Abstract
Background
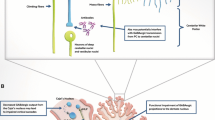
Myelin-associated glycoprotein (MAG) is a glycoprotein specific to Schwann cells. Schwann cells produce myelin for nerve cells in the peripheral nervous system. MAG also plays a role in the central nervous system (CNS) by maintaining myelin integrity and inhibiting axonal regeneration from cerebellar neurons. There is a well-established link between distal demyelinating neuropathy and anti-MAG antibodies in patients with monoclonal gammopathy of unknown significance. We describe a series of five patients with anti-MAG antibodies with evidence of cerebellar rather than just sensory ataxia and our experience of treatment with rituximab.
Methods
Cerebellar ataxia was clinically suspected and confirmed using magnetic resonance spectroscopy (MRS) of the cerebellum. All patients underwent detailed nerve conduction studies.
Results
Four patients were males. The ages ranged from 64 to 82 years. All patients were anti-MAG positive and also had IgM monoclonal gammopathy. Four patients had neuropathy, whilst one had no evidence of neuropathy. All patients were treated with rituximab and showed improvement in the MRS parameters of the cerebellum.
Conclusion
Anti-MAG antibodies might be involved in the pathogenesis of idiopathic sporadic ataxias, even in the absence of peripheral neuropathy. Rituximab seems to be a promising therapeutic intervention for those cases.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Myelin-associated glycoprotein (MAG) is a glycoprotein specific to Schwann cells. Schwann cells produce myelin for nerve cells in the peripheral nervous system. MAG also plays a role in the central nervous system (CNS) by maintaining myelin integrity and inhibiting axonal regeneration from cerebellar neurons [1].
The presence of anti-MAG antibodies is commonly associated with distal demyelinating neuropathy in patients with monoclonal gammopathy of unknown significance (MGUS). MAG-neuropathy is a form of chronic inflammatory demyelinating polyneuropathy (CIDP) characterized by disproportionate prolongation of distal latencies in both sensory and motor nerve conduction studies. Clinically, patients with MAG-neuropathy present mainly with sensory symptoms and significant degree of what was presumed to be sensory ataxia [2].
Sensory ataxia, when severe can be difficult to distinguish from cerebellar ataxia [3]. We describe a series of five patients with anti-MAG antibodies with evidence of cerebellar rather than just sensory ataxia and our experience of treatment with rituximab.
Methods
Standard protocol approvals, registrations and patient consents
This is an observational case series of patients regularly attending the Ataxia clinic based at the Royal Hallamshire Hospital (Sheffield, UK). The South Yorkshire Research Ethics Committee has confirmed that no ethical approval is indicated given that all investigations were clinically indicated and did not form part of a research study.
Patient selection
All recruited patients had clinical signs of progressive cerebellar dysfunction, which was confirmed using magnetic resonance spectroscopy (MRS) of the cerebellum. All patients underwent detailed nerve conduction studies (NCS). All patients had been extensively investigated for all causes of neuropathy and cerebellar ataxia. All were anti-MAG positive.
Neuroimaging
All patients underwent magnetic resonance imaging (MRI) of the brain including magnetic resonance spectroscopy (MRS) of the cerebellum vermis and right hemisphere). The latter technique is validated and is used to determine the presence of cerebellar dysfunction, even in the absence of cerebellar atrophy [4,5,6].
We measured the N-acetyl-aspartate/creatine (NAA/Cr) ratios in the vermis and the cerebellar hemispheres. Low NAA/Cr ratio implies abnormal metabolic activity within the area of interest (voxel) and it can be used as an indicator to cerebellar dysfunction [7]. Standardized normal values are NAA/Cr > 0.95 in the vermis and > 1.00 in the hemispheres [8].
Only patients with abnormal NAA/Cr ratios in either the vermis or the hemispheres were considered as having definite cerebellar dysfunction.
Electrophysiological evaluation
Extensive neurophysiological assessments were performed on all patients to determine the presence of neuropathy. The nerve conduction studies included median (motor and sensory), ulnar (motor and sensory), superficial radial (sensory), superficial peroneal (sensory), common peroneal (motor), sural (sensory) and tibial (motor) nerves. Because of the presence of anti-MAG antibodies, patients with no evidence of peripheral neuropathy at baseline had regular NCS to confirm, or not, the development of neuropathy over time.
Results
We identified five patients (four males, one female) with clinical evidence of cerebellar ataxia (all patients had gait and mild lower limb ataxia with two patients also having gaze-evoked nystagmus) confirmed with MRS. Balance difficulties were very prominent in their presentation (as it is often the case in MAG-neuropathy) and the reason for the neurophysiology was the clinical suspicion of peripheral neuropathy. The age at diagnosis ranged from 64 to 82 years (mean 73.0 years). In four patients neurophysiological assessment confirmed the presence of peripheral neuropathy. However, one had no evidence of neuropathy. All patients had IgM monoclonal gammopathy.
Anti-MAG associated cerebellar ataxia without MAG-neuropathy and response to rituximab
A 82-year-old Caucasian man was referred to our Ataxia Clinic because of a 2-year history of progressive unsteadiness. The patient had been diagnosed with IgM lambda MGUS with a less than 1 gm/L monoclone. The patient was found to have a high MAG antibody titer (20,400 BTU, normal values < 1000) but had no neurophysiological evidence of any neuropathy. Neurological examination revealed prominent gaze-evoked nystagmus and gait ataxia. The MRI of his brain showed no abnormalities, but the MRS of the cerebellar vermis revealed a low NAA/Cr area ratio of 0.93.
The patient had been followed-up on a 6-monthly basis and remained relatively stable for 18 months. Two years after presentation he complained of worsening of his balance and repeat MRS showed a reduction of the NAA/Cr area ratio at 0.86. Given the presence of IgM MGUS and the high level of anti-MAG antibodies the patient was given a course of rituximab following which the NAA/Cr area ratio normalized at 0.97. He remained mobile without a walking aid but he did not feel that there had been any dramatic improvement to his balance. He continued to be followed-up on a 6-monthly basis complaining of progressive deterioration of his balance. Repeat MRS showed the vermian NAA/Cr area ratio to have dropped to 0.77. Eighteen months after the first rituximab infusion he agreed to a second course which again showed dramatic increase in the NAA/Cr area ratio at 0.94, this time with subjective clinical improvement. Figure 1 shows the NAA/Cr area ratio changes over time and in relation to the rituximab infusions. Repeat neurophysiological assessments showed no evidence of a neuropathy.
MAG-neuropathy with cerebellar ataxia and response to rituximab
The remaining four patients in these case series had a combination of MAG-neuropathy and cerebellar ataxia. All patients had no evidence of cerebellar atrophy but abnormal MRS of the cerebellum. Of them, three patients subjectively reported improvement following the first rituximab course. Two of them are on regular 9-monthly rituximab courses, and one of them opted to discontinue the treatment as he developed a vasculitic rash immediately after the first course. The fourth patient reported no subjective improvement following the first rituximab course and opted not to have any repeat courses. However, all patients showed improvement in their MRS parameters following rituximab.
Table 1 summarizes the clinical and imaging data of our case series.
Discussion
We present a case series of five patients with anti-MAG associated cerebellar dysfunction. Whilst the link between distal demyelinating neuropathy and anti-MAG antibodies is well established, to our knowledge this is the first report of evidence of cerebellar dysfunction in the context of anti-MAG antibodies. It is also the first report to demonstrate the improvement in cerebellar functioning with the use of rituximab. This finding suggests that anti-MAG antibodies may be implicated in the pathogenesis of some idiopathic sporadic ataxias. Cerebellar ataxias are the result of diverse disease processes that can be genetic or acquired. Establishing a diagnosis requires a methodical approach with expert clinical evaluation and investigations. Despite extensive investigations in up to 20% of patients no diagnosis can be made [9]. Such cases are referred to as idiopathic sporadic ataxias. Based on this report we would recommend testing for anti-MAG antibodies all patients with MGUS and idiopathic sporadic ataxia even in the absence of a neuropathy. This is particularly important given that these patients appear to benefit from immunosuppression.
Cerebellar dysfunction appears to be a feature in MAG-neuropathy. The latter is a neuropathy characteristically said to result in sensory ataxia. Our results suggest that the ataxia in MAG-neuropathy may well be due to cerebellar dysfunction and not just due to the neuropathy. Investigating further such patients using MRS may be helpful. The combination of peripheral neuropathy and cerebellar ataxia is increasingly been recognized [10]. The possibility of negative biofeedback mechanisms leading to a cerebellar dysfunction when the sensory input is low remains to be determined. In our experience, however, patients with sensory ganglionopathy (a type of neuropathy that classically presents with sensory ataxia) do not have abnormal MRS of the cerebellum.
Finally all of our patients who had anti-MAG associated cerebellar dysfunction responded to rituximab. Therefore, the latter is worth considering as a therapeutic intervention in patients with anti-MAG antibodies and cerebellar ataxia, even in the absence of peripheral neuropathy, where rituximab has been shown to be particularly effective [11].
Of course, our results are essentially focusing on one case with anti-MAG associated cerebellar dysfunction with no evidence of neuropathy that responded to rituximab. Therefore, a large study is needed to confirm the association between anti-MAG antibodies and cerebellar dysfunction, even in the absence of neuropathy, and the potential of rituximab as a treatment option in such cases.
References
DeBellard ME, Tang S, Mukhopadhyay G, Shen YJ, Filbin MT (1996) Myelin-associated glycoprotein inhibits axonal regeneration from a variety of neurons via interaction with a sialoglycoprotein. Mol Cell Neurosci 7(2):89–101
Dalakas MC (2010) Pathogenesis and treatment of anti-MAG neuropathy. Curr Treat Options Neurol 12(2):71–83
Zis P, Reilly MM, Rao DG, Tomaselli P, Rossor AM, Hadjivassiliou M (2017) A novel mutation in the FGD4 gene causing Charcot-Marie-Tooth disease. J Peripher Nerv Syst. https://doi.org/10.1111/jns.12222
Hadjivassiliou M, Wallis LI, Hoggard N, Grünewald RA, Griffiths PD, Wilkinson ID (2012) MR spectroscopy and atrophy in Gluten, Friedreich’s and SCA6 ataxias. Acta Neurol Scand 126(2):138–143
Baldarçara L, Currie S, Hadjivassiliou M, Hoggard N, Jack A, Jackowski AP, Mascalchi M, Parazzini C, Reetz K, Righini A, Schulz JB, Vella A, Webb SJ, Habas C. Baldarçara L, Currie S, Hadjivassiliou M, Hoggard N, Jack A, Jackowski AP, Mascalchi M, Parazzini C, Reetz K, Righini A, Schulz JB, Vella A, Webb SJ, Habas C (2015) Consensus paper: radiological biomarkers of cerebellar diseases. Cerebellum 14(2):175–196
Hadjivassiliou M, Grünewald RA, Sanders DS, Shanmugarajah P, Hoggard N (2017) Effect of gluten-free diet on cerebellar MR spectroscopy in gluten ataxia. Neurology. https://doi.org/10.1212/WNL.0000000000004237
Shanmugarajah PD, Hoggard N, Currie S, Aeschlimann DP, Aeschlimann PC, Gleeson DC, Karajeh M, Woodroofe N, Grünewald RA, Hadjivassiliou M (2016) Alcohol-related cerebellar degeneration: not all down to toxicity? Cerebellum Ataxias 3:17. https://doi.org/10.1186/s40673-016-0055-1
Currie S, Hadjivassiliou M, Craven IJ, Wilkinson ID, Griffiths PD, Hoggard N (2013) Magnetic resonance spectroscopy of the brain. Postgrad Med J 89:94–106
Hadjivassiliou M, Martindale J, Shanmugarajah P, Grünewald RA, Sarrigiannis PG, Beauchamp N, Garrard K, Warburton R, Sanders DS, Friend D, Duty S, Taylor J, Hoggard N (2017) Causes of progressive cerebellar ataxia: prospective evaluation of 1500 patients. J Neurol Neurosurg Psychiatry 88(4):301–309
Zis P, Rao DG, Wagner BE, Nicholson-Goult L, Hoggard N, Hadjivassiliou M (2017) Cerebellar ataxia and sensory ganglionopathy associated with light-chain myeloma. Cerebellum Ataxias 5(4):1
Renaud S, Gregor M, Fuhr P, Lorenz D, Deuschl G, Gratwohl A, Steck AJ (2003) Rituximab in the treatment of polyneuropathy associated with anti-MAG antibodies. Muscle Nerve 27(5):611–615
Author information
Authors and Affiliations
Contributions
PZ: drafting/revising the manuscript, data collection, statistical analysis, accepts responsibility for conduct of research and final approval. DGR, NH and PGS: drafting/revising the manuscript, data collection, accept responsibility for conduct of research and final approval. MH: drafting/revising the manuscript, study concept and design, data collection, accepts responsibility for conduct of research and final approval.
Corresponding author
Ethics declarations
Study funding
None.
Conflicts of interest
Panagiotis Zis, Dasappaiah Ganesh Rao, Nigel Hoggard, Ptolemaios Georgios Sarrigiannis, and Marios Hadjivassiliou have nothing to disclose.
Ethical standards
For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Zis, P., Rao, D.G., Hoggard, N. et al. Anti-MAG associated cerebellar ataxia and response to rituximab. J Neurol 265, 115–118 (2018). https://doi.org/10.1007/s00415-017-8675-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-017-8675-9