Abstract
Factor V Leiden (FVL) G1691A, methylenetetrahydrofolate reductase (MTHFR) C677T, and factor II (FII) G20210A mutations are three important causes of thrombophilia, the condition that might be related to infertility and recurrent spontaneous abortion (RSA). In this study we evaluated the presence of these three mutations in 36 female patients with unexplained infertility, 65 female patients with unexplained RSA, and 62 healthy fertile women as control group. DNA was extracted from peripheral blood samples and PCR-RFLP was performed for the molecular diagnosis of each mutation. In addition, activated protein C resistance (APC-R) was also evaluated. The frequencies of FVL, MTHFR, and FII mutations (heterozygous and homozygous) in the control group were 0.0%, 38.7%, and 3.2%, respectively. The frequency of FVL mutation in patients with infertility (30.6%) or RSA (20.0%) was significantly higher than that of the control group. A significantly higher MTHFR mutation rate was also observed in patients with RSA (63.1%) as compared to controls. However, the mutation rate of MTHFR in patients with infertility (50.0%) was not statistically different from that in controls. No significant difference was observed in the frequencies of FII mutations between the patients and controls. Decreased levels of APC-R were observed in 25.0% of infertile patients and 18.9% of patients with RSA. In conclusion, our results show a skew towards higher mutation frequencies of FVL and MTHFR in patients that may necessitate detection of such mutations in these Iranian patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Recurrent spontaneous abortion (RSA) is a clinical problem that may have adverse effects on the emotional and social aspects of infertile couples’ life that wish to have a child. Recently, thrombophilias have been considered as a possible cause [1]. In the recent decades different inherited coagulation abnormalities, have been identified that predispose patients to thrombophilia [2–4]. Of these inherited abnormalities, a mutation in the factor V gene [5], a mutation in the methylenetetrahydrofolate reductase (MTHFR) gene [6], and a mutation in the prothrombin or factor II (FII) gene [6] were identified that result in thrombophilia.
Factor V Leiden (FVL) mutation is the cause of more than 95% of resistance to activated protein C (APC) [7, 8]. Resistance to APC is the most common genetic cause of venous thrombosis [7, 8]. This mutation is resulted from a G-to-A substitution at position 1691 in the coagulation factor V gene [8]. MTHFR mutation is caused by the change of C to T at position 677 and results in an increased total plasma homocysteine (tHcy) that is a risk factor for vascular disease [3, 4]. MTHFR gene has also been found to be associated with pregnancy complications particularly when it is homozygous or is concomitant with the factor V Leiden allele [9]. The mutation in the FII gene is characterized by a G-to-A substitution at position 20210 in the 3’ untranslated region and leads to elevated serum prothrombin levels [10]. This elevation causes an increased risk for venous thrombosis [11], arterial disease [12] and RSA [13, 14].
FVL mutation is reported in 5% of the healthy white population [15], 1% of the healthy black population [15] and 0% to 14% of Asian minor population [16]. Heterozygosity for the factor V Leiden mutation causes a 5-10-fold increase in the risk of thrombosis, whereas homozygosity confers a 50-100-fold increase in risk [5]. The prevalence of the MTHFR C677T mutation varies widely with ethnicity. In Caucasians [17] and Japanese [18], frequency of the mutant T allele is generally between 30 and 40% but it is much rarer in Africans [19]. FII mutation has an allele frequency of 1.2% in the general U.S. population and 3.0% in southern European populations [10]. The FII mutation is very rare in Asia and Africa [10].
In this study, the frequency of these three mutations in Iranian patients who suffered from unexplained infertility or RSA was investigated and compared with control group.
Materials and methods
Patients
Hundred and one patients with unexplained infertility or RSA, all admitted in Avesina Infertility Clinic (Tehran, Iran) during six months (2004) and 62 healthy fertile women as control group were evaluated for the presence of FVL G1691A, MTHFR C677T, and FII G20210A mutations. Patients were not selected based on the activated protein C resistance (APC-R) level. However, some of the patients were checked for APC-R level using staclot APCR kit according to the manufacturer’s instruction (Diagnostica Stago, Asnières, France). Informed consent was obtained and the study was approved by the ethics committee of the Avesina Research Institute. Three or more pregnancy losses in the first or second trimester were considered as RSA. We obtained medical histories, performed physical examinations, routine laboratory tests, endocrinologic examinations, and immunologic tests for autoantibodies for all patients.
Exclusion criteria were: anatomic abnormalities, endocrinologic dysfunction, autoimmune disease, liver function abnormalities, urogenital infection and inflammatory pelvic disease.
Genotype screening
Peripheral blood samples were collected and DNA was extracted by a standard salting out method using proteinase K [20]. PCR was performed using FVL [21], MTHFR [17], and FII [10] primers as explained previously. PCR amplification was confirmed by electrophoresing PCR products on 1.5% agarose gel. PCR products of FVL, MTHFR, and FII genes were digested by restriction enzymes Mnl1, HinfI, and HindIII respectively [10, 17, 21].
PCR product of coagulation factor V gene with 140 nucleotides has two restriction sites for Mnl1 enzyme yielding three fragments (69 bp, 36 bp, and 35 bp) after enzyme digestion. In the mutant allele restriction site between fragments 35 bp and 36 bp disappears.
In MTHFR gene PCR product has a length of 198 bp and lacks any restriction site for HinfI enzyme but the mutation creates a restriction site in the PCR product that produces two fragments (175 bp and 23 bp) after enzyme digestion.
For the amplification of FII gene a mutagenic primer was used to introduce a nucleotide substitution in the PCR product. This PCR product that has a length of 345 bp has no restriction site for HindIII enzyme but the combination of nucleotide substitution and genetic abnormality creates the HindIII enzyme cleavage site that cleaves the amplicon into two fragments (322 bp and 23 bp).
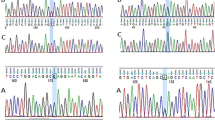
Digested products were analyzed by polyacrylamide gel electrophoresis (PAGE) and standard method of silver staining [20]. According to the number and size of bands on polyacrylamide gel, patients were classified as normal, heterozygote or homozygote for each gene (Fig. 1).
Statistical analysis
Data was processed with SPSS 11.0 software. The mutation frequencies in FVL, MTHFR, and FII genes between patient groups and the control group were analyzed using the Chi-square test. P-values of <0.05 were taken as statistically significant.
Results
Female patients (n=101) with unexplained infertility or RSA were evaluated for the presence of FVL, MTHFR, and FII mutations and APC-R level as well. An APC-R less than 120 seconds was considered as abnormal or decreased level. 36 patients (35.6%) suffered from infertility and 65 patients (64.4%) suffered from RSA. Details about mutation frequencies are shown in Table 1. Among the patients with FVL mutation, only one patient was homozysfgote and the rest of the patients (n=23) were heterozygote. 49 of the patients were heterozygote and 10 of them were homozygote for MTHFR mutation. All of the patients with FII mutation (n=4) were heterozygote.
62 healthy fertile women were also checked for these three mutations. None of them had FVL mutation, 38.7% had MTHFR mutation and 3.2% had FII mutation (Table 1).
Twenty five percent and 18.9% of the patients with infertility and RSA had low levels of APC-R, respectively (Table 1). Seventy five percent of decreased APC-R levels (12 out of 16) were detected in patients with FVL mutation and 70.6% of FVL mutations (12 out of 17) were associated with decreased APC-R level (P<0.05). Mean APC-R level in patients with FVL mutation was 103.5±43.2 seconds; whereas, the mean APC-R level in patients without this mutation was 160.4±32.6 seconds.
Discussion
The discovery of the FVL G1691A, MTHFR C677T, and FII G20210A mutations has revolutionized the diagnostic work-up of patients with thrombophilia [2–4, 6].
In this study we evaluated these three mutations in 101 patients with unexplained infertility or RSA and 62 healthy fertile women. Some of the patients were tested for alteration in APC-R level. Results are shown in Table 1.
Frequency of FVL mutation in patients with infertility (30.6%) and RSA (20.0%) was significantly higher than that in the control group (0.0%) (P<0.05) (Table 1). Frequency of FVL mutation in Iranian population is 5.5% [22] that is lower than the frequency in our patients group. Souza et al. reported that 7.1% of Brazilian patients with RSA had FVL mutation compared with 1.6% of the normal people [23]. This relation was 17% vs. 2% in the United States [24]. In another study, none of the 52 Japanese women with RSA carried FVL mutation [25]. Our data supported that the frequency of FVL mutation in Iranian patients with infertility (30.6%) or RSA (20.0%) is higher than that in these countries. However, the rate of this mutation in Iranian normal population (5.5%) [22], control group (0.0%), and Asian population (0% to 14%) [16] is lower than the frequency of the mutation in these countries, therefore, it is important to note that possibly in a normal population with low frequency of FVL mutation the association of the mutation with infertility or RSA is more significant.
This study showed that the frequency of MTHFR C677T mutation in patients with RSA is significantly higher than control group (63.1% vs. 38.7%, P<0.05) but it was not higher in patients with infertility (Table 1). Frequency of MTHFR mutation in 271 postmenopausal Iranian women was reported to be 39.8% [26] that was lower than the results of this study.
The frequency of FII G20210A mutation in Iranian population is 3.1% [22]. In this study the frequency of FII mutation in patients with infertility (2.8%) and RSA (4.6%) was not statistically higher than control group (3.2%) (P>0.05) (Table 1).
In general, it may be concluded that FVL mutation might play a role in infertility and RSA but MTHFR mutation may only act as a causative factor in RSA. This study did not show any relation between FII mutation and infertility or RSA.
In this study 75.0% of the patients with decreased APC-R level had FVL mutation and 25.0% did not (P<0.05), but Major et al. reported that more than 95% of all people with APC resistance have FVL mutation [8]. This difference indicates that other causes of increasing APC-R level are probably more common in Iran.
Diagnosis of mutations that are involved in unexplained infertility and RSA and using an appropriate treatment plan helps couples to conceive. Therefore, it is necessary for the patients with infertility problem especially RSA to undergo screening tests for mutations related to thrombophilia.
This study is one of the first studies that have been performed about thrombophilia in Iranian patients with infertility or RSA and more investigations should be done for other associated mutations in the future.
References
Kovalevsky G, Gracia CR, Berlin JA, Sammel MD, Barnhart KT (2004) Evaluation of the association between hereditary thrombophilias and recurrent pregnancy loss: a meta-analysis. Arch Intern Med 164(5):558−563
Lane DA, Mannucci PM, Bauer KA, Bertina RM, Bochkov NP, Boulyjenkov V et al (1996) Inherited thrombophilia: part 1. Thromb Haemost 76:651−662
Lane DA, Mannucci PM, Bauer KA, Bertina RM, Bochkov NP, Boulyjenkov V et al (1996) Inherited thrombophilia: part 2. Thromb Haemost 76:824−834
De Stefano V, Finazzi G, Mannucci PM. (1996) Inherited thrombophilia: pathogenesis, clinical syndromes, and management. Blood 87:3531−3544
Vefring H, Lie RT, ODegard R, Mansoor MA, Nilsen ST (2004) Maternal and fetal variants of genetic thrombophilias and the risk of preeclampsia. Epidemiology 15(3):317−322
Wisotzkey JD, Bayliss P, Rutherford E, Bell T (1999) Placental genotyping of the factor V Leiden, prothrombin 20210A and the methylenetetrahydrofolate reductase (MTHFR) C677T alleles in IUGR pregnancies. Thromb Haemost 81(5):844−845
Zoller B, Svensson PJ, He X, Dahlback B (1994) Identification of the same factor V gene mutation in 47 out of 50 thrombosis-prone families with inherited resistance to activated protein C. J Clin Invest 94:2521−2524
Major DA, Sane DC, Herrington DM (2000) Cardiovascular implications of the factor V Leiden mutation. Am Heart J 140(2):189−195
Candito M, Magnaldo S, Bayle J, Dor JF, Gillet Y, Bongain A et al (2003) Clinical B12 deficiency in one case of recurrent spontaneous pregnancy loss. Clin Chem Lab 41(8):1026−1027
Poort SR, Rosendaal FR, Reitsma PH, Bertina RM (1996) A common genetic variation in the 3’-untranslated region of the prothrombin gene is associated with elevated plasma prothrombin levels and an increase in venous thrombosis. Blood 88:3698−3703
Prandoni P, Lensing AWA, Cogo A, Cuppini S, Villalta S, Carta M et al (1996) The long-term clinical course of acute deep venous thrombosis. Ann Intern Med 125:1−7
Van den Belt AGM, Sanson BJ, Simioni P, Prandoni P, Buller HR, Girolami A et al (1997) Recurrence of venous thromboembolism in patients with familial thrombophilia. Arch Intern Med 157:2227−2232
Sarig G, Younis JS, Hoffman R, Lanir N, Blumenfeld Z, Brenner B (2002) Thrombophilia is common in women with idiopathic pregnancy loss and is associated with late pregnancy wastage. Fertil Steril 77(2):342−347
Finan RR, Tamim H, Ameen G, Sharida HE, Rashid M, Almawi WY (2002) Prevalence of factor V G1691A (factor V-Leiden) and prothrombin G20210A gene mutations in a recurrent miscarriage population. Am J Hematol 71(4):300−305
Rand JH, Luong TH (1999) Thrombophilias: diagnosis and treatment of thrombophilia relating to contraception and pregnancy. Semin Hematol 36:2−9
Rosendaal FR (1999) Venous thrombosis: a multicausal disease. Lancet 353:1167−1173
Frosst P, Blom HJ, Milos R, Goyette P, Sheppard CA, Matthews RG et al (1995) A candidate genetic risk factor for vascular disease: a common mutation in methylenetetrahydrofolate reductase. Nat Genet 10(1):111−113
Morita H, Kurihara H, Tsubaki S, Sugiyama T, Hamada C, Kurihara Y et al (1998) Methylenetetrahydrofolate reductase gene polymorphism and ischemic stroke in Japanese. Arterioscler Thromb Vasc Biol 18(9):1465−1469
Adjalla CE, Amouzou EK, Sanni A, Abdelmouttaleb I, Chabi NW, Namour F et al (2003) Low frequency of mutated methylenetetrahydrofolate reductase 677C-->T and 1298A-->C genetics single nucleotide polymorphisms (SNPs) in Sub-Saharan populations. Clin Chem Lab Med 41(8):1028−1032
Rousseau F, Rehel R, Rouillard P, DeGranpre P, Khandjian EW (1994) High throughput and economical mutation detection and RFLP analysis using a minimethod for DNA preparation from whole blood and acrylamide gel electrophoresis. Hum Mutat 4(1):51−54
Pauler HU, Voigt-Tschirschwitz T, Hinney B, Burfeind P, Wolf C, Emons G (2003) Analyzes of three common thrombophilic gene mutations in German women with recurrent abortions. Acta Obstet Gynecol Scand 82:942−947
Zeinali S, Duca F, Zarbakhsh B, Tagliabue L, Mannucci PM (2000) Thrombophilic mutations in Iran. Thromb Haemost 83(2):351−352
Souza SS, Ferriani RA, Pontes AG, Zago MA, Franco RF (1999) Factor V leiden and factor II G20210A mutations in patients with recurrent abortion. Hum Reprod 14(10):2448−2450
Glueck CJ, Wang P, Goldenberg N, Sieve L (2004) Pregnancy loss, polycystic ovary syndrome, thrombophilia, hypofibrinolysis, enoxaparin, metformin. Clin Appl Thromb Hemost 10(4):323−334
Hashimoto K, Shizusawa Y, Shimoya K, Ohashi K, Shimizu T, Azuma C et al (1999) The factor V Leiden mutation in Japanese couples with recurrent spontaneous abortion. Hum Reprod 14(7):1872−1874
Golbahar J, Hamidi A, Aminzadeh MA, Omrani GR (2004) Association of plasma folate, plasma total homocysteine, but not methylenetetrahydrofolate reductase C667T polymorphism, with bone mineral density in postmenopausal Iranian women: a cross-sectional study. Bone 35(3):760−765
Acknowledgement
We would like to express our sincerest appreciation to Dr. Akhondi as the chairman of Avesina Research Institute for his kindness in providing all of the expenses of this project.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Behjati, R., Modarressi, M.H., Jeddi-Tehrani, M. et al. Thrombophilic mutations in Iranian patients with infertility and recurrent spontaneous abortion. Ann Hematol 85, 268–271 (2006). https://doi.org/10.1007/s00277-005-0021-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-005-0021-0