Abstract
The inframammary fold (IMF) is the most critical visual landmark that affects final aesthetic outcome of augmentation mammoplasty and even post-mastectomy alloplastic breast reconstruction. Unfortunately, structural integrity of this landmark is greatly overlooked and very often neglected. Excessive undermining of the lower breast pole with aggressive disruption/lowering and subsequent poor reconstitution of the IMF scaffold combined with imbalanced implant-tissue dynamics may result in downward implant displacement with creep bottoming and upward tilt of the nipples. The current report reviews the experience of the senior author (BA) over 30 years in breast aesthetic and reconstructive surgery with IMF reconstruction and fixation to the chest wall at the inferior border of the implant. Illustrative cases are presented.
Level of Evidence V
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Alloplastic breast augmentation and reconstruction, though greatly popular and have high patient satisfaction rates, are not devoid of late post-operative complications primarily accelerated ptosis and breakdown of the inframammary fold (IMF) secondary to loading and compressive forces [1]. Considered as the most critical visual landmark of the breast [2], the IMF demarcates the degree of breast ptosis and dictates breast lower pole silhouette that should ideally form an acute angle with the thoracic wall [3]. Like all skin creases the structure and position of which should be a key consideration during planning and performance of skin and soft-tissue procedures [4,5,6], the IMF is a landmark of great anatomical, developmental, functional, and surgical importance [3]. Its anatomy has been a subject of controversy [6,7,8,9]. Lockwood proposed that the IMF, similar to other fixed skin creases, is formed by dermal connections of the superficial fascial system (SFS) [9].
The breast is made up of a unique combination of tissues with exceptional biomechanical properties and the capacity to respond to both naturally occurring and externally exerted stresses [1]. These tissues possess diverse elasticity, stiffness, compliance, and resilience [10]; fatty tissues have a constant modulus, whereas fibrous tissues are highly dependent on strain intensities [1]. Thus, as with any viscoelastic material, the degree of tissue stretching depends on any given breast overall composition, regional tissue components, and the precise location and intensity of the applied stress as well as a number of static and dynamic factors [1]. It should be noted also that despite constant loading, the mammary gland is subject to further deformation in relation to the duration of the applied stress, a concept termed as “creep deformation” [10], and when mechanical challenges exceed the elastic capacity of tissue components, irreversible stretching and deformation eventually ensues [1].
It has long been recommended that in all types of breast surgery, the IMF anatomy with the zone of adherence should be preserved. Whenever undermining is inevitable, the fold must be properly re-suspended [6, 11,12,13]. Unfortunately, this recommendation is not always respected when performing augmentation, reduction or alloplastic breast reconstruction as demonstrated by the high rate of late poor IMF positions encountered [14]. In many of these procedures, IMF position must be altered; with breast augmentation, IMF position may ascend or not change at all, and however, it must be lowered for a large number of patients, while with mastopexy or reduction mammoplasty IMF position must generally be elevated. In one study, a mean descent of 0.71 cm of the IMF following breast augmentation, an elevation of 2.28 cm following vertical pattern reduction, and 1.94 cm following vertical mastopexy were observed [14]. Similarly, modification in the IMF position is the norm following post-mastectomy breast reconstruction.
Patients and Methods
This report is not a systematic study based on a compiled series of patients. It is rather a general overview of the senior author’s (BA) experience in breast prosthetic/alloplastic aesthetic and reconstructive surgery over 30 years with IMF reconstruction and fixation to the chest wall at the inferior border of the implant as determined by preoperative assessment and measurements. We have already reported our method in breast augmentation for determination of IMF position and inframammary incision placement based on the anterior chest wall and implant footprint vertical dimensions, not the anterior curvature and implant projection. A 4–5 cm IMF incision is made at the desired position with caudal beveling to include a 1.5–2-cm soft-tissue rim with the cephalad flap following which dissection of the preoperatively chosen pocket, sub-glandular, sub-fascial, or dual plane proceeds in the standard fashion. After insertion of the implant, the soft-tissue rim is anchored to the chest wall with heavy resorbable sutures while making sure to protect the implant with a malleable retractor, thus restoring the anatomical framework of the IMF with a firm zone of adherence (Fig. 1). Skin closure then proceeds as usual. Soft tissues would adapt to the implant profile when it is well positioned with the nipple–areola complex (NAC) centered over round implants and slightly above maximal projection for pre-shaped implants [11]. For breast reconstruction, the method of determining the IMF position depends on whether bilateral mastectomy is performed with or without nipple sparing, whether nipple sparing is bilateral or unilateral, and whether unilateral mastectomy is performed with or without contralateral symmetrization. Generally, the IMF is ideally positioned at the level of the V-VI rib with its lower part extending to the VI intercostal space; the implant is placed in a sub-muscular pocket superiorly. We do not use ADM; infero-lateral implant support is provided by a dermal barrier and serratus anterior fascia [15]. For nipple-sparing mastectomy, the nipple is fixed to the underlying pectoralis major muscle in the proper position relative to the inserted implant.
a A 4–5 cm IMF incision is made with caudal beveling. b A 1.5–2 cm superiorly based soft-tissue dermo-adipose rim “flap” indicated by arrow. c Soft-tissue rim securely anchored to the chest wall with interrupted heavy Vicryl™ (Ethicon—Somerville, NJ, USA) sutures indicated by dashed line after implant insertion simulating normal IMF configuration. d Skin incision made at the determined new IMF level and carried toward the chest wall with caudal beveling. e Dermo-adipose barrier flap anchored to the chest wall after implant insertion. f Valve-like closure reinforced with natural implant pressure against the suture line
In all cases, heavy absorbable interrupted sutures, usually 0-Vicryl™ (Ethicon—Somerville, NJ, USA), are used to fix the IMF to the chest wall. For augmentation mammoplasty, the superiorly based dermo-adipose flap is fixed to the chest wall [11]. As for breast reconstruction, the dermis and superficial fascia of the lower mastectomy flap are fixed at the desired level mimicking the natural IMF curvature. With vertical pattern mastectomy incisions, fixation of a medially based dermal barrier may be enough to achieve the desired IMF definition and fixation in certain cases [15]. In some other cases with abdominal skin laxity, superior recruitment of abdominal skin may be beneficial [16, 17].
Illustrative cases
Case 1
Case 1 was a 34-year-old female requesting breast augmentation. Surgical planning and technique were as described previously [11]. The base width of the implant is selected to be 1.5 cm less than the breast base width (BBW) measured in the standing position. An inframammary incision was made at the predetermined level based on the estimated new NAC position and implant height. A superiorly based dermo-adipose flap is created, and then, a sub-glandular pocket is dissected. The 295 cc Inspira™ TSM (Allergan—Irvine, CA, USA) round prostheses were inserted; the IMF were then reconstructed by anchoring the dermo-adipose flap to the chest wall and wound closure completed. This type of closure provided stable IMF position as well as adequate and durable support for the lower pole implant (Fig. 2).
a–c Preoperative photographs of a patient presenting for breast augmentation. d–f Immediate result following sub-glandular insertion of a 295-cc round breast implant (InspiraTM TSM, Allergan) 11.75 cm in diameter. g–i Post-operative result at 1 year with good upper and lower poles breast contour. j Measurements taken and planning of the IMF incision based on anticipated post-operative NAC position and implant dimension. k Late stable and well-concealed IMF incision in the crease
Case 2
Case 2 was a 29-year-old patient presented with poor aesthetic outcome 1-year post-bilateral breast augmentation performed in another center with anatomically shaped small-height, high-profile 400-cc silicone gel implants (Cereform®, Cereplas, France) placed in a retropectoral pocket. The patient had severe bottoming with poor upper pole fullness and high mal-positioned NAC in relation to the implants that were found to have rotated at reoperation. The surgical approach was similar to what we have already described for primary breast augmentation [11]. The incision was made at the existing scar, a superiorly based dermo-adipose flap was created, and 373 cc round silicone implants were inserted; the IMF was reconstructed by anchoring the dermo-adipose flap to the chest wall at the predetermined level based on anticipated NAC position and implant diameter. Upper pole profile was improved with lipofilling in a second procedure a few months later (Fig. 3).
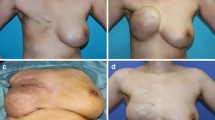
a–c Poor aesthetic outcome following breast augmentation with marked implant bottoming out and NAC malposition in relation to the implant and breast mound. Correction of deformity requires IMF repositioning at a higher level as indicated by the arrow. d Patient in upright position demonstrating poor lower pole support with implant caudal migration due to lack of IMF reconstruction. e–g Result at 1 year showing stable IMF reconstruction preventing recurrence of deformity
Case 3
Case 3 was a 50-year-old female with bilateral breast lesions on mammogram. Biopsy revealed right ductal carcinoma in situ and left invasive lobular carcinoma. She underwent left nipple-sparing and right skin-sparing mastectomies with sentinel lymph node biopsy followed by immediate breast reconstruction with permanent expander/implant (255 cc Siltex™ Contour Profile® Becker 35, Cohesive II™) (Mentor®—Santa Barbara, CA, USA) and upper abdominal skin flap recruitment for immediate IMF reconstruction. Expansion was started 2 days post-operatively and was completed by 2 weeks at the time of drain removal achieving almost symmetrical breast mounds with well-defined IMF and lower pole projection. Five months later, the patient presented for injection port removal (Fig. 4).
a–c Patient presenting for right mastectomy and prophylactic contralateral nipple-areola preserving mastectomy. d–f Result at 3 weeks following immediate bilateral breast reconstruction with Becker permanent expander implants, right IMF reconstruction by recruitment of abdominal flap and chest wall fixation (indicated by arrow), left IMF chest wall re-fixation (indicated by arrow), and rapid expansion. g–i Result at 5 month after completion of chemotherapy and before initiation of radiotherapy. Despite some loss of definition of the right inframammary fold, implants are well maintained in a stable position bilaterally
Case 4
Case 4 was a 41-year-old female with left breast multifocal invasive lobular carcinoma, grade 2/3. She underwent left total mastectomy with sentinel lymph node biopsy and right prophylactic total mastectomy. Because she requested to have larger breasts, immediate bilateral breast reconstruction was accomplished with permanent expander/implants (365 cc Contour Profile® Becker 35, Cohesive II™) (Mentor®—Santa Barbara, CA, USA). Rapid expansion was completed 3 weeks later at which time filling ports were removed and lipofilling of the breast upper pole was performed before initiation of chemotherapy (Fig. 5).
a–c Patient presenting for left skin-sparing mastectomy and prophylactic contralateral nipple-areola preserving mastectomy. d, e Incisions planning. f, g Immediate breast reconstruction with Becker permanent expander implants. IMF reconstruction bilaterally was achieved by anchoring scarpa’s fascia to the chest wall with simple sutures (h–j) result 3 weeks later following rapid expansion at the time of inflation port removal and simultaneous upper pole lipofilling
Case 5
Case 5 was a 38-year-old female with right breast infiltrating ductal carcinoma and left ductal carcinoma in situ. She underwent bilateral circumvertical pattern skin-reducing mastectomy with sentinel lymph node biopsy followed by immediate bilateral breast reconstruction with 555 cc Siltex™ Contour Profile® Becker 35, Cohesive II™ permanent expander/implants (Mentor®—Santa Barbara, CA, USA). Implant bottoming was prevented due to lower pole support by dermal barrier flaps and initial IMF reconstruction. Expander inflation was completed in 2 weeks; 6 months later, injection ports were removed and bilateral NAC reconstruction was performed with modified skate flaps and upper thigh full thickness skin grafts (Fig. 6).
Case 6
Case 6 was a 56-year-old postmenopausal patient with multifocal invasive ductal carcinoma in her right breast. She underwent right circumvertical pattern skin-reducing mastectomy with sentinel lymph node biopsy followed by immediate right breast reconstruction with a 495-cc medium-height high-profile anatomica-shaped prosthesis (Mentor®—Santa Barbara, CA, USA), dermal barrier flap, and IMF reconstruction. Contralateral mastopexy was also performed for symmetry (Fig. 7).
a–c Patient presenting for right skin-sparing mastectomy and contralateral mastopexy. d, e Initial circumvertical planning modified to include an upper lateral skin excision with immediate result of right IBR with 495-cc medium-height high-profile prosthesis and left mastopexy. f–h Final aesthetic outcome at 3 months
Results
As demonstrated by these cases, an important aspect of breast aesthetic and reconstructive surgery is control of IMF position, nipple-to-IMF length, and proper nipple-implant-chest wall relationship that is unfortunately often overlooked [18]. With good preoperative planning and estimation of the exact new IMF position, proper IMF fixation emerges as an unavoidable step in achieving highly predictable and satisfactory outcomes for breast augmentation, one-stage reconstruction, or even one-stage correction of breast implant bottoming. The fixation techniques we have applied resulted in long-lasting stable IMF reconstruction and greatly facilitated reaching this goal (Fig. 8).
Obviously, final long-term aesthetic outcome does not depend solely on IMF position. However, the various factors in play are not within the scope of this report, which is meant only to stress the value of IMF definition and fixation with stabilization of the implant inferior border in breast aesthetic and reconstructive surgery as already reported [11, 15, 19].
Discussion
Overall outcome of augmentation mammoplasty is dependent on multiple key elements such as implant fill volume, shape, skin stretch measurements, breast parenchyma thickness, breast implantation footprint and position on the chest. Thoughtful consideration of the patient’s desired aesthetic result in conjunction with selection of the appropriate implant, optimal incision, implant pocket, and inframammary fold location contributes to a satisfactory result [11, 20, 21].
Several access incisions have been described including periareolar, transareolar, transaxillary, and transumbilical incisions [22, 23]. These approaches may provide the potential advantage of inconspicuous resultant scars at the expense, however, of poor IMF and lower breast pole control [24]. Such a drawback is virtually eliminated with the inframammary incision; it allows better surgical control with more direct vision and a minimal amount of adjacent tissue trauma during pocket dissection and implant insertion [20, 25]. It remains the most preferred, widely used, and the only one that allows proper IMF fixation at the desired level [11, 25]. Nevertheless, accurate anticipation of the final position of the IMF remains a major difficulty to be overcome.
Almost all described preoperative assessment tools for augmentation mammoplasty include in their measurements proper determination of post-operative IMF position regardless of the access incision [11, 26]. This vital landmark is essential in determining the three-dimensional profile of the breast mound and most importantly the position of the nipple–areola complex (NAC) in relation to the breast mound [11, 20]. Proper nipple-implant-chest wall relationship cannot be overemphasized. Invariably triggered by implant malposition, displacement of the NAC is a most apparent deformity, which can be an aesthetically devastating problem for patients and a formidable challenge for surgeons [20, 27, 28]. Excessive undermining of the lower breast pole with aggressive disruption/lowering and subsequent poor reconstitution of the IMF scaffold combined with imbalanced implant-breast tissue dynamics may result in creep bottoming and upward tilt of the nipples [11, 29, 30].
Although the etiology of implant malposition is multifactorial and patient dependent, the two main causes are incorrect preoperatively designed nipple-to-inframammary fold (N-IMF) distance and tissue failure at the inframammary crease [20]. Large implants in particular tend to migrate the IMF caudally and induce stretching of the fibrous adherence bands even in the absence of violation [31]. Though not shared by all, it is advisable to position the IMF conservatively, slightly higher than what may be dictated [11, 26]. We share the opinion that, rather than placing the IMF incision higher, it is wiser to place the access incision precisely at the estimated new IMF position; this will make the resultant scar as inconspicuous as possible [26]. We also believe that proper IMF fixation is of utmost importance; even though it does not prevent lower pole tissue stretching, it actually defines the lower implant border, limits its descent, and preserves proper nipple-implant-chest wall relationship in terms of proper upper pole-to-lower pole ratio [11, 13, 32].
Correction of implant bottoming deformity is challenging. Provided breast and chest wall measurements and soft-tissue characteristics permit, proper implant NAC relationship may be restored rarely by simply replacing the implant by another with a larger vertical dimension. More commonly, removal of the mal-positioned implant is recommended first, and then, a new implant is inserted a few months later. In our experience, one-stage correction is possible provided proper IMF reconstruction at the optimal position is performed as demonstrated in case 2.
In post-mastectomy breast reconstruction, the IMF is an important anatomic landmark that must not be overlooked. In fact, the entire final reconstruction outcome is dependent on this landmark [2, 33]. Whenever oncologically safe, the existing structure must be respected and relocated at the predetermined level otherwise it must be reconstructed for one-stage cosmetically satisfactory reconstruction [3].
In classical two-stage expander/implant reconstructions, the device is first placed in a sub-pectoral pocket with complete muscle coverage. The inferior pectoralis major muscle is detached from the ribs and raised together with the rectus muscle, abdominal fascia, and the serratus anterior muscle. Inflation is initiated at post-operative day 10–14. In the second stage, the expander is replaced with an implant, the muscle pocket is released inferiorly, and the IMF is reconstructed. Maintaining the traditional principle of complete implant coverage commonly leads to an overly elevated point of maximal expansion with a constricted lower pole. In an attempt to overcome this limitation, modifications to the conceptual approach and surgical technique have been recently described to favor lower pole expansion and limit upper pole overexpansion. It is advised to lower the site of implant insertion 1–2 cm below the planned IMF position and most importantly to make a curvilinear fasciotomy at or just below the IMF. Moreover, departing from classical teachings, the current practice is shifting toward early and rapid implant expansion. At the second stage, the key for a successful exchange procedure remains however the reconstruction of the IMF [2].
Successful immediate single-stage reconstruction with permanent implant/expander (Becker permanent expander) placement is also popular and is becoming more popular [11, 34] contrary to the widely reported unfavorable experience with this device claiming that in the final analysis it requires replacement with a gel-filled implant similar to a standard two-stage approach due to poor aesthetics and shape asymmetries [35]. Permanent expanders are designed with the objective of combining the advantages of the silicone gel implant, saline implant, and tissue expander into one. Reported poor results with this anatomically shaped device are due to total sub-muscular pocket insertion similarly to what is performed for standard two-stage reconstruction preventing preferential maximal lower pole expansion. Within a tight musculo-fascial pocket, pressure increase with expansion moves maximal expansion superiorly closer to the device midpoint rather than staying at its desired lower pole directing it to expand into a round shape rather than into its ideal anatomical shape [2].
Mentor® Becker™ expander/breast implants are permanent expanders. Once positioned, they are supposed to be adjusted at a later date as in two-stage expander/prosthesis reconstructions [36]. Thus, it is imperative that initially the lower pole of the device must be free from the restrictive effect of the rectus abdominis fascia and that the IMF is reconstructed primarily. The pectoralis major muscle has also to be completely released inferiorly and secured to the overlying mastectomy flap to prevent superior migration [11, 34]. We believe that if the lower pole is placed in a totally subcutaneous pocket and laterally maintained by the serratus fascia, it is not necessary to position the device lower than the IMF as recently recommended [2]. In retrospect, poor results reported with the one-stage permanent expander/implant reconstruction are not due to expander characteristics but rather to improper surgical technique, an inadequate implantation pocket, and failure of IMF initial reconstruction. Moreover, when preparing the expander by aspirating air from the saline bladder, it is critical to ensure that the implant footprint is not distorted before insertion to secure proper implant footprint position over the chest wall particularly if expansion is delayed as generally recommended.
Immediate direct-to-implant breast reconstruction with a permanent prosthesis and acellular dermal matrix (ADM) lower pole support has gained popularity and has become gradually more preferred and requested by patients [37]. Despite meticulous attention to details and favorable results with this approach, some reported long-term outcomes have been somehow disappointing. Late revisions are sometimes necessary to restore symmetry by correcting the IMF and/or lateral mammary folds (LMF) [37]. Efforts have been made to minimize the rate of late revision by determining the ADM inset suture line and thus the proper position of the IMF [37]. We have described a dermal barrier with skin-sparing/reducing mastectomy for direct-to-implant single-stage immediate (DISSI) breast reconstruction [15, 38] obviating the use of ADM and facilitating IMF reconstruction (Figs. 6, 7).
The most effective method for IMF fixation remains a subject of debate. Several external and internal methods have been described in the literature involving lipo-fascial flaps, de-epithelialized skin, and a variety of suture techniques with different types of sutures including barbed sutures applied either in a continuous or single fashion. Occasional late loss of IMF definition remains however a major concern [12, 13, 30, 33, 39,40,41,42,43]. Anchoring the IMF to the rib periosteum has been recommended [44]; moreover, whether suture type has a real added value remains uncertain. Even though barbed sutures are claimed to generate more fibrous scar tissue compared to traditional sutures, no evidence has been established thus far regarding their clinical significance in promoting a stronger IMF fixation. At reoperation, all permanent sutures are typically found to be loose. Invariably, the strength of the bond is primarily determined by scar tissue [26, 40]. When compared with the standard suture method, a recently described intrarib anchor system (Micro BioComposite SutureTak, Arthrex) has been claimed to produce biomechanically superior fixation in terms of ultimate load, fixation stiffness, and displacement at failure [39]. It may be realistic, however, to postulate that a static repair may yield an unnatural look over time in view of the dynamic IMF nature; moreover, the risk of complications such as hematoma, implant injury, and additional patient discomfort becomes higher following IMF reinforcement [40]. For breast augmentation, we prefer a small superiorly based dermo-adipose flap fixed to the chest wall with interrupted heavy Vicryl sutures. This provides reliable fixation with scar tissue and limits the use of special types of suture material that may not be always available [11, 45]; it allows at the same time a degree of dynamic tolerance. We have employed this IMF fixation method successfully in breast augmentations and in one-stage repair of implant bottoming following unsatisfactory augmentation. As for breast reconstruction, the dermal barrier flap with scarpa’s fixation to the chest wall provides adequate lower pole support with durable IMF reconstruction [15, 38].
Even though this report is about IMF fixation and stabilization of the implant lower pole in breast augmentation and alloplastic breast reconstruction, IMF fixation is as critical in reduction mammoplasty or mastopexy as well. We have described the circumvertical technique in which vertical lines of the preoperative plan are drawn caudally from the lateral and medial ends of the periareolar drawing and then curved toward the breast axis line, where they meet about two fingers (2 cm) above the existing inframammary crease. Subsequent fixation of the inferior border of the medial and lateral pillars to the chest wall achieves the desired IMF elevation [19] (Fig. 7).
Conclusion
The long-term outcome of prosthetic/alloplastic breast augmentation or reconstruction is not determined only by IMF fixation and implant lower pole stabilization; nevertheless, we feel that prevention of implant caudal displacement is essential in achieving a satisfactory result. Whether long-term descent of the IMF position does occur remains to be objectively determined; however, as long as symmetry is maintained and the implant’s caudal migration is prevented, minor descent would not be clinically significant and chances for achieving high patient satisfaction may be increased. In our hands, the simple IMF fixation we are reporting has provided an efficient tool in performing satisfactory augmentation mammoplasty and alloplastic breast reconstruction.
References
Govrin-Yehudain J, Dvir H, Preise D, Govrin-Yehudain O, Govreen-Segal D (2015) Lightweight breast implants: a novel solution for breast augmentation and reconstruction mammaplasty. Aesthet Surg J 35(8):965–971
Cordeiro PG, Jazayeri L (2016) Two-stage implant-based breast reconstruction: an evolution of the conceptual and technical approach over a two-decade period. Plast Reconstr Surg 138(1):1–11
Bogetti P, Cravero L, Spagnoli G, Devalle L, Boriani F, Bocchiotti MA, Renditore S, Baglioni E (2007) Aesthetic role of the surgically rebuilt inframammary fold for implant-based breast reconstruction after mastectomy. J Plast Reconstr Aesthet Surg 60(11):1225–1232
Mallouris A, Kakgia D, Yiacomettis A, Vasilakaki T, Drougou A, Lambropoulou M, Simopoulos C, Tsaroucha AK (2016) Histological comparison of the human trunk skin creases: the role of the elastic fiber component. Eplasty 16:e15
Patel JC, Fletcher JW, Singer D, Sullivan P, Weinzweig J (2004) An anatomic and histologic analysis of the alar-facial crease and the lateral crus. Ann Plast Surg 52(4):371–374
Boutros S, Kattash M, Wienfeld A, Yuksel E, Baer S, Shenaq S (1998) The intradermal anatomy of the inframammary fold. Plast Reconstr Surg 102(4):1030–1033
Bayati S, Seckel BR (1995) Inframammary crease ligament. Plast Reconstr Surg 95(3):501–508
Van Straalen WR, Hage JJ, Bloemena E (1995) The inframammary ligament: myth or reality? Ann Plast Surg 35(3):237–241
Lockwood TE (1991) Superficial fascial system (SFS) of the trunk and extremities: a new concept. Plast Reconstr Surg 87(6):1009–1018
Vegas MR, Martin del Yerro JL (2013) Stiffness, compliance, resilience, and creep deformation: understanding implant-soft tissue dynamics in the augmented breast: fundamentals based on materials science. Aesthet Plast Surg 37(5):922–930
Atiyeh B, Dibo S, Nader M, Papazian N (2014) Preoperative assessment tool for the planning of inframammary incision and implant profile in breast augmentation. Aesth Plast Surg 38:878–886
Montemurro P, Quattrini Li A, Hedén P, Avvedimento S (2016) A four-layer wound closure technique with barbed sutures for stable reset of the inframammary fold in breast augmentation. Aesthet Surg J 36(8):966–971
Mallucci P, Branford OA (2016) Design for natural breast augmentation: the ICE principle. Plast Reconstr Surg 137:1728–1737
Swanson E (2010) Photometric evaluation of inframammary crease level after cosmetic breast surgery. Aesthet Surg J 30(6):832–837
Ibrahim AE, Atiyeh BS, Dibo SA, Sarhane KA, Abbas JS (2012) De-epithelialized dermal barrier for a safe immediate prosthetic breast reconstruction post circumvertical skin sparing/reducing mastectomy (SSM/SRM). Eur J Plast Surg 11:787–793
Atiyeh B, Dibo S, Abbas J, Papazian N (2016) Tensioned reverse abdominoplasty for reconstruction of large post-mastectomy defects. Rev Bras Cir Plást 31(2):252–256
Yacoub C, Baroudi R (2016) Extended reverse abdominalplasty: a technique for reconstructive and cosmetic application on the anterolateral area of the chest. In: Atiyeh B, Abbas J, Ibrahim A (eds) Breast cancer surgery and the principles of oncoplastic surgery for partial and total breast reconstruction. LAP LAMBERT Academic Publishing, Saarbrücken, pp 314–336
Campbell CF, Small KH, Adams WP Jr (2016) Response to “Can We Really Control the Inframammary Fold (IMF) in Breast Augmentation?”. Aesthet Surg J 36(10):317–320
Atiyeh B, Rubeiz M, Hayek S (2005) Refinements of vertical scar mammaplasty: circumvertical skin excision design with limited inferior pole subdermal undermining and liposculpture of inframammary crease. Aesthet Plast Surg 29(6):519–531
Kim YJ, Kim YW, Cheon YW (2014) Prevention of implant malposition in inframammary augmentation mammaplasty. Arch Plast Surg 41(4):407–413
Calobrace MB (2015) Teaching breast augmentation: a focus on critical intraoperative techniques and decision making to maximize results and minimize revisions. Clin Plast Surg 42(4):493–504
Hidalgo DA (2000) Breast augmentation: choosing the optimal incision, implant, and pocket plane. Plast Reconstr Surg 105:2202–2216
Atiyeh B, Al-Amm C, El-Musa KA (2002) The transverse intra-areolar infra-nipple incision for augmentation mammoplasty. Aesthet Plast Surg 26(2):151–155
Kolker AR, Austen WG Jr, Slavin SA (2010) Endoscopic-assisted transaxillary breast augmentation: minimizing complications and maximizing results with improvements in patient selection and technique. Ann Plast Surg 64(5):667–673
Cardenas-Camarena L, Ramirez-Macias R (2006) Augmentation/mastopexy: how to select and perform the proper technique. Aesthet Plast Surg 30:21–33
Montemurro P (2016) Response to “Can We Really Control the Inframammary Fold (IMF) in Breast Augmentation?”. Aesthet Surg J 36(10):315–316
Youn ES (2006) Importance of the new position of the nipple-areola complex in breast augmentation surgery. Plast Reconstr Surg 118:18S–31S
Spear SL, Albino FP, Al-Attar A (2013) Classification and management of the postoperative, high-riding nipple. Plast Reconstr Surg 131(6):1413–1421
Spear SL, Pittman T (2013) Discussion: the double-bubble deformity: cause, prevention, and treatment. Plast Reconstr Surg 132(6):1444–1445
Campbell CF, Small KH, Adams WP Jr (2016) The inframammary fold (IMF) fixation suture: proactive control of the IMF in primary breast augmentation. Aesthet Surg J 36(5):619–623
del Yerro JL, Vegas M, Fernandez V, Moreno E, Sanz I, Puga S, Vecino MG, Biggs TM (2013) Selecting the implant height in breast augmentation with anatomical prosthesis: the ‘‘Number Y’’. Plast Reconstr Surg 131:1404–1412
Mallucci P, Branford OA (2015) Shapes, proportions, and variations in breast aesthetic ideals: the definition of breast beauty, analysis, and surgical practice. Clin Plast Surg 42(4):451–464
Tomita K, Yano K, Nishibayashi A, Seike S, Hosokawa K (2016) Aesthetic outcomes of inframammary fold recreation in two-stage, implant-based, breast reconstruction. Springerplus 5(1):1656
Becker H (2013) A prospective randomized study comparing two different expander approaches in implant-based breast reconstruction: one stage versus two stages. Plast Reconstr Surg 131:643e–644e
Eriksen C, Lindgren EN, Frisell J, Stark B (2012) A prospective randomized study comparing two different expander approaches in implant-based breast reconstruction: one stage versus two stages. Plast Reconstr Surg 130:254e–264e
Farace F, Faenza M, Bulla A, Rubino C, Campus GV (2013) Is mammary reconstruction with the anatomical Becker expander a simple procedure? Complications and hidden problems leading to secondary surgical procedures: a follow-up study. J Plast Reconstr Aesthet Surg 66:741–746
Kalus R, Dixon Swartz J, Metzger SC (2016) Optimizing safety, predictability, and aesthetics in direct to implant immediate breast reconstruction: evolution of surgical technique. Ann Plast Surg 76(Suppl 4):S320–S327
Atiyeh BS, Abbas J, Costagliola M (2012) Dermal barrier for immediate prosthetic breast reconstruction. Rev Bras Cir Plást 27:630–635
Eichler C, Schell J, Uener J, Prescher A, Scaal M, Puppe J, Warm M (2016) Inframammary fold reconstruction: a biomechanical analysis. Plast Reconstr Surg Glob Open 4(3):e634
Swanson E (2016) Can we really control the inframammary fold (IMF) in breast augmentation? Aesthet Surg J 36(10):313–314
Ryan JJ (1982) A lower thoracic advancement flap in breast reconstruction after mastectomy. Plast Reconstr Surg 70:153–160
Nava M, Quattrone P, Riggio E (1998) Focus on the breast fascial system: a new approach for inframammary fold reconstruction. Plast Reconstr Surg 102:1034–1045
Handel N, Jensen JA (1992) An improved technique for creation of the inframammary fold in silicone implant breast reconstruction. Plast Reconstr Surg 89:558–562
Halls MJ (2012) Superiorly based single mastectomy flap with inferiorly based dermal flap and anchorage of the inframammary crease procedure for immediate breast reconstruction in patients with ptosis. Plast Reconstr Surg 130(4):632e–633e
Atiyeh B, Chahine F (2016) Comments on “A four-layer wound closure technique with barbed sutures for stable reset of the infra-mammary fold in breast augmentation”. Aesthet Surg J 36(9):291–292
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest to disclose and received no financial or material support.
Rights and permissions
About this article
Cite this article
Atiyeh, B., Ibrahim, A., Saba, S. et al. The Inframammary Fold (IMF): A Poorly Appreciated Landmark in Prosthetic/Alloplastic Breast Aesthetic and Reconstructive Surgery—Personal Experience. Aesth Plast Surg 41, 806–814 (2017). https://doi.org/10.1007/s00266-017-0854-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-017-0854-7