Abstract
Introduction
Periprosthetic fractures are difficult to manage. Plating technique has been considered a reliable form of management of periprosthetic fractures with a well-fixed stem, but a dependable and stable method of plate fixation to the bone is lacking. This study reports the clinical results using a locking attachment plate (LAP) instead of cable fixation to fix locking plates to a periprosthetic femoral shaft fracture.
Materials and methods
Nineteen patients with periprosthetic femoral shaft fractures around well-fixed stemmed implants were studied between August 2012 and December 2014. Patients were followed up for at least 1 year postoperatively. Median age was 74 years (range 56–96 years). Fractures were classified according to the Unified Classification System, Vancouver classification, and Su classification.
Procedure
Open reduction was performed under minimal incision and the locking plate was fixed to the lateral cortex of the femoral shaft. The part of the shaft without a stem was fixed to the plate using 5.0-mm locking screws, and the part with an underlying stem was fixed using 3.5-mm locking screws through the LAP instead of cables. Postoperatively, patients were managed using general principles for femoral shaft fractures.
Results
Average follow-up was 16 months (range 12–36 months). All cases achieved fracture healing without loss of reduction. There were no cases of implant breakage or stem loosening at final follow-up. The average number of LAPs per fixation construct was 2.1 (range 1–4), and the average number of 3.5-mm locking screws through each LAP was 3.3 (range 2–4). The average value of plate screw density was 0.55 (range 0.37–0.8), and the average working length was four holes (range 2–8).
Conclusions
Using the LAP to manage periprosthetic fractures with a well-fixed stem could obviate the need for cable around the stem area and yield acceptable outcomes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
A periprosthetic femoral fracture is a challenging surgical problem. Because of the high morbidity, treatment has changed from traction and bracing in a cast to ORIF, a revision arthroplasty procedure, or a combination thereof [1,2,3]. There is a general consensus that most fractures associated with a well-fixed stem can be treated by ORIF alone [2,3,4].
Treatment of periprosthetic fractures is challenging due to the combination of fractured bone and prosthesis, with the possibility of further complications caused by osteoporotic bone and the cement used for prosthesis fixation [5]. Stable fixation is necessary because these fractures are slow to heal, and osteopenia is frequently involved [6]. To overcome these problems, supplementary methods such as cerclage wiring or cable fixation around long bones are frequently used, but these lack stable resistance to torsional stress [7]. The failure rate was reported to be 33.9% for fractures treated by plate osteosynthesis and 43.9% for fractures treated with cerclage cables alone [8]. Monocortical locking screws with combined cable or cerclage wiring have been used successfully in several reports [9, 10]. However, in recent studies, biomechanical stability of the fixation construct was improved with the use of bicortical locking screws as compared with traditional monocortical locking screws and cable techniques [11]. Recently, the Locking Attachment Plate (LAP®; Depuy-Synthes, West Chester, PA, USA) was developed for use in combination with standard locking compression plates (LCPs), especially for the femoral shaft, as a less invasive stabilisation system (LISS; Depuy-Synthes, West Chester, PA, USA) that creates a stable construct with 3.5-mm locking screw fixation around the stem [12,13,14] (Figure 1).
The LAPs are available with 4 or 8 holes for 3.5-mm locking screws. LAPs with 4 holes were used in all cases. The 8-hole plate was necessary for more extensive soft tissue dissection (a). The plate was attached to the LCP using a connecting screw. The 3.5-mm locking screws on each side of the plate have avoided the prosthesis stem (b). The LAP is fixed to the LCP (c). The 3.5-mm locking screws passed through the cortex on an axial CT scan image (d). LAP locking attachment plate, LCP locking compression plate
The purpose of this study was to report the clinical results with use of the LAP to stabilise femoral shaft fractures around well-fixed stems without using a cable.
Materials and methods
A retrospective review of the trauma patient database at two institutions was conducted to identify cases of periprosthetic femoral shaft fractures with well-fixed implants from August 2012 to December 2014. The inclusion criteria were as follows: (1) displaced fracture in the femoral shaft with a well-fixed intramedullary stem; and (2) no evidence of infection at the fracture site. The exclusion criteria were: (1) follow-up duration of less than 1 year; (2) replacement arthroplasty without an intramedullary stem; (3) treatment with other fixation construct; and (4) violation of fixation principles. The detailed information is shown in Table 1.
The stability of the fixation of the stem was assessed on standard imaging tests preoperatively and was confirmed intraoperatively [6]. A total of 19 patients (5 males) were included in the study. The median age was 74 years (range 56–96). Regarding femoral stem types, there were ten cases of total hip replacement arthroplasty (THRA), six cases of bipolar hip arthroplasty (BPHA), and three cases of total knee replacement arthroplasty with femoral stem (TKRA). The average number of arthroplasty procedures for these patients was 1.63. The average interval between last arthroplasty and injury was 7 years and 2 months (range 1 year 4 months–22 years 1 month), and the average interval between injury and index procedure was 35 days (range 1–366). Most patients underwent osteosynthesis procedures in the acute stage, but two patients were referred to our institution after, respectively, undergoing 2 and 3 plate osteosynthesis procedures augmented with cable fixation. The interval between the injury and the index procedure for these two patients was 167 and 366 days, respectively. All injury mechanisms were of the low-energy type.
The classification of periprosthetic fractures differs among implant types, but the general rule is to classify fracture type according to the position of the stem. Recently, the Unified Classification System (UCS) has generally been used for periprosthetic fractures [15]. This classification is based on the location of the fracture, the fixation of the component, and the adequacy of the bone stock and strength for supporting the implant. UCS type B1, C, and D fractures were found in our study. The Vancouver classification is also frequently used for periprosthetic hip replacement fractures [16]. Vancouver type B1 and C fractures were found in our study. Su et al. divided fractures around a TKRA into three types according to the fracture location relative to the proximal border of the femoral component [17]. Type I and II cases were the subjects of our study (Table 2).
Surgical procedure
We followed Pike’s management principles and performed surgery using methods described previously [6, 14]. Preoperative planning should include a surgical approach if the stem is found to be unstable on intraoperative assessment and shows occult infection. In addition to a standard revision arthroplasty complement, implants and allografts for unexpected intraoperative findings should be available. The patient was positioned supine on the operating table under general or spinal anaesthesia. We used biologic fixation through bridge plating for periprosthetic femoral shaft fractures. We performed minimal dissection to obtain reduction and applied the plate. In simple spiral fractures, we achieved near anatomical reduction between the two main fragments with percutaneous cerclage wiring using a cerclage passer instrument through small lateral incisions (Fig. 2). In wedge fractures, we applied fixation to the two main fragments, leaving the wedge fragment untouched. Anatomical reduction of wedge fragments is not necessary. Furthermore, their direct reduction would risk damaging their biology. We preserved the soft tissue attachments to the wedge fragments; when the fragments are indirectly well aligned, union is enhanced (Fig. 3). In some cases, a closed reduction was not possible due to muscle interposition, hematoma or interposed periosteum. In these cases, the fracture was located by the image intensifier and a 5-cm skin incision was made at that point. After sharp dissection of the fascia, the vastus lateralis and adjacent periosteum were managed carefully. Fixation according to AO principles of relative stability can be essential [18]. The use of fixed-angle implants, such as a LISS plate, is helpful for fixation of the fracture. Fixation of femoral shaft fractures was performed using 5.0-mm locking plates for the stemless portion [2, 19]. Fixation in the well-fixed stem portion was performed using 3.5-mm locking screws through an LAP or additional 5.0-mm monocortical locking screws. We attempted to use as few LAPs as possible, only adding these to the construct if there was suspicion of instability after locking plate fixation. To obtain fracture healing in the two cases that were referred to our institution after multiple failures, all fixation materials except for arthroplasty components were removed first, and then fixation was repeated according to the above methods. Bone autografting was performed at bony defect site. Bone grafting was not performed in any of the other cases.
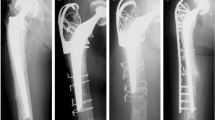
An 82-year-old female with a UCS type IV.3 D and Vancouver type C periprosthetic fracture following bipolar hip arthroplasty and total knee replacement arthroplasty. The fracture pattern was simple spiral fracture. This is a frequent finding when the injury mechanism is the low-energy type (a, b). We achieved near-anatomical reduction between the two main fragments with percutaneous cerclage wiring using a cerclage passer instrument through small 4-cm lateral incisions (c). Internal fixation with MIPO was obtained using a LISS with precontoured LCP distal femur plate. An LAP was fixed around the prosthesis stem proximally with three 3.5-mm locking screws (d–f). X-rays taken 7 months postoperatively. Fracture site healed with callus bridging. UCS unified classification system, MIPO minimally invasive plate osteosynthesis, LISS less invasive stabilisation system, LCP locking compression plate, LAP locking attachment plate
A 79-year-old female with a UCS type IV.3 B1 and Vancouver type B1 periprosthetic fracture following bipolar hip arthroplasty. She had a large spiral wedge fragment on the medial side of femoral shaft (a, b). We applied fixation to the two main fragments using MIPO technique, leaving the wedge fragment untouched. We preserved the soft tissue attachments to the wedge fragments to prevent devitalisation. Restoration of alignment, length, and rotation was achieved indirectly (c, d). The last follow-up radiographs were taken 13 months postoperatively and show satisfactory indirect healing involving the wedge fragment (e, f). UCS unified classification system, MIPO minimally invasive plate osteosynthesis
Conventional cable attached to the plate through eyelets was not applied in this study. Fixation close to the fracture and at the far ends of the plate should be employed to maximise the overall strength of the fracture construct [6]. The 3.5-mm locking screws through the LAP were mounted to the plate, avoiding the prosthetic stem. It was not possible to insert 3.5-mm locking screws through all LAP holes because of the anatomic variations of the femoral shaft, but we attempted to insert as many screws as possible through the LAPs.
Aftercare
Postoperative care was performed according to the characteristics of the individual patient and the stability of the construct. Patients were ambulated as soon as possible. In most cases, toe-touch weight bearing was recommended at a minimum of 6–12 weeks, at which time activities were increased. There was discrepancy between the institutions. Appropriate thrombo-prophylaxis and antibiotic prophylaxis were administered. Implants for fracture fixation were not removed routinely.
Outcome evaluation and fixation construct analysis
The patients were followed up at our outpatient clinic, and X-rays were obtained monthly until 6 months postoperatively. They were again evaluated at 9 and 12 months, and then annually. Fracture union was determined by the presence of callus bridging across three or four cortices and/or disappearance of visible fracture line on both the anteroposterior and the lateral radiographs. Fracture reduction was measured by using the anteroposterior and lateral radiographs. Malalignment was defined as more than 5° of angulation in both plane. Fracture union, alignment, prosthesis-related complications, and procedure-related complications were checked at the 1-year follow-up. We analysed our fixation construct for the number of LAPs, the number of 3.5-mm locking screws through an LAP, the number of 3.5-mm locking screws through LAPs in each case, and the use of additional 5.0-mm monocortical locking screws. The working length of a plate (defined as the number of plate holes between the proximal and distal screw in closest proximity to the fracture) was measured. We also checked the periprosthetic fixation length and shaft fixation length including the plate screw density. We calculated the fixation length as the number of plate holes from the most proximal fixed hole to the most distal fixed hole at each segment. We assumed that one LAP had equal quantities of 4 holes. The plate screw density was defined as the number of fixed screws divided by the fixation length.
Results
The average follow-up period for the 19 patients was 16 months (range 12–36). The average number of LAPs per fixation construct was 2.1 (range 1–4), and the average number of 3.5-mm locking screws through an LAP was 3.3 (range 2–4). The average number of 3.5-mm locking screws through LAPs in a case was 6.9 (range 3–12), and the average additional number of 5.0-mm monocortical locking screws was 0.9 (range 0–4). The average periprosthetic fixation length was 14.5 holes (range 9–28) and the average periprosthetic plate screw density was 0.65 (range 0.41–0.85). The average shaft fixation length was 8.7 holes (range 4–14) and the average shaft plate screw density was 0.63 (range 0.37–1). The average overall plate screw density was 0.55 (range 0.37–0.8). The average working length of a plate was 4 holes (range 2–8).
We obtained fracture healing without loss of reduction in all cases. There was no evidence of loosening or breakage of fixation devices at the final follow-up. At the time of fracture healing, there was no malalignment in the coronal and sagittal planes. There were no cases of revision arthroplasty performed for loosening of stemmed implants during this period. There was one case of an intertrochanteric fracture at the proximal end of the fixation plate after bony union was achieved. Since union was already attained, the plate was removed and the patient was able to walk normally after receiving surgery for the hip fracture (Fig. 4). No other case required removal of the osteosynthetic device. Another patient needed IV antibiotic therapy for surgical site infection. One patient underwent surgery for infection of bipolar hip arthroplasty, but there was no evidence of infection at the fracture site.
A 64-year-old with a long-stemmed TKRA femoral component. Bony union was achieved after osteosynthesis with LAP, but the patient suffered an intertrochanteric fracture 6 months later (a). Possible peritrochanteric fracture at the tip of a long plate can be avoided by inserting one screw through the plate to the head and neck region. The LCP was removed and fixation of the hip fracture was performed. The mechanical axis was in the normal range, but there was a limb length discrepancy at the final follow-up (b). TKRA total knee replacement arthroplasty, LAP locking attachment plate, LCP locking compression plate
Discussion
This study evaluated the management of periprosthetic femoral shaft fractures around well-fixed stems. We report the clinical results with use of LAP in combination with lateral locking plates on femoral cortical bone around well-fixed stems. Previous studies have evaluated periprosthetic plate osteosynthesis using the LAP, but reported clinical results for the femur, tibia, and humerus [13, 14]. Our study reports consecutive results using LAP for periprosthetic fractures of the femoral shaft. We obtained fracture union with our construct fixation in all cases; in contrast, a 33.3% failure rate was reported in one study [13].
According to Vancouver classification, fixation failures are more frequently seen in B1 type fractures where the proximal and/or distal fixation is more complicated than C type fractures. We attained fracture healing without fixation failure in both B1 and C types. However, more than half of the fractures are of type C. We have limited distribution of patients to represent each type of fractures from Vancouver classification.
There was a report of increased risk of death after surgery for periprosthetic fractures; in our study, there were two deaths [20, 21]. These patients were very old (90- and 96 years old, respectively) and also had cardiovascular and endocrinologic comorbidities. Bhattacharyya et al. reported a mortality rate of 11% 1 year after surgery, which is similar to the results of our study (10%) [21].
In Vancouver type B1 fractures treated with plating osteosynthesis, cemented stems had worse outcomes than uncemented stems [20]. We attained bony union in all six cases in which cemented stems were used. We believe this shows that stable fixation after sufficient apposition of the fracture site will lead to bony healing in most cases.
Biomechanical studies on fixation techniques in periprosthetic femoral shaft fractures around well-fixed stems have been conducted. The stability of fixation has been compared for LAP and other methods, such as cerclage-LCP construct [5, 12]. The stability of fixation achieved with the LAP construct is not yet fully appreciated, but it is biomechanically superior to a cerclage-LCP construct. The LAP construct allows 3.5-mm bicortical locking screw placement lateral to the prosthesis stem, providing more stable anchoring fixation than previous monocortical fixation or cerclage cable methods [22]. This is designed to prevent lateral screw pull-out, i.e., to stabilise the prosthesis stem, and thus allow early postoperative mobilisation. However, it was not always possible to place 3.5-mm locking screws in all 4 lateral arms of the LAP. In this study, we inserted an average number of 3.2 screws in four outer holes of the LAP. The fixed-angle trajectory of the locking screw into the locking hole of the LAP did not always match the diameter of the femoral shaft. We adjusted the trajectory of the screw by in situ-bending the arms of the LAP. In this process, we had trouble disengaging the bending pin or drill sleeve from the screw hole. The contour of the plate needs to be improved and an option for insertion of 3.5-mm locking screws at variable angle should be added.
We also had difficulty confirming whether the screws were inserted around the stem bicortically or transcortically on intraoperative fluoroscopy and postoperative plain radiography; this can be determined by an axial CT view, but we did not evaluate postoperative CT scans routinely. We checked a postoperative CT scan when we questioned whether the screw fixation had sufficient purchase in the bone (Fig. 1).
The ideal fixation construct can be determined by using two factors: the plate span width and the plate screw density. Current recommendations for bridge plating require a plate span width greater than 2–3, and the plate screw density should be 0.5 or less [23]. In our study, we used as long a plate as possible to cover the entire length of the femoral shaft and overlap the prosthesis. The average plate screw density was 0.5 in the LAP. We also made the fixation length around the stem as long as possible. Using a long fixation improved the lever arm of the screws. This reduced the pull-out force acting on each screw. By following these principles, our fixation construct resulted in fracture healing without failure in all cases.
In postoperative care, a rapid loss of muscle mass and power takes place in the older patients if not adequately mobilized. We allowed patients to ambulate as soon as possible with partial weight bearing including toe-touch weight bearing using a walker and crutches for a minimum of 6–12 weeks. However, older patients cannot perform partial weight bearing because of lack of power in the arms and also lack of coordination capacity. Several studies demonstrated that patient exceeded the prescribed amount of partial weight bearing [24, 25]. We presume that stable fixation with this construct will lead to work towards weight bearing faster than in our series.
Complications encountered in our study included one case of late infection after osteosynthesis around a bipolar hip arthroplasty implant and one case of superficial surgical site infection at the fracture site. This indicates that the outcome of treatment of the periprosthetic fracture was also related to the condition of the arthroplasty implantation [8]. A consensus system for assessing operative results after femoral shaft fractures is not available at present, and studies involving functional evaluation after periprosthetic fracture may cause further confusion because the status of existing arthroplasty implants must also be considered.
Conclusion
Use of the LAP in conjunction with LCP around the underlying stem is a useful method of achieving healing of periprosthetic femoral shaft fractures around well-fixed stemmed implants.
References
Fredin HO, Lindberg H, Carlsson AS (1987) Femoral fracture following hip arthroplasty. Acta Orthop Scand 58:20–22
Haidukewych GJ, Ricci W (2008) Locked plating in orthopaedic trauma: a clinical update. J Am Acad Orthop Surg 16:347–355
Haidukewych GJ, Langford JR, Liporace FA (2013) Revision for periprosthetic fractures of the hip and knee. Instr Course Lect 62:333–340
Haddad FS, Duncan CP, Berry DJ, Lewallen DG, Gross AE, Chandler HP (2002) Periprosthetic femoral fractures around well-fixed implants: use of cortical onlay allografts with or without a plate. J Bone Jt Surg Am 84-A:945–950
Wahnert D, Schroder R, Schulze M, Westerhoff P, Raschke M, Stange R (2014) Biomechanical comparison of two angular stable plate constructions for periprosthetic femur fracture fixation. Int Orthop 38:47–53
Pike J, Davidson D, Garbuz D, Duncan CP, O’Brien PJ, Masri BA (2009) Principles of treatment for periprosthetic femoral shaft fractures around well-fixed total hip arthroplasty. J Am Acad Orthop Surg 17:677–688
Fulkerson E, Tejwani N, Stuchin S, Egol K (2007) Management of periprosthetic femur fractures with a first generation locking plate. Injury 38:965–972
Lindahl H, Malchau H, Oden A, Garellick G (2006) Risk factors for failure after treatment of a periprosthetic fracture of the femur. J Bone Jt Surg Br 88:26–30
Ricci WM, Haidukewych GJ (2009) Periprosthetic femoral fractures. Instr Course Lect 58:105–115
O’Toole RV, Gobezie R, Hwang R, Chandler AR, Smith RM, Estok DM 2nd, Vrahas MS (2006) Low complication rate of LISS for femur fractures adjacent to stable hip or knee arthroplasty. Clin Orthop Relat Res 450:203–210
Graham SM, Mak JH, Moazen M, Leonidou A, Jones AC, Wilcox RK (2015) Periprosthetic femoral fracture fixation: a biomechanical comparison between proximal locking screws and cables. J Orthop Sci 20:875–880
Lenz M, Windolf M, Muckley T, Hofmann GO, Wagner M, Richards RG (2012) The locking attachment plate for proximal fixation of periprosthetic femur fractures–a biomechanical comparison of two techniques. Int Orthop 36:1915–1921
Dumpies CW, Conrad T, Marintschev I, Hofmann GO (2012) Locking attachment plate—first experience. Z Orthop Unfall 150:302–308
Kammerlander C, Kates SL, Wagner M, Roth T, Blauth M (2013) Minimally invasive periprosthetic plate osteosynthesis using the locking attachment plate. Oper Orthop Traumatol 25(398–408):410
Duncan CP, Haddad FS (2014) The Unified Classification System (UCS): improving our understanding of periprosthetic fractures. Bone Joint J 96-B:713–716
Brady OH, Garbuz DS, Masri BA, Duncan CP (1999) Classification of the hip. Orthop Clin N Am 30:215–220
Su ET, DeWal H, Di Cesare PE (2004) Periprosthetic femoral fractures above total knee replacements. J Am Acad Orthop Surg 12:12–20
Tp R, Wm M (2000) AO Principles of Fracture Management. Thieme, New York
Egol KA, Kubiak EN, Fulkerson E, Kummer FJ, Koval KJ (2004) Biomechanics of locked plates and screws. J Orthop Trauma 18:488–493
Spina M, Rocca G, Canella A, Scalvi A (2014) Causes of failure in periprosthetic fractures of the hip at 1- to 14-year follow-up. Injury 45(Suppl 6):S85–S92
Bhattacharyya T, Chang D, Meigs JB, Estok DM 2nd, Malchau H (2007) Mortality after periprosthetic fracture of the femur. J Bone Jt Surg Am 89:2658–2662
Konstantinidis L, Hauschild O, Beckmann NA, Hirschmüller A, Südkamp NP, Helwig P (2010) Treatment of periprosthetic femoral fractures with two different minimal invasive angle-stable plates: biomechanical comparison studies on cadaveric bones. Injury 41:1256–1261
Gautier E, Sommer C (2003) Guidelines for the clinical application of the LCP. Injury 34(Suppl 2):B63–B76
Hurkmans HL, Bussmann JB, Selles RW, Benda E, Stam HJ, Verhaar JA (2007) The difference between actual and prescribed weight bearing of total hip patients with a trochanteric osteotomy: long-term vertical force measurements inside and outside the hospital. Arch Phys Med Rehabil 88:200–206
Hustedt JW, Blizzard DJ, Baumgaertner MR, Leslie MP, Grauer JN (2012) Is it possible to train patients to limit weight bearing on a lower extremity? Orthopedics 35:e31–e37
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Funding
There is no funding source.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Kim, M.B., Cho, JW., Lee, Y.H. et al. Locking attachment plate fixation around a well-fixed stem in periprosthetic femoral shaft fractures. Arch Orthop Trauma Surg 137, 1193–1200 (2017). https://doi.org/10.1007/s00402-017-2745-4
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-017-2745-4