Abstract
Background
Laparoscopic common bile duct exploration (LCBDE) has become one of the main options for treating choledocholithiasis associated with cholelithiasis. Our objective was to assess the short-term outcomes of patients undergoing laparoscopic primary closure of the common bile duct (CBD) compared with laparoscopic choledochotomy plus T-tube drainage.
Methods
We retrospectively studied 137 patients undergoing primary closure following LCBDE (group A) compared with 102 cases with laparoscopic choledochotomy plus T-tube drainage (group B) between January 2007 and January 2010. Intraoperative cholangiography (IOC) and choledochoscopy were performed in all patients.
Results
Three patients in group A (2.2%) were converted to open surgery and two (2.0%) in group B because of serious adherence. According to routine IOC, unexpected CBD stones were found in 16 cases (6.8%). The duration of the operation in group A was shorter than in group B (92.4 ± 15.2 vs. 125.7± 32.6 min, P < 0.05), as was length of postoperative stay (3.1± 2.4 vs. 5.7± 4.3 days, P < 0.05). Postoperative bile leakage occurred in six patients (4.5%) in group A and four cases (4.0%) in group B; all of the patients recovered after simple drainage without reoperation. Bile peritonitis was seen in one case after T-tube removal. The median follow-up was 26 months. There were no recurrences.
Conclusions
Laparoscopic primary closure of the CBD is safe and successful for the management of CBD stones. Application of IOC and choledochoscopy to ensure clearance of the CBD and careful suturing are essential for primary closure.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
With the development of laparoscopic equipment and technique, laparoscopic common bile duct exploration (LCBDE) has become one of the main options for the treatment of choledocholithiasis associated with cholelithiasis. In 2008, the UK guidelines recommended LCBDE as the treatment of choice for patients with common bile duct (CBD) stones undergoing laparoscopic cholecystectomy [1]. This aim of this study was to assess the feasibility, efficacy, safety, and patients’ short-term outcomes after laparoscopic primary closure of the CBDC ompared with T-tube drainage. In the most recent 3 years, 239 patients were selected to undergo LCBDE followed by primary closure or T-tube drainage. The clinical outcomes were collected and analyzed.
Materials and methods
Patients and methods
This study was a retrospective analysis carried out between January 2007 and January 2010. In this period, 223 patients were diagnosed choledocholithiasis by preoperative B-type ultrasonography (US), magnetic resonance cholangiopancreatography (MRCP), or endoscopic retrograde cholangiopancreatography (ERCP); the other 16 cases were diagnosed by intraoperative cholangiography (IOC). The patients suffered from intrahepatic bile duct stone were excluded from the study. A total of 239 consecutive patients underwent LCBDE followed by primary closure (group A, n = 137) or T-tube drainage (group B, n = 102). All procedures were performed by the same consultant surgeon. The clinical demographic details and the biochemical findings are shown in Table 1 There were no significant differences between the two groups.
Operative technique
Laparoscopic cholecystectomy was performed using a standard four-port technique. We used a 30° video-laparoscope (Stryker, Kalamazoo, MI, USA) placed through a 10 mm umbilical port. A 12 mm port was placed in the subxiphisternum and two 5 mm ports in the right abdomen. In the case of gross distension of the gallbladder, its contents were aspirated with a Veress needle. During LCBDE, the 12 mm port was used to accommodate the operating choledochoscope (Olympus, Tokyo, Japan).
The operation was started with dissection of Calot’s triangle, and the cystic artery was clipped and cut off. Similarly, the distal cystic duct was clipped 1 cm away from CBD (Fig. 1). A short incision was made in the lateral wall of the cystic duct, and the catheter was passed into the CBD and secured with a clip around the cystic duct. Routine transcystic intraoperative cholangiography (IOC) was performed with 30% diatrizoate meglumine, and the number of stones in the CBD was confirmed (Fig. 2). The stump of the cystic duct was clamped with an absorbable clip (Tyco Healthcare, Norwalk, CT, USA). The gallbladder was left in situ and used for retraction until LCBDE was completed. When the CBD was approached directly, a longitudinal supraduodenal choledochotomy was undertaken using microscissors (Fig. 3). In cases where the anatomy of the extrahepatic bile ducts was not obvious, we used needle aspiration of bile to identify the CBD. The CBD stones were entirely retrieved using a wire basket in all patients, with the basket being passed through the distal CBD into the duodenum to prevent the retained stones from being incarcerated in the sphincter of Oddi muscle. After all stones were retrieved and clearance of the intrahepatic/extrahepatic bile duct was confirmed with choledochoscopy (Fig. 4) the choledochotomy was closed with interrupted 3.0 Vicryl sutures (Johnson & Johnson, New Brunswick, NJ, USA) (Fig. 5). A nonsuction drain was placed in the gallbladder bed near the CBD incision in all patients. It was removed the next day or, in cases of bile leak, when drainage ceased. For patients in whom we used T-tube drainage, the T-tube was placed in the choledochotomy and secured with the same sutures (Fig. 6). The T-tube was then led outside the body from the right upper quadrant. In the absence of pain and when the general condition permitted, the patient was discharged with the T-tube in situ. It was ligated 2 weeks after the operation and removed 12 weeks later after the routine tubogram and choledochoscopy at the outpatient department (OPD).
Transcystic cholangiogram. a Through the short incision of the cystic duct, a catheter was passed into the common bile duct (CBD) and secured with a clip around the cystic duct to prevent leakage of radiopaque materials. To avoid false-positive results, care must be taken that an air bubble is not injected into the CBD. b Routine transcystic IOC was performed with 30% diatrizoate meglumine, and the number and locations of stones in the CBD were determined
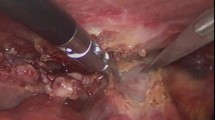
CBD stone was removed by choledochoscopy, and the intrahepatic and extrahepatic bile duct was explored. a, b Stones in the CBD were completely removed by choledochoscopy. c The basket was passed through the distal CBD into the duodenum to prevent the retained stones becoming incarcerated in sphincter of Oddi muscle. d Inflammation and edema are observed in the wall of CBD and/or sphincter of Oddi. It was confirmed that no stones remained in the intrahepatic or extrahepatic bile duct
T-tube drainage. a T-tube was placed in the CBD, and rest of the incision was closed with interrupted sutures. The T-tube was placed in the choledochotomy and secured with the same sutures. b Nonsuction drainage was placed near the CBD incision and the gallbladder bed so it could drain blood or bile directly
Follow-up
All patients were routinely assessed for complications at least 12 weeks after discharge or T-tube removal. B-Ultrasonography (US) examination and liver function tests (LFTs) were performed in every patient. The median follow-up was 26 months.
Statistical analysis
Statistical analysis was performed using SPSS 13.0 software (SPSS, Chicago, IL, USA). Variables were considered statistically significant with P < 0.05.
Results
Between January 2007 and January 2010 (36 months), we performed 239 laparoscopic explorations of the CBD and there were no perioperative deaths groups. Only three patients (2.2%) in group A were converted to open surgery and two patients (2.0%) in group B because of serious adhesions, leading to difficult anatomy and dissection. Transcystic IOC and choledochoscopy were routinely performed in all patients. Despite only slightly abnormal LFTs (e.g., alkaline phosphatase, glutamyl transpeptidase, direct bilirubin), IOC revealed the presence of CBD stones in 16 cases (6.8%), although preoperative US had shown negative results in the CBD. False-negative IOC results were found in three cases (1.3%) and a false-positive result in one case (0.4%).
The mean operating time was 92.4 ± 15.2 min in group A versus 125.7 ± 32.6 min in group B. The length of postoperative hospital stay was shorter in group A (3.1 ± 2.4 days) than in group B (5.7 ± 4.3 days). Postoperative bile leakage occurred in six patients in group A (4.5%) and four cases in group B (4.0%). All of the patients were treated with drainage and recovered within 6 to 10 days without reoperation. No postoperative pancreatitis or bile duct stricture occurred in the two groups.
In the group treated with T-tube biliary drainage, one patient (1.0%) experienced postoperative intermittent vomiting of unknown origin for 15 days, after which it spontaneously and suddenly disappeared. Bile peritonitis was seen in one patient (1.0%) after T-tube removal; another tube was then placed in the sinus tract, and the patient recovered with expectant treatment. The median follow-up was 26 months, with no recurrence or bile duct stricture occurring during that time. The postoperative clinical variables of the patients are shown in Tables 2 and 3.
Discussion
During an era of laparoscopic cholecystectomy (LC), the management of CBD stones remains controversial. For patients suspected of having CBD stones, many surgeons favor preoperative ECRP with extractions of the stones (ES). Another option is IOC with postoperative ERCP if stones are found, but such a plan necessitates reexploration if the sphincterotomy and the extraction fail. Others, therefore, advocate conversion to an open procedure if CBD stones are noted on the IOC. To increase the efficiency of procedures, many surgeons recommend LCBDE as the most efficient means to manage CBD stones.
Traditionally, exploring the CBD with open surgery or laparoscopically was accompanied by placement of T-tube drainage. The rationale for the use of a T-tube following CBD exploration was based on three main factors: (1) the potential for extracting retained stones; (2) as a method of achieving a controlled biliary fistula; and (3) easy access for radiologic visualization of the CBD. However, there are numerous reports of diminished quality of life and complications specifically associated with the use of a T-tube for biliary drainage. In general, complications include fluid and electrolyte disturbances, sepsis, premature dislodgement, bile leak, localized pain, biliary peritonitis, prolonged biliary fistulas, and late biliary stricture. It is important to note that the presence of a T-tube does not prevent bile leaks as they occur when it is still in situ or after its removal [2–5].
Previous studies comparing primary closure with T-tube drainage during open techniques [6] showed a significant reduction in hospital stay and duration of operation with comparable complication rates. Subsequently, Wu and Soper [7], in a prospective randomized experimental animal study of various laparoscopic techniques for exploring and closing the CBD, showed similar reductions in the operating time. They also reported that primary closure of the CBD resulted in a significant increase in stenosis. LCBDE was a natural step forward once laparoscopic cholecystectomy became a standard technique for managing cholecystolithiasis. The rationale was the same as for the open technique: a one-stage approach to CBD stones and avoidance of the ERCP and its associated cost and complications.
In 1994, Berci and Morgenstern, in the multiinstitutional SAGES study, paved the way for laparoscopic extraction of CBD stones [8]. However, in their study, 83% of LCBDEs were done via the transcystic route; in the case of choledochotomy, primary closure was never attempted, and 95% of patients had a T-tube drain. In 1999, Cuschieri et al. [9], in the EAES study, concluded that the laparoscopic single-stage approach for management of gallstone disease and choledocholithiasis is a better option for patients with American Society of Anesthesiologists (ASA) grades 1 and 2.
Over the years, other researchers have compared LCBDE with and without a T-tube drain. In a study of 38 patients, 12 with primary closure and 26 with Kehr’s tube, Ha et al. [10] concluded that primary closure of the CBD was feasible and safe. With increasing acceptance of the technique and the growing experience of surgeons, LCBDE without biliary drainage became more widely practiced [11–18]. Especially, use of the choledochoscope enables direct visualization of the CBD and ensures its complete clearance as well as inspection of the distal CBD for other possible causes of obstruction at the level of the sphincter of Oddi.
In our study, a group of 239 patients who suffered from choledocholithiasis associated with cholelithiasis were separated into two groups, and the clinical data were analyzed retrospectively. We achieved statistically significant shortening of the operating time and length of hospital stay for patients with primary closure versus those seen with T-tube drainage. No other significant differences were found between the two groups, such as intraoperative blood loss, postoperative bile leakage, the incidence of postoperative pancreatitis, stricture of bile duct, and recurrence.
In our opinion, the indications for laparoscopic primary closure of the CBD are as follows: (1) presence of choledocholithiasis without evidence of intrahepatic bile duct stones; (2) diameter of the CBD is ≥0.8 cm; (3) little inflammation or edema in the wall of CBD or sphincter of Oddi. The most important point for laparoscopic primary closure is to ensure that all CBD stones are retrieved, confirming their clearance by choledochoscopy.
For this reason, preoperative B-US, transcystic IOC, and choledochoscopy are used to evaluate the number and size of stones in the CBD and to make sure that no calculus is retained before suture. Transcystic IOC seems especially important to a certain extent. In our study, we found unexpected CBD stones in 16 cases (6.8%) by IOC based on slightly abnormal LFTs, although negative results in CBD by preoperative B-US was negative for CBD stones. False-negative IOC results were seen in three patients (1.3%) and false-positive results in one case (0.4%). Jameel et al. [19] found unexpected stones in the CBD in approximately 23.9% of patients who underwent LCBDE, which was more than in our study. This would represent a high rate of unexpected CBD stones during laparoscopic cholecystectomy, which proved the essentiality of IOC. Moreover, we considered the use of a T-tube appropriate only in patients who had retained impacted stones indicating burdensome extraction, serious cholangitis with frank pus in the CBD, gross inflammation, or a very thin CBD [11, 20].
In addition, sophisticated skill with suturing is of great importance to prevent postoperative bile leakage or stenosis. Interrupted sutures are recommended with absorbable material, which may reduce the recurrence of stones and stenosis of the CBD. There were 10 cases of bile leakage in the two groups, the main reason for which might be moderate edema of the wall of the CBD and the sphincter of Oddi. Fortunately, the transudative bile was completely drained by the nonsuction catheter without localized or extensive peritonitis. All of these patients were treated by drainage, and they recovered without reoperation. If the volume of bile in the drain had increased and patients started to develop signs of extensive biliary peritonitis, they would undergo another laparoscopic operation. Additional sutures would be needed if there is a leak from the choledochotomy site [19].
Conclusions
Laparoscopic primary closure of the CBD is safe and successful for the management of CBD stones. Primary closure can increase the quality of life and avoid the complications specifically associated with the use of a T-tube for biliary drainage. It is a better option, however, only if the indications are strictly followed. Because the median follow-up in our study is only 26 months, the patients’ long-term outcome needs further clinical observation. Routine IOC is applied to every patient, as far as possible, if the LFTs (e.g., alkaline phosphatase, glutamyl transpeptidase, direct bilirubin) are even slightly abnormal as unexpected CBD stones may be found. It is also useful for evaluating the number and size of stones. Choledochoscopy must be used to ensure clearance of the CBD, and careful suturing must be done to prevent bile leakage or stenosis.
References
Williams EJ, Green J, Beckingham I et al (2008) Guidelines on the management of common bile duct stones (CBDS). Gut 57:1004–1021
Wills VL, Gibson K, Karihaloot C et al (2002) Complications of biliary T-tubes after choledochotomy. ANZ J Surg 72:177–180
Moreaux J (1995) Traditional surgical management of common bile duct stones: a prospective study during a 20-year experience. Am J Surg 169:220–226
Marwah S, Singh I, Godara R et al (2004) Evaluation of primary duct closure vs T-tube drainage following choledochotomy. Indian J Gastroenterol 23:227–228
Thompson MH, Tranter SE (2002) All-comers policy of laparoscopic exploration of the common bile duct. Br J Surg 89:1608–1612
Williams JA, Treacy PJ, Sidey P et al (1994) Primary duct closure versus T-tube drainage following exploration of the common bile duct. Aust NZ J Surg 64:823–826
Wu JS, Soper NJ (2002) Comparison of laparoscopic choledochotomy closure techniques. Surg Endosc 16:1309–1313
Berci G, Morgenstern L (1994) Laparoscopic management of common bile duct stones: a multi-institutional SAG endoscopic sphincterotomy study. Surg Endosc 8:1168–1175
Cushieri A, Lezoche E, Morino M et al (1999) E.A.E.S. multicenter prospective randomised trial comparing two-stage vs. single-stage management of patients with gallstone disease and ductal calculi. Surg Endosc 13:927–952
Ha JP, Tang CN, Siu WT et al (2004) Primary closure versus T-tube drainage after laparoscopic cholecystectomy for common bile duct stones. Hepatogastroenterology 51:1605–1608
Decker G, Borie F, Millat B et al (2003) One hundred laparoscopic choledochotomies with primary closure of the common bile duct. Surg Endosc 17:12–18
Gurusamy KS, Samraj K (2007) Primary closure versus T-tube drainage after laparoscopic common bile duct stone exploration. Cochrane Database Syst Rev. doi: 10.1002/14651858.CD005641.pub2
Leida Z, Ping B, Shuguang W et al (2008) A randomized comparison of primary closure and T-tube drainage of the common bile duct after laparoscopic choledochotomy. Surg Endosc 22:1595–1600
Alhamdani A, Mahmud S, Jameel M et al (2008) Primary closure of choledochotomy after emergency laparoscopic common bile duct exploration. Surg Endosc 22:2190–2195
Zhang WJ, Xu GF, Wu GZ et al (2009) Laparoscopic exploration of common bile duct with primary closure versus T-tube drainage: a randomized clinical trial. J Surg Res 157:e1–e5
Kuroki T, Tajima Y, Tsuneoka N et al (2010) Placement of a plastic biliary stent tube with primary closure of the common bile duct after laparoscopic common bile duct exploration. Hepatogastroenterology 57:1034–1036
Huang SM, Yao CC, Cheng YW et al (2010) Laparoscopic primary closure of common bile duct combined with percutaneous cholangiographic drainage for treating choledocholithiasis. Am Surg 76:517–521
Ji WB, Zhao ZM, Dong JH et al (2011) One-stage robotic-assisted laparoscopic cholecystectomy and common bile duct exploration with primary closure in 5 patients. Surg Laparosc Endosc Percutan Tech 21:123–126
Jameel M, Darmas B, Baker AL (2008) Trend towards primary closure following laparoscopic exploration of the common bile duct. Ann R Coll Surg Engl 90:29–35
Krauss H, Kern E (1967) Some current problems of biliary tract surgery: indications and technique of choledochotomy, intraoperative cholangiomanometry, primary closure of the common bile duct. Surgery 62:983–987
Conflicts of interest
The authors report no potential or real conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is distributed under the terms of the Creative Commons Attribution Noncommercial License, which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
Rights and permissions
About this article
Cite this article
Cai, H., Sun, D., Sun, Y. et al. Primary Closure Following Laparoscopic Common Bile Duct Exploration Combined with Intraoperative Cholangiography and Choledochoscopy. World J Surg 36, 164–170 (2012). https://doi.org/10.1007/s00268-011-1346-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-011-1346-6