Abstract
Purpose
The adverse impact of first episode psychosis (FEP) upon parents’ quality of life (QoL) has been well documented. However, the determinants and levels of QoL remain poorly understood in siblings of young people experiencing FEP. This study aimed to characterise and establish the predictors of QoL for siblings of young people with FEP.
Method
Survey methodology was used to examine the experience of 157 siblings in the first 18 months of their brother or sister’s treatment for FEP. The World Health Organisation Quality of Life Scale-Bref (WHOQOL-Bref) was used to assess siblings’ QoL. A series of multivariate regression analyses were conducted to determine the relationships between illness characteristics and siblings’ QoL.
Results
Younger sisters reported the lowest satisfaction of QoL. Older brothers were the most satisfied. When the young person with FEP had attempted suicide and/or had been physically violent, siblings reported less satisfaction in all domains of QoL. Living with the ill brother or sister resulted in less satisfaction in the social domain. Multivariate analysis showed that female gender was a significant factor in explaining the impact of illness-related variables on QoL, particularly suicide attempts.
Conclusion
Suicide attempts and a history of violence impacted negatively on all four domains of QoL. Female siblings are at higher risk of reduced QoL and may be particularly vulnerable to the effects of suicide attempts and violence. These findings have significant implications for early, targeted interventions for this vulnerable group.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Family members can experience significant distress and burden when they are participating in the care of an individual with schizophrenia. Studies have shown that family members experience elevated levels of anxiety, depression and economic strain [1–3]. In addition, they have changes to their existing family roles forced upon them, and can experience helplessness, anger and despair [4–9]. Overall, a high level of distress seems to be a typical result of having a family member with a psychotic illness [2]. The available evidence suggests that when the individual has severe symptoms and a long period of illness, family members experience more distress and burden [10, 11].
Studies that have examined the experience of siblings in long-term psychotic illness have found a significant impact upon their quality of life [2, 12–19]. Siblings experience distress such as guilt and grief [14, 20–22]; and burden such as social stigma and fear of acquiring the illness [14, 20–28].
There are no quantitative studies and only a few small qualitative studies about siblings in FEP implemented by two research groups from the United Kingdom [29–31]. For example, Newman and colleagues [29] implemented a narrative analysis of four siblings of young people with FEP and found that gender resulted in different themes of experience. For the female participants (N = 2), the themes were about finding personal meaning. For the male participants, the themes related to taking on responsibilities. Participants in the studies by Sin and colleagues (N = 10; N = 31) reported during semi-structured interviews to feel overwhelmed, resentment, blame, guilt, grief, loss and shame and had stopped inviting friends home [30, 31]. Research using standardised measures with a large sample is required to further understand the impact of FEP on siblings.
There is an extensive body of research in the field of developmental psychology that focuses on the sibling relationship and the important contributions it can make to development, particularly during adolescence and early adulthood [32]. Sibling relationships are enduring, interpersonal ties that serve as important contexts for individual development, and can provide companionship, emotional support and practical support [32, 33]. Further, the protective effects of sibling support during adolescence and early adulthood have been shown to be associated with good coping skills and psychological adjustment, academic competence, higher self-esteem and life satisfaction, positive mental health, and more positive school attitudes [34–38]. Therefore, the onset of psychosis may be critical in terms of disruption and potential loss of an important reciprocal relationship during the significant developmental period of adolescence and early adulthood. Disruption could have significant implications specifically to personality development, identity formation and social support and consequently quality of life.
Birth order has been found to have an influence on personality development and results in distinctive developmental experiences [39, 40]. Thus the QoL of siblings of young people experiencing FEP may be different depending on birth order. The majority of young people who develop a psychosis will still be living at home and, in many cases, they will have a sibling [41]. Expert guidelines in the treatment of FEP emphasize the importance and benefits of family based interventions and support; however, family research and clinical practice in this area have predominantly focused on parents, spouses and offspring and have neglected siblings’ needs [2, 42, 43].
This study is the first quantitative study of siblings of young people with FEP that uses a large sample size (157 participants). This research aimed to establish the QoL of siblings of young people experiencing FEP. A second aim was to establish whether the QoL of siblings of young people with FEP is different depending on birth order and/or gender. Finally, this study aimed to understand whether the QoL of siblings differed depending on the illness-related variables they experienced or witnessed in terms of their brother or sister’s illness. The illness-related variables were identified in the literature as the most common challenges for those experiencing FEP. They include the duration of untreated psychosis before receiving treatment; hospital admissions; medication compliance; persisting positive symptoms; suicide attempts; substance use; and a history of physical violence.
Method
Sample
Siblings of individuals with FEP attending the Early Psychosis Prevention and Intervention Centre (EPPIC) (Orygen Youth Health, Melbourne, Australia) were invited to participate in the study. The accepted age range of the EPPIC program at the time of the study was 15–29 years. The age range of the study (15–29) was dictated by the study aims that were to establish the experience of siblings in the same developmental stage as the young person experiencing FEP, during adolescence/early adulthood.
The mean age for those experiencing FEP was 21.45 (SD 3.51) whilst the mean age for the sibling participants was 21.76 (SD 4.38). Siblings and their ill brother or sister were generally close in age. Previous literature shows that birth order has a more significant impact upon development than age difference due to its influence on social, cognitive, and personality factors [17–20, 27]. Thus, birth order was used in the analysis as opposed to age difference.
The study included individuals fluent in English, able to give informed consent, and had a brother or sister attending EPPIC who would provide consent for their participation. The exclusion criteria were intellectual impairment and a history of psychosis. The research and ethics committees of the North Western Mental Health Program and the La Trobe University approved the study.
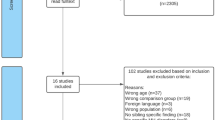
It was an ethical requirement to obtain consent from the young person experiencing FEP in order for their sibling to participate in the study. There were 388 patients attending EPPIC at the time of recruitment. Sixty-four were lost to follow-up, twenty-four did not have a sibling, and eighty-five were reported by their case manager or doctor to be too unwell to be approached. One hundred and twenty-three young people with FEP were, therefore, left to approach about gaining consent for their sibling to participate in the study (57 %). All 123 patients provided consent for a specifically identified sibling to participate. The age range of the sibling participants was from 17 to 29. Twenty-nine were under 18 years of age and required parental consent (24 %).
According to the medical record, the 123 young people with FEP had a total of 417 potential siblings that could have been offered participation; however, only 157 siblings received consent to participate (37.6 %). The mean number of children in each family (N = 123) was 3.32 children with a range of 2–7 children. Further, 39.5 % of sibling participants only had one sibling who was the young person experiencing FEP; 31.2 % and two siblings (one with FEP), 11.5 % had three siblings (one with FEP) and 10 % had six siblings (one with FEP).
Nine young people with FEP agreed for more than one sibling to participate (seven patients consented for two siblings to participate, one consented to three siblings, and one consented to six siblings). This data was not analysed separately.
This process resulted in a purposive sample of 157 siblings (see Tables 1, 2).
Measures
The World Health Organisation Quality of Life Scale-Bref [44] measures satisfaction with QoL and is a 26-item self-report measure organised into four domains: Physical QoL (7 items): activities of daily living and their energy levels; Psychological QoL (8 items): self-esteem and negative feelings; Social QoL (3 items): personal relationships and social supports; and Environment QoL (8 items): financial resources and home environment [44]. All items are rated on a 5-point scale assessing intensity, capacity, frequency or evaluation of their satisfaction. The mean scores of items within each domain are used to calculate the domain score. Mean scores are then multiplied by four to make domain scores compatible with the scores used in the WHOQOL-100 (scale range 0–100) [44, 45]. This scale required reverse scoring of items 3, 4 and 26. The method for converting raw scores to transformed scores is provided in the WHOQOL-Bref user manual (WHO, 1998). Domain scores are scaled in a positive direction with higher scores denoting higher quality of life [44].
The young person with FEP’s medical file was reviewed to obtain data on illness-related variables [i.e. the duration of untreated psychosis before receiving treatment (in months); the number of hospital admissions; history of medication compliance (non-compliant, fluctuating compliance, full compliance); persisting positive symptoms (yes/no); suicide attempts (yes/no; number of); substance use (yes/no; frequency); and history of physical violence (yes/no)].
Analysis method
Descriptive statistics for demographics and clinical variables were computed. Means, standard deviations (SD) and 95 % confidence intervals (95 % CI) were calculated to represent the preliminary population norms. Statistical differences between siblings groups (i.e. younger brother, younger sister, elder brother, older sister) were investigated using independent-samples t tests and one-way analysis of variance (ANOVA). Post hoc comparisons using the Tukey’s Honestly Significant Difference Test were undertaken to determine the significance between groups and to identify the differences that occurred between the groups.
Given the exploratory nature of the research, alpha was set at 0.05 for all analyses. No adjustments were made for multiple comparisons as they can result in a higher type II error, reduced power, and increased likelihood of missing significant findings [46].
Independent-samples t tests, ANOVAs and Pearson correlations were conducted as appropriate to examine the effect of illness-related variables of early psychosis on the QoL of participants as measured by the WHOQOL-Bref (WHO 1998 [44]). Correlation analyses were used to detect relationships between scales and variables. Pearson’s product-moment co-efficient (r) was used. The significance of the strength of correlation was interpreted in accordance with guidelines proposed by Cohen [47].
Several illness-related variables were significantly correlated with the four domains of QoL (at the p < 0.05). To determine which of these variables best predicted QoL a series of adjusted multivariate regression analyses were conducted. These variables were force-entered into four separate regression analyses controlling for the influence of age and gender, with the four domains of QoL serving as the dependent variables in each model. All statistical analyses were undertaken using SPSS-17.
Results
Gender, birth order and its relevance to quality of life
Siblings were divided into four groups for analysis—younger brother (24.8 %), older brother (26.8 %), younger sister (20.4 %), and older sister (28 %). Please see Table 1 for sibling characteristics. Table 2 outlines characteristics of the young people with FEP who provided consent for their sibling to participate.
A statistically significant difference was found between the four groups for the Physical QoL (see Table 3). In statistical analysis, no adjustments for living arrangements or age were made. Older brothers were significantly more satisfied with the Physical QoL than younger sisters, F(3, 153) = 3.66, p = 0.014, η 2 = 0.07. A statistically significant difference was also found in the Psychological QoL with older brothers again being more satisfied than both older and younger sisters, F(3, 153) = 5.75, p = 0.001, η 2 = 0.10. Younger brothers were found to be significantly more satisfied with their Psychological QoL than younger sisters. In the Social QoL, the mean score for older brothers was significantly higher than younger sisters, F(3, 153) = 3.97, p = 0.009, η 2 = 0.07. In the Environment QoL, the mean score for older brothers was again significantly higher than younger sisters, F(3, 153) = 3.93, p = 0.013, η 2 = 0.07 (see Table 3).
Illness-related variables of first episode psychosis and quality of life
Physical domain
Independent-samples t test showed a significant difference in the satisfaction of the Physical QoL scores for participants whose ill brother or sister had attempted suicide and those whose had not [t(155) = 2.27, p = 0.025]; and had a history of violence compared to no history, t(155) = −2.918, p = 0.004, η 2 = 0.05 (see Table 4). Regression analysis revealed that significant predictors of lower Physical Health QoL were history of violence and sibling female gender (see Table 5).
Psychological domain
Independent-samples t test showed a significant difference in satisfaction of the Psychological QoL for those whose ill brother or sister had attempted suicide and those whose had not [t(155) = 2.23, p = 0.027]; and had a history of violence compared to no history of violence, t(155) = −2.191, p = 0.030, η 2 = 0.02 (see Table 4). Regression analysis showed that only female gender remained a significant predictor of low Psychological QoL (see Table 5).
Social domain
Independent-samples t tests showed a significant difference in Social QoL scores for participants whose ill brother or sister had attempted suicide and those whose had not [t(155) = 2.383, p = 0.018; η 2 = 0.03]; had a history of violence compared to no history [t(155) = −3.121, p = 0.002, η = 0.06]; and those who lived with the ill brother or sister compared to those who lived away t(155) = −2.11, p = 0.036, η 2 = 0.02 (see Table 4). Regression analysis revealed that only history of violence remained a significant predictor of lower Social QoL after controlling for the influence of age and gender (see Table 5).
Environment domain
Independent-samples t tests showed a significant difference in the Environment QoL scores for participants whose ill brother or sister had attempted suicide and those whose had not t(155) = 2.47, p = 0.015; η 2 = 0.03; and for those having a brother or sister with a history of violence compared to no history, t(155) = −3.706, p = 0.001, η 2 = 0.06 (see Table 4). Regression analysis showed that significant predictors of low satisfaction in the Environment QoL were history of violence and female gender (see Table 5).
Key findings
Univariate analysis found that suicide attempts and a history of violence impacted negatively on all domains of QoL for siblings of young people suffering from FEP. Older brothers were more satisfied overall with QoL than younger sisters. Living with the young person with FEP also negatively impacted Social QoL. Multivariate analysis revealed that gender played a significant role, with females showing worse QoL in all but the social domain. In addition, history of violence by the young person with FEP remained a significant predictor of low satisfaction for siblings in Physical QoL, Social QoL and Environment QoL.
Exploratory analysis indicated that female siblings appeared to be more vulnerable to the effects of suicide attempts. Females only showed a statistically significant reduction in Physical QoL (t = 2.10, p = 0.030 in females; vs. t = 0.45; p = 0.650, in males) and Environment QoL (t = 2.38, p = 0.010 in females; vs. t = 0.46; p = 0.640, in males) in the presence of prior suicide attempts. This finding was not explained by female siblings being more exposed to suicide. While female siblings were more exposed to suicide attempts than male siblings (35 vs. 22 %) this difference was not statistically significant. Female siblings were also more exposed to violence than male siblings (13.2 vs. 6.2 %) but this too was not found to be significant.
Discussion
This research found through univariate and multivariate analyses that there were two illness-related variables of FEP that negatively impacted siblings’ quality of life. If the young person experiencing FEP had a history of physical violence or had attempted suicide, then these factors were significant predictors of low satisfaction in all the domains of quality of life. Further, this research also found that female gender resulted in less satisfaction in quality of life and were more vulnerable to the effects of suicide attempts. These three findings will now be discussed.
History of violence
Physical violence negatively affected all domains of QoL for siblings of young people with FEP. The results of this study are consistent with studies of siblings in long-term psychotic illness [27, 28]. For example, Greenberg, Kim and Greenley [26] investigated burden in 164 siblings of adults with long-term psychotic illness. They too found that siblings’ QoL was most affected by physical violence.
There is no previous study that has looked specifically at siblings of young people with FEP and the relationship between acts of physical violence and QoL. However, there are studies from the United Kingdom, Ireland, Canada and Australia that have found that a history of physical violence is not uncommon in FEP samples [48–51].
Milton and colleagues [52], from the United Kingdom examined incidents of physical violence in a FEP group over the course of 3 years (N = 168). The authors found that one-third of participants exhibited physical violence. Many were violent prior to contact with services (18.5 %) but it was more common after service contact (31 %).
Other studies have found similar rates of violence in FEP samples such as in an Irish study by Foley, Browne, Clarke, Kinsella, Larkin, and O’Callaghan [53], who implemented a retrospective case design study (N = 157) and found that 29 % of the sample had been physically violent. In another study, Spidel et al. [54] measured violence using a self-report measure that asked participants to report incidents of their physical violence over the past 12 months. The authors found that 42.7 % reported being physically violent within the previous year. All three of these studies found that a long duration of untreated psychosis, persisting substance use and persisting psychotic symptoms contributed to acts of physical violence [52–55]. This research indicates that approximately one-third of individuals experiencing FEP may exhibit violent behaviour.
Hanzawa and colleagues [56] recently investigated the psychological impact on caregivers of a family member with schizophrenia who were physically violent. They reported that non-compliance with treatment, substance abuse and low levels of insight increased the risk of violence in individuals with schizophrenia. In their sample of 116 caregivers, 29 were siblings. The participants in this study reported significant levels of post-traumatic stress disorder associated with exposure to aggressive behaviour by their psychotic family member. Further, this study found that family members who did not live with the ill individual still had significantly high psychological impact from the trauma of the individual’s behaviour.
Wehring and Carpenter [57] in an editorial in the Schizophrenia Bulletin highlighted the fact that there is a substantial underestimation of the prevalence of aggressive behaviour in those with psychotic disorders and the burden of caring and coping with this aggression, threats of violence, and violent acts falls on family members. The authors suggest that the field may have failed to adequately address this violence, in part due to an eagerness to reduce stigma, and should consider the unmet therapeutic need to address the hostility and aggression.
The findings of this study support this direction, as our findings indicate that physical violence significantly and negatively impacted upon the quality of life of siblings of young people with FEP. Further investigation into the prevalence of physical violence experienced by siblings in FEP should be conducted. It is also suggested that clinicians identify siblings who may have witnessed or experienced this violence, whether or not they live at home, to provide support and assist with coping. This may reduce the negative impact upon their quality of life.
Suicide attempts
Suicide attempts resulted in less satisfaction in each domain of the siblings’ QoL. There is no research into the consequences of suicide attempts for family members in FEP and minimal research on family members in long-term psychotic illness. More research into this impact is required. It is established in the literature that schizophrenia carries a 10 % lifetime risk of suicide with the highest risk in those who developed the illness during adolescence and within the first couple of years after diagnosis [58–61]. Studies have explored the frequency of suicidality in this population and the prevalence of suicide attempts in FEP samples is high [62, 63].
Power et al. [64] implemented a clinical audit to ascertain the prevalence of suicidal ideation in all individuals attending an early psychosis clinic in Melbourne, Australia (N = 312). Descriptive statistics showed that 46 % were rated as persistently suicidal throughout the 3-month study period.
Robinson et al. [63], also from Australia, implemented a retrospective file audit to examine the prevalence of suicide attempts in the first 2 years of treatment (N = 661). The results showed that 22 % had attempted suicide and 10 % of those had attempted multiple times. One percent had died by suicide. Further, Farrelly and colleagues [62] in Melbourne, Australia, conducted a naturalistic, prospective study to examine the prevalence of suicide attempt in a FEP sample over 7 years (N = 413). They found that 221 had made no suicide attempt over that time (53 %) but that 24 had made one attempt (6 %), 26 had made more than one attempt (6 %), and 12 had died by suicide (3 %). This study suggests that suicide risk can remain high for at least 7 years following the commencement of treatment for FEP and a key predictor of future attempts is previous attempts. Therefore, it is important to ascertain how families, and specifically siblings, cope and manage these difficult events.
A Norwegian study has been included in this discussion as it provides valuable insights into the sibling relationship when a suicide occurs. Dyregrov and Dyregrov [65] implemented a mixed method study to explore the needs of siblings after losing a brother or sister to suicide. Data were collected from 70 siblings divided into two subsamples. The first subsample consisted of 11 adolescents with a mean age of 17.7 years who lived at home with their parents at the time of the death. There were five females and six males in this younger sibling subsample. The second subsample consisted of 59 siblings with a mean age of 28.4 years who lived either alone or with their own core family at the time of the death. There were 39 older sisters and 20 older brothers in this subsample. Post-traumatic stress disorder was measured as was information about where siblings received support. Four younger siblings and five older siblings were then interviewed in-depth. The interviews aimed to further understand the siblings’ experiences, as well as the qualitative dimensions of support and coping strategies.
The findings showed that one-third of younger siblings had been aware of previous suicide attempts and knew the triggers. They kept this from their parents which burdened them with ongoing guilt. Whilst the parents in the study reported finding it difficult to understand why the suicide had happened, the siblings had different information and knowledge. This enabled them to have their own theories as to why it happened. Siblings in this study avoided talking about this with their parents in order not to reveal information given to them in confidence. They felt this information could add to their parents’ suffering. The siblings in the study reported that they did not communicate their own grief to protect their parents. As a result they felt alone. All siblings felt only partly looked after by the family’s network and professionals because most of the attention was directed toward their parents. The parents also confirmed that the bereaved siblings were “forgotten” in the days following the death [65]. This may be relevant to siblings in early psychosis, as they too may feel ‘forgotten’; however, this was not measured in this study.
Other researchers have also found that siblings often provide support to their parents rather than the other way around [30]. For example, Sin, Moone and Harris [30] found in their qualitative studies that siblings in FEP provided support to their parents and saw this as an important role. Social support was not measured in this study. While this was beyond the scope of this article further studies should investigate the social support received by siblings and its value and effectiveness. Parents may be less available for the sibling because of the stress and burden they experience. This may have a negative impact upon siblings and should be investigated further.
Cerel and colleagues [66] suggest that suicide and suicide attempts could have a profound effect on social networks for family members. Social support after any type of loss is a crucial factor in determining grief outcomes [67]. The authors proposed that social networks can be negatively impacted by communication processes that occur after suicide or attempts. Such processes include issues of blame, secrecy, social ostracism and self-isolation. Family members can blame themselves for words that were exchanged with the ill individual, or for their seeming short-comings as a parent, partner, sibling or so forth. Even if they conclude that they were not directly responsible for the death or the attempt, family members can struggle with the perceived failure to anticipate and intervene to prevent it from occurring.
Further research is required to understand further the psychological impact of suicide attempts in young people with FEP for siblings to understand their experience and ways to assist them in coping to reduce the negative impact upon their quality of life.
Gender
The findings of this study may be seen to support previous gender research where females reported more negative emotional experiences than men [68–70]; and more symptoms of dissatisfaction and depression than men [69, 71–75]. Alternatively, it has been suggested by researchers that men and women are equal in their experiences but men are more reluctant than women to admit negative experiences and feelings [68, 69, 76]. Interestingly, over 80 % of participants in studies about siblings in long-term psychotic illness are female [2, 13, 14, 18–20, 22–24, 27, 28, 77]. In these studies they report negative experiences related to a decrease in satisfaction with their quality of life such as grief, guilt, shame, sadness, self-blame, difficulty with relationships, changed life goals and direction. The female participants in the current study may also experience difficulty in witnessing their parent’s sadness and helplessness, as was found by Sin, Moone and Harris [30]. This may also impact upon their quality of life. Further research should be conducted with female siblings of young people with FEP to understand their experience.
Birth order
Older brothers in this study reported the most satisfaction in all domains of quality of life. Younger sisters reported the least satisfaction in all domains. This may again be explained in light of theories of gender relationships and link closely with the quality of the sibling relationship.
Older brothers reported over ten points more satisfaction with the social domain than both younger brothers and sisters. Older brothers in this study reported the most satisfaction in all domains of QoL. Dyregrov and Dyregrov [65] also found in their quantitative data that birth order was relevant to the level of distress experienced by the participants following suicide. These researchers found that older siblings living on their own experienced less post-traumatic distress than the younger siblings. Older siblings whose brother or sister had died by suicide were less affected than younger siblings by symptoms of depression and anxiety due to their age and developmental stage (often living out of home), marital status and external social support. These factors may also protect older siblings of young people with FEP as they are more able to avoid exposure to their parent’s distress and the characteristics of FEP such as hospital admissions, non-compliance with treatment, and/or persisting symptoms. However, further investigation should be undertaken to further explore this possibility.
The current study found that birth order, specifically for younger females, related to lower satisfaction in the participants’ psychological quality of life. The majority of younger siblings in this study lived at home: 82.1 % of younger brothers lived at home and 71.9 % of younger sisters lived at home, in comparison to 52.4 % of older brothers and 34.1 % of older sisters. Consequently, younger siblings were exposed to more negative experiences associated with FEP and the characteristics of the illness. It is, therefore, not surprising that younger siblings living at home negatively appraised the social domain, as well as the physical and environmental domains of their quality of life. One possible explanation for this may be that they are not open to sharing their experiences with others due to shame, embarrassment and stigma as was found by Barak and Solomon [23]. Younger siblings living at home may spend less time with their peer group than older siblings, therefore, receiving less external support. These findings are consistent with the work of Dyergrov and Dyregrov [65] and also with Titelman and Psyck [22], who found that siblings of those with long-term psychotic illness felt they should restrict themselves from enjoying a social life.
The findings may also relate to a change in the established protective effects of sibling support in normal samples [34–38, 78, 79]. When a young person is experiencing FEP, they may be unable to provide the previously experienced support and relationship to their sibling. This may result in increased distress for siblings when dealing with stressful life events due to the loss of comfort and security, resulting in changes to psychological adjustment, wellbeing and self-esteem [80–85]. This may also result in a decreased satisfaction in QoL. Further research should be conducted to investigate whether protective factors can still exist during FEP.
Limitations
The current study has several limitations. First, those who consented to participate in the study may represent a subgroup of siblings who have experienced high levels of distress and hardship. Second, data were not collected regarding aspects of the family that might have provided a better insight into environmental factors that influenced QoL, such as relationship with parents, parents working status, geographical location, whether any physical illnesses or disabilities existed within the family, and whether parents were receiving professional assistance for mental health problems. Third, requiring consent from the young person with FEP may have resulted in the omission of a specific sample of siblings. This research, therefore, may have been unable to gain insight into siblings who were estranged or in conflict with their ill brother or sister. Young people with FEP may also have withheld their consent if they were concerned about their sibling’s current mental health status and coping skills. Finally, a further limitation of this research was the reliability of information obtained from the medical records.
Clinical implications
The findings of this research suggest that siblings of young people with FEP find suicide attempts and physical violence the most distressing illness-related variables and consequently result in a significant decrease in satisfaction with their quality of life. Further, female siblings were more vulnerable to the impact of suicide attempts than male siblings. Further research needs to be conducted that focuses on the experience and impact of suicide attempts and physical violence on siblings. More focus on supporting family members with the trauma of these events is also required.
Clinicians are encouraged to identify early siblings of young people with FEP who have witnessed these events and provide ongoing support, coping and problem-solving strategies in order minimise the impact on their quality of life and prevent prolonged deterioration. Better knowledge of the pattern and extent of impact on siblings may create momentum for inclusion of siblings within a suite of interventions for family and peers affected by the onset of psychosis in young people. Consequences of poor quality of life may include an increased risk of depression and anxiety, and deterioration in educational, vocational, and social performance. This would have implications on the sibling’s developmental trajectory during adolescents and emerging adulthood [53]. Early intervention, preventative support, and specific targeted sibling support are recommended.
References
Barrowclough C, Tarrier N, Johnston M (1996) Distress, expressed emotion, and attributions in relatives of schizophrenia patients. Schizophr Bull 22(4):691–702
Lobban F, Barrowclough C (2009) A casebook of family interventions for psychosis. Wiley, West Sussex
Szmukler G, Burgess P, Hermann H, Colusa S, Benson A, Bloch S (1996) Caring for relatives with serious mental illness: the development of care giving inventory. Soc Psychiatry Psychiatr Epidemiol 31:137–148
Addington J, Burnett P (2004) Working with families in the early stages of psychosis. In: Gleeson J, McGorry P (eds) Psychological interventions for early psychosis. Wiley, UK, pp 99–116
Addington J, Coldham E, Jones B, Ko T, Addington D (2003) The first episode of psychosis: the experience of relatives. Acta Psychiatr Scand 108:285–289
McCann T, Lubman D, Clark E (2011) First-time primary caregivers’ experience of caring for young adults with first episode psychosis. Schiophr Bull 37(2):381–388
Sin J, Moone N, Wellman N (2005) Developing services for the carers of young adults with early-onset psychosis—listening to their experiences and needs. J Psychiatric Ment Health Nurs 12:589–597
Tennakoon L, Fannon D, Doku V, O’Ceallaigh S, Soni W, Santamario M (2000) Experience of caregiving: relatives of people experiencing a first episode of psychosis. Br J Psychiatry 177:529–533
Wong C, Davidson L, Anglin D, Link B, Gerson R, Malaspina D (2009) Stigma in families of individuals in early stages of psychotic illness: family stigma and early psychosis. Early Interv Psychiatry 3(2):108–115
Addington J, McCleery A, Addington D (2005) Three-year outcome of family work in an early psychosis program. Schizophr Res 79:107–116
Smith J, Fadden G, O’Shea M (2009) Interventions with siblings. In: Lobban F, Barrowclough C (eds) A casebook of family interventions for psychosis. Wiley, New Jersey, pp 185–210
Corcoran C, Gerson R, Sills-Shahar R, Nickou C, McGlashan T, Malaspina D, Davidson L (2007) Trajectory to a first episode of psychosis: a qualitative research study with families. Early Interv Psychiatry 1(4):308–315
Ewertzon M, Cronqvist A, Lutzen K, Andershed B (2012) A lonely like journey bordered with struggle: being a sibling on an individual with psychosis. Issues Ment Health Nurs 33(3):157–164
Gerace L, Camilleri D, Ayres L (1993) Sibling perspectives on schizophrenia and the family. Schizophr Bull 19(3):637–647
Gleeson J, Wade D, Castle D, Gee D, Crisp K, Pearce T, Newman B, Cotton S, Alverez-Jinenez M, Gilbert M, McGorry P (2008) The EPISODE 11 trial of cognitive and family therapy for relapse prevention in early psychosis: rationale and sample characteristics. JMH 17(1):19–32
Gleeson JF, Cotton S, Alvarez-Jimenez M, Wade D, Crisp K, Newman B, Spiliotacopoulos D, McGorry PD (2010) Family outcomes from a randomized control trial of relapse prevention therapy in first-episode psychosis. J Clin Psychiatry 71(4):475–483
Kinsella K, Anderson R, Anderson W (1996) Coping skills, strengths, and needs as perceived by adult offspring and siblings of people with mental illness: a retrospective study. Psychiatr Rehabil J 20(2):24–32
Lukens E, Thorning H, Lohrer S (2004) Sibling perspectives on severe mental illness: reflections on self and family. Am J Orthopsychiatr 74(4):489–501
Patterson P, Birchwood M, Cochrane R (2005) Expressed emotion as an adaptation to loss. Prospective study in first-episode psychosis. Br J Psychiatry 187(Supp 48):59–64
Lively S, Friedrich RM, Buckwalter KC (1994) Sibling perception of schizophrenia: impact on relationships, roles and health. Issues Ment Health Nurs 16:225–238
Riebschleger JL (1991) Families of chronically mentally ill people: siblings speak to social workers. Health Soc Work 16(2):94–103
Titelman D, Psyk L (1991) Grief, guilt, and identification in siblings of schizophrenic individuals. Bull Menninger Clin 55:72–84
Barak D, Solomon Z (2005) In the shadow of schizophrenia: a study of siblings’ perceptions. Isr J Psychiatry Relat Sci 42(4):234–241
Barnable A, Bennett L, Meadus R (2006) Having a sibling with schizophrenia: a phenomenological study. Res Theory Nurs Pract 20(3):247–263
Friedrich R, Lively S, Rubenstein L (2008) Siblings’ coping strategies and mental health services: a national study of siblings’ perceptions of persons with schizophrenia. Psychiatr Serv 59(3):261–267
Greenberg J, Kim H, Greenley J (1997) Factors associated with subjective burden in siblings of adults with severe mental illness. Am J Orthopsychiatry 67(2):231–241
Smith MJ, Greenberg JS (2008) Factors contributing to the quality of sibling relationships for adults with schizophrenia. Psychiatr Serv 59(1):57–62
Solomon PL, Cavanaugh MM, Gelles RJ (2005) Family violence among adults and severe mental illness: a neglected area of research. Trauma Violence Abus 6(1):40–54
Newman S, Simonds L, Billings J (2011) A narrative analysis investigating the impact of first episode psychosis on siblings’ identity. Psychosis 3(3):216–225
Sin J, Moone N, Harris P (2008) Siblings of individuals with first-episode psychosis: understanding their experiences and needs. J Psychoso Nurs Ment Health Serv 46(6):33–40
Sin J, Moone N, Harris P, Scully E, Wellman N (2011) Understanding the experiences and service needs of siblings of individuals with first-episode psychosis: a phenomenological study. Early Interv Psychiatry 6(1):53–59
East PL (2009) Adolescents’ relationships with siblings. In: Lerner R, Steinberg L (eds) Handbook of adolescent psychology. Wiley, New Jersey, pp 43–73
Bank S, Kahn M (2003) The sibling bond. Basic Books, New York
Branje S, Lieshout C, Van Aken M, Haselager GJT (2004) Perceived support in sibling relationships and adolescent adjustment. J Child Psychol Psychiatry 45:1385–1396
Gass K, Jenkins J, Dunn J (2007) Are sibling relationships protective? A longitudinal study. J Child Psychol Psychiatry 48:167–175
Goodman R (1999) The extended version of the strengths and difficulties questionnaire as a guide to child psychistric caseness and consequent burden. J Child Psychol Psychiatry 40:791–799
Norman R, Malla A, Manchanda R, Harricharan R, Takhar J, Northcott S (2005) Social support and three-year symptom and admission outcomes for first episode psychosis. Schizophr Res 80:227–234
Oliva A, Arranz E (2005) Sibling relationships during adolescence. Eur J Dev Psychol 2(3):253–270
Adler A (1928) Characteristics of the first, second, and third child. Children 3:14
Sulloway F (1996) Born to rebel: birth order, family dynamics and creative ways. Pantheon Books, New York
Australia Bureau of Statistics (2010) Mental health of young people, Retrieved from http://www.abs.gov.au/ausstats/abs@.nsf/Latestproducts/4840.0.55.001Main%20Features22007?opendocument&tabname=Summary&prodno=4840.0.55.001&issue=2007&num=&view. Accessed 02 Mar 2013
Bird V, Premkumar P, Kendall T, Whittington C, Mitchell J, Kuipers E (2010) Early intervention services, cognitive-behavioural therapy and family intervention in early psychosis: systematic review. Br J Psychiatry 197:350–356
Royal Australian and New Zealand College pf Psychiatrists (RANZCP) (2005) Clinical practice guidelines for the treatment of schizophrenia and related disorders. Aust NZ J Psychiatry 39:1–30
World Health Organisation (WHO) (1998) WHOQOL User Manual. Geneva, World Health Organisation
Hawthorne G, Hermann H, Murphy B (2006) Interpreting the WHOQOL-Brèf: preliminary population norms and effect sizes. Soc Indic Res 77(1):37–59
Rothman KJ (1990) No adjustments are needed for multiple comparisons. Epidemiology 1(1):43–46
Cohen J (1988) Statistical power analysis for the behavioural sciences. Erlbaum, Hillsdale
Large M, Nielssen O (2008) Evidence for a relationship between the duration of untreated psychosis and the proportion of psychotic homicides prior to treatment. Soc Psychiatry Psychiatr Epidemiol 43:37–44
Appleby L, Shaw J (2006) Five year report of the national confidential inquiry into suicide and homicide by people with mental illness. http://www.medicine.manchester.ac.uk/suicideprevention/nci/Useful/avoidabledeaths_full_report.pdf. Accessed 05 Apr 2013
Meehan J, Flynn S, Hunt I, Robinson J, Bickley H, Parsons R, Shaw J (2006) Perpetrators of homicide with schizophrenia: a national clinical survey in England and Wales. Psychiatr Serv 57:1648–1651
Nielssen O, Westmore B, Large M, Hayes R (2007) Homicide during psychotic illness in New South Wales between 1993 and 2002. Med J Aust 186:301–304
Milton L, Amin S, Singh S, Harrison G, Jones P, Croudace T (2001) Aggressive incidents in first episode psychosis. Br J Psychiatry 178:433–440
Foley S, Browne S, Clarke M, Kinsella A, Larkin C, O’Callaghan E (2007) Is violence at presentation by patients with first episode psychosis associated with duration of untreated psychosis? Soc Psychiatry Psychiatr Epidemiol 42:606–610
Spidel A, Lecomte T, Greaves C, Sahlstrom K, Yuille P (2010) Early psychosis and aggression: predictors and prevalence of violent behaviour amongst individuals with early psychosis. Int J Law Psychiatry 33:171–176
Arnett J (2010) Adolescence and emerging adulthood: A cultural approach, 4th edn. Prentice Hall, New York
Hanzawa S, Bae J, Bae Y, Chae M, Tanaka H, Nakane H, Ohta Y, Zhao X, Lizuka H, Nakane Y (2013) Psychological impact on caregivers traumatized by the violent behaviour of a family member with schizophrenia. Asian J Psychiatr 6:46–51
Wehring H, Carpenter W (2011) Violence and Schizophrenia. Schizophr Bull 37:877–878
Beautrais A (2003) Suicide and serious suicide attempts in youth: a multiple-group comparison study. Am J Psychiatry 160:1093–1099
Harris M, Burgess P, Chant D, Pirkis J, McGorry P (2008) Impact of a specialized early psychosis treatment programme on suicide. Retrospective cohort study. Early Interv Psychiatry 2:11–21
Nordentoft M, Jeppesen P, Abel M, Kassow P, Petersen L, Thorup A, Krarup G, Hemmingsen R (2002) OPUS study: suicidal behaviour, suicidal ideation and hopelessness among patients with first-episode psychosis. One-year follow-up of a randomised controlled trial. Br J Psychiatry 43:98–106
Siris S (2001) Suicide and schizophrenia. J Psychopharmacol 15:127–135
Farrelly S, Harrigan S, Harris M, Henry L, Jackson H, McGorry P (2010) Suicide attempt in first episode psychosis: a 7.4 year follow-up study. Schizophr Res 116(1):1–8
Robinson J, Cotton S, Conus P, Schimmelman B, McGorry P, Lambert M (2009) Prevalence and predictors of suicide attempt in an incidence cohort of 661 young people with frist-epsidoe psychosis. Aust NZ J Psychiatry 43(2):149–157
Power P, Bell R, Mills R, Hermann-Doig T, Davern M, Henry L, McGorry PD (2003) Suicide prevention in first episode psychosis: the development of a randomised controlled trial of cognitive therapy for acutely suicidal patients with early psychosis. Aust NZ J Psychiatry 37:414–420
Dyregrov K, Dyregrov A (2005) Siblings after suicide: the forgotten bereaved. Suicide Life Threat Beh 35:714–724
Cerel J, Jordan J, Duberstein P (2008) The impact of suicide on the family. Crisis 29:38–44
Styliano S, Vachon M (1993) The role of social support in bereavement. In: Stroebe M, Stroebe W, Hansson R (eds) Handbook of Bereavement. Cambridge University Press, UK, pp 397–410
Fujita F, Diener E, Sanvik E (1991) Gender differences in negative affect and well-being: the case for emotional intensity. J Pers Soc Psychol 61(3):427–434
Moksnes V, Moljord L, Espenes G, Byrne D (2010) The association between stress and emotional states in adolescence: the role of gender and self esteem. Pers Individ Dif 49(5):430–435
Polce-Lynch M, Myers B, Kliewer V, Kilmartin C (2001) Adolescent self esteem and gender: exploring relations to sexual harrassment, body image, media influence and emotional expression. J Youth Adolesc 30(2):225–244
Eaton W, Kessler L (1981) Rates of symptoms of depression in a national sample. Am J Epidemiol 114:528–538
Frerichs R, Aneshensal C, Clark V (1981) Prevalence of depression in Los Angeles county. Am J Epidemiol 113:691–699
Murrell S, Himmelfarb S, Wright K (1983) Prevalence of depression and its correlates in older adults. Am J Epidemiol 117:173–185
Piko B (2001) Gender differences and similarities in adolescents’ ways of coping. Psychol Rep 51:223–235
Rosenfield S (1980) Sex differences in depression: do women always have higher rates? J Health Soc Behav 21:33–42
Ladwig K, Marten-Mittag B, Formanek B, Dammann G (2000) Gender difference of symptom reporting and medical health care utilisation in the German population. Eur J Epidemiol 16(6):511–518
Smith J, Fadden G, Taylor L (2010) The needs of siblings in first episode psychosis. In: French P, Reed M, Smith J, Raynew M, Shiers D (eds) Early intervention in psychosis: promoting recovery. Blackwell, Oxford, pp 235–243
Forehand R, Wierson M, Thomas A, Armstead L, Kempton T, Neighbours B (1991) The role of family stressors and parent relationships on adolescent functioning. J Am Acad Child Adolesc Psychiatry 30:316–322
Wille N, Bettge S, Raverns-Sieberer U (2008) Risk and protective factors for children’s and adolescent’s mental health: results of the BELLA study. Eur Child Adolesc Psychiatry 17(suppl 1):133–147
Bandura A (1989) Social cognitive theory. Ann Child Dev 6:1–60
Brody G (1998) Sibling relationship quality: its causes and consequences. Annu Rev Psychol 49:1–24
Bowlby J (1969) Attachment. Basic Books, New York
Circirelli V (1989) Feelings of attachment to siblings and well-being in later life. Psychol Aging 4:211–216
Minuchin P (1988) Relationships within the family: a systems perspective on development. In: Stevenson-Hinde J, Hinde R (eds) Relationships within families: mutual influences. Oxford Clarendon Press, UK, pp 7–26
Whiteman S, McHale S, Crouter A (2007) Competing processes of sibling influence: observational learning and sibling deidentification. Soc Dev 16(4):642–661
Acknowledgments
Generous funding from the Anita Morawetz Family Therapy Scholarship, The University of Melbourne, supported this study. The authors wish to thank the study participants for their invaluable contributions to this research and the CR Roper Fellowship, University of Melbourne (Dr. Alvarez-Jimenez).
Conflict of interest
The authors report no additional financial or other affiliation relevant to the subject of the article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bowman, S., Alvarez-Jimenez, M., Wade, D. et al. The impact of first episode psychosis on sibling quality of life. Soc Psychiatry Psychiatr Epidemiol 49, 1071–1081 (2014). https://doi.org/10.1007/s00127-013-0817-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-013-0817-5