Abstract
Patients who have undergone implant-based breast reconstruction after skin-sparing mastectomy often complain about bulging on the upper flank or inferior axillary area. This is most likely because the subcutaneous tissue layer of the upper flank, which is continuous with the breast tissue, tends to show inferolateral drooping once the subcutaneous tissue becomes loose after eliminating the breast parenchyma. In addition, one of the weaknesses of implant surgery is that implants cannot completely replace the tissue removed during skin-sparing mastectomy (SSM). This leads to the formation of a depression and a stepping effect superior and lateral to the implant on both sides. Notably, because the pectoralis major muscle is quite thin, when there is a depression around the superolateral area of the implant, it acts as a band, which then leads to tissue bulging and serious aesthetic problems. Here, we describe a simple advancement suture technique that can be used to resolve these two aesthetic problems in direct-to-implant breast reconstruction. The advancement sutures are performed after the implant and drains are inserted following SSM and before closing the incision. First, the surgeon confirms the depression in the superolateral area of the implant insertion site by redraping a skin flap lateral to the margin. If a depression is suspected, the surgeon uses forceps to pull the subcutaneous tissue in the lateral flank pocket over to the lateral border of the pectoralis major muscle, superolateral to the implant. At this point, correction of the lateral flank bulging and depression on the superolateral border is verified. If the result is not satisfactory, the surgeon may attempt advancing the subcutaneous fat from different areas; the more posterior the tissue is advanced, the better it eliminates the lateral bulging and superolateral depression. However, too much advancement may cause extra tension, potentially resulting in tearing of the tissue. A round needle is used to suture two to three stitches, before completing wound closure. By performing this simple advancement suture, we were able to successfully minimize post-implantation deformity—bulging on the lateral flank and depression at the superolateral implant margin.
Level of Evidence IV This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Patients who have undergone implant-based breast reconstruction after skin-sparing mastectomy (SSM) often complain about bulging on the upper flank or inferior axillary area (Fig. 1). This is most likely because the subcutaneous tissue layer of the upper flank, which is continuous with the breast tissue, tends to show inferolateral drooping once the subcutaneous tissue becomes loose after eliminating the breast parenchyma [1]. In addition, one of the weaknesses of implant surgery is that implants cannot completely replace the tissue removed during SSM. This leads to the formation of a depression and a stepping effect superior and lateral to the implant on both sides [2]. Notably, because the pectoralis major muscle is quite thin, when there is a depression around the superolateral area of the implant, it acts as a band, which then leads to tissue bulging and serious aesthetic problems [3]. Here, we describe a simple advancement suture technique that can be used to resolve these two aesthetic problems in direct-to-implant (DTI) breast reconstruction.
Methods
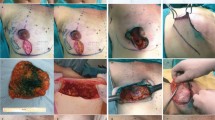
The advancement sutures are performed after the implant and drains are inserted following SSM and before closing the incision. First, the surgeon confirms the depression in the superolateral area of the implant insertion site by redraping a skin flap lateral to the margin. If a depression is suspected, the surgeon uses forceps to pull the subcutaneous tissue in the lateral flank pocket over to the lateral border of the pectoralis major muscle, superolateral to the implant. At this point, correction of the lateral flank bulging and depression on the superolateral border is verified. If the result is not satisfactory, the surgeon may attempt advancing the subcutaneous fat from different areas; the more posterior the tissue is advanced, the better it eliminates the lateral bulging and superolateral depression. However, too much advancement may cause extra tension, potentially resulting in tearing of the tissue. A round needle (1-0 Vicryl) is used to suture two to three stitches, before completing wound closure (Figs. 2, 3).
Results
From January 2013 to January 2016, 53 patients received axillary advancement sutures. Compared with patients who did not undergo axillary advancement suture, immediate aesthetic improvements can be expected in patients who were underwent this technique (Fig. 4). Moreover, a dimpling may form on the lateral flank, but this disappears in patients within a few weeks after surgery. Patients can start to perform shoulder exercises 2 weeks after surgery, and there is usually no range of motion (ROM) limitation.
Comparison of aesthetic results in patient without axillary advancement suture and patients with axillary advancement suture. (Above) Patient without axillary advancement suture, complaining about upper flank bulging and depression in the superolateral area of the breast; (centre, below) patients with axillary advancement suture, not presenting upper flank bulging and depression in the superolateral area of the breast. (Yellow circle) Superolateral area of the breast and upper flank area. (Left) Oblique view and (right) anteroposterior view
Discussion
Axillary advancement suture can be performed to minimize bulging of the lateral flank and depression of the superolateral implant margin. It also reduces dead space to subsequently minimize seroma. Although excessive advancement is associated with the risk of muscle tearing, this risk can be significantly reduced by fixing suture onto the muscle fascia. No functional problems including ROM limitations were observed even after the initiation of shoulder exercise starting from 2 weeks after the surgery. However, this technique can only correct an upper lateral stepping effect of an implant, but not an upper medial stepping effect.
Depressed areas around the implant can be subjected to lipofilling and areas of lateral flank bulging to liposuction, in place of axillary advancement suture. However, axillary advancement suture is a simple method of quilting suture among all other complex techniques and can bring about satisfactory results. And this technique can transfer remnant subcutaneous fat tissue to the depressed area and reduce the efforts of two procedures, liposuction and lipofilling. In addition, the amount of fat needed and surgery time can be reduced by using this technique even if additional liposuction or lipofilling is to be done.
Conclusion
By performing this simple advancement suture, we were able to successfully minimize post-implantation deformity—bulging on the lateral flank and depression at the superolateral implant margin.
References
Riggio E, Quattrone P, Nava M (2000) Anatomical study of the breast superficial fascial system: the inframammary fold unit. Eur J Plast Surg 23:310–315
Delay Emmanuel, Guerid Samia (2015) The role of fat grafting in breast reconstruction. Clin Plast Surg 42(3):315–323
Forsberg CG, Kelly DA, Wood BC, Mastrangelo SL, DeFranzo AJ, Thompson JT, David LR, Marks MW (2014) Aesthetic outcomes of acellular dermal matrix in tissue expander/implant-based breast reconstruction. Ann Plast Surg 72(6):S116–S120
Acknowledgment
This work was supported by the 2016 Yeungnam University Research Grant.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interests
Our authors declare that we have no conflicts of interest to disclose.
Rights and permissions
About this article
Cite this article
Lee, J.H., Yeo, CH., Chung, KJ. et al. Axillary Advancement Suture to Minimize Post-Implantation Deformity in Implant-Based Breast Reconstruction. Aesth Plast Surg 41, 1007–1009 (2017). https://doi.org/10.1007/s00266-017-0919-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-017-0919-7