Abstract
Background
The surgical procedure aimed at constructing the upper eyelid crease is the cosmetic operation most commonly requested by Asian patients. The incisional approach leaves a permanent crease, but the swelling period can last longer than 3 months, and a distinct scar usually is unavoidable. Many mini-incisional techniques with incisions of varying sizes and locations have been developed, but the removal of pretarsal tissue has not been sufficient because these procedures wipe out only small pockets of soft tissue immediately inferior to skin for placement of the suture. Thus, the formed double eyelid may not be durable. The technique the authors introduce is a modified mini-incisional technique that combines the benefits of both the incisional and the usual mini-incisional methods.
Methods
Three 3- to 4-mm mini-incisions were made on each upper eyelid. The orbicularis muscle was isolated carefully from the skin and then cut off as much as possible in three directions: down (toward the palpebral margin), left, and right. Finally, the three incisions were sutured, and a vivid fold was created. This technique was applied for 110 patients. The follow-up period ranged from 3 to 12 months. The patients were welcomed for further treatment if any problems occurred at any time. An extra 3 years of follow-up evaluation was applied for 24 patients (46 cases) to assess the long-term maintenance of the fold.
Results
This study enrolled 110 patients (212 cases). A natural-looking skin fold appeared after the edema period. The scar was not obvious. Disappearance of the fold was not found in any case during 3–12 months (mean, 9 months) of follow-up evaluation. Obvious shifting of the fold was found in four cases during the additional 3 years of follow-up evaluation, but disappearance of the fold was not found in any case.
Conclusion
This modified technique was found to be successful in developing a natural-appearing, long-lasting suprapalpebral fold with an inconspicuous scar. It combines the best of both the open and usual mini-incisional techniques. Because a large amount of pretarsal soft tissue is removed, the double fold is less likely to fade away.
Level of Evidence V
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
The surgical procedure aimed at constructing the upper eyelid crease is the cosmetic operation most commonly requested by Asian patients [1]. Techniques for double-eyelid surgery can be roughly classified into the following techniques: open, nonincisional, and semi-open procedures [2, 3].
The open (incisional) procedure leaves a permanent crease. But the swelling period lasts longer than 3 months, in some cases even a full year [4, 5]. Moreover, a distinct scar usually is unavoidable. The nonincisional technique (suture method) is an easier operation with a faster recovery and no visible scar [6]. However, the fold shaped by this technique possibly will fade away in years because the excessive pretarsal tissue affects the fixation and thus jeopardizes the effect of suturing [3].
Many mini-incisional (semi-open) techniques with incisions of varying sizes have been developed [1] that have the advantages of faster recovery and inconspicuous scars. But the amount of removed pretarsal tissue is not sufficient because only small pockets of soft tissue inferior to the skin are wiped out for placement of the suture. Thus the formed double eyelid may not be durable.
Our technique is a modified mini-incisional technique that combines the benefits of both the open and the usual mini-incisional methods and removes large amounts of pretarsal tissue through three mini-incisions.
Patients and Methods
The authors performed this mini-incisional blepharoplasty for 110 patients (102 women and 8 men) between February 2009 and August 2011 (Table 1). The mean age of the patients was 23.4 years (range, 17–35 years). The majority of the patients (n = 92, 83.6 %) were 17–24 years old, and the remaining 18 patients (16.4 %) were 25 to 35 years of age. Bilateral surgeries were performed for 101 patients and unilateral procedures for 9 patients. Because the amount of removed tissue is not as much as with the open technique and redundant skin cannot be removed in an obvious way, we do not recommend this technique for patients with obvious skin redundancy or excessively thick eyelids.
The follow-up period applied regularly for every patient was 3–12 months (average, 9 months). This means that the patient was asked to come back to our department in 3–12 months postoperatively one time to have the shape and height of the double-eyelid line assessed and recorded by the authors. Also, the patients were welcomed for further treatment at no extra charge if any problems occurred at any time. Such data also were recorded.
To assess the long-term maintenance of the fold with this technique, from 22 March to 2 April 2012, we applied an extra 3 years of follow-up evaluation for all 24 patients (46 cases) who underwent this operation in 2009.
In this study, we followed the principles outlined in the Declaration of Helsinki, and informed consent was obtained from all the patients.
Surgical Technique
The face style and eye shape of patients should be taken into full consideration. With the patient sitting, the height and shape of the desired double-eyelid line were determined by gently pressing a pair of forceps on the upper eyelid while the patient’s eyes were closed. In supine position, the fold line was marked. The height of the line was usually 6–8 mm. The symmetry of the line on the bilateral upper eyelid should be checked carefully. The line can be moved upward or downward several times according to the patient’s preference.
Three 3- to 4-mm incision lines (A, B, and C) were marked along the double-eyelid line. Point A was about 5 mm from the medial canthus. Point B was the highest point of the designed line, located immediately above the pupil (i.e., medial one third of the upper eyelash line). Point C was near the lateral canthus, about 7 mm from the end of the marked line (Fig. 1).
Photo showing the final design of the suprapalpebral fold line. The height of the double-eyelid line was 6 to 8 mm. Three 3- to 4-mm incision lines (A, B, C) were marked along the double-eyelid line. Point A was 5 mm from the medial canthus. Point B is the highest point of the designed line, located immediately above the pupil (i.e., medial one third of the upper eyelash line). Point C was near the lateral canthus, about 7 mm from the end of the marked line
Cefuroxime, aminomethylbenzoic acid pills were given for oral application preoperatively. Regular facial sterilization was performed before anesthesia. Lidocaine 2 % (1.5 ml) containing 1:100,000 of epinephrine was injected into each eyelid along the designed line.
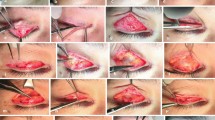
After the anesthetic effect was noted, three stab incisions were made on each side using a no. 11 sharp-pointed scalpel along the incision lines (Fig. 2). A pair of scissors was used for careful dissection to isolate the orbicularis muscle from the skin of the upper eyelid in three directions: down (toward the palpebral margin, Fig. 3a), left (Fig. 3b), and right (Fig. 3c). Blunt dissection was applied primarily in this procedure. The dissection usually needed to be repeated once for a thorough disconnection. A subcutaneous tunnel between each incision then was formed.
The removal of the muscle of each incision was applied one incision by one incision. Started with the lateral incision site of the right eye, ended at the lateral incision of the left eye. An 2- to 5-mm orbicularis bundle was held by a pair of toothed forceps at the left end of each incision, and a pair of scissors was used to cut inferiorly to the muscle bundle (Fig. 4a), and along its two sides (Fig. 4b). The muscle bundle was cut off after isolation (Fig. 4c). If the muscle stuck with the skin at a certain point, a blunt dissection was applied again in this area. The double eyelid could then be observed for many patients with thin or moderate eyelids (Fig. 5). Similarly, any remaining orbicularis was removed down (toward the palpebral margin, Fig. 6a, b) and right (Fig. 7a, b) after the isolation. The surgical sites were checked, and the orbicularis just in the incisions also was excised (Fig. 8).
In our practice, one half to two thirds of the orbicularis was removed after this procedure. For puffy eyelids, we preferred to incise the orbital septum at the lateral incision and tease out the herniated fat (Fig. 9). When the patient was asked to open his or her eyes, a vivid fold line appeared on the upper eyelid in most cases (Fig. 10).
A 5–0 silk thread was first inserted through the skin below the incision line (Fig. 11a), and then passed through the pretarsal fascia horizontally (Fig. 11b). By gentle pulling of the needle, the upper eyelid lifted as the needle was pulled if the pretarsal fascia was anchored well (Fig 11c). When the thread exited the skin above the incision line, it was tied with four knots at each point to close the incision. The fixation point on the pretarsal fascia usually was at the upper border of the tarsal plate or about 1 mm above the incision line (Fig. 11d).
The suture procedure. A 5–0 silk thread was a first inserted through the skin below the incision line and b then passed through the pretarsal fascia horizontally. c By gentle pulling of the needle, the upper eyelid lifted as the needle was pulled if the pretarsal fascia was anchored well. d The fixation point on the pretarsal fascia usually was at the upper border of the tarsal plate or about 1 mm above the incision line
The radian and symmetry were carefully rechecked when the patient’s eyes were open (Fig. 12). The location of the fixation could be readjusted as required. A thin layer of Aureomycin oculentum was spread on the surgical area (Fig. 13), which was later covered with a pressure dressing.
The patient was asked to press on the dressing with a pad of gauze for 30 min immediately after surgery. The cover was removed the next day, and sterilization was performed on the surgical sites twice a day for 7 days. The stitches were removed on postoperative day 7 or 8.
Results
The study enrolled 110 patients (212 cases). Pretarsal tissue was removed as much as possible (about 1/2 to 2/3 of muscle was removed) during the operation. A majority of the patients (n = 95) had orbital fat teased from the lateral incision. Depressions at the suturing points appeared on every patient due to uneven muscle dissection but soon became unnoticeable after 3 days. For 103 patients (93.6 %), the edema disappeared in 3 weeks (Fig. 14). For seven patients (6.4 %), the swelling period ended in 4 weeks. Obvious shifting of the double-eyelid line (≥3 mm) appeared on five patients (4.5 %), and multiple eyelids appeared on three patients (2.7 %), which recovered to double eyelids after the skin fold was adjusted and fixed with 3 M adhesive tape for 7 days.
Most patients showed disappearance of edema in 3 weeks. a View before the operation. b, c View on postoperative day 1 showing edema quite obvious and noticeable depressions. d, e View 1 week after the operation showing edema less obvious and disappearance of depressions. f, g View 3 weeks after the operation showing disappearance of edema
Hematoma and infection were not found in any case. The scars of the stab incision were no longer visible several months after the operation (Fig. 15; Table 2).
Our additional 3 years of follow-up evaluation involved 24 patients (46 cases). Obvious shifting of the fold appeared in four cases (8.7 %), two of which were serious. Still, disappearance of the fold was not found.
Discussion
It has been estimated that 30–60 % of Asians have single upper eyelids or an indiscernible supratarsal crease [5, 7, 8]. It is widely accepted that the supratarsal fold is created by insertion of the levator expansion to the skin [9]. Direct evidence was found by Cheng and Xu [10] by performing an anatomic study of Asian eyelids focused on investigating the inferior part of the upper eyelid using both electron microscopy and light microscopy. Sangki et al. [11] showed that in Asian single eyelids, the orbital septum is fused to the levator aponeurosis below the superior tarsal border, whereas fusion is above the superior tarsal border in Caucasians. Descent of the site combining the orbital septum and the levator aponeurosis together with the abundant retro-orbicular fat prevent the fibers of the aponeurosis from extending to the skin and forming the double-eyelid line [12].
The open technique can excise the abundant tissue (orbicularis and fat), and the skin can be connected to the levator aponeurosis by forming a tough scar. Thus, an upper eyelid crease is created that is not likely to fade. However, the injury to the blood vessels and the lymphatic drainage are relatively extensive. The swelling period is reportedly 3 months to a full year [4, 5].
The unavoidable scar on the upper eyelid makes many patients feel embarrassed. Ever since the first double-eyelid plasty was reported by Mikamo [1] in 1896, the nonincisional method has been very popular in Asia. The suture ligation technique (nonincisional method) leaves invisible scars and has a much shorter edema period than the open method. Nevertheless, because the skin is fixed to the levator aponeurosis by suture, the connection is not as secure as with the incisional technique. Moreover, because redundant pretarsal tissue cannot be teased out, excessive orbital fat may migrate to the area of fixation and jeopardize the effect of suturing. The reported disappearance rate for nonincisional blepharoplasty varies from 1.31 to 16.8 % [1, 13].
Our technique has several advantages over the traditional open method (incisional method) and the suture nonincisional method (suture method). Pretarsal tissue (orbicularis, pretarsal fat, and orbital fat) is selectively removed from three incisions. This procedure allows more direct contact between the dermis and the tarsus. Hence, a firmer adhesion is formed. Obviously, the upper eyelid crease is less likely to disappear than with the nonincisional method. At the same time, puffy eyelids, which give the patient a lazy and tired look, have been changed to slim eyelids. Because the fold is anchored by three points, when the upper eyelid is lifted, a smooth line is formed from point A to point C, which is more natural. The shape or height can be readjusted easily during the operation if necessary. Each incision is designed to be 3- to 4- mm to minimize injury and to enable better preservation of blood vessels and lymphatic drainage. Consequently, the swelling period (3 weeks) is much shorter than with the incisional operation, and the cicatrix is much less distinct.
Other mini-incisional techniques with incisions of varying sizes and debulking of underlying pretarsal soft tissues to enhance permanence have been developed [2, 13, 14]. However, the removal of pretarsal tissue is not sufficient because only small pockets of soft tissue immediately inferior to skin are wiped out for placement of the suture. Thus, the formed double eyelid may not be durable. Ma and Cheng [2] reported that 58 patients (11 %) subsequently underwent further operations. Among these, 32 (6.1 %) of 526 patients had subsequent surgeries to reestablish lost double folds. The timing of the reoperation ranged from 1 month to 48 months.
Our excision area covers all the way from the incision line almost to the palpebral margin and the entire lid length. Furthermore, its long-term maintenance is better. Among the 24 patients (46 cases) who underwent the procedure in 2009, disappearance of the fold was not found in any case, although obvious shifting was found in four cases, two of which were serious.
In our practice, indications for this technique are wider than for the usual mini-incisional method. Except for those with obvious skin redundancy or excessively puffy eyelids, all patients with single eyelids or indiscernible double eyelids are suitable candidates for this technique.
The following points should be noted during this operation:
-
(1)
In the blunt dissection that we adopted to isolate the muscle from the skin, a thorough disconnection is essential.
-
(2)
The removal of the orbicularis should be extended far enough medially, laterally, and down (toward the palpebral margin), and sharp dissection should not be applied superficially to the muscle to avoid unnecessary cuts on the skin.
-
(3)
If the muscle sticks to the skin at a certain point during excision, it is necessary to put the muscle back to its original place and repeat the blunt dissection procedure.
-
(4)
The pretarsal fat pad and the orbital fat in the lateral unit of the upper eyelid can be teased out, whereas the fat in the medial unit should remain because the medial fat pad is much thinner than in the lateral unit and atrophies with age.
-
(5)
The skin is anchored to the pretarsal fascia by three sutures before the cicatricial connection is formed. The crease can disappear if any of the suture loosens, leading to failure of the operation. To minimize the risk of such loosening, we suggest that each suture be tied with four knots and that postoperative management be gentle.
Conclusion
Our modified technique is a good alternative for construction of double eyelids. It combines the best of both the open and the usual mini-incisional techniques. Because a large amount of pretarsal soft tissue is removed, the double fold is less likely to fade away. Except for those with obvious skin redundancy or excessively puffy eyelids, all patients with single eyelids or indiscernible double eyelids are suitable candidates for this technique.
References
Mikamo M (1896) Mikamo’s double-eyelid operation: the advent of Japanese aesthetic surgery. Plast Reconstr Surg 99(3):664 discussion 664–669
Ma FY, Cheng MS (2010) Mini-incision double eyelidplasty. Aesthet Surg J 30:329–334
Kim YK, Kwon JD, Oh KS (2000) Double-eyelid operation with three tiny incisions. J Korean Soc Plast Reconstr Surg 27:195–198
Lam SM, Karam AM (2010) Supratarsal crease creation in the Asian upper eyelid. Facial Plast Surg Clin North Am 18:43–47
Liu X, Fan D, Guo X, Song W, Wang J (2010) A transcutaneous, subcutaneous, and intratarsal suturing procedure in double-eyelid surgery. Plast Reconstr Surg 126:2133–2139
Fan J, Low DW (2009) A two-way continuous buried-suture approach to the creation of the long-lasting double eyelid: surgical technique and long-term follow-up in 51 patients. Aesthetic Plast Surg 33:421–425
Hiraga Y (1980) The double-eyelid operation and augmentation rhinoplasty in the Oriental patient. Clin Plast Surg 7:553–567
Fernandez LR (1960) Double-eyelid operation in the Oriental in Hawaii. Plast Reconstr Surg Transplant Bull 25:257–264
Sayoc BT (1956) Absence of superior palpebral fold in slit eyes: an anatomic and physiologic explanation. Am J Ophthalmol 42:298–300
Cheng J, Xu FZ (2001) Anatomic microstructure of the upper eyelid in the Oriental double eyelid. Plast Reconstr Surg 107:1665–1668
Jeong S, Lemke BN, Dortzbach RK, Park YG, Kang HK, Jeong S, Lemke BN, Dortzbach RK, Park YG, Kang HK (1999) The Asian upper eyelid: an anatomical study with comparison to the Caucasian eyelid. Arch Ophthalmol 117:907–912
Hwang K, Kim DJ, Chung RS, Lee SI, Hiraga Y (1998) An anatomical study of the junction of the orbital septum and the levator aponeurosis in Orientals. Br J Plast Surg 51:594–598
Homma K, Mutou Y, Mutou H, Ezoe K, Fujita T (2000) Intradermal stitch blepharoplasty for orientals: does it disappear? Aesthetic Plast Surg 24:289–291
Uchida J (1962) A surgical procedure for blepharoptosis vera and for pseudo-blepharoptosis orientalis. Br J Plast Surg 15:271–276
Acknowledgment
This work was supported by funding from the Zhejiang Provincial Science and Technology Project of China (no. 2010C33170) and the National Science Foundation of China (grant no. 30800228).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhang, MY., Yang, H., Li, CY. et al. Removal of a Large Amount of Pretarsal Tissue Through Three Mini Incisions in the Construction of a Double Eyelid. Aesth Plast Surg 36, 1039–1046 (2012). https://doi.org/10.1007/s00266-012-9950-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-012-9950-x