Abstract
Introduction and hypothesis
The purpose of this study is to determine whether a Pilates exercise program and a pelvic floor muscle-training (PFMT) program could provide similar improvements in pelvic muscle strength.
Methods
Sixty-two women with little or no pelvic floor dysfunction were randomized to Pilates or PFMT. Each group had 24 biweekly 1-h sessions with either a physical therapist or Pilates instructor. Strength was measured via perineometry (cmH2O). Two questionnaires—pelvic floor distress inventory (PFDI-20) and pelvic floor impact questionnaire (PFIQ-7)—were also collected.
Results
At baseline, the Pilates and PFMT groups measured 14.9 ± 12.5 and 12.5 ± 10.4 cmH2O, respectively (p = 0.41). Both the Pilates and PFMT groups got stronger (6.2 ± 7.5 cmH2O, p = 0.0002 and 6.6 ± 7.4 cmH2O, p = 0.0002, respectively), with no difference between groups p = 0.85. PFIQ and PFDI scores improved from baseline but not between groups.
Conclusions
Further study is required to determine if Pilates can actually treat pelvic floor dysfunction.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Urinary incontinence, pelvic organ prolapse, and other manifestations of pelvic floor dysfunction are highly prevalent conditions among women [1, 2]. Women suffering from pelvic floor symptoms are often advised to “do their Kegel exercises” because virtually all such disorders may be prevented or treated through programs that improve pelvic muscle strength and coordination [3, 4].
Assuming a woman can learn to effectively exercise her pelvic floor muscles, she must then maintain her results by becoming a “lifelong Kegeler”, because—as with any exercise regimen—the intensity, frequency, and duration of pelvic floor muscle training (PFMT) will greatly influence clinical results. More simply put, if you don't use it, you lose it. Glazner et al. [5] reported long-term follow-up on a group of highly motivated women who had initially improved their post-partum incontinence symptoms via PFMT. Their initial symptomatic improvements did not persist—due in part to decreasing patient compliance with the PFMT program over time. Other authors have demonstrated similar discouraging long-term adherence to PFMT programs [6–8].
Given the obvious short-term benefits of PFMT, why are long-term adherence rates so poor? Sluijs et al. [9] showed that patients are more likely to demonstrate long-term compliance to exercise programs that cause the least disruption to their normal daily activities and include positive feedback. Perhaps the focused positive feedback (or “pay off”) recognized by patients following PFMT is not compelling enough to generate long-term adherence.
The popular exercise program, known as the “Pilates method” (named after founder, Joseph Pilates who developed these methods in the 1920s) consists of a series of low impact exercises believed to produce flexibility and strength for the entire body. Proponents of the Pilates exercise methods believe that they produce conditioning of the whole body and promote a “mind–body connection” [10]. Pilates instructors use verbal cues to teach these techniques which focus especially on “core” abdominal, lower back, and medial thigh muscles. Exercise repetitions rarely exceed ten, with resistance usually coming in the form of body weight and specially designed springs. Due to the fact that most of these exercises are performed in conjunction with a pelvic floor muscle contraction, many Pilates instructors believe that their methods can produce significant improvements in pelvic floor strength and that these improvements are very likely to persist over time [11]. If so, the Pilates methods might provide a new more compelling “full-body” alternative for the treatment and prevention of pelvic floor dysfunction. However, despite the increasing popularity of Pilates exercises, their specific effects on the female pelvic floor have not been studied.
The biologic rationale for PFMT programs has to do with improving patients' muscle strength and awareness. Therefore, the fundamental question when evaluating a Pilates program as an alternative method for PFMT should be: does the program actually result in improved pelvic floor muscle strength?
Therefore, our objective for this study was to compare the change in pelvic muscle strength achieved by women after completing either a standardized 12-week Pilates exercise program or a “traditional” 12-week pelvic muscle-training program.
Materials and methods
This study was approved by the Atlantic Health Human Studies Committee (study number R06-03-018) and was posted on the website www.clinicaltrials.gov (indicator number NCT00549458). It was a randomized controlled trial comparing a standardized physical therapy-based PFMT program to a standardized Pilates program in terms of improving pelvic floor muscle strength. In other words, we simply wanted to find out whether a Pilates exercise program could result in specific pelvic floor muscle strength improvement to the same degree as a traditional PFMT program.
Adult non-pregnant women were recruited for this study from the local community. Although some of the participants complained of lower urinary tract symptoms such as stress urinary incontinence, actual complaints of pelvic floor dysfunction were not required for participation in the study. Participants could not have prior experience with formal PFMT or Pilates. In other words, potential study participants were excluded if they had ever received formal instruction in PFMT by a healthcare provider or in Pilates techniques by a Pilates instructor. All patients underwent a screening physical exam including a pelvic exam. In an effort to optimize muscle strength assessments, no women with greater than stage 1 pelvic organ prolapse (using the pelvic organ prolapse quantification system [12]) were enrolled. All other inclusion and exclusion criteria are listed in Table 1.
A blocked random assignment technique (using blocks of six) was used to determine the allocation sequence, and sequentially numbered opaque sealed envelopes were used to conceal the group assignments. Randomization occurred immediately after enrollment. After randomization, baseline pelvic floor muscle strength (our main endpoint) was measured via a computerized vaginal pressure sensor (Pathway™ CTS 2000, The Prometheus Group, Dover, NH, USA). These measurements were obtained by a single clinical research nurse (JS). Three perineometry measurements were obtained pre-treatment and post-treatment for each participant. To do so, the perineometry probe was placed into the vagina with the center portion of the probe located 3–4 cm from the introitus. The sensor was set to zero at the start of each test. The study participants were asked to perform three maximum pelvic muscle contractions holding each for 10 s if possible. They paused at least 20 s between contractions, and they were asked to breathe normally during the measurements. Our clinical research nurse visually and manually determined that no Valsalva maneuvers or other increases in intra-abdominal pressure or contractions of abdominal musculature were contributing to the measured values. The average of the three peak pressure values made up the pre- and post-treatment scores.
Although most of the study group did not actually complain of pelvic floor dysfunction, pre- and post-treatment pelvic floor symptoms were assessed as secondary endpoints using two questionnaires—the pelvic floor distress inventory short form 20 (PFDI-20) and pelvic floor impact questionnaire short form 7 (PFIQ-7) [13]. The PFDI-20 has a total of 20 questions regarding pelvic floor symptoms within three sub-scales—pelvic organ prolapse, colorectal-anal, and urinary symptoms. The worst possible summary score for the PDFI-20 is 300 (indicating worst possible symptoms). The PFIQ-7 is a companion questionnaire to the PFDI-20. It measures the extent to which pelvic floor symptoms affect the quality of life, and the worst possible summary score is also 300.
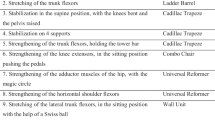
Both the PFMT and Pilates exercise programs consisted of 24 1-h sessions (i.e., twice weekly for 12 weeks). All sessions were conducted in a one-on-one fashion with either a physical therapist trained in pelvic floor rehabilitation or a certified Pilates instructor. Only two different physical therapists participated in the program (GGW and DD), and each followed the same structured protocol (Table 2) which was based on peer-reviewed regimens for PFMT [14–17]. There were four different certified Pilates instructors involved in that arm of the study, and they too followed a structured protocol (Table 3). Using verbal cues, the Pilates instructors taught full-body exercises that were also designed to emphasize the “core muscles”, especially the pelvic floor. These Pilates instructors did not follow a particular script when describing how to perform a pelvic floor contraction. The physical therapists utilized computerized biofeedback, vaginal manipulation, neuromuscular re-education, and manual therapy to focusing strictly on the pelvic floor. Each participant had to complete at least 20 of 24 possible sessions to be considered a “successful” participant. All Pilates and PFMT sessions were provided at no cost to the participants—who were also paid up to $75 for completion of the study protocol.
Baseline group characteristics and outcome measures were compared using X2 or t tests as appropriate. Based on previous measurements of pelvic floor muscle strength via perineometry [18], a prospective sample size calculation called for 24 patients in each group to have 80% power for detecting a 25% difference in muscle strength between groups.
Results
Sixty-two women were enrolled. All of these women were able to perform a pelvic muscle contraction correctly, and no screened patients were excluded on the basis of not being able to contract their pelvic floor. There were 30 and 32 participants in the Pilates and PFMT groups, respectively. There was a differential dropout rate between groups—leaving 28 and 24 participants in the final Pilates and PFMT groups, respectively. Details of enrollment and fulfillment of the study protocol are displayed in Fig. 1. There were no demographic differences between the original randomized groups and the final subsets of those groups who actually completed the study (Tables 4 and 5). The two participants who left the Pilates arm of the trial reported doing so reluctantly due to circumstances out of their control. One injured her wrist rendering her unable to continue the program, and the other had a very sick child and could no longer afford the time for study participation. In contrast, seven of the eight participants who dropped out of the PMFT arm reported doing so because they found the treatments unpleasant in some way.
Mean pre-treatment muscle strength for the Pilates and PFMT groups were 14.9 ± 12.5 and 12.5 ± 10.4 cmH2O, respectively (p = 0.41). Both groups demonstrated improved strength at the end of the study. Mean improvement in the Pilates group was 6.2 ± 7.5 cmH2O (p = 0.0002) and in the PFMT group was 6.6 ± 7.4 cmH2O (p = 0.0002). When compared between groups, these muscle strength improvements were not significantly different (p = 0.85).
Mean pre-treatment PFDI-20 scores for the Pilates and PFMT groups were 59.2 ± 42.3 and 51.9 ± 37.8, respectively (p = 0.48). After treatment, PFDI scores improved by 28.4 ± 36 points (48%) in the Pilates group (p = 0.0004) and by 27.4 ± 24.7 points (53%) in the PFMT group (p < 0.0001). When compared to each other, these improvements in PFDI-20 scores were not significantly different between groups (p = 0.86).
Mean pre-treatment PFIQ-7 scores for the Pilates and PFMT groups were 25 ± 29.9 and 22.4 ± 31.1, respectively (p = 0.74). After treatment, PFIQ scores improved by 10.9 ± 28 points (44%) in the Pilates group (p = 0.049) and by 12.3 ± 30.9 points (55%) in the PFMT group (p = 0.043). When compared to each other, these improvements in PFIQ-7 scores were not significantly different between groups (p = 0.91).
Discussion
PMFT is a widely used treatment for pelvic floor disorders such as stress urinary incontinence [1]. Two recent Cochrane systematic reviews described PFMT as the recommended first-line conservative prevention and management program for women with stress, urge, or mixed urinary incontinence as well as fecal incontinence [19, 20]. There are two hypotheses regarding the mechanisms by which PFMT may provide prevention and treatment of stress urinary incontinence and pelvic organ prolapse [4]. These two proposed mechanisms are (1) that women develop a “knack” for consciously contracting the pelvic floor muscles before and during increases in abdominal pressure, and (2) that strengthening these muscles can build up the structural support to the pelvic floor. However, some authors have called for a critical reappraisal of PFMT—given the relative dearth of evidence to support the long-term benefits of focused PFMT programs [21].
Our randomized clinical trial clearly demonstrated the feasibility of a Pilates exercise program for strengthening the pelvic floor muscles. This being a feasibility study—with change in muscle strength being the main endpoint—we did not focus on whether patients were actually experiencing pelvic floor symptoms when setting up the inclusion/exclusion criteria. Also, it is important to note that our findings are only relevant to those women who can “find” their pelvic floor muscles. Women who cannot correctly flex these muscles would not be likely to benefit from the Pilates protocol to the same extent as our study participants.
Although pelvic floor dysfunction was not required for participation in this study, we also showed a 44–55% improvement in both groups with regard to PFDI-20 and PFIQ-7 scores. Of course, the clinical significance of these subjective findings among a group of largely asymptomatic women is unclear. Nevertheless, these improved scores are intriguing given the reported “minimal clinically important difference” of approximately 15% for these questionnaires [13].
Our results are complementary to those from a recent non-randomized longitudinal study by Brubaker et al. [22] in which “pelvic fitness” classes showed promise for improving symptoms of pelvic floor dysfunction. These classes combined a total-body fitness program with education about pelvic anatomy and bladder health. Although it was assumed that increased pelvic floor muscle strength played a major role in improving these study participants' symptoms, actual pelvic floor muscle strength was not measured. Nevertheless, Brubaker et al. illustrated a very important idea—that a “non-medicalized” program incorporating pelvic muscle exercises into an appealing “gym-based” regimen can improve pelvic floor symptoms in women. Their exercise program was very similar to the Pilates program in our study.
Both groups of women who actually completed the PFMT or Pilates protocols expressed gratitude and enthusiasm for their respective treatments, yet a larger number of enrollees dropped out of the PFMT study arm. There were several characteristics of the two exercise programs that could have been responsible for the differential dropout rates between groups. Perhaps the whole experience surrounding participation in the Pilates protocol was generally more acceptable than that of the PFMT protocol. The PFMT techniques employed by the physical therapists in our study involved “invasive” techniques using vaginal manipulation—obviously requiring that the participants undress. In contrast, The Pilates program was conducted in a non-medical facility (the Bodies in Balance Pilates studio, Madison, NJ, USA) where the participants remained fully clothed. One other important difference between the two exercise regimens had to do with perceived “extra pelvic” benefits. While the PMFT program was designed to focus almost exclusively on the levator ani muscles, the Pilates program was designed to provide greater strength, flexibility, and posture for the whole body.
Another important difference between these two programs involved our primary endpoint—perineometry. The PFMT participants essentially “practiced” perineometry during each exercise session, but the Pilates participants performed that measurement only at the pre- and post-treatment data collection sessions. Thus, even given this theoretic advantage, the PFMT group did not demonstrate better post-treatment perineometry scores.
Several important limitations of this study must be considered. It is possible that our PFMT regimen was not optimal for increasing pelvic floor muscle strength. PFMT teaching recommendations tend to evolve and change over time, so our PMFT program could possibly be considered “out of date” by some providers.
Although we excluded women with prior formal training in either Pilates or PFMT, it was possible that women could have been informally exposed to one or both of these exercise methods.
Although we did meet our desired sample size of 24 participants per group (and therefore achieved our desired power), this was a relatively small study. Larger randomized trials designed to determine whether a Pilates program can actually improve significant pelvic floor dysfunction would be required before we could recommend the widespread use of this protocol for that purpose. Nevertheless, our results clearly indicate that such randomized trials are warranted.
Another possible criticism of this study could be the lack of a sham group, but we considered it impossible to feasibly create a believable sham treatment protocol.
One might also argue that we should have performed an “intention-to-treat” analysis in order to include those women who did not complete the study. The intention-to-treat principle dictates that all patients who had been randomly allocated to treatments under the auspices of the study should be included in the final data analysis as a part of their original group assignment. This principle can only be applied when some sort of outcome measure exists for all study participants [23]. Our study design did not offer any way to perform such an analysis, because we collected only one set of outcome measures at the end of the 12-week exercise period. Therefore, women who dropped out of the study did so before submitting to any collection of post-treatment data. Nevertheless, our randomization scheme seems to have worked well—as there were no statistical differences between our original study groups and the groups of women who actually completed the study.
Finally, the cost of a one-on-one Pilates instruction program such as ours (approximately $1,800) would be prohibitive for most women. However, if our results remain positive within future studies among symptomatic patients, adapting the Pilates protocol to fit a group class or even a web-based platform may be worthwhile. Our results are encouraging and may eventually lead to widespread use of Pilates-based exercise programs to treat and prevent pelvic floor dysfunction. It is easy to imagine the use of Pilates during the peripartum or perioperative periods—as a form of pelvic floor rehabilitation following vaginal deliveries and/or pelvic reconstructive surgery.
References
Rogers R (2008) Urinary stress incontinence in women. N Engl J Med 358(10):1029–1036
Bradley CS, Zimmerman MB, Wang Q, Nygaard IE (2008) Vaginal descent and pelvic floor symptoms in postmenopausal women: a longitudinal study. Obstet Gynecol 111(5):1148–1153
Shamliyan TA, Kane RL, Wyman J, Wilt TJ (2008) Systematic review: randomized, controlled trials of nonsurgical treatments for urinary incontinence in women. Ann Intern Med 148(6):459–473
Bo K (2006) Can pelvic floor muscle training prevent and treat pelvic organ prolapse? Acta Obstet Gynecol Scand 85:263–268
Glazner LM, Herbison GP, MacArthur C et al (2005) Randomised controlled trial of conservative management of potential urinary and fecal incontinence: six year follow up. Br Med J 330:337
Klarskov P, Nielsen KK, Kromann-Andersen B, Maegaard E (1991) Long-term results of pelvic floor training for female genuine stress incontinence. Int Urogynecol J Pelvic Floor Dysfunct 2:132–135
Bo K, Kvarstein NI (2005) Lower urinary tract symptoms and pelvic floor muscle exercises after 15 years. Obstet Gynecol 105(5):999–1005
Agur WI, Steggles P, Waterfield M, Freeman RM (2008) The long-term effectiveness of antenatal pelvic floor muscle training: eight-year follow up of a randomized controlled trial. BJOG 115(8):985–990
Sluijs E, Kok G, Zoe J (1993) Correlates of exercise compliance in physical therapy. Phys Ther 73:771
Latey P (2001) The Pilates method: history and philosophy. J Bodyw Mov Ther 5(4):275–282
Lately P (2002) Updating the principles of the Pilates method—Part 2. J Bodyw Mov Ther 6(2):94–101
Bump R, Mattiasson A, Bo K, Brubaker L, DeLancey J, Klarskov P (1996) The standardsiation of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175:10–17
Barber MD, Walters MD, Bump RC (2005) Short forms for two condition-specific quality of life questionnaires for women with pelvic floor disorders (PFDI-20 & PFIQ-7). Am J Obstet Gynecol 193(1):103–113
Bo K, Talseth T, Home I (1999) Single blind, randomized controlled trial of pelvic floor exercises, electrical stimulation, vaginal cones and no treatment in management of genuine stress incontinence in women. BMJ 318:487–493
Sapsford R, Hodges P (2003) Contraction of the pelvic floor muscles during abdominal maneuvers. Arch Phys Med Rehabil 2001(82):1081–1088
Bo K (2003) Pelvic floor muscle strength and response to pelvic floor muscle training for stress urinary incontinence. Neurourol Urodyn 22(7):654–658
Oyama IA, Rejba A, Lukban JC et al (2004) Modified thiele massage as therapeutic intervention for female patients with interstitial cystitis and high-tone pelvic floor dysfunction. Urology 64(5):862–865
Culligan PJ, Blackwell L, Murphy M, Ziegler C, Heit MH (2004) A randomized, double-blind, sham-controlled trial of postpartum extracorporeal magnetic innervation to restore pelvic muscle strength in primiparous patients. Am J Obstet Gynecol 192:1578–1582
Cochrane library (2006) Issue 1, Article No.: CD005654. doi:10.1002/14651858.CD005654
Hay-Smith J, Morked S, Fairbrother KA, Herbison GP (2008) Pelvic floor muscle training for prevention of urinary and faecal incontinence in antenatal and postnatal women. Cochrane Database Syst Rev 8(4):CD007471
Brostrom S, Lose G (2008) Pelvic floor muscle training in the prevention and treatment of urinary incontinence in women: what is the evidence? Acta Obstet Gynecol Scand 87:384–402
Brubaker L, Shott S, Tomezsko J, Goldberg RP (2008) Pelvic floor fitness using lay instructors. Obstet Gynecol 111(6):1298–1304
Hollis S, Campbell F (1999) What is meant by intention to treat analysis? Survey of published randomized controlled trials. BMJ 319:670–674
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was funded through the Atlantic Health Division of Urogynecology and Reconstructive Pelvic Surgery. In addition, vaginal sensors were donated by The Prometheus Group, Dover, NH, USA.
Rights and permissions
About this article
Cite this article
Culligan, P.J., Scherer, J., Dyer, K. et al. A randomized clinical trial comparing pelvic floor muscle training to a Pilates exercise program for improving pelvic muscle strength. Int Urogynecol J 21, 401–408 (2010). https://doi.org/10.1007/s00192-009-1046-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-009-1046-z