Abstract
Rabbit flexor tendons can be harvested, acellularized, and used as scaffolds for reseeding of flexor tendon constructs. The purpose of this study was to compare the biomechanical characteristics of seeded and unseeded flexor tendon constructs to autologous grafts in vivo in the rabbit model. The experimental groups were created using acellularized rabbit tendon scaffolds: scaffolds with no cells, and scaffolds re-seeded with either tenocytes or adipoderived stem cells. Autologous flexor tendon grafts were used as controls. All constructs bridged a zone II defect in the rabbit and were explanted at 2, 4, 10, or 20 weeks. These tendons were then tested for ultimate tensile strength (UTS) or processed for histology. The experimental groups exhibited UTS comparable to autologous grafts up to 4 weeks, and were significantly weaker at 10 weeks (p < 0.000–0.024). At 20 weeks, UTS was significantly improved (p = 0.013) in tenocyte-seeded constructs compared with 10 weeks. There was no significant difference in UTS between seeded or unseeded constructs at 2, 4, and 20 weeks. In all groups, there were more cells at the repair ends, and the cells penetrated to the core of the grafts over time. The goal of this technology is the development of tissue engineered tendon grafts for clinical use. This study provides proof of the concept that tissue-engineered flexor tendons—both acellularized and reseeded—can survive and incorporate over time. Further work will focus on bioreactor preconditioning of reseeded constructs to increase ultimate tensile strength.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Zone II flexor tendon losses represent a significant challenge for hand surgeons. While techniques for zone II repair with tendon grafts have been refined over the last century, clinical outcomes remain poor for many patients. In particular, two main problems exist for zone II flexor tendon defects: (1) post-operative adhesions, and 2) lack of appropriate tendon material for reconstruction. A number of strategies are currently being employed to reduce post-operative adhesion formation [1–7]. However, the development of new materials for tendon reconstruction needs to be further explored.
Many researchers have attempted to use synthetic materials to bridge flexor tendon defects. A number of materials have been studied including Dacron grafts, carbon fibers, and silastic sheets [8–10]. However, results for these materials have been poor with regard to healing and mechanical stability. It has become evident that synthetic materials are so far unsuitable for tendon reconstruction.
Currently, autologous tendons including the palmaris longus, plantaris, extensor indicis proprius, and long toe extensors are the gold standard donor grafts [11, 12]. However, use of these tendons may result in significant donor site morbidity. There is also greater demand than supply in patients with devastating injuries requiring many grafts and in patients who lack the donor tendons. Furthermore, some studies have also shown a difference in functional outcome when an intrasynovial tendon graft is used compared with extrasynovial tendon grafts such as the palmaris and plantaris tendons [13, 14]. Recently, intrasynovial donor tendons have been harvested from the flexor digitorum longus tendons of the foot in humans [15]. While results have been favorable, there will not be enough tendon material for reconstruction in cases with extensive tendon loss. Furthermore, donor site morbidity is higher when harvesting intrasynovial autologous tendons.
Human allografts have also been used to replace tendon losses in zone II flexor tendon injuries. While initial results were poor, a report of two patients receiving allograft reconstruction showed promising outcomes [16]. However, the potential for disease transmission, the need for possible immunosuppression and bioethical concerns have made the use of allograft tendons not a reasonable option.
Tissue engineering of flexor tendons is the next logical step in providing material for reconstruction. This rabbit model involves acellularization of intrasynovial flexor tendons and re-seeding with cells to recreate viable and strong tendon grafts with properties of native intrasynovial tendons. Previously, the acellularization process has been optimized [17], and the viability of the tendon grafts has been demonstrated in vitro and in vivo [18]. The purpose of this study was to further characterize the in vivo properties of our tissue-engineered rabbit flexor tendons including mechanical strength in terms of ultimate tensile strength, and histological appearance. We hypothesized that re-seeded constructs would have superior strength in vivo compared with acellularized un-seeded constructs, and comparable to those of autologous grafts.
Methods
Adult male New Zealand white rabbits (4.0–4.5 kg; Harlan Laboratories) were used. All animal experiments followed protocols approved by our institutional animal ethics committee. The experimental groups included acellularized tendons seeded with tenocytes, acellularized tendons seeded with adipoderived stem cells (ASC), and acellularized tendons that were un-seeded. Autologus zone II flexor tendon grafts served as controls.
Cell line isolation and culture
The rabbits were terminated by an intravenous injection of Euthasol (Virbac AH Inc., Fort Worth, TX). Using sterile technique under loupe magnification, the forepaw and hindpaw flexor digitorum profundus (FDP) equivalents were dissected, and 2–2.5 cm portions of the intrasynovial FDP tendon were excised. Specimens were placed into buffered Hank's saline solution with penicillin 100 IU/mL (Gibco, Rockville, MD) and streptomycin 100 μg/mL (Gibco).
Tenocytes were obtained using a previously established protocol [19]. Harvested tendons were treated with 0.5% collagenase type IA (Sigma, St. Louis, MO) for 10 min at room temperature to obtain tenocytes. The released cells were plated and cultured in Ham's F12 medium (Gibco) with 10% fetal bovine serum (Gibco).
ASCs were obtained from inguinal fat pads using a technique published by Zuk et al. [20, 21]. The fat was minced with scissors and treated with 0.075% collagenase II in a shaking water bath at 37°C for 10 min. Collagenase was then inactivated using fresh medium. The cell suspensions underwent centrifugation at 1,000 rpm for 5 min, and the supernatant was aspirated. The resulting cell pellet was re-suspended in fresh Ham's F12 medium (Gibco), and filtered through a 100-μm nylon cell strainer. The cells were put in a new tube, and centrifuged again at 1,000 rpm for 5 min. Finally, the cells were incubated and grown at 37°C in a humidified standard incubator with 5% CO2. Culture media was changed every 3 days.
Acellularization of flexor tendons
Tendons for acellularization were harvested as described above, washed with phosphate buffered saline (PBS), and subsequently frozen at –70°C. Frozen tendons were thawed to room temperature and then placed into trypsin 0.05%/ethylenediaminetetraaceticacid (EDTA) for 24 h at 37°C followed by Triton X-100 0.5% for 24 h at room temperature. Representative samples of tendon were obtained before and after treatment for evaluation by light microscopy. Evaluation of the samples confirmed that the protocol resulted in complete removal of viable cells.Reseeding of acellularized tendons in vitro
Acellular tendon scaffolds (2 cm long) were reseeded by immersion of the tendons in media with the cell mixture (tenocytes or ASCs,) at a density of 2 × 106 cells/mL. The cell-scaffold constructs were then incubated at 37°C in a humidified tissue culture chamber with 5% CO2 to allow attachment of cells. The culture medium was changed every other day during the incubation period. Only cells from passage 2–6 were used for reseeding of tendon scaffolds (Fig. 1).
In vivo implantation of reseeded tendon constructs
The rabbits were anesthetized with an intramuscular injection of acepromazine (0.01 mg/kg), xylazine 4 mg/mL (5 mg/kg), and ketamine 40 mg/mL (50 mg/kg) and maintained with inhalational Isoflurane (Baxter Health Care Corp., Deerfield, IL) delivered via face mask.
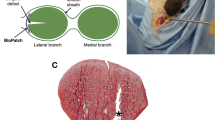
Under sterile conditions, an L-shaped incision was made on the palmar surface for access of zone III of the third or fourth digits' FDP tendons of the right forelimb. Dissection was carried out under loupe magnification to identify the FDP to the third or fourth digits. Neurovascular structures adjacent to the tendons were protected during the dissection. To ensure the surgical technique was the same as the experimental tendon graft group, the autologous tendon graft control was treated as follows. The FDP tendon too was transected 0.5 cm proximal to the A1 pulley. The cut end was immediately repaired. A separate skin incision was made over the distal phalanx, the FDP insertion was identified, and the tendon was transected approximately 3 mm proximal to it. The FDP was then pulled proximally through its sheath into the palmar wound in order to break all vinculae. The distal end of the tendon was then re-threaded though the tendon sheath as well as the pulleys, and repaired to the distal stump. As for the experimental grafts, a distal skin incision was made and the native tendon was transected approximately 3 mm proximal to the bony insertion. The native tendon was then pulled into the proximal palmar wound and cut 0.5 cm proximal to the A1 pulley. The resulting free zone II tendon section was removed and used to isolate tenocytes. Experimental constructs (i.e., acellularized tendons without cells, tenocyte-seeded tendons, and ASC-seeded tendons) were then used to fill the zone II gap which had been created. All tendon repairs were performed using a 2-core strand modified Kessler technique with an epitendinous repair using 6-0 polypropylene (Ethicon, Somerville, NJ). Of note due to institutional restrictions, the FDP tendons were unloaded near the carpal tunnel, which removed the necessity to immobilize the animal with a cast postoperatively. A single simple stitch was used to tag the proximal cut end of the native FDP to one slip of the FDS tendon to help prevent migration of the graft distally.
Animals were fed standard lab chow and allowed to roam unrestricted in their cages. The experimental tendons grafts of the third digit along with autologous graft control of the fourth digit were harvested at 2, 4, 10, and 20 weeks after surgery. The rabbits were terminated by an intravenous injection of Euthasol (Virbac AH Inc.). The FDP tendon and interpositional grafts were dissected free of surrounding tissues and subjected to mechanical testing the same day, or immersed in PBS and taken for histology.
Mechanical testing for ultimate tensile strength
Tensile testing was performed to compare the ultimate tensile strength of acellularized tendons and re-seeded flexor tendon constructs. The ultimate tensile strength (MPa) is the maximum resistance to rupture, and it is equivalent to the maximum load (N) that can be carried by one square millimeter of cross-sectional area when the load is applied as simple tension.
The ends of the tendons were glued between fine sandpaper and clamped between the grips of a materials testing system (MTS 858, MTS Corp., Eden Prairie, MN). The biomechanical testing protocol included initial application of 10 preconditioning load-unload cycles of 10 mm/min. A final 11th loading cycle then applied tensile force until tendon failure. Load-displacement data was recorded (TestwareSX, MTS Corp).
The cross-sectional area at the breaking point of the tendon constructs was determined by obtaining two orthogonal photographs of each clamped tendon using a tripod mounted high-resolution digital camera (Nikon D100, Nikon Corp., Japan) at a fixed distance together with a known length standard. Using image analysis software (ImageJ, NIH) the two orthogonal diameters were measured at the breaking region of the tendon construct, and the cross-sectional area was calculated on the basis of an ellipse.
To obtain the ultimate tensile strength, the breaking force of each tendon construct was divided by the cross-sectional area at the breaking point.
Histological analysis of tendons
Samples of harvested tissue in each group were embedded in paraffin and processed to produce hematoxylin and eosin stained slides.
Statistical analysis
The number of constructs in each group is presented in Table 1. Variations in sample size are due to animals sacrificed due to infection or other post-surgical complications. One-way analysis of variance (ANOVA) with Tukey's post-hoc test was used to compare means between groups at each time point and within each group across all time points. The significance level was set to 0.05.
Results
Macroscopic appearance
Careful dissection was performed under loupe magnification. The experimental groups including acellularized grafts, tenocyte-seeded grafts, and ASC-seeded grafts, all appeared indistinguishable from the autologous graft control. All experimental groups showed structurally intact tendon with glistening surfaces (Fig. 2). There was only minimal adhesion noted in zone II in all specimens. The results were similar comparing groups at all time points from 2 weeks to 20 weeks.
Histological appearance
All tendons within each experimental group showed similar characteristics over time. The re-seeded tendon constructs exhibited small cells with rounded nuclei. At 2 weeks these cells were populating the outermost layers of the tendon constructs, but from 10 weeks and onwards, these cells were found also in increasing numbers within the endotenon of the constructs (Fig. 3). The un-seeded tendons exhibited fewer cells compared to the re-seeded tendons. Cellularity varied along the tendon, namely there were more cells at the repair ends of the tendon grafts (not shown).
Hematoxylin and eosin-stained sections from the tenocyte-seeded experimental group at 2, 4, 10, and 20 weeks (top to bottom). Tenocyte-like cells are seen mainly in the epitenon at 2 weeks. At 10 weeks and onwards, the number of cells seen throughout the tendon scaffold including the endotenon has increased
Mechanical testing for ultimate tensile strength
Comparisons of group means were made within the four groups across the different time points 2, 4, 10, and 20 weeks to detect change over time. Also, comparisons of group means were made between the four groups at each time point.
Comparisons within groups
All experimental groups were significantly stronger at 2 weeks compared with the 10-week time point (tenocyte-seeded constructs 45.7 MPa vs 13.2 MPa, p = 0.005; ASC-seeded constructs 67.4 MPa vs 17.7 MPa, p < 0.000; acellularized constructs 61.2 MPa vs 16.4 MPa, p = 0.005). There was a tendency for the autologous graft controls to be stronger at the 2-week time point compared with the 10-week time point (51.9 MPa vs 31.2 MPa p = 0.068). All groups including the autologous graft control showed a tendency to be stronger at 20 weeks compared with the 10-week time point, and this difference was statistically significant for tenocyte-seeded constructs (tenocyte-seeded constructs 13.2 MPa vs 41.5 MPa, p = 0.013; ASC-seeded constructs 17.7 MPa vs 46.5 MPa, p = 0.075; acellularized constructs 16.4 MPa vs 38.7 MPa, p = 0.139; autologous graft controls 31.2 MPa vs 58.6 MPa p = 0.081). Thus, at the 20-week time point all four groups including the autologous graft controls had regained their ultimate tensile strength compared with the initial 2-week time point (tenocyte-seeded constructs 45.7 MPa vs 41.5 MPa, p = 0.953; ASC-seeded constructs 67.4 MPa vs 46.5 MPa, p = 0.208; acellularized constructs 61.2 MPa vs 38.7 MPa, p = 0.208; and autologous grafts 51.9 MPa vs 58.6 MPa, p = 0.895) (Fig. 4).
Ultimate tensile strength of explanted tendon constructs. Shown here is autologous graft control (white), tenocyte-seeded constructs (light grey), adipo-derived stem cell-seeded constructs (dark grey), and acellularized constructs (black) at 2, 4, 10, and 20 weeks postoperatively. T-bars indicate standard error of the mean
Comparisons between groups
There was no significant difference in ultimate tensile strength between the experimental groups and the autologous control at 2 weeks (tenocyte-seeded constructs 45.7 MPa; ASC-seeded constructs 67.4 MPa; acellularized constructs 61.2 MPa; autologous graft controls 51.9 MPa, p = 0.273), 4 weeks (tenocyte-seeded constructs 41.3 MPa; ASC-seeded constructs 42.5 MPa; acellularized constructs 45.7 MPa; autologous graft controls 41.8 MPa, p = 0.969.), and 20 weeks (tenocyte-seeded constructs 41.5 MPa; ASC-seeded constructs 46.5 MPa; acellularized constructs 38.7 MPa; autologous graft controls 58.6 MPa, p = 0.182.). At the 10-week time point, the autologous graft control constructs (31.2 MPa) were significantly stronger than the tenocyte-seeded constructs (13.2 MPa, p = 0.005), the ASC-seeded constructs (17.7 MPa, p = 0.038), and the acellularized constructs (16.4 MPa, p = 0.005) (Fig. 4).
Discussion
It is possible to acellularize rabbit flexor tendons and to use them as scaffolds for tissue engineered flexor tendon constructs [18, 22, 23]. In addition, cultured tenocytes and ASCs proliferate and produce collagen in vitro [18, 22]. Tenocytes that are re-seeded onto acellularized scaffolds have been shown to migrate into the core of tendon construct in vivo [23]. In all, these techniques make the construction of a functional tissue-engineered flexor tendon in the rabbit possible.
In the present study, re-seeded flexor tendon constructs incorporated effectively on the macroscopic level. Histologically, the re-seeded constructs exhibited cells with small rounded nuclei on the epitenon at 2 weeks, and there was an increasing number of cells at the center of the construct at 10 weeks and onwards. This phenomenon represents a growth and migration of the re-seeded cells from the periphery to the core.
Moreover, the flexor tendon constructs seeded with either tenocytes or ASCs maintained tensile strength comparable to autologous grafts up to 4 weeks, but at 10 weeks the tendons in all experimental groups became weaker compared with autologous grafts. These results are similar to those found in a study by Cao et al. where tissue engineered tendon constructs were weakest at around 10 weeks [24]. By 20 weeks, we observed an increase in ultimate tensile strength in the tenocyte group and a tendency for the ASC and acellularized groups to increase in strength.
The fact that the experimental grafts were weaker at 10 weeks compared to the autologous grafts is concerning for the clinical application of this technology. It was surprising given that the macroscopic appearances of the tendon in these groups are indistinguishable to that of the autologous grafts by several independent observers. We did not observe an inflammatory response in the re-seeded tendons compared to the autologous grafts that could explain the difference. The cell migration from the periphery to the core of the construct observed around 10 weeks may be responsible for weakening the collagen architecture. This observation would point to the importance of endotenon tenocytes embedded within the core of the tendon in preserving tensile strength. Nevertheless, weakening and regaining strength over time is also part of the natural course of healing for all tendon grafts, including autologous grafts.
Acellularized and re-seeded tendon constructs exhibited similar biomechanical characteristics as the autologous graft controls at 2, 4, and 20 weeks. The fact that acellularized tendons did not differ in ultimate tensile strength from re-seeded constructs may suggest that re-seeding of cells onto acellularized tendons is not necessary to obtain stronger constructs, contrary to current theory.
However, in recent work, re-seeded flexor tendon constructs have been shown to increase in strength when subjected to cyclic strain in a bioreactor in vitro whereas unseeded acellularized constructs did not increase strength [23]. By utilizing the bioreactor on re-seeded tendon constructs prior to implantation, tendon tensile strength may be increased. Future work in this model will focus on bioreactor pre-conditioning as an intermediate step between construct reseeding and in vivo implantation.
In conclusion, data from this study showed that acellularized tendons can be re-seeded with cells and implanted to bridge zone II flexor tendon defects in rabbits with minimal adhesions and with similar biomechanical characteristics up to 4 weeks as autologous grafts. Moreover, the results show that there is an initial decrease in strength in the re-seeded tendon constructs at 10 weeks that is similarly seen in autologous grafts. After 20 weeks, strength is significantly improved in tenocyte-seeded constructs compared with the 10-week time point. In addition, the need for re-seeding tendon constructs can be challenged since there was no significant difference in strength between re-seeded and un-seeded acellularized constructs at 20 weeks. Pre-conditioning re-seeded constructs with cyclic strain in a bioreactor prior to implantation will be the next necessary step towards increasing construct strength. Stronger constructs may be important when these tissue engineering techniques are in clinical use because they will allow for early motion training to decrease the formation of adhesions.
References
Amiel D, Ishizue K, Billings E Jr, Wiig M, Vande Berg J, Akeson WH, Gelberman R (1989) Hyaluronan in flexor tendon repair. J Hand Surg [Am] 14:837–843
Chang J, Thunder R, Most D, Longaker MT, Lineaweaver WC (2000) Studies in flexor tendon wound healing: neutralizing antibody to TGF-beta1 increases postoperative range of motion. Plast Reconstr Surg 105:148–155
Kulick MI, Brazlow R, Smith S, Hentz VR (1984) Injectable Ibuprofen: preliminary evaluation of its ability to decrease peritendinous adhesions. Ann Plast Surg 13:459–467
Nyska M, Porat S, Nyska A, Rousso M, Shoshan S (1987) Decreased adhesion formation in flexor tendons by topical application of enriched collagen solution—a histological study. Arch Orthop Trauma Surg 106:192–194
Salti NI, Tuel RJ, Mass DP (1993) Effect of hyaluronic acid on rabbit profundus flexor tendon healing in vitro. J Surg Res 55:411–415
Thomas SC, Jones LC, Hungerford DS (1986) Hyaluronic acid and its effect on postoperative adhesions in the rabbit flexor tendon. A preliminary look. Clin Orthop Relat Res 206:281–289
Zhang AY, Pham H, Ho F, Teng K, Longaker MT, Chang J (2004) Inhibition of TGF-beta-induced collagen production in rabbit flexor tendons. J Hand Surg [Am] 29:230–235
Alexander H, Weiss AB, Parsons JR (1986) Ligament and tendon repair with an absorbable polymer-coated carbon fiber stent. Bull Hosp Jt Dis Orthop Inst 46:155–173
Holtz M, Midenberg ML, Kirschenbaum SE (1982) Utilization of a silastic sheet in tendon repair of the foot. J Foot Surg 21:253–259
Lieberman JR, Lozman J, Czajka J, Dougherty J (1988) Repair of Achilles tendon ruptures with Dacron vascular graft. Clin Orthop Relat Res 234:204–208
Bunnell S (1918) Repair of tendons in the fingers and description of two new instruments. Surg Gynecol Obstet 26:103–110
White WL (1960) Tendon grafts: a consideration of their source, procurement and suitability. Surg Clin North Am 40:403–413
Bischoff RJ, Morifusa S, Gelberman RH, Winters SC, Woo SL, Seiller JG 3rd (1998) The effects of proximal load on the excursion of autogenous flexor tendon grafts. J Hand Surg [Am] 23:285–289
Seiler JG 3rd, Chu CR, Amiel D, Woo SL, Gelberman RH (1997) The Marshall R. Urist Young Investigator Award. Autogenous flexor tendon grafts. Biologic mechanisms for incorporation. Clin Orthop Relat Res 345:239–247
Leversedge FJ, Zelouf D, Williams C, Gelberman RH, Seiler JG 3rd (2000) Flexor tendon grafting to the hand: an assessment of the intrasynovial donor tendon-A preliminary single-cohort study. J Hand Surg [Am] 25:721–730
Asencio G, Abihaidar G, Leonardi C (1996) Human composite flexor tendon allografts. A report of two cases. J Hand Surg [Br] 21:84–88
Zhang AY, Bates SJ, Morrow E, Pham H, Pham B, Chang J (2009) Tissue engineered intrasynovial tendons: optimization of acellularization and seeding. J Rehabil Res Dev 46:489–498
Kryger GS, Chong AK, Costa M, Pham H, Bates SJ, Chang J (2007) A comparison of tenocytes and mesenchymal stem cells for use in flexor tendon tissue engineering. J Hand Surg [Am] 32:597–605
Klein MB, Pham H, Yalamanchi N, Chang J (2001) Flexor tendon wound healing in vitro: the effect of lactate on tendon cell proliferation and collagen production. J Hand Surg [Am] 26:847–854
De Ugarte DA, Morizono K, Elbarbary A, Alfonso Z, Zuk PA, Zhu M, Dragoo JL, Ashjian P, Thomas B, Benhaim P, Chen I, Fraser J, Hedrick MH (2003) Comparison of multi-lineage cells from human adipose tissue and bone marrow. Cells Tissues Organs 174:101–109
Zuk PA, Zhu M, Mizuno H, Huang J, Futrell JW, Katz AJ, Benhaim P, Lorenz HP, Hedrick MH (2001) Multilineage cells from human adipose tissue: implications for cell-based therapies. Tissue Eng 7:211–228
Riboh J, Chong AK, Pham H, Longaker M, Jacobs C, Chang J (2008) Optimization of flexor tendon tissue engineering with a cyclic strain bioreactor. J Hand Surg [Am] 33:1388–1396
Thorfinn J, Saber S, Angelidis IK, Ki SH, Zhang AY, Chong AK, Pham HM, Lee GK, Chang J. (2009) Flexor tendon tissue engineering: temporal distribution of donor tenocytes versus recipient cells. Plast Reconstr Surg 124:2019–2026
Cao Y, Liu Y, Liu W, Shan Q, Buonocore SD, Cui L (2002) Bridging tendon defects using autologous tenocyte engineered tendon in a hen model. Plast Reconstr Surg 110:1280–1289
Acknowledgements
Parts of this study were financially supported by Veterans Affairs Medical Merit Review Grant and a Veterans Affairs Rehabilitation Research and Development Merit Review Grant. Contributions have also been made from the Swedish Fulbright Commission, the County Council of Östergötland (Sweden), Börje Gabrielsson's Memorial Fund, the Swedish Society of Medicine, the Johan & Jakob Söderberg Foundation, and the Linköping Society of Medicine.
Author information
Authors and Affiliations
Corresponding author
Additional information
Dr. Zhang and Dr. Thorfinn share the status as first author as their contributions to this study have been equal.
Rights and permissions
About this article
Cite this article
Zhang, A.Y., Thorfinn, J., Saber, S. et al. Tissue engineered intrasynovial tendons: in vivo graft survival and tensile strength. Eur J Plast Surg 33, 283–289 (2010). https://doi.org/10.1007/s00238-010-0398-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00238-010-0398-4