Abstract
Gastroesophageal reflux is known to cause chronic cough and is also implicated in worsening of asthma. We conducted a prospective study to examine the clinical significance of gastroesophageal reflux disease (GERD) in asthmatic patients with chronic cough to analyze the temporal relationship between reflux events and coughing and to assess the effect of esomeprazole treatment on respiratory symptoms and lung function in these patients. Asthmatic patients (126) with chronic dry cough were studied. Diagnosis of GERD was based on typical symptoms and the effectiveness of therapeutic test or on pH monitoring. Patients without GERD (negative pH results) consisted of the control group. The results of pH monitoring showed that 64% of cough episodes were related to acid reflux and in 91% of reflux events preceded coughing. Esomeprazole treatment (40 mg/day for 3 months) not only diminished GERD symptoms but also improved asthma outcome Baseline FEV1 and PEF values increased significantly together with a decrease in symptom scores and the use of rescue medication. In most patients included in the extended part of the study for another 3 months, the dose of inhaled steroids could be reduced with sustained GERD therapy. Our data showing that reflux events preceded coughing in most cases and that treatment of GERD resulted in an improvement in different outcome measures of asthma suggest that GERD worsens asthma, and its treatment is of clinical importance to effectively manage these patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Gastroesophageal reflux disease (GERD) is a common condition generally caused by transient lower esophageal sphincter (LES) relaxations. Approximately 25% of patients present with classic symptoms of GERD including heartburn, postural aggravation, dysphagia and choking; however, there are several cases with atypical, extragastrointestinal symptoms such as chronic dry cough, wheezing, chest pain and chronic hoarseness [1]. A high and largely divergent prevalence of GERD (40–80%) has been reported in asthma [2]. Despite the frequency of this finding, the nature of the relationship is poorly understood. One possible interaction is that the bronchial obstruction occurring in asthmatic patients somehow promotes reflux [3, 4]. On the other hand, gastric acid can induce bronchoconstriction by increasing bronchial reactivity, causing pH changes in the airways due to microaspiration and activating reflex arch mediated by the vagal nerve [5]. Presence of acid in the esophagus is associated with the release of substance P and neurokinin A in the bronchial mucosa resulting in airway edema via a neuroinflammatory reflex mechanism. These mechanisms combined may lead to an increase in vagal efferent impulses which can augment or provoke airway hyperreactivity and lead to an increase in the severity of asthma [6]. One of the symptoms often associated with GERD is chronic dry cough, which can also accompany asthma or upper airway disease. In patients with normal chest X-rays the frequency of the different underlying diseases of dry cough are postnasal drip syndrome in approximately 40%, asthma approximately 24% and GERD — the third most frequent cause — with 21% [7]. Since both GERD and asthma can be associated with chronic dry cough, the extent of GERD contributing to coughing in asthmatic patients is not known [8–10].
To understand more precisely the clinical importance of GERD in asthma we conducted a prospective study on asthmatic patients with chronic dry cough. The aims of the study were to determine if GERD was present in these patients, to analyze the temporal relationship between reflux events and coughing recorded during pH monitoring and to evaluate the effect of GERD treatment with esomeprazole on different outcome measures of asthma including respiratory symptom score, lung function and use of medication.
Methods
Subjects
A total of 126 persistent mild or moderate asthmatic patients (49 males, 77 females, mean age 41.3, range 14–75 years) with chronic dry cough (continuous coughing for at least 3 months) were included in the study. Asthma was diagnosed according to the guidelines of the American Thoracic Society at least 12 months before the study. All patients were receiving low or moderate doses of inhaled corticosteroids and used inhaled long-acting β2-agonists as maintenance therapy. Inhaled short-acting β2-agonists were used as rescue medication. All patients were in stable condition for the last 6 weeks preceding the study with no change in their maintenance treatment. Asthmatic patients with negative results on pH monitoring (no pathological reflux detected) were included as controls (n = 26). Exclusion criteria were inappropriate cooperation (lack of compliance), inability to take a medicine orally, hypersensitivity to the components of the proton pump inhibitor (PPI), known malignant tumor, changes in smoking habit, changes in the type or dose of ACE inhibitors if used. Care was taken to ensure that no antacids were consumed up to 2 weeks before the study. The enrollment period was one year (from 01.01.2003. to 31.12.2003.)
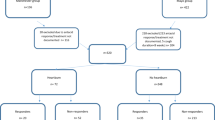
Study Design (Fig. 1)
At the screening visit medical history was taken, physical examination was carried out and asthma and GERD symptoms were evaluated. Patients satisfying the inclusion criteria were recruited in the study and were given a patient diary to record the number of inhaled short-acting β2-agonists; they were asked to return for visit 1 after 14 days. At visit 1 FEV1 and PEF were measured, symptom score was calculated and patients filled out a GERD questionnaire (symptom score) (Table 1). If patients did not have typical symptoms of GERD, 24-hour esophageal pH monitoring was performed. Patients with typical GERD symptoms received medication for GERD at visit 1, while patients with atypical symptoms received a pH monitor for 24 hours and, depending on its results, evaluated the next day and were included either in the GERD or the control group. Patients with GERD received a proton pump inhibitor (esomeprazole, 40 mg orally o.d.) for 3 months, and were asked to keep their asthma medication unchanged and return for visit 2, which was held between days 85 and 95. At visit 2, measurements were performed (lung function tests, GERD questionnaire, symptom score) and patients were asked to keep their medication stable for another 14 days while recording the use of their rescue medication and return for visit 3. If the patients did not require rescue medication during the 2 weeks, they were asked to half the dose of their inhaled corticosteroids while continuing with esomeprazole therapy for another 3 months and return for a follow-up visit (Visit 4).
Measurements
Lung Function Test
FEV1 and PEF were measured by means of an electronic spirometer (Medicor MS-11; Budapest, Hungary). The best of 3 consecutive maneuvers was accepted for evaluation. FEV1 and PEF value was expressed as a percentage of the predicted normal value for the subject’s height and age according to European Community for Coal and Steel reference values.
24 Hour Ambulatory pH Monitoring
Continuous monitoring of esophageal pH (during which cough and reflux events were recorded) was performed with the pH meter Digitrapper (type: Digitrapper MD, manufacturer: Synectics Medical AB, Stockholm, Sweden) with a catheter type anitimony nasoesophageal electrode (Medtronic Zinetics 24 M Internal Reference, Medtronic Functional Diagnostics A/S, Skovlunde, Denmark) placed 5 cm above the lower esophageal sphincter. The evaluated parameters were number of reflux episodes, number of reflux episodes longer than 5 minutes, longest reflux episode, fraction time below pH 4 (total), fraction time below pH 4 (supine) (De Meester score). Besides determining the number of reflux episodes we also analyzed the temporal association between acid reflux and coughing.
Medication
Treatment with proton pump inhibitor, 40 mg esomeprazole orally once daily was performed in patients with typical heartburn and regurgitation as a therapeutic test and also in GERD patients diagnosed with pH monitoring.
Statistical Analysis
Data are expressed as the mean ± SEM. Differences were examined for significance using one sample and two sample t-test. Z-test of a single proportion was used for analysis of the temporal association between acid reflux and coughing. Significance was established at p < 0.05.
Results
Presence of GERD in Asthmatic Patients with Chronic Cough
In the 126 recruited patients, GERD was diagnosed in 94 cases; in 31 cases the diagnosis was based on typical GERD symptoms and their cessation due to the therapeutic test, while in the other 63 patients the results of pH monitoring were used to confirm the diagnosis (Table 2). In patients with chronic cough, only respiratory symptoms were found in 89 cases while in the other 37 cases both respiratory and gastrointestinal symptoms were present (Fig. 1). Obesity, a known risk factor for GERD, was detected in 66 patients (mean BMI: 37.2).
Association Between Reflux Episodes and Coughs
We analyzed the temporal association between acid reflux and coughing (Table 3). During the pH monitoring, the 24-hour pH curve was recorded together with cough events. In 403 of 627 of the coughs (64% of all cough episodes), there was a significant association between coughing and acid reflux (p < 0.0001). Reflux events preceded coughs in 367 of 403 events (91%). Cough preceded acid reflux only in 36 of 403 events (9%). The sequence of events was stable in different patients: in 57 of 63 patients the reflux event occurred first and was followed by coughing.
Effect of GERD Treatment on Asthma
All patients diagnosed (either by positive therapeutic test or pH monitoring) with GERD (n = 94) received treatment with esomeprazole. No adverse event was observed during the study. After 3 months of esomeprazole treatment, not only GERD and asthma symptoms decreased, but also all other determined outcome measures of asthma improved: FEV1 and PEF values (Table 4), use of rescue medication (Table 5). In the control group (asthmatic patients with chronic cough without GERD), there was no change in symptom scores and FEV1 or PEF values between visits 1 and 2 (Table 4). When the changes measured between visit 1 and visit 2 were compared between the GERD and control groups, a significant difference between the changes observed in the two groups was confirmed in FEV1 (p < 0.0001) and in PEF (p < 0.0001). The frequency distribution of symptom scores demonstrated significant difference before and after therapy in patients with GERD showing pronounced improvement in symptom scores (Fig. 2) with no change in the control group (Table 4).
The number of rescue medications used after 3 months of PPI treatment (during the 2 weeks between visits 2 and 3) was significantly lower in the group of GERD patients compared to that at baseline (between visit 0 and 1) (p < 0.001), but there was no change in the control group. Thirty-nine GERD patients required no rescue medication during the 2-week observation period after the 3 months of PPI therapy (between visits 2 and 3) (Table 5). In these patients the dose of inhaled corticosteroid therapy was halved. After an additional 3 months, patients were reevaluated and only one of them showed worsening in asthma symptoms and lung function, while the rest were stable on the combination of PPI treatment and reduced dose of local corticosteroid treatment.
Discussion
The relationship of gastroesophageal reflux and pulmonary symptoms / diseases is complex. Gastroesophageal reflux can induce cough and also induce/exacerbate asthma. In the present study we investigated the occurrence of GERD in asthmatic patients with chronic dry cough, the relation between reflux events and coughing and also the effect of treatment of GERD on asthma. Our results showed that GERD was present in many patients only with atypical symptoms; reflux events preceded coughing in the majority of patients with GERD and effective control of GERD resulted in an improvement in all asthma outcome measures investigated and in patients with controlled GERD, the dose of inhaled steroids could be reduced.
The efficacy of an omeprazole test in cases with typical gastrointestinal symptoms is high (about 75–95%) [11–13]. In our study we used a new generation PPI, esomeprazole, for the therapeutic test and found the same efficiency (84%) in this group. Although our patients who presented with typical GERD symptoms but did not show a good therapeutic response to esomeprazole may have had GERD, they were excluded from the study because of the uncertainty of the diagnosis. While the cost-effective diagnostic approach in patients with typical GERD symptoms is to begin with a PPI (e.g., omeprazole or esomeprazole 40 mg/day) for 3 months, followed by 24-hr pH testing in nonresponders [14, 15], patients with chronic airway symptoms without typical GERD symptoms are ideal candidates for pH monitoring to establish early diagnosis. In our patients with atypical symptoms we could verify GERD with pH testing in 63 of 89 cases. The 24-h pH monitoring could not only confirm the pathological reflux, but the connection between acid reflux and airway symptoms as well [16, 17]. In GERD-related chronic cough, reflux and cough events were frequently associated. We found a relation between cough and acid reflux in 64% of cough events. In 91% of cough events reflux preceded suggesting that it could be responsible for coughing.
Subjects with cough-variant asthma (CVA) have been shown to have heightened cough reflex sensitivity to capsaicin relative to that of healthy controls and asthmatics without cough [18]. Therefore the results and conclusions of this study may not necessary be applicable to a population of “typical” asthmatics without associated cough. Our study, however, was not restricted to patients with CVA, but all asthmatic patients with associated chronic dry cough were considered. From our 126 asthmatic patients with chronic cough, in 94 cases the gastroesophageal reflux played an important part as the cause of cough expressly.
Our study shows that in patients with persistent mild or moderate asthma with chronic cough, pH monitoring is a very effective diagnostic approach to verify reflux as a (at least partial) cause of symptoms. Following anti-reflux treatment the results showed significant improvement not only in GERD symptoms but also in asthma outcome measures (FEV1 and PEF value, asthma symptoms and use of rescue medication).
Treatment of GERD in patients with asthma has been consistently shown to improve respiratory symptoms but not necessarily pulmonary function tests, but controlled studies are lacking [19, 20]. Although our study was not placebo-controlled, it involved large numbers of patients, and as a control, asthmatic patients with cough and without GERD were also included. By demonstrating that asthma medication could be reduced when controlling GERD, our data suggest that the potential of GERD should be considered and evaluated in coughing asthmatic patients and if diagnosed, its appropriate treatment may help to reach better asthma control.
In summary, 24-hour pH monitoring was an effective way of determining GERD as an underlying cause of chronic cough in asthmatic patients. Control of GERD improved asthma outcome measures and helped to lower the dose of medication. These data suggest that GERD should be considered for coughing asthmatic patients and its control may help to improve asthma.
References
SM Harding (1999) GERD, airway disease, and the mechanisms of interaction MR Stein (Eds) Gastroesophageal reflux disease and airway disease Dekker New York 139–173
SK Field M Underwood R Brant RL Cowie (1996) ArticleTitlePrevalence of gastroesophageal reflux symptoms in asthma Chest 109 316–322
RJ Donnelly RG Berrisford CIA Jack JA Tran CC Evans (1993) ArticleTitleSimultaneous tracheal and esophageal pH monitoring: investigating reflux-associated asthma Ann Thorac Surg 56 1029–1034
CIA Jack MJ Walshaw J Tran CR Hind CC Evans (1994) ArticleTitleTwenty-four-hour tracheal pH monitoring — a simple and nonhazardous investigation Respir Med 88 441–444
CIA Jack PMA Carverley RJ Donnelly J Tran G Russell CR Hind (1995) ArticleTitleSimultaneous tracheal and oesophageal pH measurements in asthmatic patients with gastroesophageal reflux Thorax 50 201–204
SM Harding JE Richter MR Guzzo CA Schan RW Alexander LA Bradley (1996) ArticleTitleAsthma and gastroesophageal reflux: acid suppressive therapy improves asthma outcome Am J Med 100 395–405
CJ Mello (1999) GERD, A major factor in chronic cough MR Stein (Eds) Gastroesophageal reflux disease and airway disease Dekker New York 89–106
JE Richter (2000) ArticleTitleGastroesophageal reflux disease and asthma: the two are directly related Am J Med 108 IssueIDsuppl. 4a 153S–158S
SM Harding (1999) ArticleTitleGastroesophageal reflux and asthma: Insight into the association J Allergy Clin Immunol 104 IssueIDsuppl. 2 251–259
SJ Sontag (1999) The prevalence of GERD in asthma MR Stein (Eds) Gastroesophageal reflux disease and airway disease Dekker New York 115–136
MS Kavuru JE Richter (1999) Medical treatment of gastroesophageal reflux disease and airway disease MR Stein (Eds) Gastroesophageal reflux disease and airway disease Dekker New York 179–203
PJ Kahrilas (2003) ArticleTitleDiagnosis of symptomatic gastroesophageal reflux disease Am J Gastroenterol 98 IssueIDsuppl. 3 S15–S23
P Eisendrath J Track J Deviere (2002) ArticleTitleDiagnosis of gastroesophageal reflux disease in general practice: a Belgian National Survey Endoscopy 34 998–1003
GA Ford PS Oliver JS Prior RJ Butland SP Wilkinson (1994) ArticleTitleOmeprazole in the treatment of asthmatics with nocturnal symptoms and gastro-oesophageal reflux: a placebo-contolled cross-over study Postgrad Med J 70 350–354
RH Hunt (1999) ArticleTitleImportance of pH control in the management of GERD Arch Intern Med 159 649–657 Occurrence Handle10.1001/archinte.159.7.649 Occurrence Handle1:STN:280:DyaK1M3jtlWisw%3D%3D Occurrence Handle10218743
PO Katz DO Castell (1999) Diagnosis of grastroesophageal reflux disease MR Stein (Eds) Gastroesophageal reflux disease and airway disease Dekker New York 55–67
CAM Stedman ML Barclay (2000) ArticleTitleReview article comparison of the pharmacokinetics, acid suppression and efficacy of proton pump inhibitors Aliment Pharmacol Ther 14 969–978
PV Dicpinigaitis JB Dobkin J Reichel (2000) ArticleTitleAntitussive effect of the leukotriene receptor antagonist zafirlukast in subjects with cough-variant asthma J Asthma 39 291–297
L Barclay G Vogin BM Sklar (2003) ArticleTitleProton pump inhibitors may improve asthma control in children Chest 123 973–975
V Khoshoo T Le RM Haydel SuffixJr L Landry C Nelson (2003) ArticleTitleRole of gastroesophageal reflux in older children with persistent asthma Chest 123 1008–1013
Acknowledgments
The authors thank K. Módos and M. Szőgyi Dr. (Institute of Biophysics Semmelweis University, Budapest.) for their helpful statistical advice and assistance. This study was supported by the Hungarian Research Foundation (OTKA T43396).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Böcskei, C., Viczián, M., Böcskei, R. et al. The Influence of Gastroesophageal Reflux Disease and its Treatment on Asthmatic Cough. Lung 183, 53–62 (2005). https://doi.org/10.1007/s00408-004-2526-z
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s00408-004-2526-z