Abstract
Cervical disc arthroplasty (CDA) is a powerful, motion-sparing treatment option for managing cervical radiculopathy or myelopathy. While CDA can be an excellent surgery for properly indicated patients, it is also less forgiving than cervical fusion. Optimally resolving patient symptoms while maintaining range of motion relies on near perfection in the surgical technique. Different CDA options exist on the market, with some having long-term proven success and others in early stages of clinical trials. We discuss the different options available for use, as well as strategies of positioning, approach, disc space preparation, implantation, and fusion prevention that we believe can help improve performance and outcomes of CDA.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Cervical disc arthroplasty provides a motion-preserving option to managing cervical radiculopathy and myelopathy as compared to anterior cervical discectomy and fusion. While the numbers of arthroplasties performed increased after FDA approval, surgeons still perform nearly 100 times as many anterior fusions as arthroplasties in the USA each year [1].
The relatively low utilization of CDA is multifactorial and includes clinical, economic, and technical considerations [2, 3]. While the indications for CDA have expanded to include patients with both radiculopathy as well as myelopathy, several contraindications such as facet arthrosis, severe disc degeneration and spondylosis, and osteoporosis limit more widespread use [4,5,6,7]. Economically, it is also more beneficial for surgeons in the current reimbursement system to perform an ACDF rather than a disc arthroplasty, even though healthcare costs may be lower when CDA is performed [8]. However, we believe that another significant factor limiting the more widespread use of CDA is the technical challenges of performing the operation. While a cervical fusion can be forgiving, the maintenance of motion requires near perfection in the indication of patients, removal of osteophytes, precision of endplate preparation, and positioning of the implant. A small imperfection in any of these steps can cause the patient’s symptoms to return and further surgery to be required. By discussing the options for implants and sharing our preferred technique for cervical disc arthroplasty, we hope that more successful implantation can be achieved and revision rates reduced.
Patient positioning
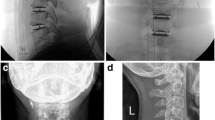
Proper implant position is vital for optimal function of a cervical disc arthroplasty. Two methods of verifying position of the implant are through radiographic and visual confirmation. Radiographic confirmation should be done throughout the case. This requires perfect AP and lateral X-rays intra-operatively. However, if the patient is not well positioned on the table, these necessary images are impossible to obtain. Positioning must therefore be compared to standing pre-operative images and confirmed with AP and lateral fluoroscopy to show correct alignment and rotation of the patient on the table with the level of interest being neutral. An example of positioning and the comparison to the upright pre-operative X-rays are shown in Fig. 1. Once perfect facet overlap on lateral X-ray is achieved, the patient’s head should be secured with tape over the forehead, chin, and above the lips to guarantee the position will be maintained (Fig. 2). Imaging should be performed at multiple times throughout the case, such as at level confirmation and implantation of the trials. At each of these time points, the bed should be rotated as needed to ensure the patient is positioned perpendicular to the floor.
An example of pre-operative and intra-operative X-rays demonstrating positioning for a patient that underwent a cervical disc arthroplasty at C6–7. a, b The lateral and A/P upright X-rays acquired prior to surgery, respectively; the arrow is pointing to C6. c, d Intraoperative lateral and A/P X-rays reproducing the same alignment as shown in a and b
Approach
Standard Smith-Robinson approach to the anterior cervical spine is utilized. We prefer to carefully mark our proposed incision in a well-lit environment with a fine-tipped marker to ensure a very cosmetically pleasing incision in the patient’s given skin crease. After standard pre-operative cleansing with alcohol and chlorhexidine, we apply sterile drapes and inject an epinephrine-containing local anaesthetic along the superficial aspect of the wound to minimize superficial bleeding during exposure. We find our predicted level and mark it with a burlisher on the medial edge of the longus colli so that we can confirm radiographically prior to entering the disc space. Once the level is confirmed, we elevate the musculature so that we can place our retractors underneath. For implants that tend to be prominent ventrally, we prefer to not fully remove the ventral overhang from the cephalad vertebrae in order to allow it to contain the implant fully; removing it would lead to the implant being prominent ventrally or a smaller implant being necessitated.
Caspar pin insertion
Once the Caspar pins are inserted just a few threads, AP and lateral X-rays can confirm centering of the pins as well as correct trajectories of the pins. Intra-operative X-ray examples are shown in Fig. 3. By confirming that the pins are centered, it can be used for referencing of centre when inserting the instruments and final implant. If the patient is noted to be malpositioned, the bed can be rotated and the c-arm adjusted to achieve perfect imaging of the operative level. Imaging can be taken again throughout the case based on the particulars of the specific disc, including after insertion of the trial and final prosthesis. The trial on the handle is inserted and confirmed to be in appropriate position. This theoretically should be inserted with the handle parallel to the Caspar pins. If the Caspar pins were inserted at a slight angle, the insertion angle of the handle can be varied until appropriate and the angle of the trial relative to the pins can be used to replicate the insertion angle of the preparation devices and final implant.
The procedural X-rays showing pin placement, implant alignment, and final X-rays. a, b The positioning of the Caspar pins in the lateral and A/P positions; of note, the caudal pin was noted in a to not be convergent with the cranial Caspar pin and adjustments are noted in c. c Good facet alignment (top arrow), but the trial is tilted by evidence of the circle not being round, and by the misalignment of the trial endplate foot-processes. d Perfect alignment with a round circle demonstrated in the middle of the trial together with a perfect lateral X-ray of the facet. e Confirmatory A/P placement of the trial. f, g Final intraoperative images of the implant
The Caspar pins should be inserted straight perpendicularly to the vertebrae in the coronal plane. In the sagittal plane, the caudal pin should be inserted at the standard roughly 15° cephalad angulation to match the endplate angle, but the cephalad pin should be inserted more directly without as much cephalad angulation. This prevents the pin from being in the way of implant insertion. Severe difference in angulation and endplate violation during disc space preparation can lead to implantation in kyphosis, while slight Caspar pin difference in angulation with careful endplate preparation and implant insertion can ensure that no kyphosis is induced. Inserting the Caspar pins as far as possible from the disc space without violating the adjacent disc space can also help ensure that adequate space is available for the necessary arthroplasty jigs. For two-level cases, the placement of Caspar pins for the second arthroplasty can be referenced clinically off the first implant after verification that it was inserted in good position (Fig. 4).
Endplate preparation
Many different designs of arthroplasty exist, and each has its own specific technique and guides for insertion. Regardless of design, it is imperative to place it centered in the disc space and flush with the endplates in order to achieve optimal biomechanics. The endplates must be planned to artistic perfection until they are microscopically flush and parallel. The disc space is prepared with Caspar pins distracted; after preparation, the distraction can be released and the disc space inspected to ensure that they are parallel, since placement of the pins even a millimeter off-centre can distract the disc spaces unevenly. Great care must be placed toward this step otherwise the arthroplasty may be tilted, or not fully resting on the bone where it needs to bond. The arthroplasty should be sized to fill the disc space anterior to posterior as large as possible, again to optimize biomechanics.
Implant preparation and insertion
Techniques of implanting the prosthesis are particular to each specific implant. If Caspar pins are centrally inserted perfectly between the uncinates, then these can be used to mark the midline for where the implant would be inserted. Figure 3 demonstrates intra-operative confirmatory images of the Caspar pin placement. In general it is important to ensure that each tool such as the rasps and trials are being inserted in a similar manner to ensure that the endplates are not violated and that the space being prepared is the identical desired position of the implant.
The largest implant possible should be inserted. This includes width as well as depth of the arthroplasty. The depth should be estimated on pre-operative imaging and confirmed with intra-operative radiographs using the trials. Height should be nearly the same as the pre-operative disc height, or the smallest height implant close to that. After inserting the first arthroplasty, fluoroscopy can confirm proper positioning and tilt (shown in Fig. 3). When performing a two-level artificial disc, the position of the second implant should be verified throughout as well; if the first was inserted well, the second one should also be referenced clinically off the first one (Fig. 4).
For devices with rails, channels must be carefully cut into the endplates for the rails to sit. The rail-cutting jigs can be hampered by sclerotic endplates, for example, if this happens then the rails are not fully cut into an endplate. This can be noticed when inserting the tool if the rails are not fully penetrating the endplates symmetrically and fully, and if the disc space is opening up while the tool is being inserted, which suggests the rails are not fully penetrating into the vertebrae. To prevent this, the distraction from the Caspar pins should be released once the jig is inserted partially into the disc space. Additionally, the rail-cutting guide can be rocked back and forth into the endplates in order to ensure adequate penetration. Some implants also have drills that can be used prior to the rail-cutting device, which set the position for where the channels will be cut. Care must be taken to adequately fit the drill guide into place and remove the Caspar pin distraction so that the drills do not skive off of the bone, otherwise the rails will not adequately cut into these preopened sites. Finally, after removing the guide, a small, curved microcurette can be used to remove any bone dust or particles that may be stuck in the channels to ensure that the final implant is able to slide smoothly into it.
Decreasing likelihood of fusion
The most common complication of cervical disc arthroplasty is fusion of the operated levels. This can be minimized through a variety of techniques. First, care must be taken during endplate preparation to avoid violating the endplates. In addition to making the surface for the disc to bond to uneven, this also exposes underlying cancellous bone and causes bleeding, which can increase likelihood of fusion. Second, after doing the discectomy, the PLL is removed. Then, we bipolar cauterize the remaining ends of the PLL to prevent traction spurs posterior to the disc, as well as OPLL. Third, all bone dust should be irrigated out. Fourth, all bleeding bone except from the endplate should be addressed with bone wax throughout the procedure to decrease peri-operative release of growth factors leading to fusion, and as a secondary effect, this will decrease the likelihood of haematoma formation. Caspar pin sites should be filled with bone wax. Additionally, when an uncinatetectomy is performed or even when the medial aspect of the uncinate is partially removed to make place for the implant, bone wax should be used liberally (in areas that will not be in contact with the arthroplasty endplate) both to prevent fusion and to minimize regrowth of the osteophytes. Wax should not be applied where the arthroplasty bonds to the endplate, as wax prevents this from happening. After the arthroplasty is implanted, we strip the anterior periosteum approximately half of the distance to the adjacent discs and wax the bone and the front of the arthroplasty to prevent anterior bone spur formation.
Meticulous haemostasis, in addition to minimizing the risk of haematoma, also helps decrease circulating growth factors promoting fusion. We prefer to wrap the released edges of the longus colli muscles with a haemostatic agent such as Surgicell; we also use a Penrose drain in all cases rather than closed suction drainage in order to decrease the risk of the smaller holes of the drain clotting off. When one or two level procedures are done on an outpatient basis, we still insert a Penrose drain and suture it to the dressing so that it can be removed with ease by the patient at home by simple removal of the dressing. Figure 5 demonstrates final X-rays for the case sample that was demonstrated in Figs. 3 and 4.
Irrigation
We purposely separated out this section to highlight the importance of irrigating all the bone dust from the site prior to disc implantation. We believe that failure to do so markedly increases the risk of undesirable ossification. We use at least 300–400 cc of irrigation using both a 20-cc syringe with an 18-gauge angiocath for high-pressure spot irrigation, as well as a 60-cc bulb irrigation syringe. We keep irrigating until every little speck of bone dust is gone.
Choosing an implant
Mobi-C
The Mobi-C artificial disc is comprised of cobalt-chromium endplates around an ultra-high-molecular-weight polyethylene core. The upper surface is rounded to match the inferior endplate, while the lower surface is more flat; these are both coated with titanium and hydroxyapatite and lined with a row of teeth. Many studies have been performed demonstrating the efficacy of the Mobi-C cervical disc arthroplasty [9,10,11]. A recent trial by Radcliff et al. analyzed 599 patients who were enrolled and showed that CDA with the Mobi-C had statistically higher success rates for two-level surgery than ACDF. Lower rate of adjacent segment surgery also occurred in single-level surgery as well [9]. A recent review showed that the Mobi-C, when compared to ACDF, led to improved range of motion at the operated level as well as significantly improved neck pain, improved patient satisfaction, and decreased rates of adjacent segment disease [10].
Bryan
The Bryan is a semi-constrained artificial disc comprised of titanium alloy endplates with a polyurethane centre piece. Porous titanium endplates are designed to improve bony ingrowth, and a ventral lip on the implant helps to prevent excessive translation or dislocation of the device. Several studies have shown long-term outcomes from the Bryan disc arthroplasty to be similar to that after ACDF [12,13,14]. Ten-year data on this device showed that success as reported by the Neck Disability Index score was higher after placement of the Bryan arthroplasty. However, there was no statistically significant difference between adjacent level re-operation after arthroplasty insertion and after ACDF [12].
ProDisc-C
The ProDisc-C is a semi-constrained device composed of two cobalt chrome alloy endplates with an internal ultra-high-molecular-weight polyethylene insert. These endplates have keels and titanium-coated surfaces to help stabilize the prosthesis to the adjacent endplates. Trials have shown safety and efficacy of the ProDisc-C, with decreased adjacent level surgery than ACDF [15,16,17]. Clinical treatment success was similar between the two groups, while at five year follow-up the patients who received ProDisc-C had significantly decreased rates of further surgery at the operated or adjacent levels than those who had ACDF [15, 16]. A seven year follow-up study also showed lower re-operation after CDA with similar clinical outcomes to those who had undergone ACDF [17].
Prestige
The Prestige is an unconstrained metal-on-metal artificial disc replacement. The Prestige ST is a stainless steel implant that uses screw fixation to attach to the adjacent bones. The Prestige LP is titanium and has rails that cut into the upper and lower endplates; ingrowth into the Prestige LP has been shown in an animal model six months after implantation [18]. Studies have shown safety and efficacy at up to seven year follow-up for the Prestige-LP [19,20,21]. While reoperation rates at adjacent levels after the Bryan disc were improved but did not show statistically significant difference, rate of adjacent level surgery at seven years was significantly improved when combining the Bryan data with the Prestige ST results [12].
SECURE-C
The SECURE-C is a semi-constrained arthroplasty with cobalt chrome alloy endplates with a central ultra-high-molecular-polyethylene piece. Two and seven year follow-up has shown statistically significant improvements in pain, function, and patient satisfaction for patients who have had arthroplasty insertion as compared to those who had ACDF [22, 23].
M6
The M6 is comprised of titanium endplates joined in a functional unit with an internal polyethylene and polycarbonate urethane disc centre. It is designed to have the internal components mimic the annulus around an inner nucleus-like core. Initial trial results suggest safety and efficacy; however, there is no substantial evidence from longer-term and comparative trials at this time [24, 25].
DISCOVER
The DISCOVER arthroplasty is an unconstrained implant comprised of titanium endplates with a centre ultra-high-molecular-weight-polyethylene core. When compared to ACDF at two year follow-up, results after arthroplasty appeared to be similar between the groups in one study, while another trial showed significant improvement in Neck Disability Index and pain scores in the arthroplasty group [26, 27].
Several other cervical disc arthroplasty designs are being studied, including the Kineflex C arthroplasty, Cervicore disc, Simplify disc, and Porous Coated Motion prosthesis.
Conclusion
While there are several technical challenges to performing perfect cervical disc arthroplasties, they can be excellent operations for properly indicated patients [28,29,30,31]. Recent evidence continues to suggest the benefit of various arthroplasties in reducing rates of secondary surgery at adjacent levels at medium-term follow-up, and improvements in arthroplasty materials and design have yielded titanium implants that are more MRI compatible and therefore allow for better-quality advanced imaging after implantation. Regardless of implant chosen, we believe that meticulous attention to surgical techniques can help optimize implantation and performance success of cervical disc arthroplasty.
References
Saifi C, Fein AW, Cazzulino A, Lehman RA, Phillips FM, An HS, Riew KD (2018) Trends in resource utilization and rate of cervical disc arthroplasty and anterior cervical discectomy and fusion throughout the United States from 2006 to 2013. Spine J 18(6):1022–1029
Lu Y, McAnany SJ, Hecht AC, Cho SK, Qureshi SA (2014) Utilization trends of cervical artificial disc replacement after FDA approval compared with anterior cervical fusion: adoption of new technology. Spine 39(3):249–255
Arrojas A, Jackson JB, Grabowski G (2017) Trends in the treatment of single and multilevel cervical stenossi: a review of the American Board of Orthopaedic Surgery Database. J Bone Joint Surg Am 99(18):e99
Nunley PD, Coric D, Frank KA, Stone MB (2018) Cervical disc arthroplasty: current evidence and real-world application. Neurosurgery 1087-1106
Leven D, Meaike J, Radcliff K, Qureshi S (2017) Cervical disc replacement surgery: indications, technique, and technical pearls. Curr Rev Musculoskelet Med 10(2):160–169
Joaquim AF, Riew KD (2017) Multilevel cervical arthroplasty: current evidence. A systematic review. Neurosurg Focus 42(2):E4
Auerbach JD, Jones KJ, Fras CI, Balderston JR, Rushton SA, Chin KR (2008) The prevalence of indications and contraindications to cervical total disc replacement. Spine J 8(5):711–716
Radcliff K, Zigler J, Zigler J (2015) Costs of cervical disc replacement versus anterior cervical discectomy and fusion for treatment of single-level cervical disc disease: an analysis of the Blue Health Intelligence database for acute and long-term costs and complications. Spine 40(8):521–529
Radcliff K, Davis RJ, Hisey MS, Nunley PD, Hoffman GA, Jackson RJ, Bae HW, Albert T, Coric D (2017) Long-term evaluation of cervical disc arthroplasty with the Mobi-C cervical disc: a randomized, prospective, multicenter clinical trial with seven-year follow-up. Int J Spine Surg 11:31
Ning GZ, Kan SL, Zhu RS, Feng SQ (2018) Comparison of Mobi-C cervical disc arthroplasty versus fusion for the treatment of symptomatic cervical degenerative disc disease. World Neurosurg 114:e224–e239
Lu H, Peng L (2017) Efficacy and safety of Mobi-C cervical artificial disc versus anterior discectomy and fusion in patients with symptomatic degenerative disc disease. Medicine 96(49):e8504
Ghobrial GM, Lavelle WF, Florman JE, Riew KD, Levi AD (2018) Symptomatic adjacent level disease requiring surgery: analysis of 10-year results from a prospective, randomized, clinical trial comparing cervical disc arthroplasty to anterior cervical fusion. Neurosurgery
Song Q, He D, Nan X, Zhang N, Wang J, Tian W (2018) Clinical and radiological outcomes of cervical disc arthroplasty: ten year follow-up study. Int Orthop 42(10):2389–2396
Lei T, Liu Y, Wang H, Xu J, Ma Q, Wang L, Shen Y (2016) Clinical and radiological analysis of Bryan cervical disc arthroplasty: eight-year follow-up results compared with anterior cervical discectomy and fusion. Int Orthop 40(6):1197–1203
Zigler JE, Delamarter R, Murrey D, Spivak J, Janssen M (2013) ProDisc-C and anterior cervical discectomy and fusion as surgical treatment for single-level cervical symptomatic degenerative dis disease: five-year results of a Food and Drug Administration study. Spine 38(3):203–209
Delamarter RB, Zigler J (2013) Five-year reoperation rates, cervical total disc replacement versus fusion, results of a prospective randomized clinical trial. Spine 38(9):711–717
Janssen ME, Zigler JE, Spivak JM, Delamarter RB, Darden BV, Kopjar B (2015) ProDisc-C total disc replacement versus anterior cervical discectomy and fusion for single-level symptomatic cervical disc disease: seven-year follow-up of the prospective randomized U.S. Food and Drug Administration investigational device exemption study. J Bone Joint Surg Am 97(21):1738–1747
Lou J, Wang B, Wu T, Li H, Liu Z, Liu H (2018) In-vivo study of osseointegration in Prestige LP cervical disc prosthesis. BMC Musculoskelet Disord 19(1):42
Gao X, Yang Y, Liu H, Meng Y, Zeng J, Wu T, Hong Y (2018) Cervical disc arthroplasty with Prestige-LP for the treatment of contiguous 2-level cervical degenerative disc disease: 5-year follow-up results. Medicine 97(4):e9671
Lanman TH, Burkus JK, Dryer RG, Gornet MF, McConnell J, Hodges SD (2017) Long-term clinical and radiographic outcomes of the Prestige LP artificial cervical disc replacement at 2 levels: results form a prospective randomized controlled clinical trial. J Neurosurg Spine 27(1):7–19
Zeng J, Liu H, Rong X, Wang B, Yang Y, Gao X, Wu T, Hong Y (2018) Clinical and radiographic outcomes of cervical disc arthroplasty with Prestige-LP disc: a minimum 6-year follow-up study. BMC Musculoskelet Disord 19(1):285
Vaccaro A, Beutler W, Peppelman W, Marzluff JM, Highsmith J, Mugglin A, DeMuth G, Gudipally M, Baker KJ (2013) Clinical outcomes with selectively constrained SECURE-C cervical disc arthroplasty: two-year results from a prospective, randomized, controlled, multicenter investigational device exemption study. Spine 38(26):2227–2239
Vaccaro A, Beutler W, Peppelman W, Marzluff JM, Mugglin A, Ramakrishnan PS, Myer J, Baker KJ (2018) Long-term clinical experience with selectively constrained SECURE-C cervical artificial disc for 1-level cervical disc disease: results from seven-year follow-up of a prospective, randomized, controlled investigational device exemption clinical trial. Int J Spine Surg 12(3):377–387
Reyes-Sanchez A, Miramontes V, Olivarez LM, Aquirre AA, Quiroz AO, Zarate-Kalfopoulos B (2010) Initial clinical experience with a next-generation artificial disc for the treatment of symptomatic degenerative cervical radiculopathy. SAS J 4(1):9–15
Thomas S, Willems K, Van den Daelen L, Linden P, Ciocci MC, Bocher P (2016) The M6-C cervical disk prosthesis: first clinical experience in 33 patients. Clin Spine Surg 29(4):e182–e187
Skeppholm M, Lindgren L, Henriques T, Vavruch L, Lofgren H, Olerud C (2015) The Discover artificial disc replacement versus fusion in cervical radiculopathy—a randomized controlled outcome trial with 2-year follow-up. Spine J 15(6):1284–1294
Rozankovic M, Marasanov SM, Vukic M (2017) Cervical disc replacement with Discover versus fusion in a single-level cervical disk disease: a prospective single-center randomized trial with a minimum 2-year follow-up. Clin Spine Surg 30(5):e515–e522
Reinke A, Behr M, Preuss A, Villard J, Meyer B, Ringel F (2017) Return to sports after cervical total disc replacement. World Neurosurg 97:241–246
Gornet MF, Lanman TH, Burkus JK, Hodges SD, McConnell JR, Dryer RF, Copay AG, Nian H, Harrell FE (2017) Cervical disc arthroplasty with the Prestige LP disc versus anterior cervical discectomy and fusion, at 2 levels: results of a prospective, multicenter randomized controlled clinical trial at 24 months. J Neurosurg Spine 26(6):653–667
Zou S, Gao J, Xu B, Lu X, Han Y, Meng H (2017) Anterior cervical discectomy and fusion (ACDF) versus cervical disc arthroplasty (CDA) for two contiguous levels cervical disc degenerative disease: a meta-analysis of randomized controlled trials. Eur Spine J 26(4):985–997
Hu Y, Lv G, Ren S, Johansen D (2016) Mid- to long-term outcomes of cervical disc arthroplasty versus anterior cervical discectomy and fusion for treatment of symptomatic cervical disc disease: a systematic review and meta-analysis of eight prospective randomized controlled trials. PLoS One 11(2):e0149312
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Makhni, M.C., Osorio, J.A., Park, P.J. et al. Cervical disc arthroplasty: tips and tricks. International Orthopaedics (SICOT) 43, 777–783 (2019). https://doi.org/10.1007/s00264-018-4259-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-018-4259-2