Abstract
Objective
Prophylactic fixation of the contralateral hip in slipped capital femoral epiphysis (SCFE) is controversial, and no reliable method has been established to predict subsequent contralateral slip. The main purpose of this study was to evaluate if magnetic resonance imaging (MRI) performed at primary diagnosis could predict future contralateral slip.
Materials and methods
Twenty-two patients with unilateral SCFE were included, all had MRI of both hips taken before operative fixation. Six different parameters were measured on the MRI: the MRI slip angle, the greatest focal widening of the physis, the global widening of the physis measured at three locations (the midpoint of the physis and 1 cm lateral and medial to the midpoint), periphyseal (epiphyseal and metaphyseal) bone marrow edema, the presence of pathological joint effusion, and the amount of joint effusion measured from the lateral edge of the greater trochanter. Mean follow-up was 33 months (range, 16–63 months). Six patients were treated for contralateral slip during the follow-up time and a comparison of the MRI parameters of the contralateral hip in these six patients and in the 16 patients that remained unilateral was done to see if subsequent contralateral slip was possible to predict at primary diagnosis.
Results
All MRI parameters were significantly altered in hips with established SCFE compared with the contralateral hips. However, none of the MRI parameters showed any significant difference between patients who had a subsequent contralateral slip and those that remained unilateral.
Conclusions
MRI taken at primary diagnosis could not predict future contralateral slip.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
In primary unilateral slipped capital femoral epiphysis (SCFE), the reported prevalence of subsequent contralateral slip diagnosed until skeletal maturity varies between 15 and 40% [1,2,3,4,5,6,7,8,9]. Most likely, this is due to racial variability [5], different radiographic criteria used to define slip, and different follow-up routines. Routine prophylactic contralateral fixation remains controversial since many patients will be treated unnecessarily with an undue risk of complications. Thus, the patients would benefit from a reliable method to predict future contralateral slip.
Magnetic resonance imaging (MRI) has traditionally not been used routinely for SCFE. However, focal or global widening of the physis, joint effusion, and bone marrow edema in the metaphysis and epiphysis adjacent to the physis have been found to be consistent findings on MRI in SCFE [10,11,12]. Futami et al. [11] performed MRI repeatedly during follow-up in ten patients with unilateral SCFE and physeal widening was clearly observed in four of ten asymptomatic contralateral hips that were fixated prophylactically. None of the other cases developed contralateral slip. Furthermore, Lalaji et al. [13] described two patients where MRI demonstrated physeal widening and bone marrow edema before the SCFE was radiographically detectable. Thus, there are some indications that MRI might be valuable in predicting subsequent contralateral slip.
The main purpose of this study was to evaluate if MRI at primary diagnosis could predict subsequent contralateral slip in unilateral SCFE.
Patients and methods
Twenty-seven patients with primary unilateral SCFE were treated in our hospital between January 2007 and November 2010. In five patients (all with unstable slip), MRI was not performed before treatment, mainly because preoperative MRI would have put an unfavorable delay to acute surgery and they were excluded from the current study. Thus, 22 patients (14 boys and eight girls) were included after parental informed consent. Approval by the Regional Ethical Committee and the Data Inspectorate were obtained before inclusion. The mean age at diagnosis was 13.3 years (range, 10.7–15.9 years) among the boys and 11.3 years (range, 8.3–13.2 years) among the girls (p = 0.009). The slip was clinically classified as stable (able to ambulate with or without crutches) or unstable (unable to ambulate with or without crutches) according to Loder’s classification [14]. The slip angle was measured on the preoperative frog-leg lateral radiographs according to the head-shaft angle described by Southwick [15]. If the head-shaft angle was below 30°, the slip was classified as mild, whereas angles between 30° and 49° were termed moderate, and angles ≥50° were classified as severe slips. MRI without intravenous contrast was performed in all patients within 8 days prior to surgery. The examinations, axial TSE T2 (TE 100/TR4020), axial STIR (70/3100/TI150), coronal TSE T1 (17/500) and coronal STIR (100/3925/150), were performed on a 1.5-Tesla MRI NT Intera system (Philips, Best, The Netherlands) using a Sense-body coil. Slice thickness was set at 4 mm (mm). Axial and coronal images were obtained in the supine position, feet first and with a sand bag placed on the legs to prevent motion. The legs were placed if possible with a slight internal rotation of both hips.
Due to a severe and unstable slip, one case was technically impossible to treat with percutaneous screw fixation and was therefore treated with the modified Dunn procedure as described by Ziebarth et al. [16]. The others were treated with percutaneous single screw fixation. In situ fixation was performed in all patients except two where spontaneous reduction occurred peroperatively. None were prophylactically fixated in the contralateral hip. All patients had clinical and radiographic follow-up every 6–12 months postoperatively until radiographic signs of physeal closure. Mean follow-up was 33 months (range, 16–63 months). Harris Hip Score (HHS) [17] was recorded at the latest follow-up. The screw was not routinely removed unless the patient had complaints due to protrusion of the distal end of the screw.
The interpretation of the pre-operative MRI images of both hips was done retrospectively after latest follow-up and independently by two experienced musculo-skeletal radiologists with the assessment of the following measurements:
-
1.
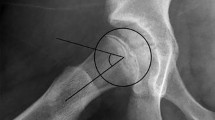
The MRI slip angle, measured as the angle between a line perpendicular to the mid-axis of the femoral neck and the epiphysis on axial view (axial T1w) (Fig. 1).
-
2.
The greatest focal widening (mm) of the physis (coronal T1w).
-
3.
The global widening (mm) of the physis measured at three locations; the midpoint of the physis and one centimeter lateral and medial to the midpoint (coronal T1w) (Fig. 2).
-
4.
Periphyseal bone marrow edema, measured as the maximum width (mm) of edema from the physis into the epiphysis and metaphysis respectively (coronal STIR) (Fig. 3).
-
5.
The presence of pathological joint effusion reported as yes or no (subjective evaluation).
-
6.
The level (mm) of joint effusion measured from the lateral edge of the greater trochanter.
A comparison of the contralateral hips that remained unaffected and those that subsequently had a contralateral slip (bilateral SCFE) was done according to these measurements with the purpose of evaluating if subsequent slip was possible to detect at primary diagnosis. The inter-observer study of the MRI interpretations was performed by the same two radiologists as observer 1 and 2, respectively.
Statistical analysis
SPSS software (version 21) was used for the statistics (IBM, Armonk, NY, USA). Categorical data were analyzed with the Chi-squared test and continuous data by the independent samples t test. We used logistic regression to analyze differences between contralateral hips that had no later slip and contralateral hips with subsequent slips. Correlations were calculated with Pearson’s correlation coefficient (r). Inter-observer agreements of the radiographic measurements (numerical data) were analyzed by the intra-class correlations coefficient (ICC) [18]. The interpretation of the ICC was as follows: 1 as perfect agreement, ≥ 0.75 as good agreement, < 0.75 as poor to moderate agreement. Inter-observer agreements for categorical data were analyzed by kappa statistics [19]. As suggested by Altman [20], we interpreted the kappa values as follows: < 0.20 as poor agreement, 0.21–0.40 as fair, 0.41–0.60 as moderate, 0.61–0.80 as good, and >0.80 as very good. All tests were two-sided. Differences were considered significant when the p value was <0.05. No power analysis was performed prior to inclusion of patients.
Results
Six patients (two boys and four girls) (27%) were treated for subsequent contralateral SCFE during the follow-up time. The mean age at the time of the index slip was 13.0 years in the patients where the SCFE remained unilateral, while the patients treated for bilateral SCFE were significantly younger (11.2 years, p = 0.032). The two boys were 13.0 and 13.1 years old while the mean age of the four girls was 10.3 years (8.3–13.2 years). The mean time interval until the diagnosis of the contralateral slip was 7.8 months (median 7 months; range 2–18 months) (Fig 4). The mean primary slip angle in the 22 unilateral SCFE was 33° (8–81°) with 19 stable and three unstable SCFE. The contralateral slips were all stable and mild slips (mean slip angle 14°, range, 6–25°). There were no major complications like avascular necrosis or chondrolysis. Ten patients have had the screw removed because of pain from the distal end of the screw. No complications occurred. At follow-up, one patient with a severe slip (81°) had significant complaints (HHS: 67 points) probably caused by femoroacetabular impingement with a marked radiographic CAM-deformity (anteroposterior and lateral alpha angle: 107° and 114°, respectively). A Southwick osteotomy combined with osteoplasty of the femoral head–neck junction was planned for, but the patient never returned for surgery. The other patients had good clinical outcomes with no physical limitation, limp or pain (HHS: 100 points). No hips showed any signs of osteoarthritis.
MRI parameters
All MRI parameters showed significant higher values in the primary affected hips with SCFE compared with the contralateral hips. The mean MRI slip angle was 55° in the primary affected hips and 24° in the contralateral hips (p < 0.001). The mean MRI slip angle in the contralateral hip in the six patients treated for subsequent contralateral slip and in the 16 patients with persistent unilateral SCFE was 21° and 24°, respectively (p = 0.43) (Table 1).
The mean greatest focal widening of the physis was 7.4 mm in the primary affected hips and 3.1 mm in the contralateral hips (p < 0.001). In the six patients treated for subsequent contralateral slip, the mean maximum width was 3.7 mm, while it was 2.9 mm in the contralateral hip in the 16 patients with persistent unilateral SCFE (p = 0.09) (Table 1).
The mean global widening of the physis at the three locations varied from 5.8 to 6.4 mm in the primary affected hips, while it was 2.7 to 2.8 mm in the contralateral hips. The difference was significant for all three locations (p > 0.001). No significant differences were found between hips with later contralateral SCFE and hips with persistent unilateral slips (Table 1).
The mean maximum width of edema into the epiphysis and into the metaphysis in the primary affected hips was 9.9 and 9.7 mm, respectively. No signs of epiphyseal or metaphyseal edema were recognized in the contralateral hips (Table 1).
Nineteen of 22 (86%) primary affected hips had pathological joint effusion. Only one patient who had a later slip had pathological joint effusion in the contralateral hip at primary diagnosis (p < 0.001). The mean amount of joint effusion in the primary affected hips and in the contralateral hips was 3.5 and 0.9 mm, respectively (p < 0.001). There was no significant difference between hips with subsequent contralateral slip and hips with persistent unilateral slip (p = 0.93) (Table 1).
Comparison between slip angle measured on MRI and radiographs
In the primary affected hips, the mean preoperative slip angle measured on MRI and on radiographs was 55° and 33°, respectively (p < 0.001) and the mean difference was 22° (−18–43°) (Fig. 5). In the contralateral hips, the mean slip angle at primary diagnosis measured on MRI was 24° and 8° on radiographs (p < 0.001) and the mean difference was 15° (0–35°). Significant correlation was found between the slip angle measured on MRI and radiographs (r = 0.81, p < 0.001).
MRI and plain radiographs in the same patient with SCFE in the left hip. MRI slip angle (MRI - SA): 38°. Southwick’s slip angle (SA): 14°. The left image has been cropped from the upper image in Fig. 1 (same patient)
Interobserver agreement
The ICC showed good agreement for MRI slip angle (0.94) and epiphyseal/metaphyseal bone marrow edema (0.93 and 0.77), while it showed moderate agreement for the remaining measurements (greatest physeal widening: 0.63, global physeal widening - midpoint: 0.73, − lateral: 0.53, − medial: 0.70 and level of joint effusion: 0.68). The agreement regarding the presence of pathologic joint effusion reported as yes or no (subjective evaluation) was good (kappa: 0.73).
Discussion
The aim of this study was to evaluate if MRI performed at primary diagnosis could predict contralateral slip in SCFE. The MRI measurements used in this study are based on previous studies [10,11,12,13]. In all six MRI parameters, there were significant differences between the primarily affected hips and the contralateral hips at diagnosis. This indicates that all parameters are relevant in the diagnosis of SCFE. The inter-observer agreement was moderate to good for all MRI parameters which we assess as acceptable considering these measurements are not being used routinely in clinical practice.
This study has some limitations. Most importantly, the number of patients is small, with only six patients with subsequent contralateral slip. No sample size calculation was performed prior to inclusion of patients, which may have caused the study to be underpowered. Although we included all available patients during a 4–year period, SCFE is a relatively rare condition and this is the main reason for the limited number of patients. Second, the patients are not precisely consecutive cases since five patients, all with unstable hips, were excluded since MRI was not practically feasible before surgery, which means that the study population does not reflect the true rate of unstable slip in SCFE.
The slip angle measured on MRI is the angle between a line perpendicular to the mid-axis of the femoral neck and the epiphysis while the slip angle measured on frog-leg radiographs [15] is the angle between a line perpendicular to the mid-axis of the femoral shaft and the epiphysis. Thus, these measurements are not exactly the same. We found the mean slip angle to be correlated (r = 0.81, p < 0.001) and significantly higher (p < 0.001) on MRI compared to radiographs. The slip angle on MRI is measured on an axial view, which visualizes the slip directly, not affected by differences in the rotation of the extremity. Therefore, we believe that MRI is a more reliable method to measure the true slip angle in SCFE and our results indicate that frog-leg lateral radiographs usually underestimate the real slip angle in SCFE.
The risk of contralateral slip in SCFE has shown to be increased in children with endocrinopathies [21], in those who are particularly young [5, 22, 23], in patients with a posterior sloping angle above 12° [24], and in patients with a modified Oxford bone score of 16, 17, or 18 [9]. Even if these predictors can be used as guidance in the decision of prophylactic fixation, they are not uniformly precise in predicting contralateral slip. A reliable method to predict subsequent contralateral slip would be of great benefit to the patients, but is still not established. The role of MRI in diagnosing a slip before it becomes symptomatic and/or detectable on plain radiographs has been evaluated in two studies with a limited number of patients [11, 13]. Futami et al. [11] performed a prospective MRI study on the growth plate in SCFE and the contralateral hip during the possible preslip stage. Ten patients with unilateral SCFE were examined with MRI repeatedly (6-month intervals) during follow-up. In four patients, the asymptomatic contralateral hip was fixated because MRI demonstrated physeal widening without slip. None of the other patients developed contralateral slip and the authors proposed repetitive MRI examinations at 6-month intervals for hips at risk of slipping. Lalaji et al. [13] presented two cases where MRI demonstrated distortion of the physis and/or periphyseal bone marrow edema before the development of radiographically detectable SCFE. In the present study, none of the MRI measurements showed any significant difference between patients that had a subsequent contralateral slip and those that remained unilateral. Furthermore, none of the contralateral hips were found to have bone marrow edema.
The patients with bilateral SCFE were significantly younger than those with unilateral SCFE (11.2 vs. 13.0 years), which is in accordance with previous studies [5, 22]. Loder [5] found that the age at presentation was younger in children with bilateral involvement compared to those with persistent unilateral disease (12.0 vs. 12.9 years) and in a study by Riad et al. [22] the mean age of patients with persistent unilateral SCFE was 11.9 years for girls and 14.2 years for boys while the mean age for patients with later contralateral slip was 11.0 years for girls and 12.1 years for boys.
In conclusion, MRI taken at primary diagnosis could not predict future contralateral slip. However, the MRI measurements were all significantly altered in hips with SCFE compared to the contralateral hip and would thus be useful in confirming the diagnosis of SCFE in patients with a symptomatic hip without any signs of slip on plain radiographs. We therefore recommend MRI in such cases and in situ fixation in case of positive findings as physeal widening, periphyseal bone marrow edema and pathological joint effusion.
References
Wilson PD, Jacobs B, Schecter L. Slipped capital femoral epiphysis: an end result study. J Bone Joint Surg Am. 1965;47:1128–45.
Hägglund G, Hansson LI, Ordeberg G, Sandström S. Bilaterality in slipped upper femoral epiphysis. J Bone Joint Surg Br. 1988;70:179–81.
Carney BT, Weinstein SL, Noble J. Long-term follow-up of slipped capital femoral epiphysis. J Bone Joint Surg Am. 1991;73:667–74.
Stasikelis PJ, Sullivan CM, Phillips WA, Polars JA. Slipped capital femoral epiphysis. Prediction of contralateral involvement. J Bone Joint Surg Am. 1996;78:1149–55.
Loder RT. The demographics of slipped capital femoral epiphysis. An international multicenter study. Clin Orthop Relat Res. 1996;322:8–27.
Yildirim Y, Bautista S, Davidson RS. Chondrolysis, osteonecrosis, and slip severity in patients with subsequent contralateral slipped capital femoral epiphysis. J Bone Joint Surg Am. 2008;90:485–92.
Wensaas A, Svenningsen S, Terjesen T. Long-term outcome of slipped capital femoral epiphysis: a 38-year follow-up of 66 patients. J Child Orthop. 2011;5:75–82.
Lehmann TG, Engesæter IØ, Laborie LB, Rosendahl K, Lie SA, Engesæter LB. In situ fixation of slipped capital femoral epiphysis with Steinmann pins: 67 patients followed for 2-16 years. Acta Orthop. 2011;82:333–8.
Popejoy D, Emara K, Birch J. Prediction of contralateral slipped capital femoral epiphysis using the modified Oxford bone age score. J Pediatr Orthop. 2012;32:290–4.
Umans H, Liebling MS, Haramati N, Macy NJ, Pritzker HA. Slipped capital femoral epiphysis: a physeal lesion diagnosed by MRI, with radiographic and CT correlation. Skelet Radiol. 1998;27:139–44.
Futami T, Suzuki S, Seto Y, Kashiwagi N. Sequential magnetic resonance imaging in slipped capital femoral epiphysis: assessment of preslip in the contralateral hip. J Pediatr Orthop B. 2001;10:298–303.
Tins B, Cassar-Pullicino V, McCall I. The role of pre-treatment MRI in established cases of slipped capital femoral epiphysis. Eur J Radiol. 2009;70:570–8.
Lalaji A, Umans H, Schneider R, Mintz D, Liebling MS, Haramati N. MRI features of confirmed “pre-slip” capital femoral epiphysis: a report of two cases. Skelet Radiol. 2002;31:362–5.
Loder RT, Richards BS, Shapiro PS, Reznick LR, Aronson DD. Acute slipped capital femoral epiphysis: the importance of physeal stability. J Bone Joint Surg Am. 1993;75:1134–40.
Southwick WO. Osteotomy through the lesser trochanter for slipped capital femoral epiphysis. J Bone Joint Surg Am. 1967;49:807–35.
Ziebarth K, Zilkens C, Spencer S, Leunig M, Ganz R, Kim YJ. Capital realignment for moderate and severe SCFE using a modified Dunn procedure. Clin Orthop Relat Res. 2009;467:704–16.
Harris WH. Traumatic arthritis of the hip after dislocation and acetabular fractures: treatment by mold arthroplasty: an end-result study using a new method of result evaluation. J Bone Joint Surg Am. 1969;51:737–55.
McGraw KO, Wong SP. Forming inferences about some intraclass coefficients. Psychol Meth. 1996;1:30–46.
Cohen J. Weighted kappa: nominal scale agreement with provision for scaled disagreement or partial credit. Psychol Bull. 1968;70:213–20.
Altman DG. Practical statistics for medical research. London: Chapman & Hall. 1991;403–9.
Loder RT, Wittenberg B, DeSilva G. Slipped capital femoral epiphysis associated with endocrine disorders. J Pediatr Orthop B. 1995;19:349–56.
Riad J, Bajelidze G, Gabos PG. Bilateral slipped capital femoral epiphysis. Predictive factors for contralateral slips. J Pediatr Orthop. 2007;27:411–4.
Azzopardi T, Sharma S, Bennet GC. Slipped capital femoral epiphysis in children aged less than 10 years. J Pediatr Orthop B. 2010;19:13–8.
Barrios C, Blasco MA, Blasco MC, Gascó J. Posterior sloping angle of the capital femoral physis. A predictor of bilaterality in slipped capital femoral epiphysis. J Pediatr Orthop. 2005;25:445–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest
Appendix
Appendix
Rights and permissions
About this article
Cite this article
Wensaas, A., Wiig, O., Hellund, J.C. et al. Magnetic resonance imaging at primary diagnosis cannot predict subsequent contralateral slip in slipped capital femoral epiphysis. Skeletal Radiol 46, 1687–1694 (2017). https://doi.org/10.1007/s00256-017-2735-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-017-2735-1