Abstract
Urocalun®, a herbal medicine prepared from an extract of Quercus salicina Blume/Quercus stenophylla Makino (QS extract), has been clinically used for the treatment of urolithiasis in Japan since 1969. In the present study, the effects of QS extract on oxalate-induced cell injury and NADPH-induced superoxide anion (O2 −) production in the injured cells were investigated. Oxalate-induced cell injury was assessed by mitochondrial reduction of 3-(4,5-dimethyl-2-thiazol)-2,5-diphenyltetrazolium bromide and leakage of lactate dehydrogenase into the extracellular fluid. When NRK-52E cells were injured by exposure to oxalate for 24 h, QS extract prevented the injury in a dose-dependent manner. In addition, QS extract suppressed the increase in NADPH-induced O2 − production, or NADPH oxidase activity, in the homogenate of cells injured by oxalate exposure. These findings suggest that the reduction in oxalate-induced O2 − production contributes to the cytoprotective effect of QS extract.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Urolithiasis is a multifactorial disorder caused by metabolic abnormalities that influence the composition of body fluids and urine. Since about 80% of stones are composed of calcium oxalate and calcium phosphate, an increase in urinary oxalate levels as well as phosphate levels plays an important role in the formation and recurrence of stones [1].
Since the rate of stone recurrence is quite high, about 50% at 10 years and 75% at 15 years when no treatment at all is given [2], dietary advice to reduce the risk seems to be important. No pharmacological treatment is available for the prevention of stone formation.
In Japan, Urocalun®, a herbal medicine extracted from the twig leaves of Quercus salicina Blume/Quercus stenophylla Makino (QS), a tall evergreen tree belonging to the family Fagaceae, has been clinically used for a long time in the treatment of urolithiasis as a medicine which facilitates the spontaneous expulsion of ureteral stones. In a rat ureteral stone model, QS extract promoted stone discharge [3] and had a diuretic effect [4]. In addition, QS extract has been reported to dissolve calcium phosphate crystals and to prevent crystal growth at a silk thread nucleus in the rat bladder [5].
There is experimental evidence for the accumulation of radicals in the kidneys of experimental urolithiasis rats fed a diet containing ethylene glycol [6]. Oxalate is considered to induce membrane injury mediated by lipid peroxidation through oxygen free radicals in LLC-PK1 (porcine renal proximal tubular) cells and MDCK (Madin-Darby canine kidney) cells [7] and to facilitate the deposition of calcium oxalate crystals after its incorporation into kidney stones [8–10].
It has recently been demonstrated that the free-radical scavenger vitamin E [11] and the antioxidant enzyme catalase [12] protect against the production of oxalate-induced reactive oxygen species (ROS) and peroxidative injury in renal tubular epithelial cells. In addition, we have shown that QS extract suppresses superoxide anion (O2 −) levels in a cell-free xanthine/xanthine oxidase system [3], although the mechanism of action is not clear. In the present study, we investigated the effect of QS extract on oxalate-induced cell injury, and the involvement of oxalate-enhanced NADPH-induced O2 − production in NRK-52E (rat renal tubular epithelial) cells.
Materials and methods
Preparation of QS extract
QS extract was produced in Nippon Shinyaku (Kyoto, Japan). The powder of QS extract was obtained from drying the aqueous extract which made by soaking the dried leaves and branches of Quercus salicina Blume/Q. stenophylla Makino in distilled water. A stock solution of 10 mg/mL QS extract was prepared in dimethylsulfoxide (Wako, Kyoto, Japan) and diluted to 30–300 μg/mL in Dulbecco’s modified Eagle’s medium (DMEM high glucose; Sigma, St Louis, MO). Although some plant parts contain oxalate, the amount of oxalate in the QS extract at 30 μg/mL, determined by UV method (Oxalic acid enzymatic bioanalysis, R-Biopharm, Darmstadt, DE) was below the lower limit of quantification (<0.01 mM).
Cell culture
Rat renal tubular epithelial (NRK-52E) cells were obtained from American Type Culture Collection (Manassas, VA). The cells were cultured in Dulbecco’s modified Eagle’s medium DMEM supplemented with 5% (v/v) fetal bovine serum (Gibco Laboratories, Grand Island, NY) at 37°C in 5% CO2.
NRK-52E cells were incubated in DMEM containing 0.1–1 mM sodium oxalate (Sigma) in the presence or absence of QS extract (3–30 μg/mL; Nippon Shinyaku, Kyoto) for 22–24 h.
Cell injury
Cell injury was assessed by measuring lactate dehydrogenase (LDH) leakage into the medium and by assaying mitochondrial reduction of 3-(4,5-dimethyl-2-thiazol)-2,5-diphenyltetrazolium bromide (MTT). For measurement of LDH leakage, 50 μL of the incubation medium was taken 24 h after exposure to oxalate, and LDH in the medium was determined with an enzymatic assay kit (Wako Pure Chemicals, Osaka). LDH leakage was expressed as a percentage of that observed in control cells incubated for 24 h in fetal-bovine-serum-free DMEM in the absence of oxalate and QS extract. For MTT assay, 22 h after exposure to oxalate, NRK-52E cells were incubated in 10 μg/mL MTT solution for 2 h at 37°C and the blue-colored MTT formazan product was extracted into isopropanol/0.1 N HCl (90:10, v/v %) containing 0.4% Triton X-100. The optical density was measured at 595 nm. The MTT-reducing activity in injured cells was expressed as a percentage of that in control cells measured after 22 h of incubation in medium without sodium oxalate or QS extract.
At the end of the experiments, NRK-52E cells were solubilized in 1 mL of 1 N NaOH and the protein content was determined by the method of Bradford with bovine serum albumin as the standard [13].
NADPH-induced O2 − production and superoxide dismutase activity
The effects of QS extract on NADPH-induced O2 − production and superoxide dismutase (SOD) activity were investigated by analyzing the NRK-52E cell homogenate after exposure of the cells to oxalate. In brief, after 24 h of exposure to oxalate in the presence or absence of QS extract, cells in a 6-well plastic dish were washed three times with phosphate-buffered saline. The cells were homogenized in 1 mL of ice-cold Hank’s balanced saline solution (HBSS), pH 7.4, with a Physcotron homogenizer (NS-310E; Nichion, Chiba). After preincubation of the homogenate for 30 min at 37°C, the reaction was carried out in a mixture containing 0.2 mM lucigenin and 1 mM NADPH in HBSS. The reaction was initiated by adding 0.2 mM lucigenin and 1 mM NADPH in HBSS to the sample, and NADPH-enhanced O2 − -dependent lucigenin chemiluminescence was measured with a spectrofluorophotometer (Wallac 1420 ARVO-SX multilabel counter, Perkin Elmer, Tokyo) for 10 min. The chemiluminescence reading was acquired at intervals of 20 s. SOD activity was measured with SOD Assay Kit-WST (Dojindo, Tokyo) in the same homogenate used for the determination of O2 −. At the end of the experiments, the cells were solubilized in 1 N NaOH (1 mL) and the protein content was determined as described above. The chemiluminescence values were expressed per mg of protein.
Statistical analysis
Data were analyzed with the SAS program (SAS/STAT, Ver. 8.2, SAS Institute, Cary, NC). All data were analyzed for statistical significance by either Student’s t test for comparison between two groups or one-way analysis of variance, followed by Dunnett’s multiple comparison test (two-tailed) against the control. A P value of less than 0.05 was considered significant.
Results
Oxalate-induced cell injury
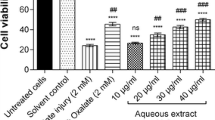
Oxalate decreased cell viability and increased LDH leakage in NRK-52E cells in a concentration-dependent manner (Fig. 1a). These changes were statistically significant at 0.3 mM oxalate or more.
Effect of QS extract on oxalate-induced cell injury in NRK-52E cells. Cells were exposed to a 0.1, 0.3 or 1 mM oxalate, b 0.3 mM oxalate in the presence or absence of 3, 10 or 30 μg/mL QS extract for 24 h. Cell injury was determined by MTT reduction and LDH leakage. Values are expressed as a percentage of the value measured in the absence of oxalate and QS extract (untreated group). Columns and bars represent the mean and SEM (N = 6). # P < 0.05, ## P < 0.01, compared with the respective untreated groups (Dunnett’s test). *P < 0.05, **P < 0.01, compared with the respective control groups (Dunnett’s test)
Reduction of oxalate-induced cell injury by QS extract
When NRK-52E cells were treated with QS extract (3, 10 and 30 μg/mL) and oxalate (0.3 mM) for 24 h, a reduction in oxalate-induced cell injury was observed (Fig. 1b), although QS extract alone had no effect on the measures of cell injury in the absence of oxalate (Fig. 2). After treated with oxalate (1 mM) and QS extract (30 μg/mL), oxalate-induced cell injury were reduced by QS extract (MTT: Control 35.3 ± 0.8%, QS extract 53.8 ± 2.2%, P < 0.01, LDH: Control 287.8 ± 8.1%, QS extract 230.4 ± 2.1%, P < 0.01).
Effect of QS extract on the cell injury markers without oxalate in NRK-52E cells. Cells were exposed to QS extract (30 μg/mL) for 24 h. Cell injury was determined by MTT assay and LDH leakage. Values were expressed as a percentage of the value measured in the absence of QS extract (control group). Columns and bars represent the mean and SEM (N = 6)
O2 − production induced by NADPH and SOD activity in the NRK-52E cell homogenate after oxalate exposure.
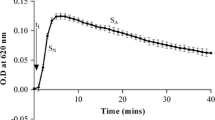
Oxalate increased NADPH-induced O2 − production in the NRK-52E cell homogenate in a concentration-dependent manner, and a significant increase was observed at 0.3 mM oxalate (Fig. 3a). SOD activity was significantly increased by exposure of the cells to 0.3 mM oxalate (Fig. 4).
Effect of QS extract on oxalate-enhanced NADPH-induced O2 − production in the NRK-52E cell homogenate. Cells were exposed to a 0.1 or 0.3 mM oxalate, b 0.3 mM oxalate in the presence or absence of QS extract (30 μg/mL), c QS extract (30 μg/mL) in the absence of oxalate for 24 h and homogenized in 1 mL of Hank’s balanced salt solution (HBSS). O2 − production induced by NADPH (1 mM) in the NRK-52E cell homogenate was measured by lucigenin-enhanced chemiluminescence with 200 μM lucigenin. Columns and bars represent the mean and SEM of the maximum value (N = 4). ## P < 0.01, compared with the control group (Dunnett’s test). *P < 0.05, compared with the oxalate alone group (Student’s t test)
Effect of oxalate on SOD activity in the NRK-52E cell homogenate. Cells were exposed to 0.1 or 0.3 mM oxalate for 24 h and homogenized in 1 mL of HBSS. Values were expressed as a percentage of the value measured in the absence of oxalate (control group). Columns and bars represent the mean and SEM (N = 4). **P < 0.01, compared with the control group (Dunnett’s test)
Reduction of NADPH-induced O2 − production by QS extract
After exposure of NRK-52E cells to oxalate (0.3 mM) and QS extract (30 μg/mL) for 24 h, O2 − production induced by NADPH in the NRK-52E cell homogenate was significantly suppressed by QS extract (Fig. 3b). QS extract alone had no significant effect on the O2 − production induced by NADPH in the NRK-52E cell homogenate in the absence of oxalate (Fig. 3c). After exposure to oxalate (1 mM) and QS extract (30 μg/mL), O2 − production induced by NADPH were slightly suppressed by QS extract [Control 303.4 ± 29.9, Oxalate 630.8 ± 46.8, Oxalate + QS extract 554.7 ± 37.9 (counts103/s/protein) (N = 4)].
Discussion
Hyperoxaluria is a major risk factor for calcium oxalate nephrolithiasis, and calcium oxalate urinary stones are the most common type of urinary stone. High levels of oxalate cause a variety of changes in the renal epithelial cells, such as an increase in free radical production and a decrease in antioxidant status [6, 7, 14, 15], followed by cell injury [7, 8, 15–17] and cell death [18, 19]. These changes are significant predisposing factors for the facilitation of crystal adherence and retention [7, 9–12, 16].
We have reported an increase in apoptosis and an up-regulation of the expression of apoptosis-related genes in renal tubular epithelial cells in the ethylene glycol rat model of urolithiasis [20]. In renal tubular epithelial cells, oxalate-induced cell injury and apoptotic changes are associated with an increased generation of free radicals, including O2 −, hydroxyl radical (OH·), hydrogen peroxide (H2O2), peroxide radical (RO·) and singlet molecular oxygen [21]. A positive correlation between urinary oxalate levels and renal tubular epithelial cell injury as well as between oxalate levels and lipid peroxides has been discovered in experimental urolithiasis rats [7] and patients with kidney stones [22]. Moreover, vitamin E, a radical scavenger, suppresses hyperoxaluria-induced calcium crystal deposition in urolithiasis rats by improving renal tissue antioxidant status [23].
In the present study, oxalate at 0.3 mM decreased MTT-reducing activity in NRK-52E cells and increased LDH activity in the culture medium. Similarly, other groups have reported that oxalate at 0.5 mM decreases cell viability as determined by LDH release and trypan blue exclusion in LLC-PK1 and MDCK cells [15, 24]. According to Coe et al. [25], normal humans excrete a reasonable upper limit of 45 mg (0.5 mM) oxalate per day, and a simple dietary excess of oxalate from food commonly increase urinary oxalate to 50–60 mg (0.556–0.667 mM) daily. In our earlier experiments, exposures NRK-52E cells to oxalate at 0.3 mM for 3, 6 and 24 h induced significant LDH leakage (only for the 24 h) and MTT reduction (for 6 and 24 h). Therefore we selected oxalate at 0.3 mM for 24 h to induce a hyperoxaluric environment in renal epithelial cells.
Oxalate increased NADPH oxidase activity in NRK-52E cells. Although the source of ROS induced by oxalate exposure is unclear, oxalate increases NADPH oxidase mRNA levels in NRK-52E cells and diphenyleneiodonium chloride, a selective NADPH oxidase inhibitor, reduces ROS production and cell injury induced by oxalate exposure in NRK-52E and LLC-PK1 cells [11, 26, 27]. These findings suggest the involvement of ROS derived from the increased NADPH oxidase levels which result in oxalate-induced cell injury in the kidney.
Oxidative stress is determined by the balance between radical production and endogenous antioxidant defense. Antioxidant enzymes, such as SOD, glutathione peroxidase and catalase, and endogenous antioxidants, such as glutathione, ascorbic acid, NADPH and α-tocopherol, participate in neutralizing free radicals. SOD and catalase reduce the oxalate-induced generation of ROS in LLC-PK1 and MDCK cells [12]. Several reports indicate that oxalate decreases antioxidant enzymes in renal tubular epithelial cells [11, 15] and urolithiasis animal models [7, 23]. However, in this study, SOD activity was increased by oxalate exposure in NRK-52E cells. It has also been reported that the SOD activity in the kidney in urolithiasis rats prepared by supplementing their diet with ethylene glycol increases during the initial period of the feeding (1–9 days) and decreases from 42 days after the feeding [6]. Therefore, it is likely that these increases in SOD activity are a physiological counteraction to the oxidative stress.
Recently several plant medicines including Heruniaria hirusta [28] and Phyllanthus niruri [29], used folk medicine to treat kidney stones. It had been demonstrated that Heruniaria hirusta had inhibitory effects on calcium crystals internalization by MDCK cells and Phyllanthus niruri had inhibited the attachment of calcium crystals to the tubular cell by coating crystal surface with itself. These effects were contributed to their direct actions on calcium crystal, which might be one of important mechanisms to prevent the adhesion and retention of crystals in the kidney. In regard to QS extract, we have reported that this extract suppresses O2 − levels in a cell-free xanthine/xanthine oxidase system [3]. We therefore hypothesized that QS extract would prevent oxalate-induced cell injury by its radical-scavenging effect. In the present study, QS extract suppressed oxalate-induced cell injury and NADPH oxidase activity in NRK-52E cells. Antioxidants such as SOD, catalase and vitamin E suppress the release of LDH and the formation of malondialdehyde in LLC-PK1 cells [11, 12, 15], indicating that the protective action of QS extract against oxalate-induced cell injury may be attributed to its radical-scavenging effects. Because aqueous solution of 1,000 μg/mL QS extract, at 30 times higher concentration in the present study, contains 0.0069 mM calcium and 0.16 mM magnesium, it is unlikely that QS extract showed cytoprotective effect due to calcium and magnesium interference. Although the mechanisms of inhibition of oxalate-induced NADPH oxidase activity by radical-scavengers are unclear, vitamin E prevents oxalate-induced cellular lipid peroxidation and attenuates oxalate-induced free radical production brought about by the activation of NADPH oxidase in LLC-PK1 cells [11]. Moreover vitamin E suppresses hyperoxaluria-induced calcium crystal deposition in urolithiasis rats [23] and human [30].These results suggest that QS extract suppresses oxalate-induced NADPH oxidase activity, thereby decreasing O2 − production, which might be followed by suppression of stone formation. However, further studies are needed for its potential in the prevention of stone formation and recurrence in in vivo urolithiasis model.
In conclusion, QS extract suppressed cell injury induced by oxalate exposure, most likely by scavenging free radicals and suppressing the activation of NADPH oxidase.
References
Finlayson B (1974) Symposium on renal lithiasis. Renal lithiasis in review. Urol Clin North Am 1:181–212
Wahl C, Hess A (2000) Kidney calculi–is nutrition a trigger or treatment? Ther Umsch 57:138–145
Natsukawa T, Hirata K, Noda K, Oka M, Tanaka M, Hamada K, Kuwabara T (2005) Promoting effect of extract of Quercus salicina Blume/Q. stenophylla Makino (UROCALUN®) on urinary stone passage. Jpn Pharmacol Ther 33:361–368
Ishigami J, Ooshima H, Saitou H (1967) Clinical effect of UROCALUN on urolithiasis in the upper urinary tract. Hifu to Hinyo 29:858–862
Ookita K, Yamada S, Johsen T, Tanaka M (1968) Uses of UC-2 for treatment of upper urinary calculi and studies on dissolution of urinary calculi by UC-2. Hifu to Hinyo 30:426–431
Huang HS, Ma MC, Chen J, Chen CF (2002) Changes in the oxidant–antioxidant balance in the kidney of rats with nephrolithiasis induced by ethylene glycol. J Urol 167:2584–2593
Selvam R (2002) Calcium oxalate stone disease: role of lipid peroxidation and antioxidants. Urol Res 30:35–47
Thamilselvan S (1998) Oxalate and calcium oxalate crystals are injurious to renal epithelial cells: results of in vivo and in vitro studies. J Nephrol 11(Suppl 1):66–69
Wiessner JH, Hasegawa AT, Hung LY, Mandel GS, Mandel NS (2001) Mechanisms of calcium oxalate crystal attachment to injured renal collecting duct cells. Kidney Int 59:637–644
Khan SR (1995) Calcium oxalate crystal interaction with renal tubular epithelium, mechanism of crystal adhesion and its impact on stone development. Urol Res 23:71–79
Rashed T, Menon M, Thamilselvan S (2004) Molecular mechanism of oxalate-induced free radical production and glutathione redox imbalance in renal epithelial cells: effect of antioxidants. Am J Nephrol 24:557–568
Thamilselvan S, Byer KJ, Hackett RL, Khan SR (2000) Free radical scavengers, catalase and superoxide dismutase provide protection from oxalate-associated injury to LLC-PK1 and MDCK cells. J Urol 164:224–229
Bradford MM (1976) A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem 72:248–254
Scheid C, Koul H, Hill WA, Luber-Narod J, Kennington L, Honeyman T, Jonassen J, Menon M (1996) Oxalate toxicity in LLC-PK1 cells: role of free radicals. Kidney Int 49:413–419
Thamilselvan S, Khan SR, Menon M (2003) Oxalate and calcium oxalate mediated free radical toxicity in renal epithelial cells: effect of antioxidants. Urol Res 31:3–9
Hackett RL, Shevock PN, Khan SR (1990) Cell injury associated calcium oxalate crystalluuria. J Urol 144:1535–1538
Ebisuno S, Kohjimoto Y, Tamura M, Ohkawa T (1995) Adhesion of calcium oxalate crystal to Madin-Darby canine kidney cells and some effects of glycosaminoglycans or cell injuries. Eur Urol 28:68–73
Schepers MS, van Ballegooijen ES, Bangma CH, Verkoelen CF (2005) Crystals cause acute necrotic cell death in renal proximal tubule cells, but not in collecting tubule cells. Kidney Int 68:1543–1553
Schepers MS, van Ballegooijen ES, Bangma CH, Verkoelen CF (2005) Oxalate is toxic to renal tubular cells only at supraphysiologic concentrations. Kidney Int 68:1660–1669
Miyazawa K, Suzuki K, Ikeda R, Moriyama MT, Ueda Y, Katsuda S (2005) Apoptosis and its related genes in renal epithelial cells of the stone-forming rat. Urol Res 33:31–38
Sarica K, Yagci F, Bakir K, Erbagci A, Erturhan S, Ucak R (2001) Renal tubular injury induced by hyperoxaluria: evaluation of apoptotic changes. Urol Res 29:34–37
Huang HS, Ma MC, Chen CF, Chen J (2003) Lipid peroxidation and its correlations with urinary levels of oxalate, citric acid, and osteopontin in patients with renal calcium oxalate stones. Urology 62:1123–1128
Thamilselvan S, Menon M (2005) Vitamin E therapy prevents hyperoxaluria-induced calcium oxalate crystal deposition in the kidney by improving renal tissue antioxidant. BJU Int 96:117–126
Byer K, Khan SR (2005) Citrate provides protection against oxalate and calcium oxalate crystal induced oxidative damage to renal epithelium. J Urol 173:640–646
Coe FL, Parks JH, Asplin JR (1992) The pathogenesis and treatment of kidney stones. N Engl J Med 327:1141–1152
Moriyama MT, Domiki C, Miyazawa K, Tanaka T, Suzuki K (2005) Effect of oxalate exposure on Madin-Darby canine kidney (MDCK) cells in culture. Urol Res 33:470–475
Umekawa T, Byer K, Uemura H, Khan SR (2005) Diphenyleneiodium (DPI) reduces oxalate ion- and calcium oxalate monohydrate and brushite crystal-induced upregulation of MCP-1 in NRK52E cells. Nephrol Dial Transplant 20:870–878
Atmani F, Farell G, Lieske JC (2004) Extract from Herniaria hirsuta coats calcium oxalate monohydrate crystals and blocks their adhesion to renal epithelial cells. J Urol 172:1510–1514
Campos AH, Schor N (1999) Phyllanthus niruri inhibits calcium oxalate endocytosis by renal tubular cells: its role in urolithiasi. Nephron 81:393–397
Srinivasan S, Pragasam V, Jenita X, Kalaiselvi P, Muthu V, Varalakshmi P (2004) Oxidative stress in urogenital tuberculosis patients: a predisposing factor for renal stone formation–amelioration by vitamin E supplementation. Clin Chim Acta 350:57–63
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Moriyama, M.T., Miyazawa, K., Noda, K. et al. Reduction in oxalate-induced renal tubular epithelial cell injury by an extract from Quercus salicina Blume/Quercus stenophylla Makino. Urol Res 35, 295–300 (2007). https://doi.org/10.1007/s00240-007-0114-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00240-007-0114-4