Abstract
Rationale
Alzheimer’s disease (AD) is a neurodegenerative disorder with irreversible loss of intellectual abilities. Current therapies for AD are still insufficient.
Objective
In this study, the effect of ellagic acid on learning and memory deficits was evaluated in intrahippocampal amyloid beta (Aβ25–35)-microinjected rats and its modes of action were also explored.
Methods
AD rat model was induced by bilateral intrahippocampal microinjection of Aβ25–35 and ellagic acid was daily administered (10, 50, and 100 mg/kg), and learning, recognition memory, and spatial memory were evaluated in addition to histochemical assessment, oxidative stress, cholinesterases activity, and level of nuclear factor-kappaB (NF-κB), Toll-like receptor 4 (TLR4), and nuclear factor (erythroid-derived 2)-like 2 (Nrf2).
Results
The amyloid beta-microinjected rats showed a lower discrimination ratio in novel object and alternation score in Y maze tasks and exhibited an impairment of retention and recall capability in passive avoidance paradigm and higher working and reference memory errors in radial arm maze (RAM). In addition, amyloid beta group showed a lower number of Nissl-stained neurons in CA1 area in addition to enhanced oxidative stress, higher activity of cholinesterases, greater level of NF-κB and TLR4, and lower level of nuclear/cytoplasmic ratio for Nrf2 and ellagic acid at a dose of 100 mg/kg significantly prevented most of these abnormal alterations.
Conclusions
Ellagic acid pretreatment of intrahippocampal amyloid beta-microinjected rats could dose-dependently improve learning and memory deficits via neuronal protection and at molecular level through mitigation of oxidative stress and acetylcholinesterase (AChE) activity and modulation of NF-κB/Nrf2/TLR4 signaling pathway.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Alzheimer’s disease (AD) is a neurodegenerative disorder and is the most common form of dementia in elderly with pathological hallmarks including extracellular accumulation of beta amyloid and intracellular neurofibrillary tangles (Mattson 2004). AD is typically represented by a progressive loss of cognitive function, dementia development, and altered behavior (Lau and Brodney 2008). Amyloid beta (Aβ) peptides have the potential to induce oxidative stress and neuroinflammation in the brain and play pivotal roles in the pathogenesis of AD (Galasko and Montine 2010). Learning and memory and spatial recognition memory deficits have been reported in Aβ-induced model of AD in rodents (Capurro et al. 2013; Ghofrani et al. 2015). Cholinergic dysfunction and its ensuing memory deficit (Daulatzai 2010), inflammatory processes, an overexpression of Toll-like receptor 4 (TLR4), and an activation of nuclear factor κB (NF-κB) signaling pathway have all contributed to Aβ-induced dysfunctions and pathology (Ma et al. 2015b). The nuclear factor erythroid-2-related factor 2 (Nrf2) pathway also plays a significant role in inducing some detoxifying enzymes and antioxidant proteins and for this reason has been suggested as a promising target for neuroprotective strategies in AD (Yang et al. 2015). Current management therapies for AD are still insufficient and research studies are underway to explore more effective therapeutics to prevent and/or retard AD pathogenic course (Golde 2016).
Ellagic acid is a polyphenol and a natural dimeric derivative of gallic acid that is found in fruits and nuts like grapes, strawberries, raspberries, pomegranate, and walnut (Priyadarsini et al. 2002). This polyphenol acts as an antioxidant and anti-inflammatory agent in mammalian cells (Hwang et al. 2010). The neuroprotective role of this compound has been reported in different experimental models (Dolatshahi et al. 2015; Ferreres et al. 2013; Kabiraj et al. 2014). In addition, ellagic acid could improve memory deficit in 6-hydroxydopamine-induced model of Parkinson’s disease (Dolatshahi et al. 2015) and is able to ameliorate cognitive disturbance following scopolamine administration (Mansouri et al. 2016) and to prevent cognitive deficits due to traumatic brain injury (Farbood et al. 2015). Anticholinesterase and antioxidant activity of ellagic acid in an in vitro setting has also been demonstrated (Ferreres et al. 2013). Since compounds capable to improve cholinergic transmission and with anti-oxidative and anti-inflammatory properties are good candidates for AD therapy, therefore, we tried to assess the neuroprotective potential of ellagic acid in an intrahippocampal Aβ25–35-injected rat model of AD and to unravel some underlying and related mechanisms.
Material and methods
Animals
Adult male Wistar rats (Pasteur’s Institute, Tehran) (200–245 g at the start of the study), three to four per cage, were kept in a temperature-controlled colony room (21–23 °C) under 12:12 light/dark cycle (lights on at 06–18). Animals allowed to habituate to their environment for 1 week prior to being tested and handled daily. All behavioral experiments carried out between 10 a.m. and 4 p.m. This study was conducted in accordance with the policies stipulated in the Guide for the Care and Use of Laboratory Animals (NIH) and approved by the Ethics Committee of Shahed University (Tehran, Iran).
Experimental procedure
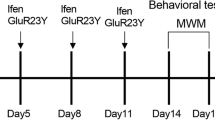
Rats (n = 72) were randomly allocated to the following equal-sized groups: sham, ellagic acid-pretreated sham at a dose of 100 mg/kg, Aβ, and ellagic acid-pretreated Aβ groups at doses of 10, 50, or 100 mg/kg. For stereotaxic surgery, rats were anesthetized with a combination of ketamine and xylazine (80 and 10 mg/kg, respectively; i.p.) and then placed in a Narishige stereotaxic apparatus (Japan) (incisor bar −3.3 mm, ear bars placed symmetrically). The scalp was disinfected with an iodine solution and incised on the midline, and a burr hole was drilled through the skull and aggregated Aβ25–35 (Sigma-Aldrich, USA) at a volume of 2 μl was delivered at coordinates −3.5 mm posterior to bregma, 2 mm lateral to sagittal suture, and 2.7–2.8 mm below dura, according to the stereotaxic atlas (Paxinos and Watson 1986). Ellagic acid (Sigma-Aldrich, USA) was dissolved in 30% Cremophor (Sigma-Aldrich, USA) and intraperitoneally administered at doses of 10, 50, or 100 mg/kg/day for 1 week and its last injection was 1 hour before surgery. Animals in the Aβ groups were bilaterally injected in the dorsal hippocampus with 2 μl of normal saline containing 10 μg aggregated Aβ25–35 (5 μg/μl). To produce neurotoxicity, normal saline-dissolved Aβ25–35 was incubated at 37 °C for 7 days to allow fibril formation (Liu et al. 2010). Sham groups received 2 μl of normal saline bilaterally instead of Aβ solution. Postoperatively, the rats were given special care until normal feeding was restored. Behavioral tests were conducted at third week post-surgery as depicted in Fig. 1 and evaluated blind to the treatments by trained observer.
Behavioral tests
Novel object discrimination (NOD) task
The used protocol of this experiment has been reported in earlier studies (Baluchnejadmojarad et al. 2017; Stuart et al. 2013; Zarezadeh et al. 2017). In this test, each animal received two successive 5-min object exploration trials separated by a 4-h inter-trial interval. During the familiarization trial, the animals were individually exposed to two similar objects, and one of the objects was selected and replaced with a third, novel object in the second trial. During these two trials, exploration of each object, defined as sniffing, licking, chewing, or having moving vibrissae while directing the nose toward and ≤1 cm from the object, was separately recorded. Sitting on an object in the absence of any directed interest was not recorded. The objects and test areas between trials were cleaned with diluted alcohol to lower odor cues and possible errors. The discrimination (D) ratio was calculated as time spent exploring the novel object compared with the familiar object relative to the total time spent exploring all objects, according to the formula: (t [novel] − t [familiar]) / (t [novel] + t [familiar]) × 100. NOD task was conducted on day 15 post-surgery.
Y maze task
Spatial recognition memory was judged by recording spontaneous alternation behavior in a single-session Y maze on the 16th day post-surgery, as described before (Roghani et al. 2006). The maze was made of black Plexiglas with arms 40 cm long, 30 cm high, and 15 cm wide. The arms converged in a triangular central arena. The procedure was as follows: each rat, naive to the maze, was placed at the end of one arm and allowed to move freely through the maze during an 8-min session. The series of arm entries were recorded. An entry was considered when the base of the animal’s tail was entirely within the arm. Alternation was defined as successive entries into the three arms on overlapping triplet sets. The maximum number of possible spontaneous alternations was determined as the total number of arms entered minus 2, and the percentage was calculated as the ratio of actual to possible alternations × 100.
Passive avoidance task
The protocol of this test has been described before (Ahshin-Majd et al. 2016; Ghofrani et al. 2015; Kiasalari et al. 2016; Nasri et al. 2012). The apparatus (40 cm long × 20 cm wide × 30 cm high) was composed of an illuminated chamber connected to a dark chamber by a guillotine door. An electric shock was delivered to the grid floor by a stimulator. On the first and second days of testing, each rat was placed in the apparatus for 10 min to be habituated. On the third day, an acquisition trial was conducted. Rats were placed individually in the illuminated chamber. After a habituation period (5 min), the guillotine door was lifted, and after rat entrance into the dark chamber, the door was lowered and an electric shock (1 mA, 1 s) applied. In this trial, the initial latency (IL) of entrance into the dark chamber was recorded, and rats with ILs greater than 60 s were excluded from the study. Twenty-four hours later, each rat was placed in the illuminated chamber to evaluate retention and recall capability. The interval between placement in the illuminated chamber and entry into the dark chamber was regarded as step-through latency (STL, up to a maximum of 300 s). This test was conducted on days 17–20 post-surgery.
Radial arm maze task
The radial arm maze apparatus used in our study comprised of eight arms, numbered from 1 to 8, extending radially from a central area. The arms were 50 cm above the floor in a dimly lighted room with various visual cues placed at the same position throughout the study. At the end of each arm, there was a food cup. The used protocol of this task has been described before (Cioanca et al. 2013; Hritcu et al. 2014). The animals were first kept on a restricted food regimen and their body weight maintained at 85% of their initial weight. Before the training started, three to four rats were simultaneously placed in the apparatus to explore it for 5 min and take food freely. The food was initially scattered throughout the maze but was gradually limited to food cups. The animals were trained for 4 days to run to the end of the arms and consume the baited food. The training trial continued until all the five baits had been used up or until 5 min has passed. After adaptation, all the rats were trained with one trial per day for seven consecutive days. The test was continued for 11 consecutive days. Each animal was placed individually in the center of the maze and checked for working and reference memory, in which the same five arms (nos. 1, 2, 4, 5, and 7) were baited for each trial. The other three arms (nos. 3, 6, and 8) were never baited. When the animals made seven or eight correct choices and less than one error in three successive sessions, they were included for further studies. Retention trials were done on day 21 post-surgery. The maze was cleaned with diluted ethanol between the trials. Finally, the number of working memory errors (entering an arm containing food but previously entered) and reference memory errors (entering an arm that never baited) was assessed. Reference memory is regarded as a long-term memory for information that remains constant over repeated trials and working memory is regarded a short-time memory in which the information to be remembered changes in every trial (Hritcu et al. 2012; Olton and Samuelson 1976).
Determination of hippocampal oxidative stress
At the end of week 3 post-surgery, rats (n = 6–7 from each experimental group) were deeply anesthetized with diethyl ether and hippocampal tissue was punched out and 10% homogenate was prepared in cold hypotonic lysis buffer and in the presence of protease inhibitor cocktail. After centrifuging, the supernatant comprising of cytosolic proteins was used as cytosolic fraction. The resulting pellets were resuspended in hypertonic buffer containing HEPES, MgCl2, NaCl, EDTA, DTT, glycerol, and PMSF and were vortexed and centrifuged. The resulting supernatant was used for determination of nuclear content of Nrf2.
Malondialdehyde (MDA) level in the supernatant was measured as described before (Baluchnejadmojarad and Roghani 2012). For determination of MDA concentration (thiobarbituric acid reactive substances, TBARS), trichloroacetic acid and TBARS reagent were added to supernatant and then mixed and incubated at boiling water for 90 min. After cooling on ice, samples centrifuged at 1000×g for 10 min and the absorbance of the supernatant were read at 532 nm. The results were reported according to tetraethoxypropane standard curve.
For catalase activity assay, Claiborne’s method was used (Claiborne 1985). Briefly, H2O2 was added to a mixture of 50 mM potassium phosphate buffer and supernatant and the rate of H2O2 decomposition assessed by measuring the absorbance changes at 240 nm.
Reduced glutathione (GSH) was measured according to earlier studies (Ellman 1959; Sedlak and Lindsay 1968). For this purpose, the supernatant was centrifuged with 5% trichloroacetic acid. Then, phosphate buffer (pH 8.4), 5′5-dithiobis(2-nitrobenzoic acid), and distilled water were added to the supernatant and the absorbance was read at 412 nm.
Supernatant nitrite (NO2 −) content was measured by Griess method, as described before (Baluchnejadmojarad and Roghani 2012). In this assay used here, NO3 − is converted to NO2 − by cadmium and this is followed by color development with Griess reagent (sulfanilamide and N-naphthyl ethylenediamine) in acidic medium. The absorbance was determined using a spectrophotometer at 540 nm.
Bradford method was used for the determination of protein content using bovine serum albumin as the standard (Bradford 1976).
Hippocampal acetylcholinesterase (AChE) and butyrylcholinesterase (BChE) activity assay
AChE and BChE activity in hippocampal lysates was determined by a modified method of Ellman’s according to Isomae et al. (Isomae et al. 2003). The activity of AChE and BChE was determined by measuring the formation of the yellow anion obtained from the reaction between Ellman’s reagent and the thiocholine formed by enzymatic degradation of acetylthiocholine and butyrylthiocholine, respectively, at a wavelength of 412 nm and data reported as micromoles of substrate hydrolyzed per minute per gram protein.
Determination of hippocampal TLR4, Nrf2, and NF-κB
The expression level of TLR4, Nrf2, and NF-κB in the hippocampal supernatant was measured using sandwich enzyme-linked immunosorbent assay and commercial kits according to the manufacturer’s instructions (Cloud-Clone Corp., Houston, USA). The absorbance of samples was read at 450 nm by Synergy HT microplate reader (BioTek, USA) and values calculated according to related standard curves.
Histological evaluation
For this purpose, the rats (n = 5 from each experimental group) were deeply anesthetized with a high dose of ketamine (150 mg/kg) and perfused through the ascending aorta with 50 ml of heparinized normal saline followed by 100–150 ml of fixative solution containing 4% paraformaldehyde in 0.1 M phosphate buffer (PB, pH 7.4). Following perfusion, brains were removed from the skull and postfixed for 1 week, left hippocampal block was prepared and embedded in paraffin, and hippocampal block was cut into 15 μm coronal sections and prepared for Cresyl violet (Nissl) staining. Neuronal counting was done in CA1 area of the hippocampus in at least three sections at a level range between −3.6 and −4.3 mm from the bregma (according to the coordinates of the stereotaxic atlas of Paxinos and Watson in an area of 0.1 mm2 using an image capturing and analysis system (Bel Engineering, Italy). Cells with a clear membrane and a visible nucleolus were included in counting. The process was repeated two times for each section and done blind to the treatments received.
Statistical analysis
All results expressed as mean ± SEM. The parametric test one-way ANOVA was used for data analysis and, if a difference was found out to be significant, pairwise comparison was done using the Tukey post hoc test. In all calculations, a difference at P < 0.05 was regarded as significant.
Result
Novel object discrimination
There was a significant reduction of discrimination ratio in amyloid beta-microinjected group relative to sham (P < 0.01), and such significant reduction was also observed for amyloid beta+ellagic acid 10 group (P < 0.05). In contrast, discrimination ratio was significantly greater in amyloid beta+ellagic acid 50 and amyloid beta+ellagic acid 100 groups relative to amyloid beta group (P < 0.05) (Fig. 2a).
Discrimination ratio in novel object discrimination paradigm (a), alternation behavior in Y maze task (b), initial (IL) and step-through (STL) latencies in single-trial passive avoidance test (c), and working and reference memory errors in radial arm maze (d). Values are means ± SEM. n = 10–12 for each group. *P < 0.05, **P < 0.01 (versus sham); #P < 0.05, ##P < 0.01 (versus amyloid beta)
Alternation behavior in Y maze task
Figure 2b illustrates the performance of rats in the Y maze task, which assesses spatial recognition memory. In this regard, alternation score was significantly different between the groups (P < 0.005). The alternation score was significantly lower in ellagic acid untreated and treated amyloid beta groups as compared to the sham group (P < 0.01 for amyloid beta and amyloid beta+ellagic acid 10 groups and P < 0.05 for the other two groups). Additionally, the score was significantly higher for amyloid beta+ellagic acid 100 group relative to amyloid beta group (P < 0.05). To exclude compounding effect of locomotor activity on the performance of rats in memory evaluation tasks, we considered total number of arms entered by rats as locomotor index. In this regard, there were no significant differences among the groups (data not shown).
Passive avoidance test
Figure 2c shows the conductance of animals in the passive avoidance task as reported by IL and STL. Regarding IL, no significant difference was found out between the groups. With respect to STL, there exists a significant difference between the groups (P < 0.005). In this regard, both amyloid beta and amyloid beta+ellagic acid 10 groups showed a significant impairment of retention and recall relative to sham group (P < 0.01). Moreover, amyloid beta+ellagic acid 50 and amyloid beta+ellagic acid 100 groups showed a significant improvement of STL as compared to amyloid beta group (P < 0.05 and P < 0.01, respectively).
Radial arm maze task
Figure 2d illustrates the performance of rats in radial arm maze as a valid indicator of spatial memory. In this regard, working and reference memory errors were significantly higher in amyloid beta and amyloid beta+ellagic acid 10 groups as compared to sham group (P < 0.01). In addition, amyloid beta+ellagic acid 100 group had a significantly lower level of these errors (P < 0.01) in comparison with amyloid beta group.
Hippocampal oxidative stress
Amyloid beta group exhibited a significantly higher level of MDA (Fig. 3a) as a reliable marker of lipid peroxidation (P < 0.01) and a significant reduction of catalase activity (Fig. 3b) (P < 0.01) and glutathione (Fig. 3c) (P < 0.05) with no significant change of nitrite (Fig. 3d) as compared to sham group. Furthermore, pretreatment of amyloid beta group with ellagic acid at doses of 50 and 100 mg/kg significantly improved MDA (P < 0.05) and GSH (P < 0.05) and such improvement for catalase activity was observed only at a dose of 100 mg/kg. Additionally, ellagic acid-pretreated amyloid beta groups did not show a significant change of nitrite versus amyloid beta group.
Hippocampal NF-κB, Nrf2, and TLR4
Expression level of hippocampal NF-κB (Fig. 4a) (P < 0.005) and TLR4 (Fig. 4c) (P < 0.01) significantly increased, and nuclear/cytoplasmic ratio for Nrf2 (Fig. 4b) (P < 0.05) significantly decreased in amyloid beta group relative to sham group (P < 0.005). Treatment of amyloid beta group with ellagic acid at a dose of 100 mg/kg significantly improved NF-κB (P < 0.05), nuclear/cytoplasmic ratio for Nrf2 (P < 0.05), and TLR4 (P < 0.05) as compared to amyloid beta group. Additionally, ellagic acid treatment of amyloid beta group at a dose of 50 mg/kg was capable to significantly restore only NF-κB and nuclear/cytoplasmic ratio for Nrf2 (P < 0.05).
Hippocampal AChE and BChE activity
AChE (Fig. 5a) and BChE (Fig. 5b) activity was significantly greater in amyloid beta group (P < 0.01 and P < 0.05, respectively). In addition, amyloid beta+ellagic acid 50 and amyloid beta+ellagic acid 100 groups had a significantly lower level of AChE activity versus amyloid beta group (P < 0.05) and ellagic acid at none of the used doses had no significant effect on BChE activity.
Histochemical findings in Nissl staining
In this study, the number of neurons per unit area in the CA1 area of hippocampus was counted and compared among the groups (Fig. 6). Our results showed that amyloid beta and amyloid beta+ellagic acid 100 groups had a significant reduction of CA1 neurons (P < 0.01 and P < 0.05, respectively) versus sham group and ellagic acid pretreatment of amyloid beta group at both doses of 50 and 100 mg/kg significantly prevented this reduction as compared to Aβ group (P < 0.05). These data clearly indicate that ellagic acid at higher doses could protect the hippocampal neurons against Aβ neurotoxicity.
Discussion
This study was undertaken to explore the mechanisms involved in protective effect of ellagic acid on learning and memory disturbances induced by intrahippocampal amyloid beta microinjection as a reliable model of AD in rodents. The findings of this study showed that ellagic acid significantly and dose-dependently improves the performance of Aβ-injected rats in novel object discrimination, Y maze, passive avoidance, and radial arm maze tasks through protection of hippocampal CA1 pyramidal neurons and appropriate modulation of oxidative stress, AChE activity, and NF-κB/Nrf2/TLR4 signaling.
Our findings on learning and memory deficits in intrahippocampal amyloid beta-microinjected rats were consistent with earlier reports. In this regard, it has been shown that bilateral intracerebroventricular (Guo et al. 2013) or intraintrahippocampal (Liu et al. 2010) microinjection of Aβ25–35 leads to learning and memory deficits in rodents. Intracerebral injection of other forms of Aβ including Aβ1–40 and Aβ1–42 could also impair learning and memory (Ghofrani et al. 2015; Liu et al. 2015; Ma et al. 2015a; O'Neal-Moffitt et al. 2015; Rasoolijazi et al. 2007). These toxic effects of Aβ are considered to be mediated by amino acid residues 25–35 and for this reason Aβ25–35 is known as the principal neurotoxic domain (Guo et al. 2013; Mattson et al. 1992). Furthermore, we observed learning and memory deficits in all conducted behavioral tasks that were in agreement with previous reports using passive avoidance (Fedotova et al. 2016; Sohanaki et al. 2016b), Y maze (Zhi et al. 2014; Zhou et al. 2014), novel object discrimination (Bogachouk et al. 2016; Choi et al. 2014; Gomes et al. 2014), and radial arm maze (Bergin and Liu 2010; Limon et al. 2009; Patricio-Martinez et al. 2016) tasks following microinjection and/or infusion of Aβ25–35. In our study, administration of ellagic acid dose-dependently improved learning and spatial memory deficits following intrahippocampal Aβ25–35. Consistent with our findings, earlier reports have also documented the beneficial improving effect of ellagic acid in various models of cognitive deficits (Dolatshahi et al. 2015; Farbood et al. 2015; Mansouri et al. 2016).
In our study, 3 weeks after intrahippocampal injection of Aβ25–35, hippocampal level of MDA as a valid marker of lipid peroxidation increased and antioxidant defensive element including GSH content and catalase activity decreased that were in line with previous reports (Chen et al. 2014; Jiang et al. 2013; Jimenez-Aliaga et al. 2011; Sohanaki et al. 2016a). All of these alterations are indicative of enhanced oxidative stress in the hippocampus following Aβ25–35. Enhanced oxidative stress plays an important role in the early development of AD. Experimental evidence have suggested that a preceding and prolonged dormant period exists for gradual and incremental impact of oxidative damage, finally leading to development of clinical and pathological symptoms of AD including cognitive deficits (Bonda et al. 2010; Swomley and Butterfield 2015). MDA level elevates in neurotoxic conditions (Zhang et al. 2016) and catalase and GSH that are two important elements of antioxidant system responsible for removal of excess free radicals are depressed following induction of brain injury (Nirwane et al. 2016). Therefore, MDA, GSH, and catalase are considered as some of the key determinants of antioxidant and pro-oxidant condition. Ellagic acid in our study attenuated oxidative stress and improved antioxidant defense system that is consistent with earlier reports (Hassoun et al. 2004; Uzar et al. 2012). Nrf2 is one of the important transcription factors responsible for regulating induction of antioxidant genes (Vomhof-Dekrey and Picklo 2012). Under stressful and toxic conditions, Nrf2 translocates into the nucleus and after binding to DNA could induce transcription of genes related to antioxidant defensive system (Li and Kong 2009). In our study, hippocampal nuclear/cytoplasmic ratio for Nrf2 decreased in Aβ25–35-microinjected rats and ellagic acid pretreatment dose-dependently reversed this inappropriate alteration. In line with these results, ellagic acid has shown a defensive role against UV-B-induced oxidative stress through upregulation of Nrf2 signaling pathway in human dermal fibroblasts (Baek et al. 2016) and could augment nuclear translocation and transcriptional activation of Nrf2 (Hseu et al. 2012).
In this study, we also measured some inflammation-related markers including NF-κB and TLR4 in hippocampal lysate. In this respect, we found out that ellagic acid is capable to efficiently reduce the level of NF-κB, in this way mitigating neuroinflammation and reducing neuronal injury as a result of Aβ, thus protecting the brain against oxidative damage. Neuroinflammation is a pathological hallmark of neurodegenerative diseases like AD (Kim et al. 2014; Pimplikar 2014). This phenomenon is mainly due to activated microglia and astrocytes. Upon Aβ exposure, these cells through generation of a wide range of proinflammatory cytokines cause neuronal damage (Li et al. 2011). NF-κB plays a key role in Aβ-induced release of proinflammatory cytokines (Bales et al. 1998). In addition to microglial activation, complement system activation also occurs in the brain of patients with AD (Johnston et al. 2011). Immune system exerts modulatory effect on learning and memory under inflammation conditions (Yirmiya and Goshen 2011). The innate immune receptor TLR4 on microglial surface is upregulated following Aβ exposure that is associated with learning and memory deficit (Ding et al. 2011). The Aβ-induced upregulation of TLR4 may accelerate neuronal inflammation, which leads itself to neurodegeneration. NF-κB is itself one of the most important downstream molecules in TLR signaling pathway (Chen et al. 2009). A previous report has indicated that ellagic acid could exert protective effect against T cell-mediated hepatitis through TLR/NF-κB signaling pathways (Lee et al. 2014) that may have also occurred in our study.
In the present study, we noted increased activity of AChE and BChE in the hippocampus of amyloid beta group and ellagic acid reduced this inappropriate alteration of AChE. Overexpression of cholinesterases including AChE is a marker of cholinergic dysfunction in the brain (Mufson et al. 1991). Recent researches have shown that cholinergic abnormality plays a critical role in Aβ neurotoxicity (Wang et al. 2014). An earlier report has also shown that ellagic acid has a weak inhibitory effect on cholinesterases (Ferreres et al. 2013). Whether ellagic acid has directly and/or indirectly affected AChE in our model of AD, this issue needs further researches.
After administration of ellagic acid to rats (50 mg/kg), its plasma concentration attains a maximum at about 1/2 h and it is detectable in all tissue fluids including the liver, kidney, and brain (Yan et al. 2014). The half-life of ellagic acid in the body is 8.4 ± 1.8 h with its ability of plasma protein binding (Hamad et al. 2009). In addition, it is assumed that ellagic acid is capable to pass through the blood–brain barrier at small quantity (Teel 1987); however, there are still no definitive documents to confirm this. In this respect, ellagic acid has been detected in the rat brain after its administration (Yan et al. 2014) and this agent could be considered a putative factor in the neuroprotection associated with the intake of certain fruits and foods (Sánchez-González et al. 2015). In our study, a neuroprotective effect of ellagic acid was observed in amyloid beta group, as was shown by preservation of CA1 pyramidal neurons.
Conclusion
Ellagic acid pretreatment of intrahippocampal amyloid beta-microinjected rats could dose-dependently improve learning and memory deficits via neuronal protection and at molecular level through mitigation of oxidative stress and AChE activity and modulation of NF-κB/Nrf2/TLR4 signaling pathway. This may be put forward as an ancillary therapeutic agent for lowering the risk and progression of neurodegenerative diseases such as AD.
References
Ahshin-Majd S, Zamani S, Kiamari T, Kiasalari Z, Baluchnejadmojarad T, Roghani M (2016) Carnosine ameliorates cognitive deficits in streptozotocin-induced diabetic rats: possible involved mechanisms. Peptides 86:102–111. doi:10.1016/j.peptides.2016.10.008
Baek B, Lee SH, Kim K, Lim HW, Lim CJ (2016) Ellagic acid plays a protective role against UV-B-induced oxidative stress by up-regulating antioxidant components in human dermal fibroblasts. Korean J Physiol Pharmacol 20:269–277. doi:10.4196/kjpp.2016.20.3.269
Bales KR, Du Y, Dodel RC, Yan GM, Hamilton-Byrd E, Paul SM (1998) The NF-kappaB/Rel family of proteins mediates Abeta-induced neurotoxicity and glial activation. Brain Res Mol Brain Res 57:63–72
Baluchnejadmojarad T, Roghani M (2012) Chronic oral epigallocatechin-gallate alleviates streptozotocin-induced diabetic neuropathic hyperalgesia in rat: involvement of oxidative stress. Iran J Pharm Res 11:1243–1253
Baluchnejadmojarad T, Kiasalari Z, Afshin-Majd S, Ghasemi Z, Roghani M (2017) S-allyl cysteine ameliorates cognitive deficits in streptozotocin-diabetic rats via suppression of oxidative stress, inflammation, and acetylcholinesterase. Eur J Pharmacol 794:69–76. doi:10.1016/j.ejphar.2016.11.033
Bergin DH, Liu P (2010) Agmatine protects against beta-amyloid25-35-induced memory impairments in the rat. Neuroscience 169:794–811. doi:10.1016/j.neuroscience.2010.05.004
Bogachouk AP, Storozheva ZI, Solovjeva OA, Sherstnev VV, Zolotarev YA, Azev VN, Rodionov IL, Surina EA, Lipkin VM (2016) Comparative study of the neuroprotective and nootropic activities of the carboxylate and amide forms of the HLDF-6 peptide in animal models of Alzheimer's disease. J Psychopharmacol 30:78–92. doi:10.1177/0269881115616393
Bonda DJ, Wang X, Perry G, Nunomura A, Tabaton M, Zhu X, Smith MA (2010) Oxidative stress in Alzheimer disease: a possibility for prevention. Neuropharmacology 59:290–294. doi:10.1016/j.neuropharm.2010.04.005
Bradford MM (1976) A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem 72:248–254
Capurro V, Busquet P, Lopes JP, Bertorelli R, Tarozzo G, Bolognesi ML, Piomelli D, Reggiani A, Cavalli A (2013) Pharmacological characterization of memoquin, a multi-target compound for the treatment of Alzheimer's disease. PLoS One 8:e56870. doi:10.1371/journal.pone.0056870
Chen G, Zhang S, Shi J, Ai J, Qi M, Hang C (2009) Simvastatin reduces secondary brain injury caused by cortical contusion in rats: possible involvement of TLR4/NF-kappaB pathway. Exp Neurol 216:398–406. doi:10.1016/j.expneurol.2008.12.019
Chen DL, Zhang P, Lin L, Zhang HM, Deng SD, Wu ZQ, Ou S, Liu SH, Wang JY (2014) Protective effects of bajijiasu in a rat model of Abeta(2)(5)(-)(3)(5)-induced neurotoxicity. J Ethnopharmacol 154:206–217. doi:10.1016/j.jep.2014.04.004
Choi YY, Maeda T, Fujii H, Yokozawa T, Kim HY, Cho EJ, Shibamoto T (2014) Oligonol improves memory and cognition under an amyloid beta(25-35)-induced Alzheimer's mouse model. Nutr Res 34:595–603. doi:10.1016/j.nutres.2014.06.008
Cioanca O, Hritcu L, Mihasan M, Hancianu M (2013) Cognitive-enhancing and antioxidant activities of inhaled coriander volatile oil in amyloid beta(1-42) rat model of Alzheimer's disease. Physiol Behav 120:193–202. doi:10.1016/j.physbeh.2013.08.006
Claiborne A (1985) Catalase activity. In: Greenwald RA (ed). CRC handbook of methods for oxygen radical research. Boca Raton, FL: CRC. 283–284
Daulatzai MA (2010) Early stages of pathogenesis in memory impairment during normal senescence and Alzheimer's disease. J Alzheimers Dis 20:355–367. doi:10.3233/jad-2010-1374
Ding BJ, Ma WW, He LL, Zhou X, Yuan LH, Yu HL, Feng JF, Xiao R (2011) Soybean isoflavone alleviates beta-amyloid 1-42 induced inflammatory response to improve learning and memory ability by down regulation of Toll-like receptor 4 expression and nuclear factor-kappaB activity in rats. Int J Dev Neurosci 29:537–542. doi:10.1016/j.ijdevneu.2011.04.002
Dolatshahi M, Farbood Y, Sarkaki A, Mansouri SM, Khodadadi A (2015) Ellagic acid improves hyperalgesia and cognitive deficiency in 6-hydroxidopamine induced rat model of Parkinson's disease. Iran J Basic Med Sci 18:38–46
Ellman GL (1959) Tissue sulfhydryl groups. Arch Biochem Biophys 82:70–77
Farbood Y, Sarkaki A, Dianat M, Khodadadi A, Haddad MK, Mashhadizadeh S (2015) Ellagic acid prevents cognitive and hippocampal long-term potentiation deficits and brain inflammation in rat with traumatic brain injury. Life Sci 124:120–127. doi:10.1016/j.lfs.2015.01.013
Fedotova J, Soultanov V, Nikitina T, Roschin V, Ordyan N, Hritcu L (2016) Cognitive-enhancing activities of the polyprenol preparation Ropren(R) in gonadectomized beta-amyloid (25-35) rat model of Alzheimer's disease. Physiol Behav 157:55–62. doi:10.1016/j.physbeh.2016.01.035
Ferreres F, Grosso C, Gil-Izquierdo A, Valentao P, Andrade PB (2013) Ellagic acid and derivatives from Cochlospermum angolensis Welw. extracts: HPLC-DAD-ESI/MS(n) profiling, quantification and in vitro anti-depressant, anti-cholinesterase and anti-oxidant activities. Phytochem Anal 24:534–540. doi:10.1002/pca.2429
Galasko D, Montine TJ (2010) Biomarkers of oxidative damage and inflammation in Alzheimer's disease. Biomark Med 4:27–36. doi:10.2217/bmm.09.89
Ghofrani S, Joghataei MT, Mohseni S, Baluchnejadmojarad T, Bagheri M, Khamse S, Roghani M (2015) Naringenin improves learning and memory in an Alzheimer's disease rat model: insights into the underlying mechanisms. Eur J Pharmacol 764:195–201. doi:10.1016/j.ejphar.2015.07.001
Golde TE (2016) Overcoming translational barriers impeding development of Alzheimer's disease modifying therapies. J Neurochem 139:224–236. doi:10.1111/jnc.13583
Gomes GM, Dalmolin GD, Bar J, Karpova A, Mello CF, Kreutz MR, Rubin MA (2014) Inhibition of the polyamine system counteracts beta-amyloid peptide-induced memory impairment in mice: involvement of extrasynaptic NMDA receptors. PLoS One 9:e99184. doi:10.1371/journal.pone.0099184
Guo LL, Guan ZZ, Huang Y, Wang YL, Shi JS (2013) The neurotoxicity of beta-amyloid peptide toward rat brain is associated with enhanced oxidative stress, inflammation and apoptosis, all of which can be attenuated by scutellarin. Exp Toxicol Pathol 65:579–584. doi:10.1016/j.etp.2012.05.003
Hamad A-WR, Al-Momani WM, Janakat S, Oran SA (2009) Bioavailability of ellagic acid after single dose administration using HPLC. Pak J Nutr 8:1661–1664
Hassoun EA, Vodhanel J, Abushaban A (2004) The modulatory effects of ellagic acid and vitamin E succinate on TCDD-induced oxidative stress in different brain regions of rats after subchronic exposure. J Biochem Mol Toxicol 18:196–203. doi:10.1002/jbt.20030
Hritcu L, Cioanca O, Hancianu M (2012) Effects of lavender oil inhalation on improving scopolamine-induced spatial memory impairment in laboratory rats. Phytomedicine 19:529–534. doi:10.1016/j.phymed.2012.02.002
Hritcu L, Noumedem JA, Cioanca O, Hancianu M, Kuete V, Mihasan M (2014) Methanolic extract of Piper nigrum fruits improves memory impairment by decreasing brain oxidative stress in amyloid beta(1-42) rat model of Alzheimer's disease. Cell Mol Neurobiol 34:437–449. doi:10.1007/s10571-014-0028-y
Hseu YC, Chou CW, Senthil Kumar KJ, Fu KT, Wang HM, Hsu LS, Kuo YH, Wu CR, Chen SC, Yang HL (2012) Ellagic acid protects human keratinocyte (HaCaT) cells against UVA-induced oxidative stress and apoptosis through the upregulation of the HO-1 and Nrf-2 antioxidant genes. Food Chem Toxicol 50:1245–1255. doi:10.1016/j.fct.2012.02.020
Hwang JM, Cho JS, Kim TH, Lee YI (2010) Ellagic acid protects hepatocytes from damage by inhibiting mitochondrial production of reactive oxygen species. Biomed Pharmacother 64:264–270. doi:10.1016/j.biopha.2009.06.013
Isomae K, Morimoto S, Hasegawa H, Morita K, Kamei J (2003) Effects of T-82, a novel acetylcholinesterase inhibitor, on impaired learning and memory in passive avoidance task in rats. Eur J Pharmacol 465:97–103
Jiang LF, Liao HL, Huang HM, Zhou LX, Li L, Cheng SX, Du CZ (2013) Potential prevention and treatment of maifanite for Alzheimer's disease based on behavior test, oxidative stress assay, and trace element analysis in hippocampus of Abeta((2)(5)(-)(3)(5))-induced AD rats. Biol Trace Elem Res 152:50–56. doi:10.1007/s12011-012-9590-7
Jimenez-Aliaga K, Bermejo-Bescos P, Benedi J, Martin-Aragon S (2011) Quercetin and rutin exhibit antiamyloidogenic and fibril-disaggregating effects in vitro and potent antioxidant activity in APPswe cells. Life Sci 89:939–945. doi:10.1016/j.lfs.2011.09.023
Johnston H, Boutin H, Allan SM (2011) Assessing the contribution of inflammation in models of Alzheimer's disease. Biochem Soc Trans 39:886–890. doi:10.1042/bst0390886
Kabiraj P, Marin JE, Varela-Ramirez A, Zubia E, Narayan M (2014) Ellagic acid mitigates SNO-PDI induced aggregation of Parkinsonian biomarkers. ACS Chem Neurosci 5:1209–1220. doi:10.1021/cn500214k
Kiasalari Z, Khalili M, Shafiee S, Roghani M (2016) The effect of vitamin E on learning and memory deficits in intrahippocampal kainate-induced temporal lobe epilepsy in rats. Indian J Pharmacol 48:11–14. doi:10.4103/0253-7613.174394
Kim M, Kim SO, Lee M, Lee JH, Jung WS, Moon SK, Kim YS, Cho KH, Ko CN, Lee EH (2014) Tetramethylpyrazine, a natural alkaloid, attenuates pro-inflammatory mediators induced by amyloid beta and interferon-gamma in rat brain microglia. Eur J Pharmacol 740:504–511. doi:10.1016/j.ejphar.2014.06.037
Lau L-F, Brodney MA (2008) Therapeutic approaches for the treatment of Alzheimer's disease: an overview. In: Lau L-F, Brodney MA (eds) Alzheimer's disease. Springer Berlin, pp 1–24
Lee JH, Won JH, Choi JM, Cha HH, Jang YJ, Park S, Kim HG, Kim HC, Kim DK (2014) Protective effect of ellagic acid on concanavalin A-induced hepatitis via toll-like receptor and mitogen-activated protein kinase/nuclear factor kappaB signaling pathways. J Agric Food Chem 62:10110–10117. doi:10.1021/jf503188c
Li W, Kong AN (2009) Molecular mechanisms of Nrf2-mediated antioxidant response. Mol Carcinog 48:91–104. doi:10.1002/mc.20465
Li C, Zhao R, Gao K, Wei Z, Yin MY, Lau LT, Chui D, Yu AC (2011) Astrocytes: implications for neuroinflammatory pathogenesis of Alzheimer's disease. Curr Alzheimer Res 8:67–80
Limon ID, Mendieta L, Diaz A, Chamorro G, Espinosa B, Zenteno E, Guevara J (2009) Neuroprotective effect of alpha-asarone on spatial memory and nitric oxide levels in rats injected with amyloid-beta((25-35)). Neurosci Lett 453:98–103. doi:10.1016/j.neulet.2009.02.011
Liu RT, Zou LB, Fu JY, Lu QJ (2010) Effects of liquiritigenin treatment on the learning and memory deficits induced by amyloid beta-peptide (25-35) in rats. Behav Brain Res 210:24–31. doi:10.1016/j.bbr.2010.01.041
Liu H, Deng Y, Gao J, Liu Y, Li W, Shi J, Gong Q (2015) Sodium hydrosulfide attenuates beta-amyloid-induced cognitive deficits and neuroinflammation via modulation of MAPK/NF-kappaB pathway in rats. Curr Alzheimer Res 12:673–683
Ma Q, Ruan YY, Xu H, Shi XM, Wang ZX, Hu YL (2015a) Safflower yellow reduces lipid peroxidation, neuropathology, tau phosphorylation and ameliorates amyloid beta-induced impairment of learning and memory in rats. Biomed Pharmacother 76:153–164. doi:10.1016/j.biopha.2015.10.004
Ma W, Ding B, Yu H, Yuan L, Xi Y, Xiao R (2015b) Genistein alleviates beta-amyloid-induced inflammatory damage through regulating Toll-like receptor 4/nuclear factor kappaB. J Med Food 18:273–279. doi:10.1089/jmf.2014.3150
Mansouri MT, Farbood Y, Naghizadeh B, Shabani S, Mirshekar MA, Sarkaki A (2016) Beneficial effects of ellagic acid against animal models of scopolamine- and diazepam-induced cognitive impairments. Pharm Biol 54:1947–1953. doi:10.3109/13880209.2015.1137601
Mattson MP (2004) Pathways towards and away from Alzheimer's disease. Nature 430:631–639. doi:10.1038/nature02621
Mattson MP, Cheng B, Davis D, Bryant K, Lieberburg I, Rydel RE (1992) Beta-amyloid peptides destabilize calcium homeostasis and render human cortical neurons vulnerable to excitotoxicity. J Neurosci 12:376–389
Mufson EJ, Presley LN, Kordower JH (1991) Nerve growth factor receptor immunoreactivity within the nucleus basalis (Ch4) in Parkinson's disease: reduced cell numbers and co-localization with cholinergic neurons. Brain Res 539:19–30
Nasri S, Roghani M, Baluchnejadmojarad T, Balvardi M, Rabani T (2012) Chronic cyanidin-3-glucoside administration improves short-term spatial recognition memory but not passive avoidance learning and memory in streptozotocin-diabetic rats. Phytother Res 26:1205–1210. doi:10.1002/ptr.3702
Nirwane A, Sridhar V, Majumdar A (2016) Neurobehavioural changes and brain oxidative stress induced by acute exposure to GSM900 mobile phone radiations in zebrafish (Danio rerio). Toxicol Res 32:123–132. doi:10.5487/tr.2016.32.2.123
Olton DS, Samuelson RJ (1976) Remembrance of places passed: spatial memory in rats. J Exp Psychol Anim Behav Process 2:97–116
O'Neal-Moffitt G, Delic V, Bradshaw PC, Olcese J (2015) Prophylactic melatonin significantly reduces Alzheimer's neuropathology and associated cognitive deficits independent of antioxidant pathways in AbetaPP(swe)/PS1 mice. Mol Neurodegener 10:27. doi:10.1186/s13024-015-0027-6
Patricio-Martinez A, Mendieta L, Martinez I, Aguilera J, Limon ID (2016) The recombinant C-terminal fragment of tetanus toxin protects against cholinotoxicity by intraseptal injection of beta-amyloid peptide (25-35) in rats. Neuroscience 315:18–30. doi:10.1016/j.neuroscience.2015.11.066
Paxinos G, Watson C (1986) The rat brain in stereotaxic coordinates, 2nd edn. Academic Press, New York
Pimplikar SW (2014) Neuroinflammation in Alzheimer's disease: from pathogenesis to a therapeutic target. J Clin Immunol 34(Suppl 1):S64–S69. doi:10.1007/s10875-014-0032-5
Priyadarsini KI, Khopde SM, Kumar SS, Mohan H (2002) Free radical studies of ellagic acid, a natural phenolic antioxidant. J Agric Food Chem 50:2200–2206
Rasoolijazi H, Joghataie MT, Roghani M, Nobakht M (2007) The beneficial effect of (-)-epigallocatechin-3-gallate in an experimental model of Alzheimer's disease in rat: a behavioral analysis. Iran Biomed J 11:237–243
Roghani M, Joghataie MT, Jalili MR, Baluchnejadmojarad T (2006) Time course of changes in passive avoidance and y-maze performance in male diabetic rats. Iran Biomed J 10:99–104
Sánchez-González C, Ciudad C, Noé V, Izquierdo-Pulido M (2015) Health benefits of walnut polyphenols: an exploration beyond their lipid profile. Crit Rev Food Sci Nutr:00–00
Sedlak J, Lindsay RH (1968) Estimation of total, protein-bound, and nonprotein sulfhydryl groups in tissue with Ellman's reagent. Anal Biochem 25:192–205
Sohanaki H, Baluchnejadmojarad T, Nikbakht F, Roghani M (2016a) Pelargonidin improves memory deficit in amyloid beta25-35 rat model of Alzheimer's disease by inhibition of glial activation, cholinesterase, and oxidative stress. Biomed Pharmacother 83:85–91. doi:10.1016/j.biopha.2016.06.021
Sohanaki H, Baluchnejadmojarad T, Nikbakht F, Roghani M (2016b) Pelargonidin improves passive avoidance task performance in a rat amyloid beta25-35 model of Alzheimer's disease via estrogen receptor independent pathways. Acta Med Iran 54:245–250
Stuart SA, Robertson JD, Marrion NV, Robinson ES (2013) Chronic pravastatin but not atorvastatin treatment impairs cognitive function in two rodent models of learning and memory. PLoS One 8:e75467. doi:10.1371/journal.pone.0075467
Swomley AM, Butterfield DA (2015) Oxidative stress in Alzheimer disease and mild cognitive impairment: evidence from human data provided by redox proteomics. Arch Toxicol 89:1669–1680. doi:10.1007/s00204-015-1556-z
Teel RW (1987) Distribution and metabolism of ellagic acid in the mouse following intraperitoneal administration. Cancer Lett 34:165–171
Uzar E, Alp H, Cevik MU, Firat U, Evliyaoglu O, Tufek A, Altun Y (2012) Ellagic acid attenuates oxidative stress on brain and sciatic nerve and improves histopathology of brain in streptozotocin-induced diabetic rats. Neurol Sci 33:567–574. doi:10.1007/s10072-011-0775-1
Vomhof-Dekrey EE, Picklo MJ Sr (2012) The Nrf2-antioxidant response element pathway: a target for regulating energy metabolism. J Nutr Biochem 23:1201–1206. doi:10.1016/j.jnutbio.2012.03.005
Wang H, Yu Y, Chen W, Cui Y, Luo T, Ma J, Jiang XC, Qin S (2014) PLTP deficiency impairs learning and memory capabilities partially due to alteration of amyloid-beta metabolism in old mice. J Alzheimers Dis 39:79–88. doi:10.3233/jad-130812
Yan L, Yin P, Ma C, Liu Y (2014) Method development and validation for pharmacokinetic and tissue distributions of ellagic acid using ultrahigh performance liquid chromatography-tandem mass spectrometry (UPLC-MS/MS). Molecules 19:18923–18935. doi:10.3390/molecules191118923
Yang Y, Jiang S, Yan J, Li Y, Xin Z, Lin Y, Qu Y (2015) An overview of the molecular mechanisms and novel roles of Nrf2 in neurodegenerative disorders. Cytokine Growth Factor Rev 26:47–57. doi:10.1016/j.cytogfr.2014.09.002
Yirmiya R, Goshen I (2011) Immune modulation of learning, memory, neural plasticity and neurogenesis. Brain Behav Immun 25:181–213. doi:10.1016/j.bbi.2010.10.015
Zarezadeh M, Baluchnejadmojarad T, Kiasalari Z, Afshin-Majd S, Roghani M (2017) Garlic active constituent s-allyl cysteine protects against lipopolysaccharide-induced cognitive deficits in the rat: possible involved mechanisms. Eur J Pharmacol 795:13–21. doi:10.1016/j.ejphar.2016.11.051
Zhang Z, Hou L, Li X, Ju C, Zhang J, Li X, Wang X, Liu C, Lv Y, Wang Y (2016) Neuroprotection of inositol hexaphosphate and changes of mitochondrion mediated apoptotic pathway and alpha-synuclein aggregation in 6-OHDA induced parkinsons disease cell model. Brain Res 1633:87–95. doi:10.1016/j.brainres.2015.12.035
Zhi WH, Zeng YY, Lu ZH, Qu WJ, Chen WX, Chen L, Chen L (2014) Simvastatin exerts antiamnesic effect in Abeta25-35-injected mice. CNS Neurosci Ther 20:218–226. doi:10.1111/cns.12190
Zhou L, Lu Z, Li L, Chen L, Qi J, Chen L (2014) Pro-neurogenesis and anti-dementia properties of tetradecyl 2,3-dihydroxybenzoate through TrkA receptor-mediated signalling pathways. Int J Neuropsychopharmacol 17:1847–1861. doi:10.1017/s1461145714000558
Acknowledgements
This work was the result of a M.Sc. thesis project approved and financially supported by a grant from Research Council of Shahed University (no. 1393-D-P; Tehran, Iran) in 2014.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there are no conflicts of interest for this research project.
Rights and permissions
About this article
Cite this article
Kiasalari, Z., Heydarifard, R., Khalili, M. et al. Ellagic acid ameliorates learning and memory deficits in a rat model of Alzheimer’s disease: an exploration of underlying mechanisms. Psychopharmacology 234, 1841–1852 (2017). https://doi.org/10.1007/s00213-017-4589-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00213-017-4589-6