Abstract
Purpose
To identify the perioperative and oncological impact of different intervals between biopsy and robot-assisted laparoscopic radical prostatectomy (RALP) for localized prostate cancer.
Methods
All consecutive patients with localized prostate cancer who underwent RALP with primary curative intent in January 2008–July 2014 in a large tertiary hospital were enrolled in this retrospective cohort study. The patients were divided into groups according to whether the biopsy–RALP interval was ≤2, ≤4, ≤6, or >6 weeks. Estimated blood loss and operating room time were surrogates for surgical difficulty. Surgical margin status and continence at the 1 year were surrogates for surgical efficacy. Biochemical recurrence (BCR) was defined as two consecutive postoperative prostate serum antigen values of ≥0.2 ng/ml.
Results
Of the 1446 enrolled patients, the biopsy–RALP interval was ≤2, ≤4, ≤6, and >6 weeks in 145 (10 %), 728 (50.3 %), 1124 (77.7 %), and 322 (22.3 %) patients, respectively. The >6 week group had a significantly longer mean operation time than the ≤2, ≤4, and ≤6 week groups. The groups did not differ significantly in terms of estimated blood loss or surgical margin status. Kaplan–Meier analysis showed that interval did not significantly affect postoperative BCR-free survival. Multivariable Cox proportional hazards model analysis showed that interval duration was not an independent predictor of BCR (≤2 vs. >2 weeks, HR = 0.859, p = 0.474; ≤4 vs. >4 weeks, HR = 1.029, p = 0.842; ≤6 vs. >6 weeks, HR = 0.84, p = 0.368).
Conclusion
Performing RALP within 2, 4, or 6 weeks of biopsy does not appear to adversely influence surgical difficulty or efficacy or oncological outcomes.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Prostate cancer (PCa) has become a common disease worldwide due to medical developments and the resulting increase in the elderly population. In particular, prostate serum antigen (PSA) screening and advances in imaging technologies have greatly accelerated the diagnosis of PCa at an early stage. Moreover, ever since robot-assisted laparoscopic radical prostatectomy (RALP) was introduced, the number of prostatectomies has increased markedly [1, 2]. RALP is a valuable therapeutic option for clinically localized PCa as its oncological and functional outcomes are at least as good as those provided by open or laparoscopic techniques; it also associates with a low risk of complications [3, 4].
Previously, it was generally agreed that there should be 4–6 weeks between a prostate biopsy and retropubic radical prostatectomy (RRP) for PCa [5, 6]. This concept was supported by imaging studies (such as with endorectal magnetic resonance imaging) that showed that biopsy-related changes in the prostate that could hamper RRP (e.g., periprostatic inflammation and hematoma) can last up to 21 days and in some cases up to 4.5 months [7–9]. However, this concept may no longer apply in the era of robotic surgery because RALP has several advantages over the open method, including high magnification of the operative field, precise dissection movements, and low blood loss. Nevertheless, there are at present insufficient data to determine the optimal minimum interval between biopsy and RALP in terms of ease and efficacy of surgery and oncological outcomes.
We hypothesized that the interval between biopsy and RALP does not affect either perioperative or oncological outcomes. To test this, we performed the present retrospective cohort study. The primary outcome was the relationship between interval from biopsy to RALP and perioperative outcomes. The secondary outcome was the association between interval from biopsy to RALP and oncological outcomes.
Materials and methods
Study cohort
This retrospective cohort study was approved by the institutional review board of our tertiary hospital (Seoul National University Bundang Hospital) in Gyeonggi-do Province, South Korea. The need for informed consent from the patients was waived due to the retrospective nature of the study. All consecutive patients with localized PCa who underwent RALP with primary curative intent between January 2008 and July 2014 were identified by searching the institutional database. Patients were excluded if they had advanced-stage PCa, a history of radiotherapy, a history of other pelvic surgery, a history of adjuvant chemotherapy, or missing clinical, operative, and pathological data. Our cohort was based on previous studies which assessed operative efficacy according to interval from biopsy to prostatectomy as following: interval of four or six weeks between biopsy and prostatectomy based on a study which assessed operative efficacy in RP [10], and interval of 2 weeks between biopsy and prostatectomy based on a study which assessed operative efficacy in RALP [11]. Every patient who underwent prostatic biopsy was given oral quinolone before and after biopsy and injected IV cefa group antibiotics at peribiopsy period. This cohort is not consisted of the experience of single surgeon. However, all surgeons who were included in this study already overcame the learning curve. Our hospital is one of the largest tertiary hospitals in Korea. Only in 2015 and only in Department of Urology, we performed robotic surgery 550 cases.
Outcomes
The patients were stratified according to the National Comprehensive Cancer Network (NCCN) risk groups [12]. The anesthesiologist-reported estimated blood loss (EBL), intraoperative transfusion rate, surgeon-reported operation time, and nerve-sparing status served as surrogates of surgical difficulty. Positive surgical margin (PSM) status and continence at the first year served as surrogates for surgical efficacy. The nerve-sparing (NS) status was scored as none, unilateral, and bilateral preserved. We decide to perform NS using risk grouping and multi-parameter MRI. We sometimes perform frozen biopsy to clarify margin status, but not to decide for NS. Postoperative continence was assessed on the basis of the use of continence pads: Continence was defined as the use of no pads. Biochemical recurrence (BCR) was defined when the PSA value was ≥0.2 ng/ml on two consecutive measurements after RALP [13].
Statistics
The patients were divided into groups according to whether the interval between biopsy and RALP was ≤2, ≤4, ≤6, or >6 weeks. Thus, the ≤4 week group contained the ≤2 week group and the ≤6 week group contained the ≤4 week group. The differences between these groups in terms of preoperative clinicopathological variables, surgical difficulty variables, and surgical efficacy variables were assessed using the Chi-squared test and Student’s t test. The differences between the interval groups in terms of postoperative BCR-free survival were assessed using Kaplan–Meier analysis followed by log-rank test. Cox univariable and multivariable regression models were used to identify the relationship between the biopsy–RALP interval and BCR. The data were expressed as hazard ratios (HR). Logistic regression analysis was performed to assess the association of each clinical variable with NS in low-risk group. All statistical analyses were performed using SPSS 22.0 for Windows (IBM® SPSS® version 22.0, IBM, Armonk, New York, USA). p values of <0.05 were considered to indicate statistical significance.
Results
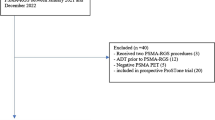
In total, 1455 men with localized PCa underwent RALP with primary curative intent during the study period. Of these, nine were excluded because they were performed previous transurethral prostatectomy (TURP) (n = 7) and holmium laser enucleation of prostate (HoLEP) (n = 1), and missing clinical, operative, and pathological data (n = 1). Thus, the final study cohort consisted of 1446 patients.
The preoperative characteristics of the study cohort are shown in Table 1. In 145 (10 %), 728 (50.3 %), 1124 (77.7 %), and 322 (22.3 %) patients, the interval between biopsy and RALP was ≤2, ≤4, ≤6, and >6 weeks, respectively. For the ≤2, ≤4, ≤6, and >6 week groups, the median time to RALP was 1.6 (interquartile range 1.3–1.9) weeks, 2.7 (interquartile range 2–3.4) weeks, 3.6 (interquartile range 2.4–4.7) weeks, and 7.9 (interquartile range 6.9–10.4) weeks, respectively. The four groups did not differ significantly in terms of preoperative age, body mass index, prostate volume, clinical stage, PSA level, or biopsy results (including positive number and maximal involvement), biopsy Gleason score, and frequency of NCCN risk groups.
Analysis of the perioperative variables that represented surgical difficulty revealed that the >6 week group had a significantly longer mean operation time than the ≤2, ≤4, and ≤6 week groups (Table 2). The four groups did not differ significantly in terms of other perioperative outcomes, namely EBL, transfusion rate, and nerve-sparing status.
Analysis of the variables that represented surgical efficacy revealed that the four groups did not differ significantly in terms of PSM status and continence at 1 year (Table 3).
Kaplan–Meier analysis of postoperative BCR-free survival showed that the ≤2 week group did not differ from the >2 week group (log-rank test, p = 0.395) (Fig. 1). The ≤4 week group also did not differ from the >4 week group in terms of BCR-free survival (log-rank test, p = 0.671) (Fig. 2). A difference between the ≤6 week group and the >6 week group in BCR survival was also not detected (log-rank test, p = 0.155) (Fig. 3).
Multivariate Cox proportional modeling that included age, body mass index, PSA level, prostate volume, clinical stage, biopsy Gleason score, positive core number, maximal core involvement, and the interval between biopsy and RALP showed that the interval between biopsy and RALP was not an independent predictor of BCR (2 weeks, HR = 0.859, p = 0.474; 4 weeks, HR = 1.029, p = 0.842; 6 weeks, HR = 0.84, p = 0.368) (Table 4).
In logistic regression analysis, maximal core involvement showed the association with NS. And interval with 2 weeks from biopsy was observed the relationship with NS in low-risk group (Table 5).
Discussion
During the era of RRP, it was generally considered that delaying surgery for at least 4–6 weeks was prudent. The argument was that the biopsy could induce changes in the prostate (inflammation and hemorrhage) that could adversely influence the facility, efficacy, and oncological efficacy of the procedure [10, 14, 15]. This recommendation continued to be followed despite the technological advances that yielded RALP, which involves better vision and more precise movements. The present study shows that this recommendation may not be evidence-based medicine as we could not detect any adverse effects of performing RALP even less than 2 weeks after biopsy. Indeed, the only significant effect of biopsy–RALP duration that we observed was that surgery late after biopsy (after 6 weeks) associated with an increased operative time. Our clinical experience suggests that this may reflect dissection difficulties that are due to the healing of the prostate or an inflammatory reaction to the biopsy. Thus, the guideline to delay surgery may no longer be appropriate in the robotic prostatectomy era.
Several other lines of evidence also suggest that the caution regarding when to perform even open radical prostatectomy may have been unnecessary. First, although the magnetic resonance imaging study of Park et al. [16] showed that hemorrhages were observed for up to 57 days after biopsy, we did not find that the different biopsy–RALP intervals associated with significant differences in EBL, which can be considered to be a surrogate of post-biopsy hemorrhage. Second, Eggener et al. [10] showed that, regardless of whether the interval from biopsy to open radical prostatectomy was ≤4 or ≤6 weeks, it did not affect operative duration, EBL, PSM status, continence, or erectile function. Similarly, the study of Lee et al. [17] found that the patients who underwent RRP before and after 2 weeks after biopsy (the median duration after biopsy for the cohort) did not differ in terms of operative time, EBL, transfusion rate, hospitalization duration, nerve-sparing status, PSM status, and continence. Thus, neither study could identify an optimal interval between biopsy and open radical prostatectomy. The over 6 weeks group might be much processed inflammatory than ≤2, ≤4, ≤6 weeks group.
Our study on RALP showed that it was feasible, oncologically effective, and safe even when the surgery was performed less than 2 weeks after biopsy. Two studies in 2011 also suggested that it is unnecessary to delay RALP after biopsy [11, 18]. The retrospective cohort study of Kim et al. with 237 patients showed that biopsy–RALP intervals of ≤2, >2–≤4, >4–≤6, >6–≤8, and >8 weeks had no effect on operative time, EBL, PSM rate, continence, and potency [18]. Similarly, the prospective clinical trial of Lee et al., where 104 patients were allocated to undergo RALP 2, 2–4, or >4 weeks after biopsy, showed that the biopsy–surgery interval did not influence operative time, PSM rate, continence, or potency [11]. The present large-scale study (1446 patients) confirms and extends these findings.
There is no reason to delay either robotic or open prostatectomy. However, there is the debate of limitation of period from biopsy to prostatectomy in the era of open prostatectomy. This observation may reflect the numerous advantages of RALP over open radical prostatectomy, as follows. First, the operative field is magnified during robot surgery. Second, it allows for delicate movements that promote precise dissection. Third, it is a minimally invasive technique that leads to a relatively rapid recovery after surgery. Therefore, we suggested the evidence of no need for delay in the era of robotic surgery.
Our study suggests that RALP does not have to be performed after a specific period. This notion is supported by several studies that show that a delay from biopsy to prostatectomy does not affect postoperative disease progression [19–21]. The prospective clinical trial of Lee et al. described above also showed that the biopsy–RALP interval does not affect the risk of BCR (pp = 0.1484). This is clinically useful information because, although a delay may be useful for some patients as they decide between the various treatment options for clinically localized PCa, other patients may desire surgery quickly due to anxiety after learning their diagnosis. There are some patients to eliminate cancer in their body as soon as possible in spite of fully informed consent. In real clinical setting, some patients worried more than their situation and they found other physicians to be operated. Nowadays, active surveillance (AS) emerged as a treatment option of low-risk PCa. Even AS patients want to be operated as soon as possible despite proper explanation. We suggest the evidence of no need for delay in the era of robotic surgery. As such, this evidence will provide the guideline for establishing the timing of prostatectomy in the era of robotic surgery.
In summary, our results show that the recommendation to wait 4–6 weeks after biopsy is no longer pertinent in the era of robotic surgery and that the patients who are eligible for such surgery can choose, after counseling with a urologist, when to undergo it.
This study has a number of limitations. First, it was performed retrospectively and thus may be subject to selection and information bias. Second, we did not investigate the effect of biopsy–surgery interval on postoperative erectile function. We did not analyze the postoperative potency comparing with preoperative potency. Therefore, we could not the accurate success of nerve sparing. We analyzed only whether performing nerve sparing or not. Third, we did not investigate the preoperative continence status. Fourth, we used continence status as a surrogate of postoperative functional outcome. Fifth, the study was performed in only one institution. However, our cohort is relatively large and our institution is a representative tertiary center. Sixth, we did not performed analysis according to the number of biopsy. There is a potential risk of bias due to the number of biopsy. However, almost all patients of our cohort were performed a single biopsy. Finally, there is no criterion for the degree of difficulty during operation. Therefore, we adapt operative time as surrogate marker as the degree of difficulty during operation. To determine the optimal interval between biopsy and RALP, a large-scale multi-institutional randomized clinical trial is needed.
Conclusion
RALP that is performed less than 4–6 weeks after prostate biopsy does not appear to be more technically difficult and does not influence the surgeon’s ability to obtain negative surgical margins or affect urinary function. Our data indicate that there is no reason to delay surgery after prostate biopsy in the era of robotic surgery. This may reassure urologists and patients who choose RALP relatively soon after biopsy.
References
Hu JC, Gu X, Lipsitz SR, Barry MJ, D’Amico AV, Weinberg AC, Keating NL (2009) Comparative effectiveness of minimally invasive vs open radical prostatectomy. JAMA 302:1557–1564
Trinh QD, Sammon J, Sun M, Ravi P, Ghani KR, Bianchi M, Jeong W, Shariat SF, Hansen J, Schmitges J, Jeldres C, Rogers CG, Peabody JO, Montorsi F, Menon M, Karakiewicz PI (2012) Perioperative outcomes of robot-assisted radical prostatectomy compared with open radical prostatectomy: results from the nationwide inpatient sample. Eur Urol 61:679–685
Montorsi F, Wilson TG, Rosen RC et al (2012) Pasadena Consensus Panel. Best practices in robot-assisted radical prostatectomy: recommendations of the Pasadena Consensus Panel. Eur Urol 62:368–381
Lim SK, Kim KH, Shin TY, Rha KH (2013) Current status of robot-assisted laparoscopic radical prostatectomy: how does it compare with other surgical approaches? Int J Urol 20:271–284
Sokoloff MH, Brendler CB (2001) Indications and contraindications for nerve-sparing radical prostatectomy. Urol Clin North Am 28:535–543
Walsh PC (2002) Radical prostatectomy. In: Walsh PC, Retik AB, Darracott Vaughan E Jr, Wein AJ (eds) Campbell’s Urology, vol 8. WB Saunders, Philadelphia, pp 3107–3129
White S, Hricak H, Forstner R et al (1995) Prostate cancer: effect of post biopsy hemorrhage on interpretation of MR images. Radiology 195:385–390
Ikonen S, Kivisaari L, Vehmas T et al (2001) Optimal timing of post-biopsy MR imaging of the prostate. Acta Radiol 42:70–73
Kaji Y, Kurhanewicz J, Hricak H et al (1998) Localizing prostate cancer in the presence of post biopsy changes on MR images: role of proton MR spectroscopic imaging. Radiology 206:785–790
Eggener SE, Yossepowitch O, Serio AM, Vickers AJ, Scardino PT, Eastham JA (2007) Radical prostatectomy shortly after prostate biopsy does not affect operative difficulty efficacy. Urology 69:1128–1133
Lee SH, Chung MS, Chung YG, Park KK, Chung BH (2011) Does performance of robot-assisted laparoscopic radical prostatectomy within 2 weeks of prostate biopsy affect the outcome? Int J Urol 18(2):141–146. doi:10.1111/j.1442-2042.2010.02675.x Epub 2010 Nov 16
NCCN (2013) Clinical practice guidelines in oncology (NCCN Guideline®). prostate cancer v4.2013. http://www.nccn.org/professionals/physician_gls/pdf/prostate.pdf
Abdollah F, Karnes RJ, Suardi N et al (2014) Predicting survival of patients with node-positive prostate cancer following multimodal treatment. Eur Urol 65:554–562
Pettus JA, Masterson T, Sokol A et al (2009) Prostate size is associated with surgical difficulty but not functional outcome at 1 year after radical prostatectomy. J Urol 182:949–955
Walsh PC, Partin AW (2007) Anatomic radical retropubic prostatectomy. In: Wein AJ, Kavoussi LR, Novick AC, Partin AW, Peters CA (eds) Campbell-Walsh urology, 9th edn. WB Saunders, Philadelphia, pp 2959–2978
Park KK, Lee SH, Lim BJ, Kim JH, Chung BH (2010) The effects of the period between biopsy and diffusion-weighted magnetic resonance imaging on cancer staging in localized prostate cancer. BJU Int (forthcoming)
Lee DK, Allareddy V, O’Donnell MA, Williams RD, Konety BR (2006) Does the interval between prostate biopsy and radical prostatectomy affect the immediate postoperative outcome? BJU Int 97:48–50
Kim IS, Na W, Nam JS, Oh JJ, Jeong CW, Hong SK, Byun SS, Lee SE (2011) Interval from prostate biopsy to robot-assisted laparoscopic radical prostatectomy (RALP): effects on surgical difficulties. Korean J Urol 52(10):664–668. doi:10.4111/kju.2011.52.10.664 (Epub 2011 Oct 19)
Boorjian SA, Bianco FJ Jr, Scardino PT et al (2005) Does the time from biopsy to surgery affect biochemical recurrence after radical prostatectomy? BJU Int 96:773–776
Khan MA, Mangold LA, Epstein JI et al (2004) Impact of surgical delay on long-term cancer control for clinically localized prostate cancer. J Urol 172(5 Pt 1):1835–1839
Nam RK, Jewett MA, Krahn MD et al (2003) Delay in surgical therapy for clinically localized prostate cancer and biochemical recurrence after radical prostatectomy. Can J Urol 10:1891–1898
Authors’ contribution
Jung Ki Jo developed the protocol/project, analyzed the data, and wrote the manuscript. Jong Jin Oh collected and managed the data. Sangchul Lee and Seong Jin Jeong analyzed the data. Sung Kyu Hong edited the manuscript. Seok-Soo Byun collected and managed the data, and edited the manuscript. Sang Eun Lee developed the protocol/project and edited the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There are no conflicts of interest relevant to this article.
Ethical statement
This study was approved by Bundang Hospital institutional review board. Jung ki Jo and Sang Eun Lee participated in the project development. Jong Jin Oh and Seok-Soo Byun conducted data collection and management. Jung Ki Jo, Sangchul Lee and Seong Jin Jeong conducted data analysis. Jung Ki Jo conducted manuscript writing. Sung Kyu Hong, Seok-Soo Byun and Sang Eun Lee participated in manuscript editing. Our paper was proofread by Bioedit (www.bioedit.com).
Rights and permissions
About this article
Cite this article
Jo, J.K., Oh, J.J., Lee, S. et al. Can robot-assisted laparoscopic radical prostatectomy (RALP) be performed very soon after biopsy?. World J Urol 35, 605–612 (2017). https://doi.org/10.1007/s00345-016-1893-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-016-1893-4