Abstract
Pathological intussusception is rare in infancy with Meckel’s diverticulum being the most common lesion. Isolated heterotopic pancreatic tissue in the serosa of the ileum causing intussusception is extremely rare. We report a case of ileal heterotopic pancreatic tissue associated with ectopic gastric mucosa causing ileocolic intussusception in an infant, with review of the literature.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Most intussusceptions that occur in infancy are idiopathic in origin [1]. In a small proportion of cases a pathological lead point is identified as the cause of an intussusception, with Meckel’s diverticulum being the most common lesion [2–4]. The incidence of intestinal ectopia in a Meckel’s diverticulum is approximately 30–50% [2]. Isolated heterotopic pancreatic tissue in the ileum causing intussusception is extremely rare [2]. Combination of ileal serosal heterotopic pancreatic tissue and an ectopic gastric mucosa as a cause of intussusception is even more of a rarity [1]. We report a case of combined ileal serosal heterotopic pancreatic and mucosal gastric tissues causing an ileocolic intussusception in an infant.
Case report
A 6-month-old, twin boy, presented with a 1-day history of crying, irritability, pallor, and drawing up his legs. He was born at 35 weeks gestation with a birth weight of 2.5 kg and had been previously well. He had a loose bowel motion (no blood) 12 h prior to presentation and no vomiting.
Physical examination revealed a pale and tachycardic child who looked unwell. The abdomen was soft and non-distended with a palpable mass in the left upper quadrant. There were no peritoneal signs, bowel sounds were present, and rectal examination was unremarkable.
An ultrasound scan was carried out, prior to surgical consultation, which confirmed the diagnosis of intussusception (Fig. 1). Attempted air enema reduction was unsuccessful.
At laparotomy an ileocolic intussusception, with extensive necrotic bowel, and reactive mesenteric lymphadenopathy was found. A limited right hemicolectomy was performed.
The patient’s post-operative recovery was uneventful and he was discharged on the fifth post-operative day.
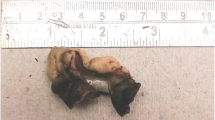
The specimen consisted of ascending colon and ileum, with 120 mm of ileum intussuscepted through the ileocaecal valve into the cecum. The distal 100 mm of the intussuscepted ileum was dark, haemorrhagic, and appeared non-viable close to the tip of the intussusception. The lead point of the intussusception was a firm pale nodule (6×5×5 mm3), which appeared to be within the wall.
On histology the nodule was heterotopic exocrine and endocrine pancreas with ducts present. It was within the serosa and the outer coat of the muscularis propria. No duct was seen connecting with the mucosa. The mucosa in this area though necrotic and haemorrhagic was thick with absent villous outline compared with adjacent mucosa. The viable glandular epithelium in this area was also different and consisted of mucous cells and rounded cells with pink cytoplasm suggestive of parietal cells. The overall appearance was consistent with heterotopic gastric mucosa (Fig. 2a, b).
a Histopathology showing firm pale nodule (6×5×5 mm3) within the serosa and the outer coat of muscularis propria at the tip of intussusception, the lead point is heterotopic pancreas in the serosa (black arrow) associated with ectopic gastric mucosa (white arrow). b Slide showing pancreatic tissue (arrow) within the ileal serosa
Discussion
Heterotopic pancreas can be defined as pancreatic tissue lacking anatomic and vascular continuity with the main body of the pancreas [2, 5]. Heterotopic pancreas has an estimated occurrence of 1 in 500 upper abdominal operations and has been reported to be present in 0.6–5.6% of autopsy cases [6]. It is rarely detected in children [2].
The most common locations of heterotopic pancreas are the stomach, duodenum, and jejunum [6, 7]. Isolated pancreatic tissue in the ileum is rare, mainly asymptomatic and usually discovered incidentally [8]. Multiple lesions are exceptional [2].
Studies have shown that heterotopic pancreas can produce clinical symptoms. Symptoms include epigastric pain, haemorrhage, weight loss, nausea, and vomiting. Reported complications include malignant change, cyst formation, pancreatitis, insulinoma, and intussusception [5].
It has been reported that two-thirds of isolated ileal heterotopic pancreas cases are found incidentally at the time of surgery [9]. Correct pre-operative diagnosis of heterotopic pancreas is not made, even in symptomatic patients, with the use of barium enema, ultrasound scan, computer tomography, or laparoscopy [9]. It should be suspected with intussusception in extremes of age, 3 months or less or greater than 2 years, and in cases of chronic intermittent, early recurrent, or double intussusception [2, 10, 11].
Symptomatic isolated ileal heterotopic pancreas should be managed by segmental resection, open or laparoscopic techniques. Incidental findings should be biopsied and sent for frozen section and resection or excision carried out [2].
There are a number of theories of origin with respect to heterotopic tissues. Skandelakis et al. suggested that metaplasia of pluripotential endodermal cells of the embryonic foregut as an origin for heterotopic tissues. This may provide an explanation for the occasional report of an unusual site such as the fallopian tube [12, 13]. Others have suggested that separation of pancreatic tissue occurs during embryonic rotation and fusion of the ventral and dorsal pancreatic buds [5]. Abel et al. suggested heterotopic pancreas, especially when associated with gastric mucosa, represents a vitellointestinal tract remnant, similar to a Meckel’s diverticulum without the diverticulum [1]. Nonetheless, all above hypotheses have not been tested yet.
On review of the English language literature the first reported case of isolated ileal heterotopic pancreas causing intussusception was by Barbosa et al. in 1946. This was followed by few case reports in paediatric and adult literatures [2, 7–9, 11, 14–19].
There have only been three cases reported in the English literature to date, of intussusception caused by combined ileal heterotopic pancreatic and gastric tissue. Iucthman et al. reported the first case in a 15-year-old boy with intermittent ileocolic intussusception [10]. Abel et al. reported the others in two 16-month-old boys with ileoileal and ileocolic intussusceptions, respectively, where the heterotopic pancreas was located in the ileal serosal tissue in both cases.
Our case is similar to Abel et al. in regard to the location of heterotopic pancreatic tissue within the serosa associated with ectopic gastric mucosa. However, the age of presentation was younger.
References
Abel R, Keen CE, Bingham JB, Maynard J, Agrawal MR, Ramachandra S (1999) Heterotopic pancreas as leadpoint in intussusception: new variant of vitellointestinal tract malformation. Pediatr Dev Pathol 2:367–370
Hamada Y, Yonekura Y, Tanano A, Takada K, Kato Y, Sato M, Sakaida N, Okamura A, Hioki K (2000) Isolated heterotopic pancreas causing intussusception. Eur J Pediatr Surg 10:197–200
Ong N-T, Beasley SW (1990) The leadpoint in intussusception. J Pediatr Surg 25:640–643
Stringer MD, Pablot SM, Brereton RJ (1992) Paediatric intussusception. Br J Surg 79:867–876
Armstrong CP, King PM, Dixon JM, Macleod IB (1981) The clinical significance of heterotopic pancreas in the gastrointestinal tract. Br J Surg 68:384–387
Barbosa J, Dockerty MB, Waugh JM (1946) Pancreatic heterotopia: review of the literature and report of 41 authenticated surgical cases of which 25 were clinically significant. Surg Gynecol Obstet 82:527–542
Moen J, Mack E (1976) Small-bowel obstruction caused by heterotopic pancreas in an adult. Am Surg 55:503–504
Pang LC (1988) Pancreatic heterotopia: a reappraisal and clinicopathological analysis of 32 cases. South Med J 81:1264–1275
Tanaka K, Tsunoda T, Eto T (1993) Diagnosis and management of heterotopic pancreas. Int Surg 78:32–35
Iuchtman M, Zamir D, Bartal T, Soimu U (1999) Radiological case of the month; intermittent ileocolic intussusception caused by an unusual choristoma. Arch Pediatr Adolesc Med 153(7):763–764
Scholz S, Loff S, Wirth H (2000) Double intussusception caused by a giant polypoid mass of heterotopic pancreas in a child. Eur J Pediatr 159:861–862
Skandalakis LJ, Rowe JS Jr Gray SW, Skandalakis JE (1993) Surgical embryology and anatomy of the pancreas. Surg Clin North Am 73:661–697
Mason TE, Quagliarello JR (1976) Ectopic pancreas in the fallopian tube: report of first case. Obstet Gynecol 48:70s–73s
Carleton CC, Ackerbaum R (1976) Intussusception secondary to aberrant pancreas in a child. JAMA 236:1047
Anseline P, Grundfest S, Carey W (1981) Pancreatic heterotopia—a rare cause of bowel obstruction. Surgery 90:110–113
Salman B, Besbas N, Coskun T (1992) Intussusception due to ectopic pancreatic tissue in a nine-month-old child. Turk J Pediatr 34:255–258
Erdener A, Avanoglu A, Ozok G (1993) Intussusception in an infant caused by aberrant pancreas. J Pak Med Assoc 43:22–23
Montgomery EA, Popek EJ (1994) Intussusception, adenovirus, and children: a brief reaffirmation. Hum Pathol 25:169–174
Keeley JL (1950) Intussusception associated with aberrant pancreatic tissue: report of a case and review of the literature. Arch Surg 60:691–698
Acknowledgment
We would like to take the opportunity and thank Dr. T. Lawrence for her effort in collecting the histopathology photographs.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Al-Zahem, A., Arbuckle, S. & Cohen, R. Combined ileal heterotopic pancreatic and gastric tissues causing ileocolic intussusception in an infant. Ped Surgery Int 22, 297–299 (2006). https://doi.org/10.1007/s00383-005-1566-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-005-1566-7