Abstract
Purpose
The hypothesis of this study was that femoral implant migration would not differ between simultaneous bilateral or unilateral short-stem THA.
Method
Implant migration of 202 femoral short-stems (100 unilateral and 102 one-stage bilateral cases) in 151 patients was assessed by “Ein-Bild-Roentgen-Analysis Femoral-Component-Analysis” in a two years follow-up (2.0-3.0 years). Migration patterns of unilateral and simultaneous cases were analysed and compared.
Results
There was no difference between the two groups regarding age, body mass index and gender. After two years mean subsidence of all 202 implants was 1.43 mm (-6.5 mm to 2.0 mm). After initial subsidence of 0.37 mm per month within the first six weeks, the mean monthly migration was reduced to 0.02 mm between one and two years post-operative. There was no statistical difference in mean migration between unilateral (1.34 mm) and simultaneous bilateral (1.51 mm) THA (p = 0.33).
Conclusion
In summary, two years post-operative there was no difference in the amount of mean implant subsidence between unilateral compared to simultaneous bilateral short-stem THA. This suggests that regarding implant fixation simultaneous bilateral short-stem THA is as safe and successful as a solely unilateral intervention.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
A recent analysis of the Swedish hip arthroplasty register revealed that 17 % of all patients receiving primary total hip arthroplasty (THA) suffer from bilateral symptoms of osteoarthritis [1]. Simultaneous bilateral THA might be an alternative to staged unilateral THA in this group of patients. Most studies describe low complication rates in simultaneous bilateral THA that are comparable to unilateral THA [2, 3]. Most authors agree with the need for proper patient selection for one-stage bilateral THA, especially with respect to a low ASA (grade I and II) score [3–5]. However, these rather healthy and post-operatively mobile patients might be at greater risk of early implant migration because of full weight bearing on both operated hips after surgery [6]. As a possible consequence, a slightly higher risk of implant revision was found in the Swedish hip arthroplasty register for patients undergoing one-stage bilateral compared to unilateral THA [1]. Early implant migration with subsidence of more than 1.5 mm within the first two years after operation is associated with a higher risk of implant failure [7]. However, in a RSA-study investigating the subsidence of a straight stem (CLS, Zimmer, Warsaw, Indiana) there was no difference found in patients with restricted versus unrestricted post-operative weight bearing for the first three months after surgery [8].
Cementless femoral short-stem arthroplasty is a bone-sparing and soft-tissue preserving alternative to conventional THA [9]. There are only a few studies describing the migration pattern of femoral short-stems [10–12]. Their short-term migration pattern showed comparable results to conventional straight stems [7, 8, 10, 12]. So far there is no study assessing the influence of simultaneous bilateral short-stem implantation on the migration pattern of the femoral implant.
We hypothesised that femoral implant migration at two years follow-up would not differ between simultaneous bilateral or unilateral THA within the first two years after surgery, assessed by “Ein-Bild-Roentgen-Analysis Femoral-Component-Analysis” (EBRA-FCA).
Patients and methods
After institutional review board approval (323/13) we identified 216 consecutive femoral short-stem implantations in 162 patients at a single institution from an ongoing prospective observational study. All patients were informed about the study and signed a consent form. Unilateral THA was performed in 108 patients. Furthermore, 54 patients (108 hips) with bilateral osteoarthritis underwent simultaneous bilateral THA. Inclusion criteria were a minimum follow-up of two years, a series of at least three consecutive radiographs accepted by the EBRA-FCA software, and acceptance of the direct post-operative and the 24 months follow-up radiograph. Eight patients (ten hips) had to be excluded because of an incomplete radiological series and three patients (four hips) deceased unrelated to the operation. There was no revision with exchange of any implant within the mean follow-up time of 2.2 years (2.0-3.0 years). Finally, inclusion criteria were fulfilled in 100 patients (100 hips) with unilateral THA and 51 patients (102 hips) with bilateral THA. The mean age of the 66 female and 85 male patients was 62.7 years (32 to 87 years) with a mean BMI of 27.9 kg/m2 (19 to 45 kg/m2) (Table 1). There was no significant difference between the two groups in respect to primary diagnosis nor pre- and post-operative pain levels and blood loss (p > 0.05).
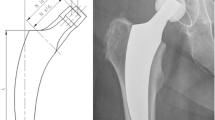
All patients received a cementless optimys short-stem (Mathys, Bettlach, Switzerland) (Fig. 1). The optimys short-stem is a type 2A short-stem according to the classification of Khanuja et al. [13]. The prosthesis is made of a titanium alloy with a plasma-sprayed surface and a calcium phosphate coating. The profile of the stem is tapered in three planes with a trapezoidal cross-section to provide femoral press-fit fixation. There are two different offset options to better reconstruct the individual anatomy. The acetabular component was a cementless press-fit cup (RM Pressfit vitamys, Mathys, Bettlach, Switzerland or Fitmore cup, Zimmer, Warsaw, USA) with a 28-mm alumina-on-highly crosslinked polyethylene bearing in all hips. All surgery was performed in the supine position using a modified anterolateral approach [14]. Full-weight-bearing, using two crutches for three weeks, was allowed in both groups immediately after surgery. Standardised digital anteroposterior radiographs of the pelvis were obtained post-operative, at six weeks, six months, 12 months and yearly thereafter.
EBRA-FCA was used to determine implant migration [15]. Implant subsidence was measured on serial radiographs in regards to the first available post-operative image of the individual case. In order to correct magnification each image was calibrated with the diameter of the head of the prosthesis. For identification of subsidence a total of 19 reference points were defined at every single radiograph (Fig. 2). Six points calculate the centre of the head, the femoral cortex is defined by eight points and the stem axis by three reproducible spots. Furthermore, the level of the greater trochanter, a point at the intersection of two defined tangents on the lesser trochanter and the tip of the prosthesis are identified. These points define predetermined distances, which are compared by the EBRA-FCA software to calculate implant migration. The EBRA-FCA software excludes radiographs with significant positioning artifacts.
Implant migration
-
1.
Implant migration of all available cases was assessed six weeks, six months, 12 months and two years after surgery in relation to the direct post-operative state.
-
2.
Furthermore, monthly migration rate was evaluated for the complete follow-up period.
Radiological examination
Post-operative radiographs were examined after two years for signs of loosening, respectively bony ingrowth [16]. Stable fixation by bone ingrowth was defined by the appearance of only minimal or no radiolucent line formation around the femoral stem.
Intra-observer reliability
Intra-observer reliability was determined by performing double measurements of 40 radiographs by one observer.
Statistics
Statistical analysis was performed with SAS 9.2 (SAS Institute, Cary, North Carolina). All variables were summarised using standard descriptive statistics. Values are reported as mean (SD) and range, qualitative categories are presented as number and percentage. The Kolmogorov-Smirnov test was used to analyse distribution of the results. Due to not normal distribution of the findings the Wilcoxon signed-rank test was used to determine differences of the unilateral and bilateral group regarding age, height, weight, BMI and gender. Furthermore, it was used to analyse subsidence at the different follow-up examination within each group. To analyse the differences between unilateral and bilateral procedures at different follow-up terms (no normal distribution, more than two independent samples) the Kruskal-Wallis-test was used. Significant results were defined with a p-value ≤ 0.05. A post-hoc power analysis was performed to determine the differences in mean stem migration between both groups.
To assess potential variations between two sets of measurements the t-test described good reliability if the difference was not significant (p > 0.05). Furthermore, Pearson product-moment correlation (PCC) was assessed to measure the strength of the relationship between two measurements (p > 0.700 high correlation).
Results
A total of 954 radiographs were analysed by one observer. The EBRA-FCA accepted 942 images and rejected 12 radiographs (1.2 %). The radiographs of 202 hips were included directly post-operative (100 unilateral and 102 bilateral), 178 images after six weeks (90 unilateral and 88 bilateral), 185 images after six months (95 unilateral and 90 bilateral), 175 radiographs after 12 months (88 unilateral and 87 bilateral) and 202 images after 24 months (100 unilateral and 102 bilateral).
Implant migration
-
1.
Mean axial migration continued over the whole follow-up period. The average axial subsidence of all implants at six weeks was 0.55 mm (-5.0 to 0.6 mm), at six months 0.90 mm (-5.4 to 1.2 mm), at 12 months 1.14 mm (-5.9 to 1.6 mm) and after 24 months 1.43 mm (-6.5 to 2 mm) (Fig. 3). There was a statistically significant migration within the first six post-operative weeks, likewise between six weeks and six months post-operative, six months and 12 months post-operative and 12 months and 24 months post-operative (p < 0.001). There was no difference in axial migration between the unilateral and simultaneous bilateral THA after two years (p = 0.32; Fig. 4). Furthermore, the average migration was equal after six weeks, six months and 12 months between both groups (Table 2). The post-hoc power analysis detected a power between 69 % (two years post-operative) and 90 % (six weeks post-operative) with an alpha failure of 0.05. Implant migration greater than 1.5 mm was observed in 79 of all 202 (39 %) cases, concerning 44 (43 %) implants after bilateral THA and 35 (35 %) after unilateral short-stem implantation (odd-ratio 1.4).
Table 2 Mean subsidence in the unilateral and bilateral group -
2.
Average monthly implant migration was 0.37 mm in the first 6 weeks postoperative for all cases, 0.08 mm between six weeks and six months, 0.04 mm between six months and 12 months and 0.02 mm between 12 months and 24 months post-operative. Within the first six weeks after surgery monthly implant migration was 0.42 mm following bilateral THA compared to 0.31 mm after unilateral arthroplasty. In the second post-operative year migration rate stabilised with 0.02 mm per month in both groups.
Radiological examination
No implant had to be revised and all devices were considered stable on plain radiographs with signs of fixation by bony ingrowth.
Intra-observer reliability
Intra-observer reliability was excellent, there was no significant difference between the first and second measurement (p = 0.77), which was reflected by a PCC of 0.998.
Discussion
Immediate full weight bearing after THA was initially performed in the 1990s following one-staged bilateral uncemented THA [17]. Until today there is controversy about the safety of immediate full weight bearing concerning implant stability, migration and osteointegration, especially in one-staged bilateral THA [18]. The main hypothesis of this EBRA-FCA-migration-study was to determine differences in implant subsidence between unilateral and simultaneous bilateral short stem THA two years after surgery.
Mean axial subsidence of all implants was 1.43 mm after two years. There was no significant difference in implant migration between unilateral and bilateral procedures. Markmiller et al. found no significant influence of partial compared to full weight bearing after cementless THA using a Spotorno-type straight stem in terms of femoral implant migration and bony ingrowth [19]. These findings were confirmed in a one-year RSA investigation comparing full weight bearing versus partial weight bearing for the first six weeks after unilateral ABG (Stryker-Howemedica, Mahwah, New Jersey) THA [20].
An in-vitro comparison of the optimys short-stem with a conventional straight-stem showed more physiological proximal load transmission of the short-stem, but neither implant could avoid stress shielding [21]. Furthermore, primary stability of the short-stem prosthesis was equal compared to the straight-stem, with implant-bone micromotions below the critical threshold of 150 μm. The investigated optimys short-stem can be classified as type 2A according to Khanuja et al. [13]. Cumulated short-term survival of type 2A short-stems was over 98 % after a mean observation period of 2.9 years in the mentioned review [13]. There are limited studies investigating implant migration after short-stem THA. Using EBRA-FCA the type 2A Metha short-stem (Braun-Aesculap, Tuttlingen, Germany) showed a mean migration of 0.7 mm after two years with partial weight bearing for the first two post-operative weeks [12]. In contrast, a mean migration of 2.04 mm after one year was described for the same type of implant with immediate full weight-bearing [22]. In the same study the Nanos short-stem (type 2A, Smith & Nephew GmbH, Marl, Germany) subsided 1.96 mm within one year after surgery. Both studies described an initial migration with stabilisation thereafter [12, 22]. In addition, a recent RSA study of the Nanos short-stem showed total implant migration of 0.46 mm two years after surgery [23]. All patients in the mentioned study performed immediate full weight bearing and almost 90 % of total migration occurred within the first three months after implantation. These findings are comparable to our investigation of the optimys short-stem migration pattern. In the group of shortened tapered conventional stems, which can be classified as type 4 according to Khanuja et al. the short-term survival rate after a mean follow-up of 3.7 years was 100 % with aseptic loosening as the end point [13]. The type 4 short-stem SMF (Smith&Nephew, Memphis, Tennessee) showed a mean migration of 0.94 mm after two years using RSA [24]. In this randomised study the implant subsidence was compared to a conventional straight stem, which migrated 0.32 mm after two years. All patients performed partial weight bearing for six weeks after surgery. No statistically significant difference was found between both groups (p = 0.66). The migration pattern of the Fitmore stem (type 4, Zimmer, Warsaw, USA) was observed in an EBRA-FCA study of 72 hips with a mean subsidence of 1.0 mm after two years with full weight-bearing immediately after surgery [10]. Similar to our study all type 4 stems showed an initial migration with stabilisation thereafter.
Implant migration was most pronounced in the early post-operative period with an average of 0.37 mm per month compared to 0.02 mm per month between one and two years after surgery for all implants in our study. Initial monthly migration was more pronounced in the bilateral group compared to the unilateral group within the first six weeks post-operative with stabilisation thereafter in all cases. Rao et al. compared femoral subsidence on conventional radiographs and clinical results after unilateral and simultaneous bilateral uncemented THA [6]. Bilateral THA with immediate full weight-bearing showed more initial subsidence of the femoral component compared to the unilateral group, but there was no difference in implant stability after two years [6]. Our findings are comparable to this study in that early implant migration was more pronounced after bilateral compared to unilateral THA. Nevertheless, between six weeks and two years after surgery subsidence was not statistically different between both groups. Furthermore, mean monthly implant migration was equal for both groups within the second post-operative year. These findings suggest a tendency towards more initial migration after bilateral compared to unilateral THA without compromising mid-term stability of the femoral device.
The main limitations of this study relate to the short follow-up period of two years and the fact that the migration pattern of the optimys stem may be specific and not comparable to other implants [25]. Nevertheless, the monthly amount of migration decreased over time and none of the implants had to be revised for any reason. Still, further investigation of implant stability and migration is necessary. Furthermore, the study was performed retrospectively instead of a prospective study design and EBRA-FCA was used rather than the more accurate RSA technique. However, EBRA-FCA does not need additional surgical efforts and demonstrated high accuracy in previous investigations [10, 15]. Biedermann et al. showed an accuracy of EBRA-FCA better than ±1.5 mm (95 % percentile) [15]. Intra-observer reliability in this study was excellent with a PCC of 0.998 demonstrating a good reproducibility of the measurements.
In summary, there was no statistical difference in the amount of mean implant subsidence between unilateral compared to simultaneous bilateral short-stem THA two years post-operatively. Nevertheless, there was a tendency towards more initial migration within the first six weeks after bilateral simultaneous THA with immediate unrestricted full weight-bearing compared to unilateral THA with the possibility of less impact because of an unaffected contralateral hip joint. Furthermore, the amount of implant migration varies between different types of femoral short-stem devices, which might also be influenced by the post-operative weight-bearing protocol.
References
Garland A, Rolfson O, Garellick G, Karrholm J, Hailer NP (2015) Early postoperative mortality after simultaneous or staged bilateral primary total hip arthroplasty: an observational register study from the Swedish hip arthroplasty register. BMC Musculoskelet Disord 16(8):77. doi:10.1186/s12891-015-0535-0
Kim YH, Kwon OR, Kim JS (2009) Is one-stage bilateral sequential total hip replacement as safe as unilateral total hip replacement? J Bone Joint Surg (Br) 91(3):316–320. doi:10.1302/0301-620X.91B3.21817
Stavrakis AI, SooHoo NF, Lieberman JR (2015) Bilateral total hip arthroplasty has similar complication rates to unilateral total hip arthroplasty. J Arthroplasty 30(7):1211–1214. doi:10.1016/j.arth.2015.02.015
Pfeil J, Hohle P, Rehbein P (2011) Bilateral endoprosthetic total hip or knee arthroplasty. Dtsch Arztebl Int 108(27):463–468. doi:10.3238/arztebl.2011.0463
Lamo-Espinosa J, Troncoso S, Valenti-Azcarate A, Diaz de Rada P, Valenti-Nin JR (2015) Clinical and radiological short-term complications after single-stage bilateral uncemented total hip arthroplasty. Musculoskelet Surg 99(1):67–73. doi:10.1007/s12306-014-0342-z
Rao RR, Sharkey PF, Hozack WJ, Eng K, Rothman RH (1998) Immediate weightbearing after uncemented total hip arthroplasty. Clin Orthop Relat Res 349:156–162
Krismer M, Biedermann R, Stockl B, Fischer M, Bauer R, Haid C (1999) The prediction of failure of the stem in THR by measurement of early migration using EBRA-FCA. Einzel-Bild-Roentgen-Analyse-femoral component analysis. J Bone Joint Surg (Br) 81(2):273–280
Wolf O, Mattsson P, Milbrink J, Larsson S, Mallmin H (2010) Periprosthetic bone mineral density and fixation of the uncemented CLS stem related to different weight bearing regimes: a randomized study using DXA and RSA in 38 patients followed for 5 years. Acta Orthop 81(3):286–291. doi:10.3109/17453674.2010.487238
Falez F, Casella F, Panegrossi G, Favetti F, Barresi C (2008) Perspectives on metaphyseal conservative stems. J Orthop Traumatol 9(1):49–54. doi:10.1007/s10195-008-0105-4
Freitag T, Kappe T, Fuchs M, Jung S, Reichel H, Bieger R (2014) Migration pattern of a femoral short-stem prosthesis: a 2-year EBRA-FCA-study. Arch Orthop Trauma Surg 134(7):1003–1008. doi:10.1007/s00402-014-1984-x
Rohrl SM, Li MG, Pedersen E, Ullmark G, Nivbrant B (2006) Migration pattern of a short femoral neck preserving stem. Clin Orthop Relat Res 448:73–78. doi:10.1097/01.blo.0000224000.87517.4c
Schmidutz F, Graf T, Mazoochian F, Fottner A, Bauer-Melnyk A, Jansson V (2012) Migration analysis of a metaphyseal anchored short-stem hip prosthesis. Acta Orthop 83(4):360–365. doi:10.3109/17453674.2012.712891
Khanuja HS, Banerjee S, Jain D, Pivec R, Mont MA (2014) Short bone-conserving stems in cementless hip arthroplasty. J Bone Joint Surg Am 96(20):1742–1752. doi:10.2106/JBJS.M.00780
Watson-Jones R (1936) Fractures of the neck of the femur. Br J Surg 23:787–808
Biedermann R, Krismer M, Stockl B, Mayrhofer P, Ornstein E, Franzen H (1999) Accuracy of EBRA-FCA in the measurement of migration of femoral components of total hip replacement. Einzel-Bild-Rontgen-Analyse-femoral component analysis. J Bone Joint Surg (Br) 81(2):266–272
Engh CA, Bobyn JD, Glassman AH (1987) Porous-coated hip replacement. The factors governing bone ingrowth, stress shielding, and clinical results. J Bone Joint Surg (Br) 69(1):45–55
Ritter MA, Vaughn BK, Frederick LD (1995) Single-stage, bilateral, cementless total hip arthroplasty. J Arthroplasty 10(2):151–156
Radl R, Aigner C, Hungerford M, Pascher A, Windhager R (2000) Proximal femoral bone loss and increased rate of fracture with a proximally hydroxyapatite-coated femoral component. J Bone Joint Surg (Br) 82(8):1151–1155
Markmiller M, Weiss T, Kreuz P, Ruter A, Konrad G (2011) Partial weightbearing is not necessary after cementless total hip arthroplasty: a two-year prospective randomized study on 100 patients. Int Orthop 35(8):1139–1143. doi:10.1007/s00264-010-1089-2
Thien TM, Ahnfelt L, Eriksson M, Stromberg C, Karrholm J (2007) Immediate weight bearing after uncemented total hip arthroplasty with an anteverted stem: a prospective randomized comparison using radiostereometry. Acta Orthop 78(6):730–738. doi:10.1080/17453670710014491
Bieger R, Ignatius A, Reichel H, Durselen L (2013) Biomechanics of a short stem: in vitro primary stability and stress shielding of a conservative cementless hip stem. J Orthop Res 31(8):1180–1186
Brinkmann V, Radetzki F, Delank KS, Wohlrab D, Zeh A (2015) A prospective randomized radiographic and dual-energy X-ray absorptiometric study of migration and bone remodeling after implantation of two modern short-stemmed femoral prostheses. J Orthop Traumatol 16(3):237–243. doi:10.1007/s10195-015-0335-1
Budde S, Seehaus F, Schwarze M, Hurschler C, Floerkemeier T, Windhagen H et al (2015) Analysis of migration of the Nanos(R) short-stem hip implant within two years after surgery. Int Orthop. doi:10.1007/s00264-015-2999-9
McCalden RW, Korczak A, Somerville L, Yuan X, Naudie DD (2015) A randomised trial comparing a short and a standard-length metaphyseal engaging cementless femoral stem using radiostereometric analysis. Bone Joint J 97-B(5):595–602. doi:10.1302/0301-620X.97B5.34994
Ruben RB, Fernandes PR, Folgado J (2012) On the optimal shape of hip implants. J Biomech 45(2):239–246. doi:10.1016/j.jbiomech.2011.10.038
Acknowledgments
The authors thank Semra Kocak for the statistical analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
An erratum to this article is available at http://dx.doi.org/10.1007/s00264-016-3205-4.
Rights and permissions
About this article
Cite this article
Kutzner, K.P., Freitag, T., Kovacevis, MP. et al. One-stage bilateral versus unilateral short-stem total hip arthroplasty: comparison of migration patterns using “Ein-Bild-Roentgen-Analysis Femoral-Component-Analysis”. International Orthopaedics (SICOT) 41, 61–66 (2017). https://doi.org/10.1007/s00264-016-3184-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-016-3184-5