Abstract
Summary
This study evaluates the efficacy of low doses of pamidronate after renal transplantation to prevent bone loss in osteopenic patients. Results show that pamidronate is safe and significantly reduced spinal bone loss when administered immediately after renal transplantation.
Introduction
The purpose of this work is to evaluate the efficacy of two intravenous infusions of pamidronate in the immediate post-transplant period in a renal transplant (RT) population.
Methods
In this 12-month, randomized, double-blind, multicenter trial, 39 kidney recipients with diagnosed osteopenia received two doses of 30 mg of disodium pamidronate (n = 24) or placebo (n = 15), at surgery and 3 months post-RT. All patients received calcium and vitamin D. Bone density of the lumbar spine and total femur was measured by dual-energy X-ray absorptiometry (DXA) and X-rays were performed at RT, 6 and 12 months post-RT. Biochemical and hormonal determinations were performed before and after treatment.
Results
Pamidronate significantly reduced spinal bone loss, but no significant benefit was found for the incidence of fractures. Elevated baseline intact parathyroid hormone (iPTH) and bone remodeling markers returned to normal levels 3 months post-RT. However, normal procollagen type I N propeptide (PINP) concentrations were only maintained in the pamidronate group. After RT, a comparable graft function was observed in both groups according to creatinine values, 25-hydroxyvitamin-D (25-OH-D) levels were improved, and serum calcium levels normalized after a transient fall during the first 3 months.
Conclusion
A low dose of pamidronate prevents bone loss in osteopenic patients when administered immediately after RT.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Post-transplantation bone disease is a major clinical problem, especially in kidney transplant patients. Besides therapy with corticosteroids, which is a major etiological factor for osteoporosis [1], the particularly high risk for kidney recipients of developing bone abnormalities is associated with underlying bone osteodystrophy. Secondary hyperparathyroidism induced by hyperphosphatemia or vitamin D deficiency is common in chronic kidney disease, often leading to significant osteopenia and abnormal mineral metabolism.
Several studies have demonstrated that both active metabolites of vitamin D and bisphosphonates can prevent or reverse the accelerated bone loss that occurs through different mechanisms early after renal transplantation (RT) [2, 3]. Bisphosphonates bind to bone mineral directly, by inhibiting osteoclastic activity and reducing the number of osteoclasts [4], whereas calcitriol facilitates intestinal calcium absorption and suppresses parathyroid hormone secretion [5]. Although oral bisphosphonates have been associated with gastrointestinal side effects, intravenous bisphosphonates (such as pamidronate, ibandronate, and zoledronate) show a favorable clinical tolerance [5], and data from clinical trials suggest that bisphosphonates are a safer and more consistently effective antiresorptive therapy for post-transplantation osteoporosis than calcitriol [5, 6]. Moreover, the benefits of bisphosphonates in RT persist after cessation of therapy, since both bone mineral density (BMD) and bone turnover markers remain stable [2, 3]. Nevertheless, pharmacological approaches to osteoporosis in the RT population are still open to discussion.
We prospectively evaluated the efficacy of two intravenous infusions of pamidronate in the immediate post-transplant period to preserve BMD in a RT population.
Materials and methods
Study design and performance
This was a 12-month prospective, randomized, double-blind, placebo-controlled trial. The study was approved by the local clinical ethics committee of each participating center and all patients provided written informed consent.
Patient population
The patients eligible for the study were adults diagnosed with chronic renal failure in a dialysis program and recipients of a kidney graft with a BMD T score of −1 or less at transplantation at the lumbar spine.
Patients younger than 18 years, multiorgan transplantation recipients, or those with a previous allergy to bisphosphonates were excluded. Other exclusion criteria were treatment based on calcitonin, creatinine clearance of <30 ml/min, estrogens, selective modulators of estrogen receptors or other bisphosphonates, and therapy with corticosteroids, anticoagulants, or anti-epileptic drugs during the 3 months before RT.
Immunosuppression
All patients received oral cyclosporine, prednisone, and mycophenolate mofetil. Basiliximab or polyclonal antibody therapy were used as induction treatments. The dose of prednisone (or methylprednisolone) was 500 mg/day after unclamping, 1 mg/kg/day from day 1 post-RT with progressive reduction to 10 mg/day over 1 month, and 5 mg/day from the third month post-RT. The dose of cyclosporine could be modified in order to maintain serum levels of 100–200 ng/mL, and the dose of mycophenolate mofetil was adjusted independently for each patient and center.
Intervention
The patients (n = 39) were included in the study on days 5–7 post-RT and started receiving calcium at 1,000 mg/day and cholecalciferol at 800 IU/day. They underwent screening tests and were assigned to either the pamidronate group (n = 24) or placebo group (n = 15) according to a randomization number. Patients in the treatment group received a single 30-mg dose of pamidronate disodium between day 7 and day 10, and 3 months post-RT. Treatment with calcium and cholecalciferol was maintained for 1 year after RT.
Study endpoints
The primary endpoint of the study was the mean percent change from baseline in BMD at the lumbar spine and proximal femur, measured by absoptiometry, at months 6 and 12. Secondary endpoints included the incidence of skeletal fractures—assessed by radiological monitoring of symptomatic and asymptomatic vertebral fractures, and by the count of peripheral fractures—and the analysis of bone remodeling, determined through the measurement of biochemical markers of bone turnover.
Evaluation
Serum parameters included creatinine, calcium, phosphorus, magnesium and aluminum (in blood and urine), acid–base equilibrium, and markers of renal and hepatic function measured by standard procedures. The biochemical markers of bone remodeling were procollagen type I N propeptide (PINP) for bone formation and C-terminal cross-linking telopeptide of type I collagen (CTx) for bone resorption. The serum level of PINP was quantified by a radiometric method using a kit from Orion (Espoo, Finland) and serum β-CTx was determined by the Elecsys β-CrossLaps serum assay (Roche Diagnostics, Mannheim, Germany). Mineral metabolism was explored through determination of intact parathyroid hormone (iPTH), 25-hydroxyvitamin-D (25-OH-D) and 1,25-dihydroxyvitamin-D (1,25-OH2-D). Serum iPTH was measured by immunoradiometric assay (Allegro Intact PTH, Nichols Institute Diagnosis, San Juan de Capistrano, California, USA), 25-OH-D was determined by a competitive protein-binding assay (Nichols Institute Diagnosis, San Juan de Capistrano, California, USA), and 1,25-OH2-D was quantified by radioreceptor assay (Nichols Institute Diagnosis, San Juan de Capistrano, California, USA). Deficiency of vitamin 1,25-OH2-D and 25-OH-D was defined as values lower than 30 pg/mL and 20 ng/mL, respectively. Parameter evolution was analyzed according to the variations registered at each visit (at days 5–7, and 3, 6, and 12 months post-RT) in relation to post-RT values. Biochemical and hormonal determinations were performed before and after treatment.
The BMD at the lumbar spine (vertebrae L2–L4) and proximal femur was measured by dual-energy X-ray absorptiometry (DXA) at baseline and 6 and 12 months post-RT using Hologic 4500 (Hologic, Waltham, Massachusetts, USA), Lunar DPX Prodigy (Madison, Wisconsin, USA), or Norland (Norland Corp., Fort Atkinson, Wisconsin, USA) instruments. Osteoporosis was defined as a T score of −2.5 or less for the lumbar and/or femoral BMD (total femur) and osteopenia as a T score of between −1 and −2.5.
X-rays of the whole spine were obtained to assess vertebral fractures at RT, and 6 and 12 months after RT. These were evaluated using a semiquantitative approach by an independent observer. Vertebral fracture was defined as a reduction of 20% or more in the anterior, middle, or posterior height compared to the adjacent vertebral body.
Statistical analysis
Statistical analyses were conducted using SAS®, version 8.2, and statistical significance was set at 5% (P = 0.05). The chi-square test was used for categorical variables and the Mann–Whitney test was used to compare continuous variables. The evolution of BMD, bone remodeling markers, and biochemical parameters was analyzed using an analysis of variance for repeated determinations to detect within and between-group differences. Dropouts were not included in the analysis and missing values were not substituted. The association between clinical, biochemical, and hormone variables was tested using an analysis of covariance that included the study group as a covariate.
Results
Study population
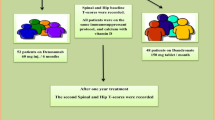
A total of 39 renal recipients were enrolled and randomized. The placebo and pamidronate groups were composed of 15 (39%) and 24 (61%) patients, respectively. Twenty-nine (74.4%) subjects completed the study and ten (25.6%) discontinued prematurely (Fig. 1). No significant differences in baseline characteristics were found between the study groups (Table 1).
Clinical evaluation and biochemical and hormonal parameters
While baseline elevated creatinine concentrations were expected due to renal failure, initial iPTH, phosphorus, 25-OH-D, and 1,25-OH2-D levels indicated secondary hyperparathyroidism, hyperphosphatemia, and hypovitaminosis D in both groups (Table 2).
The values of the monitored parameters at RT and 6 and 12 months post-RT are shown in Table 2. Although within-group differences between successive visits were statistically significant for some parameters, no differences were observed between the treatment groups.
Creatinine values revealed a comparable graft function in both groups (Fig. 2a). Serum calcium levels fell at RT, and were lower on days 5–7 post-RT than at baseline, although they recovered on days 7–10 and normalized at 3 months post-RT. Likewise, iPTH concentrations decreased considerably in both groups after RT, although they remained above normal levels throughout the study. Decreased baseline levels of 1,25-OH2-D and 25-OH-D gradually rose to normal during the study, so that at 12 months post-RT, 25-OH-D deficiency was present in four pamidronate (27%) and two placebo (29%) patients, and a further four and two subjects from each group, respectively, had a 1,25-OH2-D deficiency (33% in both cases). Finally, serum phosphorus decreased within the first 3 months post-RT before reaching normal values in both groups. No important changes were observed for the remaining parameters.
Outcome of biochemical parameters and bone mass during the follow-up period represented as a percent change from baseline. a Outcome of creatinine (median values). Creatinine variations were significant within each treatment group (P = 0.0001 at all time points except for days 5–7 and days 7–10 in the pamidronate group [P = 0.005 and P = 0.0007, respectively] and days 5–7, days 7–10, and month 3 [24 h post-infusion] in placebo patients [P = 0.04, P = 0.005, and P = 0.03, respectively]), but not between groups. b Outcome of PINP and CTx (mean values). PINP changes were significant within the pamidronate group (P = 0.02, P = 0.01, and P = 0.03 at respectively 3, 6, and 12 months post-RT). CTx variations were significant within both treatment groups (P = 0.0002, P = 0.0001, and P = 0.0001 for the pamidronate group, and P = 0.03, P = 0.02, and P = 0.03 for placebo patients at respectively 3, 6, and 12 months post-RT). Neither of these two parameters showed significant differences between groups. c Outcome of BMD at the lumbar spine (mean values). BMD change at 6 months was significant within the placebo group (P = 0.04). Comparison between treatment groups showed significant differences at 6 and 12 months (P < 0.05)
Bone remodeling
PINP and CTx were chosen as biochemical markers of bone formation and resorption, respectively. The outcome of these parameters is shown in Fig. 2b.
PINP levels, which normalized at the third month post-RT, remained stable in pamidronate patients (mean values at RT, 3, 6, and 12-months post-RT were 145, 76, 90, and 78 ng/mL, respectively, with significant differences from baseline observed at all visits), but recovered dramatically in placebo patients during the last 6 months (mean values at RT, 3, 6, and 12-months post-RT were 123, 82, 97, and 150 ng/mL, respectively, without significant differences from baseline). However, comparisons between treatment groups did not achieve statistical significance.
Conversely, a similar outcome was observed for CTx values in both groups. After a pronounced initial decrease, concentrations remained low from the third month post-RT (mean values at baseline, 3, 6, and 12 months post-RT were 2.19, 0.46, 0.55, and 0.50 ng/mL, respectively, in the pamidronate group, and 3.34, 0.71, 0.84, and 0.94 ng/mL in placebo patients). Both groups showed significant CTx reductions at all visits, with a trend of increase in the placebo group, but no significant differences were found between groups.
Bone densitometry and fractures
Measurements of BMD at the lumbar spine and proximal femur at RT, and 6 and 12 months post-RT are shown in Table 3 for both treatment groups.
Lumbar spine BMD remained stable in the pamidronate group, but fell in placebo patients which started recovering at the sixth month post-RT (Fig. 2c). BMD variations at 6 and 12 months differed significantly between treatment groups (P < 0.05), with a percent change from baseline of +1% in the pamidronate group and −6% in the placebo group at the end of the study. Although bone loss in the lumbar spine correlated significantly with a decrease in iPTH (P = 0.04), the treatment effect was maintained after adjusting for mean iPTH (adjusted percent change of +4.4% vs. −0.5%, in pamidronate and placebo patients, respectively; P = 0.01). No significant differences in the femoral neck or total femur BMD were observed between groups.
Episodes of vertebral pain were reported by one pamidronate patient at month 3 (5%) and two placebo patients, both at months 6 and 12 (18% and 20%, respectively). New vertebral fractures were not detected during the study, and only 1 subject from the pamidronate group reported a peripheral fracture at month 6 (9.1%). Therefore, differences in pain episodes and fractures were not significant between treatment groups. Immobilization periods were similar in number and length in the 2 groups.
Safety
There were no serious adverse events related to the study medication.
Rejection was observed in seven patients (18%), including three and four subjects from the placebo and pamidronate groups, respectively, without significant differences.
Discussion
Bone loss in kidney recipients is due to uncoupled bone resorption and formation. Factors contributing to both of these processes are more evident in the early post-transplantation period and include previous bone disease, immobilization periods, and immunosuppressive regimens containing corticosteroids and calcineurin inhibitors. Treatment with antiresorptive medications, such as bisphosphonates, targets several factors that contribute to bone loss in the RT population. Practice guidelines for renal transplantation recommend bisphosphonates for the prevention of bone injury in the early phase after RT in patients with an increased risk of fracture, whereas vitamin D and calcium are generally recommended in the absence of contraindications [7, 8].
In this study, we demonstrate that two intravenous infusions of pamidronate, one immediately and the other 3 months after RT, preserve BMD without side effects in the early post-transplantation period, when substantial bone loss has already occurred. Based in the results of previous studies with high doses of biphosphonates and our personal experience, we designed this trial with the aim to evaluate if it is possible to obtain such effect using only low doses avoiding the possibility of side effects, especially adynamic bone disease. Our results show a significant improvement in BMD at the lumbar spine; therefore, they are consistent with those of other studies that show the earlier recovery of BMD at the lumbar spine during the post-RT period [2, 3]. Lumbar vertebrae L2–L4 showed a gain in bone mass of 1% at 12 months in patients who received the two 30-mg intravenous pamidronate plus daily calcium and cholecalciferol, while in the placebo group BMD fell by 6%. The effect of the treatment, which was maintained after adjusting for iPTH, would explain the stabilization of spinal BMD in the treatment group. Although patients with higher bone loss in the early post-RT period are more vulnerable to bone fractures, in this series we did not find significant evidence, this could be explained because our study was not powered to detect fractures.
Baseline iPTH, PINP, CTx, phosphorus, 25-OH-D, and 1,25-OH2-D values revealed the occurrence of secondary hyperparathyroidism associated with high-turnover bone disease, hyperphosphatemia, and hypovitaminosis D in both groups. Elevated baseline levels of iPTH, CTx, and phosphorus, as well as low 1,25-OH2-D and 25-OH-D values normalized during the study and bone turnover decreased, although relatively high iPTH values persisted in both groups. The outcome of iPTH and the bone remodeling markers PINP and CTx followed the same pattern, which was characterized by an initial fall during the first 3 months in both groups, and a recovery starting at the sixth month post-RT only in the placebo group, although differences between groups were not significant.
The benefit of pamidronate in the prevention of bone loss early after RT, particularly in the lumbar spine, has been assessed in two 12-month studies. Fan et al. reported reduced bone loss in the lumbar spine and femoral neck, although only the latter persisted at 48 months [2]. Furthermore, Coco et al. reported that pamidronate preserved BMD at the lumbar spine even after treatment was discontinued, but no effect on the incidence of fractures was found [3]. A recent study by Walsh et al. using higher doses than in our series showed similar results but they also treated patients without evidence of osteopenia [9]. Pamidronate efficacy in the prevention of bone loss in the lumbar spine and femoral neck was also demonstrated in heart and lung recipients [6, 10], but not in liver recipients [11]. Similarly, the early application of ibandronate and zoledronate ameliorated bone loss in the lumbar spine and femoral neck over 1 year in renal recipients [12, 13], although short-term zoledronate therapy conferred no sustained benefit at 3 years post-RT [14].
Regarding fractures, most studies failed to correlate pamidronate with reduced fracture rates [9], except for two assays in heart and liver recipients [15, 16]. In fact, no individual intervention (bisphosphonates, vitamin D sterol, or calcitonin) has been associated with a reduction in the risk of fracture compared with placebo in kidney recipients [17].
In the present trial, intravenous administration of pamidronate was well tolerated without major adverse events. This might simplify therapy schedules, leading to better adherence and, subsequently, greater clinical efficacy. Since the 30-mg dose of pamidronate did not compromise renal function and was not associated with adverse effects, administration of 60 mg should be safe and is also recommended.
In conclusion, low doses of intravenous pamidronate disodium combined with a daily supplement of calcium and vitamin D during the early post-transplantation period is a safe and effective treatment for the prevention of spinal bone loss over 12 months in kidney recipients with diagnosed osteopenia that are going to receive steroid therapy.
References
Lukert BP, Raisz LG (1990) Corticosteroid-induced osteoporosis: pathogenesis and management. Ann Intern Med 112:352–364
Fan SL, Almond MK, Ball E, Evans K, Cunningham J (2000) Pamidronate therapy as prevention of bone loss following renal transplantation. Kidney Int 57:684–690
Coco M, Glicklich D, Faugere MC et al (2003) Prevention of bone loss in renal transplant recipients: a prospective, randomized trial of intravenous pamidronate. J Am Soc Nephrol 14:2669–2676
Rodan GA, Fleisch HA (1996) Bisphosphonates: mechanisms of action. J Clin Invest 97:2692–2696
Shane E, Addesso V, Namerow PB et al (2004) Alendronate versus calcitriol for the prevention of bone loss after cardiac transplantation. N Engl J Med 350:767–776
Bianda T, Linka A, Junga G et al (2000) Prevention of osteoporosis in heart transplant recipients: a comparison of calcitriol with calcitonin and pamidronate. Calcif Tissue Int 67:116–121
K/DOQI (2002) Clinical practice guidelines for chronic kidney disease evaluation, classification, and stratification. Am J Kidney Dis 39:S1–S266
European best practice guidelines for renal transplantation (2002) Section IV: long-term management of the transplant recipient. Nephrol Dial Transplant 17(Suppl 4):20–21
Walsh SB, Altmann P, Pattison J et al (2009) Effect of pamidronate on bone loss after kidney transplantation: a randomized trial. Am J Kidney Dis 53:856–865
Aris RM, Lester GE, Renner JB et al (2000) Efficacy of pamidronate for osteoporosis in patients with cystic fibrosis following lung transplantation. Am J Respir Crit Care Med 162:941–946
Ninkovik M, Skingle SJ, Bearcroft PW, Bishop N, Alexander GJ, Compston JE (2000) Incidence of vertebral fractures in the first three months after orthopic liver transplantation. Eur J Gastroenterol Hepatol 12:931–935
Grotz W, Nagel C, Poeschel D et al (2001) Effect of ibandronate on bone loss and renal function after kidney transplantation. J Am Soc Nephrol 12:1530–1537
Haas M, Leko-Mohr Z, Roschger P et al (2003) Zoledronic acid to prevent bone loss in the first 6 months after renal transplantation. Kidney Int 63:1130–1136
Schwartz C, Mitterbauer C, Heinze G, Woloszczuk W, Haas M, Oberbauer R (2004) Nonsustained effect of short-term bisphosphonate therapy on bone turnover three years after renal transplantation. Kidney Int 65:304–309
Shane E, Rodino MA, McMahon DJ et al (1998) Prevention of bone loss after heart transplantation with antiresorptive therapy: a pilot study. J Heart Lung Transplant 17:1089–1096
Reeves HL, Francis RM, Manas DM, Hudson M, Day CP (1998) Intravenous bisphosphonate prevents symptomatic osteoporosis vertebral collapse in patients after liver transplantation. Liver Transplant Surg 4:404–409
Palmer SC, McGregor DO, Strippoli GF (2007) Interventions for preventing bone disease in kidney transplant recipients. Cochrane Database Syst Rev 3:CD005015
Acknowledgments
The authors acknowledge the financial support of Novartis Transplantation and Immunology (Spain). We are also grateful to Infociencia Clinical Research S.L. for their assessment in the statistical analysis.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was registered in the Cochrane Renal Group ID number CRG100800151.
Rights and permissions
About this article
Cite this article
Torregrosa, JV., Fuster, D., Monegal, A. et al. Efficacy of low doses of pamidronate in osteopenic patients administered in the early post-renal transplant. Osteoporos Int 22, 281–287 (2011). https://doi.org/10.1007/s00198-010-1197-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-010-1197-2