Abstract
Purpose
To describe our surgical technique and report the oncological outcomes and complication rates using a fascial-sparing radical inguinal lymphadenectomy (RILND) technique for penile cancer patients with cN+ disease in the inguinal lymph nodes.
Methods
Over a 10-year period, 660 fascial-sparing RILND procedures were performed in 421 patients across two specialist penile cancer centres. The technique used a subinguinal incision with an ellipse of skin excised over any palpable nodes. Identification and preservation of the Scarpa’s and Camper’s fascia was the first step. All superficial inguinal nodes were removed en bloc under this fascial layer with preservation of the subcutaneous veins and fascia lata. The saphenous vein was spared where possible. Patient characteristics, oncologic outcomes and perioperative morbidity were retrospectively collected and analysed. Kaplan–Meier curves estimated the cancer-specific survival (CSS) functions after the procedure.
Results
Median (interquartile range, IQR) follow-up was 28 (14–90) months. A median (IQR) number of 8.0 (6.5–10.5) nodes were removed per groin. A total of 153 postoperative complications (36.1%) occurred, including 50 conservatively managed wound infections (11.9%), 21 cases of deep wound dehiscence (5.0%), 104 cases of lymphoedema (24.7%), 3 cases of deep vein thrombosis (0.7%), 1 case of pulmonary embolism (0.2%), and 1 case of postoperative sepsis (0.2%). The 3-year CSS was 86% (95%Confidence Interval [95% CI] 77–96), 83% (95% CI 72–92), 58% (95% CI 51–66), respectively, for the pN1, pN2 and pN3 patients (p < 0.001), compared to a 3-year CSS of 87% (95% CI 84–95) for the pN0 patients.
Conclusion
Fascial-sparing RILND offers excellent oncological outcomes whilst decreasing the morbidity rates. Patients with more advanced nodal involvement had poorer survival rates, emphasizing the need for adjuvant chemo-radiotherapy.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Penile cancer is a rare malignancy that accounts for less than 1% of all newly diagnosed cancer cases in the UK [1]. Since the early 1990s penile cancer incidence rates have increased by 25% [1]. Due to the rarity of penile cancer in the UK, the management is centralized to supra-regional penile cancer centres [2]. This allows access to centres with surgical expertise allied to specialist pathology and radiology services, thus ensuring optimal oncological and functional outcomes [3].
Although survival rates after a penile cancer diagnosis are improving in the UK, most likely due to early diagnosis and referral to specialist centres, the treatment is still associated with high rates of peri-operative and long-term morbidity[3]. Penile preserving procedures for the primary lesion are now standard of care and include wide local excision (WLE), glans resurfacing [4] and glansectomy [5]. The presence of nodal metastasis remains the most important prognostic indicator [6]. Indications for radical inguinal lymph node dissection (RILND) include metastatic disease detected by fine needle aspiration cytology (FNAC), metastatic disease detected following dynamic sentinel lymph node biopsy (DSNB) or palpable inguinal lymph nodes with obvious imaging features or confirmation on biopsy [6].
The classic, and most radical, technique of RILND was originally described by Daseler et al. and involved resection of the fascia lata, skeletalization of the femoral vessels followed by transposition of the sartorius muscle to cover the vessels [7]. The reported complications of this procedure include lymphoedema, deep venous thrombosis (DVT), wound infection, skin necrosis, lymphocele, and seroma [8]. Given the high morbidity associated with this approach, a number of modifications of the classic surgical technique have been proposed with the aim of reducing the size of the incision and/or the number of lymph nodes removed, whilst ensuring oncological outcomes that are comparable to the classic technique [3]. Notwithstanding these attempts to mitigate the morbidity associated with RILND, these approaches still remain associated with a number of significant complications, including lower limb and genital lymphoedema and wound infection/dehiscence/skin flap necrosis which may cause protracted healing, potentially permanent disfigurement and/or functional impairment [9, 10].
We aim to describe our surgical approach along with its oncological outcomes and associated morbidity using a fascial-sparing RILND technique.
Patients and methods
Data collection and patient selection
Data from 421 patents were collected from a two-centre institutional database over a 10-year period comprising a total of 660 fascial-sparing RILND being performed by 8 penile cancer surgeons using the same standard technique, having previously trained together and performed the procedure jointly.
We retrospectively identified those penile cancer patients who underwent a fascial-sparing RLND. Indications for fascial-sparing RLND were DSNB or FNAC with a positive histology for penile cancer metastasis, or clinically enlarged inguinal lymph nodes at the physical examination or radiological investigation (cN+). All of the patients who required neo-adjuvant chemotherapy, those having radiological evidence of distant metastasis or those patients having large fungating and exophytic groin masses were excluded, as they were deemed unsuitable for the fascial-sparing RILND.
Clinical and histopathological details of all patients with penile cancer treated with fascial-sparing RILND were collected retrospectively using a standardized approach in the database.
All patients were examined in the clinic preoperatively with ultrasonography of the cN0 groins performed together with computed tomography staging of the thorax, abdomen and pelvis. Those patients having a low risk of inguinal micro-metastatic (≤ pT1aG2) involvement according to the European Association of Urology (EAU) guidelines’ risk stratification tool were offered surveillance instead of invasive nodal staging [6]. Those patients with intermediate- and high-risk penile cancer with cN0 disease were offered FNAC followed by DSNB. All eligible patients with palpable inguinal nodes, imaging consistent with inguinal-node involvement, confirmed nodal metastasis on either pre-operative FNAC, and/or positive DSNB were offered fascial-sparing RILND. All specimens underwent pathology review within a multidisciplinary meeting. Tumour stage and grade were determined according to the most recent TNM classification [11].
Post-operative surgical complications were recorded and scored according to the Clavien–Dindo classification [12].
Follow-up
Following discharge from the hospital after RILND, the patients were all placed under a standard surveillance protocol at our institution, consisting of an outpatient clinic visit every 3–4 months for 2 years followed by every 6 months for one year then annually to 5 years.
Statistical analysis
The normal distribution of data was tested with the Shapiro–Wilk test. Data are presented as medians (interquartile range; IQR) for continuous variables and frequencies (proportions) for categorical variables. The median follow-up was computed with the inverse Kaplan–Meier methods.
Cancer-specific survival (CSS) was defined as the time from surgery to death because of penile cancer or to the end of follow-up.
Kaplan–Meier curves for CSS were plotted according to pN status, and survival rates estimated the post-operative survival functions at the 3-year follow-up interval.
A supplementary analysis has been performed regarding the complication rates in those patients who received a monolateral vs. a bilateral fascial-sparing RILND procedure. Chi-square was used to compare the categorical variables between the two groups.
Data were analysed using the SPSS software (SPSS Inc, Chicago, IL, USA).
Ethical statement
This was a retrospective review and audit of outcomes. The surgical procedures and treatment were in line with the institutional guidelines and operational policy and approved as part of the MDT process as part of standard management for penile cancer at our institutions. All data were anonymized. All participants gave full informed consent for surgery.
Surgical technique
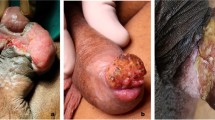
The intraoperative photos of the technique can be seen in Fig. 1, whilst the differences between the classical RILND approach and our fascial-sparing approach are summarized in Supplementary Table 1. The procedure was performed under general anaesthetic in a supine position with the lower limbs abducted. Broad-spectrum prophylactic antibiotics were used. The surgical landmarks were marked on the skin prior to the surgical incision. A subinguinal incision was performed 2 cm below the inguinal crease. An ellipse of skin was excised over any palpable nodes or as part of the scar excision from previous dynamic sentinel node biopsies. The superior border of the dissection template was a line tracked from the anterior superior iliac spine to the pubic tubercle, the lateral margin was the medial border of the Sartorius muscle and the medial margin was the lateral border of the adductor longus muscle, whilst the floor was the preserved fascia lata. Early identification and preservation of Scarpa’s fascia and Camper’s fascia ensured that the venous drainage of the skin flaps was preserved. The lymph node packet with the adjacent fibrofatty tissue containing the superficial inguinal nodes was removed en bloc under this fascial layer. Meticulous ligation of lymphatic vessels using absorbable ties was performed to reduce postoperative lymphocele and lymphorrea. The fascia lata and cribriform fascia were preserved and the inguinal lymph nodes deep to these layers were not removed. The long saphenous vein (LSV) was spared where possible. A 12Fr redivac drain was placed followed by the closure of Scarpa’s fascia and Camper’s fascia using interrupted 2–0 ensuring accurate alignment of this layer. The skin incision was closed with interrupted absorbable sutures ensuring accurate skin apposition. All patients were discharged with a one-week peri-operative course of antibiotics in combination with compression stockings until discharge. Patients were typically allowed to mobilize on post-operative day 1. The drains remained in situ until < 40 ml/day drained for 2 consecutive days.
Surgical technique. A Identification of Scarpa’s fascia. B Dissection under the Scarpa’s fascia keeping the fascia itself intact. C The lymph node packet containing the superficial inguinal lymph nodes is removed en bloc deeply to the Scarpa’s and Camper’s fasciae, which are spared to ensure adequate venous drainage of the skin flaps. D Fascia lata and cribriform fascia are identified and spared after complete excision of the lymph node packet. The long saphenous vein is also spared. E A 12Fr redivac drain is placed. The Scarpa’s and Camper’s fasciae are accurately closed with interrupted 2–0 vicryl sutures. F Final result. The skin incision is closed with interrupted vertical mattress absorbable sutures ensuring accurate skin apposition
Results
A total of 660 fascial-sparing inguinal lymphadenectomy procedures were performed in 421 patients. Patient characteristics are detailed in Table 1. Median (interquartile range, IQR) age was 63.0 (55.0–72.0) years. 86 (20.4%) patients were pT1, 203 (48.2%) pT2 and the remnants pT3 or higher at presentation.
The overall number of patients receiving a bilateral fascial-sparing RILND was 239, whilst the remaining 182 patients received a monolateral fascial-sparing RILND.
A median (IQR) number of 8.0 (6.5–10.5) nodes were removed per groin. There were 121 (28.7%) patients with stage pN0, 55 (13.1%) with stage pN1 and 201 (47.7%) with stage pN3. In 127 cases (30.1%), despite a positive DSNB, there was no further positive lymph node at completion fascial-sparing RILND.
The postoperative course was uneventful in 268/421 (63.9%) cases. A total of 153 postoperative complications (36.1%) occurred in the series, including 50 wound infections (11.9%), 21 cases of deep wound dehiscence (5.0%), 104 cases of lymphoedema (24.7%), 3 cases of deep vein thrombosis (0.7%), 1 case of pulmonary embolism (0.2%), 3 cases of urinary tract infection (0.7%), and 1 case of postoperative sepsis (0.2%). All of the cases of superficial wound infection resolved spontaneously, without the need of any antibiotic treatment or any other intervention by the end of the second week after discharge from the hospital. Deep wound infections/dehiscences were treated with a prolonged course of antibiotics in all of the cases; the wounds were left to heal by secondary intention and through vacuum-assisted closure (VAC) when necessary. Although lymphoedema was the most frequent complication, this was minor and self-limiting/conservatively managed in the majority of the patients. Perioperative mortality was never observed in this series. All the complications, along with their classification according to the Clavien-Dindo system are detailed in Table 2.
The median (IQR) follow-up duration for the survivors was 95 (84–103) months. During the follow-up period 129 patients survived, 229 died of penile cancer, and 63 from other causes. Overall, 258 developed a disease progression during follow-up, either local (penis or groins) or distant. 12 patients had lymphatic progression of the disease during the follow-up, of which 8 patients had progression in the pelvic lymph nodes whilst 4 had progression in the inguinal lymph nodes of the same site where the RILND was performed. The 3-year CSS rate was 86% (95% Confidence Interval [95% CI] 77–96) for the patients with pN1 disease, 83% (95% CI 72–92) for the pN2 patients, and 58% (95% CI 51–66) for those with pN3 disease (p < 0.001), compared to a 3-year CSS of 87% (95% CI 84–95) for the pN0 (Fig. 2).
Discussion
The presence of metastatic disease in the inguinal lymph nodes remains the most important prognostic indicator in penile cancer [6], and RILND is the standard of care in patients with evidence of nodal metastasis [6]. Although the original description of the RILND technique with extensive subfascial dissection removes the entire inguinal lymph node packet to allow oncological control, concerns regarding the high morbidity rate have led to modifications of the technique. These include smaller dissection templates as described by Catalona [13] to the more recent videoendoscopic techniques [14, 15]. The literature available with regard to the morbidity and oncological outcomes associated with RILND remains scarce and of inconsistent quality due to a number of methodological concerns including insufficient numbers, multi-centre collection of the data, heterogeneity of the study designs/inclusion criteria, and lack of standardization in reporting of the outcomes and complications.
We report the surgical technique and outcomes of our technique of RILND which focuses on sparing the Scarpa’s and Camper’s fascia and avoiding dissection deep to the fascia lata. This study has a number of strengths, including the novelty of the surgical approach, the multicentre nature of the study in high-volume supra-regional penile cancer centres, the systematic adoption of DSNB prior to RILND, the strict adherence to guidelines directing to RILND, the accurate data collection and a large patient cohort which makes the present series the largest study on this matter published in the literature. We have also previously demonstrated the nodal mapping of the inguinal nodes to demonstrate that lymphatic drainage to sentinel nodes in the lower quadrants of the original Daseler’s zones is infrequent [16].
Inguinal lymphadenectomy with preservation of the fascia lata has been previously described in the surgical treatment of vulval cancer, in a successful attempt to reduce the morbidity associated with this technique [17]. With the same aim, this approach has been more recently described in penile cancer. Yao et al. [18, 19] first described their variation of the classic RILND approach in 104 patients, introducing the preservation of the fascia lata. Their technique was comparable to our technique with the main difference being that they performed an incision of the cribriform fascia in order to obtain access to the deep inguinal compartment and clear the deeper nodes. Although they documented a very favourable complication rate (e.g., an overall complication rate of 29%) and satisfactory levels of oncological safety, a number of issues of relevance should be considered in order to meaningfully compare their outcomes with the ones presented in this study. First, although the median number of superficial inguinal lymph nodes being removed per groin (e.g., 12.5) was comparable to our findings, the median number of deep inguinal lymph nodes being retrieved was only 2.3 per groin. Moreover, no data were disclosed in the paper regarding the positivity rate of the deep vs. superficial inguinal lymph nodes, raising questions regarding the actual usefulness and benefits of performing this additional surgical step, which may have theoretically introduced further levels of morbidity, in addition to the longer operative times needed to excise these deeper nodes. Second, the indications/selection criteria for their fascial-sparing RILND approach were radically different from the one which we have adopted, as they offered their modified RILND to all of the patients with low-, intermediate- or high-risk of nodal metastasis according to the risk stratification adopted in the EAU guidelines [6] (e.g., with surveillance being proposed as an alternative to RILND only in low-risk patients). Other less invasive means to stage their patients such as FNAC or DSNB were not adopted in their series, whilst we instead performed DSNB before radical lymphadenectomy in every eligible patient with cN0 disease. The patients’ features in terms of nodal positivity rate and N-staging which were identified in their series differed substantially vs. the cohort in the present series (e.g., 22.2% vs. 52.3% of pN2/3 patients, respectively), which most likely reflects the substantially different criteria for inclusion being used in these studies. With this premise in mind, their outcomes in terms of oncological safety and morbidity should be more meaningfully compared instead with those of other series of DSNBs or with the series of modified ILNDs (mILNDs) other than to the RILND series such as the present one.
Similarly, Tsaur et al. [20] described their experience in a smaller (e.g., 29 patients) series of fascial-sparing RILND. Incision of the cribriform fascia to access to deep inguinal lymph nodes was performed in their technique, similarly to Yao et al. [18, 19]. Again there is no mention on the use of nodal staging techniques such as DSNB prior to RILND, and their fascial-sparing RILNDs were defined as therapeutic in case of radiological or clinical suspicion of nodal involvement, and prophylactic in all of the other cases (e.g., 15 and 16 patients, respectively), raising analogous concerns of comparability of their outcomes with our study. Moreover, they did not disclose the pathological N stage of their patients and the analysis of the oncological outcomes was limited to disclosing 4 cases of lymphatic inguinal recurrence, whilst no survival analysis was performed. Their complications’ profile and rate were similar to the ones which we have described.
The majority of the lymphatic tissue in the inguinal area is sited in the superficial lymph node compartment which lies deep to the Camper’s fascia, and above the fascia lata [21]. An internal Audit comprising unpublished data from our department has confirmed a low number (e.g., ranging from 1 to 2) of lymph nodes being excised deeper to the fascia lata, when these deeper lymph nodes needed to be excised. Moreover, a very low positivity rate was identified for those nodes which lie deeper to the fascia lata. Node count is typically considered the most accurate surrogate marker for the quality of the nodal dissection. The median number of the lymph nodes being retrieved in our series of fascial-sparing RILND is satisfactory and comparable with the one reported in prior studies. The oncological outcomes in terms of 3-year survival rates after RILND were also comparable to what was identified in similar RILND series, when stratified for the N-stage.
The complication rate here identified (36.1%) was more favourable as compared to the literature dealing with the classic RLND approach [9, 20, 22, 23], where the complications’ rates typically exceed 50% threshold.
Our study is not devoid of limitations. Firstly, even though the vast majority of the nodal recurrences after RILND are expected to occur within the first two years after surgery, longer follow-up may be needed to assess the risk of late recurrences. Secondly, we acknowledge that the retrospective nature of this study may have introduced biases and a further prospective collection of the data should be needed to more robustly validate this technique. Additionally, the data regarding which patients underwent a saphenous-sparing procedure in this series have not been made available here, thus preventing a better definition of the usefulness of this practice in this context. Finally, the absence of a matched control group treated with the classic RILND prevented comparison of this technique’s oncological and complications’ outcomes with the conventional approach, although historical studies have been used.
The presence of metastatic disease in the inguinal lymph nodes remains the most important prognostic indicator for penile cancer patients. Traditional RILND is associated with a high morbidity rate. We describe the technique and outcomes for fascial-sparing RILND which provides equivalent oncological outcomes with reduced morbidity rates compared to the traditional RILND. Refinements of the current surgical technique and surgical innovation in this field should be continued and further implemented in order to identify the optimal management strategy for patients with nodal metastatic penile cancer.
Data availability
Professor Asif Muneer had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Data are available for bona fide researchers who request it from the authors.
References
Christodoulidou M, Sahdev V, Houssein S, Muneer A (2015) Epidemiology of penile cancer. Curr Probl Cancer. https://doi.org/10.1016/j.currproblcancer.2015.03.010
Fankhauser CD, Ayres BE, Issa A, Albersen M, Watkin N, Muneer A et al (2021) Practice patterns among penile cancer surgeons performing dynamic sentinel lymph node biopsy and radical inguinal lymph node dissection in men with penile cancer: A eUROGEN survey. Eur Urol open Sci 24:39–42. https://doi.org/10.1016/j.euros.2020.12.009
Thomas A, Necchi A, Muneer A, Tobias-Machado M, Tran ATH, Van Rompuy A-S et al (2021) Penile cancer. Nat Rev Dis Prim 7(1):11. https://doi.org/10.1038/s41572-021-00246-5
Cakir OO, Schifano N, Venturino L, Pozzi E, Castiglione F, Alnajjar HM et al (2021) Surgical technique and outcomes following coronal-sparing glans resurfacing for benign and malignant penile lesions. Int J Impot Res. https://doi.org/10.1038/s41443-021-00452-5
Parnham AS, Albersen M, Sahdev V, Christodoulidou M, Nigam R, Malone P et al (2018) Glansectomy and split-thickness skin graft for penile cancer. Eur Urol 73(2):284–289. https://doi.org/10.1016/j.eururo.2016.09.048
Hakenberg S, Compérat OW, Minhas E, Necchi N, Protzel A, Watkin AC, Robinson R (2022) EAU guidelines on Penile Cancer. EAU Guidelines Office, Arnhem, The Netherlands. http://uroweb.org/guidelines/compilations-of-all-guidelines/. Accessed 13 Aug 2023
Daseler EH, Anson BJ, Reimann AF (1948) Radical excision of the inguinal and iliac lymph glands; a study based upon 450 anatomical dissections and upon supportive clinical observations. Surg Gynecol Obstet 87(6):679–694
Johnson DE, Lo RK (1984) Complications of groin dissection in penile cancer. Experience with 101 lymphadenectomies. Urology 24(4):312–314. https://doi.org/10.1016/0090-4295(84)90198-5
Stuiver MM, Djajadiningrat RS, Graafland NM, Vincent AD, Lucas C, Horenblas S (2013) Early wound complications after inguinal lymphadenectomy in penile cancer: a historical cohort study and risk-factor analysis. Eur Urol 64(3):486–492. https://doi.org/10.1016/j.eururo.2013.02.037
Gopman JM, Djajadiningrat RS, Baumgarten AS, Espiritu PN, Horenblas S, Zhu Y et al (2015) Predicting postoperative complications of inguinal lymph node dissection for penile cancer in an international multicentre cohort. BJU Int 116(2):196–201. https://doi.org/10.1111/bju.13009
Amin MB, Greene FL, Edge SB, Compton CC, Gershenwald JE, Brookland RK et al (2017) The eighth edition AJCC cancer staging manual: continuing to build a bridge from a population-based to a more ‘personalized’ approach to cancer staging. CA Cancer J Clin 67(2):93–99. https://doi.org/10.3322/caac.21388
Dindo D, Demartines N, Clavien P-A (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213. https://doi.org/10.1097/01.sla.0000133083.54934.ae
Catalona WJ (1988) Modified inguinal lymphadenectomy for carcinoma of the penis with preservation of saphenous veins: technique and preliminary results. J Urol 140(2):306–310. https://doi.org/10.1016/s0022-5347(17)41589-8
Tobias-Machado M, Tavares A, Molina WRJ, Forseto PHJ, Juliano RV, Wroclawski ER (2006) Video endoscopic inguinal lymphadenectomy (VEIL): minimally invasive resection of inguinal lymph nodes. Int Braz J Urol 32(3):316–321. https://doi.org/10.1590/s1677-55382006000300012
Sotelo R, Sánchez-Salas R, Carmona O, Garcia A, Mariano M, Neiva G et al (2007) Endoscopic lymphadenectomy for penile carcinoma. J Endourol 21(4):364–367. https://doi.org/10.1089/end.2007.9971.discussion367
Omorphos S, Saad Z, Kirkham A, Nigam R, Malone P, Bomanji J et al (2018) Zonal mapping of sentinel lymph nodes in penile cancer patients using fused SPECT/CT imaging and lymphoscintigraphy. Urol Oncol 36(12):530.e1-530.e6. https://doi.org/10.1016/j.urolonc.2018.09.002
Micheletti L, Borgno G, Barbero M, Preti M, Cavanna L, Nicolaci P et al (1990) Deep femoral lymphadenectomy with preservation of the fascia lata. Preliminary report on 42 invasive vulvar carcinomas. J Reprod Med 35(12):1130–1133
Yao K, Tu H, Li Y-H, Qin Z-K, Liu Z-W, Zhou F-J et al (2010) Modified technique of radical inguinal lymphadenectomy for penile carcinoma: morbidity and outcome. J Urol 184(2):546–552. https://doi.org/10.1016/j.juro.2010.03.140
Yao K, Zou Z, Li Z, Zhou F, Qin Z, Liu Z et al (2013) Fascia lata preservation during inguinal lymphadenectomy for penile cancer: rationale and outcome. Urology 82(3):642–647. https://doi.org/10.1016/j.urology.2013.05.021
Tsaur I, Biegel C, Gust K, Huesch T, Borgmann H, Brandt MPJK et al (2015) Feasibility, complications and oncologic results of a limited inguinal lymph node dissection in the management of penile cancer. Int Braz J Urol 41(3):486–495. https://doi.org/10.1590/S1677-5538.IBJU.2014.0304
Micheletti L, Levi AC, Bogliatto F (1998) Anatomosurgical implications derived from an embryological study of the Scarpa’s triangle with particular reference to groin lymphadenectomy. Gynecol Oncol 70(3):358–364. https://doi.org/10.1006/gyno.1998.5073
Hegarty PK, Dinney CP, Pettaway CA (2010) Controversies in ilioinguinal lymphadenectomy. Urol Clin North Am 37(3):421–434. https://doi.org/10.1016/j.ucl.2010.04.005
Koifman L, Hampl D, Koifman N, Vides AJ, Ornellas AA (2013) Radical open inguinal lymphadenectomy for penile carcinoma: surgical technique, early complications and late outcomes. J Urol 190(6):2086–2092. https://doi.org/10.1016/j.juro.2013.06.016
Acknowledgements
Professor Asif Muneer is supported by the NIHR Biomedical Research Centre UCLH.
Funding
This study did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
NS: Data collection, Manuscript writing, Data analysis. GF: Data analysis, Manuscript editing. SR: Data collection. EP: Data collection. JC: Data collection. FC: Data collection. MR: Data collection, Manuscript writing. PH: Data collection, RN: Data collection, Manuscript editing. RR: Data collection, Manuscript editing. VS: Data collection, Manuscript editing. ML: Data collection, Manuscript editing. AP: Data collection, Manuscript editing, Project development. HMA: Data collection, Manuscript editing, Project development. AM: Data collection, Manuscript editing, Project development.
Corresponding author
Ethics declarations
Conflict of interest
This study did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors. No conflict of interest is to be declared.
Ethics approval
This retrospective chart review study involving human participants was in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The surgical procedures were in line with the institutional guidelines and operational policy and approved as part of the MDT process as part of standard management for penile cancer at our institutions.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Schifano, N., Fallara, G., Rezvani, S. et al. Outcomes following radical inguinal lymphadenectomy for penile cancer using a fascial-sparing surgical technique. World J Urol 41, 1581–1588 (2023). https://doi.org/10.1007/s00345-023-04396-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-023-04396-x