Abstract
Although the importance of volume loss in the aging face is now well recognized and fat grafting has increasingly become an integral part of contemporary facelift procedures, general acceptance of the fat grafting technique is a relatively recent occurrence and many surgeons reluctance to adopt the technique can be traced back in part to questions they have as to how loss of volume contributes to how the face ages, how to specifically recognize those changes, and questions they have about how to perform the fat grafting procedure to correct them. In this article we attempt to answer the questions “why perform facial fat grafting during facelift procedures?”, “where should fat be placed in the face?”, “how should fat be injected?”, and “how much should be injected in each area?”.
Level of Evidence V
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Face Lift and Fat Grafting—Why?
Identifying the changes that occur as the face ages and appreciating the underlying anatomical problems is essential to the recommendation of appropriate treatment and proper planning of surgical procedures. Our traditional “lifts” of the face provided improvement in tissue sagging and skin redundancy. Fat grafting allows us to treat atrophy, something we have previously been unable to do, and stands as a powerful technique now acknowledged by most plastic surgeons and other physicians engaged in treating the aging face as the “missing link” and the most important advance in esthetic surgery in several decades or more. Properly performed, the addition of fat to areas of the face that have atrophied due to age or disease can produce a significant and sustained improvement in appearance unobtainable by other means. When a facelift is performed in conjunction with fat injections, both loss of contour and facial atrophy can be corrected, and optimal improvement can be obtained (Fig. 1).

Procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery
a, b Simultaneous facelift and fat injections. All things being otherwise equal, simultaneous facelift and fat grafting will produce a better result than either technique performed alone. a A 49 year-old patient with both tissue ptosis and redundancy and marked facial atrophy. b Same patient seen 1 year and 3 months after high-SMAS facelift, neck lift, closed forehead lift, lower blepharoplasty, and pan-facial fat injections. Combined lifting and filling of her face produced a better outcome than either technique could have alone .
Drawbacks of Fat Injections
Performing fat injections in conjunction with a facelift has certain disadvantages including the learning curve associated with any new procedure, an increase in operating room time, increased postoperative edema, a longer period of recovery, and uncertainty of graft take. In addition, certain patient (and surgeon) misconceptions will also be encountered and will have to be overcome including misguided beliefs that injected fat can migrate or fall, or that fat injections will make the face “look “fat.”
Age-related loss of facial fat rarely exists as an isolated event in the healthy patient, and thus, patients troubled by it are rarely logically or appropriately treated by fat injections alone. Isolated fat injections are also arguably of questionable benefit to the patient troubled by significant facial sagging and skin redundancy. Although aggressive filling of the sagging face with fat can produce improved contour and a smoother appearing skin surface, it generally results in an unusually large, overfilled face that appears both unnatural and unfeminine. Such an overfilled face is hard to correct in an attractive manner at a later date, and it is both more logical and practical to perform fat injections in conjunction with formal surgical lifts if needed, or sometime after ptotic tissue has been repositioned and redundant tissue has been removed.
Facelift and Fat Grafting—Where?
Areas in need of treatment will vary from patient, and planning fat injections requires looking at the face in a different way and more as a “sculptor” and less as a “tailor” as we have done in the past. Any area successfully treatable with non-autologous injectable fillers is potentially treatable with fat injections including, but not limited to, the temples, forehead, brow, glabella, radix, upper orbit (“upper eyelid”), lower orbit (“lower eyelid”), cheeks, mid-face, buccal recess, lips, peri-oral, nasolabial crease, geniomandibular groove, and jawline. Perhaps the best way to decide where fat is needed is for the surgeon to study her or his facelift outcomes carefully and identify areas where the procedure has fallen short. In most cases, the biggest shortcoming for the experienced surgeon will be evident as the failure to replenish lost volume. In time, and after engaging thoughtfully in such study, one will gain a deeper appreciation of facial atrophy and an increasing desire to correct it. Figure 2 shows a patient before and after facelift and fat injections, and the areas where fat was placed.

Procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery
a–c Patient before and after simultaneous facelift and fat injections. a Before surgery view of a woman age 45. She has had not prior surgery. b Shaded areas showing where fat was placed. Three cc were placed in each upper orbit, 6 cc was placed in each temple, 1 cc was placed in each tear trough, 3 cc was placed in each infra-orbital area, 6 cc was placed in each cheek, 1 cc was placed in each nasolabial crease, 1 cc was placed in each labiomandibular groove, 2 cc was placed in each geniomandibular groove, 1 cc was placed in each lip, and 2 cc was placed in the glabella. A total of 50 cc of fat was injected. c Same patient 2 years and 4 months after high-SMAS facelift, neck lift, lower blepharoplasty, and 50 cc of fat injections. Note youthful, soft, healthy, sensual appearance not obtainable with facelift alone. Note also that atrophy is typically a pan-facial occurrence and that fat grafting multiple sites are usually required if a balanced and harmonious rejuvenation and optimal improvement is to be obtained.
Sequencing Fat Injections with Other Procedures
There is a growing consensus that if a facelift is being concurrently performed it is best to inject fat at the beginning of the procedure before the facelift itself is begun. The reasons for this include that it is easier to harvest the fat at the beginning of the procedure before the face has been prepped or draped and when the patient is typically in a deeper plane of anesthesia. In the beginning of the procedure, the tissue planes of the face have also not been opened, the face is not swollen, and preoperatively made pen marks and facial landmarks are easier to identify. In addition, surgical principles suggest that it is best to limit the time the graft is out of the body. But perhaps the most important reason to inject the fat first is that the surgeon is technically and artistically energetic at the beginning of the procedure. If one waits until the end of a long facelift, fat grafting will be performed with less patience and care.
Facelift and Fat Grafting—How
The technique for fat grafting has been described previously [1,2,3,4], and the general principles set forth by Coleman are observed when fat grafting is performed.
Fat grafting is often mistakenly regarded as a simple procedure that can be performed in a few minutes time, and this misguided perception is one of the major impediments to success that the surgeon trying to learn the procedure will encounter. This is rarely the case, however, and such an approach will lead to frustration, disruption of workflow, and poor outcomes. For the procedure to be successful, fat must be harvested in a specific gentle, atraumatic, time-consuming manner, and it must then be processed and infiltrated in a technically and artistically demanding and time-consuming process. When anything other than a few small areas of the face are being treated the entire procedure can easily encompass an hour or more, something that can overburden a surgical team already engaged in a long and demanding facelift operation consisting of multiple procedures. Time must therefore be planned appropriately.
Fat Grafting Equipment
Special instruments are required for fat harvest and injection, in addition to a few other pieces of equipment to process the fat if optimal outcomes are to be obtained. If sharp hypodermic needles are used to inject fat (other than intradermally), fat embolization and serious related problems, including tissue infarction and visual impairment and blindness, can occur, and their use is not recommended. As such, equipment used must be considered as a variable influencing outcome when review of published data is undertaken.
Donor Site Selection
Because there is currently no scientific consensus as to what are optimal donor sites to harvest fat from for fat grafting procedures, harvest sites are typically chosen and marked in our practices in conjunction with the patient in such a manner as to improve her or his silhouette. For women, this is typically the hip, outer thigh, or abdomen, and for men the “love handle” and “spare tire” areas.
In thin patients, small harvests from multiple areas are typically required, including the inner thighs, inner knees, upper buttocks, and anterior axilla, and this will add additional time to the procedure. While not specifically addressed in the Shue et al. review, body habitus (thin vs heavy patient) is in many surgeons’ experience considered to effect outcomes and must be considered as clinically significant variable influencing outcomes in future reviews of published data.
Preoperative Marking the Face
Fat grafting cannot be performed arbitrarily or based on the patient’s appearance while supine in the operating room, and facial landmarks that serve as important reference points in performing the procedure must be marked preoperatively with the patient in an upright position. Creating an initial plan on a life-sized laser print of a photograph of the patient’s face is helpful in organizing one’s thoughts, and facilitates discussions with the patient as to which areas will be treated. Once markings are complete, additional photographs of the marked face are taken and printed up for use during the procedure. Proper and improper marking of patients will influence outcomes.
Anesthesia
Most modern facelifts are time-consuming and technically demanding, and the addition of fat grafting to the procedure can strain the patience and composure of most any surgeon, and the ability of the patient to comfortably tolerate the event. As such, it is highly recommended that one enlist the services of an anesthesiologist or competent CRNA when combined facelift and fat grafting procedures are performed. Patient comfort or discomfort during the procedure is likely to affect outcomes.
The majority of our facelifts are now performed under deep sedation administered by an anesthesiologist using a laryngeal mask airway (“LMA”). This allows the patient to be heavily sedated without compromise of their airway, but the patient need not receive muscle relaxants and can be allowed to breathe spontaneously. The heavily sedated patient is also easier to harvest fat from, especially when fat must be harvested from multiple sites. Comprehensive treatment of the face with fat is also facilitated under these conditions.
Nerve blocks are then performed with 0.25% bupivacaine with epinephrine 1:200,000 local anesthetic solution, and an adequate time allowed for a proper anesthetic and hemostatic effect. It is not necessary to directly infiltrate areas of the face to be fat grafted with local anesthetic in the facelift patient if nerve blocks are performed correctly and sedation has been administered, and fat is typically infiltrated into “dry” recipient areas. At this time, it is unclear whether local anesthetic solutions and epinephrine have a deleterious effect on fat survival or not.
Harvesting Fat
Areas marked for fat harvest are infiltrated with 0.1% lidocaine with 1:1,000,000 epinephrine solution using a multi-holed 1.6-mm, 20-cm-long local anesthetic infiltration cannula, and an adequate time allowed for a proper anesthetic and hemostatic effect. Approximately 1 cc of dilute local anesthetic solution is injected of every 3 cc of anticipated fat removal. It is not necessary or desirable to infiltrate in a “tumescent” fashion as over-wetting the harvest site will result in an over-dilute harvest and more time being spent in the harvesting process. Local anesthetic should be injected even if general anesthetic is used.
Fat is then harvested with a special 2.1–2.4-mm “Coleman,” “Carraway,” or “Tri-port” harvesting cannula attached to a 10-cc syringe using gently applied syringe suction to avoid vacuum barotrauma to the tissue. Fat harvested with these cannulas will easily pass through 0.7-mm (20 ga) injection cannulas, and the use of a small harvesting cannula is not necessary and will slow down the harvesting process. Sharp hypodermic needles should not be used. In general, at least twice as much fat is harvested as is anticipated will be used to treat the face to insure an adequate supply of processed fat will be available for use on the face as centrifuging (see below) typically reduces the apparent harvest by 30 to 50%. How fat is harvested is likely to influence overall outcomes.
Processing Harvested Fat
Harvested fat is generally not uniform in character and concentration as extracted, and some type of processing is necessary to obtain homogeneous material (uniform number of fat cells per unit volume) for injection. Centrifugation as advocated by Coleman and practiced in our Clinic allows separation of the “oil” (fat cells ruptured during the harvest process) and “water” (blood and local anesthetic) fractions from the fat cells while simultaneously concentrating these other potentially important components (“platelet plug”). How fat is processed influences overall outcomes, and comparing 1 cc of centrifuged fat to 1 cc of un-centrifuged settled fat is an erroneous comparison.
Injecting Fat
After centrifugation and the oil and water fractions have been discarded, the fat is transferred into 1-cc Luer lock syringes using an anaerobic transfer coupling or other method, as proper infiltration of fat requires injection in very small aliquots that cannot be reliably made with a 10-cc, 5-cc, or even 3-cc syringe. Cannulas [0.7 mm (20 ga), 0.9 mm (19 ga), and 1.2 mm (18 ga)] are used to infiltrate fat into the face transcutaneously through small stab incisions depending on the areas being treated (see illustrations and figure that follow).
Infiltration is made in multiple passes in planes appropriate for the area being treated, injecting on both the in and out strokes usually from two separate injection sites, while feathering into adjacent areas. Injecting from at least two separate injection sites allows “crisscrossing” of cannula passes during graft placement and smoother fat infiltration and helps avert a “row of corn” effect that might result if injection was made from only one site. How fat is injected is likely to influence overall outcomes.
Determining How Much Fat to Inject
Unless one is willing to submit to a long process of trial and error, deciding upon how much fat needs to be injected at a given site requires empirical information provided by others who have experience with the procedure and one cannot simply rely on what one sees in the operating room. Shue et al. provide a very helpful review of information available on this subject. In general, there is a tendency to treat most areas too conservatively if amounts to be administered are decided by intuition and observation alone, and some “over-correction” is needed as not all the graft will survive. It is also the case that more fat will be needed than one would use to fill a similar defect with non-autologous filler.
A prudent strategy for determining the amount of fat needed for a given site is to rate the severity of the degree of atrophy for each region of the face based on what is seen in the preoperative photographs and then to use empirical published data to choose the amount to be administered to each area.
As a practical matter, this amounts to simply rating or categorizing the severity of atrophy at each proposed site of treatment as “small,” “medium,” and “large,” and then using data published regarding range of amounts typically needed as a guide for treatment of each area. If the defect is “small,” one would choose an amount from the low end of the recommended range. If the defect is “large,” one would choose an amount from the high end, and if “medium” somewhere in between. The authors’ recommended ranges for the technique described herein are given in tables and Figs. 3, 4, and 5.
Anatomic regions and summary of range of volumes typically used to treat each area. Amounts listed are for fat harvested with a 2.1–2.4-mm harvesting cannula centrifuged for 1–3 min at 1000 rpm administered to average-sized female head in 0.5-cc aliquots using 1-cc syringe and 0.7 mm (20 ga) to 1.2 mm (18 ga) cannulas as part of a facelift procedure. Larger amounts would be expected and may be required for un-centrifuged or “tea strained” fat, larger female faces, male patients, and patients not undergoing facelift procedures. The strategy for determining the amount of fat needed for a given site is to rate the severity of atrophy based on what is seen in the preoperative photographs at each proposed site of treatment as “small,” “medium,” and “large,” and then to use the data above to determine the amount typically needed for treatment of each area. If the defect is “small,” one would choose an amount from the low end of the recommended range. If the defect is “large,” one would choose an amount from the high end, and if “medium” somewhere in between.
The insightful surgeon can see that these parameters must be considered as guidelines and not absolutes and that considerations such as what equipment was used, how the fat was harvested, how it was processed, how it was injected, and the condition of the tissues receiving the fat will all influence amounts needed and eventual outcomes. Patients who are smokers or previous smokers and patients who have undergone previous noninvasive radiofrequency and ultrasonic “skin shrinking” procedures are likely to have compromised subdermal microcirculation and microlymphatics vessels and as such are less than optimal candidates for fat grafting and need more fat than those who do not. Similarly, patients who are longstanding filler users, especially if they have used inflammatory fillers such as PLLA, are likely to have internal facial fibrosis and inflammatory changes rendering them suboptimal candidates as well for fat grafting, and they exist as patients who will require that larger volumes be administered to obtain an equivalent result. Patients undergoing concomitant facelifts will typically require less fat than patients undergoing isolated fat grafting as their skin envelope is being reduced. It is also the case that the thoughtful injector must add a compensation for a large and small face and adjust the amounts administered accordingly.
Ultimately, however, the strategy outlined above, and in particular the range of recommended volumes to administer, serves as a time-tested starting point and one that will shorten the beginning injector’s learning curve, and serve as a point of reference from which one develops her or his own ranges with experience and over time. It should be understood that the volumes ranges recommended are not absolutes and are not a guarantee of success. Nonetheless, this strategy has proven very useful in our own practices over several decades of combined experience and is the strategy we currently employ today. Taken as such, the surgeon currently seeking to incorporate fat grafting into her or his facelift procedures has a significant head start over their predecessors who had to develop these guidelines largely through trial and error.
Technique of Injection
Approximately 0.05 cc or less should be injected per pass (back-and-forth movement of the cannula). This corresponds to 20 to 40 back-and-forth cannula movements or more to empty a 1-cc syringe of processed fat. The goal is to inject the fat in a way that scatters it in the plane and place of administration and optimizes its chance of developing a blood supply and surviving. The mental model should be one of scattering tiny particles of fat into the recipient site in multiple crisscrossing fine trails in such a way that each particle sits in its own compartment and has maximal surface contact with perfused tissue and minimum contact with other injected fat cells to the extent possible. If fat is injected in a bolus, fat cells will be clumped together and only those on the periphery of the injected area will have tissue contact and will be likely survive. The majority of the more centrally situated fat particles will only have contact with each other, will be less likely to survive, and can lead to the formation of oil cysts and contour irregularities.
Advancement and withdrawal (back-and-forth movement) of the injection cannula will typically be made too slowly by the beginning injector (in a "caulking" like motion), but as familiarity with the technique is acquired the movements can and should be made faster (in a "spray painting" like manner). Ultimately, all other things being equal, faster movements are desirable in that if the injection cannula is constantly in motion intravascular injection is less likely, and the likelihood that an accidental bolus injection into one area will be made is reduced. Rapid back-and-forth movements insure the smoothest and most uniform infiltration of fat.
How the syringe is held is also important in avoiding over-injection and controlling the volume injected with each pass. If the syringe is held in the manner one would traditionally use to give an injection with the thumb on the end of the syringe plunger, it is easy to inject too much fat if tissue or injection cannula resistance suddenly decreases. More control can generally be maintained, and over-injection more easily avoided, if the syringe is held with the end of the plunger in the palm of the hand (Fig. 6). Held in this manner, a slight closing of the hand results in a small amount of fat only being expressed from the cannula, and over-injection of any one area can more readily be avoided. Smaller cannulas now available also help avoid bolus injection as their small size physically limits how fast fat can be extruded from the syringe.
Method of holding syringe to control volume expressed during injection. If the syringe is held in the way one would traditionally use to give an injection, it is easy to infiltrate too much fat if tissue or injection cannula resistance suddenly decreases. More control can be maintained, and over-injection better avoided, if the syringe is held with the end of the plunger in the palm of the hand. Held in this manner, a slight closing of the hand results in a small amount of fat only being expressed.
How can Fat be Used to Make a Facelift Better? In What Plane Should Fat be Placed?
Fat grafts will necessarily be placed in different planes depending on the areas being treated and the problem present. In many areas where multiple tissue layers exist to inject in and overlying skin is thick, injection can be made comprehensively at the treated site from periosteum to the subdermal layer. These areas typically include the geniomandibular groove (“GMG” “pre-jowl groove”), piriform, mid-face, cheek, and the chin. In other areas, injections must necessarily be placed more specifically or deep due to the anatomical characteristics of the treated sites if optimal results are to be obtained and irregularities are to be avoided. These areas include the temples which are injected subcutaneously, the upper orbit, lower orbit, and “tear trough” which should be injected in a pre-periosteal/sub-orbicularis oculi deep plane, the lips which should be injected predominantly in a submucosal plane, and the jawline which should be injected in a pre-periosteal/sub-masseteric plane of the face of the mandible. The easiest areas for the beginning injector to treat are the sites in the former category. And in the beginning, it is wise to “stay deep” and place the majority of the graft in a predominantly pre-periosteal plane. Once familiarity with the technique has been obtained, areas in the latter categories can then cautiously be treated.
The “look” the surgeon is after is also germane to depth of fat placement. In general, if one is looking to enhance the facial skeleton in the way one would with a facial implant, injections should arguably be made more deeply and near facial bone. If one is seeking more of an appearance of softness and youthful glow, at least some of the fat should be placed superficially and closer to skin if the characteristics of the recipient site allow for that.
Particulars of Sites of Treatment
Geniomandibular (“pre-jowl”) Groove (“GMG”)
Grafting of the pre-jowl/geniomandibular groove area with fat has a high esthetic payoff and is a good area for the beginning injector to gain experience with the technique (Figs. 7, 8). Filling the GMG creates a strong, uninterrupted esthetic line from chin to the posterior mandible, that cannot be achieved by lifting the jowl alone, and results in a highly desirable improvement on both the male and female face.

Procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery
Treatment of the geniomandibular groove (“GMG”) with fat injections. a Patient with deep geniomandibular groove seen preoperatively. The chin appears narrow and pointed, and there is poor continuity between the chin and jawline. b Same patient seen after facelift and injection of fat to fill the geniomandibular groove (“pre-jowl” sulcus) area. A chin implant was not placed. The chin appears broader and more esthetically integrated with the jawline. Fat was also used to strengthen the posterior jawline, lower the mandibular angle, and fill the lips, nasolabial crease, cheeks, and infra-orbital areas.
Incision sites and plan for injecting fat into the “pre-jowl”/geniomandibular groove (“GMG”) areas. Fat grafting of the pre-jowl/GMG area is performed with a 4-cm, 0.7-mm (20 ga) cannula, and fat is placed in all tissue layers between the periosteum and skin. Typically, 1–3 cc of fat is placed on each side. Level of difficulty: beginner.
Cheek
Injecting the cheek with fat can correct age-associated loss of cheek volume, improve cheek projection, and rival or even exceed the kind of improvements obtained when cheek implants are placed (Figs. 1, 2, 9, 10—see also case studies 1–3). This is because fat grafting often results in a softer more natural appearing, integrated cheek mass than cheek implants which can produce a harder and more harsh appearance. Often an asymmetrical placement of fat will be required when fat grafting the cheeks due to the common occurrence of malar asymmetry seen preoperatively in many patients.

Procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery
Enhancing the cheeks with fat. As the cheek atrophies the lower eyelid fat “bags” become more exposed and prominent. Removing lower eyelid fat would create a hollow and elderly appearance and could result in lower eyelid retraction. a Patient with atrophic cheek. The lower lid fat is exposed and appears ostensibly as a “bag.” (“pseudoblepharochalasis”) b Same patient seen after fat injections to the cheeks but no blepharoplasty. Protruding lower eyelid fat has been disguised by building up the cheek. This produces a more youthful, fit, and attractive appearance than removing lower lid fat would have (Note the upper orbit has been replenished with fat grafts as well).
Incision sites and plan for injecting fat into the cheek area. Fat grafting of the cheeks is typically performed with a 5-cm, 0.7-mm (20 ga) cannula, and fat is placed in all tissue layers between the periosteum and skin in most cases. Typically, 3–7 cc of fat is placed in each check. Level of difficulty: beginner.
Chin
Injection of the chin with fat can correct age-associated loss of chin volume, improve chin projection, increase vertical chin height, and rival the kind of improvements obtained when small chin implants are placed (Figs. 11, 12).

Secondary procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery
Using fat injections to project the chin. a Patient with under-projected chin seen before secondary facelift and fat injections (previous procedure performed by unknown surgeon). b Same patient seen after secondary facelift with fat injections to the chin. A chin implant was not placed. Injection of the chin with fat can enhance a patient’s profile and approach the kind of improvements obtained when small chin implants are placed as shown. Fat was also placed in the upper and lower orbits, cheeks, lips, and jawline areas.
Fat grafting of the chin can also correct an atrophic and feeble appearance that occurs as the chin shrinks with age by broadening and strengthening it (Figs. 12, 13), and filling in the labiomental sulcus and the sub-mental crease when indicated. The ability to modify and fill the labiomental sulcus is a distinct advantage of fat grafting over a chin implant. Typically, treatment of the chin must be undertaken in conjunction with the GMG, and the two areas will overlap each other in most cases. Overfilling the chin can produce excessive vertical height and an objectionable globular appearance.
Incision sites and plan for injecting fat into the chin. Fat grafting of the chin is typically performed with a 4-cm, 0.7-mm (20 ga) cannula, and fat is placed in all tissue layers between the periosteum and skin. Typically, 1–3 cc of fat is placed in each side of the chin. Level of difficulty: intermediate.

Procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery
Using fat injections to strengthen the aging chin. a Preoperative view of patient with atrophic and feeble appearing deflated chin. b Same patient seen after secondary facelift and fat injections to the chin, geniomandibular groove (“pre-jowl” sulcus), and jawline areas. A chin implant was not placed. The atrophic and feeble appearance was corrected with fat injections by broadening and strengthening the chin. Treatment of the chin along with the geniomandibular groove and jawline areas allows for strengthening of the entire lower facial contour.
Nasolabial Injection
One of the first areas most patients inquire about when considering fat injections, and most surgeons are eager to treat, is the nasolabial crease areas. Nonetheless, one must be aware of several misconceptions and certain limitations of the fat grafting technique in regard to the treatment of this area. The first is that treatment of the nasolabial creases with fat is generally not as effective as treatment with non-autologous fillers. Fat is softer and typically placed more deeply than non-autologous fillers, and fat is better used to treat a volume deficiency in a region of the face as opposed to a more discrete line, wrinkle, or fold that is subject to the repeated stress of facial muscle contraction and facial movement. Patients undergoing fat injections solely for treatment of their nasolabial folds will generally be disappointed with the outcome. This is not the case, however, when a simultaneous facelift is performed and cheek and mid-face tissues are repositioned and redundant cheek skin is excised. Fat is an excellent adjunct in the treatment of the nasolabial fold in such instances (see Figs. 14, 15). It is also not immediately and intuitively obvious, but increasingly more widely appreciated by those injecting non-autologous fillers into the face, that filling the upper mid cheek produces a profoundly beneficial effect on the nasolabial fold by integrating it with the rest of the face, and that treatment of the fold is more effective when combined filling of both these areas is made. If the cheek is filled, less fat is needed to improve the nasolabial fold, and an overall better result will be obtained.

Procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery
Combined lifting and filling of the nasolabial fold. a Patient with mid-face ptosis and heavy nasolabial fold. b Same patient seen after high-SMAS facelift and fat injections to the nasolabial creases. A combined lifting and filling provides a better improvement than either procedure performed alone.
Incision sites and plan for injecting fat into the piriform and nasolabial crease area. Fat grafting of the piriform and nasolabial crease is typically performed with a 4-cm, 0.7-mm (20 ga) cannula. Fat is placed subcutaneously and superficially if treatment of the nasolabial skin crease is being made. Fat is placed pre-periosteally if improvement in age-associated maxillary recession is indicated and desired. Fat is placed in all tissue layers between the periosteum and skin if both problems are present and are being treated. Typically, 1–1.5 cc of fat is placed on each side. Level of difficulty: intermediate.
It is now generally accepted that the nasolabial crease is also due, at lease in part, to age-related loss of maxillary projection and the goal in injecting fat in the nasolabial areas should be thought of at least partly as augmentation and restoration of maxillary/mid-face projection than as simple filling of the soft tissue crease. As such, the surgeon’s effort and how and where fat is injected will depend on the problem present. Injections should be made more superficially and predominantly subcutaneously if the one is treating the nasolabial crease. Injections should be placed more deeply and predominantly over the piriform in the upper nasolabial area if one is treating age-associated maxillary recession. Many patients are best served by treatment of both areas.
Overfilling the nasolabial area is a common eventual outcome of the frustration one will feel if the nasolabial crease is treated with fat in isolation and in the same way one would inject non-autologous fillers. Higher and higher volumes will be tried in a futile effort to efface the crease, but an improved outcome will not be obtained when these larger amounts of fat are injected. Instead, an abnormally heavy and objectionable appearing unesthetic fullness of the mid-face is generally obtained. In addition, overfilling the nasolabial area can produce changes in the posture of the patient’s mouth, the shape of their smile, and result in a change in their “look.” For these reasons, it is important to advise patients accordingly, for the surgeon to set reasonable goals, and to limit the amount of fat placed in the nasolabial area to a reasonable amount.
Lips
Perhaps no better example exists than the lips of the precedence of shape and contour over a simple increase in volume. The real measure of success is whether the treated area has a healthy, fit, youthful, and sensual appearance—not simply whether it is larger or not.
Despite the fact that patients and injectors are often erroneously focused on the upper lip, the lower lip in the youthful mouth will be seen to be distinctly bigger than the upper lip, and in most cases, the priority in rejuvenation of the oral area is to restore lost lower lip volume. This fact can easily be confirmed by having patients bring in photographs of themselves at a younger age and a useful esthetic goal is to restore the relationship of the upper and lower lips to a “Golden Proportion.” Overfilling the upper lip, or making the upper and lower lips the same size will result in an unnatural “punched in the mouth” appearance.
Treating the lips with fat has distinct advantages and disadvantages. The advantages include that fat is autologous and if the procedure is successful and graft “take” is good, patients will be spared the inconvenience and discomfort of having to undergo repeated filler treatments. Fat also produces a soft, natural appearing improvement, and usually slight under-correction, that we find to be most appropriate for the typical facelift patient in need of some improvement in her or his mouth (Figs. 16, 17, 18).

Reprinted with permission of the procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery
Enhancement of lip volume with fat injections. Fat grafting the lips produces a soft, natural appearing improvement in lip appearance and slight under-correction that is appropriate for the typical facelift patient in need of enhanced lip volume. Non-autologous fillers invite over-correction and tend to produce a more stylized “stung by a bee” lip appearance. a Peri-oral area of a facelift patient seen before fat injections. Note upper and lower lips appear approximately the same size. b Same patient seen after facelift that included fat grafting of the lips. The lips are fuller and healthier appearing, but soft and natural looking. Note that the lower lip is distinctly larger than the upper lip and that fat has been placed to produce a natural, sensual shape.
Incision sites and plan for injecting fat into the upper and lower lip areas. Fat grafting of the lips is performed with a 5-cm, 0.7-mm (20 ga) cannula, and fat is placed submucosally beneath the vermillion and subdermally in the “white roll” areas (see Fig. 19). Typically, a total of 1–1.5 cc is placed in each side of the upper lip and 1.5–2 cc is placed in each side of the lower lip. Level of difficulty: intermediate.

Procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery
Combined peri-oral resurfacing and fat injections. a Patient seen preoperatively with wrinkled, atrophic peri-oral area that lends an elderly, unhealthy, and objectionable appearance to the face. Note flat, un-projected appearance of mouth area. b Same patient seen 2 years and 7 months after high-SMAS facelift that included combined peri-oral fat injections and peri-oral dermabrasion. Both atrophy and wrinkling have been improved, and the mouth as a more youthful, vibrant, and healthy appearance. The combined treatment produced a better appearance than either procedure performed alone.
Fat injections to the lips have the distinct disadvantage that they usually produce a “monstrous” amount of swelling that is slow to resolve, and that the “take” of the graft varies from patient to patient. Patients seeking a quick recovery, a specific lip size or shape, a full stylized lip appearance, or nuanced changes are not optimal candidates for the procedure. These appearances are better obtained using non-autologous fillers, and patients seeking such appearances should be advised accordingly.
Typically, the first few passes of the cannula are used to place fat subcutaneously/submucosally directly under the vermillion–cutaneous junction, then under the “red roll,” and then under the “white roll.” Fat is then infiltrated submucosally beneath the wet and dry lip vermillion in a way that optimizes lip shape (Fig. 19). Movements must be made more slowly when treating the lips compared to other areas of the face.
Strategy for fat grafting the lips. The natural and attractive appearing upper lip has one central tubercle and two lateral tubercles with a sulcus on each side between them. The lower lip should have a central sulcus with a tubercle on each side of it. Fat should be injected in a manner to duplicate these appearances and not simply to make the mouth larger or to create “sausage-shaped” lips. To create a youthful and sensual appearance, and to optimize treatment of peri-oral wrinkling, fat must also be placed superficially under the vermillion–cutaneous junction as shown.
When injecting the peri-oral area care must be taken to not overfill the white upper lip in the name of wrinkle reduction as the patient’s upper lip can be lengthened, dental show can be reduced, and an abnormal convex “simian” contour in profile can result. A better strategy is to concentrate ones efforts on and near the “white roll” area where the wrinkles are typically the deepest and most objectionable appearing (Fig. 18). Results are further enhanced by injecting additional fat at the columellar–labial angle, as this helps restore a youthful transition from the nose to the lip and helps create a concave upper lip shape.
Jawline
Fat grafting of the jawline border area can enhance a patient’s facial shape and produce the kind of improvements obtained when mandibular border and “Taylor” style mandibular angle implants are placed (Figs. 20, 21).

Reprinted with permission of the procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery
Using fat injections to enhance mandibular contour and strengthen the jawline. a Patient seen before surgery with small mandible, narrow intergonial distance, and lower facial disproportion. b Same patient after high-SMAS facelift and pan-facial fat injections including lips, chin, GMG, and the jawline. No implants have been placed. Strengthening the jawline and posterior mandibular border results in a more fit and proportionate appearance and helps avert the tight and deficient mandibular contour typically seen in the elderly face after a facelift is performed.
Incision sites and plan for injecting fat into the posterior jawline. Fat grafting of the jawline is usually performed with an 8-cm, 1.2-mm (18 ga) cannula, and fat is placed in a pre-periosteal/sub-masseteric muscle position. Typically, 3–6 cc of fat is placed in each side. Note that fat is not injected subcutaneously, into the parotid, or into the masseter muscle. Level of difficulty: intermediate.
Fat injections along the mandible can also correct an atrophic and feeble appearance that occurs as the mandibular border shrinks with age by broadening and strengthening it. Typically, treatment of the jawline must be undertaken in conjunction with the GMG and the two areas will overlap each other in most cases.
Note that when treating the jawline fat is injected in a sub-masseteric/pre-periosteal plane and not injected subcutaneously, into the parotid, or into the masseter muscle.
Although not intuitively obvious, strengthening the jawline and posterior mandibular border when indicated makes one appear more youthful, fit, and attractive and is an artistically powerful adjunct to a facelift that helps avert the scrawny, deficient, and fragile mandibular contour typically seen in the aging and elderly face that is usually made worse when a facelift is performed (see case studies 1–3).
Fat grafting the jawline is particularly useful in the in the secondary facelift patient and in the patient with a “long face” seeking facial rejuvenation or improvement. Typically, the secondary facelift patient has experienced significant loss of jawline volume due to loss of, or inappropriate surgical removal of, facial fat, and this is typically compounded by over-zealous tightening of overlying tissues. These appearances are readily reversed with jawline fat grafting, and fat grafting this area comprises an important part of many of our treatment plans for our secondary and tertiary facelift patients.
Temple Area
Temporal hollowing is consistently seen in the fifth decade of life and beyond and can be readily improved with fat grafting (Figs. 22, 23).

Procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery
Filling of the temple hollow with fat. Temporal hollowing is a consistent marker of the fourth decade of life that can be readily improved with fat injections. a Patient age 45 before surgery has marked temporal hollowing. b Same patient 2 years and 4 months after high-SMAS facelift and fat injection to the temple region (Note fat has also been injected in the upper and lower orbital areas and the cheek).
Incision sites and plan for injecting fat into the temple areas. Fat grafting of the temples is performed with a 5-cm, 0.9-mm (19 ga) cannula, and fat is placed in a subcutaneous plane. Typically, 3–7 cc of fat is placed on each side. Level of difficulty: intermediate.
The temple areas are usually grafted in a subcutaneous plane from small stab incisions just within the temporal hairline (Fig. 23).
In most cases, a slightly bigger and blunter 0.9-mm (19 ga) (6 cm long) injection cannula is superior to sharper and smaller types preferred elsewhere. Using slightly larger cannulas helps minimize perforation of temporal veins predictably present in the temporal area and allows fat to be placed over and around them to conceal them.
The injection cannula is not inserted specifically above or below the veins but allowed to pass subcutaneously into the plane of least resistance in the temporal area. Should a temporal vein be accidentally penetrated during injection and swelling from the leakage of venous blood noted, it is a simple matter to hold pressure on the temporal area with a surgical sponge. Typically, after applying pressure for a few minutes bleeding stops and treatment of the area can be completed.
Buccal Recess Area
Buccal atrophy is frequently present in the fourth decade of life and beyond in patients and can be readily improved with fat grafting, as can buccal hollowing due to previous over-zealous excision of buccal fat or resulting from ill-conceived facial liposuction (Figs 24, 25).

Procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery
Correction of buccal atrophy and over-excision of buccal fat. Buccal fat excision is often erroneously recommended as a way of creating a “high cheekbone” and more angular facial appearance. In reality, it often produces an ill, haggard, gaunt, and unfeminine appearance, especially when performed aggressively. a Patient with buccal hollowing following buccal fat excision by an unknown surgeon. b Same patient 11 months after fat injections to the buccal area. Note fat has also been placed in the infra-orbital, mid-face, cheek, pre-oral, and jawline areas.
Incision sites and plan for injecting fat into the buccal hollows. Fat grafting of the buccal hollow is typically performed with a 4-cm, 0.7-mm (20 ga) cannula, and fat is placed subcutaneously and in sub-SMAS (buccal space) locations in most cases. Typically, 1–3 cc of fat is placed in each side. Level of difficulty: intermediate.
Upper Orbit/“Upper Eyelid” Area
Whether the result of illness, aging, or previous over-zealous surgical treatment, filling the hollow upper orbit can produce a remarkable rejuvenation of the upper eyelid and eliminate an unnaturally hollow and elderly appearance sometimes referred to by patients as “nursing home” or “owl” eyes (Figs. 26, 27, see also Fig. 6).

Procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery
Correcting upper orbital hollowing. a Patient with hollow upper eyelid an unnaturally hollow ocular appearance (“owl eyes”) following blepharoplasty performed by an unknown surgeon. b Same patient seen after fat injections to the upper orbit. A healthier, more youthful appearance can be seen.
Incision sites and plan for injecting fat into the upper orbital (“upper eyelid”) area. Fat grafting of the upper orbital area is typically performed with a 4-cm, 0.7-mm (20 ga) cannula, and fat is placed deep in a sub-orbicularis oculi/pre-periosteal plane. Typically, 1–3 cc of fat is placed in each upper orbit. Level of difficulty: advanced.
Where fat should be placed in the upper orbit (“upper eyelid”) is a subject of debate, but for all but the expert injector it is safest to avoid sub-septal and subcutaneous injections and limit injections to a pre-periosteal/sub-orbicularis oculi plane. A common misconception in treating the hollow upper orbit is that the fat is needed and should be injected into the pre-septal portion of the eyelid itself. The hollow upper eyelid is more properly and practically restored by placing fat along the inferior margin of the supra-orbital rim, and the process is best conceptualized as one of lowering the supra-orbital rim and filling the upper orbital area to lower skin that has retracted up into the orbit down onto the pre-septal eyelid to create a full and appropriately creased upper eyelid. Once one accepts that improvement is obtained by grafting of the orbit, and not the eyelid itself, it becomes apparent that larger volumes than might otherwise be expected are required. Smaller injection cannulas now available have made injecting the upper orbit easier and more predictable than in the past as they can be advanced more smoothly and accurately through tissues and allow the deposition of very tine aliquots of fat per pass, and it is highly recommended that small cannulas be used to treat this area.
When grafting the upper orbit, it must always be remembered that when one is working in very close proximity to the eye, and although the injection cannulas are blunt tipped, they are easily capable of perforating the ocular globe.
Fat grafting the upper orbit and “eyelid” is advanced in difficulty, and treatment of this area should be made after experience has been gained treating more forgiving areas. Once that experience is obtained, fat grafting the upper orbit can be one of the most artistically rewarding uses of autologous fat, and one that is likely to become a routine part of rejuvenating the upper eyelid in the future.
Lower Orbit/“Lower Eyelid” Area
Injecting the infra-orbital (“lower eyelid”) area has a high artistic payoff if the procedure is carried out carefully and correctly and will likely change the way all surgeons approach the aging lower eyelid (Figs. 28, 29).

Procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery
Filling the hollow lower orbit with fat. a Patient with hollow lower eyelid an unnaturally hollow and elderly infra-orbital appearance. The lower eyelid appears “long,” and there is a distinct line of demarcation between the lower eyelid and the cheek. b Same patient seen after facelift and fat injections to the infra-orbital area. There is a smooth transition form the lower eyelid to the cheek, and the patient has a more healthy, youthful, and attractive appearance (Note the upper orbit, radix, cheek, and nasolabial crease have also been treated with fat injections and the patient has undergone ptosis correction).
Correct (a) and incorrect (b) plan for injecting fat into infra-orbital (“lower eyelid”) area. Fat grafting of the infra-orbital area is typically performed with a 4-cm, 0.7-mm (20 ga) cannula and fat is placed deep in a sub-orbicularis oculi/pre-periosteal plane. Typically, 1–3 cc of fat is placed on each side. A smoother effect is obtained, and a “banana” or “sausage” (unesthetic bulge) is less likely when fat is injected perpendicular (a) rather than parallel (b) to the infra-orbital rim. Level of difficulty: advanced.
Fat grafting the infra-orbital area allows comprehensive correction of age-associated hollowness that lends the face and ill or haggard appearance, “shortens” the apparent length of the lower eyelid, and produces an youthful, attractive, and highly desirable smooth transition from the lower eyelid to the cheek that is generally unobtainable by traditional lower eyelid surgery, fat transpositions, “septal resets” mid-face lifts, free fat grafts, and other like means. As is the case in treating the upper orbit, fat need not and should not be grafted in the pre-tarsal lower eyelid. Fat should be injected deep in a sub-muscular/pre-periosteal plane while protecting the ocular globe with the index finger of one’s non-dominant hand on the infra-orbital rim, and the goal of the procedure should be thought of as raising up and anteriorly projecting the infra-orbital rim rather that filling the lid itself. Experience has shown that, unlike the upper orbit, fat is best injected into the infra-orbital area perpendicular to the infra-orbital rim, and when this is done lumps and irregularities are far less common. Fat should not be injected parallel to the lid–cheek junction in the infra-orbital area.
It is wise to avoid any subcutaneous injection in the infra-orbital area due to the extremely thin skin present and the likelihood of creating visible lumps and irregularities and to limit injections to a pre-periosteal/sub-orbicularis oculi plane.
“Tear Trough”
Where the infra-orbital area ends and the “tear trough” and cheek areas begin is hard to define and in reality, the treatment of the infra-orbital, cheek, and “tear trough” areas must be undertaken concurrently in most patients, and the treated areas will overlap each other to a certain extent. In addition, it must always be remembered that the ultimate goal of the procedure is creating youthful and attractive contour, not simply filling a specific area. Fat grafting the tear trough (Figs. 30, 31) is simpler and faster than fat transposition, septal reset, and similar procedures, and we have largely abandoned the latter procedures.

Procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery
Filling the “Tear Trough” with fat. a Patient with hollow nasojugal groove (“tear trough”) an unnaturally hollow and elderly infra-orbital appearance. b Same patient seen after fat injections. A more healthy and youth ocular appearance is noted.
Correct (a) and incorrect (b) plan for injecting fat into the nasojugal (“tear trough”) areas. Fat grafting of the nasojugal “tear trough” area is typically performed with a 4-cm, 0.7-mm (20 ga) injection cannula, and fat is placed deep in a pre-periosteal/sub-orbicularis oculi plane. Typically, 0.5–1.5 cc of fat is placed on each side depending on how far inferiorly and laterally the “tear trough” extends onto the cheek. A smoother effect is obtained, and a “sausage” (unesthetic bulge) less likely when fat is injected perpendicular (a) rather than parallel (b) to the defect. Level of difficulty: advanced.
Final Touches
Fat grafting is continued until the preoperatively determined volume of fat has been added to each target area. Treated areas are then gently palpated after they are injected to insure that the fat has been distributed smoothly in the target tissue, and any lumps or irregularities are gently pressed out. The lips, labiomandibular groove, and nasolabial areas can be bi-digitally palpated and molded by inserting a gloved finger inside the mouth, and if the orbits have been treated the ocular globe should be gently depressed and irregularities checked for in the orbital area.
Documenting What was Done
A non-scrubbed member of the operating room team should keep a detailed record of areas treated and amounts of fat injected in each, and a “Fat Injection Treatment Record” is useful for this purpose (Fig. 32—form). Tracking what was done at each procedure is essential assessing outcomes and improving one’s technique. Alternatively, amounts injected can be recorded on laser print photograph of the patients face.
Completion of Concurrently Planned Procedures
Once fat grafting is complete, attention is turned to the face, neck, forehead, upper blepharoplasty, lower blepharoplasty, peri-oral resurfacing, and other planned procedures are performed, as indicated. Because the majority of fat is needed and will be grafted in the anterior face and other areas that do not overlap the areas dissected in these other procedures, performing them after fat in injected does not interfere with carrying them out, or compromise the final outcome of the procedure. Fat placed in areas that are dissected as part of the facelift will be seen to adhere where it has been injected and not be disrupted partly due to the fact that if properly infiltrated the tissue has been saturated with it and it has not been injected in boluses of clumps, and partly due to “tissue glue” naturally secreted as a result of the infiltration process.
Postoperative Care
Patients are asked to rest quietly and apply cool compresses to their eyes and other treated areas for 15–20 min of every hour they are awake for the first 3 days after surgery, or use a commercially available thermostatically regulated water-cooled mask (AqueCool Mask - www.aqueductmedical.com San Francisco). For most patients, edema peaks at about this time. Patients are advised not to place ice or ice-cold compresses on their face as this is likely to be injurious to grafted fat and to compromise outcomes.
Patients are advised to take a soft, easy to chew and digest diet after surgery are encouraged to feed frequently on liquid and light carbohydrates foodstuffs for 2 weeks. Poor dietary intake, or intentional dieting after fat grafting procedures, is likely to put metabolic stain on grafted fat and compromise outcomes.
Case Examples
Patient Example 1
-
(a)
Before surgery view of a woman, age 45. Note overall facial laxity and pan-facial atrophy. The patient has had no previous plastic surgery.
-
(b)
Same patient, 2 years and 4 months after high-SMAS facelift [6,7,8], neck lift, closed forehead lift, lower eyelift, and fat transfer to the temples, cheeks, lips, nasolabial, geniomandibular groove, labiomandibular grooves, and upper and lower eye lid areas (see Fig. 2 for diagram fat placement). A total of 50 cc of fat has placed. Note soft, natural facial contours and the absence of a tight, pulled, or “face lifted” appearance. Facial atrophy has also been simultaneously corrected, and the patient has a healthier, more youthful, and feminine appearance. The combined facelift and fat injection procedures have produced a result that could arguably not be obtained by either procedure alone. Procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery

Patient Example 2
-
(a)
Before surgery view a man, age 68. The patient has sagging cheeks, deep cheek folds, and jowls. Loss of facial volume is also evident in the cheeks, infra-orbital, peri-oral, and geniomandibular groove areas.

-
(b)
Same patient, 1 year and 9 months after high-SMAS facelift [6,7,8], neck lift, closed forehead lift, upper and lower eye lifts, partial facial fat injections, and ear lobe reduction. A total of 28 cc of fat was placed. Note restoration of youthful and masculine facial shape without a tight or pulled appearance. Facial atrophy has also been simultaneously corrected, and the patient has a healthier, more youthful, and masculine appearance. Note fuller cheeks and stronger, more athletic appearing posterior jaw line. The combined facelift and fat injection procedures have produced a result that could arguably not be obtained by either procedure alone. Procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery
Patient Example 3
-
(a)
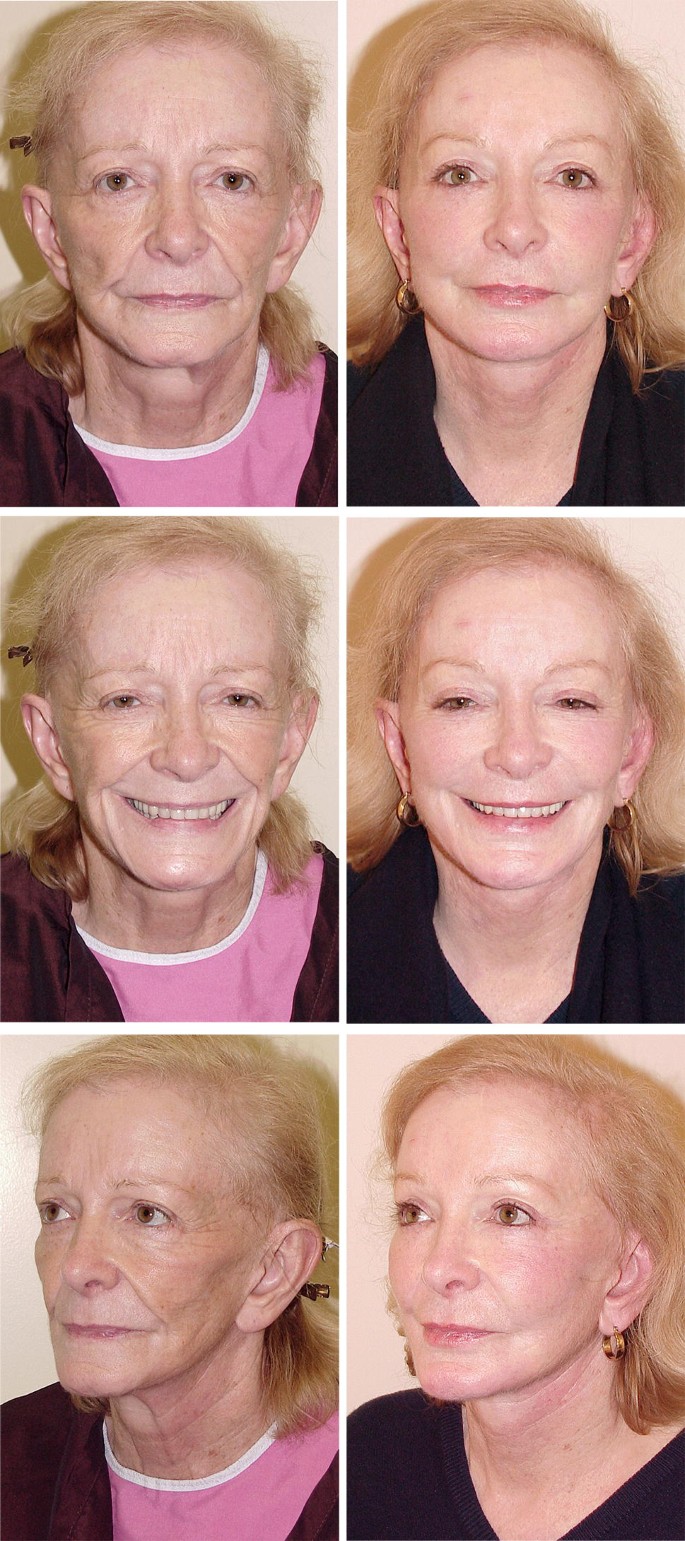
Preoperative view of a woman, age 75, who has had multiple prior facelifts and related procedures including previous laser resurfacing performed by unknown plastic surgeons. Note marked cheek laxity despite prior surgeries, and fragile, elderly appearance due to uncorrected pan-facial atrophy. Another facelift would predictably produce a gaunt, haggard or even ill appearance [5].
-
(b)
Same patient, 1 year and 7 months after high-SMAS facelift [6,7,8], neck lift, forehead lift, upper and lower eyelifts, canthopexy, and fat transfer to the temples, cheeks, mid-face, upper and lower eyelids, lips, nasolabial creases, labiomandibular grooves, geniomandibular grooves, chin, and jaw line. A total of 90 cc of fat was placed simultaneously with the facelift and related procedures. No skin resurfacing, facial implants, or other ancillary procedures were performed. In these situations, fat injections are arguably more important to the overall outcome than the facelift itself. Facial contour has been significantly enhanced, and facial volume restored. The patient has healthy, fit, and feminine appearance, and one that could not be obtained by either procedure performed alone. Procedure performed by Timothy Marten, MD, FACS – reprinted with permission of the Marten Clinic of Plastic Surgery
Summary
Despite what we thought in the past, “lifting” cannot correct all aspects of the aging change in the face and fat grafting allows treatment of age-associated loss of facial volume not addressed by face lift surgery. Fat grafting comprises the “missing link” in facial rejuvenation, and it stands as the most important new addition to facelift surgery since the introduction of the SMAS technique.
Abundant clinical and scientific evidence exists, confirming that fat grafting produces a persistent and worthwhile improvement. Fat grafting works best when sagging tissues have been repositioned and redundant skin excised and simultaneous facelift and fat grafting will provide a better result than either technique performed alone.
Fat grafting is an artistically powerful adjunct to a facelift that results in a more healthy, fit, youthful, sculptural, and sensual appearance than facelift alone. Patient and surgeon pre-occupation with the swollen face stand as evidence that volume addition has artistic merit. Fat grafting may be functionally important in the facelift patient and provide support to the lower eyelid and other facial tissues. Patients with full faces often have regional atrophy and can benefit from fat grafting. In many instances, fat grafting can replace or preclude the need for facial implants and adding fat grafting to a facelift procedure essentially provides the opportunity to perform simultaneously and at a much reduced cost the equivalent of a chin implant, pre-jowl groove implant, malar implant, sub-malar implant, jawline (Taylor) implant, “tear trough” implant, and temple implant.
Incorporating fat grafting into facial rejuvenation procedures is arguably more important that what facelift technique is used. Fat grafting may result in an improvement in skin quality mediated through a stem cell effect, and effect not only evident on the face but on the dorsum of the hands, the décolletage, and the neck. Fat grafting is often more important to rejuvenating the secondary facelift patient than the facelift itself. These benefits may offset the drawbacks of increased operating time, uncertainty of graft take, and a longer period of recovery associated with the fat grafting procedure.
References
Marten T, Elyassnia D (2018) Simultaneous facelift and fat grafting. In: Coleman S, Mazzola R, Pu L (eds) Fat injection—from filling to regeneration. Thieme Medical Publishers, Inc, New York
Marten T, Elyassnia D (2016) Simultaneous facelift and fat grafting. In: Connell BF, Sundine MJ (eds) Aesthetic rejuvenation of the face and neck. Thieme Medical Publishers, Inc, New York
Marten T, Elyassnia D (2015) Fat grafting in facial rejuvenation. In: Pu L, Yoshimura K, Coleman S (eds) Clinics in plastic surgery (fat grafting: current concept, clinical application, and regenerative potential, part 1), vol 42, no 2. Elsevier, Philadelphia
Marten TJ (2011) Simultaneous facelift and fat grafting: combined lifting and filling of the face. In: Nahai F (ed) The aesthetic plastic surgery: principles and techniques, 2nd edn. Quality Medical Publishing, Saint Louis
Marten TJ (2018) Facelift: secondary deformities and the secondary facelift. In: Neligan P, Rubin JP (eds) Plastic surgery (aesthetic), vol 2, 4th edn. Elsevier, London
Marten TJ (2011) Lamellar high SMAS face and mid-lift: improved design of the SMAS facelift for better results in the mid-face and infra-orbital region. In: Nahai F (ed) The aesthetic plastic surgery: principles and techniques, 2nd edn. Quality Medical Publishing, Saint Louis
Marten TJ (2008) High SMAS facelift—combined single flap lifting of the jawline, cheek, and midface. In: Paul M (ed) Clinics plastic surgery, vol 35, no 4. Elsevier, Philadelphia
Marten TJ (1997) Facelift: planning and technique. In: Paul M (ed) Clinics in plastic surgery, vol 24, no 2. WB Saunders, Philadelphia
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest to disclose.
Additional information
Portions of this article were reproduced from the chapter entitled “Simultaneous Facelift and Fat Grafting” that appeared in the book “Aesthetic Rejuvenation of the Face and Neck”, by BF Connell and MJ Sundine (Thieme, 2016). All figures, illustrations, tables, and descriptions of concepts, methods, and technique included in this chapter are courtesy of the Marten Clinic of Plastic Surgery and are used with permission.
Rights and permissions
About this article
Cite this article
Marten, T., Elyassnia, D. Facial Fat Grafting: Why, Where, How, and How Much. Aesth Plast Surg 42, 1278–1297 (2018). https://doi.org/10.1007/s00266-018-1179-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-018-1179-x
























