Abstract
Aim
The objective of this paper was to discuss the psychological impact of active surveillance (AS) for prostate cancer (PCa) and the resulting implications of psychological wellbeing for treatment decision making and acceptance of AS protocols.
Method
Qualitative and quantitative research in the area of anxiety, depression, and distress is discussed drawing from PCa literature as well other health conditions from which parallels can be drawn.
Results
Attention is given to the role of the clinician in treatment decision making, including the value of information provision, and perceived trust in the AS as a management approach.
Conclusion
Given that research is conflicted regarding the psychological impact of AS for PCa, it is suggested that focus shifts away from debate of the ‘true’ experience of AS rather researchers and clinicians should seek to identify the factors associated with positive and negative psychological response to diagnosis and AS to improve psychological and physical outcomes. Recommendations for clinical practice are discussed.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Active surveillance (AS) is a stratified medicine approach used in the management of low-risk localised prostate cancer. AS involves delaying receipt of curative approaches until disease progression occurs. With increases in global ageing population coupled with the utilisation of screening programmes in western countries, and issues with specificity and sensitivity of Prostate Specific Antigen (PSA) testing, the incidence of low-risk localised PCa is high. AS provides an opportunity to offset the potential damage associated with overdiagnosis and overtreatment of lower risk PCa. The clinical profile of men deemed eligible for AS varies by centre, as does the AS follow-up protocol itself. The generally accepted criteria are men diagnosed with ‘favourable risk’ disease (i.e. Gleason score ≤ 7, PSA < 20 ng/mL and clinical stage T1-T2b [1]). Despite variation in follow-up schedules, AS programmes tend to manage patients with a combination of frequent PSA tests, Digital Rectal Examination (DRE), biopsy, and MRI to detect progression. Often AS is conflated with Watchful Waiting (WW), with studies including patients from both in the same participant group. The nature of WW and AS differ fundamentally in terms of the intent of treatment—with WW offering no opportunity for curative intent based on clinical profile of patients combined with a life expectancy of < 10 years. In contrast, men on an AS pathway should be offered curative therapies should disease progression become evident, the success of this curative therapy is not expected to be adversely affected by the period of time spent on AS [2].
From a medical perspective, the efficacy of AS has been well documented [3] with intention‐to‐treat analysis at a median follow‐up of 10 years from a large scale RCT identifying an overall mortality rate of ~ 1% in localised PCa patients irrespective of allocation to AS or curative treatment conditions [4]. However, the perception of living with untreated cancer can be an additional emotional burden for AS patients [5]. As stated by Bailey and colleagues [6], “The slow-growing and often indolent nature of PCa differentiates this cancer from others and makes it more amenable to AS protocol than more aggressive tumours. However, PCa is still a ‘cancer’, and this word produces fear and substantial uncertainty in diagnosed men.” [6]. These sentiments are reiterated in a number of qualitative studies, with men articulating this burden by describing feelings of uncertainty, feeling afraid, chronic worry [7], and describing a perception of risking one’s life by undergoing AS [8].
Balancing the perceived threat of progression and/or death with a desire to preserve quality of life is not unique to PCa. Therefore, the value of understanding men’s experiences of living with an ‘untreated’ tumour extends beyond PCa and can also be applied to other populations in similar clinical scenarios. Advances in screening technology has led to an increase in the incidence of early-stage and low-risk Ductal Carcinoma in Situ (DCIS) of the breast [9], thyroid cancer [10], and premalignant conditions such as Monoclonal Gammopathy of Unknown Significance (MGUS [11]). This in turn has placed patients newly diagnosed with these early-stage, lower risk conditions in a similar predicament to men diagnosed with favourable-risk PCa, having to manage the uncertainty and perceived risk associated with delaying curative treatment to preserve quality of life (QoL [10]).
Research evidence for the psychological impact of living with AS for PCa is mixed in its conclusions regarding men’s emotional state, with some concluding that men are satisfied with care, feel supported by their clinicians, are confident of their treatment approach, and relieved and grateful to have the opportunity to delay (or avoid) treatment toxicity, while other research concludes that men had not internalised the low-risk nature of their disease, were unsure of monitoring and the ability of their clinicians and the clinical tools’ ability to detect progression, ultimately resulting in a persistent fear of a cancer-related death and a desire to pursue curative treatment despite lack of disease progression [5, 12, 13]. It is difficult to determine the reasons for these stark differences in responses. Some authors suggest that differences can be explained by sociodemographic characteristics of the patient groups and their treating hospitals e.g. education level, health literacy, social support, or personality types [14], some authors offer explanations related to narratives of traditional, stereotypical masculinities [15], others suggest issues inherent to PCa and surveillance itself related to information provision, the clinician-patient relationship, complexities in treatment decision making, and quality of psychosocial support are the issue [16].
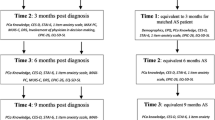
A mixed methods study recruiting participants at their diagnosis/treatment discussion appointment and following up over 9 months in 3 month intervals, found that AS patients’ generalised anxiety symptoms was highest relative to men opting for immediate curative treatments and non-cancer controls in the quantitative phase of the study [17], these findings offer an alternative perception to previous studies conducted in this area [14, 18,19,20]. These differences may be attributable to the setting in which AS research is being conducted. For example, in the Netherlands PRIAS researchers consistently find low anxiety, depression, and uncertainty in their cohort of men undergoing AS [14, 18]. However, this research centre and the clinical setting in which it is associated has been focussed on studying and refining their AS protocol, procedures, and diagnosis experience for decades, arguably leading to a greater acceptance and trust in AS by both patients and clinicians alike. Qualitative research conducted by Seaman and colleagues [21] found that men were content with their decision to undergo AS for PCa, the authors attributed this contentment to high PCa knowledge and understanding of AS in this cohort of participants who described a close relationship with their clinician that was built on trust. These men described a feeling of comfort in regular monitoring and reassurance that this would detect potential PCa progression, therefore findings may not be reflective of those with less PCa knowledge or trust in the AS monitoring process. The qualitative phase of the mixed methods study previously reported [22] conducted 9–12 months post-diagnosis, offered a view that management via AS was a source of anxiety [22]. Men discussed how their AS related anxiety was particularly exacerbated by lack of emotional integration of patient intellectual understanding of PCa and PCa risk (i.e. they could relay information about the low risk nature of their condition, yet continued to discuss their risk of PCa progression and death), lack of trust in their clinician, a desire for more regular monitoring appointments, and, perhaps most importantly, awareness of the schedule and pattern of follow up including the role of each clinician played in managing their care. This finding, taken with those of Seaman et al. [21], clearly demonstrates the importance of the clinical relationship in navigating the experience of a PCa diagnosis and management with AS.
With regard to misperception of risk of PCa disease progression and death, similar patterns of results were found in studies of women with low risk Ductal Carcinoma in Situ (DCIS) of the breast and women with early invasive breast cancer (BCa), this was in spite of vast differences in level of risk between the two groups of women [9]. Study authors state that women have “grossly inaccurate perceptions of their risks of recurrent DCIS or invasive BCa” [9] creating a significant barrier to patients engaging fully in informed decision making. Similarly, findings from qualitative PCa studies [7], women with DCIS did not understand their diagnosis, were unsure of its severity, and were unclear if they were at risk of death [9].
One could be forgiven for assuming that the nature of AS itself is the issue, that positive psychological adjustment is fundamentally incompatible with living with an ‘untreated’ cancer. However, findings from research exploring AS for thyroid cancer do not support this. Due to similarities between PCa and thyroid cancer in terms of increased screening and increased numbers of early stage diagnoses resulting in treatment options of AS or more invasive thyroidectomy, findings from research exploring AS for thyroid cancer offers a useful opportunity to explore the use of AS more generally. Patients eligible for AS for early stage thyroid cancer cite desire to avoid treatment induced side-effects and understanding of the slow growing, low risk nature of the disease as rationale for opting for AS [10]. This concurs with qualitative interviews with PCa patients undergoing AS, however thyroid AS patients appear to respond to AS with less distress and uncertainty. It is possible that this is a result of differences in the demographic profile of thyroid and prostate cancers patients particularly in gender and age, however findings warrant exploring in terms of how decision-making and information provision is supported and delivered while also promoting patient autonomy.
One study that sought to systematically assess decision making for PCa screening in the USA found that the PCa decisions were generally not shared between the patient and clinician due to lack of balance in information provision, limited PCa knowledge, and lack of focus on patient preference [23]. ProtecT, the only large-scale trial to randomise PCa patients to curative treatment or an adapted form of AS (referred to as active monitoring in the trial), offers a unique opportunity to explore information provision and how this contributes to men’s acceptance of randomisation but also has implications for delivering treatment related information in broader clinical settings [24]. Donovan [24] described the procedure for relaying treatment and trial information to potential participants; trained participant recruiters were instructed to illicit men’s preferences on available treatments and to explore men’s reasons for these preferences before providing details about the various treatments and the ProtecT trial more broadly. The basic premise of these discussions was that patients’ views about their treatment should always be acknowledged and respected, however all patients regardless of how well-informed they may be regarding their treatment options should be provided with information about all treatment options. Donovan [24] flags this as particularly important for clinical practice for individuals eligible for AS, due to less mainstream understanding of monitoring approaches to cancer and public fears of cancer that reinforces a sense of urgency to immediately opt for and commence curative treatment. However, findings from ProtecT demonstrate that surgeons and oncologists inadvertently create an additional barrier to AS with their own personal preferences for treatments and difficulties in presenting AS as an option equal to that of more traditional, curative treatments [24,25,26,27,28]. Given these findings, addressing the issue of patient distrust of AS is potentially premature, when clinicians themselves appear to struggle to present AS as an option equal to surgery or radiation.
Based on findings from mixed methods study [29] and supported by previous literature, recommendations for clinical practice have been identified. First, personal priorities of the patient must remain central to discussing treatment options, this may take the form of a structured conversation between clinician and patient, or including psychological screening when patient presents to clinician. This is supported by lessons learned from the ProtecT trial [24]. Second, clinicians should be aware that favourable prognosis may not necessarily equate to favourable psychological response to diagnosis and treatment. Patients with the ‘best’ prognosis (i.e. Gleason 6 PCa) should be treated with the same sensitivity as those presenting with higher risk PCa. Similar issues in terms of misperception of risk have been identified in studies comparing patients diagnosed with DCIS of the breast and early stage invasive BCa [9]. Clinicians should not assume that patients can integrate intellectual knowledge of low-risk status to override the emotional reaction to a cancer diagnosis. Third, improved clarity and communication of AS protocol is needed. Patients interviewed were uncertain regarding appointment schedules and the clinician responsible for the various aspects of their care (e.g. PSA testing with GP, monitoring with CNS, annual/biannual biopsy with Consultant Urologist) [22]. Fourth, and finally, also in qualitative interviews [22], AS patients suggested that the diagnosis experience could be enhanced with a written summary of their diagnosis following consultation with their clinician. This would allow them to communicate their diagnosis to their friends/family with greater ease and could compensate for feeling overwhelmed with information during consultation appointment resulting in difficulty recalling important diagnosis and treatment information.
References
National Institute for Clinical Excellence N: Prostate cancer: diagnosis and management NICE guideline [NG131]. . https://www.nice.org.uk/guidance/ng131 (2019). Accessed 24 Sept 2020
National Institute for Clinical Excellence N: Prostate cancer: diagnosis and treatment (CG175). http://www.nice.org.uk/guidance/CG175 (2014). Accessed 24 Sept 2020
Culp MB, Soerjomataram I, Efstathiou JA, Bray F, Jemal A (2020) Recent global patterns in prostate cancer incidence and mortality rates. Eur Urol 77(1):38–52
Hamdy FC, Donovan JL, Lane J, Mason M, Metcalfe C, Holding P et al (2016) 10-year outcomes after monitoring, surgery, or radiotherapy for localized prostate cancer. N Engl J Med 375:1415–1424
McIntosh M, Opozda MJ, Evans H, Finlay A, Galvão DA, Chambers SK et al (2019) A systematic review of the unmet supportive care needs of men on active surveillance for prostate cancer. Psycho-oncology 28(12):2307–2322
Bailey DE Jr, Wallace M, Mishel MH (2007) Watching, waiting and uncertainty in prostate cancer. J Clin Nurs 16(4):734–741
Hedestig O, Sandman P-O, Widmark A (2003) Living with untreated localized prostate cancer: a qualitative analysis of patient narratives. Cancer Nurs 26(1):55–60
Kazer MW (2012) Conversion from active surveillance to active treatment for prostate cancer: a qualitative analysis. J Nurs Educ Pract 2(2):80
Partridge A, Adloff K, Blood E, Dees EC, Kaelin C, Golshan M et al (2008) Risk perceptions and psychosocial outcomes of women with ductal carcinoma in situ: longitudinal results from a cohort study. J Natl Cancer Inst 100(4):243–251
D’Agostino TA, Shuk E, Maloney EK, Zeuren R, Tuttle RM, Bylund CL (2018) Treatment decision making in early-stage papillary thyroid cancer. Psycho-oncology 27(1):61–68
McShane CM, Murphy B, Lim KH, Anderson LA (2018) Monoclonal gammopathy of undetermined significance as viewed by haematology healthcare professionals. Eur J Haematol 100(1):20–26
Ruane-McAteer E, Porter S, O’Sullivan JM, Santin O, Prue G (2017) Active surveillance for favorable-risk prostate cancer: Is there a greater psychological impact than previously thought? A systematic, mixed studies literature review. Psycho-oncology 26(10):1411–1421
Kinsella N, Stattin P, Cahill D, Brown C, Bill-Axelson A, Bratt O et al (2018) Factors influencing men’s choice of and adherence to active surveillance for low-risk prostate cancer: a mixed-method systematic review. Eur Urol 74(3):261–280
van den Bergh RC, Essink-Bot ML, Roobol MJ, Wolters T, Schröder FH, Bangma CH et al (2009) Anxiety and distress during active surveillance for early prostate cancer. Cancer Interdiscip Int J Am Cancer Soc 115(17):3868–3878
Chapple A, Ziebland S (2002) Prostate cancer: embodied experience and perceptions of masculinity. Soc Health Illn 24(6):820–841
Davison BJ, Breckon E (2012) Factors influencing treatment decision making and information preferences of prostate cancer patients on active surveillance. Patient Educ Couns 87(3):369–374
Ruane-McAteer E, Porter S, O’Sullivan J, Dempster M, Prue G (2019) Investigating the psychological impact of active surveillance or active treatment in newly diagnosed favorable-risk prostate cancer patients: a 9-month longitudinal study. Psycho-oncology 28(8):1743–1752
Venderbos L, Roobol M, Bangma C, Korfage I (2015) Five-year follow-up after active surveillance or curative treatment: preliminary quality of life outcomes of men with prostate cancer. Qual Life Res springer van godewijckstraat 30, 3311 gz dordrecht, netherlands. p. 30
Couper JW, Love AW, Dunai JV, Duchesne GM, Bloch S, Costello AJ et al (2009) The psychological aftermath of prostate cancer treatment choices: a comparison of depression, anxiety and quality of life outcomes over the 12 months following diagnosis. Med J Aust 190:S86–S89
Parker PA, Davis JW, Latini DM, Baum G, Wang X, Ward JF et al (2016) Relationship between illness uncertainty, anxiety, fear of progression and quality of life in men with favourable-risk prostate cancer undergoing active surveillance. BJU Int 117(3):469–477
Seaman AT, Taylor KL, Davis K, Nepple KG, Lynch JH, Oberle AD et al (2019) Why men with a low-risk prostate cancer select and stay on active surveillance: a qualitative study. PLoS ONE 14(11):e0225134
Ruane-McAteer E, Porter S, O’Sullivan JM, Prue G (2018) A cognitive-emotional see-saw: Men’s experiences of undergoing active surveillance for prostate cancer. Psycho-oncology: Wiley 111 River st, Hoboken 07030–5774, NJ USA. p. 170
Hoffman RM, Couper MP, Zikmund-Fisher BJ, Levin CA, McNaughton-Collins M, Helitzer DL et al (2009) Prostate cancer screening decisions: results from the National Survey of Medical Decisions (DECISIONS study). Arch Intern Med 169(17):1611–1618
Donovan JL (2012) Presenting treatment options to men with clinically localized prostate cancer: the acceptability of active surveillance/monitoring. J Natl Cancer Inst Monogr 2012(45):191–196
Fowler FJ Jr, Collins MM, Albertsen PC, Zietman A, Elliott DB, Barry MJ (2000) Comparison of recommendations by urologists and radiation oncologists for treatment of clinically localized prostate cancer. JAMA 283(24):3217–3222
Hanna C, Mason M, Donovan J, Barber J (2002) Clinical oncologists favour radical radiotherapy for localized prostate cancer: a questionnaire survey. BJU Int 90(6):558–560
Mills N, Donovan JL, Wade J, Hamdy FC, Neal DE, Lane JA (2011) Exploring treatment preferences facilitated recruitment to randomized controlled trials. J Clin Epidemiol 64(10):1127–1136
Wade J, Donovan JL, Lane JA, Neal DE, Hamdy FC (2009) It’s not just what you say, it’s also how you say it: opening the ‘black box’of informed consent appointments in randomised controlled trials. Soc Sci Med 68(11):2018–2028
Ruane-McAteer E (2017) Exploring the psychological impact of active surveillance for favourable-risk prostate cancer: a mixed methods study. Queen’s University Belfast, Belfast
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
ER-M and GP contributed equally to protocol/project development, data collection and management, data analysis, and manuscript writing/editing.
Corresponding author
Ethics declarations
Conflict of interest
No conflicts of interests/competing interests to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ruane-McAteer, E., Prue, G. Psychological aspects of active surveillance. World J Urol 40, 9–13 (2022). https://doi.org/10.1007/s00345-020-03553-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-020-03553-w