Abstract
We investigated the changes in the expression of vascular endothelial growth factor-C (VEGF-C) and its receptor, VEGFR-3, in the rat hippocampus following transient forebrain ischemia. The expression profiles of VEGF-C and VEGFR-3 were very similar in the control hippocampi, where both genes were constitutively expressed in neurons in the pyramidal cell and granule cell layers. The spatiotemporal expression pattern of VEGF-C was similar to that of VEGFR-3 in the ischemic hippocampus, and in the CA1 and dentate hilar regions both VEGF-C and VEGFR-3 were strongly expressed in activated glial cells rather than in neurons. Most of the activated glial cells expressing both genes were reactive astrocytes, although some were a subpopulation of brain macrophages. In the dentate gyrus, however, VEGFR-3 expression was transiently increased in the innermost layer of granule cells on days 7–10 after reperfusion, coinciding with an increase in polysialylated neural cell adhesion molecule staining—a marker for immature neurons. These data suggest that VEGF-C may be involved in glial reaction via paracrine or autocrine mechanisms in the ischemic brain and may carry out specific roles in adult hippocampal neurogenesis during ischemic insults.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Vascular endothelial growth factor (VEGF) is regarded as a major regulator of angiogenesis during development, as well as a potent mediator of vascular permeability [5, 6]. Recent studies also recognize VEGF as a possible neurotrophic and neuroprotective factor (for reviews, see [2, 28, 37]). In particular, the role of VEGF has been studied extensively during ischemic injury [3, 9, 11, 17, 22, 26]. All of these studies addressed the role of VEGF-A, the key molecular regulator of angiogenesis.
In addition to VEGF-A, the VEGF gene family encodes five other polypeptide growth factors, VEGF-B, -C, -D, -E, and placenta growth factor [1, 13, 25, 28]. VEGF-C, a member of the VEGF family, primarily stimulates lymphangiogenesis [15, 33]. VEGFR-3, a receptor for VEGF-C and VEGF-D has been reported to be absent from the brain [35], and is expressed predominantly in lymphatic endothelial cells [14]. However, Jenny et al. [10] reported the expression of VEGF-C and VEGFR-3 in normal human brain and in brain tumors that are devoid of lymphatic vessels. Furthermore, Le Bras et al. [20] showed that VEGF-C and VEGFR-3 are expressed in neural progenitor cells of Xenopus laevis and mouse embryos and that VEGF-C deficiency leads to a severe defect in the proliferation of neuroepithelial cells expressing VEGFR-3, suggesting that VEGF-C is a trophic factor for neural progenitors in embryonic brain. Thus, it may be speculated that VEGF-C’s action in nervous tissue is much more broadly based than was initially supposed, i.e., its well characterized role in the lymphatic system. However, little is known about the pathophysiological role of VEGF-C in disease models of the brain.
In this paper, we have therefore examined the spatiotemporal regulation of VEGF-C and VEGFR-3 mRNA in the rat hippocampus following transient forebrain ischemia using in situ hybridization and reverse transcriptase-polymerase chain reaction (RT-PCR) analysis. Double and triple labeling techniques were used to identify the phenotypes of cells expressing VEGF-C and its specific receptor. Their expression profiles during ischemic insults lead to a better understanding of the role of VEGF-C in ischemic injury.
Materials and methods
Animal preparation
All experimental procedures performed on the animals were conducted with the approval of the Catholic Ethics Committee of the Catholic University of Korea, and in accordance with the US National Institutes of Health Guide for the Care and Use of Laboratory Animals (NIH Publication No. 80–23, revised 1996).
Adult male Sprague Dawley rats (250–300 g) were used in this study. Transient forebrain ischemia was induced by the four-vessel occlusion and reperfusion method described by Pulsinelli and Brierley [27], with minor modifications [21]. Briefly, the vertebral arteries were electrocauterized and cut to stop circulation in these vessels. After 24 h, both common carotid arteries were occluded for 10 min with miniature aneurismal clips. Only those animals showing completely flat electroencephalograms after vascular occlusion were classified as ischemic and used in the study. Body temperatures (measured rectally) were maintained at 37.5 ± 0.3°C with a heating lamp during and after ischemia. Sham-operated rats, with cauterized vertebral arteries and ligatures placed around the carotid arteries, were used as controls. No animal convulsed or died following reperfusion or sham operation.
Animals were allowed to live for 1, 3, 7, or 14 days after reperfusion. At each time point, three rats were sacrificed for use in RT-PCR analysis and seven were sacrificed for use in in situ hybridization histochemistry and immunohistochemistry. Sham-operated animals were treated using the same schedule as the ischemic/reperfused animals. In this experiment, 64 rats were used in total, 24 rats in the sham-operated group, and 40 the ischemic group. At each time point following reperfusion, animals were deeply anesthetized with 16.9% urethane (10 ml/kg) and killed by transcardial perfusion with a fixative containing 4% paraformaldehyde in 0.1 M phosphate buffer (pH 7.4), or by decapitation. This was followed by the removal of the hippocampi, which were quickly frozen in liquid nitrogen.
Semi-quantitative RT-PCR
For semiquantitative RT-PCR, total RNA was extracted from microdissected pieces of the CA1 region of both hippocampi from each rat using TRIzol reagent (Invitrogen, Carlsbad, CA, USA). RNA samples were quantified by measuring optic absorbance at 260 nm with a spectrophotometer. First-strand cDNA was synthesized using reverse transcriptase M-MLV (Takara Korea Biomedical Inc., Korea) in accordance with the manufacturer’s instructions. Equal amounts (1 μl) of the reverse transcription products were then PCR-amplified using Perfect Premix Version 2.1 (Ex Taq version; Takara Korea Biomedical Inc.). Amplification commenced with denaturation at 94°C for 4 min followed by 25–30 cycles at 94°C for 30 s, 58°C for 30 s, and 72°C for 30 s. The final extension was made at 72°C for 10 min. One picomole of each primer, which was specific for rat VEGF-C (sense, 5′-caaacaccttctttaaacctccat-3′, antisense, 5′-gctccacatgaattaaggaaaagt-3′; GenBank accession no. AY032729; nucleotides 518–1,064), or for rat VEGFR-3 (sense, 5′-ctgaggcagaatatcagtctggag-3′, antisense, 5′-agatgctcatacgtgtagttgtcc-3′; GenBank accession no. AF402785; nucleotides 1,222–1,763), was used in the amplification reaction. Ten microliters of each PCR reaction product were electrophoresed on 1.5% (w/v) agarose gels containing ethidium bromide (1 μg/μl). For semiquantitative measurements, we amplified the VEGF-C or VEGFR-3 mRNAs with rat glyceraldehyde-3-phosphate dehydrogenase (GAPDH) mRNA and optimized the number of PCR cycles to maintain amplification within a linear range. RT-PCR products were quantified by photographic densitometry of the ethidium bromide-stained agarose gel, and VEGF-C/GAPDH or VEGFR-3/GAPDH product ratios were calculated as indices of VEGF-C or VEGFR-3 mRNA expression. Three animals were used for PCR at each time point and each sample per animal was tested in triplicate. The average value for the optical density was calculated separately for every animal before the means and standard errors were determined for the total number of animals (n = 3) included per group. Results are expressed as a percentage of sham-operated rats.
In situ hybridization histochemistry
Specific sequences for VEGF-C or VEGFR-3 were prepared using RT-PCR, and antisense and sense riboprobes were labeled with digoxigenin (DIG) by in vitro transcription using a DIG RNA Labeling Kit (Roche, Germany). Coronal cryostat sections (25 μm thick) were hybridized with antisense or sense probes diluted in hybridization solution (150 ng/ml) at 52°C for 18 h. Hybridization was visualized using an alkaline phosphatase-conjugated sheep anti-DIG antibody (Roche; dilution 1:2000) with 4-nitroblue tetrazolium chloride (0.35 mg/ml) and 5-bromo-4-chloro-3-indolyl phosphate (0.18 mg/ml) as substrates. Tissue sections were visualized using a microscope and photographed using a digital camera (Jenoptik, Germany). Images were converted to TIFF format and contrast levels adjusted using Adobe Photoshop v. 7.0 (Adobe Systems, San Jose, CA, USA). The same intensity of light in the microscope and the same parameters in the digital camera were used when images were acquired, so minor adjustments were made to establish uniform contrast for all figures.
Double and triple labeling
After hybridization, as described above, some sections were incubated for 2 h with biotin-conjugated mouse monoclonal anti-DIG antibody (Jackson ImmunoResearch, West Grove, PA, USA; dilution 1:200) at room temperature. For double- or triple-immunofluorescence histochemistry, sections were incubated at 4°C overnight with following antibodies; monoclonal mouse anti-glial fibrillary acidic protein (GFAP; Chemicon International Inc., Temecula, CA, USA; dilution 1:500), monoclonal mouse anti-rat endothelial cell antigen-1 (RECA-1; Serotec; Oxford, UK; dilution 1:200), polyclonal rabbit anti-ionized calcium-binding adaptor molecule 1 (Iba1; Wako Pure Chemical Industries, Ltd., Osaka, Japan; dilution 1:500), monoclonal mouse anti-polysialylated neural cell adhesion molecule (PSA–NCAM; Chemicon International Inc.; dilution 1:200), alexa fluor 488 conjugated monoclonal mouse anti-neuronal nuclear antigen (NeuN; Chemicon International Inc.; dilution 1:100), polyclonal rabbit anti-calbindin (SIGMA, St. Louis, MO, USA; dilution 1:500) and monoclonal mouse anti-ED1 (Serotec; dilution 1:100). Antibody staining was visualized with the following secondary antibodies; Cy3-conjugated streptavidin (Jackson ImmunoResearch; dilution 1:1500), FITC-conjugated anti-mouse antibody (Jackson ImmunoResearch; dilution 1:50), FITC-conjugated anti-rabbit antibody (Jackson ImmunoResearch; dilution 1:50) and Cy5-conjugated anti-mouse antibody (Jackson ImmunoResearch; dilution 1:500). In controls, the primary antibody was omitted from the incubation solution. Counterstaining of cell nuclei was carried out by incubating the sections with DAPI (4′,6-diamidino-2′-phenyindole; Roche; dilution 1:1000) for 10 min.
Slides were viewed with a confocal microscope (LSM 510 Meta; Carl Zeiss Co., Ltd., Germany) equipped with four lasers (Diode 405, Argon 488, HeNe 543, HeNe 633). Images were converted to TIFF format, and contrast levels adjusted using Adobe Photoshop v. 7.0.
Bromodeoxyuridine administration and triple labeling
For labeling proliferating cells, sham-operated (n = 3) and ischemic rats (n = 3) were injected with bromodeoxyuridine (BrdU; SIGMA; 100 mg/kg) intraperitoneally once daily on days 7–9 after the sham operation or ischemia, and were sacrificed the next day after last injection. The choice to inject BrdU during this period was based on the report that ischemia-induced cell proliferation in the dentate gyrus is most prominent at 8 days following a forebrain ischemic injury in rats [36]. For triple-immunofluorescence histochemistry, hybridized sections were pretreated to denature DNA and incubated with monoclonal rat anti-BrdU antibody (Accurate Chemical & Scientific Corporation, Westbury, NY, USA; dilution 1:200) and PSA–NCAM. The sections were then reacted with a mixture of Cy3-conjugated streptavidin, FITC-conjugated anti-mouse antibody and Cy5-conjugated anti-rat antibody (Jackson ImmunoResearch; dilution 1:500) for 2 h at room temperature. Slides were viewed with a confocal microscope.
Results
Semiquantitative RT-PCR for VEGF-C and VEGFR-3 following transient forebrain ischemia
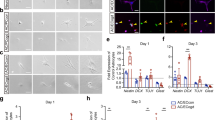
Semiquantitative RT-PCR analysis showed that VEGF-C expression was upregulated in the hippocampal CA1 region following transient forebrain ischemia. An increase in VEGF-C mRNA was observed in the hippocampi of animals subjected to 10 min of ischemia as early as 1 day later. The levels increased to maximum values at 3 days and then declined, although the enhanced expression was maintained until, at least, day 14, which was the latest time point examined (Fig. 1a). The expression of VEGFR-3 mRNA in the CA1 region obtained from rats subjected to 10 min of ischemia showed a temporal pattern similar to that of VEGF-C (Fig. 1b), but significant increases in VEGFR-3 expression were not observed at 1 and 14 days after ischemia.
RT-PCR analysis of genes for VEGF-C (a) and VEGFR-3 (b) in the microdissected CA1 region of the hippocampus of controls (Cont) and experimental rats at 1, 3, 7, and 14 days after transient forebrain ischemia. As an internal standard, GAPDH mRNA was measured. PCR products were run on the gel, and relative optical densities of the bands were obtained from three independent experiments, each performed in triplicate. The density of the VEGF-C or VEGFR-3 band was divided by the density of the band of GAPDH mRNA, representing the normalization factor. Both VEGF-C and VEGFR-3 signals increased 1 day after ischemia, reached a peak at 3 days, and remained elevated at 14 days. The data are expressed as the mean ± SEM. * P < 0.05 compared with sham-operated controls
Temporal profiles and phenotype of VEGF-C mRNA following transient forebrain ischemia
The distribution and cellular localization of VEGF-C mRNA in the hippocampus following 10 min of ischemia was examined using in situ hybridization histochemistry. Weak expression of VEGF-C mRNA was mainly localized to neurons of the pyramidal cell and granule cell layers in the hippocampi in control rats at all time points (Fig. 2a, e). Adjacent sections in these animals were routinely processed for in situ hybridization with the VEGF-C sense probe, and no specific cellular labeling was observed (insets in Fig. 2a, e). This was also true for all experimental animals. Three days after the 10-min period of ischemia, the signals for VEGF-C mRNA were observed in small cells predominantly in the strata radiatum and oriens of the CA1 region, and the dentate hilar region (Fig. 2b, f, g). The distribution pattern and morphology of these cells suggested that they might represent glial cells. At 7 days (Fig. 2c) and 14 days (Fig. 2d, h) after reperfusion, the labeling pattern was similar to those seen at 3 days after ischemia, but the labeling intensity decreased. Double labeling with VEGF-C mRNA and GFAP revealed that most VEGF-C-expressing cells in the CA1 region following ischemic injury were GFAP immunoreactive astrocytes (Fig. 3a–f). In addition, triple labeling with VEGF-C, Iba1, and ED1 identified that VEGF-C expression was localized in a small proportion of Iba1+/ED1+ cells, which were large, round, amoeboid-like brain macrophages in the CA1 pyramidal cell layer (Figs. 3g–l).
Changes in VEGF-C mRNA in the hippocampus following transient forebrain ischemia. a In control sections, in situ hybridization signals for VEGF-C mRNA were restricted to neurons of the granule cell and pyramidal cell layers. DG dentate gyrus. (Inset in a) section hybridized to sense-stranded probe showed the specificity of the probe. b Three days after ischemia, VEGF-C expression was detected in the dendritic layers of CA1 and the dentate hilar regions. At seven (c) and 14 (d) days after ischemia, the labeling intensity and pattern of VEGF-C expression were similar to those seen in the hippocampus 3 days after ischemia, but the labeling intensity was decreased. e–h Higher magnification views of the boxed areas in a, b, and d, respectively. GL granule cell layer; pcl pyramidal cell layer; PL polymorphic layer; sr stratum radiatum. (Inset in e) higher magnification view of the boxed area in inset of a. Scale bars = 300 μm for a–d, inset in a; 50 μm for e–h, inset in e
Identification of phenotypes of VEGF-C expressing cells in the CA1 of hippocampi seven days following transient forebrain ischemia. Hippocampal sections were processed consecutively for VEGF-C with in situ hybridization histochemistry (a, d, g, j), and GFAP (b, e), Iba1/ED1 (h), Iba1 (k) or ED1 (l) immunohistochemistry. c, f, i Superimposed images of in situ signals labeled by Cy3 (a, d, g), and FITC staining (b, e) or FITC/Cy5 (h). Note that most VEGF-C expressing cells were GFAP immunopositive astrocytes (arrows in d–f), whereas some labeled cells in the pyramidal cell layer (pcl) were Iba1/ED1 double labeled brain macrophages (arrowheads in j–l). d–f Higher magnification views of the boxed areas in a–c, respectively. j–l Higher magnification views of the boxed areas in g–i, respectively. sr stratum radiatum. Scale bars = 50 μm for a–c, g–i; 20 μm for d–f, j–l
Temporal profiles of VEGFR-3 mRNA following transient forebrain ischemia
Hybridization signals for VEGFR-3 mRNA in sham-operated rats were localized in neurons of the pyramidal cell and granule cell layers (Fig. 4a). The signals were also evident at a weaker intensity in some scattered cells outside the pyramidal cell layer and in the dentate hilar region. In adjacent control sections, routinely processed for in situ hybridization with the VEGFR-3 sense probe, absolutely no cellular labeling was observed (insets in Fig. 4a, e). Three days after reperfusion, the signals were evident in small cells, which were located adjacent to the pyramidal cell layer of the CA1 and CA3 regions and in the molecular layer and the hilar region of the dentate gyrus (Fig. 4b), and this expression pattern was maintained for 7 days (Fig. 4c). During the second week after reperfusion, labeling intensity gradually decreased, but the labeling pattern was still similar to that seen at 7 days in the CA1 region (Fig. 4d). As shown at higher magnifications in Fig. 4e–h, intense signals in the stratum radiatum of the CA1 region seemed to be from glial cells; this was confirmed by double or triple labeling with VEGFR-3 and GFAP, or Iba1/ED1. Most VEGFR-3-expressing cells were reactive astrocytes (Fig. 5a–f), and only a few cells were Iba1+/ED1+ microglia (Fig. 5g–l). In addition, VEGFR-3 expressing cells closely associated with blood vessels were also co-labeled with RECA-1, a marker for vascular endothelial cells (Fig. 5m–o).
Changes in VEGFR-3 mRNA in the hippocampus following transient forebrain ischemia. a In control sections, in situ hybridization signals for VEGFR-3 mRNA were observed in neurons of the granule cell and pyramidal cell layers, and in some scattered cells in the CA1 and dentate hilar regions. DG, dentate gyrus. (Inset in a) section hybridized to sense-stranded probe showed the specificity of the probe. b Three days after ischemia, significant induction of VEGFR-3 expression was detected in the dendritic layers of the CA1 and the dentate hilar regions. At seven (c) and 14 (d) days after ischemia, the labeling intensity and pattern of VEGFR-3 expression were similar to those seen in the hippocampus 3 days after ischemia. e–h Higher magnification views of the boxed areas in a–d, respectively. pcl pyramidal cell layer; sr stratum radiatum. (Inset in e) Higher magnification view of the boxed area in inset of a. Scale bars = 300 μm for a–d, inset in a; 50 μm for e–h, inset in e
Identification of phenotypes of VEGFR-3 expressing cells in the CA1 region of hippocampi seven days following transient forebrain ischemia. Hippocampal sections were processed consecutively for VEGFR-3 with in situ hybridization histochemistry (a, d, g, j, m), and GFAP (b, e), Iba1/ED1 (h), Iba1 (k), ED1 (l) or RECA-1 (n) immunohistochemistry. c, f, i, o Superimposed images of in situ signals labeled by Cy3 (a, d, g, m), and FITC staining (b, e, n) or FITC/Cy5 (h). Note that most VEGFR-3 expressing cells were GFAP immunopositive astrocytes, whereas some labeled cells were Iba1/ED1 immunoreactive brain macrophages (arrows in j–l). Note also that the VEGFR-3 labeled cells were also labeled with RECA-1, a marker for vascular endothelial cells (arrowheads in m–o). pcl pyramidal cell layer; sr stratum radiatum. Scale bars = 50 μm for a–c, g–i; 20 μm for d–f, j–o
Characteristics of VEGFR-3-expressing cells in the innermost layer of granule cells
Interestingly, 7 days after reperfusion (Figs. 6b, b1), increased expression of VEGFR-3, compared with sham-operated control animals (Fig. 6a, a1), was clearly evident along the innermost layer of granule cells of the dentate gyrus adjacent to the subgranular zone, a well recognized germinal center [7]. This expression pattern was maintained at 10 days (data not shown). At 14 days, the labeling intensity in these regions, although still more evident than in the sham-operated control animals, was considerably reduced from that at day 7 (Fig. 6c).
VEGFR-3 expression in the dentate granule cells following transient forebrain ischemia. a–c Higher magnification views of the boxed areas in Fig. 4 a (sham-operated control), c (7 days after ischemia) and d (14 days after ischemia), respectively. a1, b1 Higher magnification views of the boxed areas in Fig. 6 a, b, respectively. Note that strong VEGFR-3 expression was observed in the innermost layer of granule cells at 7 days after ischemia, compared with sham-operated control animal. d–f Double labeling for VEGFR-3 (d) and PSA-NCAM (e) in the dentate gyrus at day 7 after ischemic injury. Note that most PSA–NCAM immunoreactive cells coexpressed strong VEGFR-3 labeling. Scale bars = 50 μm for a–c, a1, b1; 20 μm for d, f
The pattern of intense VEGFR-3 expression in the innermost layer of granule cells overlapped with that of PSA–NCAM staining, a marker for immature neurons. Seven days after reperfusion, most PSA–NCAM immunoreactive cells coexpressed strong VEGFR-3 labeling (Fig. 6d–f), and these patterns were observed 10 days after reperfusion (data not shown). Triple labeling for VEGFR-3, PSA-NCAM, and either NeuN or calbindin revealed that cells expressing VEGFR-3 strongly were positive for PSA–NCAM but negative or weakly positive for NeuN, a mature neuronal marker (Fig. 7a–d), or calbindin, the dentate mature granule cell marker (Fig. 7e–h). By contrast, VEGFR-3 expression was relatively weak in NeuN or calbindin immunoreactive cells. Injecting BrdU at days 7–9 after reperfusion and sacrificing the animals the day following the last injection revealed that some VEGFR-3-expressing cells were double labeled with BrdU and PSA-NCAM (Fig. 7i–l).
Identification of phenotypes of VEGFR-3 expressing cells in the dentate gyrus following transient forebrain ischemia. a–h Triple labeling for VEGFR-3 (a, e), PSA-NCAM (b, f) and either NeuN (c) or calbindin (g) in the dentate gyrus seven days after ischemia. Note that cells expressing VEGFR-3 strongly were positive for PSA–NCAM, but negative or weakly positive for NeuN or calbindin (asterisks in a–h). i–l Triple labeling for VEGFR-3 (i), PSA–NCAM (j) and BrdU (k). Note that one VEGFR-3-expressing cell was double labeled with PSA–NCAM and BrdU (arrowheads in i–l). Scale bars = 20 μm for a–l
Discussion
In the present study, for the first time, we demonstrated the change in the expression of both VEGF-C and its tyrosine kinase receptor, VEGFR-3, in a rat model of cerebral ischemia. The expression profiles of VEGF-C and VEGFR-3 are very similar in the control hippocampi, but regulation of the two genes in the ischemic hippocampus showed characteristic region- and cell-dependent expression patterns. VEGF-C expression was upregulated in the CA1 and the dentate hilar regions, whereas upregulation of VEGFR-3 occurred in two distinct regions of the ischemic hippocampus: first in the CA1, CA3 and hilar regions, and second in the innermost layer of granule cells of the dentate gyrus.
In the CA1 and dentate hilar regions, which are particularly vulnerable areas within ischemic hippocampi, VEGF-C and VEGFR-3 were upregulated in activated glial cells, but not in any neurons. Activated glial cells expressing both genes were predominantly reactive astrocytes. The semiquantitative RT-PCR and in situ hybridization data indicated that expression for VEGF-C and VEGFR-3 in these areas was prominent by 3 days after reperfusion, and this was sustained up to at least day 14 after reperfusion, which correlates with the time points of astrogliosis following ischemic injury [12]. Thus, our data provide direct evidence that reactive astrocytes in the ischemic hippocampus synthesize both VEGF-C and the relevant receptor and that the temporal correlation of the two genes in astrocytes suggests a regulated response that enables enhanced paracrine or autocrine effects of VEGF-C in astrocytic responses to ischemic injury. Several studies have shown that VEGF-A is essential for astroglial proliferation and maintenance during repair following brain injury [2, 3, 18, 23, 37], but little is known about the function of the VEGF-C/VEGFR-3 axis in glial cells following brain injury. Thus, further studies are needed to investigate the role of VEGF-C in the astroglial reaction.
In addition, both VEGF-C and VEGFR-3 were induced in a small proportion of microglial cells in the CA1 and dentate hilar regions. VEGF-C- and VEGFR-3-expressing cells are ED1/Iba1 immunoreactive cells, which have large, round shape and are mostly restricted to the CA1 pyramidal cell layer, a site of intense neural damage. Considering that the ED1 antigen is expressed in the membranes of phagolysosomes in microglia and macrophages [4] and that the progressive activation of microglial cells is characterized by morphological transformation from ramified resting cells to bush-like cells during early activation and ultimately to phagocytic cells [19], we conclude that VEGF-C and VEGFR-3 were induced in brain macrophages. Interestingly, Jenny et al. [10] reported that VEGF-C and VEGFR-3 are expressed in human brain tumor and that VEGF-C is predominantly localized in macrophages, which is suggestive of its role in tumor-associated inflammation. In addition, murine macrophages express VEGF-C and VEGFR-3, and VEGF-C affects macrophage migration via VEGFR-3 [29, 30]. Thus, our data suggest that VEGF-C may function as a chemoattractant for microglia/macrophages via interaction with VEGFR-3 and that VEGF-C may be involved in microglial activation via paracrine or autocrine mechanisms. However, it is unclear why the induction of VEGF-C and its receptor was observed in a subpopulation of reactive microglial cells in the ischemic hippocampus.
Upregulation of VEGFR-3 was not confined solely to the glial cells in the CA1 and dentate hilar regions of the ischemic hippocampus. Increased expression of VEGFR-3 mRNA was induced in the innermost layer of granule cells on days 7–10 after reperfusion. This subsequently decreased. We found that upregulation of VEGFR-3 and PSA-NCAM had overlapping expression patterns in the innermost granule cells of the ischemic hippocampus, which were usually negative for the more mature neuronal markers NeuN and calbindin. Further, VEGFR-3 expression was relatively weak in mature granule cells expressing NeuN or calbindin, which were located deeper in the granule cell layer. In addition, a subpopulation of VEGFR-3/PSA-NCAM-expressing cells was colabeled with BrdU. These findings indicate increased VEGFR-3 expression in young, migrating neuronal cells and a rapid downregulation in maturing neurons, but weak expression of VEGFR-3 may be maintained in granule cells during differentiation. In support of this, newly generated granule cells strongly expressed PSA–NCAM on days 5–10 after transient global ischemia, indicating that proliferation and migration of progenitor cells had already commenced on day 5 after ischemic injury [32]. Overall, our data suggest that cells showing transient upregulation of VEGFR-3 in the innermost layer of granule cells following ischemic injury may be young neuroblasts and that VEGF-C may be involved in regulating the differentiation of neural precursor cells expressing VEGFR-3 in the ischemic hippocampus.
It has been reported that VEGF enhances postischemic neuronal proliferation and differentiation [16, 31, 34]. All of those studies addressed the role of VEGF-A in postischemic neurogenesis but not the function of the VEGF-C/VEGFR-3 axis. Involvement of VEGF-C in cerebral ischemia was shown by Gu et al. [8], who reported that VEGF-C and VEGFR-3 were upregulated in the ischemic cerebral cortex after photothrombotic ring stroke and that VEGF-C may promote early angiogenesis after stroke. In addition to its well-known role in lymphangiogenesis, VEGFR-3 is expressed by murine neural progenitor cells, and VEGF-C deficiency leads to severe defects in the proliferation of neuroepithelial cells [20]. Furthermore, Maurer et al. [24] found in their in vitro study that hypoxia induced VEGFR-3 mRNA in neural stem cells from hippocampus. These findings, together with our observations, lead us to speculate that VEGF-C may have specific roles in adult hippocampal neurogenesis during ischemic insults, but it remains to be elucidated whether the transient upregulation of VEGFR-3 in immature neurons reflects the function of its ligand in postischemic neurogenesis.
In summary, our data show that VEGF-C and VEGFR-3 are upregulated in activated glial cells, mostly reactive astrocytes and some microglia and macrophages in ischemic hippocampi. In addition, VEGFR-3 expression was transiently increased in the innermost layer of granule cells, which also expressed PSA-NCAM, following ischemic injury. These data suggest that the VEGF-C/VEGFR-3 axis may be involved in glial reaction in the ischemic brain and that VEGF-C may have specific roles in adult hippocampal neurogenesis during ischemic insults.
References
Achen MG, Stacker SA (1998) The vascular endothelial growth factor family; proteins which guide the development of the vasculature. Int J Exp Pathol 79:255–265. doi:10.1046/j.1365-2613.1998.700404.x
Brockington A, Lewis C, Wharton S, Shaw PJ (2004) Vascular endothelial growth factor and the nervous system. Neuropathol Appl Neurobiol 30:427–446. doi:10.1111/j.1365-2990.2004.00600.x
Choi JS, Kim HY, Cha JH, Choi JY, Chun MH, Lee MY (2007) Upregulation of vascular endothelial growth factor receptors Flt-1 and Flk-1 in rat hippocampus after transient forebrain ischemia. J Neurotrauma 24:521–531. doi:10.1089/neu.2006.0139
Damoiseaux JG, Döpp EA, Calame W, Chao D, MacPherson GG, Dijkstra CD (1994) Rat macrophage lysosomal membrane antigen recognized by monoclonal antibody ED1. Immunology 83:140–147
Dvorak HF, Detmar M, Claffey KP, Nagy JA, van de Water L, Senger DR (1995) Vascular permeability factor/vascular endothelial growth factor: an important mediator of angiogenesis in malignancy and inflammation. Int Arch Allergy Immunol 107:233–235
Ferrara N, Davis-Smyth T (1997) The biology of vascular endothelial growth factor. Endocr Rev 18:4–25. doi:10.1210/er.18.1.4
Gage FH, Kempermann G, Palmer TD, Peterson DA, Ray J (1998) Multipotent progenitor cells in the adult dentate gyrus. J Neurobiol 36:249–266. doi :10.1002/(SICI)1097-4695(199808)36:2<249::AID-NEU11>3.0.CO;2-9
Gu W, Brännström T, Jiang W, Bergh A, Wester P (2001) Vascular endothelial growth factor-A and -C protein up-regulation and early angiogenesis in a rat photothrombotic ring stroke model with spontaneous reperfusion. Acta Neuropathol 102:216–226
Issa R, Krupinski J, Bujny T, Kumar S, Kaluza J, Kumar P (1999) Vascular endothelial growth factor and its receptor, KDR, in human brain tissue after ischemic stroke. Lab Invest 79:417–425
Jenny B, Harrison JA, Baetens D et al (2006) Expression and localization of VEGF-C and VEGFR-3 in glioblastomas and haemangioblastomas. J Pathol 209:34–43. doi:10.1002/path.1943
Jin KL, Mao XO, Nagayama T, Goldsmith PC, Greenberg DA (2000) Induction of vascular endothelial growth factor receptors and phosphatidylinositol 3’-kinase/Akt signaling by global cerebral ischemia in the rat. Neuroscience 100:713–717. doi:10.1016/S0306-4522(00)00331-6
Jørgensen MB, Finsen BR, Jensen MB, Castellano B, Diemer NH, Zimmer J (1993) Microglial and astroglial reactions to ischemic and kainic acid-induced lesions of the adult rat hippocampus. Exp Neurol 120:70–88. doi:10.1006/exnr.1993.1041
Joukov V, Pajusola K, Kaipainen A et al (1996) A novel vascular endothelial growth factor, VEGF-C, is a ligand for the Flt4 (VEGFR-3) and KDR (VEGFR-2) receptor tyrosine kinases. EMBO J 15:290–298
Kaipainen A, Korhonen J, Mustonen T et al (1995) Expression of the fms-like tyrosine kinase 4 gene becomes restricted to lymphatic endothelium during development. Proc Natl Acad Sci USA 92:3566–3570. doi:10.1073/pnas.92.8.3566
Karkkainen MJ, Haiko P, Sainio K et al (2004) Vascular endothelial growth factor C is required for sprouting of the first lymphatic vessels from embryonic veins. Nat Immunol 5:74–80. doi:10.1038/ni1013
Kawai T, Takagi N, Mochizuki N et al (2006) Inhibitor of vascular endothelial growth factor receptor tyrosine kinase attenuates cellular proliferation and differentiation to mature neurons in the hippocampal dentate gyrus after transient forebrain ischemia in the adult rat. Neuroscience 141:1209–1216. doi:10.1016/j.neuroscience.2006.04.064
Kovács Z, Ikezaki K, Samoto K, Inamura T, Fukui M (1996) VEGF and flt. Expression time kinetics in rat brain infarct. Stroke 27:1865–1873
Krum JM, Mani N, Rosenstein JM (2002) Angiogenic and astroglial responses to vascular endothelial growth factor administration in adult rat brain. Neuroscience 110:589–604. doi:10.1016/S0306-4522(01)00615-7
Ladeby R, Wirenfeldt M, Garcia-Ovejero D et al (2005) Microglial cell population dynamics in the injured adult central nervous system. Brain Res Brain Res Rev 48:196–206. doi:10.1016/j.brainresrev.2004.12.009
Le Bras B, Barallobre MJ, Homman-Ludiye J et al (2006) VEGF-C is a trophic factor for neural progenitors in the vertebrate embryonic brain. Nat Neurosci 9:340–348. doi:10.1038/nn1646
Lee MY, Shin SL, Choi YS et al (1999) Transient upregulation of osteopontin mRNA in hippocampus and striatum following global forebrain ischemia in rats. Neurosci Lett 271:81–84. doi:10.1016/S0304-3940(99)00526-1
Lennmyr F, Ata KA, Funa K, Olsson Y, Terént A (1998) Expression of vascular endothelial growth factor (VEGF) and its receptors (Flt-1 and Flk-1) following permanent and transient occlusion of the middle cerebral artery in the rat. J Neuropathol Exp Neurol 57:874–882
Mani N, Khaibullina A, Krum JM, Rosenstein JM (2005) Astrocyte growth effects of vascular endothelial growth factor (VEGF) application to perinatal neocortical explants: receptor mediation and signal transduction pathways. Exp Neurol 192:394–406. doi:10.1016/j.expneurol.2004.12.022
Maurer MH, Tripps WK, Feldmann RE Jr, Kuschinsky W (2003) Expression of vascular endothelial growth factor and its receptors in rat neural stem cells. Neurosci Lett 344:165–168. doi:10.1016/S0304-3940(03)00407-5
Olofsson B, Pajusola K, Kaipainen A et al (1996) Vascular endothelial growth factor B, a novel growth factor for endothelial cells. Proc Natl Acad Sci USA 93:2576–2581. doi:10.1073/pnas.93.6.2576
Plate KH, Beck H, Danner S, Allegrini PR, Wiessner C (1999) Cell type specific upregulation of vascular endothelial growth factor in an MCA-occlusion model of cerebral infarct. J Neuropathol Exp Neurol 58:654–666. doi:10.1097/00005072-199906000-00010
Pulsinelli WA, Brierley JB (1979) A new model of bilateral hemispheric ischemia in the unanesthetized rat. Stroke 10:267–272
Raab S, Plate KH (2007) Different networks, common growth factors: shared growth factors and receptors of the vascular and the nervous system. Acta Neuropathol 113:607–626. doi:10.1007/s00401-007-0228-3
Skobe M, Hamberg LM, Hawighorst T et al (2001) Concurrent induction of lymphangiogenesis, angiogenesis, and macrophage recruitment by vascular endothelial growth factor-C in melanoma. Am J Pathol 159:893–903
Stepanova OI, Krylov AV, Lioudyno VI, Kisseleva EP (2007) Gene expression for VEGF-A, VEGF-C, and their receptors in murine lymphocytes and macrophages. Biochemistry (Mosc) 72:1194–1198. doi:10.1134/S0006297907110041
Sun Y, Jin K, Xie L et al (2003) VEGF-induced neuroprotection, neurogenesis, and angiogenesis after focal cerebral ischemia. J Clin Invest 111:1843–1851
Tanaka R, Yamashiro K, Mochizuki H et al (2004) Neurogenesis after transient global ischemia in the adult hippocampus visualized by improved retroviral vector. Stroke 35:1454–1459. doi:10.1161/01.STR.0000126480.40967.b3
Veikkola T, Jussila L, Makinen T et al (2001) Signalling via vascular endothelial growth factor receptor-3 is sufficient for lymphangiogenesis in transgenic mice. EMBO J 20:1223–1231. doi:10.1093/emboj/20.6.1223
Wang Y, Jin K, Mao XO et al (2007) VEGF-overexpressing transgenic mice show enhanced post-ischemic neurogenesis and neuromigration. J Neurosci Res 85:740–747. doi:10.1002/jnr.21169
Witmer AN, Dai J, Weich HA, Vrensen GF, Schlingemann RO (2002) Expression of vascular endothelial growth factor receptors 1, 2, and 3 in quiescent endothelia. J Histochem Cytochem 50:767–777
Yagita Y, Kitagawa K, Ohtsuki T et al (2001) Neurogenesis by progenitor cells in the ischemic adult rat hippocampus. Stroke 32:1890–1896
Yasuhara T, Shingo T, Date I (2004) The potential role of vascular endothelial growth factor in the central nervous system. Rev Neurosci 15:293–307
Acknowledgments
This research was supported by a grant (M103KV010010-08K2201-01010) from Brain Research Center of the 21st Century Frontier Research Program funded by the Ministry of Science and Technology, The Republic of Korea.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Shin, YJ., Choi, JS., Lee, JY. et al. Differential regulation of vascular endothelial growth factor-C and its receptor in the rat hippocampus following transient forebrain ischemia. Acta Neuropathol 116, 517–527 (2008). https://doi.org/10.1007/s00401-008-0423-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00401-008-0423-x