Abstract
Purpose
To determine the cause of retinochorioditis in a patient with a granulomatous retinal exudate and an exudative retinal detachment.
Case
A 45-year-old man presented at another hospital with increased visual disturbances of the left eye. He was diagnosed with uveitis, and treated with topical steroids for 1 month. However, the uveitis worsened, and he was referred to our hospital. Ophthalmoscopy showed a yellowish-white granulomatous exudate, and an exudative retinal detachment in the lower peripheral retina. The retinal detachment worsened and affected the macula. Pars plana vitrectomy was performed, and the retina was reattached. During the surgery, ocular samples were collected for further examinations. The titers of antibodies against 12 kinds of ascaridis were examined, and elevated titers of specific antibodies against porcine ascarids were detected in the subretinal fluid, but not in the aqueous humor, vitreous, or serum.
Conclusions
Vitrectomy with the collection of ocular samples, especially subretinal fluid, was a key procedure in the diagnosis and treatment of retinochoroiditis associated with the porcine ascarids.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Ocular ascariasis is usually caused by the larvae of Toxocara canis or Toxocara cani that migrate into ocular tissues in humans. It is characterized by uveitis, vitreous opacities, and granulomas in the retina[1]. Enzyme-linked immunosorbed assay (ELISA) is an effective test for making a diagnosis of ocular ascariasis, especially its detection in the aqueous humor and vitreous fluid.
We report a case of retinochoroiditis associated with porcine ascarids diagnosed by antibodies in only the subretinal fluid.
Case report
A 45-year-old man presented at another hospital with decreased vision of his left eye in September 2006. He was diagnosed with anterior uveitis and treated with topical steroids for 1 month. In spite of the treatment, his visual acuity continued to decrease, and he was referred to our hospital on 3 October 2006. He had been told that he had bilateral hilar lymphadenopathy after a routine health check 6 months earlier, and was diagnosed with sarcoidosis by a biopsy of the lymph nodes. However, he appeared healthy and did not have clinical symptoms of sarcoidosis systemically and ocularly. He was a forestry worker, and lived near the forest. He was also a hunter and had killed wild boars and deer several times, and had eaten raw liver of a deer 1 year earlier.
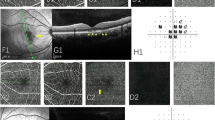
On his first visit, his corrected visual acuity was 20/20 OD and 8/20 OS, and the intraocular pressure was 15 mmHg OD and 11 mmHg OS. The right eye was normal. However, the anterior chamber of his left eye was mildly inflamed, and the vitreous had dense opacities. In addition, a yellowish-white granulomatous exudate with retinal hemorrhages and an exudative retinal detachment were present in the lower peripheral retina (Fig. 1). Fluorescein angiography showed hyperfluorescence of the optic disc and severe retinal nodal periphlebitis in his left eye.
The results of his laboratory examination were essentially normal except for an increased rate of erythrocyte sedimentation of 30 mm/hour. The result of his tuberculin test was negative.
A differential diagnosis for ocular toxocariasis and sarcoidosis was required because of his medical history and fundus findings. He was treated with 60 mg/day of prednisone systemically for 1 week, and his vitreous opacities decreased slightly, but the exudative retinal detachment worsened and affected the macula. His visual acuity decreased to 4/20 OS. Thus, pars plana vitrectomy with phacoemulsification and aspiration of the lens, implantation of intraocular lens, and silicon oil replacement was performed on October 20, 2006. The subretinal exudative lesion was removed with the overlying retina because the adhesion of the lesion to the retina was firm. During the surgery, samples of the aqueous humor, vitreous fluid, and subretinal fluid were collected for further examinations. After the vitrectomy, the retina was reattached, but the retinal nodal periphlebitis and small retinal exudates still remained.
Histopathological examination of the removed exudates showed extensive fibrous connective tissues, accompanied by many vessels and plasma cells. These findings indicated chronic severe inflammation. Epithelioid cells and giant-cell generally associated with sarcoidosis were not observed in the specimens.
The titers of antibodies against 12 kinds of ascarids, including Toxocara canis, feline ascarids, and porcine ascarids, determined by multiple dot ELISA were all negative in the serum, aqueous humor, and vitreous. Therefore, microtiter plate ELISA, which is more sensitive than multiple dot ELISA, was performed for the 12 kinds of ascarids on ocular samples including subretinal fluid that had not been tested. Elevated titers of antibodies against porcine ascarids were detected only in the subretinal fluid (×90) and not in the aqueous humor, vitreous, and serum (Fig. 2). From these findings, we diagnosed our patient with retinochoroiditis associated with porcine ascarids.
He was treated systemically with 600 mg/day of albendazole (eskazole®) combined with 20 mg/day of prednisolone. Three weeks later, the ocular inflammation resolved and his visual acuity improved to 20/30 OS on January 12, 2007.
Discussion
A clinical diagnosis of ocular ascariasis is usually made by specific immunotests that show elevated titers of antibodies. In our case, steroid therapy was not effective, and the pathological findings were not specific for sarcoidosis. In addition, the titers of antibodies against 12 kinds of ascariasis were negative in the serum, aqueous humor, and vitreous by multiple dot ELISA. However, elevated titers of a specific antibody against porcine ascarids were detected in the subretinal fluid by microtiter plate ELISA. Thus, we diagnosed our patient with retinochoroiditis associated with porcine ascarids.
It has been reported that even if antibodies against toxocariasis are not detected in the serum, they can often be positive in ocular samples, e.g., aqueous humor and the vitreous, by ELISA [2–4] because the antibodies are localized in the lesions accompanying the toxocariasis. Thus, examinations of ocular samples are recommended for the diagnosis of ocular ascariasis. However, a search of Medline did not extract any reports of elevated titers of antibodies against ascarids in only the subretinal fluid, and negative in the serum, aqueous humor, and vitreous. In addition, most of the reports of ocular ascarids were associated with Toxocara canis. Therefore, this is the first case of ocular ascarids associated with porcine ascarids determined by specific immuno testing.
These results demonstrated the importance of testing ocular fluids in cases of uveitis of unknown cause. Vitrectomy with the collection of ocular samples, especially subretinal fluid, was a key for the diagnosis of ascariasis retinochoroiditis associated with the porcine ascarids.
References
Pollard ZF, Jarrett WH, Hagler WS, Allain DS, Schantz PM (1979) ELISA for diagnosis of ocular toxocariasis. Ophthalmology 86:743–749
Sharkey JA, McKay PS (1993) Ocular toxocaiasis in a patient with repeatedly negative ELISA titre to Toxocara canis. Br J Ophthalmol 77:253–254
Benitez del Castillo JH, Herreros G, Gillen JL (1995) Bilateral ocular Toxocariasis demonstrated by aqueous humor enzyme-linked immunosorbent assay. Am J Ophthalmol 119:514–516
Biglan AW, Glickman LT, Lobes LA (1979) Serum and vitreous Toxocara antibody in nematode endophthalmitis. Am J Ophthalmol 88:898–901
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Matsuyama, K., Ogata, N., Takahashi, K. et al. Case of retinochoroiditis associated with porcine ascarids diagnosed by antibodies in subretinal fluid. Graefes Arch Clin Exp Ophthalmol 246, 1065–1067 (2008). https://doi.org/10.1007/s00417-008-0790-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-008-0790-y