Abstract
The aim of this study was to investigate the characteristics of proprioception in patients with an anaterior-cruciate-ligament (ACL)-injured knee and to determine whether there is a correlation between proprioception and performance. We studied 32 patients with unilateral isolated ACL ruptures. Proprioception of the knee was evaluated by examining the joint position sense. Functional performance was evaluated with the one-leg hop (OLH) and one-leg vertical jump (OLV) tests. The mean error angle of the joint position sense was 3.6±1.5° on the intact side and 5.2±1.9° on the injured side. The joint position sense was thus clearly reduced on the injured side (p<0.05). The distance of jumping in the OLH test and the height of jumping in the OLV test was also clearly reduced on the injured side compared with that on the intact side (p<0.01) both with and without visual control. Moreover, we found a significant correlation between proprioception and performance in the ACL-injured knees, and this correlation was more distinct with visual deprivation. In conclusion, decreased proprioception in patients with ACL deficiency reduced their functional ability.
Résumé
Le but de cette étude était d’étudier les caractéristiques de proprioception chez les malades avec une lésion du LCA, et déterminer s’il y avait une corrélation entre proprioception et performance. Nous avons étudié 32 malades avec une rupture isolée unilatérale du LCA. La proprioception du genou a été évalué en examinant le sens des positions de l’articulation. La fonction a été évaluée avec le saut à cloche-pied (OLH) et saut vertical unipodal (OLV). L’angle moyen d’erreur de position était 3,6±1,5° sur le côté intact et 5,2±1,9° sur le côté blessé. Le sens de position était donc notablement réduit du côté blessé (p<0.05). La distance de saut dans l’épreuve OLH et la hauteur du saut dans l’épreuve OLV ont aussi été réduite du côté blessé comparé avec le côté intact (p<0.01) les deux avec et sans contrôle visuel. De plus, nous avons trouvé une corrélation certaine entre proprioception et performance dans les genoux avec lésion du LCA, et cette corrélation était encore plus nette avec privation visuelle. En conclusion, la diminution de la proprioception chez les malades avec une insuffisance du LCA à réduit leur capacité fonctionnelle.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
There are several studies on proprioception in knees with a ruptured anterior cruciate ligament (ACL) [3–5, 7]. Barrack et al. [2] reported decreased proprioception in knees with a ruptured ACL on the basis of an evaluation of the joint position sense. Ochi et al. [15] also studied joint position sense in knees with a ruptured ACL and demonstrated decreased joint position sense in patients with marked knee instability. However, there are also reports denying a relationship between ACL injury and changes in proprioception [9].
On the other hand, changes in the exercise ability of patients with a ruptured ACL have long been studied, and the majority of studies showed decrease in performance [1, 20]. Among various methods that have been used in evaluating performance, Noyes et al. [14] and Itoh et al. [11] recommended the one-leg hop (OLH) test as a simple and reliable test.
Thus, it is becoming increasingly clear that knees with ruptured ACL gradually develop changes not only in performance but also in proprioception. However, as reported by Noyes et al. [13], we encounter individuals who readily perform high levels of athletic activities despite injury to the ACL [6]. In this connection, evaluation of how changes in proprioception of knees with a ruptured ACL is reflected in athletic activities is considered important. The objective of this study was to prospectively study proprioception and performance in individuals with an isolated injury of the ACL and to evaluate the relationship between them.
Materials and methods
Thirty-two patients with 32 knees with a ruptured ACL consented to enrollment after having received an explanation of the intention of the study. The patients had no other lower-limb disorders, were aged between 16 and 40 (mean 25.6) years, and consisted of 17 males and 15 females. The left knee was injured in 14 and the right in 18. All patients had a diagnostic arthroscopy performed shortly after injury, and a rupture of the ACL was confirmed. In six patients, an injury of the lateral meniscus was observed and in one a grade I injury of the medial collateral ligament. In three, a partial meniscectomy was performed. Immediately after diagnosis, rehabilitation was started (e.g., icing, emphasizing hamstring muscle strengthening, range of motion exercise, and weight-bearing exercise). The patients were judged to have recovered from the acute period on the basis of absence of inflammatory signs, absence of pain—also during walking—and no restriction in range of motion. The mean period of rehabilitation was 5.6 (3–11) months.
Proprioception measurement
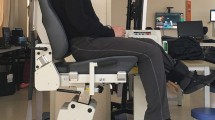
Proprioception of the knee was evaluated by examining the joint position sense according to the methods of Skinner et al. [18] and Ochi et al. [15]. In brief, the measurement method was first explained to the subjects until they understood it. The subjects wore short pants to eliminate external stimulation and a pair of special boots during measurement. They also wore eye masks and headphones to block visual and acoustic stimulation. Then, using a Biodex machine, the knee was extended slowly from 90° flexion at an angle velocity of 10°/s. Extension was stopped for 3 s at a randomly determined angle between 5° and 25°. The subject was instructed to remember this angle, and the knee was returned to 90° flexion. The subject was instructed to extend the knee to the angle that the subject remembered and to push the hold switch of the Biodex at that point. The difference between the angle initially determined by the examiner and the angle that the subject remembered (“error angle”) was measured. This test was performed ten times with each leg, and the mean error angle was used for analysis. The intact legs were regarded as the control group.
Functional performance measurement
The OLH and one-leg vertical jump (OLV) tests were adopted as the performance tests. The measurements were carried out after the subjects had warmed up sufficiently for 5 min by exercising, including pedaling an aerobike. The hop test, as developed by Barber et al. [1], was designed to assess both strength and confidence in the leg. Standing on one leg with the hands free along the side, the patients hop as far forward as possible on the same leg, and the distance hopped was measured. The OLV test was performed according to Gobbi et al. [8]. Standing on one leg with hands free along the side, the subject was instructed to jump vertically as high as possible, landing on the same leg. Both the OLH and OLV were carried out with and without visual control. The measurements were performed five times with each leg and with the eyes open and closed, respectively. The mean values for distance and height were used for analysis.
Statistical analysis
The two-tailed Student’s t test was used for comparisons within and between the groups, and Pearson’s coefficients of correlation were calculated. All statistical procedures were performed using the Stat-View software. A p value of less than 0.05 was considered significant.
Results
The mean error angle of the joint position sense was 3.6±1.5° on the intact side and 5.2±1.9° on the injured side (p<0.05). The distance of jumping in the OLH test was clearly reduced on the injured side compared with that on the intact side (p<0.01) both with the eyes open and closed. Similarly, the height of jumping in the OLV was clearly reduced on the injured side compared with that on the intact side (p<0.01) both with the eyes open and closed (Table 1). Vision did not affect the performance on the same side, i.e., there was no significant difference in the performance of the injured leg or the intact leg between the open-eye and closed-eye conditions (Table 1).
On the intact side, there was no correlation between OHL, respectively, OLV, and joint position sense, regardless of the visual condition. On the injured side, however, a correlation was observed (Table 2) [(p<0.05)], and this correlation was more pronounced when the eyes were closed. In patients who showed large inaccuracy of the joint position sense on the injured side, the distance of jumping and of height was reduced (Figs. 1, 2), and more so with the eyes closed (Table 2).
Discussion
The most important role that ligaments, including the ACL, play is providing mechanical support to the joint. Disruption of this support mechanism changes the joint kinematics and induces joint instability and osteoarthritic changes [10, 17]. However, Kennedy et al. [12] reported in 1982 that clinical symptoms characteristic of knees with ACL injury (e.g., giving way, progressive laxity, and early degenerative changes) occur due to the disappearance of mechanoreceptor feedback in addition to altered kinematics. This report was followed by studies on proprioception of knees with a ruptured ACL [2–5, 7]. Barrack et al. [2] demonstrated a correlation between the magnitude of joint instability and the reduction of proprioception in knees with a ruptured ACL, and Ochi et al. [15] performed an electrophysiological study of knees with a ruptured ACL using somatosensory evoked potential (SEP) and concluded that SEP was low in patients with reduced joint position sense. We examined subjects who were given rehabilitation in the acute period after ACL injury and had no marked difficulty in daily activities including walking. We noted a marked decrease in the joint position sense on the injured side, indicating the occurrence of changes in proprioception after the acute period.
It has been reported that knee instability due to ACL injury is compensated for by other structures during activities of daily living but becomes overt during athletic activities involving cutting [19]. Various functional tests have been performed to evaluate the function of knees with a ruptured ACL [1, 11, 14, 20]. Among them, the OLH and OLV are considered to be simple but useful functional tests [11, 14]. We also considered that visual perception of the environment affects the performance and carried out the tests while controlling vision. By this method, we observed a reduction in the performance on the injured side compared with that on the intact side, as reported previously.
Then how are changes in proprioception related to the performance in patients with a ruptured ACL? This study showed a correlation between the joint position sense and performance. The performance was reduced in patients with poor joint position sense, and this correlation was more pronounced when the subjects were deprived of visual information. These results suggest that the exercise ability decreases with proprioceptive function. There is the view of the “Rule of thirds” proposed by Noyes et al. [13] concerning the outcome of ACL injury. Noyes’ “first third” may be related to this proprioceptive function, i.e., a high level of activities including athletic activities may be maintained even in individuals with a ruptured ACL if this proprioception remains sufficiently intact. Also, as it has been reported that proprioception can be improved by taping and the use of braces [16], making resumption of athletic activities possible; evaluation of the relationship between proprioception and performance is thus considered to be important. Moreover, the joint position sense can be measured relatively easily and safely, and the results are considered to be useful for the evaluation of treatments after ACL injury, including surgical reconstruction. However, this study was of a cross-sectional study and was limited in that changes in the lower-limb function after proprioceptive rehabilitation were not evaluated. This theme must be approached in future studies.
The following conclusions were reached from the results of our study: The joint position sense and the performance were reduced compared with the normal knee; a correlation was observed between the joint position sense and performance, and this correlation was affected by visual control.
References
Barber SD, Noyes FR, Mangine RE, McCloskey JW, Hartman W (1990) Quantitative assessment of functional limitations in normal and anterior cruciate ligament-deficient knees. Clin Orthop 255:204–214
Barrack RL, Skinner HB, Buckley SL (1989) Proprioception in the anterior cruciate deficient knee. Am J Sports Med 17:1–6
Beard DJ, Kyberd PJ, Fergusson CM, Dodd CA (1993) Proprioception after rupture of the anterior cruciate ligament. An objective indication of the need for surgery? J Bone Joint Surg [Br] 75:311–315
Borsa PA, Lephart SM, Irrgang JJ, Safran MR, Fu FH (1997) The effects of joint position and direction of joint motion on proprioceptive sensibility in anterior cruciate ligament-deficient athletes. Am J Sports Med 25:336–340
Corrigan JP, Cashman WF, Brady MP (1992) Proprioception in the cruciate deficient knee. J Bone Joint Surg [Br] 74:247–250
Fitzgerald GK, Axe MJ, Snyder-Mackler L (2000) A decision-making scheme for returning patients to high-level activity with nonoperative treatment after anterior cruciate ligament rupture. Knee Surg Sports Traumatol Arthrosc 8:76–82
Friden T, Roberts D, Movin T, Wredmark T (1998) Function after anterior cruciate ligament injuries. Influence of visual control and proprioception. Acta Orthop Scand 69:590–594
Gobbi A, Tuy B, Mahajan S, Panuncialman I (2003) Quadrupled bone-semitendinosus anterior cruciate ligament reconstruction: a clinical investigation in a group of athletes. Arthroscopy 19:691–699
Good L, Roos H, Gottlieb DJ, Renstrom PA, Beynnon BD (1999) Joint position sense is not changed after acute disruption of the anterior cruciate ligament. Acta Orthop Scand 70:194–198
Hawkins RJ, Misamore GW, Merritt TR (1986) Followup of the acute nonoperated isolated anterior cruciate ligament tear. Am J Sports Med 14:205–210
Itoh H, Kurosaka M, Yoshiya S, Ichihashi N, Mizuno K (1998) Evaluation of functional deficits determined by four different hop tests in patients with anterior cruciate ligament deficiency. Knee Surg Sports Traumatol Arthrosc 6:241–245
Kennedy JC, Alexander IJ, Hayes KC (1982) Nerve supply of the human knee and its functional importance. Am J Sports Med 10:329–335
Noyes FR, Mooar PA, Matthews DS, Butler DL (1983) The symptomatic anterior cruciate-deficient knee. Part I. The long-term functional disability in athletically active individuals. J Bone Joint Surg [Am] 65:154–162
Noyes FR, Barber SD, Mangine RE (1991) Abnormal lower limb symmetry determined by function hop tests after anterior cruciate ligament rupture. Am J Sports Med 19:513–518
Ochi M, Iwasa J, Uchio Y, Adachi N, Sumen Y (1999) The regeneration of sensory neurones in the reconstruction of the anterior cruciate ligament. J Bone Joint Surg [Br] 81:902–906
Ramsey DK, Wretenberg PF, Lamontagne M, Nemeth G (2003) Electromyographic and biomechanic analysis of anterior cruciate ligament deficiency and functional knee bracing. Clin Biomech (Bristol, Avon) 18:28–34
Sherman MF, Warren RF, Marshall JL, Savatsky GJ (1988) A clinical and radiographical analysis of 127 anterior cruciate insufficient knees. Clin Orthop 227:229–237
Skinner HB, Barrack RL, Cook SD, Haddad RJ Jr (1984) Joint position sense in total knee arthroplasty. J Orthop Res 1:276–283
Tegner Y, Lysholm J, Gillquist J, Oberg B (1984) Two-year follow-up of conservative treatment of knee ligament injuries. Acta Orthop Scand 55:176–180
Tegner Y, Lysholm J, Lysholm M, Gillquist J (1986) A performance test to monitor rehabilitation and evaluate anterior cruciate ligament injuries. Am J Sports Med 14:156–159
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Katayama, M., Higuchi, H., Kimura, M. et al. Proprioception and performance after anterior cruciate ligament rupture. International Orthopaedics (SICOT) 28, 278–281 (2004). https://doi.org/10.1007/s00264-004-0583-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-004-0583-9