Abstract
Purpose
Transverse testicular ectopia (TTE) is a well described, rare congenital abnormality of testicular descent, in which both testes migrate through one inguinal canal. The objective of this work was to present three cases of TTE, one of them with a common vas deferens. To our knowledge, a fused vas deferens has only been reported four times in previously published reports.
Methods
Three patients presented with inguinal hernia and contralateral cryptorchidism. In case 1, the diagnosis of TTE was made preoperatively by palpating two testes in one hemiscrotum. The diagnosis of case 2 was made intraoperatively and was found to be of a rare form in which the two vasa deferentia fused in the inguinal canal to form a common vas deferens. The diagnosis of case 3 was also done intraoperatively and a laparoscopy was performed to document the anatomy of TTE and to rule out the presence of Müllerian duct remnants. We also performed a literature search for other reports of TTE.
Results
The three cases were operated with trans-septal orchidopexy. In addition, laparoscopy was performed in case 3 to clarify the anatomy. Biopsy revealed normal testicular tissue from both testes in the first two patients. Follow-up with ultrasound, 6 months after operation showed normal size and blood flow of both testes.
Conclusion
Transverse testicular ectopia should be suspected in a boy with an inguinal hernia and contralateral non palpable testis. Trans-septal orchidopexy is recommended when vasa deferentia are fused. Laparoscopy is useful to document the anatomy and to rule out the presence of Müllerian remnants.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Transverse testicular ectopia (TTE) is a rare anatomic abnormality in which both testes migrate toward the same hemiscrotum. Different nomenclature has been used for this condition: crossed testicular ectopia, testicular pseudo duplication, unilateral double testes, and transverse aberrant testicular maldescent. Most of the cases (65 %) are diagnosed intraoperatively during an inguinal hernia repair. Only a few are diagnosed preoperatively [1].
The aim of this report was to present our experience with three cases of TTE and to send an important message: laparoscopy should be performed as the first step in cases with inguinal hernia and a contralateral non palpable testis.
Patients and methods
Three children that presented with inguinal hernias and contralateral non palpable testis were found to have TTE. The clinical reports, radiological findings, and operative notes were reviewed retrospectively. We describe each case separately to give a better clue on the findings and at the same time to highlight the options for management.
Results
Case 1
A healthy 4.5-year-old boy was referred to the pediatric surgical clinic for left inguinal hernia. Physical examination revealed two testis-like masses in the left hemiscrotum (Fig. 1) and an empty right hemiscrotum. Ultrasonography (US) was performed and showed two testes in the left hemiscrotum. No testis was found on the right side and no remnants of Müllerian ducts could be shown. Exploration of the left groin revealed two normal-sized testes, each with its separate vas and blood supply. After herniotomy, the ectopic testis was placed trans-septally into the right hemiscrotum. Biopsy from both testes showed normal histological findings. After 6 months, a follow-up US of the scrotum revealed normal size and blood flow of both testes.
Case 2
A healthy 5-year-old boy was referred to the pediatric surgical clinic with left inguinal hernia. Physical examination revealed a left inguinal hernia and an empty right hemiscrotum. Exploration of the left groin revealed a hernia sac and two normal-sized testes, each with its separate vas and blood supply. Both vasa deferentia fused in the left inguinal canal (Fig. 2) to form a common vas deferens, which subsequently passed along the retroperitoneal area on the left side. Because of vasa deferentia fusion, both testes were brought down through the left inguinal canal to avoid damage to the common vas. The left testis was placed in the left hemiscrotum while the right testis was placed in the right hemiscrotum after trans-septal incision. Biopsy from both testes showed normal histological findings. Follow-up with US of the scrotum, 6 months after operation, revealed normal blood flow and normal size of both testes.
Case 3
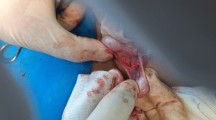
An 1-month-old boy was referred with a right-sided inguinal hernia. He had a palpable testis in his right inguinal canal but no palpable testis on the left side. A pre-operative US confirmed the position of the right testis but could not identify the left testis. A right-sided herniotomy was performed at 6 weeks of age. At dissection, the hernia sac was found to contain two testes. The gubernacula of the two testes were fused (Fig. 3). Each testis had separate epididymis, vas and vessels. A 5-mm laparoscopic camera was inserted through an infra-umbilical incision. In addition to apparently normal right-sided vas and vessels, the left vas deferens entered the abdomen through the right internal inguinal ring and crossed the dome of the bladder obliquely in the direction of the seminal vesicle on the left side (Fig. 4). The vessels to the left testis were readily identified at the right inguinal ring. The left internal inguinal ring was closed and no funicular structures could be indentified (Fig. 4). A trans-septal orchidopexy was performed. Follow-up with clinical examination, 12 weeks after the operation, showed two normal-sized testes in a symmetrical scrotum.
Discussion
Transverse testicular ectopia was first described by Von Lenhossek [2], who in 1886 observed this form of ectopic testis in an autopsy performed by his father. The mean age at the time of diagnosis of TTE is 4 years [3]. Most of the cases (65 %) are diagnosed intraoperatively during an inguinal hernia repair; only few are diagnosed preoperatively [3]. Actually, the few reported cases of preoperative diagnosis of TTE have been based on US [4] or MRI [5]. Case 1 was diagnosed by clinical examination (Fig. 1). To our knowledge there is no previously reported case of TTE that was diagnosed by clinical examination.
Several theories have been proposed in an attempt to explain the etiology of this rare anomaly. Berg [6] thought that the two testes arose from the same germinal ridge. Josso [7] suggested various anatomical factors that may result in such an anomaly: defective implantation of the gubernaculum, obstruction of the inguinal ring and development of adhesions between the testes and adjacent structure. Clarnette [8] postulated that distal gubernaculotomy in the rat could prevent development of the processus vaginalis because of mechanical disruption of the gubernaculum. Despite this wide variety of theories, the exact mechanism for the etiology of this condition is still not fully understood. In case 1, the left testis was attached to a normal gubernaculum, while the right testis was not. The testes and their vas also were not attached to each other. Disruption of the distal gubernaculum seems to be the most plausible explanation as a possible mechanism for the etiology in this case.
In case 2, the two vasa were fused to form a common vas deferens, and the possible mechanism for etiology can be explained by one of two suggested theories: (1) both testes developed from the same germinal ridge on one side, descended to the same side, with both testes having a common vas deferens and blood supply. (2) Bilateral development of the testes, one being carried to the opposite side with its blood supply and both testes having a common vas deferens arising from one side. Laparoscopy could be the first step to document the anatomy but at that time we were not prepared for laparoscopy. To our knowledge, a fused vas deferens has only been reported four times in the literature. In case 3 we performed laparoscopy to clarify the anatomy, which allowed exclusion of Müllerian duct remnants. Since the 1990s laparoscopy has played a big role in the management of TTE. Balaji and Diamond [11] first reported a case of TTE that was both diagnosed and treated by laparoscopy. Laparoscopy is useful for the diagnosis of associated anomalies like common vas deferens or Müllerian duct remnants. Genitourinary developmental abnormalities have been documented in 20 % of the cases in the form of defective Mullerian regression (rudimentary uterus), common vas deferens, seminal vesicle cyst, and bilateral renal dysgenesis [1, 9, 10, 12]. Testicular malignancies have been identified in some cases, seminoma being the pathology in the majority of cases [13].
The three cases were operated with trans-septal orchidopexy. This approach is recommended to minimize the risk of injuries to vas and vessels. The authors stress an important message: laparoscopy should be performed as the first step in cases with inguinal hernia and a contralateral non palpable testis.
Conclusion
Transverse testicular ectopia should be suspected in a boy with an inguinal hernia and a contralateral non palpable testis. Both clinical examination and US are useful for preoperative diagnosis. Laparoscopy is recommended to confirm the diagnosis and treat TTE. Trans-septal orchidopexy gives an excellent cosmetic appearance with minimal dissection and risk of injuries to vas and vessels.
References
Hammoudi S (1989) Transverse testicular ectopia. J Pediatr Surg 24(2):223–224
Von Lenhossek M (1886) Ectopia testes transverse. Anat Anz 1:376
Gauderer MW, Grisoni ER, Stellato TA (1982) Transverse testicular ectopia. J Pediatr Surg 17:43–47
Chen KC, Chu CC, Chou TY (2000) Transverse testicular ectopia: preoperative diagnosis by ultrasonography. Pediatr Surg Int 16(1–2):77–79
Lam WW, Le SD, Chan KL et al (2002) Transverse testicular ectopia detected by MR imaging and MR venography. Pediatr Radiol 32:126–129
Berg AA (1904) Transverse ectopy of the testis. Ann Surg 40:223–224
Josso N (1977) Development and descent of the fetal testis. In: Bierich JL, Rager K, Ranke MB (eds) Maldescensus testis. Urban and Schwarzenberg, Munich, pp 3–11
Clarnette TD, Hutson JM, Beasley SW (1996) Factors affecting the development of the processus vaginalis in the rat. J Urol 156:1463–1466
Kimura T (1981) Transverse ectopia of the testis with masculine uterus. Ann Surg 68:420–425
Hughes DT, Croitoru DP (2007) Case report: crossed testicular ectopia. J Pediatr Surg 42(9):1620–1622
Balaji KC, Diamond DA (1995) Laparoscopic diagnosis and management of transverse testicular ectopia. Urology 46:879–880
Avolio L, Belville C, Bragheri R (2003) Persistent mullerian duct syndrome with crossed testicular ectopia. Urology 62(2):350
Fujita J (1980) Transverse testicular ectopia. Urology 16(4):400–402
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Naji, H., Peristeris, A., Stenman, J. et al. Transverse testicular ectopia: three additional cases and a review of the literature. Pediatr Surg Int 28, 703–706 (2012). https://doi.org/10.1007/s00383-012-3105-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-012-3105-7