Abstract
Purpose
The present study aims to establish a method that provides fast, precise and reproducible pharmacokinetic (PK) parameters of antibody-calicheamicin conjugates. The method should discriminate between PK of the antibody moiety and PK of the conjugated calicheamicin (CM).
Methods
The conjugates gemtuzumab ozogamicin (CMA-676, Mylotarg®) or inotuzumab ozogamicin (CMC-544) were injected in the tail vein of nude mice. At regular time intervals, 5 μl whole blood samples were taken from the tail artery. Concentrations of conjugated CMA-676 or CMC-544 as well as concentrations of their respective antibody moiety were determined by sandwich plasmon resonance. This detection system measures changes in the plasma resonance angle caused by the interaction of macromolecules on biosensor chips. We determined as a first measure the binding of CMA-676 or CMC-544 to their respective antigens, CD33 or CD22. As a second measure we determined the amount of CM on the antigen-bound conjugates. This was done by determination of changes in plasma resonance angle after binding of an anti-CM antibody.
Results
Sandwich plasmon resonance allowed detection of both conjugates in blood of mice in a range of 100–1,000 ng/ml protein. Due to the precision of the sampling and detection methods, PK values of each conjugate were determined in individual mice. Calicheamicin bound to antibody was eliminated faster than the antibody alone. The presence of a CD22-expressing tumour in mice reduced the plasma levels of the CD22-targeting conjugate but not of the CD33-targeting one.
Conclusions
Using small blood samples from a mouse, the sandwich plasmon resonance method provided PK-values of CM-conjugates and information about the stability of the linkage in vivo. Comparison between the PK-values of CM-conjugates in tumour-bearing and tumour-free mice suggested that retention of the conjugate in tumour tissue due to antigen targeting could be deduced from the plasma levels.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Synthetic and natural macromolecules have become established therapeutics in cancer treatment. Antibodies in particular have proven clinical efficacy not only as naked antibody (e.g. rituximab, [1]) but also as conjugates to radioisotopes (e.g. ibritumomab tiuxetan, [2]) or cytotoxic chemotherapeutic agents (gemtuzumab ozogamicin, [3]). The validity of this approach has justified extensive research (for a review see [4]) into expansion of its application range. Obviously, the generation of antibodies against various tumour-associated antigens (TAA) was a first step in achieving this objective. However, to date we have no complete appreciation of the physiological characteristics required from an antibody or an antibody conjugate to obtain the most favourable therapeutic index in the clinic. Simple biochemical characteristics (e.g. the affinity of antibody for its antigen) of the molecule may not necessarily give the required insight to predict improved efficacy, although intuitively one would presume that enhanced affinity of the antibody would translate into enhanced efficacy. Recent reports [5] argue against the general validity of this presumption. Biological parameters in vivo such as circulation half-life, tissue distribution rates of antibodies and conjugates as well as speed of degradation of conjugates are possibly more helpful in comparing the potential therapeutic efficacy of these molecules. Unfortunately, the pragmatic and logistic challenges of preclinical experiments designed to assess these pharmacokinetic parameters do not allow for a convenient comparison of these parameters among multiple immunoconjugates. Measurement of radiolabelled conjugate and determination of the amount of naked or conjugated antibody by means of radioimmunoassays (RIAs) or Enzyme Linked Immuno Sorbent Assays (ELISA) are the most commonly used methods to monitor the presence of immunoglobulins in plasma. Radiolabelling of immunoconjugates poses several logistic problems associated with the use of radioisotopes. Especially when mice are used, the sample size required for accurate determination of the concentration of immunoglobins by these methods is often too large to allow multiple samples to be taken over time in the same animal. To resolve some of these issues, we developed an assay for detection of intraperitoneally or intravenously administered immunoconjugates of calicheamicin and a concomitant method for the accurate and direct sampling of 5 μl peripheral mouse blood. The amount of antibody or antibody conjugated to calicheamicin was determined by means of a ‘sandwich’ plasmon resonance method. This analytical method relies on the measurement of changes in the plasma resonance angle caused by the interaction of macromolecules on biosensor chips [6, 7]. The presented data show that the method can reproducibly determine the concentration of an anti-CD33 (gemtuzumab ozogamicin, [3]) and an anti-CD22 (inotuzumab ozogamicin, [8]) calicheamicin conjugate in the plasma of mice. We also showed that the concentration of total and conjugated antibody could be monitored in individual mice allowing the calculation of pharmacokinetic parameters (plasma half-life, area under the curve, clearance, volume of distribution) in each animal. Furthermore, the influence of expression of TAA by subcutaneous tumours on the plasma levels of a conjugate was evaluated.
Materials and methods
Cell line and culturing conditions
The Ramos cell line (CRL-1923) was obtained from the American Type Culture Collection (ATCC). Ramos is a CD22+, CD33− cell line derived from a human B-cell lymphoma. The cells were maintained in suspension cultures in RPMI1640 supplemented with 10 mM HEPES, 1 mM sodium pyruvate, 0.2 % (w/v) glucose, 100 U/ml penicillin G sodium, 100 μg/ml streptomycin sulphate and 10% (v/v) fetal bovine serum.
Antigens, antibodies and conjugates
RaCM is a rabbit polyclonal antibody against calicheamicin. The antibody was isolated from rabbits that were immunized with Keyhole Limpet Haemocyanin (KLH) linked to N-acetyl gamma calicheamicin dimethyl amide with the acid stabile (4-mercapto-4-methyl-pentanoic acid) Amide linker (Wyeth, Pearl River, NY, USA).
Gemtuzumab ozogamicin and inotuzumab ozogamicin are calicheamicin conjugates of the anti-CD33 and anti-CD22 antibodies, hP67.6 and G5/44, respectively. Gemtuzumab ozogamicin is the generic name for the marketed drug Mylotarg® (Wyeth, Madison, NJ, USA) and is also referred to as CMA-676 and hP67.6-AcBut-CalichDMH [9]. The calicheamicin conjugate, inotuzumab ozogamicin (Wyeth), is currently in phase I/II clinical trials. Alternative names of this immunoconjugate are CMC-544 and G5/44-AcBut-CalichDMH [9]. We will refer hereafter to the conjugates as CMA-676 and CMC-544. To obtain these conjugates, hP67.6 and G5/44 were linked to N-acetyl gamma calichemicin dimethyl hydrazide with the acid labile (4-(4′ acetylphenoxy)butanoic acid (AcBut) linker. For our studies we used CMA-676 with a loading of 35 μg calicheamicin per mg hP76.6. CMC-544 had 73 μg calicheamicin conjugated to 1 mg G5/44.
Animals and procedures in vivo
Adult Balb/c nude mice (Charles River Laboratories, Wilmington, MA, USA) were irradiated with 400 rad gamma rays (137Cs). Ramos cells (107/200 μl) were injected in the right flank of mice. We conducted two experiments. In the first experiment, the pharmacokinetic parameters of CMA-676 were determined in two groups of five mice. The average body weight of the first group was 19 g (SD = 1 g). Mice in this group were not tumour-bearing. The second group of 5 mice weighed on average 20 g (SD = 1 g). These mice had a xenografted Ramos tumour with an average volume of 528 mm3 (SD = 102 mm3). In the second experiment, the pharmacokinetic parameters of CMC-544 were determined in two groups of mice. The average body weight of the first group was 19 g (SD = 1 g). This group consisted of three non-tumour-bearing mice. The second group consisted of six mice with an average body weight of 22 g (SD = 1 g). Mice in this group carried xenografted Ramos tumours with an average volume of 1,276 mm3 (SD = 398 mm3). Two days prior to treatment with conjugates, a 5 μl blood sample was taken from each mouse. A single dose of 150 μl (3 μg calicheamicin per mouse) CMA-676 or CMC-544 was injected in the lateral tail vein. At time intervals specified in the result section and in Figs. 3 and 4, blood samples of exactly 5 μl were taken. To obtain reproducible small samples, the mice were kept under a heating lamp until tail arteries became visible. After disinfection of the tail with 70% isopropyl alcohol, the tail artery was ruptured with a 255/8 G needle. This generated a blood drop that was aspirated with a capillary mounted to a micropettor (Drummond, Broomall, PA, USA) preset to an aspiration volume of 5 μl. This blood sample was immediately transferred to a test tube that contained 195 μl of the following mixture: 0.01 M HEPES (pH 7.4), 0.15 M NaCl, 3 mM EDTA, 0.005% Surfactant P20 (HBS-EP buffer, BIAcore, Uppsala, Sweden). All procedures with experimental animals were conducted conforming to PRACUC guidelines for humane treatment of animals.
Plasmon resonance analysis
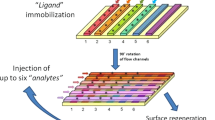
All analyses were performed on a BIAcore 3,000 instrument (GE Healthcare, Piscataway, NJ, USA). The detection system of this instrument relies in principle on the measurement of refractive index changes caused by the interaction of macromolecules on biosensor chips [6, 7, 10]. The method to determine CMC-544 binding to CD22 was published earlier [8] and is essentially similar to determine CMA-676 binding to CD33. Briefly, antigens were immobilized on the surface of a CM5 biosensor chip at a density of 4,000–9,000 resonance units per flow cell. The chip was activated by the coupling reagent 1-ethyl-3-(3-dimethylaminopropyl)-carbodiimide-HCl/N-hydroxysuccinimide at a flow rate of 5 μl/minute for 6 min, followed by the addition of antigens. CD33mFc or CD22mFc were covalently linked to CM5 chips by contacting the chip to 0.1 mg/ml protein in a solution of 10 mM sodium acetate (pH 5) at a flow rate of 2 μl per minute for 30 min. The chip was then washed with HBS-EP containing 300 mM NaCl. This high NaCl concentration decreased the background binding of plasma components without affecting binding of the antibody-conjugate.
Following immobilization of the antigen, diluted plasma of mice treated with CMA-676 or CMC-544 was run over the chip. The plasma was diluted in HBS-EP buffer and passed over the chip at a flow rate of 30 μl/min to allow binding. The amount of conjugate present in plasma was determined following interpolation of the RU values from a calibration curve depicting the RU value as a function of standard quantities of conjugate.
Pharmacokinetic calculations and statistical analysis
Pharmacokinetic values of the conjugates were analyzed using a non-compartmental analysis module (Model 201) of the pharmacokinetic software package WinNonlin, V4.1 (Pharsight, CA, USA). The model applies a model-independent approach as a standard method as described by Gibaldi and Perrier [11]. Significance of differences was probed by the two-tailed Student’s t test (SAS-excel). In a few cases, Satterthwaite approximate degrees of freedom were used because of the large differences in standard deviation.
Results
Sensitivity and linear range of determination of CMA-676 and CMC-544
To determine the total amount of antibody and the amount of calicheamicin conjugated to antibody, we designed a sandwich detection method. The principle of this method is illustrated in Fig. 1. Two consecutive responses were measured. A first response determines the number of resonance units (RUs) after passing a sample that contains the conjugate over the BIAcore chip with immobilized antigen recognized by the antibody moiety of the conjugate. This response is proportional to the sum of the free and conjugated antibody in the sample. A second response is obtained after running a solution of an anti-calicheamicin antibody over the material already bound to the immobilized antigen. This signal over the baseline of the first response is proportional to the amount of antibody conjugated to calicheamicin. Figure 2 shows the correlation between the concentration of standard samples of CMA-676 and CMC-544 and the number of RUs. The sensorgrams presented in Fig. 2a show that the method proposed in Fig. 1 is valid to detect CMA-676 in a concentration range from 100 to 1,000 ng/ml. Since plasma samples were immediately diluted 40-fold, the detection limit for CMA-676 in mouse plasma was 4 μg/ml. The relationship between the concentration of conjugate and the number of RUs is shown in Fig. 2b. The response after binding CMA-676 to CD33 was linear for a concentration range of conjugate between 0 and 500 ng/ml. A similar linear relationship was also found after binding of the conjugate to CD33 followed by a secondary response induced by the binding of raCM (CMA-676 + raCM). The difference of these responses (raCM) was also linear within this range. The regression coefficients of the quadratic equations of these functions were larger than 0.99 when a concentration range of 0–1,000 ng/ml was used. Interpolation by using a quadratic equation of a ‘concentration-RU’-plot allowed thus for the accurate determination of the concentration of a sample containing between 0 and 1,000 ng/ml conjugate.
Sensorgram of sandwich detection method. In the first phase of the curve (between arrows 1 and 2) the sample of conjugate was run over the immobilized antigen. Following a washing period (gray circle) a second phase (between arrows 3 and 4) was initiated by adding the antibody against calicheamicin, raCM. Response 1 indicates mass addition (expressed as resonance units, RU) proportionate to the concentration of antibody in the sample. Response 2 is proportionate to the amount of antibody conjugated to calicheamicin
Detection of standard concentrations of CMA-676 and CMC-544 in 1.4% mouse serum. a Shows the BIAcore sensorgrams determined for a concentration range (0–1,000 ng/ml) of CMA-676. These sensorgrams resemble the theoretical model depicted in Fig. 1. The amount of CMA-676 bound to CD33 increases as a function of the concentration of the conjugate (first phase of the sensorgram). The second phase of the sensorgram corresponds to the amount of CM bound to CMA-676. b, c Show the calibration curves obtained by sandwich plasmon resonance for CMA-676 and CMC-544, respectively. The correlation coefficients of approximately 1.00 allow for accurate determination of the total amount of antibody and the amount of calicheamicin bound to antibody
A similar strategy was followed to establish the calibration curves depicting the relationship between RU and the concentration of the antibody and CM conjugated to G5/44. This relationship was also best described (r > 0.99) by a quadratic equation for a concentration range between 0 and 1,000 ng/ml. It should be noted that a response to raCM was not observed with the naked antibodies, hP67.6 and G5/44 (data not shown), indicating that the response to raCM was specific for the presence of CM on the antibody.
Determination of pharmacokinetic values of CMA-676 in mouse plasma
Figure 3a shows the concentration of CMA-676 in plasma of nude mice at various time points following intravenous injection of a single dose of conjugate. A dose of 3 μg calicheamicin was given per mouse regardless of the mass of the animal. The actual dose of antibody as mg/kg body mass is indicated in the legend of Fig. 3a. Since 5 μl of total blood was used for the analysis, the concentration of the conjugate in plasma was calculated by correcting for a normal haematocrit of 45%. It was also assumed that the conjugate was not bound to the cell fraction of the blood. This is a reasonable assumption for the following reason. The administered dose of 3 μg calicheamicin translates into 86 μg protein in a blood volume of 1.5 ml (approximate blood volume of a 20 g mouse). Theoretically, one would thus anticipate 86 × 1.82 × 0.67 = 105 μg/ml as a maximum concentration. The experimental concentration determined after 20 min approximates 80 μg/ml. The amounts of conjugate that were given to each mouse varied depending on the actual body mass of the animal. Within a range of 4.1–4.5 mg conjugate per kg, the administered dose was not directly proportional to the maximum concentration of the conjugate in plasma. The data also did not indicate that this dose variation was responsible for inter-animal variations in circulation half-life. However, we found the highest plasma levels in a single mouse that received a dose of 5 mg conjugate per kg. The pharmacokinetic values of the antibody moiety of CMA-676 were also not influenced by presence of a CD33− tumour (Table 1). The mean clearance (Cls) values were 0.69 and 0.78 ml/min per kg in non-tumour and tumour-bearing animals, respectively. This low clearance corresponded to long circulation half-life (t 1/2) values of 109 and 110 h, respectively. The mean AUC0–∞ values were 7,665 and 6,735 μg h/ml, respectively. The mean volume of distribution (Vdss) for non-tumour-bearing and tumour-bearing animals was 95 and 94 l/kg, respectively suggestive of low distribution. There was no statistical difference in PK parameters of tumour- and non-tumour bearing mice.
Concentration of CMA-676 in plasma following intravenous injection of the conjugate in nude mice. Each mouse received a single dose of 3 μg calicheamicin (86 μg protein) in the lateral tail vein. The conjugate that was used had a loading ratio of 35 μg CM per mg hP67.6 antibody. a Shows the decreasing amount of antibody moiety of CMA-676 as measured by the amount of conjugate bound to CD33 (see response 1, Fig. 1). A steeper decline (b) of the concentration of CMA-676 was observed when the amount of conjugate was determined after measuring the amount of hP67.6 conjugated to calicheamicin (see response 2, Fig. 1). This was also illustrated by the decline of conjugated CM as a function of time (inset in b). Notice that the presence of a CD22-positive tumour (solid lines) has no influence on the kinetics of CMA-676 in plasma. Each point in the graphs represents a single determination of [CMA-676]
The amount of hP67.6 conjugated to calicheamicin has a shorter circulation half-life and reduced AUC0–∞ as compared to the antibody moiety (Fig. 3b, Table 1) of the conjugate. This was graphically illustrated by a consistently declining concentration of conjugated CM as a fraction of the antibody-moiety of CMA-676 (insert Fig. 3b). The presence of a CD33− tumour did not influence the PK-values of the amount of hP67.6 conjugated to calicheamicin. It should be noted that the presented sandwich method allowed for an evaluation of the clearance of calicheamicin conjugate. However, the method could not discriminate between a reduction of calicheamicin on all the conjugate molecules and the generation of a fraction of unconjugated antibody. Nonetheless, independent of the actual molecular change in the conjugate, the sandwich method showed a reproducible reduction of total calicheamicin bound to antibody that was not influenced by the presence of the Ramos tumour.
Determination of pharmacokinetic values of CMC-544 in mouse plasma
Similar to CMA-676, the amount of CMC-544 in plasma of mice was also determined by the sandwich plasmon resonance method. Figure 4 shows the declining concentration of the antibody moiety of CMC-544 in plasma of tumour-bearing and non-tumour-bearing mice. Concentrations of the antibody moiety of CMC-544 (Fig. 4a) and of the amount of CM bound to G5/44 (Fig. 4b) declined faster in tumour-bearing mice. Significant differences were observed in clearance and AUC0–∞ (Table 2). Despite similar body weight of tumour- and non-tumour-bearing nude mice, total systemic clearance (Cls) of CMC-544 and the corresponding AUC0–∞—values were significantly different (P < 0.05). This was also reflected in the decreased circulation half-life of CMC-544. However, this decrease was not statistically significant. The presence of a tumour that expresses the target of CMC-544 thus enhanced the removal of the conjugate from plasma. Most likely, retention of the antibody by the tumour was responsible for this observation. The decline of the calicheamicin concentration as a function of time was identical in tumour-bearing and non-tumour-bearing mice (insert Fig. 4b). Therefore, the presence of the tumour probably did not influence the release of CM from the antibody moiety of the conjugate.
Concentration of CMC-544 in plasma following intravenous injection of the conjugate in nude mice. Each mouse received a single dose of 3 μg calicheamicin (42 μg protein) in the lateral tail vein. CMC-544 was loaded with 72 μg CM per mg G5/44 antibody. a Shows the kinetics of the antibody moiety of CMC-544 as measured by the amount of conjugate bound to CD22 (see response 1, Fig. 1). Analogous to the kinetic pattern of CMA-676, a steeper decline (b) of the concentration of CMC-544 was observed when the amount of conjugate was determined after measuring the amount of G5/44 conjugated to CM (see response 2, Fig. 1). Notice that the presence of the CD22-positive Ramos tumour (solid lines) decreases the average concentration of CMC-544 in plasma (inset in b). Removal of CM from the antibody was not influenced by the presence of the tumour (dotted lines and solid lines intertwine in the inserted graph of b). Each point in the graphs represents a single determination of [CMC-544]
Discussion
The presented data show that sandwich plasmon resonance can reproducibly evaluate the circulation time of calicheamicin conjugates. Because of its sensitivity, a small sample of 5 μl whole blood is sufficient to determine the concentration of antibody and conjugated antibody at a given point in time. Therefore, not only the pharmacokinetic parameters of the antibody carrier of the conjugate, but also information about the stability of the linker can be inferred from the data.
The sensitivity and the inherent precision (detection interval of 100–1,000 ng) of the described BIAcore method can offer several advantages over the previously described methods for the determination of pharmacokinetic values of conjugated or naked biopharmaceuticals (e.g. antibodies or receptor ligands).
As opposed to traditional RIAs and ELISAs, the BIAcore method eliminates the use of labeled secondary reagents [12] and, therefore, abrogates the potential affinity changes resulting from the labeling [13]. Moreover, this method also renders the determination of the concentration of radiolabelled conjugate in plasma obsolete. Apart from avoiding the potential affinity changes of the reagents due to radiolabelling, the lack of requirement for radioisotopes also provides a practical benefit. By using the BIAcore method, safety issues concerning the use and disposal of radioactive substances and contaminated laboratory animals can be completely circumvented. Because of the need for minute samples, this method is ideally apt for multiple sampling in the same animal (longitudinal investigation). The suitability for longitudinal investigation also limits the number of animals needed for pharmacokinetic determinations without jeopardizing the quality of the results.
The BIAcore sandwich method was designed to answer critical questions regarding the biological distribution of calicheamicin conjugates that were not readily approachable by the traditional detection methods. Most cytotoxic anticancer pharmaceuticals have notoriously low therapeutic indices. For this reason, preclinical evaluation in test animals of the relationship between tolerated plasma concentration and efficacy of the drug is imperative to project therapeutic feasibility in humans. Calicheamicin immunoconjugates, in particular, were designed to overcome the systemic toxicity caused by calicheamicin [9]. By linking calicheamicin to the immunoglobulin carrier, the plasma half-life of this drug has been extended. Furthermore, the conjugate accumulates in tumour tissue and releases its DNA targeting agent after binding to a tumour-associated antigen [8]. Administering calicheamicin as an immunoconjugate has proven therapeutic value in a preclinical [8] and clinical setting [3]. Nonetheless, the physicochemical properties of the carrier molecule that quantitatively could influence the efficacy of a conjugate are still obscure. More specifically, the optimum range of PK-values that translates into a maximum accumulation of a macromolecular carrier in a tumour is yet to be established. As mentioned earlier, several elements in the design of traditional accumulation studies render it less feasible to address this issue. To distinguish between the accumulation rate of the antibody and calicheamicin, two experiments are usually conducted. One experiment requires radiolabelling of the antibody moiety of the conjugate. In a separate experiment, an immunoconjugate of radiolabelled calicheamicin has to be used. Apart from the logistic difficulties, these experiments require rather large groups of test animals [e.g. 14] limiting the number of conditions that can be explored. Most of these issues can be bypassed by using the presently described method. A group of three mice is sufficient to determine not only the PK-values of the antibody but also those of the intact conjugate. A distinction was noticed between the circulating half-lives (t 1/2) of intact CMA-676 and CMC-544 and their respective carrier antibodies hP67.6 and G5/44. As anticipated, the t 1/2 was shorter for the conjugates as compared to the antibody fraction. This indicated that the method could provide a measure of linker stability ‘in vivo’. Surprisingly, the plasma levels of CMC-544 in RAMOS-tumour-bearing animals were consistently lower than the plasma levels of this conjugate in non-tumour-bearing mice. Because this difference was not noticed with CMA-676 and since RAMOS expresses CD22 and not CD33, one possible explanation would be that the reduced plasma levels of CMC-544 were caused by the retention of the conjugate in the tumour. If so, this would pose the interesting prospect that the retention of a conjugate can be deduced from the PK-values.
In conclusion, we provided two examples of pharmacokinetic determinations of calicheamicin conjugates by using the BIAcore method. Combined with the precise frequent sampling technique, this method can become a powerful tool to empirically correlate circulating half-life of the conjugate and the stability of the linker on the one hand to the therapeutic efficacy and systemic toxicity on the other hand.
References
McLaughlin P, Grillo-Lopez AJ, Link BK, Levy R, Czuczman MS, Williams ME, Heyman MR, Bence-Bruckler I, White CA, Cabanillas F, Jain V, Ho AD, Lister J, Wey K, Shen D, Dallaire BK (1998) Rituximab chimeric anti-CD20 monoclonal antibody for relapsed indolent lymphoma: half of the patients respond to a four-dose treatment program. J Clin Oncol 16:2825–2833
Wiseman GA, Gordon LI, Multani PS, Witzig TE, Spies S, Bartlett NL, Schilder RJ, Murray JL, Saleh M, Allen RS, Grillo-Lopez AJ, White CA (2002) Ibritumomab tiuxetan radioimmunotherapy for patients with relapsed or refractory non-Hodgkin lymphoma and mild thrombocytopenia: a phase II multicenter trial. Blood 99:4336–4342
Sievers EL, Appelbaum FR, Spielberger RT, Forman SJ, Flowers D, Smith FO, Shannon-Dorcy K, Berger MS, Bernstein ID (1999) Selective ablation of acute myeloid leukemia using antibody-targeted chemotherapy: a phase I study of an anti-CD33 calicheamicin immunoconjugate. Blood 93:3678–3684
Schrama D, Reisfeld RA, Becker JC (2006) Antibody targeted drugs as cancer therapeutics. Nat Rev 5:147–159
Graff CP, Wittrup KD (2003) Theoretical analysis of antibody targeting of tumour spheroids: importance of dosage for penetration and affinity for retention. Cancer Res 63:1288–1296
Karlsson R, Michaelsson A, Mattsson L (1991) Kinetic analysis of monoclonal antibody-antigen interactions with a new biosensor based analytical system. J Immunol Methods 145:229–240
Johne B, Gadnell M, Hansen K (1993) Epitope mapping and binding kinetics of monoclonal antibodies studied by real time interaction analysis using surface plasmon resonance. J Immunol Methods 160:191–198
DiJoseph JF, Armellino DC, Boghaert ER, Khandke K, Dougher MM, Sridharan L, Kunz A, Hamann PR, Gorovits B, Udata C, Moran J, Popplewell AG, Stephens S, Frost P, Damle NK (2004) Antibody-targeted chemotherapy with CMC-544: a CD22-targeted immunoconjugate of calicheamicin for the treatment of B-lymphoid malignancies. Blood 103(5):1807–1814
Boghaert ER, Khandke K, Sridharan L, Armellino D, Dougher M, DiJoseph JF, Kunz A, Hamann PR, Sridharan A, Jones S, Discafani C, Damle NK (2006) Tumoricidal effect of calicheamicin immuno-conjugates using a passive targeting strategy. Int J Oncol 28:675–684
Johne B, Hansen K, Mørk E, Hotlund J (1995) Colloidal gold conjugated monoclonal antibodies, studied in the BIAcore biosensor and in Nycocard immunoassay format. J Immunol Methods 183:167–174
Gibaldi M, Perrier D (1982) Pharmacokinetics, 2nd edn. Marcel-Dekker. New York
Mason S, La S, Mytych D, Swanson SJ, Ferbas J (2003) Validation of the BIACORE 3000 platform for detection of antibodies against erythropoietic agents in human serum samples. Curr Med Res Opin 19:651–659
Pearson JE, Kane JW, Petrarki-Kallioti I, Gill A, Vadgama P (1998) Surface plasmon resonance: a study of the effect of biotinylation on the selection of antibodies for use in immunoassays. J Immunol Methods 221:87–94
Xie H, Audette C, Hoffee M, Lambert JM, Blättler WA (2004) Pharmacokinetics and biodistribution of the antitumor conjugate, Cantuzumab Mertansine (huC242-DM1), and its two components in mice. J Pharmacol Exp Ther 308:1073–1082
Acknowledgment
The authors thank Dr. Roger French for the statistical analysis of the data.
Author information
Authors and Affiliations
Corresponding author
Additional information
Erwin R. Boghaert and Kiran M. Khandke contributed equally to the presented results.
Rights and permissions
About this article
Cite this article
Boghaert, E.R., Khandke, K.M., Sridharan, L. et al. Determination of pharmacokinetic values of calicheamicin-antibody conjugates in mice by plasmon resonance analysis of small (5 μl) blood samples. Cancer Chemother Pharmacol 61, 1027–1035 (2008). https://doi.org/10.1007/s00280-007-0560-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00280-007-0560-2