Abstract
The purpose of this study was to evaluate various parameters potentially influencing poor prognosis in Bell’s palsy and to assess the predictive value for Bell’s palsy. A single-center prospective patient collected observation and validation study was conducted. To evaluate the correlation between patient characteristics and poor prognosis, we performed univariate and multivariate analyzes of age, gender, side of palsy, diabetes mellitus, hypertension, and facial grading score 1 week after onset. To evaluate the accuracy of the facial grading score, we prepared a receiver operating characteristic (ROC) curve and calculated the area under the ROC curve (AUROC). We also calculated sensitivity, specificity, positive/negative likelihood ratio, and positive/negative predictive value. We included Bell’s palsy patients who attended Ehime University Hospital within 1 week after onset between 1977 and 2011. We excluded patients who were less than 15 years old and lost-to-follow-up within 6 months. The main outcome was defined as non-recovery at 6 months after onset. In total, 679 adults with Bell’s palsy were included. The facial grading score at 1 week showed a correlation with non-recovery in the multivariate analysis, although age, gender, side of palsy, diabetes mellitus, and hypertension did not. The AUROC of the facial grading score was 0.793. The Y-system score at 1 week moderate accurately predicted non-recovery at 6 months in Bell’s palsy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Bell’s palsy is defined as an acute facial nerve paralysis of unknown origin, and is the most common cause of peripheral facial palsy, with an annual incidence of about 20–30 per 100,000 persons [1]. According to recent clinical studies, Bell’s palsy is believed to be caused by the reactivation of latent herpes simplex virus type-1 (HSV-1) infection in the geniculate ganglion [2]. The natural course of the disease is generally favorable, and approximately 70 % of patients recover completely with no treatment [3]. However, more than 10 % of the patients are unable to regain normal facial function, and about 5 % of them suffer from severe sequelae, such as facial spasm, synkinesis, and contracture [4], even with appropriate treatment.
Steroids and antiviral agents are the main drugs for treating Bell’s palsy. Steroid treatment cures 90 % of Bell’s palsy [4], and antiviral agents are limited to patients with a poor prognosis [5]. The steroid and antiviral agent should be given as soon as possible, because early treatment has a good prognosis [6]. Therefore, we should decide whether the patient needs an antiviral agent, and avoid over treatment and the adverse effects of antiviral agents. Electroneurography is the most powerful tool for evaluating the prognosis of non-recovery in Bell’s palsy [7, 8], but the electroneurography is reliable 7–10 days after onset [9]. In addition, access of electroneurography is limited. Therefore, a prognostic tool that is readily available without requiring specialized equipment is needed.
Factors that can predict prognosis have been sought in previous studies based on a clinical evaluation of acute symptoms and signs, concurrent medical disease (hypertension and diabetes mellitus), age, and the facial grading score [10–12]. The facial grading score is correlated with non-recovery of Bell’s palsy comparatively [12]. However, the accuracy of the facial grading score has not been evaluated sufficiently and it is uncertain when the facial grading score should be used. In this study, we established a prognostic model using clinical parameters including the Yanagihara facial grading system (Y-system) (Table 1) [13].
Methods
Study design and setting
We conducted a prospective patient collected observational study at Ehime University Hospital from January 1977 to December 2011. We included Bell’s patients 15 years of age or older who first visited the hospital within 1 week after onset. Patients whose facial palsy was due to zoster sine herpete, and those who could not be followed for more than 6 months or until complete recovery, were excluded. Y-system scores were recorded each time the patient visited our clinic. We also prospectively recorded patient age, gender, date of Bell’s palsy onset, side of palsy, concurrent medical diseases (diabetes mellitus, hypertension) and Y-system score.
Treatment of Bell’s palsy in our hospital
Since 1977, Bell’s palsy has been treated in our hospital using the following strategy. Prednisolone administration is tapered from 60 mg/day for 5 days, 30 mg/day for 3 days, and 10 mg/day for 2 days. In 1990, we changed this protocol by adding an antiviral agent to prednisolone for patients whose Y-system scores were 0–8.
Outcome measures
The primary outcome was non-recovery at 6 months after onset. Recovery was defined as an improvement of the Y-system score to 36 or more without sequelae, according to the facial paralysis guidelines of the Japan Society of Facial Nerve Research. A Y-system score of 36 was considered comparable to HB-system grade II [14].
Statistical analysis
To evaluate any bias due to excluding the lost-to-follow-up patients, we examined the difference between the patients analyzed and excluded using the Chi-square test (gender, side of palsy, diabetes mellitus, hypertension) and Student’s t test (age, Y-system score). To evaluate the correlation between patient characteristics and poor prognosis, we performed univariate analyzes using the Chi-square test (gender, side of palsy, diabetes mellitus, hypertension) and Student’s t test (age, Y-system score). Then we performed multivariate logistic regression analysis including the factors with p < 0.2 in the univariate analyzes. Likelihood ratio methods were used for the logistic regression analysis.
We estimated the prognostic ability of the Y-system score at 1 week for Bell’s palsy by plotting a receiver operating characteristic (ROC) curve and calculating the area under the ROC curve (AUROC) with the 95 % confidence interval (95 % CI). The accuracy of the AUROC is classified as low if the area is 0.5–0.7, moderate if 0.7–0.9, and as high if >0.9. We also prepared the ROC curve and calculated the AUROC of Y-system score at 2 and 4 weeks, and the worst score. Then, we calculated each Y-system score’s cut-off line sensitivity, specificity, positive likelihood ratio (LR+), negative likelihood ratio (LR–), positive predictive value (PPV), and negative predictive value (NPV) with the 95 % CI. Data were analyzed using SPSS ver. 19.0 for Windows (SPSS, Chicago, IL, USA).
Results
Patient characteristics
Between 1967 and 2011, 893 patients diagnosed with Bell’s palsy were seen within 1 week after onset. Of them, 214 patients [113 males, 101 females; mean age 50.4 ± 17.1; mean Y-system score 12.4 ± 7.4; left side palsy = 98 (45.8 %), diabetes mellitus = 20 (9.3 %), hypertension = 45 (21.0 %)] were excluded because they were lost-to-follow-up. Thus, 679 patients (320 males, 359 females; mean age 48.7 ± 16.8; mean Y-system score 14.8 ± 8.1; left side palsy = 359 (52.8 %), diabetes mellitus = 74 (11.0 %), hypertension = 122 (18.0 %)) were included. Excluded patients had higher Y-system scores (p < 0.001), but there was no difference in age, gender, side of palsy, or concurrent medical disease between the excluded and included patients. In the included patients, one patient refused prednisolone treatment, 25 patients underwent facial nerve decompression surgery, and the overall non-recovery rate was 11.6 % (79/679).
Table 2 provides an overview of the characteristics of the included patients, the univariate analyzes, and the multivariate analysis. The p values of the Y-system scores and age were less than 0.2 in univariate analyzes. Thus, we included these two factors in the multivariate logistic regression analysis. Only the Y-system score significantly predicted poor prognosis.
ROC curve of Y-system for Bell’s palsy
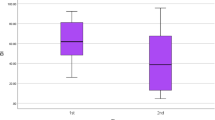
Figure 1 shows the ROC curve of the Y-system score at 1, 2, and 4 weeks, and the worst score. Y-system score was assessed in 74.4 % (n = 505) of the patients at 2 weeks and in 48.5 % (n = 329) at 4 weeks. The AUROC was 0.793 at 1 week, 0.861 at 2 weeks, 0.947 at 4 weeks, and 0.823 at the worst score. At 4 weeks, the Y-system score was not assessed in half of the patients, so we calculated the AUROC using the substituted Y-system score at 4 weeks to avoid a deficit data bias. Substituting the deficit Y-system score at 4 weeks using the score at 3 weeks [n = 130 (19.1 %)] or at 5 weeks [n = 39 (5.7 %)], or the average of the scores at 3 and 5 weeks [n = 64 (9.4 %)] changed the AUROC from 0.947 to 0.956. Table 2 provides the sensitivity, specificity, LR+, LR–, PPV, and NPV of each Y-system score at 1 week.
Discussion
We evaluated the prognostic value of patient age, gender, palsy side, Y-system score at 1 week, diabetes mellitus, and hypertension. Multivariate logistic regression analysis showed that only the Y-system score at 1 week was a prognostic factor in Bell’s palsy patients. Our multivariate logistic regression analysis revealed no correlation between age, gender, and palsy side and non-recovery, in agreement with many previous reports [7, 8, 10, 12]. Takemoto et al. [7] reported a correlation between diabetes mellitus and non-recovery in a multiple regression analysis, but our multivariate analysis showed no such correlation. In an animal study, Esaki et al. [15] reported that drug-induced diabetes led to worse HSV-1 induced facial palsy. Neither our report nor Takemoto et al. assessed the severity of diabetes and form of treatment. Further detailed analysis is needed to evaluate the correlation between diabetes mellitus and non-recovery.
In our study, the diagnostic accuracy of the worst facial grading score was higher than the score at 1 week, and lower than the score at 2 and 4 weeks (Fig. 1). The diagnostic accuracy of facial grading for predicting non-recovery in Bell’s palsy increases with time and the AUROC of the facial grading score at 4 weeks for predicting non-recovery reached 0.947 (near 1.000), as in previous reports [12]. Therefore, we should predict non-recovery of Bell’s palsy 4 weeks after onset when we cannot use ENoG. The cut-off of a “Y-system score <24 at 4 weeks”, which is compatible with a House-Brackmann facial grading system (HB-system) score ≥IV [16], was the nearest to the left upper corner in the ROC curve. This cut-off point had 92.7 % (84.7–100.0 %) sensitivity, 85.9 % (81.7–89.8 %) specificity, 48.1 % (37.1–59.1 %) PPV, and 98.8 % (97.5–100.0 %) NPV. In other words, 99.8 % of Bell’s palsy patients who had a Y-system score ≥24 at 4 weeks after onset would be cured.
The facial grading system score helps to decide whether a patient needs an antiviral agent. Van der Veen et al. reported a small effect of antiviral therapy in their meta-analysis [5], which retrieved patients who had a HB-system score ≥IV, which is compatible with a Y-system score <24 [16]. In our results (Fig. 1), the sensitivity of “Y-system score <24 at 1 week” reached 98.7 % and the LR of “Y-system score <24 at 1 week” reached 0.07. Only one patient with “Y-system score ≥24 at 1 week” did not reached recovery at 6 months. The cut-off of the facial grading score for recommending an antiviral agent is under discussion. The facial paralysis guidelines of the Japan Society of Facial Nerve Research recommend giving an antiviral agent to Bell’s palsy patients with a “Y-system score <10 at 1 week” [17]. “Y-system score <12” was nearest and “Y-system score <10” was second nearest to the left upper corner of the ROC curve of the Y-system score at 1 week. Therefore, the facial grading score cut-off of the Japan Society of Facial Nerve Research is reasonable.
Limitations
This study had some limitations. First, 25 % of the patients were lost-to follow-up. It is difficult to follow Bell’s palsy patients without losses, because the natural history of Bell’s palsy is good and the treatment is limited in the acute phase. The recovery rate in this study was similar to previous studies [18], but our results could not avoid some lost-to-follow-up bias. Second, during the study period, all patients did not receive the same treatment. Our database was lack of whether the patients had antiviral therapy or not. We could not analyze any effect of antiviral therapy, although the efficacy of antiviral therapy was low [5, 19]. Third, since 1977 when the Y-system was developed, we had to consider a validation study of the Y-system. However, the analysis in this study was not preplanned.
Conclusions
This study showed that the Y-system score at 1 week can predict non-recovery of Bell’s palsy at 6 months (AUROC 0.793). This model might be a useful additional tool for predicting non-recovery in the clinical setting and can be used to select patients for antiviral therapy. In addition, our results suggest that non-recovery can be predicted using the Y-system score at 4 weeks.
References
Hauser WA, Karnes WE, Annis J, Kurland LT (1971) Incidence and prognosis of Bell’s palsy in the population of Rochester, Minnesota. Mayo Clin Proc Mayo Clin 46(4):258–264
Murakami S, Mizobuchi M, Nakashiro Y, Doi T, Hato N, Yanagihara N (1996) Bell palsy and herpes simplex virus: identification of viral DNA in endoneurial fluid and muscle. Ann Intern Med 124(1 Pt 1):27–30
Peitersen E (2002) Bell’s palsy: the spontaneous course of 2,500 peripheral facial nerve palsies of different etiologies. Acta Otolaryngol Suppl 549:4–30
Salinas RA, Alvarez G, Daly F, Ferreira J (2010) Corticosteroids for Bell’s palsy (idiopathic facial paralysis). Cochrane Database Syst Rev (3):CD001942. doi:10.1002/14651858.CD001942.pub4
van der Veen EL, Rovers MM, de Ru JA, van der Heijden GJ (2012) A small effect of adding antiviral agents in treating patients with severe Bell palsy. Otolaryngol Head Neck Surg Off J Am Acad Otolaryngol Head Neck Surg 146(3):353–357. doi:10.1177/0194599811432537
Marsk E, Hammarstedt L, Berg T, Engstrom M, Jonsson L, Hultcrantz M (2010) Early deterioration in Bell’s palsy: prognosis and effect of prednisolone. Otol Neurotol Off Publ Am Otol Soc Am Neurotol Soc Eur Acad Otol Neurotol 31(9):1503–1507. doi:10.1097/MAO.0b013e3181f2f21f
Takemoto N, Horii A, Sakata Y, Inohara H (2011) Prognostic factors of peripheral facial palsy: multivariate analysis followed by receiver operating characteristic and Kaplan-Meier analyses. Otol Neurotol Off Publ Am Otol Soc Am Neurotol Soc Eur Acad Otol Neurotol 32(6):1031–1036. doi:10.1097/MAO.0b013e31822558de
Mantsopoulos K, Psillas G, Psychogios G, Brase C, Iro H, Constantinidis J (2011) Predicting the long-term outcome after idiopathic facial nerve paralysis. Otol Neurotol Off Publ Am Otol Soc Am Neurotol Soc Eur Acad Otol Neurotol 32(5):848–851. doi:10.1097/MAO.0b013e31821da2c6
Tojima H, Aoyagi M, Inamura H, Koike Y (1994) Clinical advantages of electroneurography in patients with Bell’s palsy within two weeks after onset. Acta Otolaryngol Suppl 511:147–149
Yeo SW, Lee DH, Jun BC, Chang KH, Park YS (2007) Analysis of prognostic factors in Bell’s palsy and Ramsay Hunt syndrome. Auris Nasus Larynx 34(2):159–164. doi:10.1016/j.anl.2006.09.005
Ushio M, Kondo K, Takeuchi N, Tojima H, Yamaguchi T, Kaga K (2008) Prediction of the prognosis of Bell’s palsy using multivariate analyses. Otol Neurotol Off Publ Am Otol Soc Am Neurotol Soc Eur Acad Otol Neurotol 29(1):69–72. doi:10.1097/mao.0b013e31815c2aa0
Marsk E, Bylund N, Jonsson L, Hammarstedt L, Engstrom M, Hadziosmanovic N, Berg T, Hultcrantz M (2012) Prediction of nonrecovery in Bell’s palsy using Sunnybrook grading. Laryngoscope 122(4):901–906. doi:10.1002/lary.23210
Yanagihara N (1977) Grading of facial palsy. Facial Nerve Surgery. Aesculpius, Birmingham, AL
Berg T, Jonsson L, Engstrom M (2004) Agreement between the Sunnybrook, House-Brackmann, and Yanagihara facial nerve grading systems in Bell’s palsy. Otol Neurotol Off Publ Am Otol Soc Am Neurotol Soc Eur Acad Otol Neurotol 25(6):1020–1026
Esaki S, Yamano K, Kiguchi J, Katsumi S, Keceli S, Okamoto H, Goshima F, Kimura H, Nishiyama Y, Murakami S (2012) Diabetic mice show an aggravated course of herpes-simplex virus-induced facial nerve paralysis. Otol Neurotol Off Publ Am Otol Soc Am Neurotol Soc Eur Acad Otol Neurotol 33(8):1452–1457. doi:10.1097/MAO.0b013e318268d54d
Satoh Y, Kanzaki J, Yoshihara S (2000) A comparison and conversion table of ‘the House-Brackmann facial nerve grading system’ and ‘the Yanagihara grading system’. Auris Nasus Larynx 27(3):207–212
Murakami S (2011) Treatment of peripheral facial paralysis in acute phase. In: Japan Society of Facial Nerve Research (ed) Guideline for facial paralysis—Bell’s palsy and Hunt syndrome, Kanehara shuppan, Japan, pp 55–59
Berg T, Marsk E, Engstrom M, Hultcrantz M, Hadziosmanovic N, Jonsson L (2009) The effect of study design and analysis methods on recovery rates in Bell’s palsy. Laryngoscope 119(10):2046–2050. doi:10.1002/lary.20626
Lockhart P, Daly F, Pitkethly M, Comerford N, Sullivan F (2009) Antiviral treatment for Bell’s palsy (idiopathic facial paralysis). Cochrane Database Syst Rev (4):CD001869. doi:10.1002/14651858.CD001869.pub4
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fujiwara, T., Hato, N., Gyo, K. et al. Prognostic factors of Bell’s palsy: prospective patient collected observational study. Eur Arch Otorhinolaryngol 271, 1891–1895 (2014). https://doi.org/10.1007/s00405-013-2676-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-013-2676-9