Abstract
Purpose
The aim of this study was to evaluate mid-term outcomes of Bankart repair with Hill-Sachs remplissage (BHSR) and to highlight prognostic factors of failure.
Methods
Thirty-four patients operated on for anterior shoulder instability with BHSR were enrolled in a prospective non-randomised study. Clinical and radiographic evaluation was performed at 1.5, three, six months and yearly thereafter. Outcome measures included Rowe and Walch-Duplay score.
Results
At mean follow-up of 35 months (24–63), the Rowe and Walch-Duplay scores reached respectively 92.7 and 88.2 points. The mean deficit in external rotation was 6° in ER1 and 1° in ER2 (p = 0.4, p = 0.9 respectively). Five patients (14.7%) had a recurrence of instability and three others had a persistent anterior apprehension. In the failure group, the Hill-Sachs lesion was deeper (26% vs 19% of the humeral diameter; p = 0.04) and range of motion at 1.5 months postoperatively was greater. Age at surgery, pre-operative instability severity index score (ISIS), hyperlaxity, type and level of sport, amount of glenoid bone loss had no correlation with failure rate.
Conclusions
The rate of failure at mid-term follow-up of BHSR was higher than commonly reported. The premature recovery of range of motion seems to be a clinical sign of failure at follow-up. Moreover, in case of deep Hill-Sachs lesion (>20%) an alternative procedure should be considered.
Level of evidence
Level IV.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
In 2004, Wolf and Pollack [22] described the arthroscopic technique of Hill-Sachs remplissage associated with a Bankart repair (BHSR) and ushered the perspective of a new option to treat anterior shoulder instability with the capsulotenodesis of the infraspinatus into the humeral head defect as an augmentation of the Bankart repair [23].
Most authors considered that the main criteria to indicate a Bankart repair reinforced with a remplissage procedure was the size of the Hill-Sachs lesion [2, 22, 23]. More recently the “glenoid track” concept took into account combined criteria as the position, the width and glenoid bone lost associated with the Hill-Sachs lesion. It depicted differently Hill-Sachs lesions that should be addressed because they could engage onto the glenoid rim and be responsible of a failure of a Bankart repair alone [9, 24]. The literature reported short-term promising outcomes after this surgical technique with a failure rate of less than 10% and no major complication [2, 4, 6, 10, 14, 15, 17, 25].
We hypothesised that arthroscopic BHSR performed primarily was a reliable option to treat chronic anterior shoulder instability without substantial glenoid bone loss. Thereby, the aim of this study was, firstly, to evaluate clinical outcomes at mid-term follow-up of this procedure and, secondly, to identify prognostic factors of failure.
Materials and methods
Patient selection
In a prospective design study, we included patients who had surgery between 2009 to 2013. Inclusion criteria were: (1) patient operated on for traumatic anterior shoulder instability with an Instability Severity Index Score (ISIS) above 3 points [1], (2) no substantial glenoid bone loss (<25%), (3) treated with an arthroscopic Bankart repair associated with a Hill-Sachs remplissage and (4) followed for a minimum of 24 months. Exclusion criteria were: (1) revision surgery, (2) voluntary instability in any direction and (3) first-time dislocation or subluxation. Patients gave their written agreement prior the enrolment and this study was approved by our local institutional review board.
Surgical technique
The procedure was performed by a single surgeon with the patient in a beach-chair position under general anaesthesia with an interscalene nerve block. Three different portals were used for the arthroscopic BHSR procedure: a standard posterior portal and anterosuperior portals for the Bankart repair and capsularshift, and an accessory posterolateral out-in portal for the remplissage of the humeral bone defect.
Firstly, with a 30° scope introduced in the posterior portal, the joint was explored, confirming Bankart lesion, the amount of glenoid and/or humeral bone defect, and antero-inferior capsular redundancy. Dynamically with abduction and external rotation of the arm, the “engaging” nature of Hill-Sachs lesion was explored [5]. Then, the labrum was mobilised from the two to six o’clock position and the anterior glenoid rim was debrided in order to prepare the Bankart repair. The anterior capsule was shifted upward with a temporary suture traction as described by Boileau et al. [3]. The first single loaded, impacted and absorbable anchor (Gryphon BR; DePuy Mitek, Raynham, MA, USA) was placed at the five o’clock position without tightening the suture in order to facilitated the next step.
Secondly, the scope was switched from posterior to anterior portal and the accessory posterolateral portal was created with a spine needle oriented perpendicular to the Hill-Sachs lesion. A posterior to anterior manual translation of the humeral head enhanced the view and the access to the posterior chamber. A working 6.5-mm cannula was pushed through the deltoid muscle and was positioned outside the joint, in the sub-deltoid space. The Hill-Sachs lesion was abraded directly with the drill guide used to insert the anchors. Two single loaded, impacted and absorbable anchors (Gryphon BR; DePuy Mitek) were placed in the valley of the defect, one superior and one inferior, through transtendinous passage. Then, with a penetrating grasper, one limb of each suture was retrieved through the posterior aspect of the capsule and the infraspinatus tendon, in order to prepare two mattress stitches (tied at the last step of the procedure).
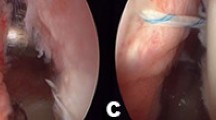
Thirdly, after switching back the scope in the posterior portal, the Bankart repair and the capsular shift was performed with a minimum of two others anchors placed at the four and three o’clock positions [3]. Then, the Hill-Sachs lesion was filled by tying blindly the two last mattress stitches one the bursal side of the infraspinatus, creating a capsulotenodesis (Fig. 1a-c).
Post-operative care
The arm was placed in a sling in internal rotation for six weeks, with no external rotation above the neutral position during this period. Self pendulum exercises were required immediately after the surgery and formal physiotherapy was delayed at three weeks. Sports activities without risk for the shoulder were allowed at three months, and overhead or contact sports at six months post-operatively.
Clinical evaluation
The patients were prospectively evaluated at six weeks, three months, six months and every year. After two years’ follow-up, clinical assessment was done during a specific visit by an independent observer. Active ranges of motion were measured pre-operatively and post-operatively, in forward flexion, external rotation elbow at side and at 90° of abduction, and internal rotation (level of the thumb on the spine). Pre-operative hyperlaxity was defined as an external rotation elbow at the side greater than 85° and/or a positive Gagey test [1]. An apprehension test in abduction external rotation was performed post-operatively at each review, beyond the third month. Objective functional results were evaluated with Rowe and Walch-Duplay scores, including sports activity, motion, pain, functional results, and stability [18, 21]. Subjective results were based on Simple Shoulder Value (SSV), ranging from 0 to 100% [12].
Radiographic evaluation
Pre-operatively, X-rays (anteroposterior and Bernageau views) and computed tomography (CT) scan (with three-dimensional reconstruction) or arthro-CT scan were systematically required to assess bone defects. On CT scan, Hill-Sachs lesion was qualified pre-operatively as “on-track” or “off-track” [9]. Its depth was quantified as the ration with the humeral head diameter. Glenoid bone defect was analysed using the Sugaya’s method [20].
Post-operatively, X-rays were performed at each review and allowed to follow radiographic evolution of absorbable anchors used for the Bankart repair and the Hill-Sachs remplissage. Signs of osteolysis around the anchors were carefully looking at. Glenohumeral osteoarthritis was classified according to Samilson and Prieto classification [19].
Statistical analysis
Measurements were expressed as the mean, range and standard deviation. The D’Agostino-Pearson test was used to analyse data distribution. Paired values were compared by using the paired t-test, and unpaired results were compared by using the Mann-Whitney test. The chi-squared or Fisher’s exact test was used to compare categorical data. The significance level was set at p < 0.05.
Results
Patient population
From November 2009 to January 2014, 191 patients were operated on for traumatic anterior instability of the shoulder in our department. Forty-three patients were treated with an arthroscopic BHSR. Thirty-seven patients fulfilled the inclusion criteria and three patients were excluded because of revision surgery, leaving 34 patients (34 shoulders) available for this study.
The mean age at the time of surgery was 26 years old (range, 15-49; ± 8.5); there were 30 males and 4 females. Twenty-four (70%) patients participated in at least one sports activity and 7 (30%) at a competitive level: 1 patient in a sports category without risk for the shoulder, 14 patients in a contact-sports category and nine patients in an overhead-sports category. There were signs of hyperlaxity in 13 (38%) shoulders and the mean preoperative ISIS was 4.2 ± 1.9 points (range, 3-9).
The dominant shoulder was involved in 13 cases (38%) and the mean number of dislocation and/or subluxation before the procedure was respectively 3.4 ± 4 (range, 0-20) and 11.7 ± 24 (range, 0-100) respectively. Only two patients did not report frank shoulder dislocation requiring a reduction manoeuvre in the emergency department and presented subluxation of their shoulder. The mean time between the first episode of instability and the procedure was 59 ± 67 months (range, 6-240).
On pre-operative radiographic analysis, all Hill-Sachs lesion were “on-track” and the mean depth was 20.1% ± 8.7 (range, 7-40). Only 11 (32%) patients had a bone loss on the glenoid side, with a mean of 12.1% ± 5.9 of the glenoid width (range, 5.4-23.2).
Overall functional results
At a mean follow-up of 35 months (range, 24–63), the mean Rowe and Walch-Duplay score achieved 92.7 ± 10.5 points (range, 58-100) and 88.2 ± 18.4 points (range, 35-100) respectively.
Comparing active range of motion pre-operatively and at last follow-up, the deficit in external rotation elbow at side and at 90° of abduction was of 6° and 1° respectively (p > 0.05) (Table 1).
Return to sport
Post-operatively, 18 (53%) patients resumed the same sports activities and 15 (44%) exactly at the same level. The delay to return to sport was 6.5 ± 3.4 months (5–13).
Recurrences
Five (14.7%) patients had a recurrence of instability with at least one subluxation or dislocation, and three others had persistent apprehension or pain in abduction external rotation during clinical examination without true instability. The five failures occurred during the firstyear period following the procedure (mean 10 months; range, 6-12). In the postoperative period, these patients recovered significantly faster range of motion than patients who remained stable overtime especially at 1.5 months (Fig. 2a-d). No significant correlations were found with the amount of glenoid bone loss, hyperlaxity, pre-operative ISIS, age at surgery, gender, sport activity and the risk of recurrent instability. However, unstable shoulders had a deeper Hill-Sachs lesion compared with stable shoulders (26% vs 19%) (Table 2).
Complications and reoperation
No iatrogenic post-operative complications were reported. One patient described a persistent posterior shoulder pain in abduction beyond six months after the surgery. An MRI identified a bursitis and inflammatory aspect of the infraspinatus muscle-tendon junction.
Three-fifths of the unstable patients after the primary surgery required a revision with an open Latarjet procedure without complication. All of them were stable with no apprehension at follow-up.
Radiographic analysis
At follow-up, two patients had signs of osteoarthritis and were classified type 2 according Samilson and Prieto classification (6%). Osteolysis around the anchors used for the remplissage was identified in two cases on Bernageau view, without clinical consequences.
Discussion
The purpose of this study was to evaluate clinical outcomes of arthroscopic BHSR in case of anterior shoulder instability. At mean follow-up of 35 months, the rate of recurrence reached 14.7% and two main predictive factors of failure were identified: the first was related to the deepness of the Hill-Sachs lesion and the second was related to the way of post-operative range-of-motion recovery.
The rate of recurrence after BHSR commonly reported was less than 10% [2, 4, 6, 14, 15, 17, 25]. Wolf et al. [23] found only 4% of recurrence at two to tenyear follow-up, even in case of critical glenoid bone defect. More recently, Garcia et al. [11] reported a rate of 12% at an average of five year follow-up. Revision surgery and increased preoperative number of dislocations were identified as predictive factors of failure. With 15% of subluxation at 30 months of follow-up, Park et al. [16] reported the highest rate, in a selected population with Hill-Sachs lesion of more than 25% of the humeral head diameter. Almost at the same follow-up and with a mean depth of 20%, our study supported this findings and gave a value to investigations of Hill-Sachs’ features.
Previously Burkhart et al. [5] described the so-called “engaging” lesion, when it engaged onto the glenoid rim during examination under arthroscopy. This dynamic concept was more accurately explained with the “glenoid track” theory, which took into account the position and the width of the Hill-Sachs lesion related to the amount of glenoid bone loss associated [9, 24]. An “off-track lesion” is at risk to engage and, thereby, should be considered as a predictive factor of recurrence after a Bankart repair alone. In our study, every Hill-Sachs were surprisingly “on-track” and should not be absolutely addressed according this concept. However, our indication of a BHSR was mostly based on pre-operative ISIS (above 3 points), the engaging nature during arthroscopic exploration of the Hill-Sachs lesion and the absence of substantial bone loss on the glenoid side. Respecting these criteria, Boileau et al. [2] reported a failure rate of 2% at short-term follow-up.
The depth of the Hill-Sachs lesion was the only pre-operative predictive parameter of failure of this series. One explanation would be related to non-healing of the capsulotenodesis into the Hill-Sachs lesion, leaving the Bankart repair alone to stabilise the shoulder [7, 8, 15, 16]. According a biomechanical model of the capsulotenodesis fixation into a Hill-Sachs lesion, we have shown that a deep and narrow defect made the fixation more critical (see Appendix). Basically, pull-out forces applied on the tendon are concentrated into the point of fixation of the tendon into the bone when the defect is deep and narrow. As a consequence, tissue healing into the Hill-Sachs lesion would be altered in these conditions.
The second predictive factor was clinical, with a faster range of motion recovery post-operatively in the unstable group of patient. Once again, this would explain a subsequent failure of the capsulotenodesis in the deep humeral defect. Previous studies reported that healing of the capsulotenodesis was successful in up to 75% after a remplissage [2, 14]. Unfortunately, we did not investigate the healing in our study, and could not validate the correlation with success or failure of the procedure.
According to these findings, the indication of BHSR is debatable in case of deep and engaging Hill-Sachs lesion. Degen et al. [8] proved that either Latarjet and BHSR procedures reduced frequency of dislocation in a 25% of humeral defect model on cadavers. However, Latarjet seemed to stabilise more specimens than BHSR (94% vs 84% of testing scenarios), and thereby could be proposed as an alternative procedure. The other option would be to consider a bone graft reconstruction [13].
This study has some limitations. The mean follow-up of 35 months remained too short to clearly determine the rate of recurrence after a BHSR, so that the number of failures would increase after the fifth year. Moreover, the amount of patients included was limited and other predictive factors of failure would probably be highlighted in a larger cohort. We did not perform a power analysis to increase the validity of our statistical methods. The second limitation was related to the lack of investigation in the healing of the capsulotenodesis of infraspinatus. Therefore, we could not correlate failures with this parameter.
Conclusions
The BHSR is a safe procedure to address anterior shoulder instability. However, in this series, the rate of failure at mid-term follow-up is higher than commonly reported. The depth of the Hill-Sachs of more than 20% of the humeral head would be a limit to indicate a BHSR, and an alternative surgery should be considered in this preoperative situation. Moreover, the premature recovery of range of motion would be a clinical indicator of failure at follow-up.
References
Balg F, Boileau P (2007) The instability severity index score. A simple pre-operative score to select patients for arthroscopic or open shoulder stabilisation. J Bone Joint Surg Br 89:1470–1477
Boileau P, O’Shea K, Vargas P, Pinedo M, Old J, Zumstein M (2012) Anatomical and functional results after arthroscopic Hill-Sachs remplissage. J Bone Joint Surg Am 94:618–626
Boileau P, Villalba M, Hery JY, Balg F, Ahrens P, Neyton L (2006) Risk factors for recurrence of shoulder instability after arthroscopic Bankart repair. J Bone Joint Surg Am 88:1755–1763
Brilakis E, Mataragas E, Deligeorgis A, Maniatis V, Antonogiannakis E (2016) Midterm outcomes of arthroscopic remplissage for the management of recurrent anterior shoulder instability. Knee Surg Sports Traumatol Arthrosc 24:593–600
Burkhart S, De Beer JF (2000) Traumatic glenohumeral bone defects and their relationship to failure of arthroscopic Bankart repairs: significance of the inverted-pear glenoid and the humeral engaging Hill-Sachs lesion. Arthroscopy 16:677–694
Buza JA 3rd, Iyengar JJ, Anakwenze OA, Ahmad CS, Levine WN (2014) Arthroscopic Hill-Sachs remplissage: a systematic review. J Bone Joint Surg Am 96:549–555
Cho NS, Yoo JH, Juh HS, Rhee YG (2016) Anterior shoulder instability with engaging Hill-Sachs defects: a comparison of arthroscopic Bankart repair with and without posterior capsulodesis. Knee Surg Sports Traumatol Arthrosc 24:3801-3808
Degen RM, Giles JW, Johnson JA, Athwal GS (2014) Remplissage versus latarjet for engaging Hill-Sachs defects without substantial glenoid bone loss: a biomechanical comparison. Clin Orthop Relat Res 472:2363–2371
Di Giacomo G, Itoi E, Burkhart SS (2014) Evolving concept of bipolar bone loss and the Hill-Sachs lesion: from “engaging/non-engaging” lesion to “on-track/off-track” lesion. Arthroscopy 30:90–98
Franceschi F, Papalia R, Rizzello G et al (2012) Remplissage repair—new frontiers in the prevention of recurrent shoulder instability: a 2-year follow-up comparative study. Am J Sports Med 40:2462–2469
Garcia GH, Wu HH, Liu JN, Huffman GR, Kelly JD 4th (2016) Outcomes of the remplissage procedure and its effects on return to sports: average 5-year follow-up. Am J Sports Med 44:1124–1130
Gilbart MK, Gerber C (2007) Comparison of the subjective shoulder value and the constant score. J Shoulder Elb Surg 16:717–721
Lynch JR, Clinton JM, Dewing CB, Warme WJ, Matsen FA 3rd (2009) Treatment of osseous defects associated with anterior shoulder instability. J Shoulder Elb Surg 18:317–328
Merolla G, Paladini P, Di Napoli G, Campi F, Porcellini G (2015) Outcomes of arthroscopic Hill-Sachs remplissage and anterior Bankart repair: a retrospective controlled study including ultrasound evaluation of posterior capsulotenodesis and infraspinatus strength assessment. Am J Sports Med 43:407–414
Nourissat G, Kilinc AS, Werther JR, Doursounian L (2011) A prospective, comparative, radiological, and clinical study of the influence of the “remplissage” procedure on shoulder range of motion after stabilization by arthroscopic Bankart repair. Am J Sports Med 39:2147–2152
Park MJ, Tjoumakaris FP, Garcia G, Patel A, Kelly JD 4th (2011) Arthroscopic remplissage with Bankart repair for the treatment of glenohumeral instability with Hill-Sachs defects. Arthroscopy 27:1187–1194
Rashid MS, Crichton J, Butt U, Akimau PI, Charalambous CP (2016) Arthroscopic “remplissage” for shoulder instability: a systematic review. Knee Surg Sports Traumatol Arthrosc 24:578–584
Rowe CR, Patel D, Southmayd WW (1978) The Bankart procedure: a long-term end-result study. J Bone Joint Surg Am 60:1–16
Samilson RL, Prieto V (1983) Dislocation arthropathy of the shoulder. J Bone Joint Surg Am 65:456–460
Sugaya H, Moriishi J, Dohi M, Kon Y, Tsuchiya A (2003) Glenoid rim morphology in recurrent anterior glenohumeral instability. J Bone Joint Surg Am 85:878–884
Walch G (1991) Recurrent shoulder dislocation. Rev Chir Orthop Reparatrice Appar Mot 77:178–192
Wolf EM, Pollack ME (2004) Hill-Sachs “remplissage”: an arthroscopic solution for the engaging Hill-Sachs lesion. Arthroscopy 20:14–15
Wolf EM, Arianjam A (2014) Hill-Sachs remplissage, an arthroscopic solution for the engaging Hill-Sachs lesion: 2- to 10-year follow-up and incidence of recurrence. J Shoulder Elb Surg 23:814–820
Yamamoto N, Itoi E, Abe H, Minagawa H, Seki N, Shimada Y, Okada K (2007) Contact between the glenoid and the humeral head in abduction, external rotation, and horizontal extension: a new concept of glenoid track. J Shoulder Elb Surg 16:649–656
Zhu YM, Lu Y, Zhang J, Shen JW, Jiang CY (2011) Arthroscopic Bankart repair combined with remplissage technique for the treatment of anterior shoulder instability with engaging Hill-Sachs lesion: a report of 49 cases with a minimum 2-year follow-up. Am J Sports Med 39:1640–1647
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Funding
There was no funding source.
Ethical approval
The institutional review board approved this study. This article was approved by our Ethical Committee of Research.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Appendix
Appendix
The Hill-Sachs lesion was modelled by a triangular notch as described in Fig. 3. The shape factor u described the ratio of the half-length x by the depth of the lesion l. The tendon tension force F was balanced by the button force B and by the reaction force (normal force N, tangential force T) of one face of the lesion. This force located by s along the lesion face was dependent upon the friction coefficient f and adhesion angle ϕ between the tendon and the host bone. The resolution of the static equilibrium of the tendon segment gave the forces N, T and B which were scaled by dividing by F, and the location of the reaction force on the bone which was scaled by the contact length of the tendon with the lesion.
The first order Taylor expansion of output measures g(u) was obtained by eq. (2a), δu being the perturbation of the variable u. The sensitivity of g(u) was expressed by eq. (2b) and g(u) was successively N(u), T(u), B(u) and s(u). The sensitivities S N(u) , S T(u ), S B(u) and S s(u) obtained from eq. (2) were scaled relative to the normal force sensitivity as shown in eq. (2c). Forces and location were shown in Fig. 4a and b for u varying from 0.5 to 1.5 and f = 0.2.
a Distribution pattern of forces (normal force N, tangential force T, button force B) and location s of the bone-tendon resulting force in the triangular model of the Hill-Sachs lesion for u = x / l describing the shape factor. b Sensitivities of B, T and s scaled to N sensitivity for u varying from 0.5 to 1.5
Figure 4a showed that all forces were increasing with the u increase. The force B applied by the button upon the tendon was significantly dependent upon the shape factor u of the lesion. For lower value corresponding with a narrow lesion, this force was lower than the tension for F on the tendon. On the contrary, the contribution of the button in the equilibrium of the assembling was increasing for larger value of u corresponding with lesions that were more open.
Whatever u values, the normal force N between the tendon and the bone lesion was greater than 1 which meant that the force at the interface between the lesion and the tendon was greater than the tension force F into the tendon. The tangential force T was lower than 0.5. These forces should favour the initial tissue healing at the tendon-bone interface and further remodelling. Despite this, it was found that for lower values of shape factor, the interface forces were significantly decreasing. Moreover, the location s of these forces was moving towards the extremity of the interface (s ∼0.1), which meant that the forces were concentrated and that the amount of host tissue involved into the healing was diminished.
The friction coefficient between the tendon and the host bone affected the forces magnitudes and the non-linear variation with u, but it did not drastically the distribution patterns.
The relative sensitivity to the lesion shape factor u plotted in Fig. 4b provided complementary information. The ratio between tangential force T and normal force N was independent from u but the contribution of the button force B and the force location s compared with that of the normal force N was strongly influence by the shape factor especially for narrow lesion. For u ≥ 1 the relative sensitivities tended to be independent from the shape factor. In other terms, for depth lesion, the initial condition of tendon fixation into the lesion could be more critical for the postoperative tissue healing and it could be more dependent upon the surgical technique.
Rights and permissions
About this article
Cite this article
Bonnevialle, N., Azoulay, V., Faraud, A. et al. Results of arthroscopic Bankart repair with Hill-Sachs remplissage for anterior shoulder instability. International Orthopaedics (SICOT) 41, 2573–2580 (2017). https://doi.org/10.1007/s00264-017-3491-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-017-3491-5