Abstract
The mechanisms responsible for how resveratrol inhibits pathological left ventricular hypertrophy (LVH) but not physiological LVH have not been elucidated. Herein, we show that in rat cardiomyocytes, lower concentrations of resveratrol (0.1 and 1 μM) are efficient at selectively inhibiting important regulators involved in pathological LVH (such as nuclear factor of activated T cells (NFAT)) while not affecting pathways involved in physiological LVH (Akt and p70S6 kinase (p70S6K)). These differential responses are also observed in both mouse and rat models of in vivo physiological and pathological LVH. Interestingly, in all of the experiments involving a low concentration of resveratrol (1 μM), the observed effects on Akt, p70S6K, and NFAT were independent from AMP-activated protein kinase (AMPK) activation while these effects at higher concentrations of resveratrol (50 μM) were potentiated by AMPK activation. In summary, we show that resveratrol can concentration/dose selectively inhibit various pro-hypertrophic signaling pathways and that resveratrol has differential effects on the modification of these signaling cascades in response to pathological stimuli versus physiological stimuli. This has important clinical implications as our findings support the concept that resveratrol may be useful in the selective treatment of pathological LVH.
Key message
-
Resveratrol differentially regulates pathological and physiological cardiac hypertrophy.
-
Resveratrol dose selectively inhibits pathological cardiac signaling pathways.
-
Resveratrol inhibits NFAT-dependent transcription.
-
At low concentrations, effects of resveratrol are AMPK-independent.
-
Resveratrol may be used to selectively treat pathological cardiac hypertrophy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pathological stimuli such as pressure overload or hypertrophic agonists induce maladaptive growth of the myocardium that is associated with an increased rate of morbidity and mortality [1]. In contrast, physiological hypertrophy induced by stimuli such as chronic exercise and growth factors induce adaptive growth of the heart that is not linked to cardiac dysfunction [2]. Although, physiological and pathological left ventricular hypertrophy (LVH) are distinct entities, overlap exists between the molecular mechanisms that control the physiological and pathological growth of the heart. For example, both physiological and pathological LVH involve the activation of the p70S6 kinase (p70S6K) pathway that contributes to enhanced protein synthesis [3], which is necessary for growth of the cardiomyocyte. p70S6K can be regulated by several other kinase cascades, including AMP-activated protein kinase (AMPK) and Akt [4, 5]. Previous work has shown that increasing AMPK activity inhibits p70S6K phosphorylation, which prevents LVH [6–8].
While p70S6K activation is involved in both physiological and pathological LVH processes, other hypertrophic pathways appear to be predominantly involved in pathological LVH. For instance, the nuclear factor of activated T cells (NFAT), which promotes a pro-hypertrophic gene expression profile [9], is not activated by physiologic stimuli, suggesting that activation of NFAT may specifically regulate pathological remodeling of the myocardium [10]. Interestingly, although the primary mediator of NFAT is the calcium/calmodulin-activated protein phosphatase, calcineurin [9], previous work has shown that AMPK activation can inhibit NFAT-mediated transcription [6, 8]. As such, previous findings demonstrate that AMPK controls both p70S6K and NFAT and implicates AMPK as an important regulator of LVH [4].
Resveratrol (Resv) is a naturally occurring polyphenolic molecule that is beneficial for the cardiovascular system [11]. We have recently demonstrated that concentrations of Resv above 50 μM attenuated phenylephrine-induced cardiomyocyte cell growth and inhibited protein synthesis through the activation of AMPK and the inhibition of p70S6K phosphorylation [6]. We and others have also demonstrated that Resv prevented various pathological forms of LVH [12–17], including angiotensin (Ang)-II-induced LVH in vivo [18]. More recently, we showed that Resv supplementation during exercise training of rats improved LV function and augmented physical performance [19]. Together, these findings suggest that Resv could be utilized to alleviate the pathological development of LVH without affecting adaptive physiological cardiac growth. However, the mechanisms mediating the differential effects of Resv in the setting of physiological versus pathological LVH are unknown. Therefore, the purpose of this study was to investigate how Resv regulates AMPK, p70S6K, and NFAT activation in response to physiological and pathological pro-hypertrophic stimuli.
Materials and methods
Materials
Primary antibodies utilized in this study were purchased from Cell Signaling Technology (Danvers, MA), with the exception of the anti-actin primary antibody and secondary antibodies for goat anti-rabbit and donkey anti-goat, which were from Santa Cruz Biotechnology (Dallas, TX). Most other cell culture reagents and chemicals were purchased from Sigma (St. Louis, MO) and Invitrogen (Carlsbad, CA). The luciferase activity assay kit was purchased from Promega (Madison, WI).
Human ethics
The collection and use of human atrial samples for this study was approved by the University of Alberta’s Health Research Ethics Board (Biomedical Panel).
Animal care and diets
The University of Alberta Animal Policy and Welfare Committee adheres to the principles for biomedical research involving animals developed by the Council for International Organizations of Medical Sciences (CIOMS). All rodents were obtained from Charles River Laboratories (Sherbrooke, QC). Rodents had free access to drinking water and were fed ad libitum with either an AIN93G standard chow diet or an AIN93G standard chow diet that contained 4 g Resv/kg diet (Dyets Inc., Bethlehem, PA), which is consistent with previous studies [18–21]. For spontaneously hypertensive rats (SHRs) and Wistar rats, the dosage of Resv was equivalent to ∼146 mg Resv/kg/day. For mice, the dosage was equivalent to ∼320 mg Resv/kg/day. For angiotensin (Ang)-II-induced hypertrophy, Alzet osmotic micro-pumps (Cupertino, CA) were implanted into C57BL/6 mice by a small incision that was made dorsal interscapularis to form a small subcutaneous pocket allowing for the delivery of saline or Ang-II (1.4 mg/kg/day). The same cohort of mice as described previously [18] consumed the diets for 2 weeks following implantation of the osmotic mini-pumps. For insulin-like growth factor (IGF)-1-induced hypertrophy, recombinant IGF-1 was purchased from Sigma and administered to C57BL/6 mice at 4 mg/kg/day for 7 days via subcutaneous injection. As described previously [19, 21], the same cohort of Wistar rats were subjected to 60 min of treadmill running at 20 m/min for a total of 12 weeks. These exercise-trained Wistar rats were used as the model of exercise-induced physiological LVH. Rodents were euthanized with an intraperitoneal injection of euthanyl (0.5 ml/kg body weight).
Cell culture
Hearts were isolated from newborn (1–3-day-old) rats, and neonatal rat cardiac myocytes (NRCMs) were isolated and cultured as we have previously described [6, 22] and treated as indicated in the figure legends.
Immunoblot analysis
Cells were lysed and heart tissue was homogenized according to previously reported methods [6, 12]. NRCMs were the protein concentration was assayed using Bradford protein reagent; 15–20 μg of protein was used for SDS-PAGE and immunoblot analysis using phosphoprotein and protein-specific antibodies.
Quantitative real-time PCR
Specific quantitative assays were designed from mouse and rat sequences available in GenBank. Standard RNA was made for all assays by the T7 polymerase method (Ambion, Austin, TX) using total RNA isolated from rat and mouse heart tissues. Inventoried primer and probe sequences for the mouse and rat Hprt, Anf, Bnp, β-Mhc and Mcip1 genes were purchased from Applied Biosystems. All other sequences are listed in Table S1. Real-time qPCR was performed using a 7900HT Fast Real-Time PCR System (Applied Biosystems). Data are presented as mRNA molecules per nanogram total RNA relative to the control housekeeping gene (Hprt).
Luciferase activity assays
Cells are infected at a multiplicity of infection (MOI) of 10 with the NFAT-luciferase reporter gene adenovirus (Ad.NFAT-Luc; Seven Hills Bioreagents) that is driven by the alpha myosin heavy chain promoter containing multiple NFAT binding sites and previously validated to be calcineurin responsive [10]. Cells were treated with the indicated concentrations of compounds or the respective vehicles for 24 h. Subsequently, cells were harvested with the reporter lysis buffer supplied by the manufacturer (Promega). Luminescence (luciferase activity) was measured using the MicroBeta luminometer (Perkin Elmer).
Statistical analysis
Data are expressed as mean ± standard error of the mean (S.E.M.). Comparisons between rat strains or treatment groups were performed using the non-parametric unpaired student’s t test or the Mann-Whitney U test to compare the differences in scores between groups where appropriate. A probability value of <0.05 is considered significant.
Results
High concentrations of resveratrol inhibit molecular signals controlling cardiomyocyte protein synthesis and inhibit NFAT-mediated transcription
Our previous work demonstrated that high concentrations (50 and 100 μM) of Resv inhibits hypertrophy of NRCMs through the inhibition of p70S6K, eukaryotic elongation factor 2 (eEF2), and protein synthesis [6]. Therefore, we sought to determine whether lower, more physiologically relevant concentrations of Resv also had similar effects. Consistent with our previous report, 24 h treatment of NRCMs with 50 μM Resv increased phosphorylation of AMPK at Thr172 (P-AMPK; Fig. 1a), an effect that was not observed at lower concentrations. Since AMPK phosphorylates acetyl-CoA carboxylase (ACC), we measured phosphorylation of ACC at Ser79 (P-ACC) as an additional marker of AMPK activity. In agreement with the P-AMPK results, P-ACC was increased following 24 h of treatment with 50 μM Resv, but not at lower concentrations (Fig. 1b). In contrast to our previous report using higher concentrations of Resv [6], Resv treatment (0.1–50 μM) for 24 h did not significantly change Akt phosphorylation at Ser473 (Fig. 1c). However, 10 and 50 μM concentrations of Resv were sufficient to inhibit phosphorylation of p70S6K at Thr421 (Fig. 1d) and Thr389 (Fig. 1e), respectively. Furthermore, 50 μM Resv increased eEF2 phosphorylation (indicating eEF2 inactivation), while lower concentrations of Resv did not alter eEF2 phosphorylation (Fig. 1f). In addition, the range of Resv concentrations between 0.1 and 50 μM did not affect SIRT1 expression in the cardiomyocytes (Fig. S1a). Together, these data suggest that Resv inhibited signals controlling cardiomyocyte protein synthesis only at 50 μM and not at the lower concentrations that we tested.
Resveratrol (Resv) concentration-dependently activates AMPK, and inhibits p70S6K and NFAT activities in neonatal rat cardiomyocytes. Cardiomyocytes were treated with vehicle (1 μl ethanol) or increasing concentrations of Resv ranging from 0.1 to 50 μM for 24 h. Immunoblot analysis of phosphorylated T172 AMPK (P-AMPK) levels were quantified by densitometry and normalized against total AMPK (a). Levels of phosphorylated S79 ACC (P-ACC) were quantified by densitometry and normalized against total ACC (b). Levels of phosphorylated S473 Akt (P-Akt) were quantified by densitometry and normalized against total Akt (c). Levels of phosphorylated T389 p70S6K (P-p70S6K) were quantified by densitometry and normalized against actin (d). Levels of phosphorylated T421/S424 p70S6K (P-p70S6K) were quantified by densitometry and normalized against actin (e). Levels of phosphorylated eEF2 (P-eEF2) were quantified by densitometry and normalized against total eEF2 (f). NFAT-luciferase reporter activity (g) and MCIP-1 mRNA expression (h) were measured in lysates from rat cardiomyocytes treated with increasing concentrations of resveratrol. Values are the mean ± S.E.M. of n = 4 separate neonatal rat cardiomyocyte preparations in each group. * indicates asignificant difference (p < 0.05) between vehicle control and Resv-treated groups
To further examine the anti-hypertrophic actions of Resv, we measured NFAT-dependent transcriptional activity in NRCMs. To do this, we utilized an NFAT promoter-driven luciferase reporter gene to determine NFAT-mediated transcription. In addition, we measured the expression of an NFAT-regulated gene, modulatory calcineurin interacting protein 1 (MCIP-1), as a surrogate marker of NFAT-mediated transcriptional activity. As expected, Resv concentration dependently and significantly reduced NFAT-dependent transcription compared to vehicle-treated controls as judged by the reduced NFAT-luciferase reporter gene activity (Fig. 1g) and MCIP-1 mRNA expression (Fig. 1h) at concentrations that were below the level sufficient to inhibit protein synthesis. Together, these data indicate that low concentrations of Resv are efficient at selectively inhibiting important regulators involved in pathological LVH (such as NFAT) while not affecting pathways involved in physiological LVH (such as Akt and p70S6K).
Resveratrol inhibits mechanisms associated with the development of pathological cardiac hypertrophy
Since we observed differential effects on AMPK, p70S6K, and NFAT at 1 and 50 μM Resv, we investigated whether these two concentrations also induced similar changes in response to stimuli that is involved in promoting pathological LVH, namely Ang-II. To do this, NRCMs were treated with either vehicle (0 μM), 1 μM, or 50 μM Resv in the presence of hypertrophic stimuli Ang-II (1 μM) for 24 h and cells were harvested for immunoblot analysis and measurement of NFAT activity. In the absence of Resv, Ang-II did not affect AMPK phosphorylation (Fig. 2a), but significantly increased P-Akt (Fig. 2b) and phosphorylated T421/S424 p70S6K (P-p70S6K) (Fig. 2c, d) as well as NFAT-mediated transcriptional activity (Fig. 2e, f). In all instances of Ang-II induced activation, 1 and 50 μM Resv attenuated the levels of P-Akt, P-p70S6K, and NFAT-mediated transcription (Fig. 2b–f). Interestingly, 1 μM Resv was sufficient to return these molecular responses to Ang-II back to baseline (Fig. 2b–f). Moreover, the effect of 1 μM Resv occurred in the absence of AMPK activation (Fig. 2a) suggesting that AMPK was not responsible for these dramatic changes. Consistent with this, despite the effect of 50 μM Resv to significantly increase P-AMPK (Fig. 2a), the response of the other signaling pathways was either unchanged or only modestly altered (Figs. 2b–f).
Low concentrations of resveratrol (Resv) inhibits NFAT and induction of pathological hypertrophy in neonatal rat cardiomyocytes and hypertrophic SHRs. Cardiomyocytes were treated with either 1 or 50 μM resveratrol in the presence of hypertrophic stimuli Ang-II (1 μM) for 24 h. Immunoblot analysis of phosphorylated T172 AMPK (P-AMPK) levels were quantified by densitometry and normalized against total AMPK (a). Levels of phosphorylated S473 Akt (P-Akt) were quantified by densitometry and normalized against total Akt (b). Levels of phosphorylated T389 p70S6K (P-p70S6K) were quantified by densitometry and normalized against actin (c). Levels of phosphorylated T421/S424 p70S6K (P-p70S6K) were quantified by densitometry and normalized against actin (d). NFAT-luciferase reporter activity (e) and MCIP-1 mRNA expression (f) were measured in lysates from rat cardiomyocytes treated with increasing concentrations of resveratrol. Values are the mean ± S.E.M. of n = 4 separate neonatal rat cardiomyocyte preparations in each group. * indicates a significant difference (p < 0.05) between vehicle-treated and Resv-treated groups, § indicates a significant difference (p < 0.05) between control and Ang-II groups, ¶ indicates a significant difference (p < 0.05) between Ang-II and the Ang-II Resv-treated groups using ANOVA with a Bonferroni post-test
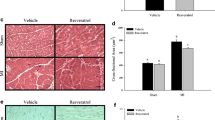
In order to confirm that Ang-II had similar effects on the cardiomyocytes in vivo, we utilized a mouse model of Ang-II infusion. Mice infused with Ang-II (1.4 mg/kg/day) for 2 weeks, exhibited cardiac LVH (increased heart weight to tibia length (HW/TL) ratio; Fig. 3a) and increased the expression of MCIP-1 (Fig. 3b), which is a surrogate marker of in vivo NFAT-dependent transcription [10]. In addition, Ang-II increased the expression of additional cardiac hypertrophy-associated genes, including atrial natriuretic factor (ANF) and brain natriuretic peptide (BNP), though not β-myosin heavy chain (MHC) in the heart (Fig. 3c). While Ang-II modestly reduced phosphorylation of AMPK in the heart (Fig. 3d), Ang-II infusion significantly increased the phosphorylation of both Akt and p70S6K compared to vehicle-treated mice (Fig. 3e, f). When Ang-II treated mice were co-administered Resv, cardiac LVH was prevented (Fig. 3a). This was associated with attenuated expression of MCIP-1 mRNA (Fig. 3b) as well as ANF and BNP, though β-MHC expression was unaffected by Resv (Fig. 3c). The addition of Resv to the Ang-II infusion maintained phosphorylation of AMPK (Fig. 3d), did not affect SIRT1 expression (Fig. S1c), and significantly reduced levels of both Akt (Fig. 3e) and p70S6K (Fig. 3f) phosphorylation in the heart. Together, these data suggest that Resv treatment of mice-administered Ang-II may reduce LVH by the activation of AMPK, inhibition of NFAT-mediated transcription, as well as by the significant attenuation of additional pro-hypertrophic pathways such as Akt and p70S6K.
Resveratrol (Resv) inhibits cardiac hypertrophy and MCIP-1 mRNA expression in angiotensin (Ang)-II infused mice. Heart weight to tibia length (HW/TL) ratios of mice infused with saline or Ang-II (1.4 mg/kg/day) and fed either a control diet or diet containing resveratrol (4 g/kg diet) (a). MCIP-1 mRNA expression relative to HPRT in mouse heart (b). ANF, BNP, and β-MHC mRNA expression relative to HPRT in mouse heart (c). Immunoblot analysis was performed on homogenates from heart tissue isolated from the four groups of mice. Levels of phosphorylated T172 AMPK (P-AMPK) were quantified by densitometry and normalized against total AMPK (d). Levels of phosphorylated S473 Akt (P-Akt) were quantified by densitometry and normalized against total Akt (e). Levels of phosphorylated T389 p70S6K (P-p70S6K) were quantified by densitometry and normalized against tubulin (f). Values are the mean ± S.E.M. of n = 6 mice/hearts in each group. § indicates a significant difference (p < 0.05) between control (saline) and Ang-II-infused groups, ¶ indicates a significant difference (p < 0.05) between Ang-II and the Ang-II Resv groups using ANOVA with a Bonferroni post-test
Resveratrol inhibits signaling pathways involved in a rat model of pathological cardiac hypertrophy
As increased Ang-II levels are also thought to be a contributing factor to the development of LVH in the spontaneously hypertensive rats (SHRs) [23], we investigated whether 5 weeks of Resv administration (4 g/kg diet) had any effect on LVH in the SHRs. SHRs displayed a significant increase in the HW/TL ratio (Fig. 4a) compared to untreated Wistar rats, which were associated with a significant increase in MCIP-1 gene expression (Fig. 4b). Consistent with previous studies [12, 18], hearts from SHRs displayed impaired AMPK signaling (Fig. 4c) and significantly elevated P-p70S6K (Fig. 4e) even in the absence of any changes in P-Akt (Fig. 4d). Of importance, Resv treatment of SHRs attenuated LVH in the SHRs (Fig. 4a) and normalized the expression of NFAT-regulated MCIP-1 gene expression (Fig. 4b). Moreover, Resv also attenuated P-p70S6K levels compared to untreated SHRs and maintained these levels similar to those observed in healthy hearts from Wistar controls (Fig. 4e). Collectively, these data confirm our findings in Ang-II-treated NRCMs and mice, that Resv prevents the induction of pathological LVH and this likely occurs via the inhibition of pro-hypertrophic pathways involving NFAT-mediated transcription as well as AMPK and p70S6K.
Resveratrol (Resv) inhibits cardiac hypertrophy and MCIP mRNA expression in spontaneously hypertensive rats (SHRs). Heart weight to tibia length (HW/TL) ratios in 15-week-old normotensive control Wistar rats, control SHRs, and SHRs fed with resveratrol (4 g/kg diet) (a). MCIP-1 mRNA expression in rat heart (b). Immunoblot analysis was performed on homogenates from heart tissue isolated from the three groups of rats. Levels of phosphorylated T172 AMPK (P-AMPK) were quantified by densitometry and normalized against total AMPK (c). Levels of phosphorylated S473 Akt (P-Akt) were quantified by densitometry and normalized against total Akt (d). Levels of phosphorylated T389 p70S6K (P-p70S6K) were quantified by densitometry and normalized against tubulin (e). Values are the mean ± S.E.M. of n = 5 rats/hearts in each group. * indicates a significant difference (p < 0.05) between SHRs and Wistar rats, # indicates a significant difference (p < 0.05) between SHR-control and SHR-Resv groups using ANOVA with a Bonferroni post-test
Resveratrol does not inhibit IGF-1-induced growth signaling pathways involved in cardiomyocyte growth
Physiological and/or adaptive LVH is well-established to occur during exercise [2]. Since rodents undergoing chronic exercise training have increased serum levels of IGF-1 [24, 25], and IGF-1 has been shown to induce cardiomyocyte hypertrophy [2, 26], we examined whether Resv altered the molecular response of NRCMs to IGF-1. To do this, we treated cultured NRCMs for 24 h with 100 nM IGF-1 in the presence of vehicle (0 μM), 1 μM, or 50 μM Resv. In the absence of Resv, IGF-1 did not affect levels of P-AMPK in NRCMs (Fig. 5a), but significantly increased Akt (Fig. 5b) and p70S6K (Fig. 5c, d) phosphorylation. In contrast to Ang-II, IGF-1 did not significantly increase NFAT-regulated transcriptional activity (Fig. 5e, f), suggesting that IGF-1 does not activate a major component responsible for the induction of pathological LVH. Interestingly, as opposed to what was observed with Ang-II, 1 μM Resv was not sufficient to blunt the IGF-1-induced responses with the exception of a minor reduction in NFAT-luciferase activity (Fig. 5b–f). However, 50 μM Resv resulted in a significant inhibition of IGF-1-induced p70S6K phosphorylation (Fig. 5c, d), which was associated with increased P-AMPK (Fig. 5a) and reduced P-Akt (Fig. 5b). This result suggests that either AMPK activation and/or Akt inhibition are necessary for Resv to blunt p70S6K activation by IGF-1. Importantly, our findings show that while lower concentrations of Resv are able to inhibit the activation of Akt and p70S6K in response to pathological stimuli such as Ang-II, they are not able to prevent the activation of these same pathways in response to physiological stimuli such as IGF-1.
Low concentrations of resveratrol (Resv) do not inhibit IGF-1-stimulated hypertrophy in rat cardiomyocytes. Cardiomyocytes were treated with either 1 or 50 μM Resv in the presence of hypertrophic stimuli IGF-1 (100 nM) for 24 h. Immunoblot analysis of phosphorylated T172 AMPK (P-AMPK) levels were quantified by densitometry and normalized against total AMPK (a). Levels of phosphorylated S473 Akt (P-Akt) were quantified by densitometry and normalized against total Akt (b). Levels of phosphorylated T389 p70S6K (P-p70S6K) were quantified by densitometry and normalized against actin (c). Levels of phosphorylated T421/S424 p70S6K (P-p70S6K) were quantified by densitometry and normalized against actin (d). NFAT-luciferase reporter activity (e) and MCIP-1 mRNA expression (f) were measured in lysates from rat cardiomyocytes treated with increasing concentrations of resveratrol. Values are the mean ± S.E.M. of n = 4–6 separate neonatal rat cardiomyocyte preparations in each group. * indicates a significant difference (p < 0.05) between vehicle-treated and Resv-treated groups, § indicates a significant difference (p < 0.05) between control and IGF-1 groups, ¶ indicates a significant difference (p < 0.05) between IGF-1 and the IGF-1 Resv-treated groups using ANOVA with a Bonferroni post-test
In order to confirm that IGF-1 had similar effects on the cardiomyocytes in vivo, we examined C57BL6 mice that received control chow or a Resv-containing diet during the administration of IGF-1. Vehicle or IGF-1 (4 mg/kg) was administered to mice via daily subcutaneous injections for a period of 7 days. In the absence of Resv, mice-administered IGF-1 exhibited cardiac LVH (increased HW/TL ratio; Fig. 6a) without alterations in NFAT-regulated MCIP-1 gene expression (Fig. 6b), compared to vehicle-treated controls. In addition, IGF-1 significantly reduced phosphorylation of AMPK and increased the phosphorylation of both Akt and p70S6K compared to vehicle-treated mice (Fig. 6c, d, e). However, unlike what was observed with Ang-II infusion, when IGF-1-treated mice were co-administered Resv, cardiac LVH was not prevented (Fig. 6a). This finding is associated with Resv treatment not preventing a rise in the phosphorylation of p70S6K (Fig. 6e) or preventing a drop in the phosphorylation of AMPK (Fig. 6c). In contrast, the rise in IGF-1-induced Akt phosphorylation was partially prevented by Resv although this response had no effect on p70S6K phosphorylation or hypertrophic growth. Together, these data suggest that Resv treatment of mice-administered IGF-1 fails to activate AMPK and that this may be necessary for the ability of Resv to inhibit p70S6K and subsequent cardiac LVH.
Resveratrol (Resv) does not inhibit IGF-1-induced cardiac hypertrophy and p70S6K in the mouse heart. Mice consumed control diets or diets containing Resv (4 g/kg diet) throughout the administration of 4 mg/kg/day of IGF-1 to induce cardiac hypertrophy and compared to non-hypertrophic mice-administered vehicle (saline). Heart weight to tibia length (HW/TL) ratios (a). Mouse heart MCIP-1 mRNA expression (b). Immunoblot analysis was performed on homogenates from heart tissue isolated from the three groups of mice. Levels of phosphorylated T172 AMPK (P-AMPK) were quantified by densitometry and normalized against total AMPK (c). Levels of phosphorylated S473 Akt (P-Akt) were quantified by densitometry and normalized against total Akt (d). Levels of phosphorylated T389 p70S6K (P-p70S6K) were quantified by densitometry and normalized against tubulin (e). Values are the mean ± S.E.M. of n = 5 mice/hearts in each group. * indicates a significant difference (p < 0.05) between vehicle saline and IGF-1 treated groups, § indicates a significant difference (p < 0.05) between IGF-1 control and IGF-1 Resv groups using ANOVA with a Bonferroni post-test
Resveratrol does not inhibit signaling pathways involved in controlling the development of cardiac hypertrophy during exercise
Since chronic exercise training increases serum levels of IGF-1 [24, 25], but Resv failed to prevent LVH in IGF-1 treated mice, we investigated whether Resv had any effects of exercise-induced LVH. To do this, we examined the effects of Resv administration to rats undergoing 12 weeks of treadmill exercise training. Exercise training of rats increased the HW/TL by approximately 18 % (Fig. 7a), which was similar to the extent of hypertrophy observed in the SHRs (Fig. 4a). Notably, Resv did not significantly alter the HW/TL ratio in normal healthy sedentary Wistar rats (Fig. 7a), nor did it prevent the exercise-induced increase in HW/TL (Fig. 7a). As expected, exercise training did not increase the mRNA expression of MCIP-1, ANF, BNP, or β-MHC in the rat heart (Fig. 7b, c), as was observed in pathological models of LVH (Figs. 3b, c and 4b). In fact, exercise training reduced MCIP-1, ANF, BNP, and β-MHC mRNA levels in the rat heart (Fig. 7b, c). In addition, Resv did not significantly affect the cardiac expression of MCIP-1 in healthy sedentary rats (Fig. 7b) and the combination of Resv and exercise training did not further reduce MCIP-1 mRNA expression induced by exercise alone (Fig. 7b). Consistent with this, the combination of Resv with exercise training did not further reduce the mRNA expression of the ANF, BNP, or β-MHC genes in the rat heart (Fig. 7c). Collectively, these findings rule out NFAT activation as being involved in the exercise-induced LVH. In addition, although Resv administered in combination with exercise training stimulated P-AMPK (Fig. 7d), it did not significantly decrease P-Akt or P-p70S6K levels in the heart (Fig. 7e, f), suggesting that Resv does not alter the response of these kinases to physiological stimuli involved in promoting adaptive cardiac hypertrophy.
Resveratrol (Resv) does not inhibit exercise-induced cardiac hypertrophy in Wistar rats. Heart weight to tibia length (HW/TL) ratios in sedentary and treadmill-trained rats and fed control or resveratrol (4 g/kg diet) containing diets (a). MCIP-1 mRNA expression relative to HPRT in rat heart (b). ANF, BNP, and β-MHC mRNA expression relative to HPRT in rat heart (c). Immunoblot analysis was performed on homogenates from heart tissue isolated from Control or resveratrol-treated rats. Levels of phosphorylated T172 AMPK (P-AMPK) were quantified by densitometry and normalized against total AMPK (d). Levels of phosphorylated S473 Akt (P-Akt) were quantified by densitometry and normalized against total Akt (e). Levels of phosphorylated T389 p70S6K (P-p70S6K) were quantified by densitometry and normalized against actin (f). Values are the mean ± S.E.M. of n = 6 rats/hearts in each group. * indicates a significant difference (p < 0.05) between control and Resv groups, § indicates a significant difference (p < 0.05) between sedentary and exercise groups using ANOVA with a Bonferroni post-test
Resveratrol modifies P-AMPK, P-Akt, and P-p70S6K levels in human heart explants
To examine whether the effects of Resv on these important molecular signaling pathways are preserved in human hearts, we treated explanted atrial tissues (obtained from patients that have undergone CABG surgery) with Resv for 24 h. Although 1 μM Resv did not alter P-AMPK levels in these explants, consistent with our findings utilizing NRCMs, 24 h treatment of explanted atrial tissue with 50 μM Resv increased P-AMPK (Fig. 8a). Similarly, while treatment of these explants with 1 μM Resv for 24 h did not affect P-Akt or P-p70S6K levels, 50 μM Resv significantly reduced both P-Akt (Fig. 8b) and P-p70S6K (Fig. 8c) levels. Together, these data show that 50 μM Resv inhibited the kinases responsible for controlling cardiomyocyte protein synthesis, suggesting that Resv may also control LVH in humans.
Resveratrol (Resv) activates AMPK and inhibits hypertrophic signaling pathways in human left atrial explanted atrial tissues. Explanted tissues were treated with either 1 or 50 μM Resv for 24 h and flash frozen in liquid nitrogen for subsequent immunoblot analysis. Levels of phosphorylated T172 AMPK (P-AMPK) were quantified by densitometry and normalized against total AMPK (a). Levels of phosphorylated S473 Akt (P-Akt) were quantified by densitometry and normalized against total Akt (b). Levels of phosphorylated T389 p70S6K (P-p70S6K) were quantified by densitometry and normalized against actin (c). Values are the mean ± S.E.M. of n = 6 human atrial tissues in each group and * indicates a significant difference (p < 0.05) using a student’s t test between vehicle-treated and Resv-treated explants
Discussion
The major findings of our study are that: (1) Resv can concentration/dose selectively inhibit various pro-hypertrophy signaling pathways and (2) Resv has differential effects on the modification of these signaling cascades in response to pathological stimuli versus physiological stimuli. For the former, in the absence of pro-hypertrophic stimuli, low concentrations of Resv (0.1 and 1 μM) are efficient at selectively inhibiting important regulators involved in pathological LVH (such as NFAT) while not affecting pathways involved in physiological LVH (such as AMPK, Akt, and p70S6K). While the activation of SIRT1 by Resv has been correlated with reduced hypertrophy [27], research using transgenic rodent models has demonstrated that the effect of SIRT1 on the growth of the myocardium is dependent upon its level of expression [11]. In our experiments, we did not observe that Resv affected SIRT1 expression in isolated cardiomyocytes nor in the mouse and rat models of LVH (Fig. S1), suggesting that increased SIRT1 expression is not involved in the effects of Resv on the hypertrophic growth of the cardiomyocyte at these lower concentrations. However, since concentrations of 25 μM have been shown in cultured cells to be nontoxic and less damaging than 50 μM [28], these lower concentrations may more closely represent specific effects of Resv as opposed to secondary effects in response to cellular damage. In addition, these low concentrations of Resv are more likely to be achieved in vivo, and thus may be more reflective of physiological responses to Resv treatment.
Equally important as the concentration/dose selective inhibition of various pro-hypertrophy signaling pathways is the striking difference that 1 μM of Resv has on these pathways in response to pathological stimuli versus physiological stimuli. For instance, while a lower concentration of Resv is able to inhibit the activation of Akt and p70S6K in response to pathological stimuli such as Ang-II, it is not able to prevent the activation of these same pathways in response to physiological stimuli such as IGF-1. These same responses are also observed in vivo and across species (i.e., rat and mouse) confirming that the control of these pathways by Resv contributes to differential effects of the development of LVH.
Based on previous studies, feeding mice and rats these doses of Resv used herein results in plasma Resv levels between 10 and 120 ng/ml, respectively [29, 30]. However, the concentration needed to produce similar results in cultured cells is considerably higher than what may result from higher doses of Resv feeding in vivo. Although it is not currently known why this is, a metabolite of Resv could be responsible for the reported effects and the level of this metabolite could presumably be much lower in cultured cells. Alternatively, Resv may accumulate in cells in vivo and the concentration in the cells/tissues may be higher than that observed in blood, or in specific cells. It is also possible that Resv metabolites may be regenerated back to the parent compound, thus increasing the cellular concentration of Resv [31].
In agreement with previous findings [10], it is clear from our data that NFAT activation occurs in response to stimuli that promotes pathological LVH and not physiological LVH. As such Resv play less of a role in regulating NFAT-mediated transcription during physiological LVH. Consistent with this, previous in vivo studies demonstrated that Resv prevented pressure overload [13, 32] and hypertension-induced [12, 14, 16, 18, 33] cardiac hypertrophy, yet did not affect exercise-induced [19] or volume overload-induced [32] cardiac hypertrophy. However, what is not clear is how Resv regulates Akt and p70S6K differently depending on the type of pro-hypertrophic stimuli. One obvious possibility is that stimuli that promote pathological LVH versus physiological LVH work through different upstream kinases to regulate Akt and p70S6K phosphorylation and that Resv acts to inhibit only one of these pathways. While this is an attractive hypothesis, we have yet to test this possibility.
Another interesting component of our study is the information that is provided about the involvement of AMPK in the anti-hypertrophic effects of Resv. In all of the experiments involving the low concentrations of Resv, the observed effects on Akt, p70S6K, and NFAT were independent from AMPK activation. However, with a higher dose of Resv (50 μM), almost all of the observed effects on Akt, p70S6K, and NFAT were potentiated by AMPK activation. This finding is consistent with previous observations that there are overlapping effects of Resv that are both AMPK-dependent and AMPK-independent [11, 28, 34]. Interestingly, we observed some variable responses with respect to AMPK activation of LVH in our animal models. For instance, LVH is prevented by Resv in the Ang-II and SHRs models (which have elevated P-AMPK) and not in the IGF-1 model (which has no increase in P-AMPK). However, LVH is not suppressed in the exercise model (which has elevated P-AMPK). Together, these findings demonstrate that AMPK activation may be partially responsible for mediating some of the anti-hypertrophic effects of Resv but that other AMPK-independent pathways may also be involved.
One limitation of our experiments is that we have not provided histological quantification of cardiomyocyte cross sectional area to support that cardiomyocyte cell growth is occurring. That said, our echocardiographic data as well as HW/TL data support our claims that cardiac hypertrophy is occurring in our animal models. Nevertheless, even though we show changes in signaling controlling protein synthesis, we do not demonstrate cardiomyocyte growth. In addition, our previously published findings demonstrated that Resv lowers blood pressure in Ang-II-infused mice and SHRs [18]. Thus, we cannot conclude that the cardiac effects observed in these in vivo models are due to Resv acting directly on the cardiomyocytes. In fact, the molecular changes that we attribute to Resv may result secondary to the anti-hypertensive effects of Resv. However, given that similar signaling pathways are altered by Resv in isolated cardiomyocytes, we can speculate that at least part of the effects observed in the heart are due to direct signaling effects of Resv in the cardiomyocyte. However, based on these limitations, we cannot unequivocally state that cardiomyocyte growth is altered by Resv treatment.
In summary, we show that Resv can concentration/dose selectively inhibit various pro-hypertrophy signaling pathways and that the modification of these pathways differ in response to pathological stimuli or physiological stimuli. We also show that the anti-hypertrophic effects of Resv have AMPK-dependent and AMPK-independent effects. While all of the complex interactions involved in the anti-hypertrophic effects of Resv are yet to be fully elucidated, it is clear from our findings that Resv is effective at inhibiting pathological LVH and not physiological LVH. Moreover, we also show that Resv is able to modulate many of the same signaling pathways in human atrial samples, indicating that Resv may also control LVH in humans. Together, this study has important clinical implications as our findings support the concept that Resv may be useful in the treatment of pathological LVH and/or in the early treatment of conditions such as hypertension where adaptive LVH is necessary but a transition into pathological LVH can be prevented.
References
Lorell BH, Carabello BA (2000) Left ventricular hypertrophy: pathogenesis, detection, and prognosis. Circulation 102:470–479
Ellison GM, Waring CD, Vicinanza C, Torella D (2012) Physiological cardiac remodelling in response to endurance exercise training: cellular and molecular mechanisms. Heart 98:5–10
Hannan RD, Jenkins A, Jenkins AK, Brandenburger Y (2003) Cardiac hypertrophy: a matter of translation. Clin Exp Pharmacol Physiol 30:517–527
Dolinsky VW, Dyck JR (2006) Role of AMP-activated protein kinase in healthy and diseased hearts. Am J Physiol Heart Circ Physiol 291:H2557–H2569
Zarrinpashneh E, Beauloye C, Ginion A, Pouleur AC, Havaux X, Hue L, Viollet B, Vanoverschelde JL, Bertrand L (2008) AMPKalpha2 counteracts the development of cardiac hypertrophy induced by isoproterenol. Biochem Biophys Res Commun 376:677–681
Chan AY, Dolinsky VW, Soltys CL, Viollet B, Baksh S, Light PE, Dyck JR (2008) Resveratrol inhibits cardiac hypertrophy via AMP-activated protein kinase and Akt. J Biol Chem 283:24194–24201
Chan AY, Soltys CL, Young ME, Proud CG, Dyck JR (2004) Activation of AMP-activated protein kinase inhibits protein synthesis associated with hypertrophy in the cardiac myocyte. J Biol Chem 279:32771–32779
Li HL, Yin R, Chen D, Liu D, Wang D, Yang Q, Dong YG (2007) Long-term activation of adenosine monophosphate-activated protein kinase attenuates pressure-overload-induced cardiac hypertrophy. J Cell Biochem 100:1086–1099
Molkentin JD, Lu JR, Antos CL, Markham B, Richardson J, Robbins J, Grant SR, Olson EN (1998) A calcineurin-dependent transcriptional pathway for cardiac hypertrophy. Cell 93:215–228
Wilkins BJ, Dai YS, Bueno OF, Parsons SA, Xu J, Plank DM, Jones F, Kimball TR, Molkentin JD (2004) Calcineurin/NFAT coupling participates in pathological, but not physiological, cardiac hypertrophy. Circ Res 94:110–118
Dolinsky VW, Dyck JR (2014) Experimental studies of the molecular pathways regulated by exercise and resveratrol in heart, skeletal muscle and the vasculature. Molecules 19:14919–14947
Dolinsky VW, Chan AY, Robillard Frayne I, Light PE, Des Rosiers C, Dyck JR (2009) Resveratrol prevents the prohypertrophic effects of oxidative stress on LKB1. Circulation 119:1643–1652
Juric D, Wojciechowski P, Das DK, Netticadan T (2007) Prevention of concentric hypertrophy and diastolic impairment in aortic-banded rats treated with resveratrol. Am J Physiol Heart Circ Physiol 292:H2138–H2143
Liu Z, Song Y, Zhang X, Liu Z, Zhang W, Mao W, Wang W, Cui W, Zhang X, Jia X et al (2005) Effects of trans-resveratrol on hypertension-induced cardiac hypertrophy using the partially nephrectomized rat model. Clin Exp Pharmacol Physiol 32:1049–1054
Rimbaud S, Ruiz M, Piquereau J, Mateo P, Fortin D, Veksler V, Garnier A, Ventura-Clapier R (2011) Resveratrol improves survival, hemodynamics and energetics in a rat model of hypertension leading to heart failure. PLoS One 6:e26391
Thandapilly SJ, Wojciechowski P, Behbahani J, Louis XL, Yu L, Juric D, Kopilas MA, Anderson HD, Netticadan T (2010) Resveratrol prevents the development of pathological cardiac hypertrophy and contractile dysfunction in the SHR without lowering blood pressure. Am J Hypertens 23:192–196
Toklu HZ, Sehirli O, Ersahin M, Suleymanoglu S, Yiginer O, Emekli-Alturfan E, Yarat A, Yegen BC, Sener G (2010) Resveratrol improves cardiovascular function and reduces oxidative organ damage in the renal, cardiovascular and cerebral tissues of two-kidney, one-clip hypertensive rats. J Pharm Pharmacol 62:1784–1793
Dolinsky VW, Chakrabarti S, Pereira TJ, Oka T, Levasseur J, Beker D, Zordoky BN, Morton JS, Nagendran J, Lopaschuk GD et al (2013) Resveratrol prevents hypertension and cardiac hypertrophy in hypertensive rats and mice. Biochim Biophys Acta 1832:1723–1733
Dolinsky VW, Jones KE, Sidhu RS, Haykowsky M, Czubryt MP, Gordon T, Dyck JR (2012) Improvements in skeletal muscle strength and cardiac function induced by resveratrol contribute to enhanced exercise performance in rats. J Physiol 590:2783–2799
Dolinsky VW, Rueda-Clausen CF, Morton JS, Davidge ST, Dyck JR (2011) Continued postnatal administration of resveratrol prevents diet-induced metabolic syndrome in rat offspring born growth restricted. Diabetes 60:2274–2284
Dolinsky VW, Rogan KJ, Sung MM, Zordoky BN, Haykowsky MJ, Young ME, Jones LW, Dyck JR (2013) Both aerobic exercise and resveratrol supplementation attenuate doxorubicin-induced cardiac injury in mice. Am J Physiol Endocrinol Metab 305:E243–E253
Kovacic S, Soltys CL, Barr AJ, Shiojima I, Walsh K, Dyck JR (2003) Akt activity negatively regulates phosphorylation of AMP-activated protein kinase in the heart. J Biol Chem 278:39422–39427
Mizutani S, Ishii M, Hattori A, Nomura S, Numaguchi Y, Tsujimoto M, Kobayshi H, Murohara T, Wright JW (2008) New insights into the importance of aminopeptidase A in hypertension. Heart Fail Rev 13:273–284
Neri Serneri GG, Boddi M, Modesti PA, Cecioni I, Coppo M, Padeletti L, Michelucci A, Colella A, Galanti G (2001) Increased cardiac sympathetic activity and insulin-like growth factor-I formation are associated with physiological hypertrophy in athletes. Circ Res 89:977–982
Yeh JK, Aloia JF, Chen M, Sprintz S (1994) Effect of growth hormone administration and treadmill exercise on the body composition of rats. J Appl Physiol (1985) 77:23–29
McMullen JR, Jennings GL (2007) Differences between pathological and physiological cardiac hypertrophy: novel therapeutic strategies to treat heart failure. Clin Exp Pharmacol Physiol 34:255–262
Sundaresan NR, Pillai VB, Gupta MP (2011) Emerging roles of SIRT1 deacetylase in regulating cardiomyocyte survival and hypertrophy. J Mol Cell Cardiol 51:614–618
Price NL, Gomes AP, Ling AJ, Duarte FV, Martin-Montalvo A, North BJ, Agarwal B, Ye L, Ramadori G, Teodoro JS et al (2012) SIRT1 is required for AMPK activation and the beneficial effects of resveratrol on mitochondrial function. Cell Metab 15:675–690
Lagouge M, Argmann C, Gerhart-Hines Z, Meziane H, Lerin C, Daussin F, Messadeq N, Milne J, Lambert P, Elliott P et al (2006) Resveratrol improves mitochondrial function and protects against metabolic disease by activating SIRT1 and PGC-1alpha. Cell 127:1109–1122
Baur JA, Pearson KJ, Price NL, Jamieson HA, Lerin C, Kalra A, Prabhu VV, Allard JS, Lopez-Lluch G, Lewis K et al (2006) Resveratrol improves health and survival of mice on a high-calorie diet. Nature 444:337–342
Patel KR, Andreadi C, Britton RG, Horner-Glister E, Karmokar A, Sale S, Brown VA, Brenner DE, Singh R, Steward WP et al (2013) Sulfate metabolites provide an intracellular pool for resveratrol generation and induce autophagy with senescence. Sci Transl Med 5:205ra133
Wojciechowski P, Juric D, Louis XL, Thandapilly SJ, Yu L, Taylor C, Netticadan T (2010) Resveratrol arrests and regresses the development of pressure overload- but not volume overload-induced cardiac hypertrophy in rats. J Nutr 140:962–968
Chan V, Fenning A, Iyer A, Hoey A, Brown L (2011) Resveratrol improves cardiovascular function in DOCA-salt hypertensive rats. Curr Pharm Biotechnol 12:429–436
Um JH, Park SJ, Kang H, Yang S, Foretz M, McBurney MW, Kim MK, Viollet B, Chung JH (2010) AMP-activated protein kinase-deficient mice are resistant to the metabolic effects of resveratrol. Diabetes 59:554–563
Acknowledgments
The authors acknowledge the excellent technical assistance of Jamie Boisvenuee, Amy Barr, Jody Levasseur, and Yang Zhao of the University of Alberta. This research was supported by grants from the Canadian Institutes of Health Research (CIHR) to JRBD. VWD is the Dr. J.A. Moorhouse fellow of the Diabetes Foundation of Manitoba. AYMC was a holder of a HSFC Doctoral Research Award and an AHFMR MD/PhD Studentship Award.
Conflict of interest
There are no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOC 728 kb)
Rights and permissions
About this article
Cite this article
Dolinsky, V.W., Soltys, CL.M., Rogan, K.J. et al. Resveratrol prevents pathological but not physiological cardiac hypertrophy. J Mol Med 93, 413–425 (2015). https://doi.org/10.1007/s00109-014-1220-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00109-014-1220-8