperosmolarity induces alterations of sorbitol-producing and -converting enzymes in RPE cells. The impact of high extracellular NaCl for the development of diabetic retinopathy is also emphasized by animal studies, which showed that high-salt diet aggravates degenerative retinal alterations in diabetes such as intracellular edema in retinal ganglion cells and mitochondrial swelling in glial cells [23]. Here, we show that high extracellular osmolarity induces expression of the sorbitol-producing, but not the sorbitol-converting enzyme, in RPE (Figs. 1e, g and 3a, c, d) and retinal glial cells (Fig. 2a). Both alterations may stimulate the production of sorbitol resulting in compensation of the osmotic gradient, which increases the viability of RPE cells under hyperosmotic conditions (Fig. 7b, c). However, overproduction of sorbitol may result in osmotic cell injury. It remains to be determined whether aldose reductase inhibition has different effects on cell viability in dependence on the level or duration of the extracellular osmolarity increase and under various pathogenic conditions. The present data may suggest that one mechanism by which high intake of dietary salt aggravates diabetic retinopathy is a direct effect of elevated extracellular osmolarity on RPE and glial cells, independently of hypertension. The contradictory effects of sorbitol production in dependence on the level and duration of the extracellular osmolarity increase may explain the limited benefits of aldose reductase inhibitors in the treatment of diabetic retinopathy [54].
References
Cunha-Vaz J, Ribeiro L, Lobo C (2014) Phenotypes and biomarkers of diabetic retinopathy. Prog Retin Eye Res 41:90–111
Kowluru RA (2005) Diabetic retinopathy: mitochondrial dysfunction and retinal capillary cell death. Antioxid Redox Signal 7:1581–1587
Zheng L, Kern TS (2009) Role of nitric oxide, superoxide, peroxynitrite and PARP in diabetic retinopathy. Front Biosci 14:3974–3987
Vinores SA, van Niel E, Swerdloff JL, Campochiaro PA (1993) Electron microscopic immunocytochemical demonstration of blood-retinal barrier breakdown in human diabetics and its association with aldose reductase in retinal vascular endothelium and retinal pigment epithelium. Histochem J 25:648–663
Aizu Y, Oyanagi K, Hu J, Nakagawa H (2002) Degeneration of retinal neuronal processes and pigment epithelium in the early stage of the streptozotocin-diabetic rats. Neuropathology 22:161–170
Xu H, Song Z, Fu S, Zhu M, Le Y (2011) RPE barrier breakdown in diabetic retinopathy: seeing is believing. J Ocul Biol Dis Inform 4:83–92
Omri S, Behar-Cohen F, Rothschild PR, Gélizé E, Jonet L, Jeanny JC, Omri B, Crisanti P (2013) PKCζ mediates breakdown of outer blood-retinal barriers in diabetic retinopathy. PLoS One 8, e81600
Énzsöly A, Szabó A, Kántor O, Dávid C, Szalay P, Szabó K, Szél Á, Németh J, Lukáts Á (2014) Pathologic alterations of the outer retina in streptozotocin-induced diabetes. Invest Ophthalmol Vis Sci 55:3686–3699
Klein R, Klein BE, Moss SE, Cruickshanks KJ (1998) The Wisconsin Epidemiologic Study of Diabetic Retinopathy: XVII. The 14-year incidence and progression of diabetic retinopathy and associated risk factors in type 1 diabetes. Ophthalmology 105:1801–1815
Kamoi K, Takeda K, Hashimoto K, Tanaka R, Okuyama S (2013) Identifying risk factors for clinically significant diabetic macula edema in patients with type 2 diabetes mellitus. Curr Diabetes Rev 9:209–217
UK Prospective Diabetes Study Group (1998) Tight blood pressure control and risk of macrovascular and microvascular complications in type 2 diabetes: UKPDS 38. BMJ 317:703–713
Adler AI, Stratton IM, Neil HA, Yudkin JS, Matthews DR, Cull CA, Wright AD, Turner RC, Holman RR (2000) Association of systolic blood pressure with macrovascular and microvascular complications of type 2 diabetes (UKPDS 36): prospective observational study. BMJ 321:412–419
Neuhofer W (2010) Role of NFAT5 in inflammatory disorders associated with osmotic stress. Curr Genomics 11:584–590
Hammes HP (2003) Pathophysiological mechanisms of diabetic angiopathy. J Diabetes Complicat 17(2 Suppl):16–19
Dagher Z, Park YS, Asnaghi V, Hoehn T, Gerhardinger C, Lorenzi M (2004) Studies of rat and human retinas predict a role for the polyol pathway in human diabetic retinopathy. Diabetes 53:2404–2411
Chung SS, Chung SK (2005) Aldose reductase in diabetic microvascular complications. Curr Drug Targets 6:475–486
Asnaghi V, Gerhardinger C, Hoehn T, Adeboje A, Lorenzi M (2003) A role for the polyol pathway in the early neuroretinal apoptosis and glial changes induced by diabetes in the rat. Diabetes 52:506–511
Cheung AK, Fung MK, Lo AC, Lam TT, So KF, Chung SS, Chung SK (2005) Aldose reductase deficiency prevents diabetes-induced blood-retinal barrier breakdown, apoptosis, and glial reactivation in the retina of db/db mice. Diabetes 54:3119–3125
He FJ, Markandu ND, Sagnella GA, de Wardener HE, MacGregor GA (2005) Plasma sodium: ignored and underestimated. Hypertension 45:98–102
Obika LO, Amabebe E, Ozoene JO, Inneh CA (2013) Thirst perception, plasma osmolality and estimated plasma arginine vasopressin concentration in dehydrated and oral saline loaded subjects. Niger J Physiol Sci 28:83–89
Kenney WL, Chiu P (2001) Influence of age on thirst and fluid intake. Med Sci Sports Exerc 33:1524–1532
Khaw KT, Barrett-Connor E (1988) The association between blood pressure, age and dietary sodium and potassium: a population study. Circulation 77:53–61
Qin Y, Xu G, Fan J, Witt RE, Da C (2009) High-salt loading exacerbates increased retinal content of aquaporins AQP1 and AQP4 in rats with diabetic retinopathy. Exp Eye Res 89:741–747
Hollborn M, Vogler S, Reichenbach A, Wiedemann P, Bringmann A, Kohen L (2015) Regulation of the hyperosmotic induction of aquaporin 5 and VEGF in retinal pigment epithelial cells: involvement of NFAT5. Mol Vis 21:360–377
Veltmann M, Hollborn M, Reichenbach A, Wiedemann P, Kohen L, Bringmann A (2016) Osmotic induction of angiogenic growth factor expression in human retinal pigment epithelial cells. PLoS One 11, e0147312
Klawitter J, Rivard CJ, Brown LM, Capasso JM, Almeida NE, Maunsbach AB, Pihakaski-Maunsbach K, Berl T, Leibfritz D, Christians U, Chan L (2008) A metabonomic and proteomic analysis of changes in IMCD3 cells chronically adapted to hypertonicity. Nephron Physiol 109:1–10
Cheung CY, Ko BC (2013) NFAT5 in cellular adaptation to hypertonic stress - regulations and functional significance. J Mol Signal 8:5
Moriyama T, Garcia-Perez A, Burg MB (1989) Osmotic regulation of aldose reductase protein synthesis in renal medullary cells. J Biol Chem 264:16810–16814
Miyakawa H, Woo SK, Dahl SC, Handler JS, Kwon HM (1999) Tonicity-responsive enhancer binding protein, a rel-like protein that stimulates transcription in response to hypertonicity. Proc Natl Acad Sci U S A 96:2538–2542
Park J, Kim H, Park SY, Lim SW, Kim YS, Lee DH, Roh GS, Kim HJ, Kang SS, Cho GJ, Jeong BY, Kwon HM, Choi WS (2014) Tonicity-responsive enhancer binding protein regulates the expression of aldose reductase and protein kinase Cδ in a mouse model of diabetic retinopathy. Exp Eye Res 122:13–19
Lin LR, Carper D, Yokoyama T, Reddy VN (1993) The effect of hypertonicity on aldose reductase, alpha B-crystallin, and organic osmolytes in the retinal pigment epithelium. Invest Ophthalmol Vis Sci 34:2352–2359
Sato S, Lin LR, Reddy VN, Kador PF (1993) Aldose reductase in human retinal pigment epithelial cells. Exp Eye Res 57:235–241
Chen R, Hollborn M, Grosche A, Reichenbach A, Wiedemann P, Bringmann A, Kohen L (2014) Effects of the vegetable polyphenols epigallocatechin-3-gallate, luteolin, apigenin, myricetin, quercetin, and cyanidin in retinal pigment epithelial cells. Mol Vis 20:242–258
Limb GA, Salt TE, Munro PM, Moss SE, Khaw PT (2002) In vitro characterization of a spontaneously immortalized human Müller cell line (MIO-M1). Invest Ophthalmol Vis Sci 43:864–869
An WG, Kanekal M, Simon MC, Maltepe E, Blagosklonny MV, Neckers LM (1998) Stabilization of wild-type p53 by hypoxia-inducible factor 1α. Nature 392:405–408
Arsenijevic T, Vujovic A, Libert F, Op de Beeck A, Hébrant A, Janssens S, Grégoire F, Lefort A, Bolaky N, Perret J, Caspers L, Willermain F, Delporte C (2013) Hyperosmotic stress induces cell cycle arrest in retinal pigmented epithelial cells. Cell Death Dis 4, e662
Fraser-Bell S, Kaines A, Hykin PG (2008) Update on treatments for diabetic macular edema. Curr Opin Ophthalmol 19:185–189
Latz E, Xiao TS, Stutz A (2013) Activation and regulation of the inflammasomes. Nat Rev Immunol 13:397–411
Yu Q, Stamenkovic I (2000) Cell surface-localized matrix metalloproteinase-9 proteolytically activates TGF-β and promotes tumor invasion and angiogenesis. Genes Dev 14:163–176
Natarajan K, Singh S, Burke TR Jr, Grunberger D, Aggarwal BB (1996) Caffeic acid phenethyl ester is a potent and specific inhibitor of activation of nuclear transcription factor NF-kB. Proc Natl Acad Sci U S A 93:9090–9095
Lee K, Lee JH, Boovanahalli SK, Jin Y, Lee M, Jin X, Kim JH, Hong YS, Lee JJ (2007) (Aryloxyacetylamino)benzoic acid analogues: a new class of hypoxia-inducible factor-1 inhibitors. J Med Chem 50:1675–1684
Schust J, Sperl B, Hollis A, Mayer TU, Berg T (2006) Stattic: a small-molecule inhibitor of STAT3 activation and dimerization. Chem Biol 13:1235–1242
Ruepp B, Bohren KM, Gabbay KH (1996) Characterization of the osmotic response element of the human aldose reductase gene promoter. Proc Natl Acad Sci U S A 93:8624–8629
Woo SK, Lee SD, Kwon HM (2002) TonEBP transcriptional activator in the cellular response to increased osmolality. Pflugers Arch 444:579–585
Ho SN (2003) The role of NFAT5/TonEBP in establishing an optimal intracellular environment. Arch Biochem Biophys 413:151–157
Mylari BL, Beyer TA, Siegel TW (1991) A highly specific aldose reductase inhibitor, ethyl 1-benzyl-3-hydroxy-2(5H)-oxopyrrole-4-carboxylate, and its congeners. J Med Chem 34:1011–1018
Burg MB, Ferraris JD, Dmitrieva NI (2007) Cellular response to hyperosmotic stresses. Physiol Rev 87:1441–1474
Henry DN, Frank RN, Hootman SR, Rood SE, Heilig CW, Busik JV (2000) Glucose-specific regulation of aldose reductase in human retinal pigment epithelial cells in vitro. Invest Ophthalmol Vis Sci 41:1554–1560
Virgili G, Parravano M, Menchini F, Evans JR (2014) Anti-vascular endothelial growth factor for diabetic macular oedema. Cochrane Database Syst Rev 10, CD007419
Miwa K, Nakamura J, Hamada Y, Naruse K, Nakashima E, Kato K, Kasuya Y, Yasuda Y, Kamiya H, Hotta N (2003) The role of polyol pathway in glucose-induced apoptosis of cultured retinal pericytes. Diabetes Res Clin Pract 60:1–9
Kubo E, Urakami T, Fatma N, Akagi Y, Singh DP (2004) Polyol pathway-dependent osmotic and oxidative stresses in aldose reductase-mediated apoptosis in human lens epithelial cells: role of AOP2. Biochem Biophys Res Commun 314:1050–1056
Fu J, Tay SS, Ling EA, Dheen ST (2007) Aldose reductase is implicated in high glucose-induced oxidative stress in mouse embryonic neural stem cells. J Neurochem 103:1654–1665
Bringmann A, Uckermann O, Pannicke T, Iandiev I, Reichenbach A, Wiedemann P (2005) Neuronal versus glial cell swelling in the ischaemic retina. Acta Ophthalmol Scand 83:528–538
Ryan GJ (2007) New pharmacologic approaches to treating diabetic retinopathy. Am J Health Syst Pharm 64:S15–S21
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The Geschwister Freter Stiftung (Hannover, Germany) and the Deutsche Forschungsgemeinschaft provided financial support in the form of grants (KO 1547/7-1). The sponsors had no role in the design or conduct of this research.
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Winges, A., Garcia, T.B., Prager, P. et al. Osmotic expression of aldose reductase in retinal pigment epithelial cells: involvement of NFAT5. Graefes Arch Clin Exp Ophthalmol 254, 2387–2400 (2016). https://doi.org/10.1007/s00417-016-3492-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-016-3492-x